How Do You Choose a Second-Line Treatment Option for Depression?
A majority of patients with major depression do not remit or adequately respond to initial antidepressant therapy. When response is insufficient, a diagnosis of depression and any comorbidities should be confirmed, treatment adherence should be established, and antidepressant dosages should be optimized as tolerated. If response is still insufficient, then implementing second-line treatment strategies is warranted. Second-line strategies of switching to or combining/augmenting the initial agent with one of a variety of antidepressant medications and/or psychotherapies improves remission rates, although no single approach or agent has demonstrated clear superiority over any other. Second-line treatment selections should be driven by safety considerations, patients’ symptom profiles, and patient preference. Comorbid medical conditions, especially cardiac and cerebrovascular complications, and potential drug-drug interactions should be considered when making treatment decisions.
(J Clin Psychiatry 2010;71[suppl 1]:21-26)
From the Department of Psychiatry, University of North Carolina, Chapel Hill; Department of Psychiatry, Duke University, Durham, North Carolina; and private practice, Raleigh, North Carolina.
This article is derived from the planning teleconference series “Looking Past First-Line Therapy for Major Depressive Disorder,” which was held in January 2010 and supported by an educational grant from AstraZeneca.
Dr Weisler has been/is a member of the speakers bureaus for Abbott, AstraZeneca, Biovail, Bristol-Myers Squibb, Burroughs Wellcome, Cephalon, Ciba Geigy, Eli Lilly, Forest, GlaxoSmithKline, Janssen, Johnson & Johnson, Novartis, Organon, Pfizer, Sanofi, Sanofi-Synthelabo, Shire, Solvay, Validus, and Wyeth; has been/is a consultant for Abbott, AstraZeneca, Biovail, Bristol-Myers Squibb, Cephalon, Corcept, Eli Lilly, Forest, GlaxoSmithKline, Johnson & Johnson, Otsuka, Pfizer, Pharmacia, ProPhase, Sanofi, Sanofi-Synthelabo, Shire, Solvay, Takeda, Validus, and Wyeth; has received/is receiving research support from Abbott, AstraZeneca, Biovail, Bristol-Myers Squibb, Burroughs Wellcome, Cenerx, Cephalon, Ciba Geigy, CoMentis, Dainippon Sumitomo, Eisai, Eli Lilly, Forest, GlaxoSmithKline, Janssen, Johnson & Johnson, Lundbeck, McNeil, Medicinova, Merck, the National Institute of Mental Health, Neurochem, New River, Novartis, Organon, Pfizer, Pharmacia, Repligen, Saegis, Sandoz, Sanofi, Sanofi-Synthelabo, Schwabe/Ingenix, Sepracor, Shire, Synaptic, Takeda, TAP, UCB, Vela, and Wyeth; and was/is a stock shareholder of Bristol-Myers Squibb, Cortex, Merck, and Pfizer.
Corresponding author: Richard H. Weisler, MD, 700 Spring Forest Rd, Ste 125, Raleigh, NC 27609 ([email protected]).
doi:10.4088/JCP.9104su1c.04
© Copyright 2010 Physicians Postgraduate Press, Inc.
Adults with major depressive disorder (MDD) are at a high risk for having functional impairments and psychiatric and medical comorbidities. On average, people with serious mental illness, including MDD, die 25 years earlier than the general population.1 Recurrent depressive and/or severe episodes are associated with worse patient outcomes, so selecting an effective first-line treatment is paramount. Unfortunately, nonresponse or partial response to antidepressant therapy is common, and only a minority of patients will achieve full remission after initial treatment.2 Thus, to help patients achieve remission, which will in turn reduce their risk of depressive relapse and improve their functioning and quality of life, clinicians should be knowledgeable of assessing treatment response and selecting and implementing effective second-line treatment strategies for major depression.
Unsuccessful First-Line Treatment
To determine if initial antidepressant treatment is successful, clinicians must objectively assess whether or not a patient has achieved remission. For an in-depth review of defining and assessing treatment response and remission, see the article in this supplement by Roger S. McIntyre, MD, FRCPC, “When Should You Move Beyond First-Line Therapy for Depression?”3
For Clinical Use
- Systematically assess patients’ treatment response, and, when insufficient, confirm the unipolar diagnosis, ensure treatment adherence, and optimize the dosage before initiating second-line treatment strategies.
- Select second-line treatments according to patients’ symptom profiles, adverse event profiles, medical histories, and treatment preferences.
- Be aware of patients’ current medication regimens so as to avoid potentially harmful drug-drug interactions; encourage patients to adhere to minimal or no use of alcohol and to abstain from illicit and licit drug abuse.
A poor response to first-line antidepressant therapy could also be indicative of undiagnosed bipolar disorder. Bipolar disorder is often misdiagnosed as MDD4 because many patients only seek treatment during one of their more frequently occurring depressive episodes, making mania or hypomania and other indications of bipolarity difficult to detect. All patients presenting with depressive symptomatology should be screened for past mania or hypomania, and clinicians should familiarize themselves with risk factors for bipolar depression, such as an early age at depression onset, higher episode recurrence, or a family history of bipolar disorder,5 among others. Getting input from significant others about past or present symptoms of mania or hypomania can be helpful.
If a patient has not sufficiently responded to initial antidepressant treatment, clinicians should ensure that the prescribed dose and duration were adequate; this is the recommended first step when entering the second-line treatment phase, though optimization can be difficult due to patient-specific variables. For instance, blood level measurements of tricyclic antidepressants (TCAs) show tremendous variability among individuals, complicating the predictability of attaining therapeutic dosages based on individual’s size, gender, or ethnicity. With some of the newer antidepressants, such as the selective serotonin reuptake inhibitors (SSRIs) and the serotonin-norepinephrine reuptake inhibitors (SNRIs), dose optimization in patients who are not responding optimally is, in some ways, even more difficult because blood level measurements are not typically useful. The generally accepted antidepressant optimization strategy is to steadily uptitrate the dose within approved ranges until the patient responds to the medication or experiences intolerable side effects.
Treatment nonadherence is also a major issue when treating any condition, particularly depression. Many patients may falsely report being adherent; may improperly take the medication and inadvertently increase the occurrence of adverse events, which can contribute to nonadherence; or may initially comply with the medication regimen but, after time, only take it intermittently, which can lead to withdrawal symptoms or increased depressive symptoms that might be mistaken for a depressive relapse despite still being on medication. Educating patients and their families about the importance of treatment adherence, particularly about faithfully taking the medication at the correct time, in the proper fashion (ie, with or without food and with an awareness of concomitant medications), and for the established duration, has been shown to substantially improve patients’ adherence,6 thereby increasing treatment response rates.
After confirming a diagnosis of unipolar depression, if a patient is not sufficiently responsive to the optimized dose of an initial antidepressant and adherence is not an issue, or if a patient experienced intolerable adverse effects from the initial antidepressant, then second-line treatment options must be considered.
Selecting Second-Line Treatments
After initial antidepressant therapy is deemed unsuccessful, several second-line pharmacologic strategies are available, such as switching to a different antidepressant, combining the initial antidepressant with a second antidepressant, or augmenting the antidepressant with a nonantidepressant (eg, a mood stabilizer). Several antidepressants are currently available to use in second-line switching or combination strategies (Table 1).7 Nonantidepressant augmentation options include the mood stabilizers lithium, lamotrigine, and divalproex; the thyroid hormones triiodothyronine (T3) and thyroxine (T4); psychostimulants; and atypical antipsychotics. Some research also suggests augmenting with l-methylfolate can be helpful even when folate levels are within the normal range.8
Patient Symptomatology
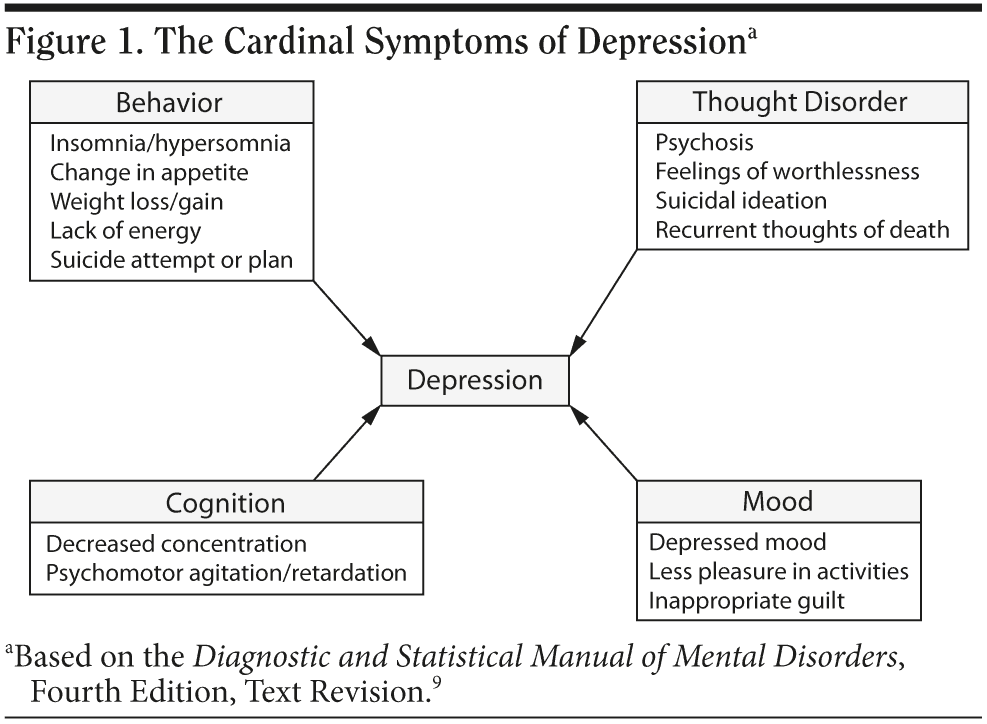
Clinicians should choose a second-line treatment according to a patient’s individual symptom profile, history of adverse events or family history of response to particular medications, and preference. The cardinal symptoms of depression can be categorized as behavior, thought disorder, cognition, and mood, which can help guide treatment selection (Figure 1).9
Behavior. Behavioral symptoms in depression include insomnia or hypersomnia, changes in appetite or weight, lack of energy, and suicide attempts or plans. For patients experiencing insomnia, clinicians might choose a sedating antidepressant such as mirtazapine, trazodone, or occasionally certain TCAs. For example, the SSRI paroxetine may be more sedating than other SSRIs for some patients, or, if augmenting a nonsedating antidepressant, the atypical antipsychotics quetiapine or olanzapine might be useful. For patients with depression experiencing hypersomnia, clinicians might initially consider a more activating medication such as bupropion or a monoamine oxidase inhibitor (MAOI) or, for augmentation, aripiprazole. While this approach of selecting treatment based on adverse event profiles is commonly used, clinicians may often find that some patients respond paradoxically. For example, they will not be sedated on drugs thought to be potentially sedating or be activated by drugs thought to be potentially activating.
Many patients with MDD experience a decreased appetite, which may cause significant weight loss. In these cases, choosing an effective antidepressant with the known potential for appetite stimulation, such as mirtazapine, TCAs, or paroxetine, could be beneficial, but just treating the underlying depression with any antidepressant may improve appetite, or vice versa. Among the adjunctive agents, quetiapine or olanzapine may increase appetite and weight. If weight gain or obesity is an issue, clinicians can prescribe medications with less of an impact on appetite, such as bupropion or augmentation with aripiprazole. As previously noted with sedation, some patients may not gain weight when taking medications generally considered likely to increase appetite. Patients should always be encouraged to follow a proper diet and to exercise, which may increase energy levels. Guidance from The Texas Medication Algorithm Project (TMAP)7 recommends that patients with depression exercise (eg, walk, jog, swim) at least 3 times weekly for at least 30 minutes each time; other guidance suggests 150 minutes or more of moderate physical activity per week. As with insomnia, choosing a more activating antidepressant, or at least trying to minimize daytime sedation, may also help some patients maintain regular energy levels.
Previous suicide attempts and repeated self-harm are also behavioral symptoms and are predictive of future suicide attempts and completed suicide.10 A survey10 of hospitalized patients who had attempted suicide found that time from a suicidal thought to an actual suicide attempt was often as little as 10 minutes. For patients at a risk for suicide attempt, clinicians may want to consider augmentation strategies because switching medications risks losing any benefit received from the initial antidepressant and could theoretically increase suicidality. Potentially shortening the time to response is also important in patients who are thought to be at risk for suicide, which may strengthen the argument for augmenting antidepressant monotherapy, if the primary antidepressant is tolerated.
Thoughts. Psychosis, including delusional feelings of worthlessness and guilt, and significant recurrent suicidal thoughts and ideation are critical for clinicians to assess and treat for patients with depression. Antidepressant monotherapy is usually inadequate; this population may respond best to an antidepressant plus an atypical antipsychotic. Electroconvulsive therapy (ECT) is also a reasonable option.7
Suicidal thoughts and feelings of worthlessness are common in depression and should be assessed regularly and monitored carefully, particularly when starting, titrating, augmenting, or discontinuing antidepressants. Fortunately, when patients respond well to depression treatment, suicide risk sharply declines, regardless of the intervention used; although antidepressants do have a black-box warning for increased suicidality in patients younger than 25 years. Adjunctive lithium is efficacious, in some cases, in reducing suicide risk and has a strong evidence base supporting its role in the reduction of suicidality.11 Most importantly, achieving improvement, or optimally, remission of depressive symptoms usually leads to diminution or the loss of suicidal thoughts and behaviors.
Cognition. Patients with MDD have been shown to have hippocampal volume loss, which can negatively affect cognitive functioning, particularly in areas of memory and concentration.12 These deficits in cognitive functioning can help clinicians to select appropriate medications. For example, tricyclic-like antidepressants or antidepressants with significant muscarinic receptor-activating properties may adversely impact depressed patients’ memory more so than other, less anticholinergic agents.
The presence of psychomotor agitation or retardation, both of which fall within the cognition category, may be addressed by selecting agents that are either more activating or more sedating than others. Atypical antipsychotic augmentation can be useful in reducing agitation, although these agents can carry an increased risk for akathisia, which could exacerbate agitation in some cases. Akathisia can usually be managed by dose reduction and/or benzodiazepines, β-blockers, or benztropine, or just a careful monitored period of waiting to allow accommodation.
Mood. Primary symptoms of depression include depressed mood and loss of pleasure in once enjoyable activities; the mood category also encompasses inappropriate guilt. Some patients who experience extreme, nearly delusional levels of guilt may feel convinced that they are bad people or failures, which may exacerbate the depression and create additional mood problems. Clinicians should follow the general treatment guidelines for depression when treating mood symptoms, but, if the mood issues are severe, augmentation with a mood stabilizer or an atypical antipsychotic could be required. Patients with strong feelings of guilt may also be candidates for psychotherapy, as are those with low self-esteem, anxiety, or relationship or substance abuse problems.
Cardiovascular Events
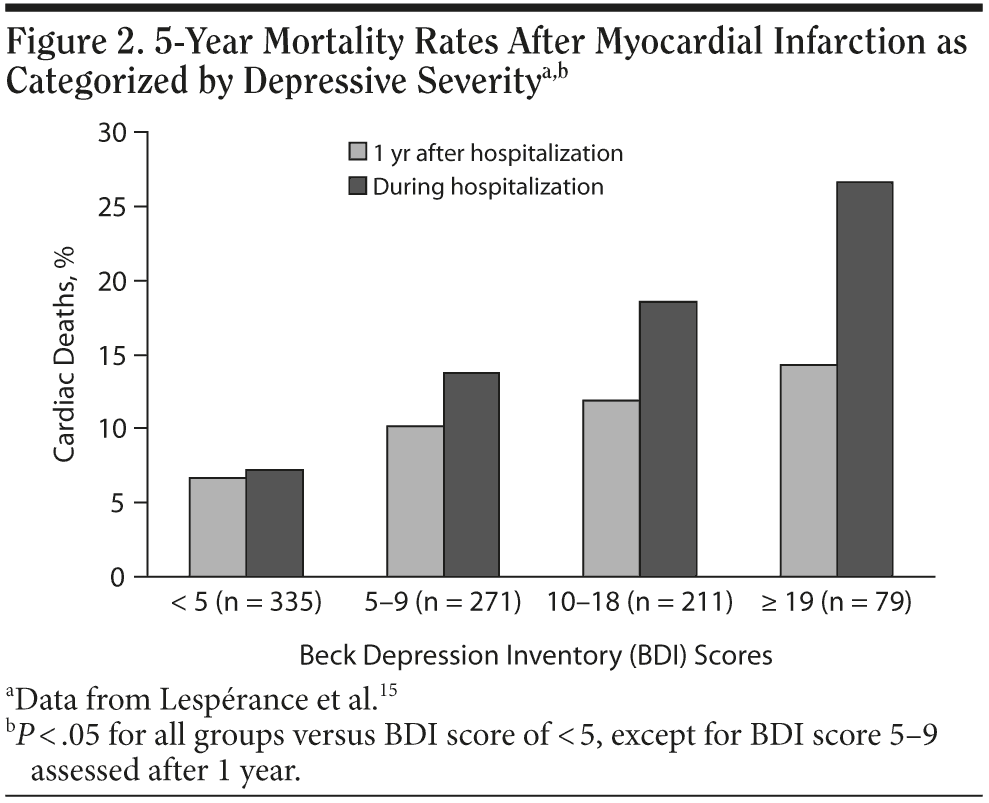
Major depression is associated with an increased risk of coronary heart disease, ischemic heart disease, myocardial infarction (MI), and cardiac mortality, but the relationship has not been definitively established.13-16 For example, men experiencing a depressive episode during the previous 10 years had a 3-fold increase in risk for developing ischemic heart disease compared with the control group (P = .01).13 Lespérance et al14 reported that 27.5% of patients hospitalized for MI had 1 or more previous episodes of major depression, and approximately one-fourth experienced depression during hospitalization. Compared with lower depression scores, higher depression scores assessed during hospitalization for MI and 1-year after MI were significantly associated with increased cardiac mortality (Figure 2).15 Additionally, Penninx et al16 reported that patients with major depression and cardiac disease had almost twice the risk of cardiac mortality of those with minor depression and cardiac disease.
Depression in patients with cardiac problems should be treated aggressively, but to avoid exacerbating the cardiac illness, antidepressants that might increase blood pressure or negatively affect the heart rate should be avoided. Thus, MAOIs, TCAs, and possibly atypical antipsychotics, which have a black box warning for increased mortality in elderly patients, as well as T3 augmentation should generally not be used in this population. SSRIs, particularly sertraline, which has been more intensively studied in this area, may be beneficial for depressed patients with cardiac complications.17 SNRIs might be helpful, but some agents may raise blood pressure at certain doses, particularly higher doses of venlafaxine.
Cerebrovascular Events
After having a stroke, approximately 40% of patients will develop depression at some point, which substantially worsens their daily functioning and increases their risk of mortality.18 In evaluating poststroke recovery, Parikh et al19 found similar levels of impairment during hospitalization for patients with or without depression. However, at the 2-year follow-up, patients with minor or major depression during hospitalization for stroke were significantly more impaired than those without depression, and patients with major depression remained more impaired even after achieving remission from depression.
For patients with depression who have experienced an embolic stroke, SSRIs may be the best antidepressant choice to treat the depression. For example, in a study20 of the improvement of cognitive disabilities with escitalopram, poststroke patients receiving the active agent demonstrated improved cognition, particularly in verbal and visual memory, compared with those receiving placebo or problem-solving therapy, an effect independent of the agent’s antidepressant effect. To avoid worsening cerebrovascular conditions, TCAs, SNRIs, and, particularly, MAOIs should probably be avoided in this population; augmentation with atypical antipsychotics is also not recommended. To determine the efficacy of specific antidepressants in treating poststroke depression, including possible preventive properties, more research is needed.
Safety Considerations and Drug Interactions in Administering Antidepressants
When complicating factors are not present in patients with depression, safety and tolerability profiles should guide clinicians’ treatment selection. However, depression is a complex disorder that often has several complicating factors such as various symptom presentations and co-occurring conditions. In these instances, antidepressants with less-than-desirable safety profiles may be necessary depending on individual patient illness presentations. For example, although TCAs may be useful in treating certain subpopulations with depression, a small overdose (less than a week’s worth) can be lethal. Newer antidepressants, such as SSRIs and SNRIs, and augmentation with atypical antipsychotics are generally safer in overdose than TCAs.
Clinicians should be aware that patients with depression and comorbid conditions that cause pain are often prescribed analgesics such as opioids to alleviate the pain. In the last 15 years, opioid prescription for medical use has increased 10-fold.21 Unfortunately, opioids are associated with a risk of unintentional overdose and suicide, and risk of unintentional death can occur when benzodiazepines are used in combination with opiates in depressed patients. As of 2007, unintentional drug poisoning deaths have outnumbered suicides and motor vehicle accident deaths in several states.22 For patients presenting with depression and pain, optimally clinicians should choose antidepressants that might decrease or prevent the need for adjuvant pain medications. For instance, duloxetine and venlafaxine,23 as well as some of the TCAs, may reduce pain while treating depression, thereby obviating or decreasing the need for opiate use in some patients.
Ideally, because medications have the potential for negative drug-drug interactions, clinicians should be aware of all prescription and over-the-counter medications and herbal remedies that their patients are taking before prescribing antidepressants. Unfortunately, some patients do not accurately report over-the-counter medications or medications they might be receiving from other doctors. To help clinicians assess patients’ real-time, scheduled prescription medication regimens, online systems called Prescription Drug Monitoring Programs are available in 34 states, and other states are currently implementing the systems.24 Pharmacy prescription records can also be very helpful.
Depression and Sexual Side Effects
Sexual side effects are common with most antidepressants and frequently contribute to treatment nonadherence. For example, therapy with SSRIs can reduce patients’ libidos and negatively impact sexual functioning in relationships.25 Obtrusive sexual adverse effects may reduce treatment adherence, particularly in younger patients who may be more sexually active than older patients with depression. When choosing a second-line treatment for patients who have experienced sexual side effects, options with lower risks of sexual interference include norepinephrine-dopamine reuptake inhibitors (NDRIs) and some atypical antipsychotics. For instance, the NDRI bupropion has a reduced sexual side effect profile compared with SSRIs,26 and quetiapine appears to have lower sexual side effects than risperidone.27 Additionally, buspirone has been found to partially reverse sexual side effects associated with previous SSRI therapy.28
Second-Line Treatment Efficacy: Results From the STAR*D Study
The Sequenced Treatment Alternatives to Relieve Depression (STAR*D) study2,29,30 evaluated several medications and cognitive therapy as second-line switching or augmentation options. In level 1 of the study, patients with MDD received citalopram (mean dose, 55 mg/d). Those who did not remit or who could not tolerate the drug proceeded to level 2, in which various switching, combination, or augmentation strategies were employed.
Switching
Patients randomly assigned to switch medications in level 2 of STAR*D2,29 received either sustained-release (SR) bupropion (mean dose, 282.7 mg/d), sertraline (mean dose, 135.5 mg/d), extended-release (XR) venlafaxine (mean dose, 193.6 mg/d), or cognitive therapy.
Approximately 25% of subjects achieved remission after switching to a different antidepressant; no significant differences regarding remission and response rates, tolerability, or adverse events were found among the medications.29 Compared with medication switch, cognitive therapy switch showed similar response and remission rates, although fewer adverse events were reported.2
Combination/Augmentation
Patients randomly assigned to receive antidepressant combination/augmentation in level 2 of STAR*D received either bupropion SR (mean dose, 267.5 mg/d), buspirone (mean dose, 40.9 mg/d), or cognitive therapy (mean, 11.4 sessions) in addition to citalopram.
Approximately 30% of subjects achieved remission with no significant differences between bupropion SR and buspirone in remission rates. However, the bupropion SR group had a greater reduction in Quick Inventory of Depressive Symptomatology (QIDS) symptoms (P < .04), lower mean total QIDS scores (P < .02), longer adherence to treatment, lower rates of discontinuation owing to intolerance, and a lower rate of treatment cessation than the buspirone group.30 Compared with medication augmentation, those receiving augmentation with cognitive therapy had similar rates of response or remission, although the time to remission was longer.2
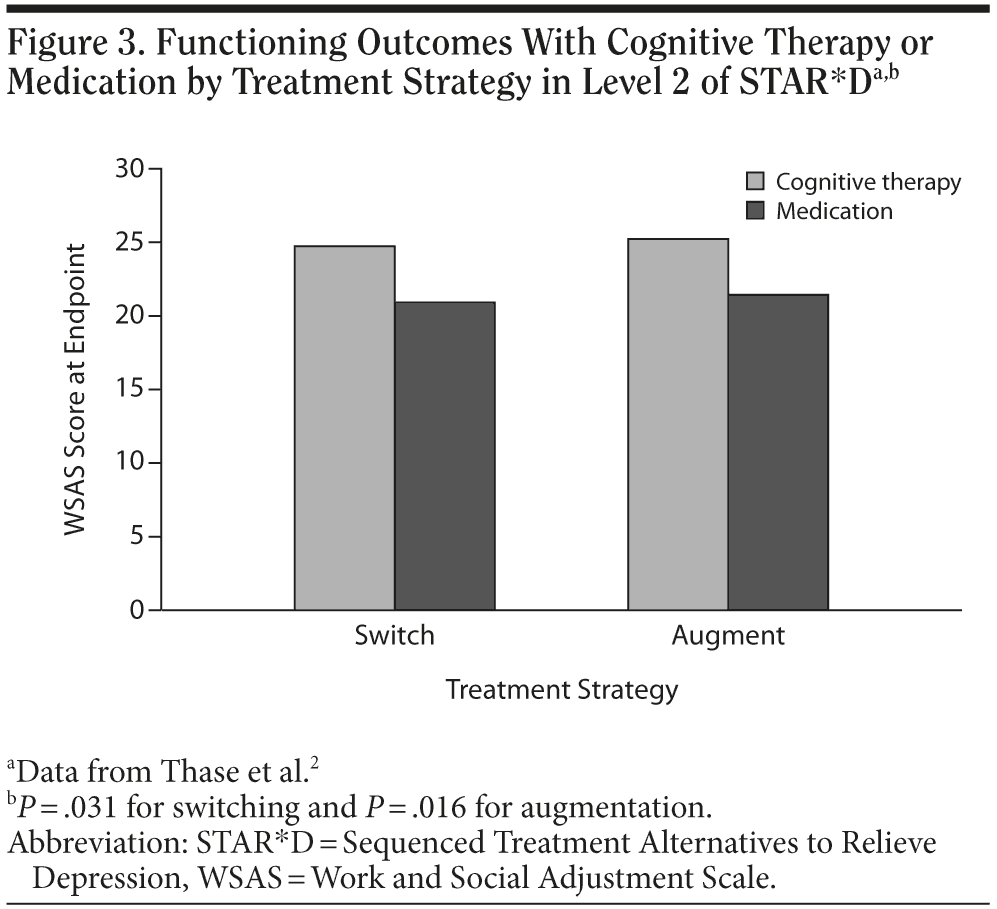
Cognitive therapy was as effective as both a switch and an augmentation strategy and was significantly more effective in reducing occupational and interpersonal impairment than medication (Figure 3).2 However, more research is needed to determine cognitive therapy’s efficacy over the long-term compared with pharmacotherapy. Additionally, because the sample sizes in the STAR*D study were small for the cognitive therapy groups (n = 65 for switch and n = 36 for augmentation), statistical power may have been limited.
When considering the results of STAR*D, clinicians should keep in mind that about 30% of subjects dropped out of the study after both levels 1 and 2 and approximately 40% of the remaining subjects dropped out after level 3. In STAR*D, like in clinical practice, the window of opportunity for selecting an effective antidepressant treatment strategy may only be open very briefly for many patients.
Conclusion
Before selecting and initiating a second-line therapy, clinicians should assess their patients’ treatment responses. For those patients who respond poorly to an initial antidepressant, clinicians should confirm a diagnosis of MDD, assess for possible comorbidities, ensure that patients are adherent to the current medication regimen, and optimize the dosage. If patients continue to receive an insufficient benefit from the initial antidepressant, then a second-line strategy is warranted.
When selecting second-line treatment for depression, clinicians should always consider individual patient symptom presentations. For instance, depressive symptom clusters can help guide treatment decisions, such as treating depression with insomnia versus hypersomnia or lethargy versus agitation. Cardiac and cerebrovascular events, adjuvant medications for pain, and potential drug interactions also play a role in treatment selection.
Switching and combination/augmentation strategies have demonstrated similar remission rates as second-line treatment interventions. Further, psychotherapy appears to be as effective as medication as either a switch or augmentation option and it can also help improve treatment adherence. Within-class or out-of-class differences are not apparent when initiating a second antidepressant. Patient preference and safety should be determining factors when choosing between switching or combination/augmentation.
Future research is needed to evaluate combinations and augmentations of antidepressants and to assess the efficacy and safety of initiating treatment with 2 medications to achieve a more rapid response.
Drug names: aripiprazole (Abilify), benztropine (Cogentin and others), bupropion (Aplenzin, Wellbutrin, and others), buspirone (BuSpar and others), citalopram (Celexa and others), clomipramine (Anafranil and others), desipramine (Norpramin and others), desvenlafaxine (Pristiq), divalproex (Depakote and others), doxepin (Silenor and others), duloxetine (Cymbalta), escitalopram (Lexapro and others), fluoxetine (Prozac and others), fluvoxamine (Luvox and others), imipramine (Tofranil and others), lamotrigine (Lamictal and others), lithium (Lithobid and others), milnacipran (Savella), mirtazapine (Remeron and others), nortriptyline (Pamelor, Aventyl, and others), olanzapine (Zyprexa), paroxetine (Paxil, Pexeva, and others), phenelzine (Nardil), protriptyline (Vivactil and others), quetiapine (Seroquel), risperidone (Risperdal and others), selegiline (EmSam and others), sertraline (Zoloft and others), thyroxine (Levoxyl, Levo-T, and others), tranylcypromine (Parnate and others), trazodone (Oleptro and others), trimipramine (Surmontil and others), venlafaxine (Effexor and others).
Disclosure of off-label usage: The author has determined that, to the best of his knowledge, aripiprazole and quetiapine XR are approved by the US Food and Drug Administration only as adjunctive treatment for depression, and benztropine, buspirone, clomipramine, divalproex, doxepin, fluvoxamine, lamotrigine, lithium, milnacipran, olanzapine, quetiapine, risperidone, thyroxine, l-methylfolate, mianserin, reboxetine, and triiodothyronine are not approved for the treatment of depression.
References
1. National Association of State Mental Health Program Directors. Morbidity and Mortality in People with Serious Mental Illness. Technical Reports. Alexandria, VA: National Association of State Mental Health Program Directors Medical Directors Council; 2006.
2. Thase ME, Friedman ES, Biggs MM, et al. Cognitive therapy versus medication in augmentation and switch strategies as second-step treatments: a STAR*D report. Am J Psychiatry. 2007;164(5):739-752. PubMed doi:10.1176/appi.ajp.164.5.739
3. McIntyre RS. When should you move beyond first-line therapy for depression? J Clin Psychiatry. 2010;71(suppl 1):16-20.
4. Hirschfeld RM, Lewis L, Vornik LA. Perceptions and impact of bipolar disorder: how far have we really come? results of the National Depressive and Manic-Depressive Association 2000 survey of individuals with bipolar disorder. J Clin Psychiatry. 2003;64(2):161-174. PubMed doi:10.4088/JCP.v64n0209
5. Akiskal HS, Walker P, Puzantian VR, et al. Bipolar outcome in the course of depressive illness: phenomenologic, familial, and pharmacologic predictors. J Affect Disord. 1983;5(2):115-128. PubMed doi:10.1016/0165-0327(83)90004-6
6. Lin EH, Von Korff M, Katon W, et al. The role of the primary care physician in patients’ adherence to antidepressant therapy. Med Care. 1995;33(1):67-74. PubMed doi:10.1097/00005650-199501000-00006
7. Suehs BT, Argo TR, Bendele SD, et al. Texas Medication Algorithm Project Procedural Manual: Major Depressive Disorder Algorithms. Austin, TX: Texas Department of State Health Services; 2008.
8. Fava M, Mischoulon D. Folate in depression: efficacy, safety, differences in formulations, and clinical issues. J Clin Psychiatry. 2009;70(suppl 5):12-17. PubMed doi:10.4088/JCP.8157su1c.03
9. American Psychiatric Association. Diagnostic and Statistical Manual of Mental Disorders, Fourth Edition, Text Revision. Washington, DC: American Psychiatric Association; 2000.
10. Deisenhammer EA, Ing CM, Strauss R, et al. The duration of the suicidal process: how much time is left for intervention between consideration and accomplishment of a suicide attempt? J Clin Psychiatry. 2009;70(1):19-24. PubMed doi:10.4088/JCP.07m03904
11. Guzzetta F, Tondo L, Centorrino F, et al. Lithium treatment reduces suicide risk in recurrent major depressive disorder. J Clin Psychiatry. 2007;68(3):380-383. PubMed doi:10.4088/JCP.v68n0304
12. Cole J, Toga AW, Hojatkashani C, et al. Subregional hippocampal deformations in major depressive disorder. J Affect Disord. 2010;126(1-2):272-277. PubMed doi:10.1016/j.jad.2010.03.004
13. Hippisley-Cox J, Fielding K, Pringle M. Depression as a risk factor for ischaemic heart disease in men: population based case-control study. BMJ. 1998;316(7146):1714-1719. PubMed
14. Lespérance F, Frasure-Smith N, Talajic M. Major depression before and after myocardial infarction: its nature and consequences. Psychosom Med. 1996;58(2):99-110. PubMed
15. Lespérance F, Frasure-Smith N, Talajic M, et al. Five-year risk of cardiac mortality in relation to initial severity and one-year changes in depression symptoms after myocardial infarction. Circulation. 2002;105(9):1049-1053. PubMed doi:10.1161/hc0902.104707
16. Penninx BW, Beekman AT, Honig AT, et al. Depression and cardiac mortality: results from a community-based longitudinal study. Arch Gen Psychiatry. 2001;58(3):221-227. PubMed doi:10.1001/archpsyc.58.3.221
17. Jiang W, O’ Connor C, Silva SG, et al. Safety and efficacy of sertraline for depression in patients with CHF (SADHART-CHF): a randomized, double-blind, placebo-controlled trial of sertraline for major depression with congestive heart failure. Am Heart J. 2008;156(3):437-444. doi:10.1016/j.ahj.2008.05.003 PubMed
18. Starkstein SE, Mizrahi R, Power BD. Antidepressant therapy in post-stroke depression. Expert Opin Pharmacother. 2008;9(8):1291-1298. PubMed doi:10.1517/14656566.9.8.1291
19. Parikh RM, Robinson RG, Lipsey JR, et al. The impact of poststroke depression on recovery in activities of daily living over a 2-year follow-up. Arch Neurol. 1990;47(7):785-789. PubMed
20. Jorge RE, Acion L, Moser D, et al. Escitalopram and enhancement of cognitive recovery following stroke. Arch Gen Psychiatry. 2010;67(2):187-196. PubMed doi:10.1001/archgenpsychiatry.2009.185
21. Centers for Disease Control and Prevention. Unintentional drug poisoning in the United States. http://www.cdc.gov/HomeandRecreationalSafety/Poisoning/brief.htm. Published March 18, 2010. Accessed September 14, 2010.
22. Paulozzi LJ, Weisler RH, Patkar AA. Unintentional drug poisoning deaths: a national epidemic. http://www.medscape.com/viewarticle/724186. Published June 28, 2010. Accessed September 14, 2010.
23. Mohr P, Bitter I, Svestka J, et al. Management of depression in the presence of pain symptoms. Psychiatr Danub. 2010;22(1):4-13. PubMed
24. Office of Diversion Control, Drug Enforcement Administration, US Dept of Justice. Questions and answers: state prescription drug monitoring programs. http://www.deadiversion.usdoj.gov/faq/rx_monitor.htm. Updated July 2010. Accessed July 31, 2010.
25. Rosen RC, Lane RM, Menza M. Effects of SSRIs on sexual function: a critical review. J Clin Psychopharmacol. 1999;19(1):67-85. PubMed doi:10.1097/00004714-199902000-00013
26. Demyttenaere K, Jaspers L. Review: Bupropion and SSRI-induced side effects. J Psychopharmacol. 2008;22(7):792-804. PubMed doi:10.1177/0269881107083798
27. Westheide J, Cvetanovska G, Albrecht C, et al. Prolactin, subjective well-being and sexual dysfunction: an open label observational study comparing quetiapine with risperidone. J Sex Med. 2008;5(12):2816-2826. PubMed doi:10.1111/j.1743-6109.2008.00859.x
28. Landén M, Eriksson E, Agren H, et al. Effect of buspirone on sexual dysfunction in depressed patients treated with selective serotonin reuptake inhibitors. J Clin Psychopharmacol. 1999;19(3):268-271. PubMed doi:10.1097/00004714-199906000-00012
29. Rush AJ, Trivedi MH, Wisniewski SR, et al, for the STAR*D Study Team. Bupropion-SR, sertraline, or venlafaxine-XR after failure of SSRIs for depression. N Engl J Med. 2006;354(12):1231-1242. PubMed doi:10.1056/NEJMoa052963
30. Trivedi MH, Fava M, Wisniewski SR, et al, for the STAR*D Study Team. Medication augmentation after the failure of SSRIs for depression. N Engl J Med. 2006;354(12):1243-1252. PubMed doi:10.1056/NEJMoa052964