Objective: Early and higher detection rates of depression among dermatology patients can lead to better prognosis. Increased depression literacy among dermatologists might play a vital role in the early and successful detection and treatment of depression among their patients. The objective of this study was to investigate depression literacy among dermatologists working in India.
Methods: An online survey with a questionnaire comprising sociodemographic variables and the Depression Literacy Questionnaire was conducted to collect data on depression literacy among dermatologists between July 6, 2019, and August 6, 2019. Sociodemographic variables included age, sex, educational qualification, practice location, practice duration, and practice type.
Results: The response rate was 56.99%. The majority of respondents were aged 31-50 years, female, and working in urban areas. The mean ± SD total score of the respondents was 17.4 ± 2.36, with the lowest score being 10 and the highest score 22. More correct answers (98.1%) were recorded for the items "loss of confidence and poor self-esteem may be symptoms of depression" and "sleeping too much or too little may be sign of depression." The mean total score of female respondents was higher than that of men, and the difference was significant (P = .003).
Conclusions: The study revealed good depression literacy status among dermatologists working in India. Female respondents were found to have higher depression literacy.
Depression Literacy Among Dermatologists:
An Online Survey Study in India
ABSTRACT
Objective: Early and higher detection rates of depression among dermatology patients can lead to better prognosis. Increased depression literacy among dermatologists might play a vital role in the early and successful detection and treatment of depression among their patients. The objective of this study was to investigate depression literacy among dermatologists working in India.
Methods: An online survey with a questionnaire comprising sociodemographic variables and the Depression Literacy Questionnaire was conducted to collect data on depression literacy among dermatologists between July 6, 2019, and August 6, 2019. Sociodemographic variables included age, sex, educational qualification, practice location, practice duration, and practice type.
Results: The response rate was 56.99%. The majority of respondents were aged 31-50 years, female, and working in urban areas. The mean ± SD total score of the respondents was 17.4 ± 2.36, with the lowest score being 10 and the highest score 22. More correct answers (98.1%) were recorded for the items "loss of confidence and poor self-esteem may be symptoms of depression" and "sleeping too much or too little may be sign of depression." The mean total score of female respondents was higher than that of men, and the difference was significant (P = .003).
Conclusions: The study revealed good depression literacy status among dermatologists working in India. Female respondents were found to have higher depression literacy.
Prim Care Companion CNS Disord 2020;22(6):20m02608
To cite: Uvais NA, Abdul Latheef EN, Hafi B, et al. Depression literacy among dermatologists: an online survey study in India. Prim Care Companion CNS Disord. 2020;22(6):20m02608.
To share: https://doi.org/10.4088/PCC.20m02608
© Copyright 2020 Physicians Postgraduate Press, Inc.
aDepartment of Psychiatry, IQRAA International Hospital and Research Center, Kozhikode, Kerala, India
bDepartments of Dermatology, Venereology and Leprosy, Kozhikkod Government Medical College, Kozhikode, Kerala, India
cDepartment of Dermatology, IQRAA International Hospital and Research Center, Kozhikode, Kerala, India
dDepartment of Psychiatry, Central Michigan University, Mt Pleasant, Michigan
*Corresponding author: Bishurul Hafi, MD, Department of Dermatology, IQRAA International Hospital and Research Center, Wayanad Rd, Malapparamb Junction, Kozhikode, Kerala 673009, India ([email protected]).
Mental health conditions have emerged as an important public health issue worldwide, and with rapid changes in the socioeconomic status of developing societies like India, common mental disorders, especially depression, are increasing. A recent multisite population-based cross-sectional study1 regarding prevalence of depression found that the weighted prevalence of lifetime and current depressive disorder was 5.25% and 2.68%, respectively, indicating that around 23 million adults would need care for depressive disorder in India at any given time.
Depression is one of the most commonly diagnosed mental disorders in primary care settings. In India, it is estimated that nearly one-third of patients seeking help from health care facilities could have symptoms related to depression.1 Depression has also been found to be associated with various dermatologic conditions. A cross-sectional multicenter study2 among dermatologic outpatients in 13 European countries found that 10.1% of patients had clinical depression, and the association with depression was highest for patients with psoriasis, atopic dermatitis, hand eczema, and leg ulcers. Moreover, other studies3,4 have also shown significantly increased risks for depression and suicidality in psoriasis patients, and psoriasis has been independently associated with major depression. The burden of depression among dermatology patients is further amplified by its "cause and consequence" relationship with the primary dermatologic conditions.
Despite depressive disorder being a leading cause of disability, the public’s awareness of depression is poor, and many people with depressive disorder do not receive treatment. A study5 explored the undertreatment of people with major depressive disorder in 21 countries and found that only a minority of participants with depressive disorder received minimally adequate treatment: 1 in 5 people in high-income and 1 in 27 in low/lower middle-income countries. Although depression screening in dermatology outpatient departments is relatively easy with standardized screening tools such as the Patient Health Questionnaire-2 (PHQ-2),6 it is not practiced by most dermatologists. A survey7 of US dermatologists regarding screening for depression and suicidality in psoriasis patients found that only 27% ask about mood in the majority of their patient encounters, only 7% reported using a depression screening tool, and < 30% were familiar with the PHQ-2.
Health literacy is an individual’s ability to obtain, understand, and use health information to make appropriate decisions about health problems and how to seek treatment if necessary.8 However, dermatology patients may have poor knowledge regarding different types of mental disorders. Dermatologists are in a unique position to impart mental health literacy among the patients they encounter, to identify depressive disorder, and to help patients seek treatment. To this end, dermatologists must have sufficient depression literacy. One of the major reasons for the lack of depression detection among dermatology patients could be that dermatologists do not have proper training in the assessment and treatment of depression. A few studies9,10 have assessed the knowledge and competence of dermatologists in the recognition and treatment of depressive disorders. Because an understanding of the depression literacy of dermatologists may be helpful in the delivery of psychiatric care, the objective of this study was to investigate depression literacy in a sample of dermatologists working in India.
METHODS
We conducted an online survey with a questionnaire comprising sociodemographic variables and the Depression Literacy Questionnaire11 to collect data on depression literacy from July 6, 2019, to August 6, 2019. Sociodemographic variables included age, sex, qualification, practice location, practice duration, and type of dermatology practice. The Depression Literacy Questionnaire consists of 22 items.11 Respondents can answer each item with 1 of 3 options: true, false, or don’ t know, and each correct response receives 1 point. The total score ranges from 0 to 22. Higher scores indicate higher mental health literacy of depression. This scale has been used in the Indian population in the local language of Kannada. We identified 186 dermatologists working in India from online dermatology groups, and the study questionnaire in Google forms was sent to them through e-mail or WhatsApp. We followed up to confirm the physicians received the form. After all forms were received, the data were analyzed using SPSS version 21 (IBM, Armonk, New York). Data were analyzed for depression literacy score and its association with other factors. Depression literacy status was assessed in terms of the mean and SD of the items as well as the total scale. Cross tabulation was performed to assess the relationship of the Depression Literacy Questionnaire to sociodemographic variables by χ2 test and Fisher exact test. A P value < .05 was considered statistically significant. Ethical approval for this study was obtained from the institutional ethics committee before the commencement of the work.
RESULTS
Of 186 dermatologists, 106 responded to the questionnaire (response rate: 56.99%). The mean ± SD age of the respondents was 39.22 ± 9.48 years (range, 25 to 71 years). Most respondents were from the age group 31-50 years (70.7%), and 68% were women. Most respondents were from an urban area (48%) and were in a hospital-based practice (55.7%). Sociodemographic details are summarized in Table 1.
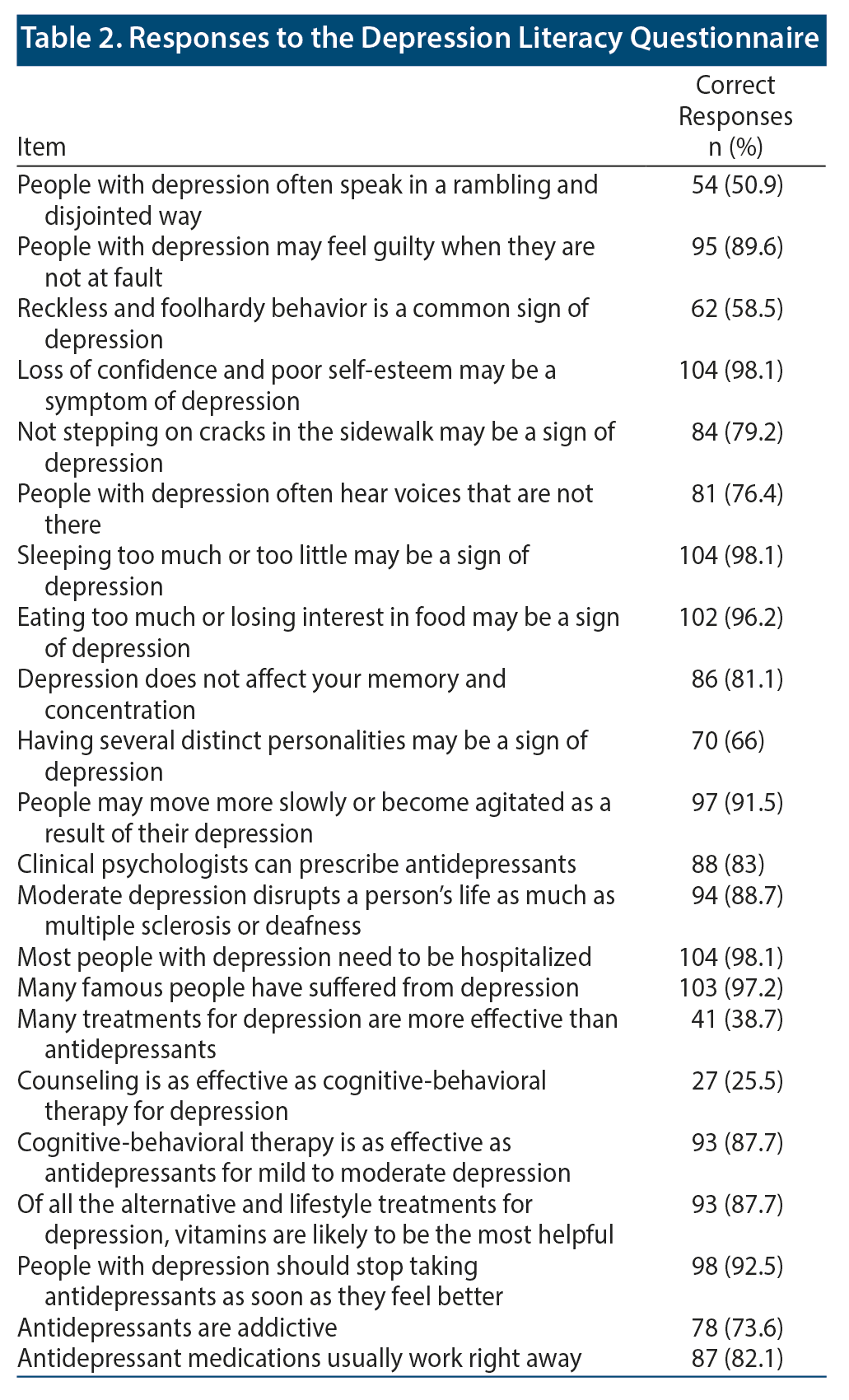
The mean ± SD total score of the respondents was 17.4 ± 2.36, with the lowest score being 10 (single respondent) and the highest score being 22 (2 respondents). The most correct answers (98.1%) were recorded for the items "loss of confidence and poor self-esteem may be symptoms of depression" and "sleeping too much or too little may be a sign of depression." The percentage of correct answers was low for the items "counseling is as effective as cognitive-behavioral therapy for depression" and "many treatments for depression are more effective than antidepressants" (25.5% and 38.7%, respectively). The responses are summarized in Table 2.
Mean total scores of female respondents were higher than those for men (17.86 ± 2.06 vs 16.44 ± 2.67), and the difference was significant (P = .003). No significant difference was noted between mean total scores and highest educational qualification, practice type, years of practice, or practice location.
DISCUSSION
We aimed to evaluate the depression literacy status of dermatologists working in India. The mean score of the Depression Literacy Questionnaire was 17.4, indicating a good overall depression literacy status among Indian dermatologists. The study revealed good literacy status in recognition of biological and cognitive symptoms of depression, as well as the impact of depression on the person. However, there was relatively poor literacy status in the recognition of some domains of behavioral symptoms, as well as the treatment aspects of depression. Considering our study results, there is a need to conduct training programs specifically for the management of depression, as most of the respondents could not differentiate counseling from cognitive-behavioral therapy for depression and also believed that many forms of treatments for depression are more effective than antidepressants.
Compared to past studies12,13 among medical or college students from India, our results show that dermatologists have significantly higher depression literacy. Ram et al12 studied depression literacy among 339 students in a tertiary care center in South India and found that depression literacy was poor among health care professional students, particularly paramedical students. Another study13 exploring depression literacy using a standardized tool, the Mental Health Literacy Questionnaire, among college students in Delhi found that more than half of the subjects had adequate awareness to identify depression.
Identification of symptoms and signs of depression by dermatologists in their patients is important for timely and effective management of depression. Our study results are encouraging in that a majority of dermatologists could identify symptoms of depression. Research14 has shown that among mental health disorders, depression is the easiest for non-mental health doctors to identify. In a mental health literacy survey of non-mental health professionals in 6 general hospitals in the Hunan Province of China, the identification rate for depression was the highest, followed by schizophrenia and generalized anxiety disorder.
However, how literacy of depression translates to clinical practice requires further evaluation among Indian dermatologists. A recent study7 evaluating dermatologists’ practices and comfort in screening for and discussing depression in psoriasis patients among 74 US dermatologists found that > 70% of participants screen for depression in less than half of encounters, which highlights an important practice gap. Another study15 evaluated the concordance between clinical assessment of depression by a dermatologist with the Hospital Anxiety and Depression Scale. The study15 found that agreement between dermatologists and Hospital Anxiety and Depression Scale scores was poor to fair for the diagnosis of depression, indicating that dermatologists tend to underestimate depressive disorder. However, most of the respondents felt relatively comfortable asking their patients about depression, and the factors associated with increased comfort included use of a screening tool, PHQ-2 familiarity, increased screening frequency, and belief that patients should be regularly monitored.15

- Early and higher detection rates of depression among dermatology patients can lead to better prognosis.
- Depression literacy among dermatologists might play a vital role in the detection and management of depression among their patients.
- Future research should explore the practical aspects of depression screening, management, and referral among Indian dermatologists.
In conclusion, depression literacy among this sample of dermatologists was positive, and it is encouraging that they have the ability to obtain, understand, and use health information to make appropriate decisions with regard to depressive disorder for their patients. Future research should explore the practical aspects of depression screening, management, and referral among Indian dermatologists, as comorbid depression with dermatologic conditions should be identified and treated.
Submitted: February 24, 2020; accepted May 15, 2020.
Published online: November 19, 2020.
Potential conflicts of interest: None.
Funding/support: None.
REFERENCES
1.Arvind BA, Gururaj G, Loganathan S, et al; NMHS collaborators group. Prevalence and socioeconomic impact of depressive disorders in India: multisite population-based cross-sectional study. BMJ Open. 2019;9(6):e027250. PubMed CrossRef
2.Dalgard FJ, Gieler U, Tomas-Aragones L, et al. The psychological burden of skin diseases: a cross-sectional multicenter study among dermatological out-patients in 13 European countries. J Invest Dermatol. 2015;135(4):984-991. PubMed CrossRef
3.Kurd SK, Troxel AB, Crits-Christoph P, et al. The risk of depression, anxiety, and suicidality in patients with psoriasis: a population-based cohort study. Arch Dermatol. 2010;146(8):891-895. PubMed
4.Cohen BE, Martires KJ, Ho RS. Psoriasis and the risk of depression in the US population: National Health and Nutrition Examination Survey 2009-2012. JAMA Dermatol. 2016;152(1):73-79. PubMed CrossRef
5.Thornicroft G, Chatterji S, Evans-Lacko S, et al. Undertreatment of people with major depressive disorder in 21 countries. Br J Psychiatry. 2017;210(2):119-124. PubMed CrossRef
6.Kroenke K, Spitzer RL, Williams JB. The Patient Health Questionnaire-2: validity of a two-item depression screener. Med Care. 2003;41(11):1284-1292. PubMed CrossRef
7.Liang SE, Cohen JM, Ho RS. Screening for depression and suicidality in psoriasis patients: a survey of US dermatologists. J Am Acad Dermatol. 2019;80(5):1460-1462. PubMed CrossRef
8.Jorm AF, Korten AE, Jacomb PA, et al. "Mental health literacy": a survey of the public’s ability to recognize mental disorders and their beliefs about the effectiveness of treatment. Med J Aust. 1997;166(4):182-186. PubMed CrossRef
9.Gee SN, Zakhary L, Keuthen N, et al. A survey assessment of the recognition and treatment of psychocutaneous disorders in the outpatient dermatology setting: how prepared are we? J Am Acad Dermatol. 2013;68(1):47-52. PubMed CrossRef
10.Picardi A, Amerio P, Baliva G, et al. Recognition of depressive and anxiety disorders in dermatological outpatients. Acta Derm Venereol. 2004;84(3):213-217. PubMed CrossRef
11.Gulliver A, Griffiths KM, Christensen H, et al. Internet-based interventions to promote mental health help-seeking in elite athletes: an exploratory randomized controlled trial. J Med Internet Res. 2012;14(3):e69. PubMed CrossRef
12.Ram D, Benny N, Gowdappa B. Relationship between depression literacy and medication adherence in patients with depression. Journal of Mood Disorders. 2016;6(4):183-188. CrossRef
13.Arundev U, Gupta S, Sharma K, et al. Mental health literacy among university students from University Of Delhi. Indian J Psychiatric Nursing. 2017;13(1):1-7. CrossRef
14.Wu Q, Luo X, Chen S, et al. Mental health literacy survey of non-mental health professionals in six general hospitals in Hunan Province of China. PLoS One. 2017;12(7):e0180327. PubMed CrossRef
15.Dalgard FJ, Svensson Å, Gieler U, et al. Dermatologists across Europe underestimate depression and anxiety: results from 3,635 dermatological consultations. Br J Dermatol. 2018;179(2):464-470. PubMed
Enjoy this premium PDF as part of your membership benefits!