Objective: To explore brain wave changes associated with cranial electrotherapy stimulation (CES) among subjects receiving psychiatric care.
Methods: Quantitative electroencephalogram data were obtained before and after a 20-minute session of CES. The investigators recruited active-duty military subjects from Walter Reed National Military Medical Center’s Psychiatry Continuity Service, Bethesda, Maryland. Fifty subjects participated in this prospective, convenience sample study from August 2016 through March 2017. The main outcome measures were changes in brain wave activity and the Subjective Units of Distress Scale.
Results: The typical subject was mildly depressed and had severe trauma-related symptoms and sleep problems. There was a significant increase (P = .000) in the higher beta frequencies (18-21 Hz, 21-33 Hz, and 33-48 Hz) and a strong effect (with the Cohen d around 1.5) immediately following the 20-minute CES. Ten minutes after CES, slower wave activity (4-8 Hz and 8-12 Hz) significantly decreased (P < .05), while higher beta wave activity (13-15 Hz, 18-21 Hz, and 21-33 Hz) increased. A strong effect (with the Cohen d around 1.5) persisted in the beta brain wave bands 18-21 Hz and 21-33 Hz.
Conclusions: Brain wave measurements taken immediately after the 20-minute CES session showed a significant and strong effect in the beta region, suggesting an increase in mental alertness, focus, and concentration. Ten minutes after the CES session, an even more marked change in brain wave activity occurred. The significant and strong effect in the beta region persisted but was joined by a reduction in slower wave activity, indicating an increase in mental alertness.
Trial Registration: ClinicalTrials.gov identifier NCT03298308
Prospective Study of Brain Wave Changes Associated With Cranial Electrotherapy Stimulation

ABSTRACT
Objective: To explore brain wave changes associated with cranial electrotherapy stimulation (CES) among subjects receiving psychiatric care.
Methods: Quantitative electroencephalogram data were obtained before and after a 20-minute session of CES. The investigators recruited active-duty military subjects from Walter Reed National Military Medical Center’s Psychiatry Continuity Service, Bethesda, Maryland. Fifty subjects participated in this prospective, convenience sample study from August 2016 through March 2017. The main outcome measures were changes in brain wave activity and the Subjective Units of Distress Scale.
Results: The typical subject was mildly depressed and had severe trauma-related symptoms and sleep problems. There was a significant increase (P = .000) in the higher beta frequencies (18-21 Hz, 21-33 Hz, and 33-48 Hz) and a strong effect (with the Cohen d around 1.5) immediately following the 20-minute CES. Ten minutes after CES, slower wave activity (4-8 Hz and 8-12 Hz) significantly decreased (P < .05), while higher beta wave activity (13-15 Hz, 18-21 Hz, and 21-33 Hz) increased. A strong effect (with the Cohen d around 1.5) persisted in the beta brain wave bands 18-21 Hz and 21-33 Hz.
Conclusions: Brain wave measurements taken immediately after the 20-minute CES session showed a significant and strong effect in the beta region, suggesting an increase in mental alertness, focus, and concentration. Ten minutes after the CES session, an even more marked change in brain wave activity occurred. The significant and strong effect in the beta region persisted but was joined by a reduction in slower wave activity, indicating an increase in mental alertness.
Trial Registration: ClinicalTrials.gov identifier NCT03298308
Prim Care Companion CNS Disord 2018;20(1):17m02214
To cite: Lande RG, Gragnani CT. Prospective study of brain wave changes associated with cranial electrotherapy stimulation. Prim Care Companion CNS Disord. 2018;20(1):17m02214.
To share: https://doi.org/10.4088/PCC.17m02214
© Copyright 2018 Physicians Postgraduate Press, Inc.
aPsychiatry Continuity Service, Behavioral Health Directorate, Walter Reed National Military Medical Center, Bethesda, Maryland
*Corresponding author: R. Gregory Lande, DO, Psychiatry Continuity Service, Behavioral Health Directorate, Walter Reed National Military Medical Center, 8901 Rockville Pike, Bethesda, MD 20889 ([email protected]).
Cranial electrotherapy stimulation (CES) is a noninvasive intervention marketed by manufacturers for the treatment of pain, insomnia, and emotional disorders such as depression and anxiety. Devices differ in terms of such fundamental variables as electrode placement, frequency ranges, and stimulation patterns, all of which compound the difficulties researchers confront when investigating the efficacy of CES. Despite these obstacles, investigators continue efforts to examine the efficacy and putative mechanism of actions for CES as a nonpharmacologic treatment.1
As a potential therapeutic modality, CES relies in part on a long history of clinicians using both electricity and magnets for various medical treatments. Modern examples include electroconvulsive therapy, transcranial magnetic stimulation, and deep-brain stimulation, all of which are best reserved for individuals with treatment-resistant depression and other severe, chronic psychiatric disorders.2-4 Efficacy aside, these treatments have significant limitations in terms of cost, training, and side effects, which are major obstacles to widespread availability.5
CES is microcurrent therapy: a less intensive version of transcranial electrical stimulation, requiring less training and exposing the recipient to fewer side effects. Modern CES can trace its development to the 1970s when early efforts to standardize the procedure resulted in 2 earlobe-attached electrodes, the delivery of microamperage, and a 20-minute treatment duration. The combination of electrodes and their placement, amount of microamperage, waveform characteristics, duration of exposure, and type of stimulation together constitute the definition of a CES dose. In 1979, the US Food and Drug Administration recognized CES as class III devices for the treatment of anxiety, depression, and insomnia. Since that time, manufacturers have brought new devices to the commercial market with different dosing criteria.6
Dosing parameters are critical variables in determining the potential value of CES. Perhaps the most fundamental issue is whether ear electrode placement and pulsed microcurrent stimulation actually penetrate the skull and reach deeper-lying brain regions; a question affirmatively answered through a computer-based modeling study.7
A review8 of published literature cited improvement in anxiety, depression, and insomnia as the result of microcurrent-induced changes in the neurophysiology of the brain. Researchers reported the effectiveness of CES for anxiety, depression, and insomnia through randomized, double-blind, sham-controlled designs.9-11
Aside from possible changes in CES-induced neurotransmitter levels, another line of inquiry explored by investigators and the subject of this research involves variations in brain wave activity as a consequence of the microcurrents. Among presumably healthy volunteers, a 20-minute session of CES resulted in an increase in alpha wave activity and decreased delta and theta waves with subjective reports of mental clarity.12 In another small study13 of healthy individuals, investigators reported a decrease in the alpha brain wave’s median frequency and the beta brain wave’s power band.
In this study, we examined brain wave changes associated with CES among subjects receiving psychiatric care. We hypothesized that CES would decrease subjective reports of anxiety by increasing alpha wave activity or paradoxically be interpreted as anxiolytic by an increase in beta wave activity, favorably improving concentration, focus, and mental acuity. Walter Reed National Military Medical Center’s Institutional Review Board approved this prospective study. Trial registration information is available from ClinicalTrials.gov (identifier NCT03298308).

- Cranial electrotherapy stimulation (CES) is easily administered in the typical office or hospital setting.
- CES is a nonpharmacologic treatment alternative—an option to consider when other approaches have not achieved optimum results.
- On the basis of the study findings, CES may improve concentration and reduce distractibility.
METHODS
This study was conducted from August 2016 through March 2017 among active-duty service members receiving treatment at the Psychiatry Continuity Service, Walter Reed National Military Medical Center in Bethesda, Maryland. The Psychiatry Continuity Service is an outpatient partial hospital program staffed by a group of multidisciplinary clinicians and provides intensive care for all psychiatric disorders requiring this level of treatment.14
Subjects supplied quantitative electroencephalogram (qEEG) data using the NeuroSky MindSet (San Jose, California), a wireless single-channel dry electrode device processing research-grade electrical activity from the Fp1 (frontal scalp, position 1 location).15 NeuroSky’s ThinkGear ASIC Module processes the brain’s electrical activity and reports EEG values and signal quality.16,17 Its qEEG data acquisition offers convenience, reliability, and reproducibility.18
The investigators analyzed the qEEG data using the SmartMind Research Kit (BrainTrain, North Chesterfield, Virginia), which incorporates software bandpass filters and minimizes artifacts from eye and muscle movement. SmartMind reports the mean and standard deviation in microvolts for each sampled brain wave frequency for a user-defined period of time.19,20
Subjects received CES from the Alpha-Stim AID (Electromedical Products International, Mineral Wells, Texas). Through ear clip electrodes, the Alpha-Stim AID delivers 0-500 microamperes adjustable in 50-microampere increments at a frequency of 0.5 Hz (pulses per second) combined with a constant 0.4 Hz, producing a mean pulse repetition frequency rate of 0.8 Hz, with bipolar asymmetric rectangular waves at a 50% duty cycle repeating periodically at 10-second intervals.21
Subjects received an orientation on use of the equipment after providing written consent. The subjects placed the qEEG device on their head with their eyes open and their head resting against a wall in a quiet room for the duration of the experiment. An investigator assured proper positioning of the CES ear clips and then adjusted the microamperage to the point of mild subjective discomfort, then reduced the microamperage to eliminate that sensation, which replicates the process performed in clinical practice. Subjects received CES for 20 minutes. We recorded 30-second measurements of brain wave activity at baseline immediately preceding CES, immediately after the 20-minute CES, and 10 minutes after CES.
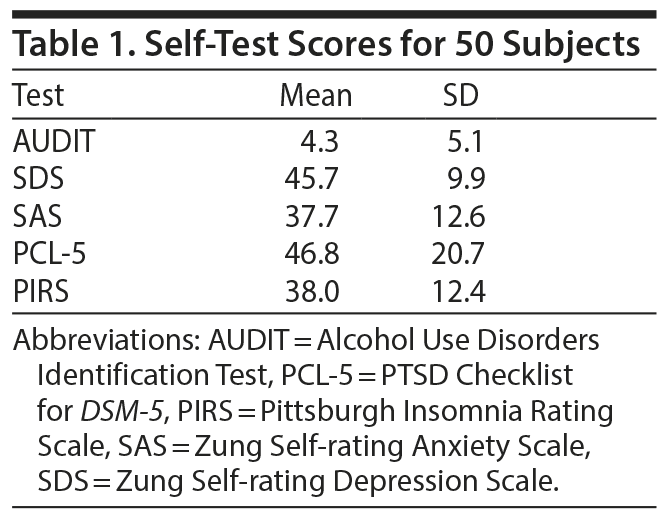
In addition to the brain wave measurements, just before and after CES, study participants completed the Subjective Units of Distress Scale.22 Baseline self-assessment instruments included the Alcohol Use Disorders Identification Test (AUDIT),23 PTSD Checklist for DSM-5 (PCL-5),24 Pittsburgh Insomnia Rating Scale (PIRS),25 Zung Self-rating Anxiety Scale (SAS),26 and Zung Self-rating Depression Scale (SDS).27 For purposes of screening clinical conditions, the following thresholds apply: AUDIT ≥ 8, PCL-5 ≥ 33, PIRS ≥ 21, SAS ≥ 45, and SDS ≥ 45.
Data were studied through correlations, independent samples t test, paired samples t test, frequencies, and descriptive analyses using SPSS version 22.
RESULTS
Fifty subjects participated in this study; most were male (n = 34/50, 68%), enlisted service members (n = 39/50, 78%) between the ages of 21 and 40 years (n = 37/50, 74%). The typical subject was mildly depressed and had severe trauma-related symptoms and sleep problems (Table 1).
There was a significant difference in the subjective units of distress before CES (n = 50, mean = 4.12, SD = 2.12) and after CES (n = 50, mean = 3.26, SD = 2.19, P = .000, Cohen d = 0.4). Microamperage during CES ranged between 0.5 and 5.0 (n = 50, mean = 3.28, SD = 0.98).
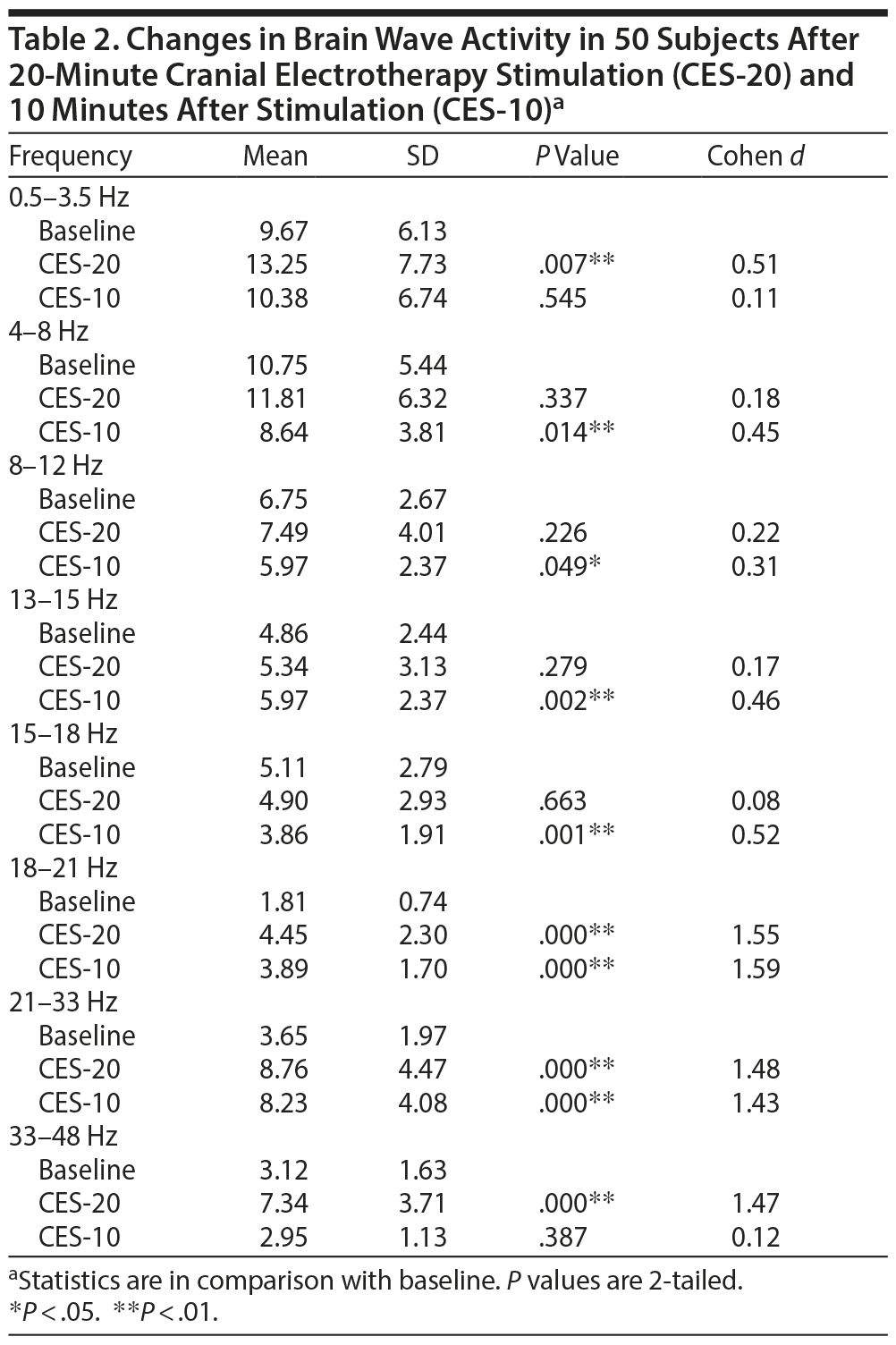
In terms of brain wave changes, there was a significant increase (P = .000) in the higher beta frequencies (18-21 Hz, 21-33 Hz, and 33-48 Hz) and a strong effect (with the Cohen d around 1.5) immediately following the 20-minute CES (Table 2).
Ten minutes after CES, slower wave activity (4-8 Hz and 8-12 Hz) significantly decreased, while higher beta wave activity (13-15 Hz, 18-21 Hz, and 21-33 Hz) increased. A strong effect (with the Cohen d around 1.5) persisted in the beta brain wave bands 18-21 Hz and 21-33 Hz (Table 2).
There was a direct correlation between the amount of microamperage delivered and brain wave activity between 13-15 Hz (n = 50, r = 0.27, P = .05) and 18-21 Hz (n = 50, r = 0.33, P = .02). Age and sex did not correlate with any brain wave changes.
DISCUSSION
We explored acute brain wave changes associated with CES in a manner specifically designed to reduce external variables that might affect the results. At the same time, subjects received CES with the microamperage adjusted as in clinical practice. In sham-controlled studies,10 the electrical current is not adjusted, leaving the clinical relevance of this approach unanswered. Findings from this study would suggest that variations in the microamperage predominately affect midrange beta waves.
Brain wave activity was grouped into 5 categories on the basis of their respective frequencies: alpha (8-12 Hz), theta (4-8 Hz), beta (13-15 Hz, 15-18 Hz, 18-21 Hz, and 21-33 Hz), delta (0-3.5 Hz), and gamma (33-48 Hz). Alpha waves correlate with a relaxed mental state, theta waves correlate with drowsiness, beta waves correlate with increased attention and cognition, delta waves may occur while awake but are more prominent in deep sleep, and gamma waves correlate with global consciousness and synchronized neuronal activity.28,29 The frequency range of 13-15 Hz is a transition phase with functional elements of both mental tranquility and alertness, which overlaps slightly with the next frequency range.30 The progression from the slow-frequency delta waves to the high-frequency gamma waves represents increasing levels of mental acuity in the broadest and simplest description of functional activity.
Brain wave measurements taken immediately after the 20-minute CES session showed a significant increase and strong effect size in the beta region, suggesting an increase in mental alertness, focus, and concentration.
An even more marked change in brain wave activity occurred 10 minutes after the CES session. The significant increase and strong effect size in the beta region persisted but was joined by a reduction in slower wave activity, indicating an increase in mental alertness.
Participants in this study subjectively reported a significant reduction in distress following the CES session. This finding raises the possibility that the subjective assessment of stress reduction following CES may be related to an increase in beta wave activity. Improved mental focus and a corresponding decrease in distraction may be a welcome relief among individuals with overlapping anxiety, depression, and trauma symptoms as reflected in this study group.
This study was designed to balance the actual clinical use of CES with scientific rigor. As in clinical practice, the micoamperage of CES was tailored for each subject. On the other hand, to minimize distractions we conducted the study in a quiet office, specifically limited all communication, required that the subjects keep their eyes open, and minimized the time span between qEEG measurements in an effort to avoid other confounding variables affecting brain wave activity.
We acknowledge that balancing clinical use and scientific rigor is not perfect. This open-label study exposed the subjects to limited interactions, such as positioning the brain wave-sensing headset, with the investigators. While other factors such as the subjects’ awareness of the stimulation phase of CES may impose a potential bias on the study’s results, it is at least partially mitigated by the number of subjects, the strength of the findings, and the value in determining the role of microamperage dosing.
With these limitations in mind, the findings of this study would benefit from replication with a larger study group among subjects with similar behavioral profiles. Future research could also further explore the anxiolytic effects of increasing beta wave activity among individuals with varying degrees of mental distraction.
Submitted: August 30, 2017; accepted October 12, 2017.
Published online: January 18, 2018.
Potential conflicts of interest: None.
Funding/support: None.
Disclaimer: The views expressed in this presentation are those of the authors and do not reflect the official policy of the Department of the Army/Navy/Air Force or the Department of Defense. The identification of specific products or scientific instrumentation does not constitute an endorsement or implied endorsement on the part of the authors, Department of Defense, or any component agency. While we generally excise references to products, companies, manufacturers, and organizations in government-produced works, the abstracts produced and other similarly situated researchers present a special circumstance when such product inclusions become an integral part of the scientific endeavor.
REFERENCES
1. Mindes J, Dubin MJ, Altemus M. Cranial Electrical Stimulation. In: Knotkova H, Rasche D, eds. Textbook of Neuromodulation. New York, NY: Springer; 2015:127-150.
2. Livingston R, Anandan S, Moukaddam N. Electroconvulsive therapy, transcranial magnetic stimulation, and deep brain stimulation in treatment-resistant depression. Psychiatr Ann. 2016;46(4):240-246. CrossRef
3. Pinna M, Manchia M, Oppo R, et al. Clinical and biological predictors of response to electroconvulsive therapy (ECT): a review [published online ahead of print October 25, 2016]. Neurosci Lett. 2016. PubMed CrossRef
4. Perera T, George MS, Grammer G, et al. The clinical TMS society consensus review and treatment recommendations for TMS therapy for major depressive disorder. Brain Stimul. 2016;9(3):336-346. PubMed CrossRef
5. Cusin C, Dougherty DD. Somatic therapies for treatment-resistant depression: ECT, TMS, VNS, DBS. Biol Mood Anxiety Disord. 2012;2(1):14. PubMed CrossRef
6. Guleyupoglu B, Schestatsky P, Edwards D, et al. Classification of methods in transcranial electrical stimulation (tES) and evolving strategy from historical approaches to contemporary innovations. J Neurosci Methods. 2013;219(2):297-311. PubMed CrossRef
7. Datta A, Dmochowski JP, Guleyupoglu B, et al. Cranial electrotherapy stimulation and transcranial pulsed current stimulation: a computer-based high-resolution modeling study. Neuroimage. 2013;65:280-287. PubMed CrossRef
8. Kirsch DL, Nichols F. Cranial electrotherapy stimulation for treatment of anxiety, depression, and insomnia. Psychiatr Clin North Am. 2013;36(1):169-176. PubMed CrossRef
9. Barclay TH, Barclay RD. A clinical trial of cranial electrotherapy stimulation for anxiety and comorbid depression. J Affect Disord. 2014;164:171-177. PubMed CrossRef
10. Lande RG, Gragnani C. Efficacy of cranial electric stimulation for the treatment of insomnia: a randomized pilot study. Complement Ther Med. 2013;21(1):8-13. PubMed CrossRef
11. McClure D, Greenman SC, Koppolu SS, et al. A pilot study of safety and efficacy of cranial electrotherapy stimulation in treatment of bipolar II depression. J Nerv Ment Dis. 2015;203(11):827-835. PubMed CrossRef
12. Kennerly R. QEEG analysis of cranial electrotherapy: a pilot study. J Neurother. 2004;8:112.
13. Schroeder MJ, Barr R. Quantitative analysis of the electroencephalogram during cranial electrotherapy stimulation. Clin Neurophysiol. 2001;112(11):2075-2083. PubMed CrossRef
14. Lande RG, Pourzand M. Components and characteristics of a psychiatric partial hospital military program. Mil Med. 2016;181(3):213-218. PubMed CrossRef
15. Poltavski DV. The use of single-electrode wireless EEG in biobehavioral investigations. Methods Mol Biol. 2015;1256:375-390. PubMed CrossRef
16. Hu A. Computer Science and Applications: Proceedings of the 2014 Asia-Pacific Conference on Computer Science and Applications (CSAC 2014), December 27-28, 2014. Shanghai, China: CRC Press; 2015.
17. Katona J, Farkas I, Ujbanyi T, et al. Evaluation of the NeuroSky MindFlex EEG headset brain waves data. Paper presented at the 2014 IEEE 12th International Symposium on Applied Machine Intelligence and Informatics (SAMI); January 23-25, 2014: Herl’ any, Slovakia.
18. Rogers JM, Johnstone SJ, Aminov A, et al. Test-retest reliability of a single-channel, wireless EEG system. Int J Psychophysiol. 2016;106:87-96. PubMed CrossRef
19. Scherrer JF, Salas J, Sullivan MD, et al. The influence of prescription opioid use duration and dose on development of treatment resistant depression. Prev Med. 2016;91:110-116. PubMed CrossRef
20. Nguyen NT, Tojo S, Nguyen LM, et al. Intelligent Information and Database Systems: 9th Asian Conference, ACIIDS 2017. April 3-5, 2017, Proceedings. Kanazawa, Japan; Springer International Publishing; 2017.
21. Kirsch DL. The Science Behind Cranial Electrotherapy Stimulation. Edmonton, Canada: Medical Scope Publishing Corporation; 2002.
22. Wolpe J. The Practice of Behavior Therapy. Oxford, United Kingdom; Pergamon Press; 1969.
23. Saunders JB, Aasland OG, Babor TF, et al. Development of the Alcohol Use Disorders Identification Test (AUDIT): WHO collaborative project on early detection of persons with harmful alcohol consumption’ II. Addiction. 1993;88(6):791-804. PubMed CrossRef
24. Weathers FW, Litz BT, Keane TM, et al. The PTSD Checklist for DSM-5 (PCL-5). National Center for PTSD website. https://www.ptsd.va.gov/professional/assessment/adult-sr/ptsd-checklist.asp. Accessed December 14, 2017.
25. Moul DE, Pilkonis PA, Miewald JM, et al. Preliminary study of the test-retest reliability and concurrent validities of the Pittsburgh Insomnia Rating Scale (PIRS). Sleep. 2002;25 (abstract supplement): A246-A247.
26. Zung WW. A rating instrument for anxiety disorders. Psychosomatics. 1971;12(6):371-379. PubMed CrossRef
27. Zung W. Zung Self-Rating Depression Scale and Depression Status Inventory. Assessment of Depression. New York, NY: Springer; 1986:221-231.
28. Sanei S. Adaptive Processing of Brain Signals. West Sussex, United Kingdom; John Wiley & Sons; 2013.
29. Perry EK, Collerton D, LeBeau FEN, et al, eds. New Horizons in the Neuroscience of Consciousness. Amsterdam, The Netherlands: John Benjamins Publishing; 2010.
30. Young JS, Cashwell CS. Clinical Mental Health Counseling: Elements of Effective Practice. Thousand Oaks, CA: SAGE Publications; 2016.
Enjoy this premium PDF as part of your membership benefits!