Objective: To determine the prevalence of excessive daytime sleepiness among medical students and establish a relationship between self-perceived sleepiness and psychological distress.
Methods: In a cross-sectional study, 441 medical students from a public-sector university in Pakistan completed a questionnaire from August to December 2018. The questionnaire included the Epworth Sleepiness Scale (ESS), which measured daytime sleepiness, and the 12-item General Health Questionnaire (GHQ-12), which measured mental health. Pearson correlations and student t tests were used for comparisons with a significance level of P < .05.
Results: Many of the students (44.9%) obtained a high score (≥ 10) on the ESS (ie, experience excessive daytime sleepiness). On average, higher scores on the ESS correlated with higher scores on the GHQ-12. A statistically significant correlation (P < .05) between ESS scores and GHQ-12 scores was obtained when the students with higher (≥ 10) ESS scores were compared with students with lower (< 10) ESS scores.
Conclusions: Excessive daytime sleepiness is frequent among medical students and significantly associated with psychological distress. Thus, careful investment in planning appropriate university policies and class schedules is required to encourage healthy and adequate sleep among students, which could have a significant impact on learning, academic performance, and health of medical students.
Association of Excessive Daytime Sleepiness With Psychological Distress in Medical Students
ABSTRACT
Objective: To determine the prevalence of excessive daytime sleepiness among medical students and establish a relationship between self-perceived sleepiness and psychological distress.
Methods: In a cross-sectional study, 441 medical students from a public-sector university in Pakistan completed a questionnaire from August to December 2018. The questionnaire included the Epworth Sleepiness Scale (ESS), which measured daytime sleepiness, and the 12-item General Health Questionnaire (GHQ-12), which measured mental health. Pearson correlations and student t tests were used for comparisons with a significance level of P < .05.
Results: Many of the students (44.9%) obtained a high score (≥ 10) on the ESS (ie, experience excessive daytime sleepiness). On average, higher scores on the ESS correlated with higher scores on the GHQ-12. A statistically significant correlation (P < .05) between ESS scores and GHQ-12 scores was obtained when the students with higher (≥ 10) ESS scores were compared with students with lower (< 10) ESS scores.
Conclusions: Excessive daytime sleepiness is frequent among medical students and significantly associated with psychological distress. Thus, careful investment in planning appropriate university policies and class schedules is required to encourage healthy and adequate sleep among students, which could have a significant impact on learning, academic performance, and health of medical students.
Prim Care Companion CNS Disord 2020;22(1):19m02531
To cite: Sameer HM, Imran N, Tarar TN, et al. Association of excessive daytime sleepiness with psychological distress in medical students. Prim Care Companion CNS Disord. 2020;22(1):19m02531.
To share: https://doi.org/10.4088/PCC.19m02531
© Copyright 2020 Physicians Postgraduate Press, Inc.
aKing Edward Medical University/Mayo Hospital, Lahore, Pakistan
bDepartment of Child and Family Psychiatry, King Edward Medical University/Mayo Hospital, Lahore, Pakistan
cDepartment of Psychiatry, UT Southwestern Medical Center, Dallas, Texas
dDepartment of Neurology, UT Southwestern Medical Center, Dallas, Texas
eCenter for Sleep Medicine, VA Medical Center, Dallas, Texas
fDepartment of Psychiatry, University of Oklahoma, Norman, Oklahoma
*Corresponding author: Hafiz M. Sameer, MBBS, King Edward Medical University/Mayo Hospital, Nelagumbad, Anarkali, Lahore, Pakistan 54000 ([email protected]).
Excessive daytime sleepiness is a difficulty in maintaining a desired level of wakefulness, often accompanied by symptoms such as psychomotor slowing and closing eyelids for a longer time than necessary for blinking.1,2 Daytime sleepiness is a significant problem, exhibited by 50% of college students compared to 36% of adolescents and adults.3 At least 3 days a week, 60% of college students report that they are dragging, tired, or sleepy.4 Moreover, daytime sleepiness has been found to be a factor in motor vehicle and work accidents, difficulties in adapting to new situations, social maladjustment problems, and decrease in quality of life.5-8 Although sleepiness or sleep deprivation has effects on many aspects of health, this article will focus on the areas that can be problematic for medical students.
Medical school is a time of intellectual growth and development of a young medical student into a professional doctor, and for the optimal return on the investment of time, effort, and money, students need to maximize their goals with regard to learning and academic and personal growth. Sleepiness from any cause can compromise these goals through its impact on learning, memory, grades, perception of effort, and mood. Of college students, 82% believe that inadequate sleep and sleepiness impact their school performance.9 College students rank sleep problems second only to stress among factors that negatively impact academic performance.4
Psychological distress is a general term used to describe unpleasant feelings or emotions that interfere with daily activities of life.10 It can result in the development of negative views of the environment, others, and even one’s self. Sadness, anxiety, distraction, and other symptoms of mental illness are manifestations of psychological distress.10
Information is lacking about the prevalence of pathological daytime sleepiness and its association with psychological distress among medical students. Such data could help in the planning of appropriate interventions to promote university policies and class schedules that encourage healthy and adequate sleep that may have a significant impact on learning, academic performance, and the health of medical students.
Therefore, the purpose of this study was to assess the prevalence of excessive daytime sleepiness among medical students using the Epworth Sleepiness Scale (ESS)11 and to establish a relationship between self-perceived sleepiness and psychological distress, as measured by the 12-item General Health Questionnaire (GHQ-12).12
METHODS
A cross-sectional study was conducted at a public-sector university in Pakistan from August to December 2018. The university institutional review board approved the study. The study was conducted in compliance with the Declaration of Helsinki’s ethical principles for medical research involving human subjects. Participation in the study was entirely voluntary. The confidentiality of the participants was ensured. Nonprobability convenience sampling was used to include medical students in the study after obtaining written informed consent. The data collection tool was a closed-ended, self-administered questionnaire, which included the ESS, GHQ-12, and demographic information such as age (years), sex (male, female), residence (home, hostel, private accommodation), average sleep time (< 6 hours, 6-< 7 hours, 7-8 hours, >8 hours), and year in medical school. Additional information on the use of regular sleeping aids (eg, sleeping pills) and use of caffeinated drinks per day (< 1 cup, 1-2 cups, 3-4 cups, >4 cups) was also included. The ESS is a standardized, validated questionnaire that assesses the likelihood of the subject to fall asleep during certain activities.10 It comprises 8 questions on different situations commonly encountered in daily life, and the subjects must rate their chances of dozing off or falling asleep during these situations. The responses range from 0 to 3 for each item and include would never doze, slight chance of dozing, moderate chance of dozing, and high chance of dozing based on the subject’s recent lifestyle. ESS scores are obtained by adding the scores of all 8 questions. ESS scores range from 0 to 24 and can be used to categorize subjects as within normal limits (ESS < 10) or as suffering from excessive daytime sleepiness (ESS ≥ 10).11

- Excessive daytime sleepiness is a highly prevalent but treatable condition among medical students that is often unrecognized in primary health care settings.
- Clinicians can help medical students achieve their educational goals more efficiently through early recognition and prompt treatment of excessive daytime sleepiness.
- Current evidence supports that pathological sleep habits have a negative impact on mental health among medical students.
The GHQ-12 is a measure of current mental health developed by Goldberg and Williams.12 It focuses on 2 major areas—the inability to carry out normal functions and the appearance of new and distressing experiences. It has 12 items with a Likert score of 0 to 3 for each. GHQ-12 scores are obtained by adding the scores of all 12 questions. Total score ranges from 0 to 36. A GHQ-12 score > 15 suggests evidence of distress, while a GHQ-12 score > 20 suggests severe problems and psychological distress.
Data Analysis
The data obtained in the study were analyzed using SPSS for Windows version 25.0 (SPSS Inc, Chicago, Illinois). The reliability of the ESS and GHQ-12 was determined through internal consistency by applying Cronbach α. The α value was set at 0.05. Descriptive statistics were calculated for the full dataset. Continuous variables are expressed as mean ± SD and compared using independent sample t test. For categorical variables, the number and percentages of students in each category were calculated, and χ2 test was used to compare independent groups. A P value < .05 was considered statistically significant.
RESULTS
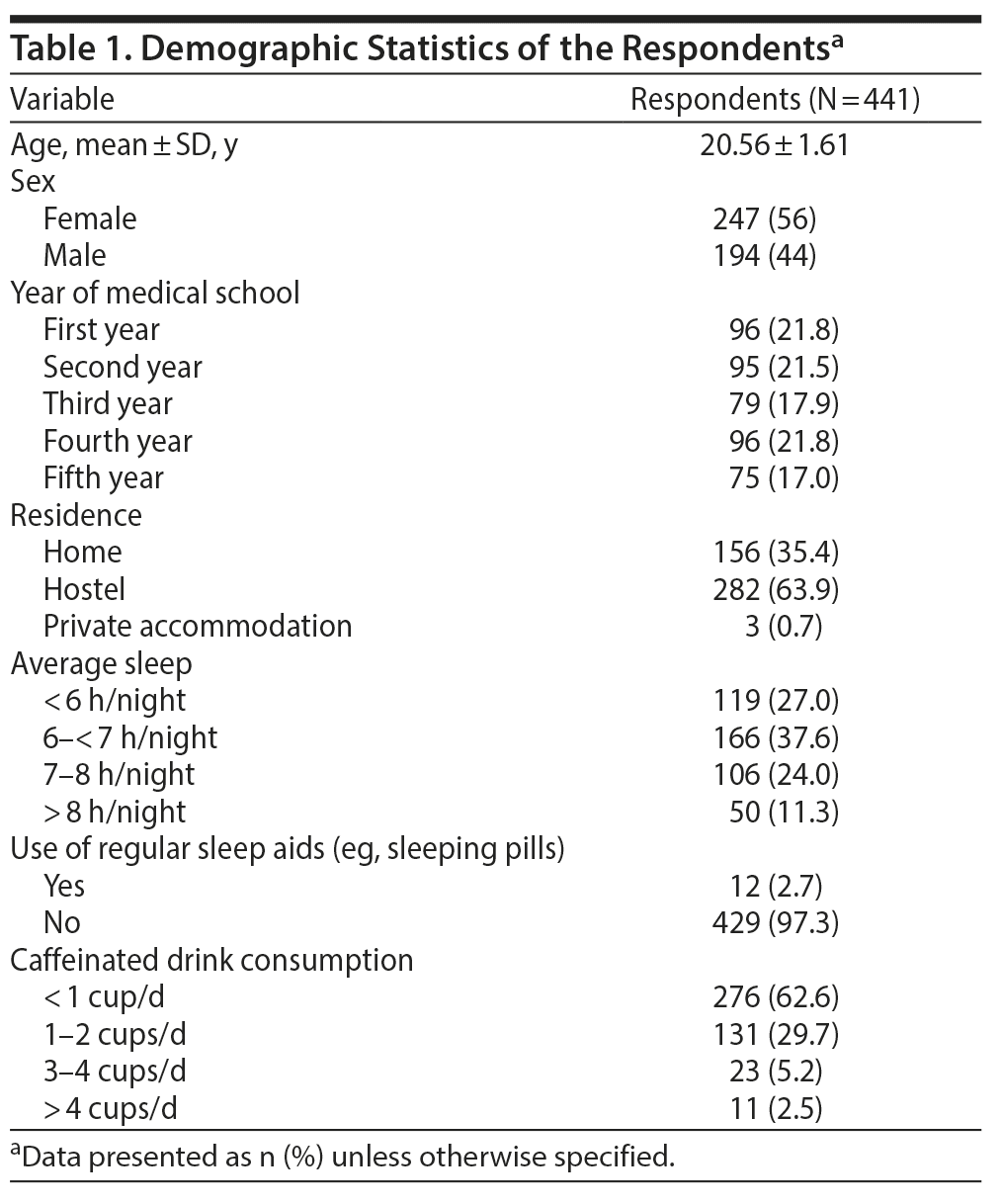
A total of 596 questionnaires were distributed among university students. Of the students, 441 responded, resulting in a 73.9% response rate. The mean ± SD age of the study population was 20.56 ± 1.61 years. The sample comprised 56% female and 44% male students. Students from all years of medical education were included in the study. The demographics of the study group are shown in Table 1.
The Cronbach α coefficient expressed the degree of internal uniformity among the items of the questionnaire. The overall Cronbach α coefficient of the ESS was 0.692, while the coefficient for the GHQ-12 was 0.867.
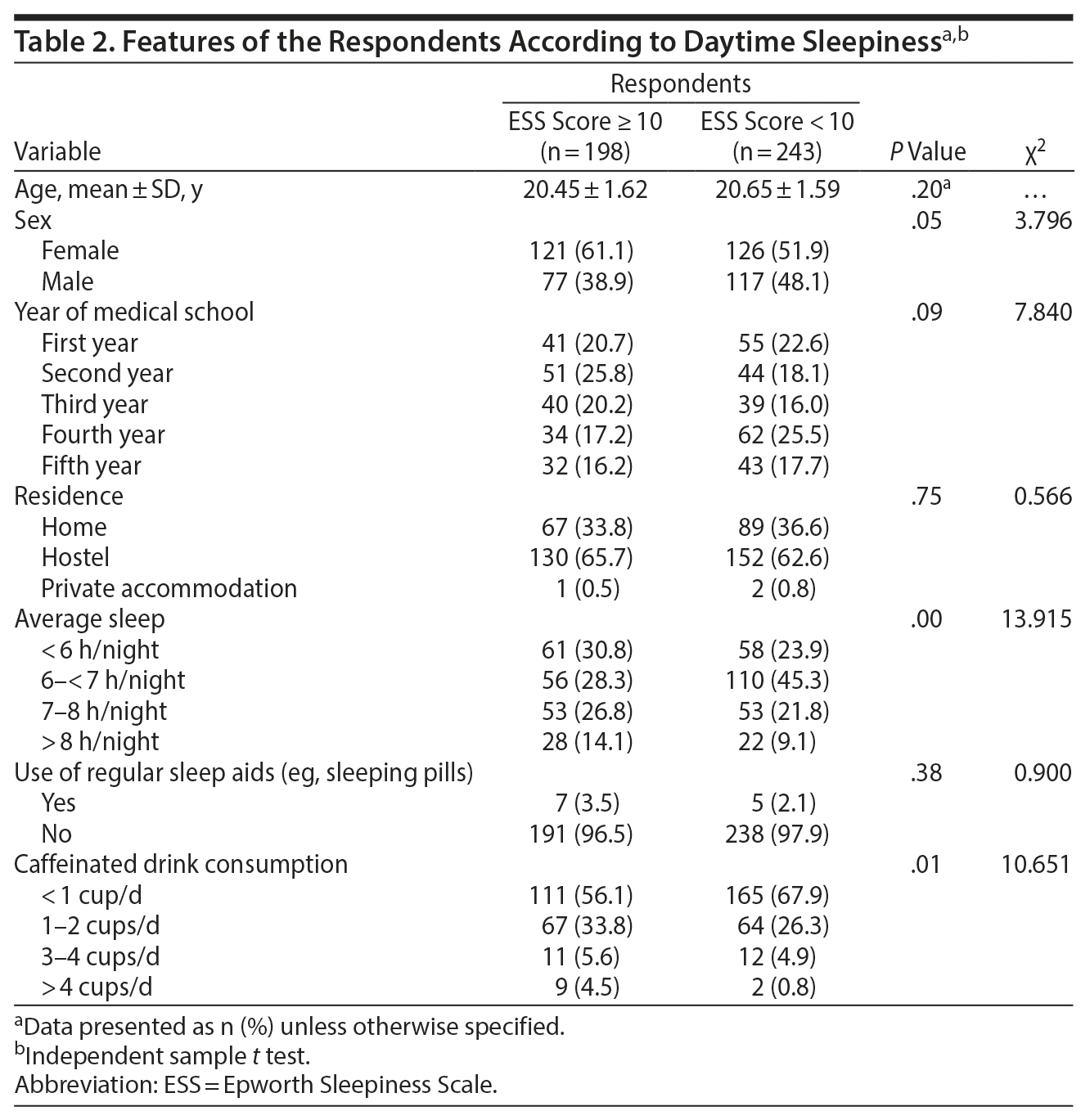
In our sample, 44.9% (n = 198) of the students were sleepy during the day (ESS score ≥ 10), and the mean ESS score of the whole study sample was 9.39 ± 3.94. Also, 121 (61.1%) women and 77 (38.9%) men scored ≥ 10 on the ESS. When the ESS scores were compared by sex, a P value of .05 was obtained. When sleep habits of the students were observed, it was found that 119 (27%) of 441 students had an average sleep time of less than 6 hours. However, 61 (30.8%) students among the group that scored ≥ 10 on the ESS had a mean sleep time of less than 6 hours, which was statistically significant (P < .05) compared to the group with an ESS score < 10. Only a small number of the students (n = 12, 2.7%) said that they used sleep aids regularly in the form of alprazolam, diphenhydramine, zolpidem, and eszopiclone taken orally. Sleep characteristics based on the status of sleepiness are shown in Table 2.
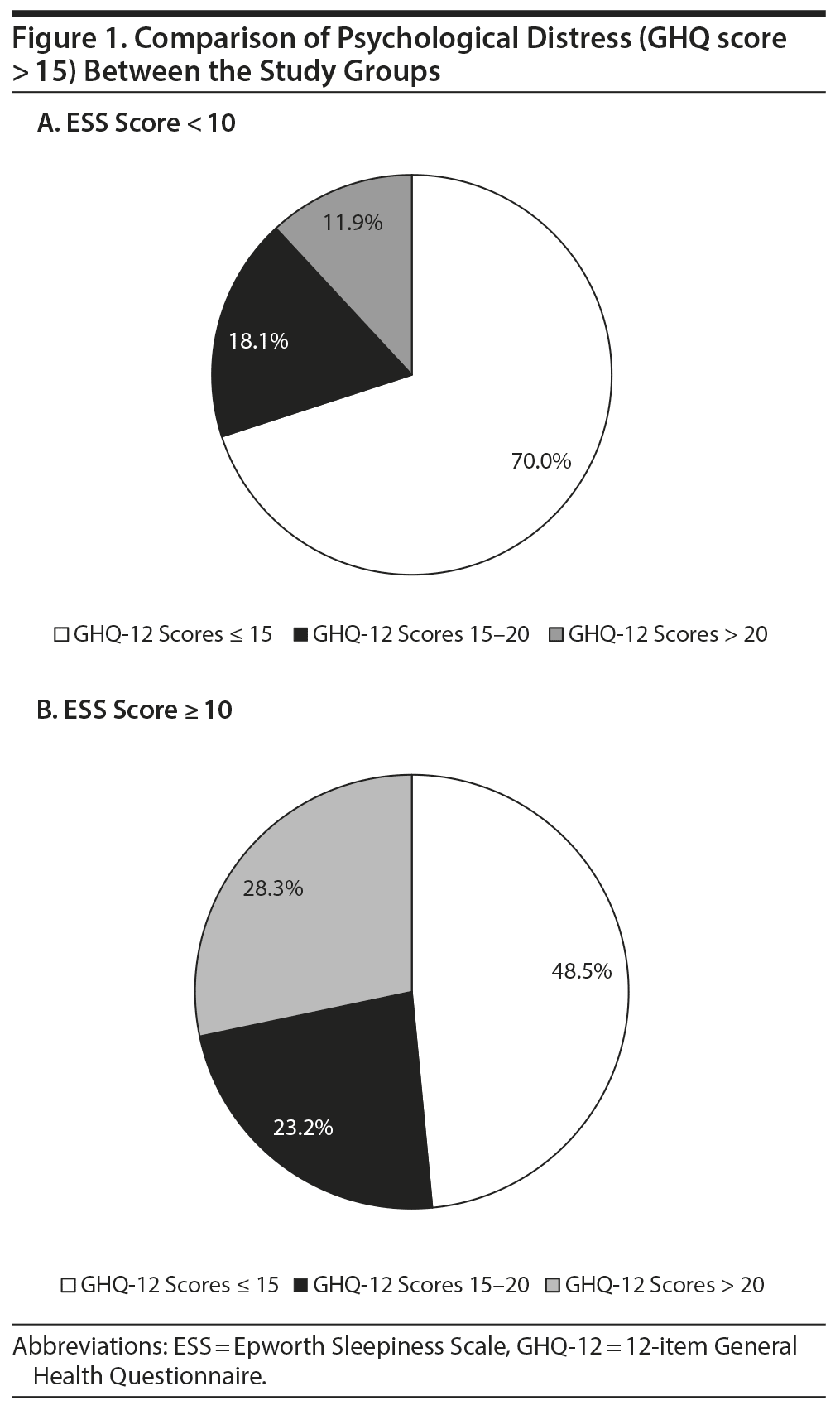
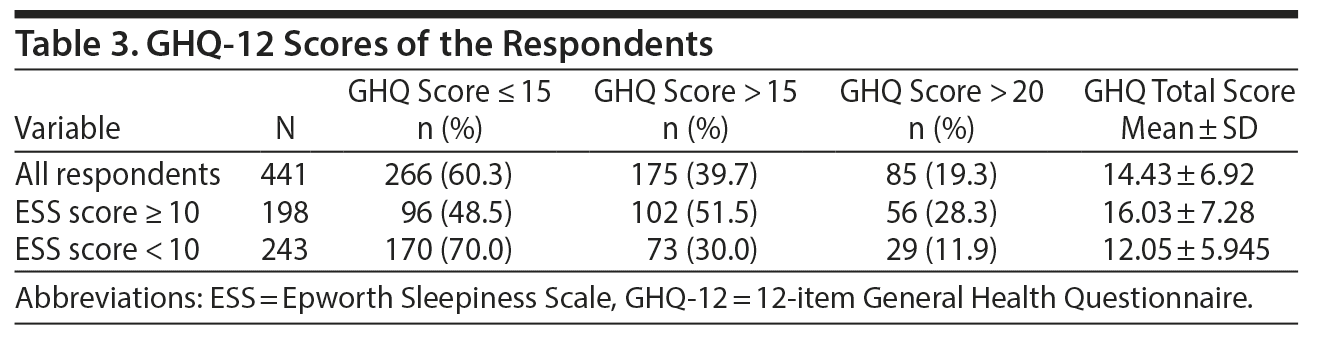
The mean ± SD GHQ-12 score of all respondents was 14.43 ± 6.92 (Table 3). The GHQ-12 scores of both ESS groups (≥ 10 and < 10) are shown in Table 3 and compared in Figure 1.
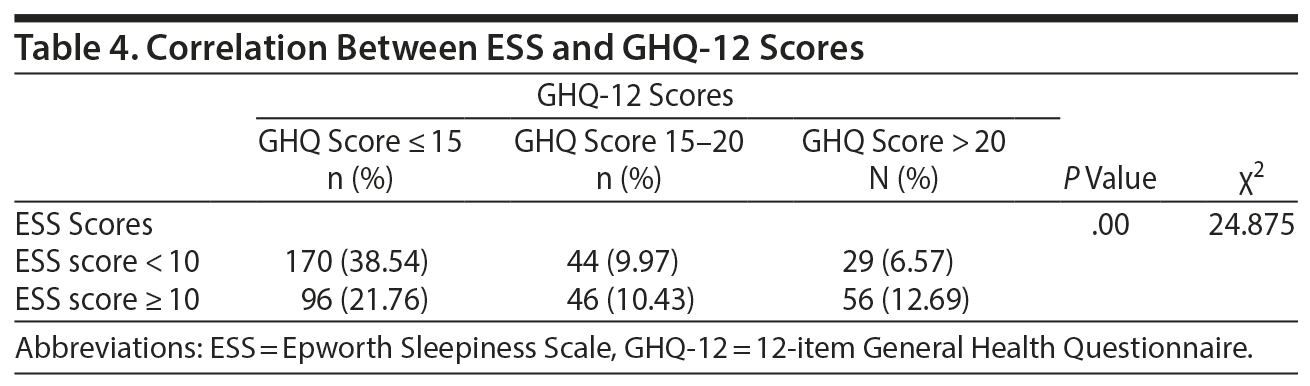
Among all respondents, 175 students (39.7%) showed symptoms of psychological distress (GHQ-12 score > 15), while 85 (19.3%) had symptoms of a severe mental health problem and psychological distress. However, 102 (51.5%) students among the ESS score ≥ 10 group showed symptoms of psychological distress (GHQ-12 score > 15), and 56 (28.3%) had symptoms of a severe mental health problem and psychological distress. This difference was statistically significant (P = .00, Table 4). Hence, the study shows that excessive daytime sleepiness has a significant impact on the mental health of medical students.
DISCUSSION
This study established that excessive daytime sleepiness is frequent among medical students and significantly associated with mental health problems. In our sample, 44.9% of the students (n = 198) were sleepy during the day (ESS score > 10), and a mean ± SD ESS score of 9.39 ± 3.94 was observed. The results are different from that of a study13 conducted in the general population that reported that 1 in 5 adults suffer from daytime sleepiness. In a study14 performed among academic and private practice physicians, a mean ESS score of 7.8 and a prevalence of excessive daytime sleepiness of 23% were reported, which is lower than the prevalence observed in our population.
Excessive daytime sleepiness among medical students correlated positively and significantly (P < .05) with average hours of sleep/night and number of caffeinated drinks consumed/day. Many of the students with a higher ESS score (≥ 10) usually sleep less than 6 hours per night (61 of a total of 198). This finding is consistent with another study15 that found medical students to be poor sleepers. Possible reasons for this behavior, especially in young adults, might include excessive use of energy drinks, use of stimulants (eg, amphetamine, nicotine), exam stress, noisy neighborhood, and excessive technology use before bedtime.9 All these factors heighten cognitive alertness, increase sleep latency, and eventually lead to difficulties falling asleep, repeated awakenings, or waking up too early.9 This subjective sense of not getting enough sleep at night might force students to take long afternoon naps, a factor leading to pathological daytime sleepiness.
On the other hand, 28 of 198 (14.1%) students with higher ESS scores (≥ 10) sleep more than 8 hours per night. This finding indicates that sleep deprivation is not the only cause of excessive daytime sleepiness. Excessive sleepiness in these students may be due to abuse of substances like alcohol or poor sleep quality at night.9 Possible causes of poor sleep quality might include sleep disorders (such as obstructive sleep apnea, parasomnia, or hypersomnia) and psychiatric disorders (such as depression), both of which are highly prevalent in the general population.9
Also, in our study sample, 4.5% of students with higher ESS scores had caffeine intake > 4 cups/day, while only 0.8% of students with a low (< 10) ESS score consumed that much caffeine. Previous research16 conducted on the impact of caffeine on excessive daytime sleepiness also showed high caffeine intake in people with ESS scores ≥ 10. When sex was compared with ESS scores, a P value of .05 was obtained. A P value < .05 is considered statistically significant, so in our study sex did not correlate significantly with ESS scores. Although the P value was not significant, the probability that ESS scores are not influenced by sex is still very low, as the obtained P value (.05) is very close to significance. Also, some international research1,16-18 found females to have more daytime sleepiness compared to males. Thus, our study highlights sex, average hours of sleep/night, and the number of caffeinated drinks consumed/day as reliable indicators of excessive daytime sleepiness among medical students.
In the current study, a highly significant association between excessive daytime sleepiness and GHQ-12 scores was observed (P < .01). Students with high ESS scores obtained higher mean GHQ-12 scores in comparison to students with lower ESS scores. These results are unequivocally striking, since a clear majority of the medical students perceive themselves as healthy and active individuals, with the belief that their sleep habits have no impact on their mental health. Hence, our study establishes that excessive daytime sleepiness is a contributory factor leading to poor mental health in medical students. To the best of our knowledge, no publication concerning the relationship between excessive daytime sleepiness and mental health of medical students is available from the academic institutions in Pakistan. One study19 of this issue reported sleep problems to have a significant impact on depression and anxiety in Estonian medical students, with daytime sleepiness being highlighted as a problem related to depressive symptoms in female students. Another study20 reported that personal sleep debt and daytime sleepiness mediate the relationship between short sleep and depression and anxiety risk in young adults. Also, some studies21,22 reported a negative impact of excessive daytime sleepiness on cognition of students, eventually leading to poor academic performance, while those done with physicians showed a decline in occupational performance. From a public health policy perspective, our study suggests that controlling excessive daytime sleepiness should be a priority in the prevention and reduction of mental health problems in the general population.
Our study has its own limitations since it was performed with medical students of a single public-sector university. Being cross-sectional, the study cannot explain causation, as it is unknown whether disturbed mental health is causing poor sleep quality and vice versa. More research is needed in this regard. The sample population included a narrow age range limit, thus results cannot be generalized.
In summary, excessive daytime sleepiness is frequent among medical students and significantly associated with mental health problems.
Submitted: August 19, 2019; accepted November 15, 2019.
Published online: February 20, 2020.
Potential conflicts of interest: None.
Funding/support: None.
REFERENCES
1.Chellappa SL, Araújo JF. Excessive daytime sleepiness in patients with depressive disorder. Br J Psychiatry. 2006;28(2):126-129. PubMed CrossRef
2.Santamaria J. How to evaluate excessive daytime sleepiness in Parkinson’s disease. Neurology. 2004;63(suppl 3):S21-S23. PubMed CrossRef
3.Oginska H, Pokorski J. Fatigue and mood correlates of sleep length in three age-social groups: school children, students, and employees. Chronobiol Int. 2006;23(6):1317-1328. PubMed CrossRef
4.American College Health Association: National College Health Assessment II. Reference Group Executive Summary, Fall 2011. American College Health Association website. https://www.acha.org/documents/ncha/ACHA-NCHA-II_ReferenceGroup_ExecutiveSummary_Fall2011.pdf. 2011. Accessed January 10, 2020.
5.Leger D. The cost of sleep-related accidents: a report for the National Commission on Sleep Disorders Research. Sleep. 1994;17(1):84-93. PubMed CrossRef
6.Briones B, Adams N, Strauss M, et al. Relationship between sleepiness and general health status. Sleep. 1996;19(7):583-588. PubMed CrossRef
7.Lyznicki JM, Doege TC, Davis RM, et al. Sleepiness, driving, and motor vehicle crashes. Council on Scientific Affairs, American Medical Association. JAMA. 1998;279(23):1908-1913. PubMed CrossRef
8.Mitler MM, Dement WC, Dinges DF. Sleep medicine, public policy, and public health. In: Kryger MH, Roth T, Dement W, eds. Principles and Practice of Sleep Medicine. Fifth ed. 2010:453-462.
9.Hershner SD, Chervin RD. Causes and consequences of sleepiness among college students. Nat Sci Sleep. 2014;6:73-84. PubMed CrossRef
10.Mirowsky J, Ross CE. Selecting outcomes for the sociology of mental health: issues of measurement and dimensionality. J Health Soc Behav. 2002;43:152-170. PubMed
11.Johns MW. A new method for measuring daytime sleepiness: the Epworth Sleepiness Scale. Sleep. 1991;14(6):540-545. PubMed CrossRef
12.Goldberg DP, Williams P. User’s Guide to the General Health Questionnaire. Windsor, UK: nferNelson; 1988.
13.Young TB. Epidemiology of daytime sleepiness: definitions, symptomatology, and prevalence. J Clin Psychiatry. 2004;65(suppl 16):12-16. PubMed
14.Chen I, Vorona R, Chiu R, et al. A survey of subjective sleepiness and consequences in attending physicians. Behav Sleep Med. 2008;6(1):1-15. PubMed CrossRef
15.Surani AA, Zahid S, Surani A, et al. Sleep quality among medical students of Karachi, Pakistan. J Pak Med Assoc. 2015;65(4):380-382. PubMed
16.Jun N, Lee A, Baik I. Associations of caffeinated beverage consumption and screen time with excessive daytime sleepiness in Korean high school students. Clin Nutr Res. 2017;6(1):55-60. PubMed CrossRef
17.Doi Y, Minowa M. Gender differences in excessive daytime sleepiness among Japanese workers. Soc Sci Med. 2003;56(4):883-894. PubMed CrossRef
18.Fatani A, Al-Rouqi K, Al Towairky J, et al. Effect of age and gender in the prevalence of excessive daytime sleepiness among a sample of the Saudi population. J Epidemiol Glob Health. 2015;5(suppl 1):S59-S66. PubMed CrossRef
19.Eller T, Aluoja A, Vasar V, et al. Symptoms of anxiety and depression in Estonian medical students with sleep problems. Depress Anxiety. 2006;23(4):250-256. PubMed CrossRef
20.Dickinson DL, Wolkow AP, Rajaratnam SMW, et al. Personal sleep debt and daytime sleepiness mediate the relationship between sleep and mental health outcomes in young adults. Depress Anxiety. 2018;35(8):775-783. PubMed CrossRef
21.Rodrigues RN, Viegas CA, Abreu E Silva AA, et al. Daytime sleepiness and academic performance in medical students. Arq Neuropsiquiatr. 2002;60(1):6-11. PubMed CrossRef
22.Ozder A, Eker HH. The prevalence of excessive daytime sleepiness among academic physicians and its impact on the quality of life and occupational performance. Int J Occup Med Environ Health. 2015;28(4):721-730. PubMed CrossRef
Enjoy this premium PDF as part of your membership benefits!