Continuity of Depressive Disorders From Childhood and Adolescence to Adulthood: A Naturalistic Study in Community Mental Health Centers
Objective: To determine and compare rates of homotypic continuity of childhood- and adolescent-onset depression into adulthood.
Method: This was a naturalistic, prospective cohort study of children and adolescents receiving psychiatric care at all community mental health centers in Madrid, Spain, from January 1986 to December 2007. Data were obtained from a regional registry wherein all psychiatric visits to public mental health centers are recorded. Patients received their first diagnosis of an ICD-10 F32 or F33 depressive disorder between 6 and 17 years of age and were at least 20 years old at the time of their last visit. Subjects whose first diagnosis was in childhood (aged 6-12 years: depressed-child group) and subjects whose first diagnosis was in adolescence (aged 13-17 years: depressed-adolescent group) were compared in terms of demographic characteristics, psychiatric comorbidity, and rates of homotypic continuity in adulthood.
Results: Five hundred twenty-eight patients with depressive disorders met inclusion criteria. The depressed-adolescent group had a higher proportion of girls (60.3%) compared to the depressed-child group, but did not differ on other demographic or clinical variables. Most subjects who later received treatment in adult mental health facilities (n = 243; 57.2%; 95% CI, 50.9-57.2) continued to be diagnosed with a depressive disorder. High rates of anxiety disorders, bipolar disorder, personality disorders, and psychotic disorders in adulthood were observed among subjects from both groups. The absence of psychiatric comorbidity prior to age 18 years was associated with homotypic continuity of depressive disorder into adulthood.
Conclusions: Subjects with adolescent-onset depression and subjects without comorbid psychiatric disorders in youth appear to have a higher level of homotypic continuity into adulthood. Both children and adolescents with depressive disorders are at risk for other psychiatric disorders in adulthood.
Prim Care Companion CNS Disord 2011;13(5): doi:10.4088/PCC.11m01150
© Copyright 2011 Physicians Postgraduate Press, Inc.
Submitted: January 25, 2011; accepted February 23, 2011.
Published online: September 8, 2011 (doi:10.4088/PCC.11m01150).
Corresponding author: Enrique Baca-Garc×a, MD, PhD, Department of Psychiatry, Fundacion Jimenez Diaz University Hospital, Autonomous University of Madrid, Avenida Reyes Catolicos 2, 28040 Madrid, Spain ([email protected]).
The US National Institute of Mental Health’s new strategic plan stresses the importance of obtaining longitudinal data regarding the course of the psychiatric disorders that we treat.1 However, few clinical studies have focused on the continuity of psychiatric disorders from childhood or adolescence to adulthood.2 These investigations are of great importance, given that the study of the long-term course of psychiatric disorders among children and adolescents may be crucial for predicting adult psychopathology and for planning early intervention and prevention.3
Epidemiologic and clinical investigations indicate that onset of depressive disorders usually occurs during adolescence or early adulthood. Although less frequent, onset during childhood has also been documented.4-10 The clinical presentation of adolescent-onset depression shares a variety of features with that of adult onset. Both are more common in females; are frequently associated with anxiety disorders, substance use disorders, and/or suicidal behavior; and result in impairment in social and academic or occupational functioning.4,11-14 On the other hand, depressive disorders with onset during childhood are habitually characterized by marked irritability, appear to be more prevalent among males, and are associated with disruptive behavior disorders.11,15-17
Clinical Points
- Onset of depressive disorders usually occurs during adolescence or early adulthood.
- Adolescents with depressive disorders evaluated in community mental health centers show a high level of homotypic continuity in adulthood.
- Clinicians should be aware of the importance of early recognition and treatment of these disorders with enduring manifestations.
These differences in clinical presentations across developmental stages raise the question of whether childhood-onset depressive disorder is a different illness than adolescent-onset or adult-onset depressive disorders. Further, because most studies of childhood depression have not shown continuity with depression in adulthood,18-20 the question of whether depressive disorders in childhood are more likely to be associated with a nonspecific increased risk for other psychiatric diagnoses in adulthood, such as bipolar disorder, anxiety disorders, or substance abuse, compared to depressive disorders in adolescence remains unanswered. This would imply significant heterotypic continuity of depressive disorders with onset in childhood. In contrast, epidemiologic studies of depressive disorders with onset in adolescence have reported a more specific course and a higher level of continuity in adulthood.14
Some authors have postulated that psychiatric comorbidity in youth may exert a significant influence on the observed homotypic continuity of depressive disorder in adulthood.16-18 However, not all studies agree in this regard.16
The objective of our investigation was to determine the frequency of homotypic and heterotypic continuity of depressive disorders in patients followed in clinical services since childhood or adolescence. On the basis of previous studies, we hypothesized that children with depressive disorders would be less likely to show homotypic continuity in adulthood than adolescents with depressive disorders. We also hypothesized that children with depressive disorders would show a higher prevalence of other psychiatric disorders (such as bipolar disorder, anxiety disorders, and substance abuse disorders) in adulthood than adolescents with depressive disorders. On the basis of previous reports that have considered variables affecting the persistence and recurrence of depressive disorders over time, we intended to explore the association of sex and psychiatric comorbidity with the following aspects: (1) duration of follow-up and (2) the recurrence of depressive disorders in adulthood.
METHOD
The Madrid Psychiatric Cumulative Register Study is a naturalistic study of diagnostic stability and consistency over time.21 From January 1986 to December 2007, public mental health centers in the province of Madrid, Spain, have recorded all psychiatric visits in a regional registry (Registro Acumulativo de Casos de la Comunidad de Madrid). Individual service users are reliably identified in the database used for our analyses because each patient is given a unique identifying number (a numeric code is used to ensure patient anonymity), which remains the same throughout all contacts with psychiatric services within the study area.21
Setting
Services were provided at psychiatric outpatient centers that are part of the Spanish National Health Services, which are financed by taxes and provide coverage free of charge for all Spanish citizens and legal immigrants.
Diagnostic Procedure
We extracted regional registry data regarding all psychiatric visits to community mental health centers in Madrid, Spain. Mental disorders were recorded according to the International Classification of Diseases, Tenth Revision (ICD-10) by experienced psychiatrists and psychologists. Treating clinicians had standard clinical training in diagnostic assessment and were hired by the National Mental Health System to specifically treat the children and adolescent population. Clinical data regarding diagnosis were registered at every follow-up visit. Psychiatrists/psychologists recorded a maximum of 2 diagnoses per patient per visit for administrative purposes.
Participants
The target population was 49,529 children and adolescents who were identified from the cumulative clinical records database within the region of Madrid since 1986 and who were at least 20 years old at the time of the current study.
From this sample, we selected patients who met the following inclusion criteria:
1. Patient’s diagnosis had to be classified under the ICD-10 system.
2. Subjects were aged 6-17 years old at first diagnosis of depressive disorder in mental health services.
3. Depressive disorder diagnoses had to be one of the following ICD-10 categories: depressive episodes (F32.0, F32.1, F32.2, F32.3, F32.8, and F32.9) or recurrent depressive disorders (F33.0, F33.1, F33.2, F33.3, F33.4, F33.8, and F33.9).
Data Management
We divided the sample into 2 groups according to the US National Library of Medicine and the National Institutes of Health classification of ages: subjects whose first diagnosis of depressive disorder was received in childhood (aged 6-12 years: depressed-child group) and subjects whose first diagnosis of depressive disorder was received in adolescence (aged 13-17 years: depressed-adolescent group). Between these 2 groups, homotypy was defined as the retention of a depressive disorder diagnosis in adulthood as evidenced by the regional registry records at least at 1 visit.
Data Analysis
We used χ2 analyses to compare demographic variables of the depressed-child and depressed-adolescent groups (sex, maternal and paternal education attainment, maternal and parental employment status).
To test our first hypothesis, rates of homotypic continuity of depressive disorders in adulthood in the 2 groups were compared by using χ2 analysis. To test our second hypothesis, we compared rates of other psychiatric disorders in adulthood among the 2 groups using χ2 analyses for each ICD-10 psychiatric diagnosis studied. For our exploratory hypotheses, the association of sex and psychiatric comorbidity with the length of follow-up in adult mental health services and with the continuity of depressive disorders in adulthood was examined using Cox regression analyses. Cox regression analyses were conducted in order to adjust for differences in the length of time subjects spent in follow-up.
We conducted 2 types of Cox regression analysis. In the first analysis, the outcome variable was the presence (versus absence) of follow-up in adult mental health services among subjects with depressive disorders with onset in childhood or adolescence. We included as independent variables the list of variables that differentiated depressive subjects with follow-up in adult mental health services from those without follow-up in adult mental health services, as determined by χ2 analyses. Similarly, a second Cox regression analysis was conducted to classify subjects with homotypic continuity of depressive disorders in adulthood. This model was adjusted using the list of variables that differentiated depressive subjects who continued to be diagnosed with depressive disorders in adulthood from those who did not receive a diagnosis of depressive disorder in adulthood as determined by χ2 analyses. SPSS statistical software, edition 14.0 for Windows (IBM Corporation, Somers, New York) was used.
RESULTS
Demographic Characteristics
Of the 49,529 children and adolescents in the registry, 528 met inclusion criteria. Of the 528 subjects, 85 (16%) had received a depressive disorder diagnosis in childhood (depressed-child group), while 443 (84%) were adolescents at the time of first diagnosis of depressive disorder (depressed-adolescent group). Significantly more males (62.4%) than females (37.6%) were initially diagnosed with a depressive disorder during childhood; however, significantly more females (60.3%) than males (39.7%) were diagnosed with a depressive disorder during adolescence.
Depressed-child and depressed-adolescent groups did not differ in other demographic variables studied. Nearly half of the parents had finished basic studies (equivalent to eighth grade in the United States). The level of illiteracy in parents was low (< 2%), which is similar to the low level of illiteracy in Madrid in all age groups. The rate of unemployment was 16.3% in fathers and 25% in mothers.
Homotypic Continuity of Depressive Disorders in Adulthood
Of the 528 subjects included in our study, only 243 (46%) subjects were followed in adulthood at mental health centers in Madrid. Approximately 28.2% of subjects in the depressed-child group were followed up at adult mental health centers, whereas 49.4% of subjects in the depressed-adolescent group were followed up at those mental health centers.
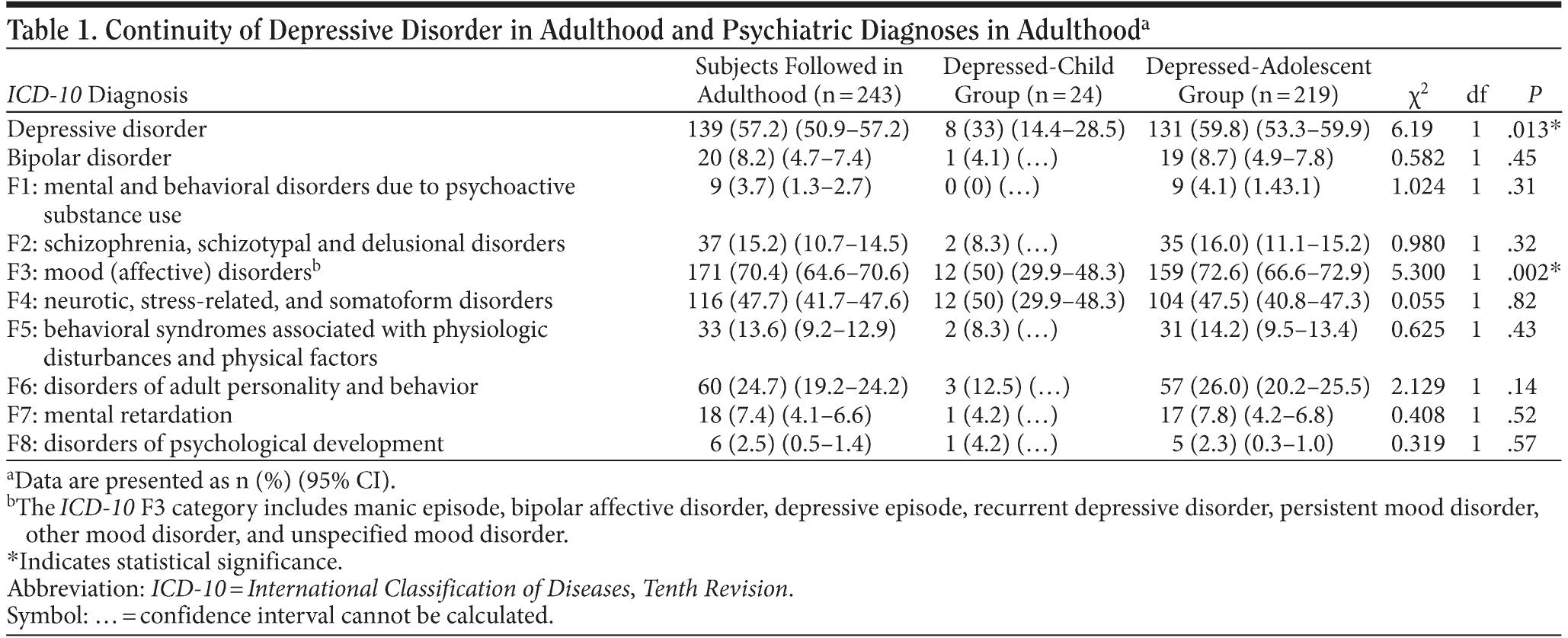
Up to 57.2% (95% CI, 50.9-57.2) of patients who continued their follow-up in adult mental health services were diagnosed with a depressive disorder in adulthood. As hypothesized, we found that fewer subjects in the depressed-child group showed homotypic continuity in adulthood compared to subjects in the depressed-adolescent group (33% [95% CI, 14.4-28.5] versus 59.8% [95% CI, 53.3-59.9]; χ21 = 6.19; P = .013) (Table 1).
Psychiatric Diagnoses in Adulthood
Contrary to our second hypothesis, subjects in the depressed-child group did not show a higher prevalence of other psychiatric disorders than subjects in the depressed-adolescent group. Specifically, no significant differences between the depressed-adolescent and depressed-child groups were found regarding the proportions of subjects with bipolar disorder, anxiety disorders, or substance abuse disorders in adulthood (see Table 1).
Influence of Sex and Psychiatric Comorbidity on Length of Follow-Up in Adult Mental Health Services
No demographic differences between subjects who continued to be followed up in adulthood and subjects who were not were found regarding parental education attainment and parental employment status (data available upon request). Only age at first diagnosis of depressive disorder was different between those who did and those who did not continue follow-up in adult mental health services (χ21 = 1.30, P < .001). More subjects in the depressed-adolescent group continued follow-up in adult mental health services compared to subjects in the depressed-child group.
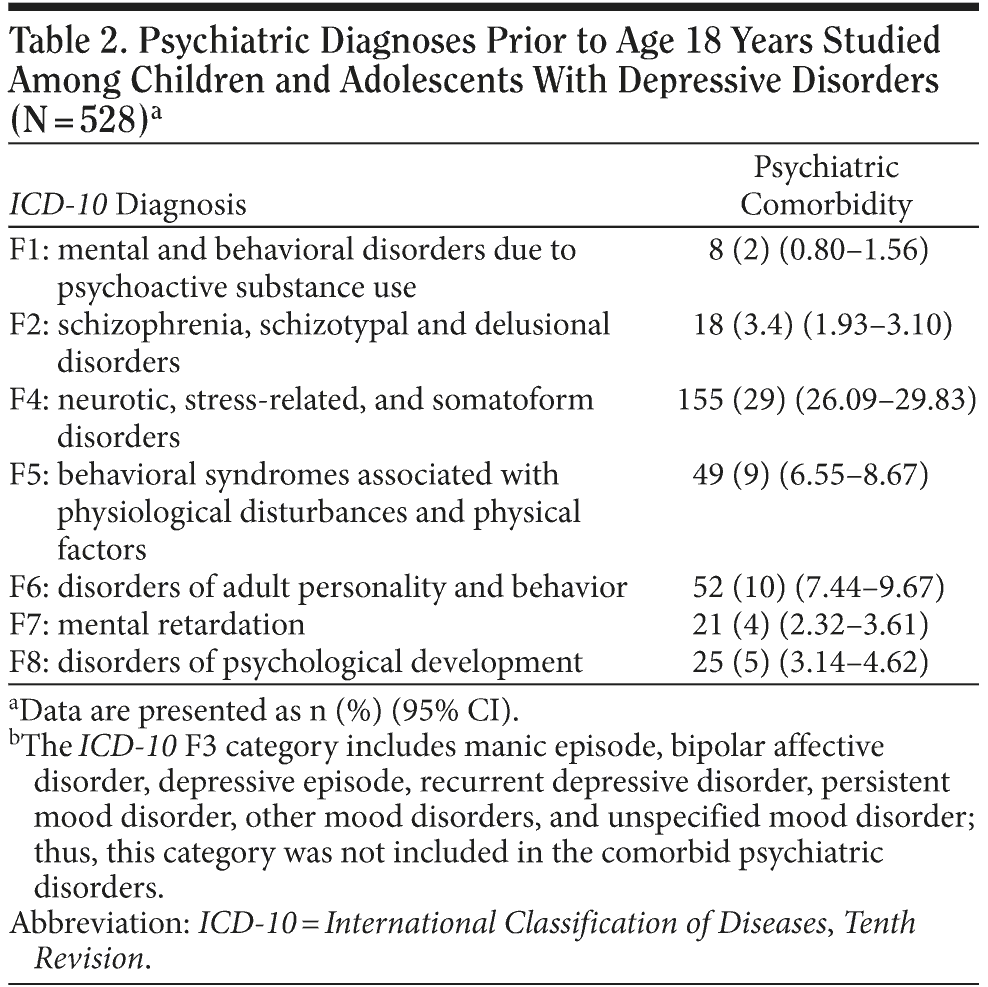
Psychiatric comorbidity prior to age 18 years was very frequent. Of the 528 subjects diagnosed with a depressive disorder in childhood or adolescence, 249 subjects were diagnosed with at least another comorbid psychiatric disorder prior to age 18 years. The most common comorbid psychiatric disorders were diagnoses of the ICD-10 F4 category (neurotic, stress-related, and somatoform disorders) (Table 2). The ICD-10 F3 category includes manic episode, bipolar affective disorder, depressive episode, recurrent depressive disorder, persistent mood disorder, other mood disorders, and unspecified mood disorder; thus, this category was not included in the comorbid psychiatric disorders.
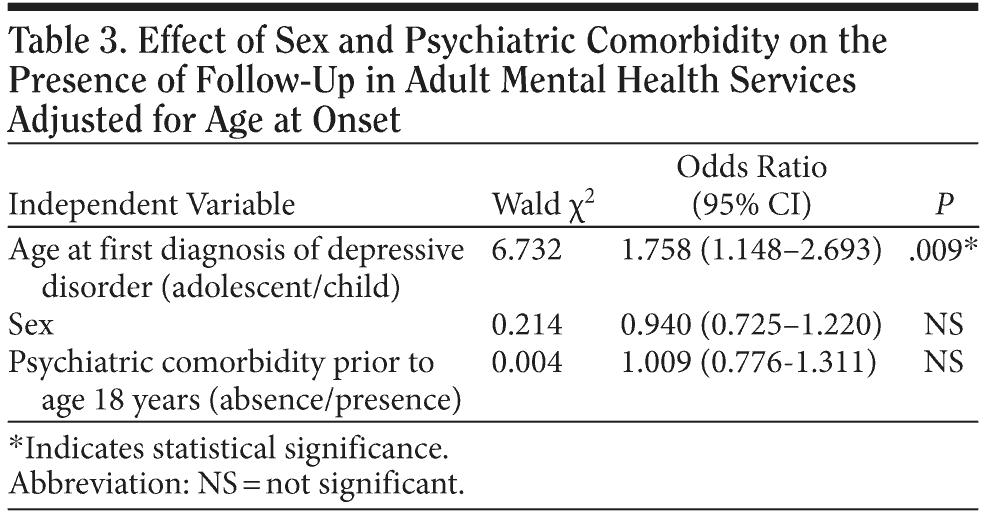
Cox regression analysis showed that subjects in the depressed-adolescent group were more likely to be followed up in adult mental health services. Sex and psychiatric comorbidity prior to age 18 years did not predict follow-up in adult mental health services when the duration of follow-up was accounted for (Table 3).
Influence of Sex and Psychiatric Comorbidity Prior to Age 18 Years on Homotypic Continuity of Depression
Cox regression analysis showed that the absence of psychiatric comorbidity prior to age 18 years was related to a higher likelihood of homotypic continuity of depressive disorder in adulthood (Table 4).
DISCUSSION
Our data suggest that adolescents with depressive disorders evaluated in community mental health centers show a higher level of homotypic continuity in adulthood. In contrast, homotypy is less common among those whose first diagnosis of depressive disorder occurs during childhood. These findings are in agreement with previous work in epidemiologic and clinical samples14,16,22-28 and underscore the importance of early recognition and treatment of these disorders with enduring manifestations.
It could be argued that those with an earlier onset of the depressive disorder would have a higher genetic and biological liability for the development of the depressive disorder and, as a result, would be more susceptible to suffer from additional and similar episodes through development. Accordingly, homotypic continuity should be expected. This genetic liability has been reported especially in adolescent-onset depression, whereas childhood-onset depression has been linked more frequently to environmental factors, such as adverse early experiences.17 It may also be that subjects who suffer from childhood depressive disorders might be affected in such a way that normal development is derailed, facilitating the occurrence of other psychopathology. Another possibility is that childhood-onset depression has a protean evolution and can be a harbinger of a host of psychiatric conditions.
Contrary to our hypothesis, we did not find higher rates of comorbid psychiatric disorders in adulthood among subjects whose first diagnosis of depressive disorder occurred in childhood compared to subjects whose first diagnosis occurred in adolescence. The rate of bipolar disorder did not differ between groups and was about 8%. Although this rate is significantly higher than the rate reported in a normal population,29 the rate found in our study was lower than figures reported in previous studies (20%-30%).30,31 Given that the mean age of the study participants was roughly 25 years old, some patients were not at the age of risk yet and, therefore, had not had time to develop full-blown bipolar disorder. This fact might partially explain our low figures.
Notably, the presence of neurotic, stress-related, and somatoform disorder diagnoses was high in adulthood for both groups, with almost half of the sample suffering from these disorders in adulthood. This finding is in accordance with the notion that anxiety and depressive disorders share a common vulnerability and with previous reports that indicate that one disorder in youth predicts the other.19 In this line, Costello et al19 carried out a longitudinal epidemiologic study among children and adolescents and reported a significant heterotypic evolution from depression to anxiety on the one hand, and from anxiety to depression on the other. Nevertheless, anxiety and depressive disorders have been described as distinct psychiatric categories that are often comorbid.18-20,32
Personality disorders were also common in subjects with depressive disorder with onset in childhood or adolescence. Nearly one-quarter of the sample developed a personality disorder in adulthood, a finding that supports results from previous epidemiologic samples.33-35 It has been proposed that early-onset depressive disorders not only severely affect mood and self-view, but also interfere with social interactions and acquisition of adequate social competence, which affects interpersonal relationships and may facilitate the later development of personality disorders.33-35 It is intriguing that roughly 10% of children and adolescents with depressive disorders in our sample received an ICD-10 F6 diagnosis (disorder of adult personality and behavior) prior to 18 years of age. Although it is commonly recognized that adult personality disorders have their roots in a variety of developmental and temperamental factors, there is limited knowledge regarding childhood and adolescent antecedents of adult personality disorders.33
We failed to demonstrate a high prevalence of substance use disorders in adulthood among subjects with depressive disorders with onset in youth. In our clinical sample, only 4% of the subjects went on to develop such disorders. Given that in Spain, subjects with substance use problems are treated in specialized substance use programs, it could be that a proportion of patients were being followed up in those services and were not receiving treatment at adult mental health centers.
Of interest, we found a high prevalence of ICD F2 diagnoses (schizophrenia, schizotypal and delusional disorder) in adulthood among subjects with depressive disorder with onset in childhood or adolescence. This finding is in line with previous reports that have shown that the earliest manifestations of schizophrenia are depressive and negative symptoms, and that a prodromal phase with a mean duration of 5 years precedes the first psychotic episode in schizophrenia in the vast majority of the cases.36 However, mania in adolescents is frequently associated with psychotic symptoms, and since the early course of bipolar disorder in adolescents seems to be more chronic and refractory to treatment than adult onset, these aspects may affect the diagnostic process. It could be that affective psychotic symptoms may have been misdiagnosed, inflating the rate of ICD-10 F2 diagnoses.
Some authors have shown that psychiatric comorbidity may facilitate the homotypic continuity of depressive disorders throughout development and into young adulthood.18 Nonetheless, others have not found any effects of comorbidity on the continuity of depressive disorder over time.16 We found that the absence of psychiatric comorbidity prior to age 18 years was related to a higher likelihood of homotypic continuity of depressive disorder in adulthood.
As has been shown by other groups,37-39 prevalence of depressive disorders was higher in adolescent females than in their male counterparts. However, we did not find sex differences either in the rate of follow-up in adult mental health services or in the rate of homotypic continuity of depressive disorder in adulthood. This finding suggests that although adolescent females might be more vulnerable for the development of the depressive disorder than males, this vulnerability is not linked to differences in the duration of follow-up or in the homotypic course of the disorder in adulthood.
Strengths and Limitations
This is the largest naturalistic study evaluating the homotypic continuity of depressive disorders in children and adolescents treated in community mental health services. Up to 57.2% (95% CI, 50.9-57.2) of patients who continued their follow-up in adult mental health services were diagnosed with a depressive disorder in adulthood. These figures are similar to those presented in previous studies despite differences in ascertainment, number of assessments, diagnostic criteria, or demographic variables. Nevertheless, our results must be interpreted with caution and in the context of several limitations discussed below.
ICD-10 diagnoses were established clinically. Therefore, accuracy might have been affected due to lack of the use of standardized assessments. Treating psychiatrists/psychologists often were able to review past records and diagnoses. No specific training to maintain interrater reliability was offered for clinicians who assigned the diagnoses.
It is also possible that the most severely depressed patients, for instance those with greater comorbidity, followed alternative pathways of treatment. This might be a confounding factor affecting rates of homotypic continuity. Rates of annual residential changes to other provinces in Spain or other countries among young people are estimated at less than 2% (National Statistics Institute; http://www.ine.es). In addition, given that most Spaniards receive medical and mental heath care in public services, it is unlikely that many patients sought treatment in other settings. On the other hand, we intentionally selected subjects with a clinical diagnosis of depressive disorder; thus, our results may not be generalizable to subclinical-disordered subjects. This limitation may have clinical implications, since previous epidemiologic investigations have pointed out that subsyndromal manifestations may be early indicators of long-term risk. We also lacked data on the efficacy of the treatment interventions carried out.
Another caveat is that we used chronological criteria to separate children from adolescents. Other authors have used pubertal status to differentiate groups.14 Also, the regional registry does not provide data regarding the precise onset of the psychiatric disorders, although it does allow for collection of data regarding the exact dates when a diagnosis is first given at outpatient mental health services. Another limitation is that almost half of patients diagnosed with depressive disorders in childhood or adolescence were not followed in adult mental health services.
Finally, psychiatrists/psychologists recorded a maximum of 2 diagnoses per patient per visit for administrative purposes. The fact that we did not find higher rates of comorbid psychiatric disorders in adulthood among subjects whose first diagnosis of depressive disorder occurred in childhood might be related to this limitation.
Despite all these limitations, the high level of homotypic continuity of depressive disorder in adulthood, especially among those with an adolescent onset, is of clinical interest. This information could be useful to develop secondary prevention interventions for children and adolescents suffering from depressive disorders treated in community mental health centers.
Author affiliations: Department of Psychiatry at Fundación Jimenez Diaz, Hospital and Autonoma University of Madrid, Madrid, Spain (Drs Carballo, Îœu×±oz-Lorenzo, Blasco-Fontecilla, Lopez-Castroman, Garc×a-Nieto, and Baca-Garc×a); Department of Psychiatry and Behavioral Science, Faculty of Medicine and Health Sciences, United Arab Emirates University, United Arab Emirates, and Department of Child and Adolescent Neuropsychiatry, University Hospital, Medical University of Vienna, Vienna, Austria (Dr Dervic); Department of Psychiatry, New York State Psychiatric Institute, Columbia University, New York (Drs Oquendo and Baca-Garc×a), and Centro de Investigación Biomédica en Red de Salud Mental, Madrid, Spain (Drs Blasco-Fontecilla, Lopez-Castroman, and Baca-Garc×a).
Potential conflicts of interest: Dr Carballo has received grant/research support from the Alicia Koplowitz Foundation. Drs Blasco-Fontecilla and Lopez-Castroman have received grant/research support from the Fundacion Espa×±ola de Psiquiatria y Salud Mental and Instituto de Salud Carlos III (RIO HORTEGA research funding). Dr Garc×a-Nieto has received grant/research support from the Alicia Koplowitz Foundation. Dr Oquendo has received grant/research support from American Foundation for Suicide Prevention, AstraZeneca, Bristol-Myers Squibb, Eli Lilly, Janssen, Moody’s Foundation, National Institute of Mental Health, National Institute on Alcohol Abuse and Alcoholism, and Pfizer and is a stock shareholder in Bristol-Myers Squibb. Drs Îœu×±oz-Lorenzo, Dervic, and Baca-Garc×a report no conflicts of interest related to the subject of this article.
Funding/support: None reported.
Previous presentation: Presented at the 163rd Annual Meeting of the American Psychiatric Association; May 22-26, 2010; New Orleans, Louisiana.
REFERENCES
1. US Department of Health & Human Services National Institutes of Health NIH NIMH Strategic Plan 2009. Publication No. 08-6368, revised 2008. http://www.nimh.nih.gov/about/strategic-planning-reports/index.shtml. Accessed April 5, 2011.
2. Kim-Cohen J, Caspi A, Moffitt TE, et al. Prior juvenile diagnoses in adults with mental disorder: developmental follow-back of a prospective-longitudinal cohort. Arch Gen Psychiatry. 2003;60(7):709-717. PubMed doi:10.1001/archpsyc.60.7.709
3. Reef J, Diamantopoulou S, van Meurs I, et al. Child to adult continuities of psychopathology: a 24-year follow-up. Acta Psychiatr Scand. 2009;120(3):230-238. PubMed doi:10.1111/j.1600-0447.2009.01422.x
4. Birmaher B, Ryan ND, Williamson DE, et al. Childhood and adolescent depression: a review of the past 10 years, part II. J Am Acad Child Adolesc Psychiatry. 1996;35(12):1575-1583. PubMed doi:10.1097/00004583-199612000-00008
5. Nobile M, Cataldo GM, Marino C, et al. Diagnosis and treatment of dysthymia in children and adolescents. CNS Drugs. 2003;17(13):927-946. PubMed doi:10.2165/00023210-200317130-00001
6. Ryan ND. Diagnosing pediatric depression. Biol Psychiatry. 2001;49(12):1050-1054. PubMed doi:10.1016/S0006-3223(01)01143-X
7. McCauley E, Myers K, Mitchell J, et al. Depression in young people: initial presentation and clinical course. J Am Acad Child Adolesc Psychiatry. 1993;32(4):714-722. PubMed doi:10.1097/00004583-199307000-00003
8. Barkow K, Heun R, Wittchen HU, et al. Mixed anxiety-depression in a 1 year follow-up study: shift to other diagnoses or remission? J Affect Disord. 2004;79(1-3):235-239. PubMed doi:10.1016/S0165-0327(02)00343-9
9. Culverhouse R, Bucholz KK, Crowe RR, et al. Long-term stability of alcohol and other substance dependence diagnoses and habitual smoking: an evaluation after 5 years. Arch Gen Psychiatry. 2005;62(7):753-760. PubMed doi:10.1001/archpsyc.62.7.753
10. Mattanah JJ, Becker DF, Levy KN, et al. Diagnostic stability in adolescents followed up 2 years after hospitalization. Am J Psychiatry. 1995;152(6):889-894. PubMed
11. Birmaher B, Williamson DE, Dahl RE, et al. Clinical presentation and course of depression in youth: does onset in childhood differ from onset in adolescence? J Am Acad Child Adolesc Psychiatry. 2004;43(1):63-70. PubMed doi:10.1097/00004583-200401000-00015
12. Kovacs M. Presentation and course of major depressive disorder during childhood and later years of the life span. J Am Acad Child Adolesc Psychiatry. 1996;35(6):705-715. PubMed doi:10.1097/00004583-199606000-00010
13. Kovacs M. Gender and the course of major depressive disorder through adolescence in clinically referred youngsters. J Am Acad Child Adolesc Psychiatry. 2001;40(9):1079-1085. PubMed doi:10.1097/00004583-200109000-00017
14. Weissman MM, Wolk S, Goldstein RB, et al. Depressed adolescents grown up. JAMA. 1999;281(18):1707-1713. PubMed doi:10.1001/jama.281.18.1707
15. Birmaher B, Arbelaez C, Brent D. Course and outcome of child and adolescent major depressive disorder. Child Adolesc Psychiatr Clin N Am. 2002;11(3):619-637. PubMed doi:10.1016/S1056-4993(02)00011-1
16. Fombonne E, Wostear G, Cooper V, et al. The Maudsley long-term follow-up of child and adolescent depression, 1: psychiatric outcomes in adulthood. Br J Psychiatry. 2001;179(3):210-217. PubMed doi:10.1192/bjp.179.3.210
17. Rutter M, Kim-Cohen J, Maughan B. Continuities and discontinuities in psychopathology between childhood and adult life. J Child Psychol Psychiatry. 2006;47(3-4):276-295. PubMed doi:10.1111/j.1469-7610.2006.01614.x
18. Copeland WE, Shanahan L, Costello EJ, et al. Childhood and adolescent psychiatric disorders as predictors of young adult disorders. Arch Gen Psychiatry. 2009;66(7):764-772. PubMed doi:10.1001/archgenpsychiatry.2009.85
19. Costello EJ, Mustillo S, Erkanli A, et al. Prevalence and development of psychiatric disorders in childhood and adolescence. Arch Gen Psychiatry. 2003;60(8):837-844. PubMed doi:10.1001/archpsyc.60.8.837
20. Pine DS, Cohen P, Gurley D, et al. The risk for early-adulthood anxiety and depressive disorders in adolescents with anxiety and depressive disorders. Arch Gen Psychiatry. 1998;55(1):56-64. PubMed doi:10.1001/archpsyc.55.1.56
21. Baca-Garc×a E, Perez-Rodriguez MM, Basurte-Villamor I, et al. Diagnostic stability of psychiatric disorders in clinical practice. Br J Psychiatry. 2007;190(3):210-216. PubMed doi:10.1192/bjp.bp.106.024026
22. Canals J, Domרnech-Llaberia E, Fernסndez-Ballart J, et al. Predictors of depression at eighteen: a 7-year follow-up study in a Spanish nonclinical population. Eur Child Adolesc Psychiatry. 2002;11(5):226-233. PubMed doi:10.1007/s00787-002-0286-y
23. Fergusson DM, Horwood LJ, Lynskey MT. Prevalence and comorbidity of DSM-III-R diagnoses in a birth cohort of 15 year olds. J Am Acad Child Adolesc Psychiatry. 1993;32(6):1127-1134. PubMed doi:10.1097/00004583-199311000-00004
24. Harrington R, Fudge H, Rutter M, et al. Adult outcomes of childhood and adolescent depression, I: psychiatric status. Arch Gen Psychiatry. 1990;47(5):465-473. PubMed
25. Kovacs M, Feinberg TL, Crouse-Novak M, et al. Depressive disorders in childhood, II: a longitudinal study of the risk for a subsequent major depression. Arch Gen Psychiatry. 1984;41(7):643-649. PubMed
26. Rao U, Ryan ND, Birmaher B, et al. Unipolar depression in adolescents: clinical outcome in adulthood. J Am Acad Child Adolesc Psychiatry. 1995;34(5):566-578. PubMed doi:10.1097/00004583-199505000-00009
27. Reinke WM, Ostrander R. Heterotyic and homotypic continuity: the moderating effects of age and gender. J Abnorm Child Psychol. 2008;36(7):1109-1121. PubMed doi:10.1007/s10802-008-9236-6
28. Weissman MM, Wolk S, Wickramaratne P, et al. Children with prepubertal-onset major depressive disorder and anxiety grown up. Arch Gen Psychiatry. 1999;56(9):794-801. PubMed doi:10.1001/archpsyc.56.9.794
29. Merikangas KR, Akiskal HS, Angst J, et al. Lifetime and 12-month prevalence of bipolar spectrum disorder in the National Comorbidity Survey replication. Arch Gen Psychiatry. 2007;64(5):543-552. PubMed doi:10.1001/archpsyc.64.5.543
30. Strober M, Carlson G. Bipolar illness in adolescents with major depression: clinical, genetic, and psychopharmacologic predictors in a three- to four-year prospective follow-up investigation. Arch Gen Psychiatry. 1982;39(5):549-555. PubMed
31. Geller B, Fox LW, Clark KA. Rate and predictors of prepubertal bipolarity during follow-up of 6- to 12-year-old depressed children. J Am Acad Child Adolesc Psychiatry. 1994;33(4):461-468. PubMed doi:10.1097/00004583-199405000-00003
32. Clark LA, Watson D. Tripartite model of anxiety and depression: psychometric evidence and taxonomic implications. J Abnorm Psychol. 1991;100(3):316-336. PubMed doi:10.1037/0021-843X.100.3.316
33. Cohen P, Cohen J, Brook J. An epidemiological study of disorders in late childhood and adolescence, II: persistence of disorders. J Child Psychol Psychiatry. 1993;34(6):869-877. PubMed doi:10.1111/j.1469-7610.1993.tb01095.x
34. Kasen S, Cohen P, Skodol AE, et al. Influence of child and adolescent psychiatric disorders on young adult personality disorder. Am J Psychiatry. 1999;156(10):1529-1535. PubMed
35. Kasen S, Cohen P, Skodol AE, et al. Childhood depression and adult personality disorder: alternative pathways of continuity. Arch Gen Psychiatry. 2001;58(3):231-236. PubMed doi:10.1001/archpsyc.58.3.231
36. an der Heiden W, Häfner H. The epidemiology of onset and course of schizophrenia. Eur Arch Psychiatry Clin Neurosci. 2000;250(6):292-303. PubMed doi:10.1007/s004060070004
37. Lewinsohn PM, Rohde P, Klein DN, et al. Natural course of adolescent major depressive disorder, I: continuity into young adulthood. J Am Acad Child Adolesc Psychiatry. 1999;38(1):56-63. PubMed doi:10.1097/00004583-199901000-00020
38. Lewinsohn PM, Rohde P, Seeley JR. Major depressive disorder in older adolescents: prevalence, risk factors, and clinical implications. Clin Psychol Rev. 1998;18(7):765-794. PubMed doi:10.1016/S0272-7358(98)00010-5
39. Lewinsohn PM, Rohde P, Seeley JR, et al. Natural course of adolescent major depressive disorder in a community sample: predictors of recurrence in young adults. Am J Psychiatry. 2000;157(10):1584-1591. PubMed doi:10.1176/appi.ajp.157.10.1584