Depression, Quality of Life, Work Productivity, Resource Use, and Costs Among Women Experiencing Menopause and Hot Flashes: A Cross-Sectional Study

ABSTRACT
Objective: To examine the effect of depression on health-related quality of life, work productivity, resource use, and costs among women experiencing menopausal symptoms, including hot flashes.
Method: The study included data from the 2005 US National Health and Wellness Survey (N = 41,184), a cross-sectional, Internet-based survey representative of the adult US population. Among women who reported experiencing menopausal symptoms, including hot flashes, women who reported experiencing depression in the last year (n = 1,165) were compared with women who did not report experiencing depression in the last year (n = 2,467), controlling for demographic and health characteristics. Outcome measures included health-related quality of life (Medical Outcomes Study 8-item Short-Form Health Survey [SF-8]), work productivity within the past 7 days, self-reported health care resource use within the past 6 months, and indirect and direct costs.
Results: Women experiencing depression were significantly more likely to be white, to be unemployed, to be uninsured, to currently smoke, to not exercise, and to be obese (all P < .05). After controlling for these differences, women experiencing depression reported significantly lower mental (39.66 vs 50.85, P < .05) and physical (44.05 vs 46.38, P < .05) SF-8 component summary scores. Similarly, the prevalences of time missed from work (5.31% vs 2.80%, P < .05), impairment while at work (25.00% vs 14.32%, P < .05), and impairment of daily activities (37.32% vs 23.16%, P < .05) due to health were greater among women experiencing depression. The numbers of physician visits (2.47 vs 1.77, P < .05), emergency room visits (0.27 vs 0.16, P < .05), and days hospitalized (0.36 vs 0.18, P < .05) in the past 6 months were also higher among women experiencing depression. Per woman per year indirect and direct costs were $3,066 and $1,075 higher, respectively, for women experiencing depression compared with those not experiencing depression.
Conclusion: Approximately one-third of women experiencing menopausal symptoms, including hot flashes, also reported experiencing depression. These women reported significantly worse quality of life and significantly greater work productivity loss, health care resource use, and costs. Given the prevalence and burden, these findings suggest that proper assessment and management of depressive symptoms among women with menopause may have an important humanistic and economic benefit.
Prim Care Companion CNS Disord 2012;14(6):doi:10.4088/PCC.12m01410
© Copyright 2012 Physicians Postgraduate Press. Inc.
Submitted: May 14, 2012; accepted August 2, 2012.
Published online: November 1, 2012.
Corresponding author: Jennifer Whiteley, EdD, Pfizer Inc, 235 East 42nd St, New York, NY 10017 ([email protected]).
Approximately 2 million women in the United States will reach the age of menopause onset each year for the next decade.1 Although menopause is considered a normal aspect of aging, many women experience significant adverse health symptoms during the menopausal transition.2-5 It is estimated that half to three-fourths (or more) of perimenopausal and postmenopausal women experience symptoms associated with the menopausal transition.2-5 These symptoms, which include hot flashes,4,6-8 night sweats,4,6-8 low self-rated health,6 sexual difficulties,4,7 insomnia,4,6-9 anxiety,7,9 and depression,10-13 can last years.1,5 In 1 study, 26% of women reported experiencing hot flashes between 6 and 10 years after menstrual cessation.2 Kronenberg et al14 found that the average duration of hot flashes was 4 years.
Hot flashes, in particular, have been shown to be a bothersome symptom of menopause15 experienced by approximately 75% of women over the age of 50 years.5,6,16 Prior studies have observed a significant association between hot flashes and impaired health-related quality of life.17,18 Women with moderate-to-severe hot flashes can be particularly affected, as they have reported low levels of health-related quality of life (assessed using the Medical Outcomes Study 36-item Short-Form Health Survey [SF-36]) along with increased sleep and sexual difficulties.19
The presence of hot flashes during menopause is often concomitant with the presence of depression.20,21 Among women experiencing moderate or severe depressive symptoms, the odds of reporting recent hot flash or night sweat symptoms were twice as high compared with women without depressive symptoms.12 Conversely, the odds of presenting depressive symptoms were 4 times higher among women with hot flashes or night sweats compared with women without hot flashes or night sweats, an association that persisted even after controlling for history of depression.11 Although depressive symptoms have been associated with decreased physical and social functioning22 and productivity impairment23 among middle-aged women, the combined impact of depression and hot flashes among women has not been previously examined. The objective of the current study was to evaluate the impact of depression on health-related quality of life and productivity and health care resource utilization and costs among women experiencing menopausal symptoms and hot flashes.
METHOD
Sample and Procedure
Participants were selected from the 2005 US National Health and Wellness Survey (NHWS; Consumer Health Sciences, now part of Kantar Health; Princeton, New Jersey; http://www.chsinternational.com/nhws.html). The NHWS is a cross-sectional Internet survey given to a sample of adults (aged 18 years and older) identified through a Web-based consumer panel. Members are recruited to the panel through opt-in e-mails, coregistration with other panels, e-newsletter campaigns, and online banner placements. All panelists explicitly agreed to become panel members, registered through unique e-mail addresses, and completed in-depth demographic registration profiles. Although the NHWS is conducted annually, the 2005 survey was used in the present study, as it was the most recent survey that assessed menopausal symptoms.
A stratified random sampling procedure was implemented (with strata based on gender, age, and race/ethnicity) to ensure that respondents to the NHWS were representative of the US adult population. As a result, the relative proportion of invitations across gender, age, and race/ethnicity groups to complete the NHWS was identical to that of the US Census. Comparisons between NHWS and the US Census are described in detail elsewhere.24 The study was approved by the Essex Institutional Review Board (Lebanon, New Jersey; http://www.essexirb.com/).

- The presence of hot flashes during menopause is often concomitant with the presence of depression.
- For women experiencing menopausal symptoms, depression is associated with worse quality of life and greater work productivity loss, health care resource use, and costs.
- Clinicians’ proper assessment and management of depressive symptoms may have an important humanistic and economic benefit.
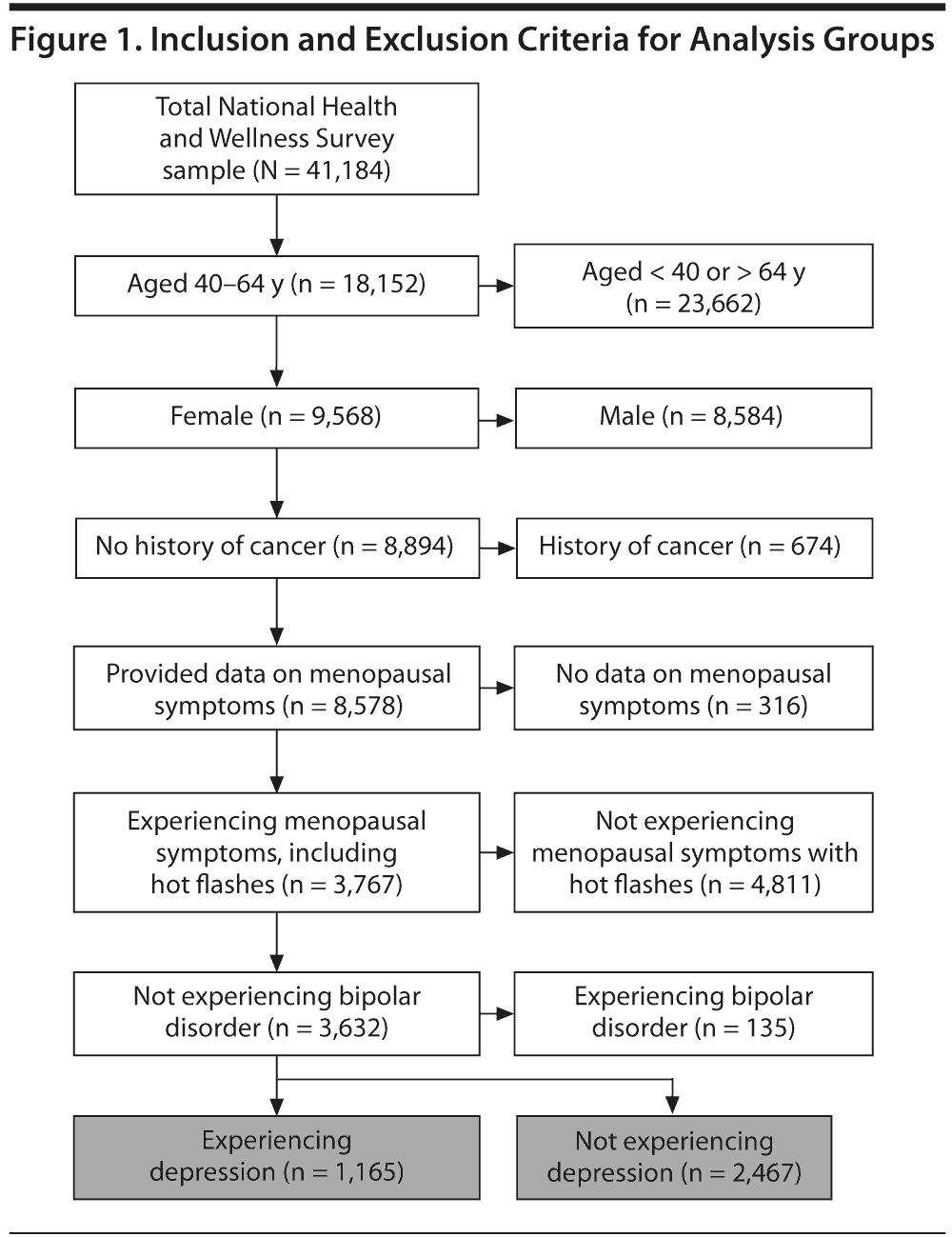
A total of 229,000 members of the Web-based panel were invited to participate in the 2005 NHWS; 65,588 (28.6%) responded to the invitation. Of those respondents, 41,184 (62.8%) were aged 18 years or older, provided informed consent, and completed the survey instrument. The present study included female respondents between 40 and 64 (inclusive) years of age from the NHWS sample who reported experiencing menopause symptoms and hot flashes, did not have a history of cancer, and did not have bipolar disorder. Figure 1 provides inclusion/exclusion criteria. A total of 3,632 women met these criteria and were included in the analyses. Women who reported experiencing depression in the past 12 months were compared with women who did not report experiencing depression in the past 12 months.
Measures
Depression. All women were asked whether or not they had experienced depression in the last 12 months (yes vs no).
Sociodemographics. All participants provided sociodemographic data. The following information was obtained: age (40-44 years, 45-49 years, 50-54 years, 55-59 years, or 60-64 years), race/ethnicity (non-Hispanic white, non-Hispanic black, Hispanic, Asian, and other), marital status (married vs all else), education (high school degree or less vs some college or more), annual household income (< $25,000, $25,000 to < $50,000, $50,000 to < $75,000, ≥ $75,000, or decline to answer), employment status (full-time employed, part-time employed, self-employed, or unemployed), and possession of health insurance (yes vs no).
Health risk behaviors. All participants provided data on their exercise behavior (exercised for 20 minutes at a time or more at least once in the last month vs not), smoking behavior (currently smoke vs do not currently smoke), alcohol consumption (currently drink vs do not currently drink), and height and weight. Height and weight (if provided) were used to calculate body mass index and to categorize women into the following categories: underweight, normal, overweight, obese, or decline to answer.
Health-related quality of life. Health-related quality of life was assessed using the Medical Outcomes Study 8-item Short-Form Health Survey (SF-8), an 8-item generic instrument of health status.25 The SF-8 is an abbreviated version of the SF-36 and assesses the same 8 health domains. The current study examined the physical component summary and mental component summary scores. These scores range from 0 to 100, with higher scores indicating better health status, and are standardized to the US population (a mean of 50 and a standard deviation of 10).
Work productivity loss. Work productivity loss was measured using the Work Productivity and Activity Impairment (WPAI) questionnaire.26 The WPAI scale is a validated instrument used to measure work productivity and impairment in daily activities. The current study used 3 metrics derived from the WPAI instrument: absenteeism (percentage of time missed from work due to health in the past 7 days), presenteeism (percentage of impairment experienced at work due to health in the past 7 days), and activity impairment (percentage of impairment experienced in daily activities in the past 7 days). Only women who were currently employed provided data for absenteeism and presenteeism. All women provided data for activity impairment.
Absenteeism was calculated by dividing the number of work hours a participant missed in the past week because of her health by the total number of hours a participant could have worked (the number of hours they did work plus the number of hours they missed because of their health) and converting this proportion into a percentage; that is, absenteeism = (number of hours missed) ×· (number of hours missed + number of hours worked). Presenteeism was calculated by a participant’s response to her level of impairment experienced while at work in the past 7 days (from 0 to 10), which was then multiplied by 10 to create a percentage. Activity impairment was measured by a participant’s response to her level of impairment experienced in daily activities in the past 7 days (from 0 to 10), which was then multiplied by 10 to create a percentage, with a range from 0% to 100%.
Work productivity loss was converted into indirect costs using a human capital approach. Median weekly income figures were obtained through the US Bureau of Labor Statistics.27 For each respondent, an hourly wage was estimated by dividing the median weekly income by 40, which is the number of hours in a typical US work week. Next, the number of hours missed in the last week because of one’s health (absenteeism) and the number of hours missed in the last week because of health impairment while at work (presenteeism) were each multiplied by the hourly wages to arrive at total lost wages. These figures were then multiplied by 50 (mean number of US work weeks in a year) to obtain annual estimates. The sum of both absenteeism and presenteeism costs was considered total indirect costs.
Health care resource utilization. Health care resource use was defined by the number of traditional health care provider visits (calculating the sum of the following question: “How many times have you seen the following traditional health care providers in the past 6 months?” [eg, general practitioner, internist, etc]), emergency room (ER) visits (“How many times have you been to the ER for your own medical condition in the past 6 months?”), and the number of days hospitalized (“What is the total number of days you were hospitalized for your own medical condition in the past 6 months?”).
Health care resource utilization was converted into direct costs by doubling the number of provider visits, ER visits, and hospitalizations in the 6-month recall period to create an estimate of annual health care resource utilization and by assigning costs according to the mean cost for each type of service. Service costs were obtained from the Medical Expenditure Panel Survey database.28-30 These costs represent all direct payments by individuals, insurers, and miscellaneous public sources to health care providers. The sum of provider visits, ER visits, and hospitalization costs was considered total direct costs.
Statistical Analyses
The sociodemographic and health risk behavior characteristics defined above were compared between the groups of women with and without depression using χ2 tests, as all variables were categorical. Multiple regression analyses and generalized linear models were conducted to examine differences between the 2 groups on health-related quality of life, work productivity loss, and health care resource utilization variables, accounting for potential confounding variables. Covariates included age, ethnicity, marital status, education, annual household income, employment status, health insurance possession, exercise behavior, smoking behavior, alcohol consumption, and body mass index.
In the analyses that controlled for potential confounders, multiple regression analyses were used for the health-related quality of life outcomes because the distribution of both mental component summary scores and physical component summary scores approximated normality. Adjusted means are provided for both analysis groups on these outcomes. Generalized linear models were used for health care resource utilization and work productivity loss variables because the distributions of these variables were highly skewed. A negative binomial distribution and a log-link function were specified. For the generalized linear models, the log of the dependent variable is modeled and, as such, adjusted means were originally provided in log values. These means were converted to the original metric by taking the antilog; the converted adjusted means are presented here for greater interpretability. All analyses were conducted in SAS version 9.1 (SAS Institute, Inc; Cary, North Carolina). The a priori cutoff for statistical significance was set as P < .05.
RESULTS
Sample Characteristics and Baseline Comparison
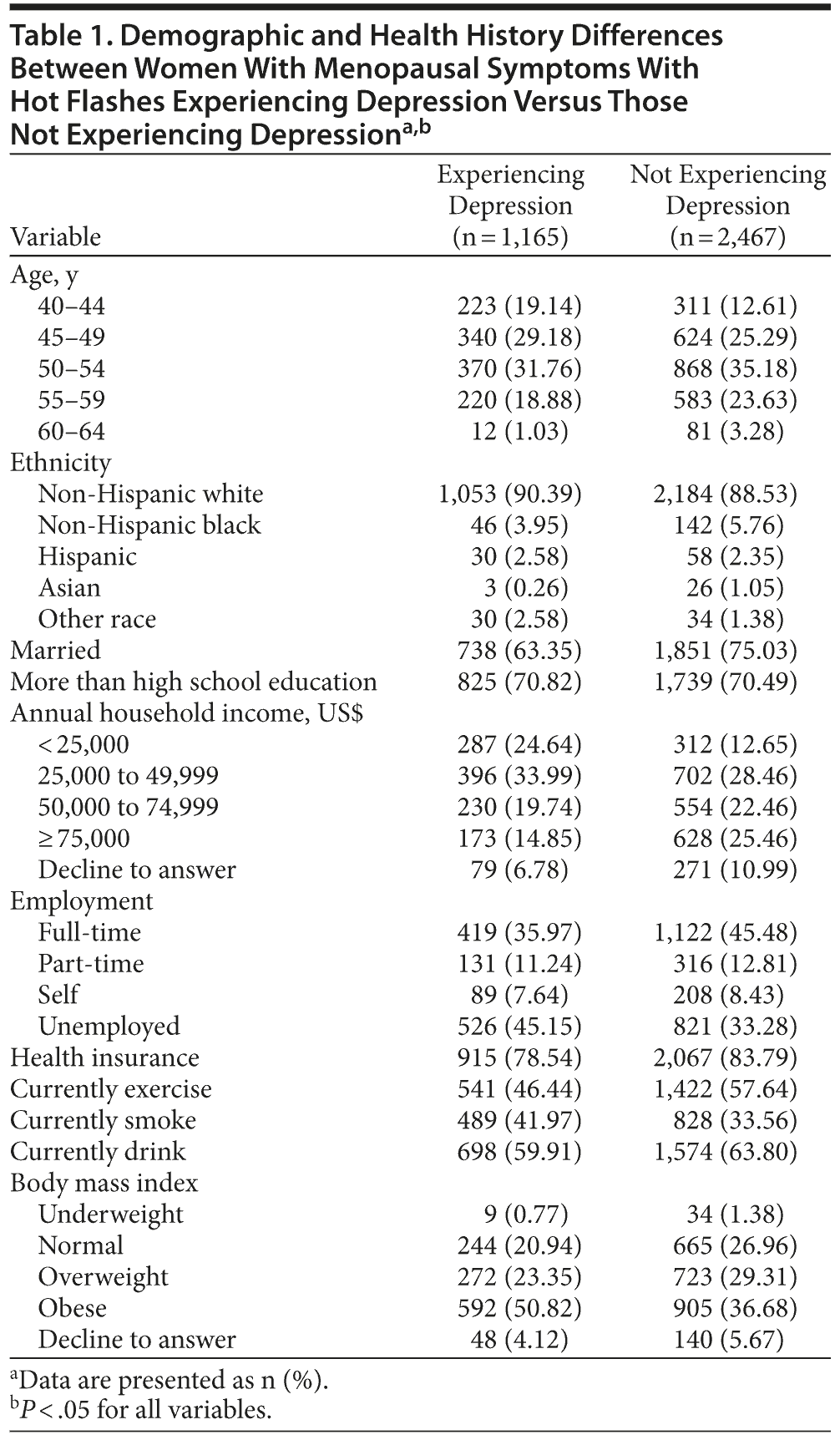
Among women who reported currently experiencing menopausal symptoms with hot flashes, 32.1% (n = 1,165) reported experiencing depression and 67.9% (n = 2,467) did not report experiencing depression. Several sociodemographic and health history differences were observed between these groups. Specifically, women experiencing depression were significantly more likely to be aged 40-44 years and 45-49 years than women not experiencing depression (P < .05) (Table 1). Women experiencing depression were also significantly more likely to be white, to be unmarried, to have annual household incomes below $50,000, to be unemployed, to be uninsured, to currently smoke, to not exercise, and to be obese (P < .05 for all).
Adjusted Health-Related Quality of Life, Work Productivity, and Resource Use
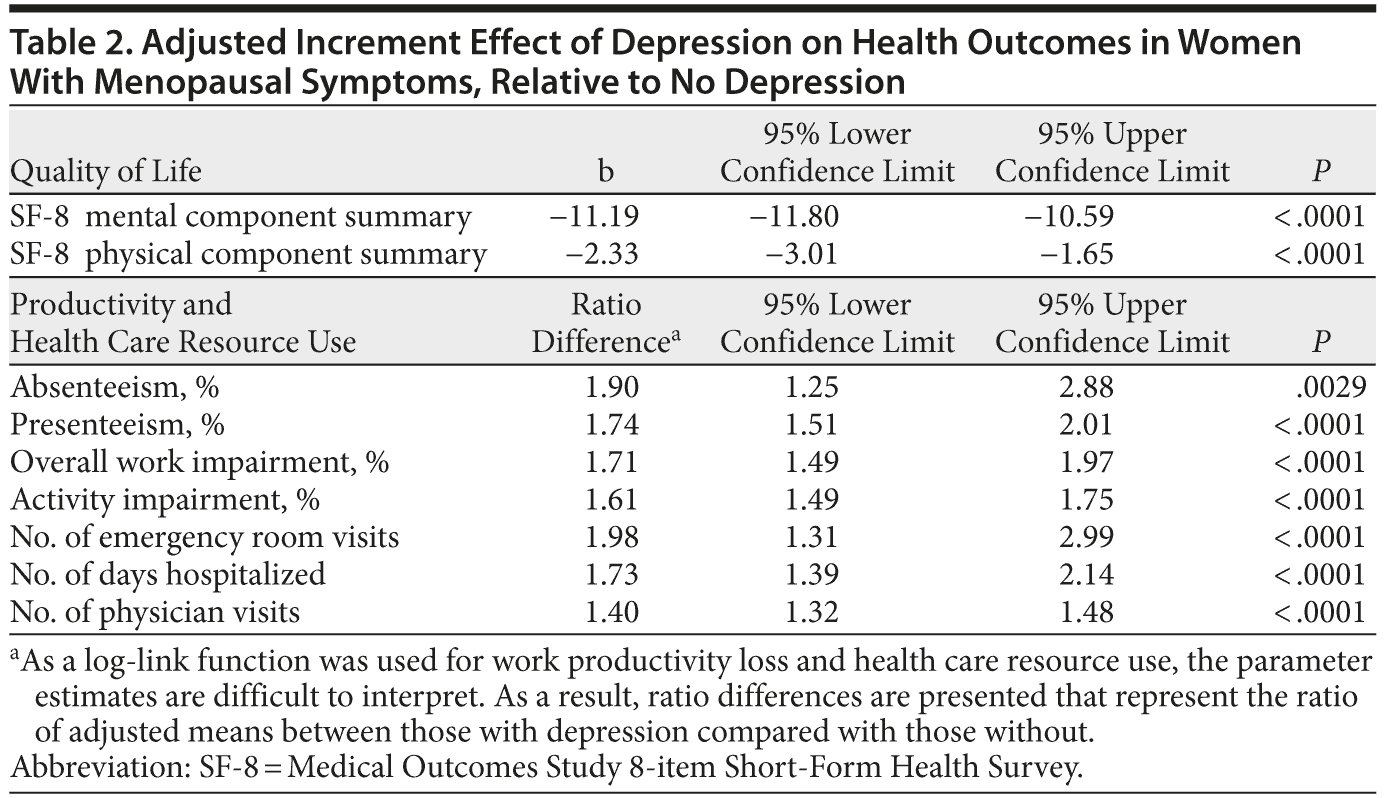
After controlling for sociodemographic and health risk behavior differences, women with depression reported significantly worse health outcomes than women without depression (Table 2). Specifically, lower levels of both mental and physical health-related quality of life were observed among women experiencing menopausal symptoms and experiencing depression (mental component summary: adjusted mean = 39.66 vs 50.85, P < .05; physical component summary: adjusted mean = 44.05 vs 46.38, P < .05). The effect of concomitant menopausal symptoms and depression was also observed on work productivity loss. Women with depression reported significantly greater levels of absenteeism (adjusted mean = 5.31% vs 2.80%, P < .05), presenteeism (adjusted mean = 25.00% vs 14.32%, P < .05), and activity impairment (adjusted mean = 37.32% vs 23.16%, P < .05) than women without depression. The numbers of physician visits (adjusted mean = 2.47 vs 1.77, P < .05), ER visits (adjusted mean = 0.27 vs 0.16, P < .05), and days hospitalized (adjusted mean = 0.36 vs 0.18, P < .05) were also higher among women with depression compared with those without.
Indirect and Direct Costs
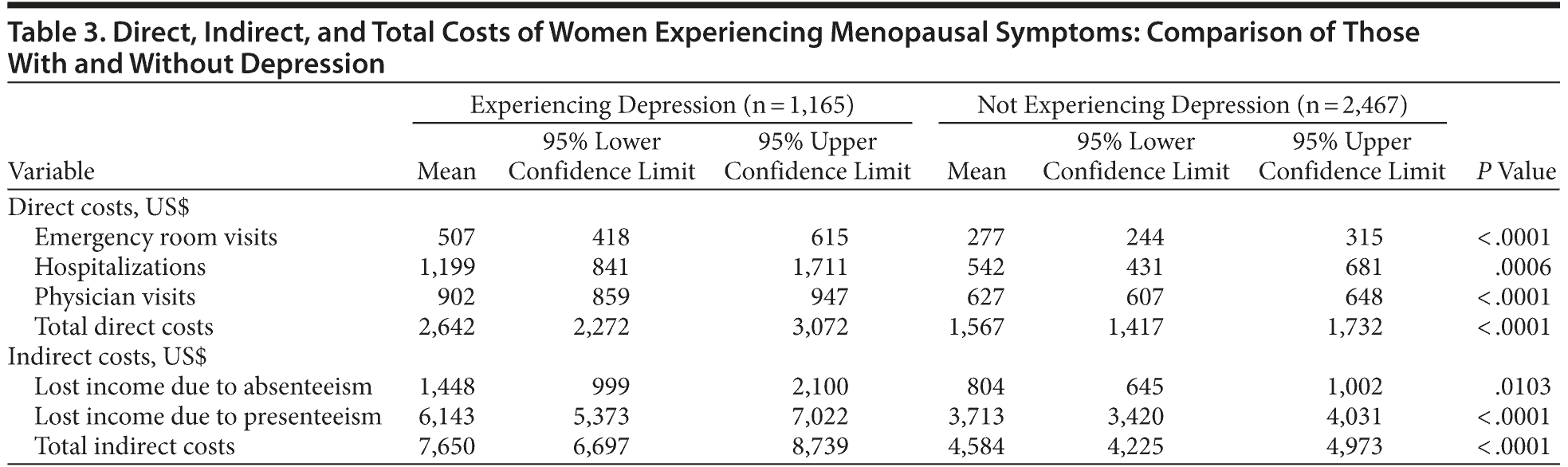
As expected, given the significant differences between the groups on work productivity loss and resource use, all measures of indirect and direct costs were significantly higher among women experiencing depression (Table 3). The majority of indirect total costs were due to productivity losses, particularly presenteeism, and resulted in $7,650 per employed woman per year for those with depression and $4,584 per employed woman per year for those without depression (P < .0001). Direct costs, which were based on provider visits, ER visits, and hospitalizations, were $2,642 per woman per year for those with depression and $1,567 per woman per year for those without depression (P < .0001).
DISCUSSION
The objective of the current study was to evaluate the impact of depression on health-related quality of life, productivity, and health care resource utilization and costs among women experiencing menopausal symptoms and hot flashes. Although studies have examined the burden of hot flashes17,18 and the burden of depression,22,23 no study has examined the combined impact of depression and hot flashes among menopausal women. Our results suggest a significant burden, both humanistic and economic, for women with concomitant depression and menopause symptoms with hot flashes. As suggested by prior research,11,12 a notable number of women reported experiencing depression. On the basis of the current study, 32% of women currently experiencing menopause symptoms with hot flashes also report suffering from depression.
Although previous studies have observed a significant quality of life burden among women experiencing menopausal symptoms and hot flashes across a variety of health domains,17 our results suggest that the presence of depression may be, at least partially, responsible for these effects. Indeed, mental component summary scores for women without depression were slightly above population norms suggesting that, without comorbid depression, menopause and hot flashes may not have a sizeable impact on mental quality of life. However, both groups were below population norms for physical component summary scores, though scores were significantly lower among women with comorbid depression.
The productivity results also highlight a tremendous burden experienced by women with both menopause symptoms with hot flashes and depression who are still currently employed. Comparisons with prior research are difficult, as studies examining the impact of hot flashes/vasomotor symptoms or depression among women have not used the WPAI instrument. Studies have shown a significant impact for women with depression in the workforce19; however, our results suggest that the combined effect of both hot flashes and depression among women with menopause symptoms can result in approximately twice the level of impairment, even after accounting for an array of confounding variables. When monetized, an additional $3,000 per woman per year could be attributed to depression among women experiencing menopause with hot flashes.
It should also be noted that the presence of depression could result in reduced labor force participation itself, as women with depression were 12% more likely to be out of the workforce than women without depression. In other words, the presence of the depression could have resulted in the inability or unwillingness to seek employment. Although beyond the scope of the current set of analyses, future economic studies should consider the inclusion of labor force participation, as this may be a substantial source of indirect costs from a societal perspective.
The resource use and direct costs comparisons were also significantly higher among women with depression when compared with women without depression. Although ER visits and hospitalizations were uncommon overall, women with depression reported approximately twice the number of these events, which resulted in significantly more direct costs.
In sum, a tremendous societal burden was observed for women experiencing menopause with hot flashes and depression. Although prior studies have highlighted a burden of menopause symptoms, and hot flashes in particular, our results suggest that comorbid depression may be partially responsible for these previously reported effects. The strongest relationships were observed on work productivity and indirect costs, emphasizing the need for these conditions to be addressed by employers. However, quality of life and health care resource use were also significantly affected. Physicians should be aware of the high prevalence of depression among women with menopause and hot flashes and the impact that these conditions can have. Improved management of depression among these women may have a tremendous benefit, from both quality of life and economic perspectives.
Limitations
The self-reported nature of NHWS could have introduced additional measurement error. The measure of depression was only self-reported depression in the past year, and it is unclear how the results would differ if the analyses focused just on those women whose depression has been diagnosed. Because the study was cross-sectional, causal relationships between depression and health outcomes cannot be inferred. These relationships may be explained by unmeasured confounding variables. Indeed, the analyses were limited by the information available in the NHWS and the manner in which it was collected. More detailed assessment of our covariates (eg, smoking history, alcohol use, exercise behavior, etc) may have influenced the size of the observed effects. The cost figures were estimated from available multipliers and may vary from actual costs. Indirect cost estimates in particular did not account for education level (only age) and, therefore, may underestimate the total direct costs associated with depression among women with hot flashes. It is possible that the sample from the current study differs meaningfully from the population of women experiencing menopause with hot flashes. These differences might influence the extent to which the results can be generalized.
Author affiliations: Health Sciences Practice, Kantar Health, New York, New York (Dr DiBonaventura and Mr Wagner); and Pfizer Inc, New York, New York (Drs Alvir and Whiteley).
Potential conflicts of interest: Dr Whiteley is an employee of and Dr Alvir is an employee of and stock shareholder in Pfizer. Dr DiBonaventura and Mr Wagner are employees of Kantar Health Inc, who were paid consultants to Pfizer in connection with the study and the development of this manuscript.
Funding/support: This study was sponsored by Pfizer Inc.
REFERENCES
1. Burdette L, Moore A, Speroff L, et al. Hormone therapy in menopause: applying research findings to optimal patient care and education. Women’s Health Care (Don Mills). 2009;8(5):10-21.
2. Feldman BM, Voda A, Gronseth E. The prevalence of hot flash and associated variables among perimenopausal women. Res Nurs Health. 1985;8(3):261-268. PubMed doi:10.1002/nur.4770080308
3. Freeman EW, Sammel MD, Lin H, et al. The role of anxiety and hormonal changes in menopausal hot flashes. Menopause. 2005;12(3):258-266. PubMed doi:10.1097/01.GME.0000142440.49698.B7
4. NIH State-of-the-Science Conference Statement on Management of Menopause-Related Symptoms. NIH Consens State Sci Statements. 2005;22(1):1-38. PubMed
5. Utian WH. Psychosocial and socioeconomic burden of vasomotor symptoms in menopause: a comprehensive review. Health Qual Life Outcomes. 2005;3(1):47. PubMed doi:10.1186/1477-7525-3-47
6. Berecki-Gisolf J, Begum N, Dobson AJ. Symptoms reported by women in midlife: menopausal transition or aging? Menopause. 2009;16(5):1021-1029. PubMed doi:10.1097/gme.0b013e3181a8c49f
7. Kuh DL, Wadsworth M, Hardy R. Women’s health in midlife: the influence of the menopause, social factors and health in earlier life. Br J Obstet Gynaecol. 1997;104(8):923-933. PubMed doi:10.1111/j.1471-0528.1997.tb14352.x
8. Keenan NL, Mark S, Fugh-Berman A, et al. Severity of menopausal symptoms and use of both conventional and complementary/alternative therapies. Menopause. 2003;10(6):507-515. PubMed doi:10.1097/01.GME.0000064865.58809.3E
9. Baker A, Simpson S, Dawson D. Sleep disruption and mood changes associated with menopause. J Psychosom Res. 1997;43(4):359-369. PubMed doi:10.1016/S0022-3999(97)00126-8
10. Cohen LS, Soares CN, Vitonis AF, et al. Risk for new onset of depression during the menopausal transition: the Harvard Study of Moods and Cycles. Arch Gen Psychiatry. 2006;63(4):385-390. PubMed doi:10.1001/archpsyc.63.4.385
11. Freeman EW, Sammel MD, Lin H, et al. Associations of hormones and menopausal status with depressed mood in women with no history of depression. Arch Gen Psychiatry. 2006;63(4):375-382. PubMed doi:10.1001/archpsyc.63.4.375
12. Joffe H, Hall JE, Soares CN, et al. Vasomotor symptoms are associated with depression in perimenopausal women seeking primary care. Menopause. 2002;9(6):392-398. PubMed doi:10.1097/00042192-200211000-00003
13. Reed SD, Ludman EJ, Newton KM, et al. Depressive symptoms and menopausal burden in the midlife. Maturitas. 2009;62(3):306-310. PubMed doi:10.1016/j.maturitas.2009.01.002
14. Kronenberg F, Cote LJ, Linkie DM, et al. Menopausal hot flashes: thermoregulatory, cardiovascular, and circulating catecholamine and LH changes. Maturitas. 1984;6(1):31-43. PubMed doi:10.1016/0378-5122(84)90063-X
15. Avis NE, Crawford SL, McKinlay SM. Psychosocial, behavioral, and health factors related to menopause symptomatology. Womens Health. 1997;3(2):103-120. PubMed
16. Thurston RC, Bromberger JT, Joffe H, et al. Beyond frequency: who is most bothered by vasomotor symptoms? Menopause. 2008;15(5):841-847. PubMed doi:10.1097/gme.0b013e318168f09b
17. Avis NE, Ory M, Matthews KA, et al. Health-related quality of life in a multiethnic sample of middle-aged women: Study of Women’s Health Across the Nation (SWAN). Med Care. 2003;41(11):1262-1276. PubMed doi:10.1097/01.MLR.0000093479.39115.AF
18. Avis NE, Colvin A, Bromberger JT, et al. Change in health-related quality of life over the menopausal transition in a multiethnic cohort of middle-aged women: Study of Women’s Health Across the Nation. Menopause. 2009;16(5):860-869. PubMed doi:10.1097/gme.0b013e3181a3cdaf
19. Bobula JD. Vasomotor symptoms and quality of life (QoL) in postmenopausal women. Value Health. 2003;6(6):707. doi:10.1016/S1098-3015(10)61803-7
20. Brown JP, Gallicchio L, Flaws JA, et al. Relations among menopausal symptoms, sleep disturbance and depressive symptoms in midlife. Maturitas. 2009;62(2):184-189. PubMed doi:10.1016/j.maturitas.2008.11.019
21. Freeman EW. Associations of depression with the transition to menopause. Menopause. 2010;17(4):823-827. PubMed doi:10.1097/gme.0b013e3181db9f8b
22. Bromberger JT, di Scalea TL. Longitudinal associations between depression and functioning in midlife women. Maturitas. 2009;64(3):145-159. PubMed doi:10.1016/j.maturitas.2009.09.017
23. Wollersheim JP. Depression, women, and the workplace. Occup Med. 1993;8(4):787-795. PubMed
24. DiBonaventura MD, Wagner JS, Yuan Y, et al. Humanistic and economic impacts of hepatitis C infection in the United States. J Media Econ. 2010;13(4):709-718. PubMed doi:10.3111/13696998.2010.535576
25. Ware JE, Kosinksi M, Dewey JE, et al. How to Score and Interpret Single-Item Health Status Measures: A Manual for Users of the SF-8 Health Survey. Lincoln, RI: QualityMetric Incorporated; 2001.
26. Reilly MC, Zbrozek AS, Dukes EM. The validity and reproducibility of a work productivity and activity impairment instrument. Pharmacoeconomics. 1993;4(5):353-365. PubMed doi:10.2165/00019053-199304050-00006
27. US Department of Labor. Highlight of Women’s Earnings in 2005. Washington, DC: US Bureau of Labor Statistics; 2006
28. Machlin SR, Carper K. Expenses for Office-Based Physician Visits by Specialty, 2004. Rockville, MD: Agency for Healthcare Research and Quality; 2007.
29. Machlin SR. Expenses for a Hospital Emergency Room Visit, 2004. Rockville, MD: Agency for Healthcare Research and Quality; 2006.
30. Merrill CT, Elixhauser A. Hospitalization in the United States, 2002. HCUP Fact Book No. 6. AHRQ Publication No. 05-0056. Rockville, MD. Agency for Healthcare Research and Quality; 2005