Depression in Premedical Undergraduates: A Cross-Sectional Survey
Background: Medical students and residents are known to have high rates of depression, a common stress-related challenge that impairs quality of life and job satisfaction and predisposes those affected to general medical illness. Our primary hypothesis was that premedical students would exhibit greater depressive symptoms than nonpremedical students. A secondary aim was to explore the interactions of premedical student status with gender and ethnicity in the context of depression.
Method: In this cross-sectional study 647 premedical and 1,495 nonpremedical undergraduates at the University of California, San Diego, were surveyed to examine whether seeds of depression can be identified even before formal medical training. Participants completed a series of demographic questions along with the 9-item Patient Health Questionnaire to gauge depression intensity. The survey was made available online for a period of 3 months from March 2009-June 2009.
Results: Premedical students were more likely to meet screening criteria suggestive of the presence of major depressive disorder and to exhibit more severe depression than nonpremedical students. Female premedical students exhibited greater depression than female nonpremedical students and males in general. Hispanic premedical students, in particular, had a greater prevalence of depression and greater intensity of depressive symptoms than other premedical students and Hispanic nonpremedical students. No differences were found in current, past, or family history between premedical and nonpremedical students.
Conclusions: These findings underscore the importance of understanding the unique strains and mental health consequences of a premedical curriculum, especially for women and certain minority ethnic populations. A meaningful next step would be a larger study, conducted by several representative university campuses, to confirm these findings; a follow-up of these cohorts could track longitudinal progress. More research must be done to determine the etiology of these findings with the ultimate intention of identifying opportunities for prevention and early intervention, which may provide significant public health payoffs in the long run.
Prim Care Companion J Clin Psychiatry 2010;12(6):e1-e6
© Copyright 2010 Physicians Postgraduate Press, Inc.
Submitted: January 27, 2010; accepted April 22, 2010.
Published online: November 25, 2010 (doi:10.4088/PCC.10m00958blu).
Corresponding author: Daniel Z. Fang, BS, Department of Psychiatry, University of California San Diego, 9500 Gilman Dr, 9116A, La Jolla, CA 92093 ([email protected]).
Medical students, interns, and resident physicians are exposed to unique pressures that render them vulnerable to a variety of stress-related health challenges. One example that has received much recent attention is the development of major depressive disorder (MDD). MDD is common in medical students and residents, can radically impair quality of life, may lead to career shifts, and can have substantial psychosocial, general medical, and psychiatric adverse sequelae.1-3 Does the risk for these occupational hazards begin in medical school, or can their seeds be identified earlier in life? The answer may help identify opportunities for prevention and early intervention that could provide huge public health payoffs in the long run. This article attempts to answer that question by assessing the intensity and prevalence of depressive symptoms in premedical students before entering formal medical training.
A debilitating and life-shortening illness, MDD is a prominent cause of disability, health impairment, and mortality and is largely, but not exclusively, related to increased rates of suicide.3 The current literature suggests that there are high levels of depression in medical students,1 interns, and residents,4-6 which may contribute to the higher rates of physician suicide.7 The suicide rate among male and female physicians is 40% and 130% higher, respectively, than that of men and women in the general population.8 Problems with drug abuse and alcohol and increased access to and knowledge about potentially lethal medications, especially under circumstances of heightened stress, have been cited as reasons for this elevation in suicide rate. Among female physicians, degrading experiences and sexual harassment may also be contributing factors.7,9
Clinical Points
- Premedical students have greater depression prevalence and severity than nonpremedical students.
- Premedical female students and certain minority groups, such as Hispanics and Asians, may be at increased risk for depression.
- Awareness of certain premedical students’ risk for depression may alert university administrators, student health services, and physicians to develop targeted primary prevention strategies, screening and diagnostic programs, and accessible early intervention.
Because of the high levels of MDD in medical students, house staff, and other physicians, a natural next step is to identify whether the risk for MDD begins in medical school or perhaps even earlier. One possibly rewarding place to look is during undergraduate years. With increasing pressures to achieve top grade point averages, score highly on the Medical College Admission Test, and involve oneself in multiple commitments such as clinical volunteering, research, and other extracurricular activities, premedical student expectations are high. Although it has been shown that medical students enter their first year of training with similar depression intensity as the general public,2 little empirical data have been collected regarding depression among premedical college undergraduates.
To begin to rectify these gaps in our knowledge, this cross-sectional study surveys premedical and nonpremedical undergraduates at the University of California, San Diego (UCSD), in order to assess the intensity of depression among college premedical undergraduates. Our primary hypothesis is that premedical students will exhibit greater depressive symptoms than nonpremedical students. As a secondary aim, we will also explore the interactions of premedical student status with gender and ethnicity in the context of depression.
METHOD
Participants and Procedure
The original online survey sample consisted of 2,427 participants who were recruited through 3 means: (1) UCSD Psychology Department Experimetrix course credit program, (2) an invitational e-mail sent to all members of the Health and Medical Professions Preparation Program, and (3) an invitational e-mail sent to all UCSD undergraduate students who had declared 1 or more of the 8 majors in the biology department: biochemistry and cell biology; ecology, behavior, and evolution; general biology; microbiology; molecular biology; bioinformatics; human biology; and physiology and neuroscience.10 Participants were informed that the study aimed to assess depression in undergraduates and were offered either course credit or entry into a raffle for gift cards as compensation. Precautions such as removal of all identifying markers were taken to ensure anonymity of the responses. The survey was made available online for a period of 3 months from March 2009-June 2009.
The depression questionnaire consisted of demographic and basic clinical questions, and the 9-item Patient Health Questionnaire (PHQ-9).11 Demographic and clinical information included gender, ethnicity, age, major, premedical status, graduation date, past and current history of MDD, family history of MDD, and perceived financial strain (scale of 1-7).
Measuring depression. The PHQ-9 consists of 9 questions based on the DSM-IV criteria for a major depressive episode. This depression screening tool has proven to be reliable and valid relative to diagnoses provided by mental health professionals and other depression assessment tools across many populations.11-13 Scoring of the PHQ-9 followed standard procedures; individual item scores ranged from 0 (never) to 3 (nearly every day), and the total possible score ranged from 0 to 27. Total mean scores were used as an index of depression symptom intensity. Standard PHQ-9 criteria were used to designate cut-off points for insignificant, mild, moderate, moderately severe, and severe depression symptomatology as well as for symptoms suggestive of MDD14 as follows:
- Criteria for insignificant depression: total PHQ-9 score of 0-4
- Criteria for mild depression: total PHQ-9 score of 5-9
- Criteria for moderate depression total PHQ-9 score of 10-14
- Criteria for moderately severe depression: total PHQ-9 score of 15-19
- Criteria for severe depression: total PHQ-9 score of 20-27
- Criteria for symptoms suggestive of MDD (yes or no): at least 5 of the 9 questions are answered with either “more than half the days” or “nearly every day,” 1 of which must be either question 1 (feeling little interest or pleasure in doing things) or question 2 (feeling down, depressed, or hopeless). Participants who meet these criteria are designated “met DSM criteria.” This is in comparison to subjects designated as “diagnosed MDD” who answered positively to our survey query asking if participants have been given a current clinical diagnosis of MDD.
Analysis
For continuous variables, an analysis of variance was used to compare groups and to test interactions between different covariates. For categorical variables, χ2 statistical analysis was used to explore differences between premedical students and the presence of MDD as defined by PHQ-9 criteria, current diagnosis of MDD, past history of MDD, family history of MDD, and the 5 categories of depression severity. In our analysis of ethnicity, 22 African American students, 69 Indian American students, and 92 “other” students were grouped together into 1 category labeled “other.” As part of the analysis for gender and ethnicity, MDD prevalence and mean PHQ-9 scores between premedical and nonpremedical students were analyzed for males and females separately; the same was done for each of the ethnic groups. Tukey’s HSD test was used for post hoc analysis when appropriate. Although PHQ-9 data were not normally distributed, parametric analysis was utilized because of the large sample size. All tests were 2-sided with a type I error rate of 0.05 and were done with SPSS version 17.00 (SPSS Inc, Chicago, Illinois).
RESULTS
Of the original 2,427 participants, the 285 students who did not answer the demographic questions regarding gender, ethnicity, and premedical status or who omitted items on the PHQ-9 were excluded from all analyses. The remaining 2,142 students consisted of 647 premedical and 1,495 nonpremedical undergraduate students at UCSD.
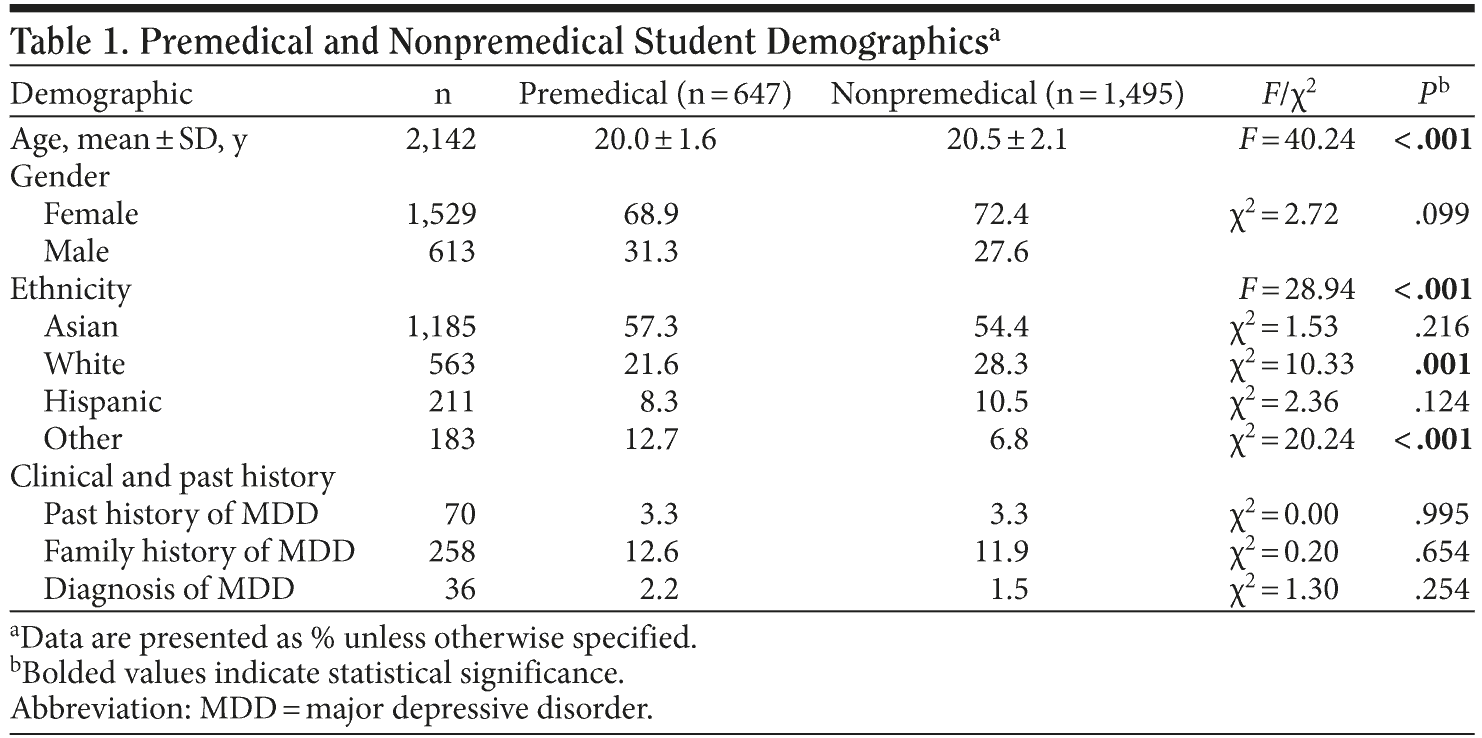
Overall. As seen in Table 1, the premedical and nonpremedical groups were significantly different on their age (F2 = 40.24, P < .001); however, this difference is not clinically relevant (20.0 vs 20.5). These groups also had similar gender distributions. The majority of participants were Asian American (n = 1,185), with whites (n = 563) and Hispanics (n = 211) being the next largest populations, followed by other (n = 183) (F = 28.94, P < .001). A greater portion of the nonpremedical students were white compared to premedical students (28.3% vs 21.6%, χ2 = 10.33, P = .001). On the other hand, the group classified as “other” comprised a greater portion of the premedical group than the nonpremedical group (12.7% vs 6.8%, χ2 = 20.24, P < .001). There were no differences between groups in past or family histories of MDD or in the likelihood of being diagnosed with MDD.
As seen in Table 2, premedical students had significantly greater PHQ-9 mean scores for depression intensity than nonpremedical students (8.0 vs 6.9, F2 = 17.94, P < .001) and were more likely to meet PHQ-9 symptomatic criteria for MDD (14.7% vs 10.6%, χ2 = 7.34, P = .007). A significant relationship was observed between the PHQ-9 severity cut-offs and premedical status (F = 28.94, P < .001), with premedical students more likely to be rated as severely depressed (4.8% vs 2.5%, χ2 = 7.88, P = .005) and less likely to have insignificant depression than nonpremedical students (33.4% vs 40.1%, χ2 = 8.72, P = .003).
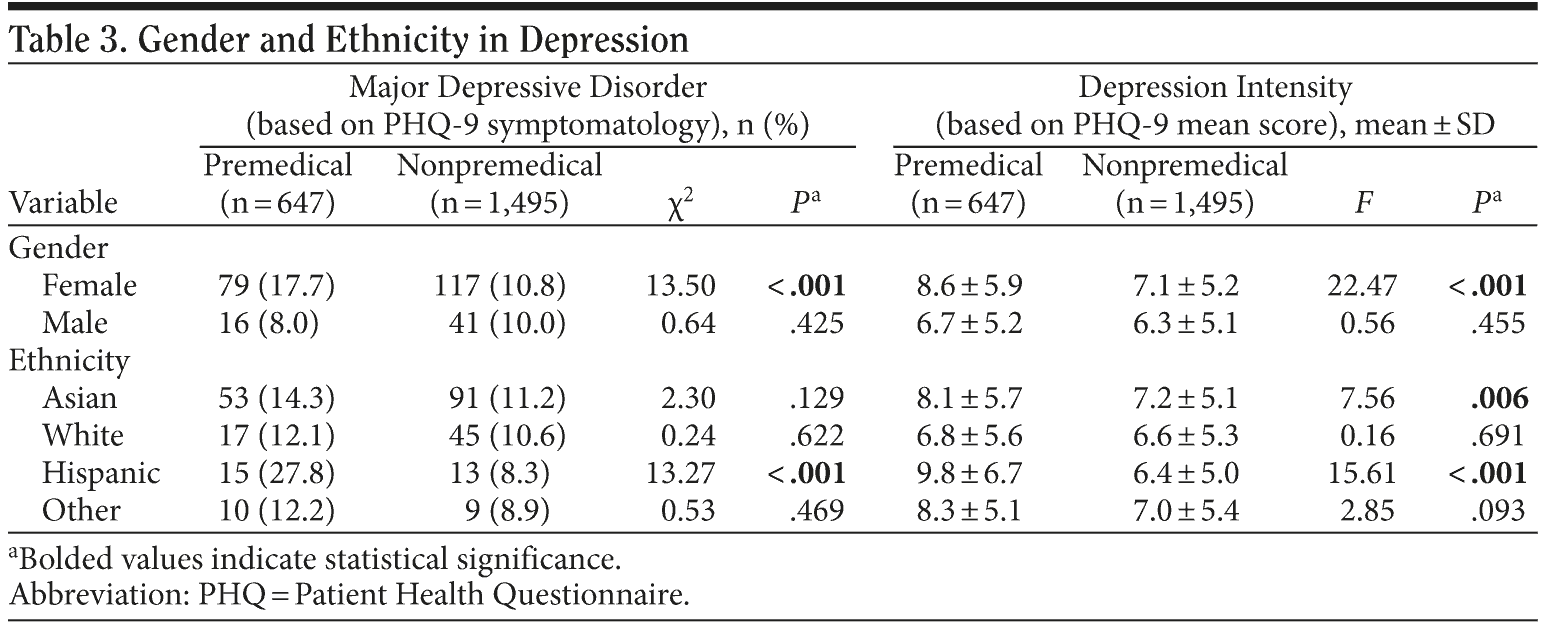
Gender and depression. Overall, female students were more likely to meet PHQ-9 symptomatic criteria for MDD than male students (12.8% vs 9.3%, χ2 = 5.21, P = .023). A 2-way analysis of variance revealed a significant interaction between premedical status and gender (F2 = 4.10, P = .043), with female premedical students having higher mean PHQ-9 scores than female nonpremedical students (8.6 ± 5.9 vs 7.1 ± 5.2) and male students both premedical (8.6 ± 5.9 vs 6.7 ± 5.2) and nonpremedical (8.6 ± 5.9 vs 6.3 ± 5.1). As seen in Table 3, more premedical females than nonpremedical females met PHQ-9 criteria for MDD (17.7% vs10.8%, χ2 = 13.50, P < .001). Premedical females also showed greater depression intensity than nonpremedical females based on mean PHQ-9 scores (8.6 vs 7.1, P < .001). There were no differences between premedical and nonpremedical males in either MDD prevalence or depression intensity.
Ethnicity and depression. There was a significant interaction between premedical status and ethnicity with regard to mean PHQ-9 scores (F2 = 3.57, P = .14). Post hoc analysis found greater depression intensity in Hispanic premedical students compared to white premedical students (9.8 ± 6.7 vs 6.8 ± 5.6, P = .006) and to Hispanic nonpremedical students (9.8 ± 6.7 vs 6.4 ± 5.0, P < .001). Hispanic premedical students were more likely to meet symptomatic criteria for MDD than Hispanic nonpremedical students (27.8% vs 8.3%, χ2 = 13.27, P < .001) and all other ethnicities (27.8% vs 12.1%-14.3%, χ2 = 8.06, P = .005). Finally, Asian premedical students had greater mean depression intensity than Asian nonpremedical students (8.1 vs 7.2, P = .006). There were no significant 3-way interactions between premedical status, gender, and ethnicity.
Current, past, and family history of MDD. As expected, students with symptoms suggestive of MDD as defined by the PHQ-9 were more likely to carry a current diagnosis of MDD (9.6% vs 0.6%, χ2 = 106.85, P < .001), to have had a past diagnosis of MDD (10.6% vs 2.4%, χ2 = 45.49, P < .001), and to have had a family history of MDD (16.7% vs 11.5%, χ2 = 5.59, P = .018). No differences were found in current, past, or family history between premedical and nonpremedical students.
DISCUSSION
This study is the first we are aware of that examines depression in undergraduate premedical students. The results support our main hypothesis that premedical students would have higher scores on the PHQ-9, indicating greater depressive symptoms, than nonpremedical students.
Key findings include greater intensity of depression in premedical students compared to nonpremedical students, particularly among female and Hispanic students. There was a substantial discrepancy between the number of students with MDD based on PHQ-9 criteria and the number actually carrying a clinical diagnosis of MDD.
Premedical Student Depression
Premedical students were found to have both greater depression intensity and prevalence of MDD than nonpremedical students. Furthermore, nearly twice the number of premedical students belonged in the category of “severely depressed” as nonpremedical students. These results extend several previous studies showing greater intensity and prevalence of depression in medical students, interns, residents, and physicians than in age-matched controls1,4,5 and suggests a continuity of depressive symptoms in physicians going back at least as far as undergraduate studies. This is one of the first studies to show an early emergence of depression during the premedical stage of training. The discrepancy between the number of premedical students diagnosed with MDD (2.2%) and the number of premedical students meeting PHQ-9 criteria for MDD (14.7%) is consistent with a previous study in which 15.2% of medical students were found to be depressed, yet only 26.5% of them were receiving treatment.15 Taken together, these findings suggest that premedical and medical students with clinically significant self-rated depressive symptoms may be both underdiagnosed and undertreated.
Gender and Premedical Status Interaction
Premedical female students were found to have both greater depression intensity and prevalence of MDD than nonpremedical female and male students. This result is similar to many previous studies that have found strong associations between female gender and increased depression rates.5 For example, 1 study calculated a 2:1 female to male ratio for both MDD and dysthymia.11 This study suggests that females who choose to pursue medicine may have 2 risk factors that combine and result in an even greater overall depression intensity than being a female or a premedical student alone. Furthermore, these findings support previous research showing differences in depression by gender with higher rates among female medical students.5 The lack of differences in MDD prevalence and depression intensity between premedical and nonpremedical males students may suggest the possibility of a gender-specific phenomenon. More research must be done in order to determine the exact relationships between gender, depression, and premedical status.
Ethnicity and Premedical Status Interaction
Hispanic premedical students had greater depression intensity than white premedical students and Hispanic nonpremedical students with a prevalence of MDD twice that of other ethnicities. This finding is similar to those of a previous study of Hispanic medical students in which the Hispanic medical students were 3.4 times more likely to be depressed than non-Hispanic students.16
Additionally, Asian American premedical students were found to have greater depression intensity than Asian American nonpremedical students. An underlying reason for this vulnerability may include culturally specific maladaptive and parent-driven perfectionism, which has been linked with risk for depression among Asian Americans.17 Also, Asian Americans were less likely to seek social and emotional support and more likely to be depressed than whites.18,19 This sense of perfectionism alongside a lesser tendency to seek support, when combined with the stress of trying to get into medical school, may lead Asian American premedical students to greater levels of depression than nonpremedical students.
For both Asian American and Hispanic premedical students, research leading to a better understanding of the complex relationship between culture and depression may help lead to development of meaningful primary prevention and early intervention strategies targeting these groups. Such discoveries could provide enormous public health benefits.
Limitations
Several limitations must be considered in the context of these findings. First, the nonpremedical students outnumbered the premedical students by over 2-fold. Second, the gender distribution was such that roughly 70% of the responders were female. Third, the ethnic distribution of the responders (55% Asian American, 26% white, 10% Hispanic, and 9% other) was not representative of the US population, making generalization to other student groups difficult. Fourth, the survey population consisted primarily of students with interests in biology, psychology, or medicine. Thus, results may not be generalizeable to all undergraduates at UCSD or premedical students at other universities. Finally, the cross-sectional nature of this study precludes the possibility of making causal connections. These caveats aside, the substantial sample, and the implementation of validated and psychometrically sound measures of depression, provide important preliminary findings in a clinically meaningful area of investigation.
Concluding Remarks
Premedical students face a variety of extrinsic and intrinsic pressures. Fierce competition for medical school placement breeds high extrinsic pressures to achieve stellar grade point averages, possess unique extracurricular activities, produce remarkable research experiences, and participate in meaningful volunteer work. Intrinsic pressures of self-motivation, perfectionism, hard work, and determination, the very things we admire physicians for, may be the same traits, which, when combined with extrinsic pressures, become a hindrance to a person’s well being. Additional contributing factors, such as female gender and Hispanic ethnicity, together paint an overall picture of a premedical student’s vulnerable mental health. A dynamic interplay of many factors contributes to stress, strain, mental health, and mental illness. However, due to the lack of research, especially randomized, longitudinal studies, these conclusions still remain speculative. A meaningful next step should be a larger study, possibly conducted at several representative university campuses, to confirm these results; a follow-up to these cohorts could track longitudinal progress. Above all, more research in these important areas must be done to better understand premedical student mental health with the ultimate purpose of developing methods to recognize, support, and treat those in need of help.
Author affiliations: Department of Psychiatry, University of California, San Diego.
Potential conflicts of interest: None reported.
Funding/support: The John A. Majda, MD Memorial Fund provided financial support.
Previous presentation: A version of this manuscript was presented as an abstract at the Western Student Medical Research Forum; January 28, 2010; Carmel, California.
REFERENCES
1. Dyrbye LN, Thomas MR, Massie FS, et al. Burnout and suicidal ideation among US medical students. Ann Intern Med. 2008;149(5):334-341. PubMed
2. Dyrbye LN, Thomas MR, Shanafelt TD. Systematic review of depression, anxiety, and other indicators of psychological distress among US and Canadian medical students. Acad Med. 2006;81(4):354-373. PubMed doi:10.1097/00001888-200604000-00009
3. Goldsmith SK, Pellmar TC, Kleinman AM, et al, eds. Reducing Suicide: A National Imperative. Washington, DC: National Academies Press; 2002.
4. Shanafelt TD, Bradley KA, Wipf JE, et al. Burnout and self-reported patient care in an internal medicine residency program. Ann Intern Med. 2002;136(5):358-367. PubMed
5. Goebert D, Thompson D, Takeshita J, et al. Depressive symptoms in medical students and residents: a multischool study. Acad Med. 2009;84(2):236-241. PubMed doi:10.1097/ACM.0b013e31819391bb
6. Dunn LB, Green Hammond KA, Roberts LW. Delaying care, avoiding stigma: residents’ attitudes toward obtaining personal health care. Acad Med. 2009;84(2):242-250. PubMed doi:10.1097/ACM.0b013e31819397e2
7. Fridner A, Belkic K, Marini M, et al. Survey on recent suicidal ideation among female university hospital physicians in Sweden and Italy (the HOUPE study): cross-sectional associations with work stressors. Gend Med. 2009;6(1):314-328. PubMed doi:10.1016/j.genm.2009.04.006
8. Schernhammer ES, Colditz GA. Suicide rates among physicians: a quantitative and gender assessment (meta-analysis). Am J Psychiatry. 2004;161(12):2295-2302. PubMed doi:10.1176/appi.ajp.161.12.2295
9. Schernhammer E. Taking their own lives: the high rate of physician suicide. N Engl J Med. 2005;352(24):2473-2476. PubMed doi:10.1056/NEJMp058014
10. UC San Diego General Catalog 2009-2010. http://www.ucsd.edu/catalog/index.html. Accessed August 23, 2010.
11. Spitzer RL, Kroenke K, Williams JB. Validation and utility of a self-report version of PRIME-MD: the PHQ primary care study. Primary Care Evaluation of Mental Disorders. Patient Health Questionnaire. JAMA. 1999;282(18):1737-1744. PubMed doi:10.1001/jama.282.18.1737
12. Chen TM, Huang FY, Chang C, et al. Using the PHQ-9 for depression screening and treatment monitoring for Chinese Americans in primary care. Psychiatr Serv. 2006;57(7):976-981. PubMed doi:10.1176/appi.ps.57.7.976
13. Martin A, Rief W, Klaiberg A, et al. Validity of the Brief Patient Health Questionnaire Mood Scale (PHQ-9) in the general population. Gen Hosp Psychiatry. 2006;28(1):71-77. PubMed doi:10.1016/j.genhosppsych.2005.07.003
14. Spitzer RL, Kroenke K, Williams JBW. (PHQ) Patient Health Questionnaire. http://www.phqscreeners.com/overview.aspx. Accessed August 23, 2010.
15. Weissman MM, Bland RC, Canino GJ, et al. Cross-national epidemiology of major depression and bipolar disorder. JAMA. 1996;276(4):293-299. PubMed doi:10.1001/jama.276.4.293
16. Tjia J, Givens JL, Shea JA. Factors associated with undertreatment of medical student depression. J Am Coll Health. 2005;53(5):219-224. PubMed doi:10.3200/JACH.53.5.219-224
17. Yoon J, Lau AS. Maladaptive perfectionism and depressive symptoms among Asian American college students: contributions of interdependence and parental relations. Cultur Divers Ethnic Minor Psychol. 2008;14(2):92-101. PubMed doi:10.1037/1099-9809.14.2.92
18. Taylor SE, Sherman DK, Kim HS, et al. Culture and social support: who seeks it and why? J Pers Soc Psychol. 2004;87(3):354-362. PubMed doi:10.1037/0022-3514.87.3.354
19. Young CB, Fang DZ, Zisook S. Depression in Asian-American and Caucasian undergraduate students. J Affect Disord. 2010;125(1-3):379-382. doi:10.1016/j.jad.2010.02.124 PubMed