Improvement in Functional Outcomes With Adjunctive Aripiprazole Versus Placebo in Major Depressive Disorder: A Pooled Post Hoc Analysis of 3 Short-Term Studies

ABSTRACT
Objective: To evaluate the effect of adjunctive aripiprazole to antidepressant therapy (ADT) on functional outcomes, as assessed by the Sheehan Disability Scale (SDS).
Method: A post hoc analysis of pooled data from 3 similarly designed randomized, placebo-controlled trials was conducted (CN138-139 [September 2004-December 2006], CN138-163 [June 2004-April 2006], and CN138-165 [March 2005-April 2008]). Patients with DSM-IV major depressive disorder who had a prior inadequate response to ADT received adjunctive aripiprazole or placebo to standard ADT. The change from baseline to endpoint on total SDS score and on individual SDS domains and the distributional categorical shifts of patient-reported severity of functional impairment on the SDS were assessed.
Results: Aripiprazole compared to placebo augmentation produced significant improvements in self-reported functioning levels in the SDS mean total score (-1.2 vs -0.7, P ≤ .001) and social life (-1.4 vs -0.7, P ≤ .001) and family life (-1.4 vs -0.7, P ≤ .001) domains. Additionally, a significant number of patients exhibited a shift from a severe/moderate level of impairment at baseline to a mild level of functional impairment after 6 weeks of adjunctive aripiprazole treatment compared with placebo in the SDS mean total score (P = .001) and social life (P ≤ .001) and family life (P = .001) scores.
Conclusions: Aripiprazole augmentation of standard antidepressant therapy resulted in significant improvements in both total and individual domains of functioning, as assessed by the SDS, with significant categorical shifts from severe/moderate to mild levels of functioning compared with placebo augmentation.
Trial Registration: ClinicalTrials.gov identifiers: NCT00095823, NCT00095758, and NCT00105196
Prim Care Companion CNS Disord 2012;14(6):doi:10.4088/PCC.12m01394
© Copyright 2012 Physicians Postgraduate Press, Inc.
Submitted: April 11, 2012; accepted July 2, 2012.
Published online: Decmber 20, 2012.
Corresponding author: Tanya J. Fabian, PharmD, PhD, Ste 430 WPIC, 3811 O’ Hara St, Pittsburgh, PA 15213 ([email protected]).
Depression is among the leading causes of disability in the United States and worldwide. Most patients with major depressive disorder (MDD) report some degree of symptom-related functional impairment. The term functioning in MDD encompasses interrelated social, physical, and occupational domains. By one estimation, approximately 80% of people with MDD have reported some level of functional impairment, and 27% have reported serious difficulties in work and home life.1 On average, 27.2 work days per year are lost due to MDD.2 Reports estimate that patients with MDD have an unemployment rate 5 times higher than nondepressed individuals.3 Indeed, depressive symptoms are often associated with impaired psychosocial functioning and reduced quality of life,4 resulting in social isolation, marital problems, and impaired occupational functioning.5 Untreated or undertreated depression affects diverse parameters, such as difficulty forming and maintaining relationships with family and friends and carrying out activities of daily living, including work and/or school tasks.6
Response and remission to treatment in MDD are associated with clinically significant improvements in quality of life, well-being, and functional status, as well as lower health care costs and productivity gains.7 More importantly, as functioning domains are interrelated, improvements in one domain may in turn lead to beneficial effects on other aspects of functioning.6 Therefore, treatment goals in MDD should address both symptomatic reduction and functional recovery to allow patients to return to their pre-depressive episode level of functioning. It is important to regain prior levels of functioning because unresolved symptoms after antidepressant therapy (ADT) can lead to long-term psychosocial impairment and increased rates of relapse.8,9 Evidence from the Sequenced Treatment Alternatives to Relieve Depression (STAR*D) trial10 showed that even after an adequate ADT trial, approximately two-thirds of patients failed to achieve remission, defined as a score ≤ 7 on the 17-item Hamilton Depression Rating Scale (HDRS-17). It has been shown that pharmacologic augmentation of standard ADT may provide symptomatic improvement in patients with MDD who have not fully responded to standard ADT.11 Indeed, such a treatment strategy has been recommended in a recent update of the American Psychiatric Association’s clinical practice guidelines for the treatment of MDD,12 in which it is suggested that pharmacologic augmentation may increase the rates of response or remission of depressive symptoms in patients who typically have not responded to more than 2 medication trials, including augmentation with atypical antipsychotics, even when psychotic symptoms are not present.
Evidence from 3 randomized, double-blind, placebo-controlled studies demonstrated the efficacy of aripiprazole adjunctive to standard ADT for the treatment of MDD symptoms and led to its approval for adjunctive therapy in MDD by the US Food and Drug Administration.13-15 The mechanism underlying the efficacy of aripiprazole in the treatment of MDD has been attributed to the action of aripiprazole as a partial agonist of dopamine D2/D3 and serotonin 5-HT1A receptors and as an antagonist of 5-HT2A receptors. Interestingly, evidence from animal models that reproduce the mode of action of aripiprazole augmentation showed increased firing of serotonin, norepinephrine, and dopamine neurons when aripiprazole was added to rats exposed for 14 days to the selective serotonin reuptake inhibitor (SSRI) escitalopram.16 Treatment failures and adverse events associated with SSRIs have been attributed in part to their inhibitory action on both norepinephrine and dopamine neurotransmission via the activation of 5-HT2A and 5-HT2C receptors, respectively. By blocking 5-HT2A and 5-HT2C receptors, aripiprazole may counterbalance this inhibitory action of SSRIs, thus preserving norepinephrine and dopamine firing that may be relevant to improvement in symptoms of MDD.16

- The majority of patients with major depressive disorder have reported some level of functional impairment such as difficulties in work and home life.
- Patient self-rated scales, such as the Sheehan Disability Scale, can assess impairment in social life, family life, and work/school responsibilities related to depression.
- Current evidence supports aripiprazole augmentation of antidepressant therapy to improve functioning in depression.
Data from 3 similarly designed aripiprazole studies13-15 in MDD were pooled, and a post hoc analysis was conducted to evaluate the effect of aripiprazole adjunctive to ADT on functional outcomes in patients with MDD who had a prior inadequate response to standard ADT. Changes in Sheehan Disability Scale (SDS) total and domain scores were a secondary outcome measure of the studies’ design. The objective of the current post hoc analysis was to assess the change from baseline to endpoint on total SDS score and on individual SDS domains and the distributional categorical shifts of patient-reported severity of functional impairment on the SDS.
METHOD
Study Design
Details of the study methods, as well as inclusion and exclusion criteria, have been described previously.13-15 In brief, data were pooled from 3 similarly designed multicenter, randomized, double-blind, placebo-controlled phase 3 studies (CN138-139 [September 2004-December 2006], CN138-163 [June 2004-April 2006], and CN138-165 [March 2005-April 2008]; ClinicalTrials.gov identifiers: NCT00095758, NCT00095823, and NCT00105196, respectively). Two of the 3 studies included (CN138-139 and CN138-163) were nearly identical in design. All 3 studies were conducted in the United States to investigate the efficacy and safety of adjunctive aripiprazole to standard ADT in patients with MDD (DSM-IV criteria) who showed an inadequate response (defined as < 50% reduction in severity of depressive symptoms) to at least 1 historical and 1 prospective ADT. Patients were not included if they had failed > 3 prior ADTs. Each of the 3 studies comprised 3 separate phases: a screening phase (7-28 days) in which prohibited medications (including benzodiazepines and hypnotic agents) were discontinued, a prospective ADT phase (8 weeks), and a randomization phase (6 weeks; actual study visits: weeks 9-14). During the prospective ADT phase, patients with MDD (HDRS-17 total score ≥ 18) received 8 weeks of therapy with escitalopram, fluoxetine, paroxetine controlled release, sertraline, or venlafaxine extended release, per investigator choice under standard dosing guidelines, as well as an adjunctive placebo. Neither patients nor study physicians knew when the second phase ended and the third phase began. Patients with an inadequate response at the end of the second phase (< 50% reduction in HDRS-17 total score, HDRS-17 score ≥ 14, and Clinical Global Impressions-improvement scale score ≥ 3) were randomized in a double-blind fashion to either continue with adjunctive placebo or begin receiving adjunctive flexible-dose aripiprazole (2-20 mg/d; starting dose: 5 mg/d) for 6 additional weeks of therapy. For patients who received aripiprazole adjunctive to paroxetine controlled release and fluoxetine, the maximum dose of aripiprazole was 15 mg/d.
Functioning Assessment
Patient functioning was assessed by the change in SDS score from week 8 (end of prospective treatment) to week 14 (end of adjunctive treatment).
The SDS assesses functional impairment in 3 domains: social life, family life, and work/school responsibilities.5 Each item is scored on a severity scale of 0-10, with 0-3 indicating not at all to mildly impaired, 4-6 indicating moderately impaired, and 7-10 indicating markedly to extremely impaired.5 Mean and individual domain SDS scores were retrospectively categorized at baseline (week 8) and endpoint (week 14) as mild (0-3), moderate (4-6), or severe (7-10) functional impairment. Total SDS scores were calculated as a mean of the 3 individual domains. For patients not currently working or enrolled in school, only 2 domains were used: social life and family life.
Statistical Analyses
All 3 studies were similar in design and methods; therefore, the data were pooled to further evaluate functional outcomes. Changes in SDS mean total and work/school, social life, and family life domain scores were calculated from the end of the prospective phase (week 8) to the end of the randomization phase (week 14 visit, last observation carried forward [LOCF]). Changes from baseline (week 8) to endpoint (week 14) in mean SDS total scores and domain scores were compared using an analysis of covariance between patients randomized to 6 weeks of adjunctive aripiprazole or adjunctive placebo treatment, with double-blind treatment and protocol as main effects and end of prospective phase assessment as covariate. In addition to changes in SDS scores from baseline, categorical shifts in the distribution of total SDS scores and individual domain scores were compared between adjunctive aripiprazole and adjunctive placebo treatment using a generalized estimating equation proportional odds model with double-blind treatment, time, and treatment-by-time interaction as categorical effects and an independent working covariance matrix. Relative risks were calculated for the likelihood that an individual patient experienced a shift from severe or moderate impairment at baseline to mild impairment at endpoint.
RESULTS
Patient Characteristics
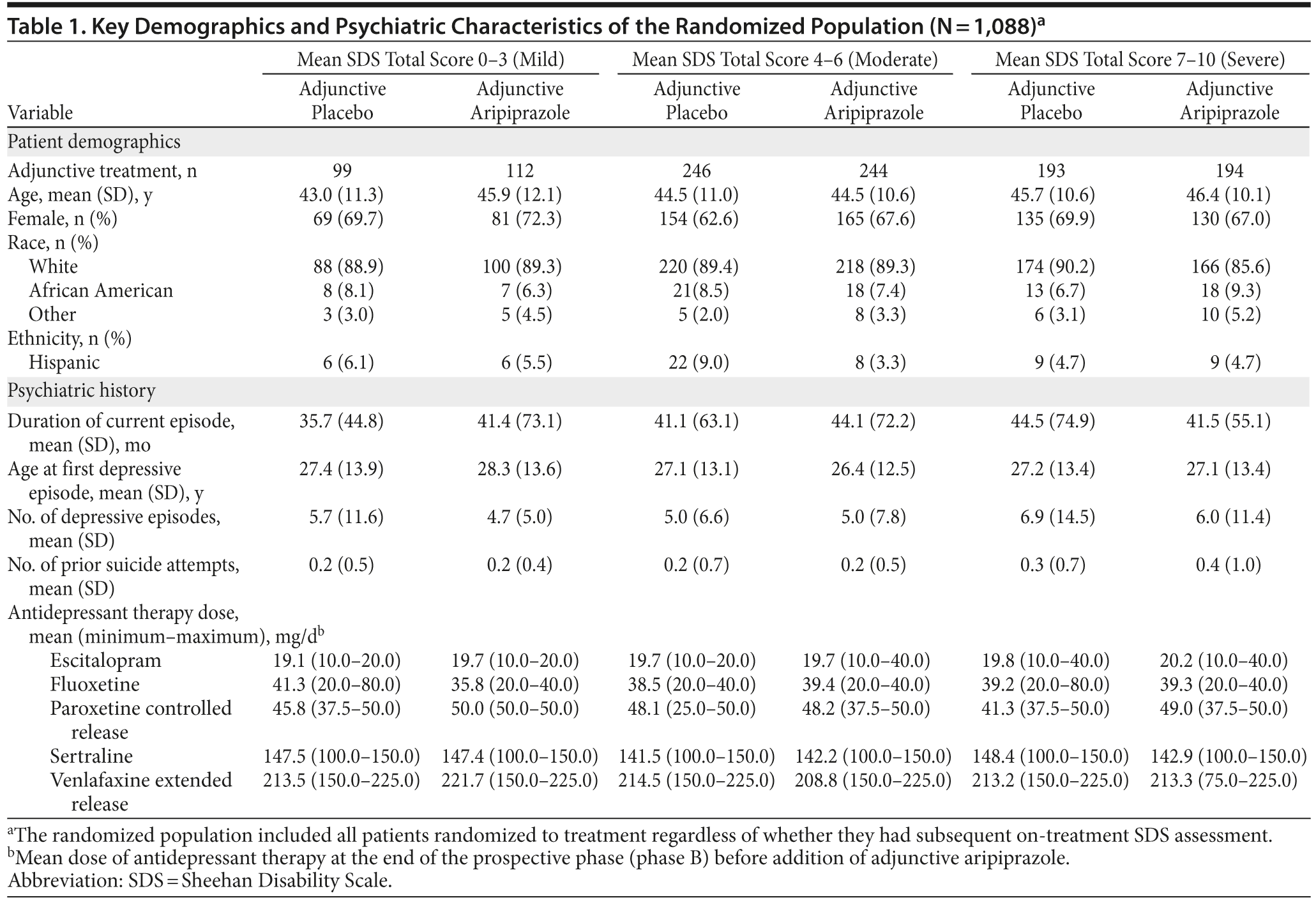
Baseline demographic and psychiatric characteristics of the randomized population by level of severity are summarized in Table 1. The baseline psychiatric characteristics of the 1,088 patients were similar among the 3 severity groups. Interestingly, patients with a severe mean SDS total score had experienced 1 more depressive episode than patients with a mild or moderate SDS total score. Mean ADT dose and duration were adequate in both augmentation treatment arms and comparable among patients across all disability levels. Patients’ functional status was assessed at baseline (week 8) and endpoint (week 14, LOCF) and was stratified according to SDS score as mild (0-3), moderate (4-6), or severe (7-10). Moderate to severe functional impairments were observed in 81% (n = 877/1,088) of the randomized population at baseline, as assessed by mean SDS total scores.
Functional Assessments
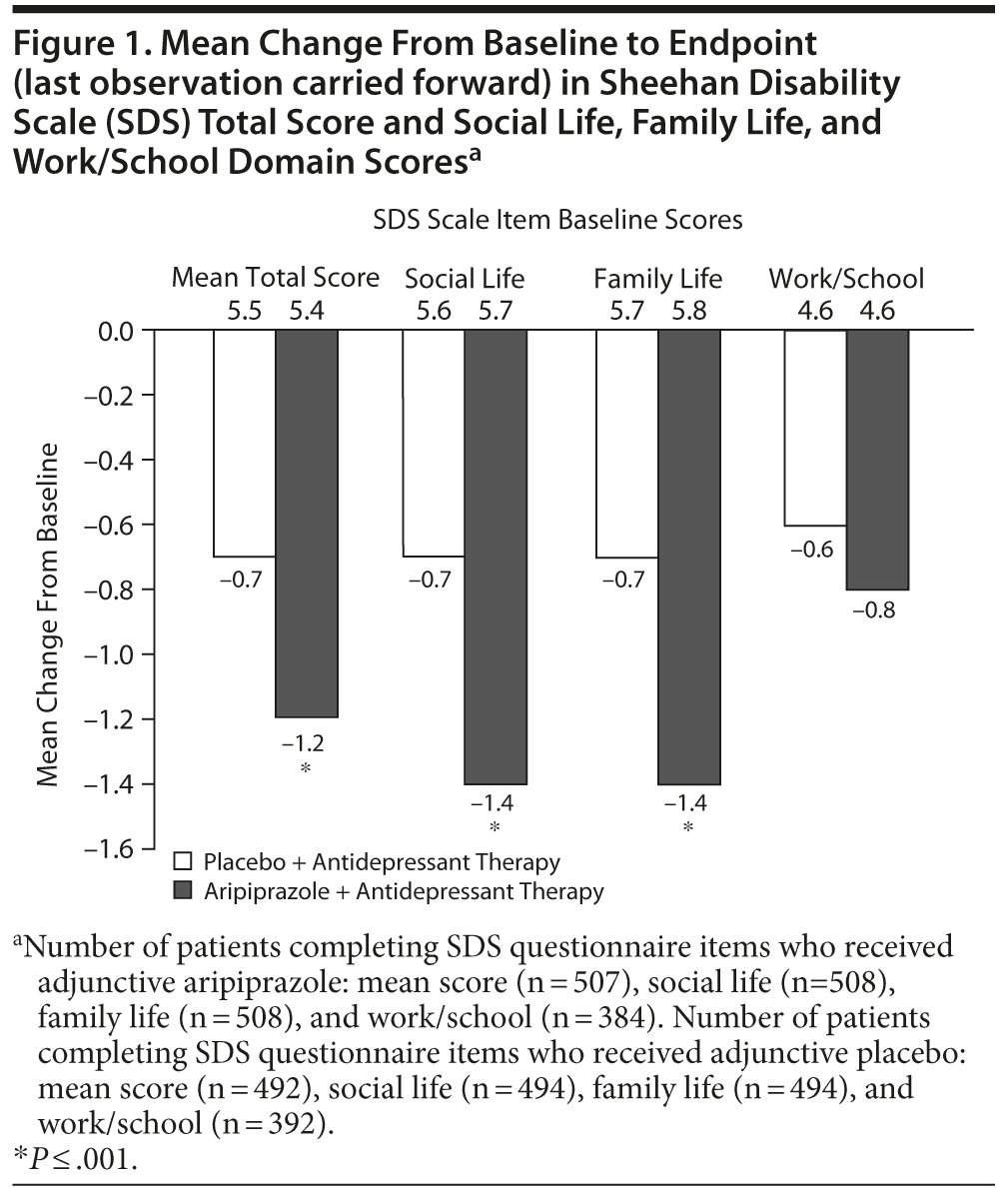
Mean change in SDS total scores and individual domain scores are shown in Figure 1. Patients receiving adjunctive aripiprazole showed significant functional gains compared with placebo in SDS mean total score (-1.2 vs -0.7, P ≤ .001; n = 507 vs n = 492), as well as in the social life (-1.4 vs -0.7, P ≤ .001; n = 508 vs n = 494) and family life (-1.4 vs -0.7, P ≤ .001; n = 508 vs n = 494) domains, as assessed by mean changes from baseline to endpoint (LOCF). There was no statistically significant difference in the mean change from baseline to endpoint (LOCF) for the work/school domain of the SDS among patients in either augmentation group (-0.8 vs -0.6, P = .337; n = 384 vs n = 392).
Shifts in Functional Impairments
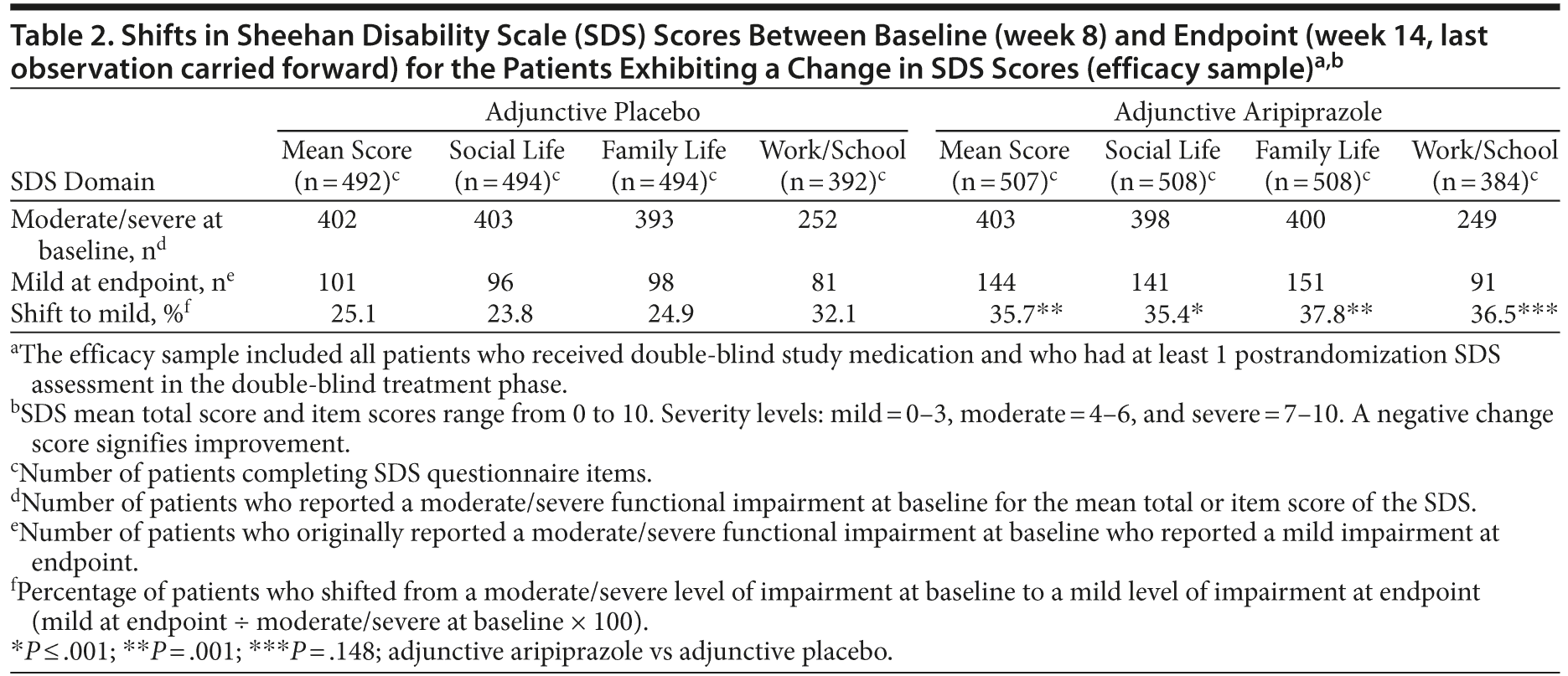
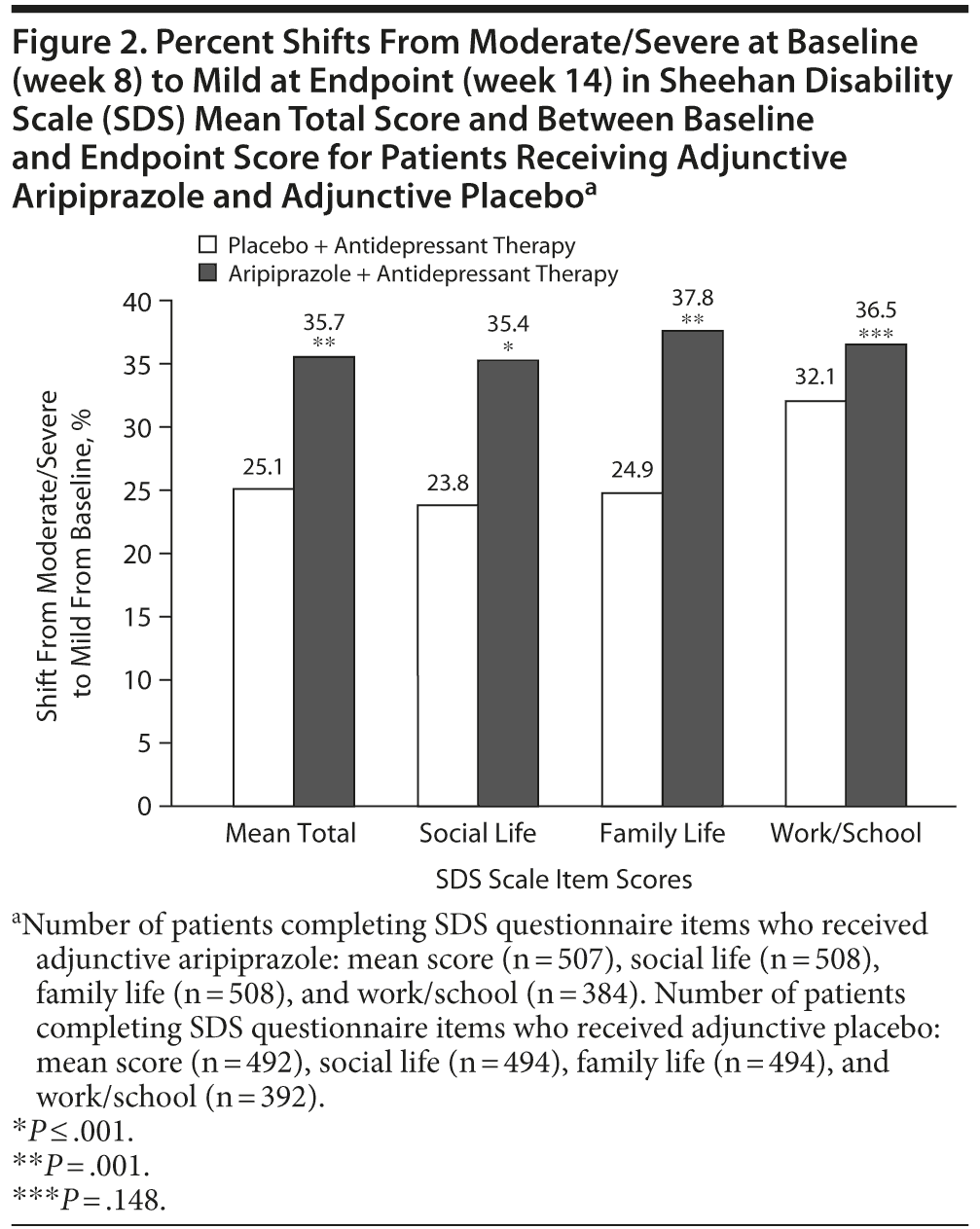
At baseline, 403 patients in the adjunctive aripiprazole group reported a moderate or severe level of impairment. After 6 weeks of adjunctive aripiprazole treatment, 144 patients reported a mild impairment, as assessed by the SDS mean total score, indicating that 35.7% of the total adjunctive aripiprazole population had shifted to a less severe level of impairment (Table 2). Similar shifts from severe/moderate levels of severity at baseline to mild levels of severity at endpoint were observed for the social life (35.4%), family life (37.8%), and work/school (36.5%) domains in the adjunctive aripiprazole group. Patients receiving adjunctive placebo also reported shifts from moderate/severe levels of impairment at baseline to mild levels of impairment at endpoint in the SDS mean total score (25.1%), social life (23.8%), family life (24.9%), and work/school (32.1%) domains (Table 2). A representation of the shifts from moderate/severe to mild in SDS mean and domain item scores between baseline and endpoint are shown in Figure 2.
There was a significant reduction from baseline to endpoint in the number of patients reporting a severe/moderate impairment in the social life domain in the adjunctive aripiprazole group (398 to 288) compared with the adjunctive placebo group (403 to 338, P ≤ .001). A similar statistically significant reduction in the family life domain was observed for the number of patients reporting a severe/moderate impairment from baseline to endpoint in the adjunctive aripiprazole group (400 to 277) compared with the reduction in the adjunctive placebo group (393 vs 335, P = .001). Although there was a reduction from baseline to endpoint in the number of patients reporting a severe/moderate impairment in the work/school domain for the adjunctive aripiprazole group (249 to 193), the reduction was not statistically significant when compared with the reduction from baseline to endpoint in the number of patients in the adjunctive placebo group (252 to 211, P = .148).
Relative-Risk Analysis
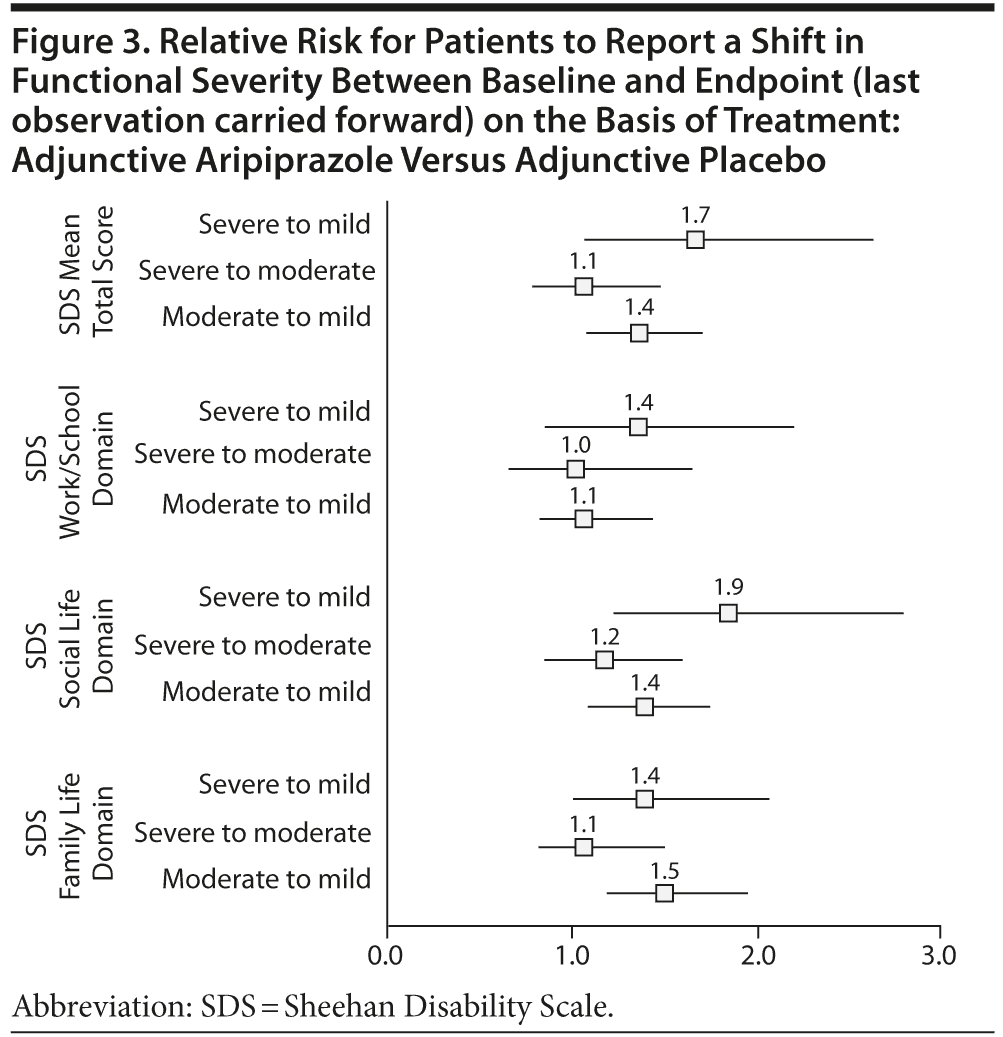
A relative-risk analysis for categorical improvement in SDS mean score shift showed that patients receiving adjunctive aripiprazole treatment were more likely to report shifts from severe to mild functional impairments compared with patients receiving adjunctive placebo (Figure 3); the relative risk for patients to report a shift from severe impairment at baseline in the SDS mean total score to a mild functional impairment was 1.7 (95% CI = 1.1-2.6). Adjunctive aripiprazole-treated patients were also significantly more likely to achieve a reduction in SDS mean total score from moderate impairment to mild impairment than placebo-treated subjects (relative risk = 1.4; 95% CI = 1.1-1.7). Improvements in social life and family life domains were seen; however, the 95% CI for patients to report a shift from severe to mild family life impairment included 1.0, indicating that improvements were not significantly different. All shifts for the work/school domain were > 1.0, although not significantly different between adjunctive aripiprazole and adjunctive placebo.
DISCUSSION
The current pooled post hoc analysis showed that patients treated with aripiprazole augmentation to standard ADT experienced significant improvements in both total and individual domains of functioning, as assessed by the SDS. As improved functioning is a clinically meaningful marker of overall improvement for patients with psychiatric disorders,9 these results are consistent with treatment goals for MDD, aiming to return patients to levels of functioning comparable with those assessed before the beginning of the depressive episode. Aripiprazole augmentation also resulted in significantly more patients experiencing an improvement in functioning over the course of treatment than placebo, as evidenced by the greater number of patients experiencing a shift in SDS total scores from severe/moderate to mild levels of functional impairment. In addition, patients receiving adjunctive aripiprazole exhibited significant improvements in SDS total, social life, and family life domain scores compared with patients receiving adjunctive placebo.
Functional recovery after a major depressive episode should be the goal of treatment, as enduring unresolved symptoms can lead to long-term psychosocial impairment.9 In fact, impairments in social functioning are a significant aspect of MDD and are distinct from general symptoms of depression, as social functioning encompasses how individuals interact with their environment and fulfill their roles at work, within social activities, and in relationships with partners and family.6 It has long been recognized that there is an association between depression and impaired social functioning, and it is acknowledged that recovery from depression requires both the resolution of depressive symptoms and an improvement in the interactions of individuals with their social and work environments.6 Unfortunately, despite multiple rounds of pharmacotherapy and/or long-term treatment, functional impairments persist long after resolution of symptoms. Although the assessment of functional impairments is influenced by the scale used, regardless of instrument used, there is an increased awareness that the patient’s perspective should be foremost.
The current analysis showed that aripiprazole augmentation to ADT significantly improved patient-rated functional impairments—in particular, in the social and family life domains of the SDS. The lack of significant improvement in the SDS work/school domain scores may reflect that those patients reporting on that domain were a less severely impaired subgroup of patients than the overall population. The latter is consistent with lower baseline scores reported for the SDS work/school domain by patients receiving adjunctive aripiprazole and adjunctive placebo. In addition, because patients not working or in school were not required to report on the work/school domain of the SDS, the study may have been underpowered to detect changes in work/school-related functional impairments. Furthermore, it is possible that treatment periods beyond 6 weeks may be necessary to observe significant improvements on the work/school domain. Nevertheless, the improvements in functional outcomes in patients receiving adjunctive aripiprazole for the treatment of MDD are encouraging. A survey of approximately 9,000 US households showed that the role impairment, as measured by the SDS, was substantial: 59.3% of patients with a diagnosis of MDD in the prior 12 months reported severe or very severe role impairment.17
Patients who exhibit an inadequate response to treatment for MDD are highly likely to experience a prolonged loss of quality of life, functional status, and productivity and to incur higher health care costs compared with patients with adequate response and remission with pharmacologic treatment.7 Therefore, identifying and assessing the severity of functional impairments experienced by patients with MDD is as important as identifying an adequate pharmacotherapy to ensure their return to pre-episode levels of functioning.
Limitations
The findings in this study should be considered with regard to several limitations. First, the findings reported were generated from a pooled post hoc analysis. The nearly identical design of the 3 clinical trials allowed for pooling of data. Each of the 3 trials included disability assessments; however, the specific measure of categorical shifts was not previously assessed. Therefore, the evaluation of categorical shifts in disability conducted in the pooled analysis was exploratory in nature. The study protocol excluded patients who had failed > 3 prior ADTs, and evidence from STAR*D showed that 33% of patients fail to remit after 4 stages of treatment, leaving tremendous unmet medical needs.10 However, the dose and duration of antidepressants were adequate in the adjunctive aripiprazole trials, which is not normally the case in real-world situations. The short duration (6 weeks) of the trial does not allow for conclusions about long-term benefits of aripiprazole augmentation on functioning. Moreover, the analysis is also limited by the lack of data for patients who were not scored for the work/school item of the SDS. Therefore, no assumptions were made, and we cannot tell from the current dataset whether the subpopulation was not working by choice or by impairment due to their depressive symptoms.
The SDS is a generic self-report of well-being and functional status, but its single-item scores for each of the 3 domains may lack specificity in highly comorbid patients. Nevertheless, despite its brevity, the SDS is considered to be a good initial assessment of functional status.18 In addition, the SDS has been shown to perform well when treated as a numeric scale, and mean changes in SDS scores to endpoint have been analyzed using parametric statistics5 as was done in the current analysis.
CONCLUSION
Patients with an inadequate response to standard ADT often experience marked functional impairments, particularly in social and family relationships. In this study, aripiprazole augmentation of standard ADT resulted in significant improvements in both total and individual domains of functioning, as assessed by the SDS. Furthermore, significant categorical shifts from severe/moderate to mild levels of functioning were observed in patients treated with aripiprazole augmentation compared with placebo augmentation. However, further research is needed to show whether functional gains in patients with MDD treated with aripiprazole augmentation result in improved quality of life, well-being, and adherence to treatment.
Drug names: aripiprazole (Abilify), escitalopram (Lexapro and others), fluoxetine (Prozac and others), paroxetine (Paxil, Pexeva, and others), sertraline (Zoloft and others), venlafaxine (Effexor and others).
Author affiliations: Western Psychiatric Institute and Clinic, Pittsburgh, Pennsylvania (Dr Fabian and Ms Tang); Bristol-Myers Squibb Co, Plainsboro, New Jersey (Drs Cain, Ammerman, and Berman and Mr Eudicone); Bristol-Myers Squibb Co, Wallingford, Connecticut (Dr Rollin); and Otsuka Pharmaceutical Development and Commercialization, Inc, Princeton, New Jersey (Drs Forbes and Baker).
Potential conflicts of interest: Drs Cain, Ammerman, Rollin, and Berman and Mr Eudicone are employees of Bristol-Myers Squibb. Dr Berman also receives salary and stock options from Bristol-Myers Squibb. Dr Baker is an employee of and Dr Forbes is a former employee of Otsuka Pharmaceutical Development and Commercialization (Princeton, New Jersey). Dr Forbes is currently an employee of Genentech. Dr Fabian and Ms Tang report no conflicts of interest related to the subject of this article.
Funding/support: This study was supported by Bristol-Myers Squibb (Princeton, New Jersey) and Otsuka Pharmaceutical Co, Ltd (Tokyo, Japan).
Previous presentations: 50th Annual New Clinical Drug Evaluation Unit meeting; June 14-17, 2010; Boca Raton, Florida ▪ 19th Annual European Psychiatric Association European Congress of Psychiatry; March 12-15, 2011; Vienna, Austria.
Acknowledgments: Editorial support for the preparation of this manuscript was provided by Ogilvy Healthworld Medical Education. The authors thank Madhukar H. Trivedi, MD (University of Texas Southwestern Medical Center, Dallas); Stephen R. Wisniewski, PhD (University of Pittsburgh, Pittsburg, Pennsylvania); J. Craig Nelson, MD (University of California, San Francisco); Christina M. Dording, MD (Massachusetts General Hospital, Harvard Medical School, Boston); and Edward S. Friedman, MD (University of Pittsburgh Medical Center, Pittsburgh, Pennsylvania) for their contributions to the analysis and interpretation of data. Drs Trivedi, Wisniewski, Nelson, Dording and Friedman report no conflicts of interest related to the subject of this article.
References
1. Pratt LA, Brody DJ. Depression in the United States Household Population, 2005-2006. Atlanta, GA: National Center for Health Statistics; 2008.
2. Kessler RC, Akiskal HS, Ames M, et al. Prevalence and effects of mood disorders on work performance in a nationally representative sample of US workers. Am J Psychiatry. 2006;163(9):1561-1568. PubMed doi:10.1176/appi.ajp.163.9.1561
3. Lerner D, Adler DA, Chang H, et al. Unemployment, job retention, and productivity loss among employees with depression. Psychiatr Serv. 2004;55(12):1371-1378. PubMed doi:10.1176/appi.ps.55.12.1371
4. Keller MB. Past, present, and future directions for defining optimal treatment outcome in depression: remission and beyond. JAMA. 2003;289(23):3152-3160. PubMed doi:10.1001/jama.289.23.3152
5. Sheehan KH, Sheehan DV. Assessing treatment effects in clinical trials with the discan metric of the Sheehan Disability Scale. Int Clin Psychopharmacol. 2008;23(2):70-83. PubMed doi:10.1097/YIC.0b013e3282f2b4d6
6. Bosc M. Assessment of social functioning in depression. Compr Psychiatry. 2000;41(1):63-69. PubMed doi:10.1016/S0010-440X(00)90133-0
7. Mauskopf JA, Simon GE, Kalsekar A, et al. Nonresponse, partial response, and failure to achieve remission: humanistic and cost burden in major depressive disorder. Depress Anxiety. 2009;26(1):83-97. PubMed doi:10.1002/da.20505
8. Fava M, Rush AJ, Trivedi MH, et al. Background and rationale for the Sequenced Treatment Alternatives to Relieve Depression (STAR*D) study. Psychiatr Clin North Am. 2003;26(2):457-494. PubMed doi:10.1016/S0193-953X(02)00107-7
9. Kennedy N, Foy K, Sherazi R, et al. Long-term social functioning after depression treated by psychiatrists: a review. Bipolar Disord. 2007;9(1-2):25-37. PubMed doi:10.1111/j.1399-5618.2007.00326.x
10. Rush AJ, Trivedi MH, Wisniewski SR, et al. Acute and longer-term outcomes in depressed outpatients requiring one or several treatment steps: a STAR*D report. Am J Psychiatry. 2006;163(11):1905-1917. doi:10.1176/appi.ajp.163.11.1905 PubMed
11. Shelton RC, Papakostas GI. Augmentation of antidepressants with atypical antipsychotics for treatment-resistant major depressive disorder. Acta Psychiatr Scand. 2008;117(4):253-259. PubMed doi:10.1111/j.1600-0447.2007.01130.x
12. American Psychiatric Association. Practice Guideline for the Treatment of Patients With Major Depressive Disorder. 3rd ed. Arlington, VA: American Psychiatric Association; 2010.
13. Berman RM, Marcus RN, Swanink R, et al. The efficacy and safety of aripiprazole as adjunctive therapy in major depressive disorder: a multicenter, randomized, double-blind, placebo-controlled study. J Clin Psychiatry. 2007;68(6):843-853. PubMed doi:10.4088/JCP.v68n0604
14. Marcus RN, McQuade RD, Carson WH, et al. The efficacy and safety of aripiprazole as adjunctive therapy in major depressive disorder: a second multicenter, randomized, double-blind, placebo-controlled study. J Clin Psychopharmacol. 2008;28(2):156-165. PubMed doi:10.1097/JCP.0b013e31816774f9
15. Berman RM, Fava M, Thase ME, et al. Aripiprazole augmentation in major depressive disorder: a double-blind, placebo-controlled study in patients with inadequate response to antidepressants. CNS Spectr. 2009;14(4):197-206. PubMed
16. Chernoloz O, El Mansari M, Blier P. Electrophysiological studies in the rat brain on the basis for aripiprazole augmentation of antidepressants in major depressive disorder. Psychopharmacology (Berl). 2009;206(2):335-344. PubMed doi:10.1007/s00213-009-1611-7
17. Kessler RC, Berglund P, Demler O, et al; National Comorbidity Survey Replication. The epidemiology of major depressive disorder: results from the National Comorbidity Survey Replication (NCS-R). JAMA. 2003;289(23):3095-3105. PubMed doi:10.1001/jama.289.23.3095
18. Klinkman MS. Assessing functional outcomes in clinical practice. Am J Manag Care. 2009;15(suppl 11):S335-S342. PubMed