Improving Quality of Depression Care Using Organized Systems of Care: A Review of the Literature
Objective: To establish the need for a chronic disease management strategy for major depressive disorder (MDD), discuss the challenges involved in implementing guideline-level treatment for MDD, and provide examples of successful implementation of collaborative care programs.
Data Sources: A systematic literature search of MEDLINE and the US National Library of Medicine was performed.
Study Selection: We reviewed clinical studies evaluating the effectiveness of collaborative care interventions for the treatment of depression in the primary care setting using the keywords collaborative care, depression, and MDD. This review includes 45 articles relevant to MDD and collaborative care published through May 2010 and excludes all non-English-language articles.
Results: Collaborative care interventions include a greater role for nonmedical specialists and a supervising psychiatrist with the major goal of improving quality of depression care in primary care systems. Collaborative care programs restructure clinical practice to include a patient care strategy with specific goals and an implementation plan, support for self-management training, sustained patient follow-up, and decision support for medication changes. Key components associated with the most effective collaborative care programs were improvement in antidepressant adherence, use of depression case managers, and regular case load supervision by a psychiatrist. Across studies, primary care patients randomized to collaborative care interventions experienced enhanced treatment outcomes compared with those randomized to usual care, with overall outcome differences approaching 30%.
Conclusions: Collaborative care interventions may help to achieve successful, guideline-level treatment outcomes for primary care patients with MDD. Potential benefits of collaborative care strategies include reduced financial burden of illness, increased treatment adherence, and long-term improvement in depression symptoms and functional outcomes.
Prim Care Companion CNS Disord 2011;13(1):e1-e8
© Copyright 2011 Physicians Postgraduate Press, Inc.
Submitted: May 20, 2010; accepted July 19, 2010.
Published online: February 10, 2011 (doi:10.4088/PCC.10r01019blu).
Corresponding author: Wayne Katon, MD, Department of Psychiatry & Behavioral Sciences, Box 356560, University of Washington Medical School, 1959 NE Pacific, Seattle, WA 98195 ([email protected]).
Approximately 6%-10% of primary care patients meet diagnostic criteria1 for major depressive disorder (MDD). However, only 50% of patients with MDD are accurately diagnosed by primary care physicians, and many patients do not receive guideline-level treatment for MDD.2 For example, among primary care patients with diabetes and comorbid MDD, 51% of patients identified with MDD were diagnosed with depression in the 12 months prior to screening, approximately 33% of treated patients received adequate pharmacotherapy (duration ≥ 90 days), and 6.7% received adequate psychotherapy (≥ 4 visits in 1 year).3
The lack of recognition and effective treatment of patients with MDD is significant due to the potential chronicity of the illness. Successful treatment of MDD should involve a chronic disease management strategy that requires patient care that is consistent with treatment guidelines, with the overall goals of remission, recovery of psychosocial functioning, and prevention of recurrent episodes.4,5 The collaborative care model is a promising approach to achieving these goals.6 Earlier studies of collaborative care models in primary care settings demonstrated success in improving clinical outcomes7,8 and patient satisfaction with treatment.7 The objectives of this review are to establish the need for a chronic disease management strategy for MDD, discuss challenges in the implementation of treatment guidelines/algorithms, and provide examples of successful collaborative care programs.
This review includes clinical studies evaluating the effectiveness of collaborative care interventions for the treatment of depression in the primary care setting. A systematic literature search of MEDLINE and the US National Library of Medicine was performed using the keywords collaborative care, depression, and MDD. This review includes articles describing clinical studies published through May 2010 and excludes all non-English-language articles.
MDD Is a Chronic Illness
Chronic illnesses commonly last longer than 3 months, are not self-limiting, and affect approximately 50% of the US population.9 MDD is an example of a chronic illness that is often characterized by multiple recurrent episodes and is potentially disabling.10 Furukawa and colleagues11 evaluated patients with a single episode of MDD over 10 years of follow-up and demonstrated that patients spent 75% (95% CI, 74-76) of follow-up months in euthymia, 19% (95% CI, 18-20) in subthreshold depression, and 6% (95% CI, 6-7) in a major depressive episode. The risk of recurrence of MDD is 60% after the initial episode, 70% after 2 episodes, and 90% after 3 episodes.10 Furukawa et al11 reported that over 10 years of follow-up, 18% of patients recovered with no recurrence, 30% recovered but experienced a subthreshold recurrence, and 45% recovered but experienced a full episode recurrence.
Clinical Points
- Primary care-based studies show major gaps in quality of depression care.
- Primary care patients who are prescribed antidepressants often receive little education about depression and have infrequent follow-up visits leading to poor adherence to treatment.
- Collaborative care has been shown to be an effective health services model in improving quality of depression care and depression outcomes.
Untreated or undertreated depression is often associated with substantial impairment in psychosocial functioning.12 This functional impairment is often comparable to, or more profound than, that reported among patients with other chronic medical conditions, such as hypertension, diabetes, or arthritis.13-15 Although the extent of functional impairment in depressed patients may vary according to the duration and severity of the illness, impaired functioning is not always confined to the depressive episode, with subthreshold depressive symptoms often resulting in continued functional impairment.16,17
Depression is often comorbid with illnesses such as diabetes, asthma, and heart disease, among others.18 Depression can serve as a risk factor for development or exacerbation of some comorbid illnesses, including cardiovascular disease, type 2 diabetes, cerebrovascular disease, and pulmonary disease.19-21 The risk of developing type 2 diabetes is an estimated 37% higher in adults with depression versus adults without depression.20 Comorbid depression can also increase the risk of poor management of other illnesses. Mancuso et al22 demonstrated that patient-reported depressive symptoms were associated with increased asthma severity and poor asthma control. Patients with depression and comorbid medical illnesses often have a greater medical symptom burden, additive functional impairment, poor self-care, and substantially greater medical costs21; are 3 times more likely to be nonadherent to treatment23; and have a substantial increased risk of death compared with nondepressed patients.24-27
The financial impact of depression (eg, health care costs, absenteeism, decreased productivity) is among the largest of any disease.28-31 Results of a 4-year, prospective study (N = 2,558) demonstrated that patients with significant depressive symptoms had 50% higher health care costs versus patients with no depressive symptoms, even after controlling for age, gender, and severity of chronic medical illness.28 A separate clinical study showed that patients with depression had 2-fold greater total health care costs (inpatient, outpatient, pharmacy, and emergency treatment costs) versus age- and gender-matched controls over 12 months.29 The high cost of depression was comparable to other common medical illnesses in a recent study by Lurie et al.31 No statistically significant differences were observed in total and out-of-pocket costs for depression versus costs for asthma, arthritis, cardiovascular disease, diabetes, or stroke.31
Disease management strategies for depression should mirror those of other chronic conditions, such as asthma, for which treatment is used to alleviate acute episodes and maintain remission. The importance of regularly monitoring symptoms and ensuring that treatment continues until the patient reaches a nearly asymptomatic state and is used to maintain response cannot be overstated. Growing evidence demonstrates that such chronic disease management strategies can lower health care costs, improve the cost-effectiveness of treatment, decrease absenteeism, and improve work performance.32-35 Schoenbaum et al36 evaluated the cost-effectiveness of 2 quality improvement (QI) interventions versus usual care and their effects on patient employment. Matched primary care practices were randomly assigned to provide usual care or to 1 of 2 interventions offering training to practice nurses, enhanced educational resources, and either nurses for monitoring of medication adherence (QI-meds) or trained psychotherapists (QI-therapy). Mean total medical costs were 11% higher for QI-meds participants and 13% higher for QI-therapy participants versus usual care patients. However, QI-meds participants had 17.9 more employed days and QI-therapy participants had 20.9 more employed days compared with usual care participants over 24 months (P = .07 and P = .03, respectively).36 Thus, implementation of QI interventions may be a cost-effective way to help primary care organizations provide guideline-concordant care for patients with MDD.
Challenges in the Implementation of Depression Management Guidelines
Existing practice guidelines generally address clinical issues (eg, treatment selection and duration, frequency of follow-up) rather than implementation or quality of care.37 However, treatment guidelines are not necessarily reflected in clinical practice. Results of the National Comorbidity Survey Replication showed that over 12 months, only 51.6% of patients with MDD received any treatment at all, and only 41.9% received treatment considered adequate (4 outpatient visits for psychopharmacology or ≥ 8 outpatient visits with any mental health professional lasting ≥ 30 minutes).38 Implementation of current treatment guidelines may fall short because MDD is not recognized as a disease requiring chronic care strategies for successful treatment outcomes; additional barriers to depression care involve patients, health care professionals, the medical system, and financial constraints.
Rates of patient adherence to antidepressant treatment are inadequate,39-42 and nonadherence is common across all classes of prescribed antidepressants.43,44 A prospective, naturalistic cohort study42 showed that 49% of patients with a new episode of MDD discontinued treatment prematurely and that 33% of premature discontinuations occurred during the acute phase of treatment. Only 25%-50% of primary care patients adhere to antidepressant treatment for the duration of time recommended by treatment guidelines,33 and 15% of patients never start treatment with the prescribed medication.45
Many patients do not adhere to treatment recommendations because they lack sufficient knowledge of depression and treatment options. Melartin et al42 demonstrated that patients with negative attitudes toward treatment at 18 months reported nonadherence to antidepressants significantly more often versus patients with positive or neutral attitudes (79% vs 20%, respectively; P < .001). The most frequently reported reasons for negative attitudes were fears of dependence on medication (43%) and adverse effects (41%). Demyttenaere and colleagues40 found that 53% of patients discontinued antidepressant treatment after 6 months. The most frequently cited reasons for dropping out were feeling better (55%) and adverse events (23%).
Medical system barriers to depression care include inadequate patient monitoring and minimal time to educate patients or to support behavioral changes.6 The National Depressive and Manic-Depressive Association identified characteristics of health care providers contributing to undertreated depression as poor professional education about depression, limited training in interpersonal skills, inadequate time to evaluate and treat depression, failure to consider psychotherapeutic approaches, and prescribing inadequate doses of antidepressant treatments for inadequate durations.12 Indeed, chronically ill patients often receive brief, infrequent visits with the physician that are far below the minimum standard.9,46 Bull et al45 evaluated predictors of premature treatment discontinuation in patients with MDD and found that patients with ≥ 3 depression-related follow-up visits within 120 days of initiating antidepressant medication were significantly more likely to continue antidepressant therapy versus patients with < 3 follow-up visits (P = .002). Lin and colleagues41 showed that patients who received more educational messages from primary care physicians regarding antidepressant treatment were more likely to adhere to medication than those who did not receive such communication. Thus, more frequent patient-physician contact may increase the likelihood that depressed patients will continue antidepressant therapy. Smolders and colleagues47 identified several practice and professional characteristics that were significantly associated with guideline adherence. Higher rates of guideline adherence were associated with the health care professionals’ stronger confidence in depression identification, collaboration with mental health specialists, and fewer perceived barriers for guideline implementation after controlling for patient characteristics.47
Organizational issues also serve as barriers to improving quality of depression care.6 A need exists for information technology (eg, electronic records) to maintain consistency in delivery of medical care. In addition, there is a lack of disease registries that would allow monitoring of patient adherence and treatment outcomes. Few studies have evaluated organizational changes to improve treatment outcomes in depression. The Veterans Administration (VA) Quality Enhancement Research Initiative is a strategically focused, population-based system that utilizes information technology, goal setting, monitoring of treatment outcomes, and technical assistance to support quality of care among patients with MDD and schizophrenia.48 In this regard, Shortell and colleagues49 observed that the use of chronic disease management strategies increased substantially in organizations that received financial rewards for quality, participated in QI programs, had electronic medical records in place, and were profitable.
Legal barriers can also impede improvement in the quality of depression care.50 Confidentiality laws relevant to mental health can be more restrictive than those pertaining to physical health, creating a significant hurdle in terms of sharing relevant clinical information between mental health and primary care providers. Further, fulfilling the requirements of these laws is time consuming and associated with significant financial burden for the practice. A lack of incentive to improve communication between specialty and primary care providers contributes to an isolated approach to mental health care.
Financial and payment system barriers to implementing quality care also present challenges. For example, state and private payers often have different policies and reimbursement codes based on the specialty of the provider. With regard to the patient, public and private insurance carriers vary widely in their mental health coverage, copayments, and requirements for prior authorization.50 Limitations on coverage leading to potentially greater out-of-pocket costs for the patient (eg, higher copayments for mental health services or restricting the number of covered visits per year) or policies that create inconveniences (eg, the need to schedule appointments on different days because the carrier does not allow billing of a therapy visit on the same day as an evaluation and management visit) can be frustrating for patients. Steps to improving financial constraints at the provider level should include the restructuring of financial incentives and reimbursement plans so that a collaboration of physician services would include additional therapy and medical code funding.50 Policies requiring parity in terms of health plan coverage of and reimbursement for mental health services (eg, the Medicare Improvements for Patients and Providers Act50) may help to mitigate financial barriers at both the provider and the patient level.
Collaborative Care Model for Management of MDD
Collaborative care involves a greater role for a structured team of care managers and psychiatrists working with primary care physicians to augment the quality of primary care. Collaborative care interventions reorganize clinical practice to include (1) a clear definition of the clinical problem, (2) development of a care plan with specific goals and implementation strategies, (3) support for self-management training, (4) sustained patient follow-up,6 and (5) decision support from psychiatrists regarding medication changes.
Gilbody et al51 conducted a meta-analysis of 37 randomized, controlled trials that compared collaborative care interventions with usual primary care in depressed patients (N = 12,355). A positive effect of collaborative care on standard depression outcomes was observed at 6 months (standardized mean difference [SMD] = 0.25; [95% CL, 0.18, 0.32]) and up to 5 years in some studies (SMD = 0.15; [95% CL, 0.001, 0.30]). Characteristics associated with the most effective collaborative care programs were improvement in antidepressant adherence, use of mental health specialists as depression case managers, and regular psychiatric supervision.51 The authors noted that, although collaborative care trials of the late 1980s and early 1990s had a high degree of heterogeneity with many negative results, more positive studies emerged in the mid 1990s, and sufficient evidence accumulated by 2000 that demonstrated the consistent and statistically significant benefit of collaborative care versus standard care. The overall effect size for collaborative care has remained consistent (SMD = 0.20-0.29), indicating that there are adequate data for the focus on collaborative care to transition from research to implementation.51
Katon and colleagues7 assessed the effectiveness of a primary care collaborative intervention, which included increased patient education, more frequent office visits, monitoring of treatment adherence, training of primary care physicians in the treatment of depression, and 2 to 3 visits of shared care with a psychiatrist. Intervention participants had significant improvements in treatment adherence, satisfaction with depression treatment, and clinical outcomes versus usual care patients (P < .01 for each measure).7
Simon et al34 evaluated the cost-effectiveness of a stepped collaborative care program versus usual care for primary care patients with persistent MDD following 6 to 8 weeks of antidepressant treatment. The program included systematic patient education, initial visit with a psychiatrist, 2 to 4 months of shared care with the psychiatrist and primary care physician, and monitoring of follow-up visits and medication adherence. Collaborative care patients (n = 110) experienced 16.7 additional depression-free days over 6 months versus usual care patients (n = 109).34 The incremental cost-effectiveness of collaborative care treatment was $21.44 per depression-free day.
Additional, larger, randomized controlled clinical trials of collaborative care interventions relevant to MDD include the Improving Mood-Promoting Access to Collaborative Treatment (IMPACT),52 Prevention of Suicide in Primary Care Elderly: Collaborative Trial (PROSPECT),53 Pathways,54 and Re-Engineering Systems for the Treatment of Depression in Primary Care (RESPECT)55studies.
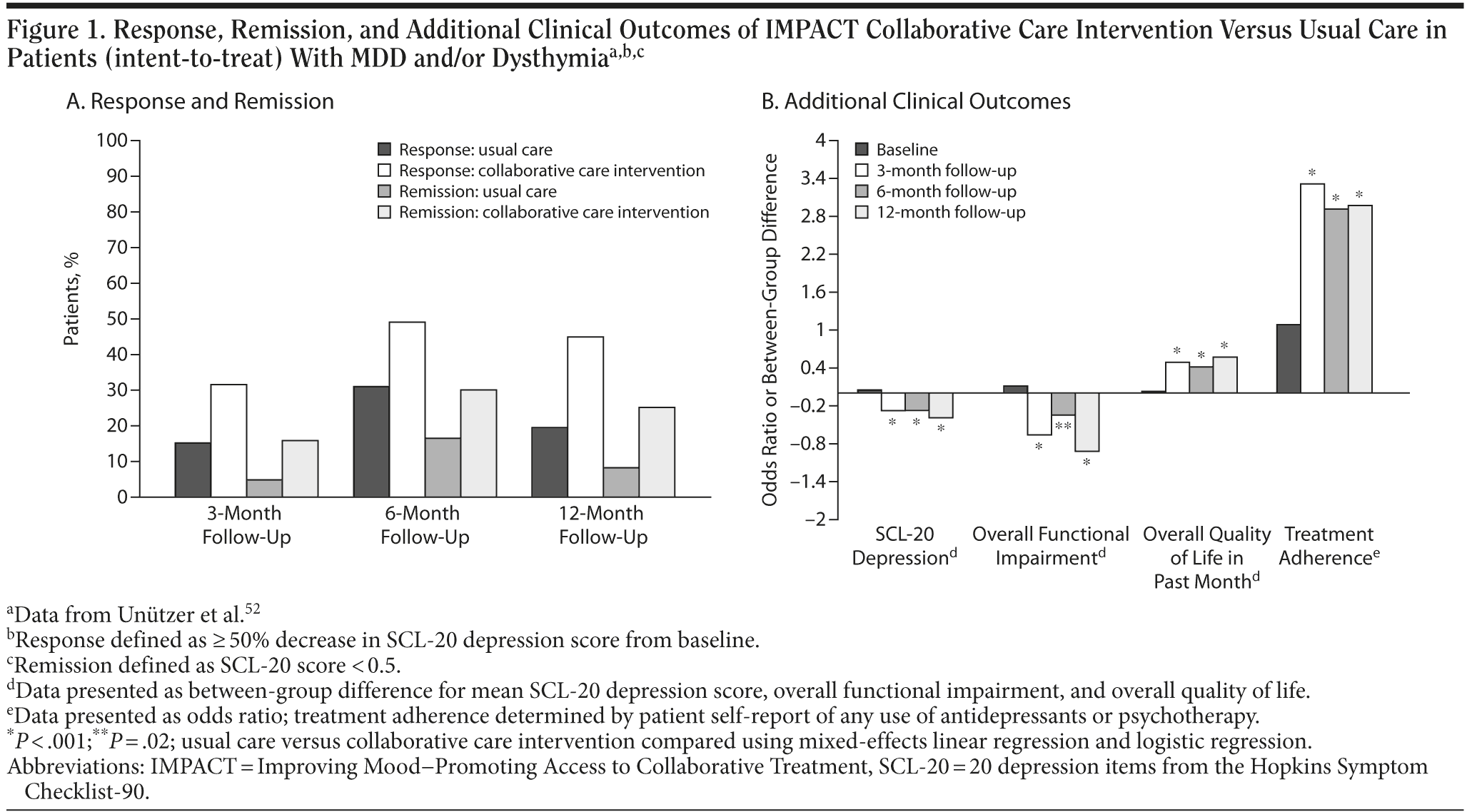
The IMPACT study52 assessed the effectiveness of a collaborative care program for late-life depression in elderly patients aged ≥ 60 years with MDD (17%), dysthymic disorder (30%), or both (53%). Patients received usual care (n = 895) or the IMPACT intervention (n = 906), which included access (for up to 12 months) to a depression care manager, who provided an initial choice of antidepressant medication or problem-solving therapy. The depression care manager carefully tracked patient symptoms with the 9-item Patient Heath Questionnaire56 and received weekly supervision by a psychiatrist. At all follow-up points, intervention participants had significantly better medication adherence, as measured by patient self-report, and lower depression severity, as measured by the 20 items from the Hopkins Symptom Checklist-90 (SCL-20)57 total depression scores, versus usual care participants (P < .001).52 At the 12-month follow-up, intervention participants had significantly higher rates of treatment response (≥ 50% reduction in SCL-20 score from baseline) and complete remission (SCL-20 score < 0.5) versus usual care participants (P < .001 for each comparison; Figure 1).52 Intervention participants also had less functional impairment (P < .001) and greater quality of life versus usual care participants (P < .001; Figure 1). During the final sessions with patients, depression care managers developed a relapse prevention plan that identified prodromal symptoms of relapse, length of time to remain on antidepressants, methods to track depression symptoms, stress reduction techniques, and a professional to contact if symptoms recurred.58 At the 24-month follow-up, intervention patients continued to show improvements in depressive symptoms versus usual care patients, suggesting that the relapse prevention plan was effective.59
The PROSPECT study53 evaluated the effect of a primary care intervention on suicidal ideation and depression in older patients with MDD (N = 598). The PROSPECT intervention included (1) physician knowledge, which was addressed by a clinical algorithm for treating geriatric depression in a primary care setting, and (2) treatment management, including a choice of medication or brief interpersonal psychotherapy, directed by depression care managers supervised weekly by psychiatrists. Rates of suicidal ideation were significantly reduced for intervention participants versus usual care patients at 4 and 8 months (P = .01 and P = .003, respectively). Intervention patients had a greater reduction in depression severity versus usual care patients at 4-, 8-, and 12-month assessments (P < .001, P < .001, and P = .006, respectively) on the basis of 17-item Hamilton Depression Rating Scale60 total scores. The authors concluded that collaborative interventions to improve the quality of care for geriatric patients with depression can effectively reduce depressive symptoms and the risk of suicide late in life.
In the RESPECT trial,55 depression care managers supervised by psychiatrists provided telephone support and enhanced education to patients with MDD, tracked symptoms and adverse effects, encouraged treatment adherence, and facilitated return visits to primary care physicians with recommendations on changing medication based on psychiatric supervision. This collaborative intervention enhanced quality of care and outcomes over a 6-month period versus usual care.55
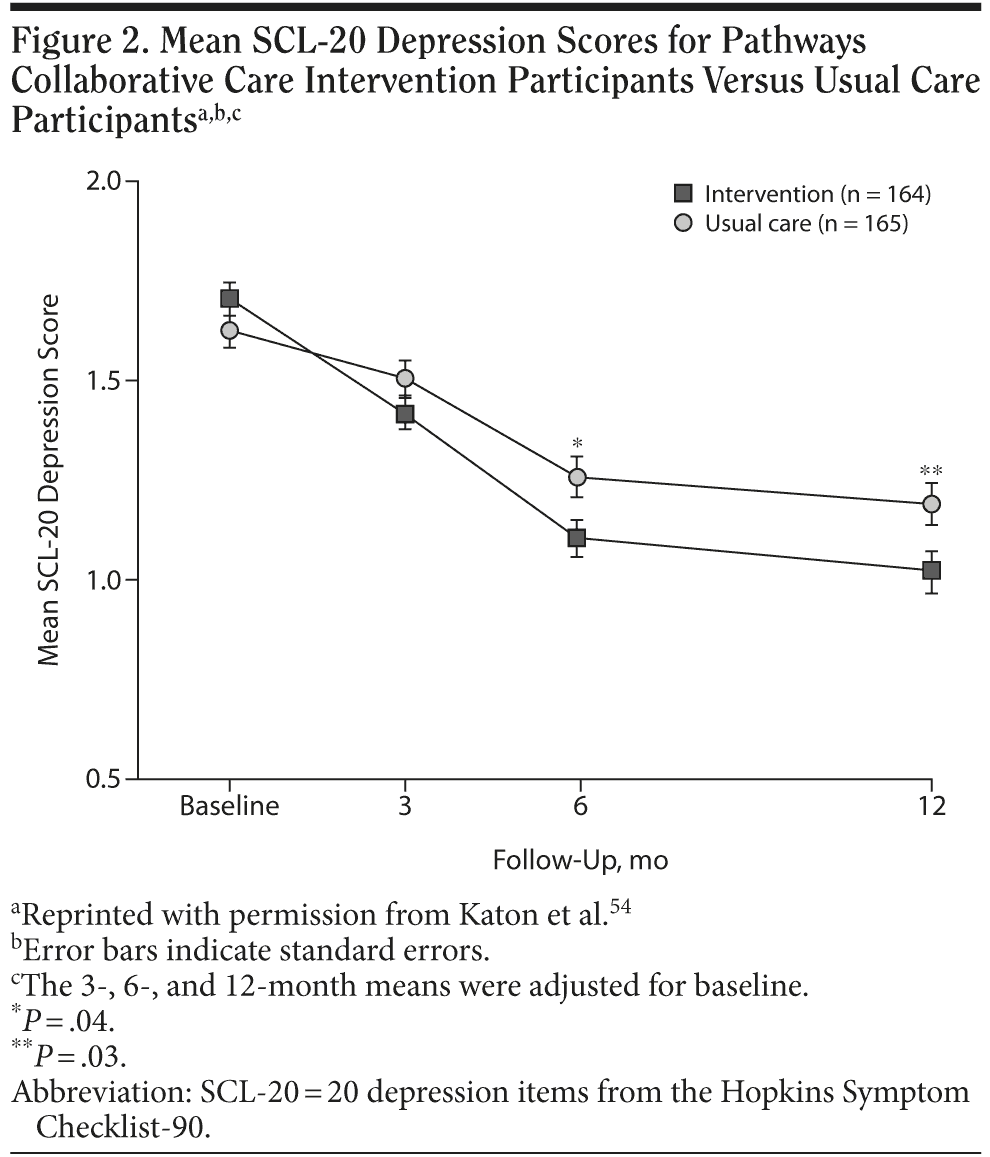
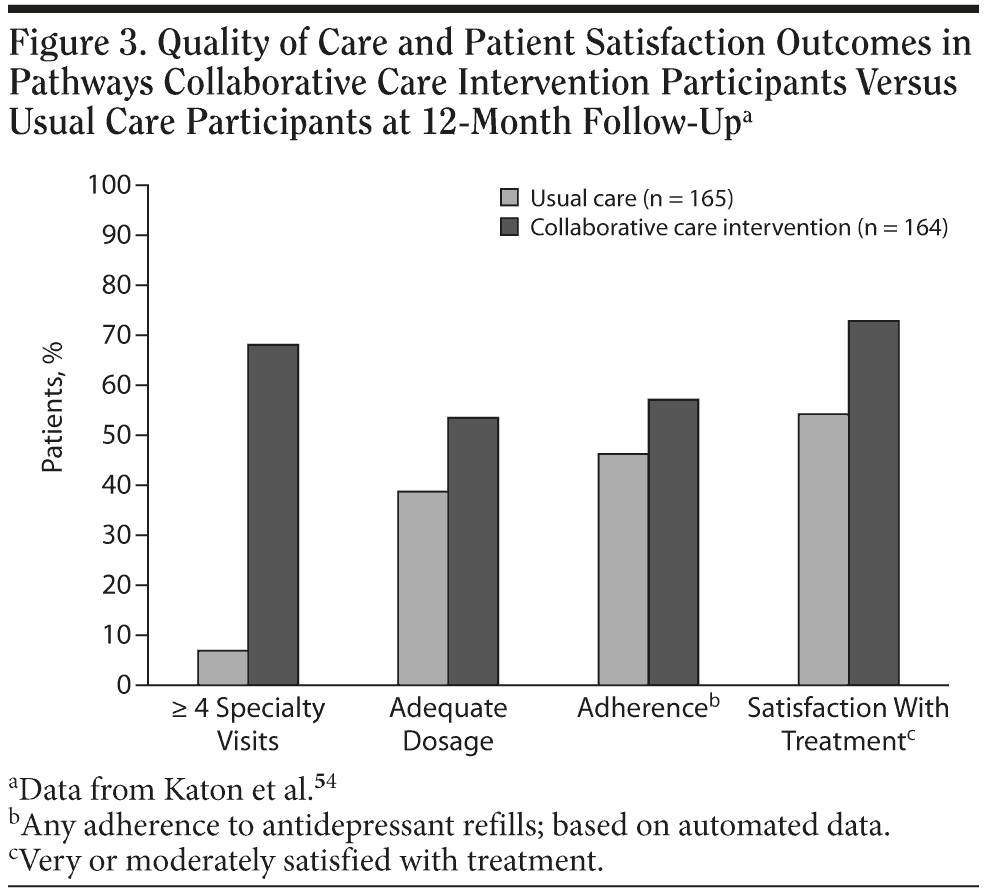
The Pathways clinical trial54 assessed whether collaborative care intervention improved treatment outcomes in primary care patients with depression and diabetes. Patients with diabetes mellitus and comorbid MDD and/or dysthymia received usual care (n = 165) or Pathways intervention (n = 164), a stepped-care program provided by a depression clinical specialist nurse (who had weekly psychiatric supervision) in collaboration with the primary care physician. Patients were offered a choice of psychotherapy or antidepressant treatment. Compared with usual care participants, intervention patients had significantly lower adjusted mean SCL-20 scores at 6-month and 12-month assessments (P = .04 and P = .03, respectively; Figure 2). A significantly higher percentage of intervention patients versus usual care patients had greater improvement in adequacy of antidepressant dosage during the first 6 months of treatment (57% vs 40%; OR = 4.15; 95% CL, 2.28, 7.55) and greater satisfaction with treatment at 12 months (73% vs 54%; OR = 2.88; 95% CL, 1.67, 4.97; Figure 3).54 The Pathways intervention demonstrated a cost-offset effect, such that the associated increased mental health care costs were offset by greater savings in total medical costs over a 2-year period.61
The demonstrated success of collaborative care models in improving quality of care and depressive outcomes has resulted in implementation of evidence-based collaborative care programs for depression by large health care organizations in the United States.62 Examples within primary care include the Veterans Affairs (VA) project Translating Initiatives for Depression into Effective Solutions (TIDES)63 and the Depression Improvement Across Minnesota, Offering a New Direction (DIAMOND) program.64
The TIDES project was designed to adapt collaborative care models for patients with depression to VA settings, support and assess these interventions, and disseminate the program throughout the VA.48 The TIDES program has resulted in positive treatment outcomes, including substantial improvements in treatment adherence, and follow-up visits and notable, sustained improvements in depression severity and functional impairment scores after 6 months.63 The DIAMOND project modifies how depression care is both delivered and paid for, making the roles of care manager and consulting psychiatrist reimbursable. Over 2,400 patients have enrolled in the DIAMOND program, and after 6 months of collaborative care, 43% were in remission and 60% had experienced a ≥ 50% reduction in the severity of depressive symptoms.64
The goal of achieving remission and preventing relapse in patients with MDD is challenging, and the consequences associated with failure to achieve and maintain remission underscore the importance of ensuring the highest quality patient care. Although a focus on implementation and delivery of quality care consistent with treatment guidelines is effective in improving outcomes, programs that provide incentives specifically for achieving treatment outcomes may also be of benefit. The Bridges to Excellence program65 is an example of a collaborative care program that emphasizes remission as the goal of treatment in patients with MDD. This program provides financial rewards to physicians who achieve high rates of remission in their clinical practices.65,66 While it is premature to determine if these incentives will result in a substantial improvement in quality of depression care, the association of potential rewards with rates of remission is an important experiment in exploring changes in incentives.
CONCLUSION
An unmet need exists for improvement in mental heath care in the United States, as growing evidence indicates that mental health disorders are as disabling as cancer or heart disease with regard to lost productivity and premature death.50 A collaborative care model is the optimal approach to treatment of MDD, a chronic disorder with no cure and a high likelihood of repeated symptomatic episodes, but for which numerous interventions that provide relief of symptoms are available. Successful treatment of MDD requires collaboration between primary care and mental health specialists, structured symptom monitoring to guide treatment, and ongoing support for patient self-management.
Collaborative care models have demonstrated improved treatment outcomes for patients with MDD in primary care settings, with overall outcome differences between intervention and usual care approaching 30%. Benefits of collaborative care include reduced financial burden, substantial increases in treatment adherence, and long-term improvement in depression symptoms and functional outcomes. We now have sufficient evidence demonstrating the effectiveness of an organized system of care to adopt and implement collaborative care models for the treatment of patients with MDD.
Author affiliations: University of Washington Medical School, Seattle (Dr Katon); and Pfizer Inc, formerly Wyeth Research, Collegeville, Pennsylvania (Dr Guico-Pabia).
Potential conflicts of interest: Dr Katon has received honoraria from Eli Lilly, Forest, Pfizer, and Wyeth and has served on the advisory boards of Eli Lilly and Pfizer. Dr Guico-Pabia is an employee of Pfizer.
Funding/support: This analysis was sponsored by Wyeth Research, Collegeville, Pennsylvania, which was acquired by Pfizer Inc in October 2009. Medical writing support for this manuscript was funded by Wyeth and provided by Callie Grimes, PhD, of Embryon, LLC (Somerville, New Jersey), A Division of Advanced Health Media, LLC (formerly Medesta Publications Group, A Business of Advogent).
REFERENCES
1. American Psychiatric Association. Diagnostic and Statistical Manual of Mental Disorders, Fourth Edition. Washington, DC: American Psychiatric Association; 1994.
2. Simon GE. Evidence review: efficacy and effectiveness of antidepressant treatment in primary care. Gen Hosp Psychiatry. 2002;24(4):213-224. PubMed doi:10.1016/S0163-8343(02)00198-6
3. Katon WJ, Simon G, Russo J, et al. Quality of depression care in a population-based sample of patients with diabetes and major depression. Med Care. 2004;42(12):1222-1229. PubMed doi:10.1097/00005650-200412000-00009
4. American Psychiatric Association. Practice Guideline for the Treatment of Patients With Major Depressive Disorder (revision). Am J Psychiatry. 2000;157(4 suppl):1-45. PubMed
5. Agency for Health Care Policy and Research. Clinical Practice Guideline Number 5; Volume 2: Treatment of Major Depression, 1993. http://www.ncbi.nlm.nih.gov/bookshelf/br.fcgi?book=hsarchive&part=A15593. Accessed June 2, 2010.
6. Katon WJ. The Institute of Medicine “Chasm” report: implications for depression collaborative care models. Gen Hosp Psychiatry. 2003;25(4):222-229. PubMed doi:10.1016/S0163-8343(03)00064-1
7. Katon W, Von Korff M, Lin E, et al. Collaborative management to achieve treatment guidelines: impact on depression in primary care. JAMA. 1995;273(13):1026-1031. PubMed doi:10.1001/jama.273.13.1026
8. Katon W, Von Korff M, Lin E, et al. Population-based care of depression: effective disease management strategies to decrease prevalence. Gen Hosp Psychiatry. 1997;19(3):169-178. PubMed doi:10.1016/S0163-8343(97)00016-9
9. Von Korff M, Gruman J, Schaefer J, et al. Collaborative management of chronic illness. Ann Intern Med. 1997;127(12):1097-1102. PubMed
10. Trivedi MH, Lin EH, Katon WJ. Consensus Recommendations for Improving Adherence, Self-Management, and Outcomes in Patients With Depression. CNS Spectr. 2007;12(suppl 13):1-27. PubMed
11. Furukawa TA, Yoshimura R, Harai H, et al. How many well vs unwell days can you expect over 10 years, once you become depressed? Acta Psychiatr Scand. 2009;119(4):290-297. PubMed doi:10.1111/j.1600-0447.2008.01288.x
12. Hirschfeld RM, Keller MB, Panico S, et al. The National Depressive and Manic-Depressive Association consensus statement on the undertreatment of depression. JAMA. 1997;277(4):333-340. PubMed doi:10.1001/jama.277.4.333
13. Wells KB, Stewart A, Hays RD, et al. The functioning and well-being of depressed patients: results from the Medical Outcomes Study. JAMA. 1989;262(7):914-919. PubMed doi:10.1001/jama.262.7.914
14. Hays RD, Wells KB, Sherbourne CD, et al. Functioning and well-being outcomes of patients with depression compared with chronic general medical illnesses. Arch Gen Psychiatry. 1995;52(1):11-19. PubMed
15. Ormel J, Petukhova M, Chatterji S, et al. Disability and treatment of specific mental and physical disorders across the world. Br J Psychiatry. 2008;192(5):368-375. PubMed doi:10.1192/bjp.bp.107.039107
16. Möller HJ. Outcomes in major depressive disorder: the evolving concept of remission and its implications for treatment. World J Biol Psychiatry. 2008;9(2):102-114. PubMed doi:10.1080/15622970801981606
17. Judd LL, Akiskal HS, Zeller PJ, et al. Psychosocial disability during the long-term course of unipolar major depressive disorder. Arch Gen Psychiatry. 2000;57(4):375-380. PubMed doi:10.1001/archpsyc.57.4.375
18. Moussavi S, Chatterji S, Verdes E, et al. Depression, chronic diseases, and decrements in health: results from the World Health Surveys. Lancet. 2007;370(9590):851-858. PubMed doi:10.1016/S0140-6736(07)61415-9
19. Halaris A. Comorbidity between depression and cardiovascular disease. Int Angiol. 2009;28(2):92-99. PubMed
20. Knol MJ, Twisk JW, Beekman AT, et al. Depression as a risk factor for the onset of type 2 diabetes mellitus: a meta-analysis. Diabetologia. 2006;49(5):837-845. PubMed doi:10.1007/s00125-006-0159-x
21. Xu W, Collet JP, Shapiro S, et al. Independent effect of depression and anxiety on chronic obstructive pulmonary disease exacerbations and hospitalizations. Am J Respir Crit Care Med. 2008;178(9):913-920. PubMed doi:10.1164/rccm.200804-619OC
22. Mancuso CA, Wenderoth S, Westermann H, et al. Patient-reported and physician-reported depressive conditions in relation to asthma severity and control. Chest. 2008;133(5):1142-1148. PubMed doi:10.1378/chest.07-2243
23. DiMatteo MR, Lepper HS, Croghan TW. Depression is a risk factor for noncompliance with medical treatment: meta-analysis of the effects of anxiety and depression on patient adherence. Arch Intern Med. 2000;160(14):2101-2107. PubMed doi:10.1001/archinte.160.14.2101
24. Lin EH, Heckbert SR, Rutter CM, et al. Depression and increased mortality in diabetes: unexpected causes of death. Ann Fam Med. 2009;7(5):414-421. PubMed doi:10.1370/afm.998
25. Ang DC, Choi H, Kroenke K, et al. Comorbid depression is an independent risk factor for mortality in patients with rheumatoid arthritis. J Rheumatol. 2005;32(6):1013-1019. PubMed
26. Bush DE, Ziegelstein RC, Tayback M, et al. Even minimal symptoms of depression increase mortality risk after acute myocardial infarction. Am J Cardiol. 2001;88(4):337-341. PubMed doi:10.1016/S0002-9149(01)01675-7
27. Barefoot JC, Helms MJ, Mark DB, et al. Depression and long-term mortality risk in patients with coronary artery disease. Am J Cardiol. 1996;78(6):613-617. PubMed doi:10.1016/S0002-9149(96)00380-3
28. Un×¼tzer J, Patrick DL, Simon G, et al. Depressive symptoms and the cost of health services in HMO patients aged 65 years and older: a 4-year prospective study. JAMA. 1997;277(20):1618-1623. PubMed doi:10.1001/jama.277.20.1618
29. Simon GE, VonKorff M, Barlow W. Health care costs of primary care patients with recognized depression. Arch Gen Psychiatry. 1995;52(10):850-856. PubMed
30. Simon GE, Barber C, Birnbaum HG, et al. Depression and work productivity: the comparative costs of treatment versus nontreatment. J Occup Environ Med. 2001;43(1):2-9. PubMed doi:10.1097/00043764-200101000-00002
31. Lurie IZ, Manheim LM, Dunlop DD. Differences in medical care expenditures for adults with depression compared to adults with major chronic conditions. J Ment Health Policy Econ. 2009;12(2):87-95. PubMed
32. Von Korff M, Katon W, Bush T, et al. Treatment costs, cost offset, and cost-effectiveness of collaborative management of depression. Psychosom Med. 1998;60(2):143-149. PubMed
33. Katon W, Von Korff M, Lin E, et al. Rethinking practitioner roles in chronic illness: the specialist, primary care physician, and the practice nurse. Gen Hosp Psychiatry. 2001;23(3):138-144. PubMed doi:10.1016/S0163-8343(01)00136-0
34. Simon GE, Katon WJ, VonKorff M, et al. Cost-effectiveness of a collaborative care program for primary care patients with persistent depression. Am J Psychiatry. 2001;158(10):1638-1644. PubMed doi:10.1176/appi.ajp.158.10.1638
35. Simon GE, Von Korff M, Ludman EJ, et al. Cost-effectiveness of a program to prevent depression relapse in primary care. Med Care. 2002;40(10):941-950. PubMed doi:10.1097/00005650-200210000-00011
36. Schoenbaum M, Un×¼tzer J, Sherbourne C, et al. Cost-effectiveness of practice-initiated quality improvement for depression: results of a randomized controlled trial. JAMA. 2001;286(11):1325-1330. PubMed doi:10.1001/jama.286.11.1325
37. Qaseem A, Snow V, Denberg TD, et al; Clinical Efficacy Assessment Subcommittee of American College of Physicians. Using second-generation antidepressants to treat depressive disorders: a clinical practice guideline from the American College of Physicians. Ann Intern Med. 2008;149(10):725-733. PubMed
38. Kessler RC, Berglund P, Demler O, et al; National Comorbidity Survey Replication. The epidemiology of major depressive disorder: results from the National Comorbidity Survey Replication (NCS-R). JAMA. 2003;289(23):3095-3105. PubMed doi:10.1001/jama.289.23.3095
39. Kobak KA, Taylor L, Katzelnick DJ, et al. Antidepressant medication management and Health Plan Employer Data Information Set (HEDIS) criteria: reasons for nonadherence. J Clin Psychiatry. 2002;63(8):727-732. PubMed
40. Demyttenaere K, Enzlin P, Dewé W, et al. Compliance with antidepressants in a primary care setting, 1: beyond lack of efficacy and adverse events. J Clin Psychiatry. 2001;62(suppl 22):30-33. PubMed
41. Lin EH, Von Korff M, Katon W, et al. The role of the primary care physician in patients’ adherence to antidepressant therapy. Med Care. 1995;33(1):67-74. PubMed doi:10.1097/00005650-199501000-00006
42. Melartin TK, Rytsälä HJ, Leskelä US, et al. Continuity is the main challenge in treating major depressive disorder in psychiatric care. J Clin Psychiatry. 2005;66(2):220-227. PubMed doi:10.4088/JCP.v66n0210
43. Lingam R, Scott J. Treatment non-adherence in affective disorders. Acta Psychiatr Scand. 2002;105(3):164-172. PubMed doi:10.1034/j.1600-0447.2002.1r084.x
44. Pampallona S, Bollini P, Tibaldi G, et al. Patient adherence in the treatment of depression. Br J Psychiatry. 2002;180(2):104-109. PubMed doi:10.1192/bjp.180.2.104
45. Bull SA, Hu XH, Hunkeler EM, et al. Discontinuation of use and switching of antidepressants: influence of patient-physician communication. JAMA. 2002;288(11):1403-1409. PubMed doi:10.1001/jama.288.11.1403
46. Wagner EH, Austin BT, Von Korff M. Improving outcomes in chronic illness. Manag Care Q. 1996;4(2):12-25. PubMed
47. Smolders M, Laurant M, Verhaak P, et al. Which physician and practice characteristics are associated with adherence to evidence-based guidelines for depressive and anxiety disorders? Med Care. 2010;48(3):240-248. PubMed doi:10.1097/MLR.0b013e3181ca27f6
48. Owen RR, Cannon D, Thrush CR; Quality Enhancement Research Initiative. Mental Health QUERI Initiative: expert ratings of criteria to assess performance for major depressive disorder and schizophrenia. Am J Med Qual. 2003;18(1):15-20. PubMed doi:10.1177/106286060301800104
49. Shortell SM, Gillies R, Siddique J, et al. Improving chronic illness care: a longitudinal cohort analysis of large physician organizations. Med Care. 2009;47(9):932-939. PubMed doi:10.1097/MLR.0b013e31819a621a
50. Collins C, Hewson DL, Munger R, et al. Evolving Models of Behavioral Health Integration in Primary Care. New York, NY: Milbank Memorial Fund; 2010.
51. Gilbody S, Bower P, Fletcher J, et al. Collaborative care for depression: a cumulative meta-analysis and review of longer-term outcomes. Arch Intern Med. 2006;166(21):2314-2321. PubMed doi:10.1001/archinte.166.21.2314
52. Un×¼tzer J, Katon W, Callahan CM, et al; IMPACT Investigators. Improving Mood-Promoting Access to Collaborative Treatment. Collaborative care management of late-life depression in the primary care setting: a randomized controlled trial. JAMA. 2002;288(22):2836-2845. PubMed doi:10.1001/jama.288.22.2836
53. Bruce ML, Ten Have TR, Reynolds CF 3rd, et al. Reducing suicidal ideation and depressive symptoms in depressed older primary care patients: a randomized controlled trial. JAMA. 2004;291(9):1081-1091. PubMed doi:10.1001/jama.291.9.1081
54. Katon WJ, Von Korff M, Lin EH, et al. The Pathways Study: a randomized trial of collaborative care in patients with diabetes and depression. Arch Gen Psychiatry. 2004;61(10):1042-1049. PubMed doi:10.1001/archpsyc.61.10.1042
55. Dietrich AJ, Oxman TE, Williams JW Jr, et al. Re-engineering systems for the treatment of depression in primary care: cluster randomised controlled trial. BMJ. 2004;329(7466):602. PubMed doi:10.1136/bmj.38219.481250.55
56. Kroenke K, Spitzer RL, Williams JB. The PHQ-9: validity of a brief depression severity measure. J Gen Intern Med. 2001;16(9):606-613. PubMed doi:10.1046/j.1525-1497.2001.016009606.x
57. Williams JW Jr, Stellato CP, Cornell J, et al. The 13- and 20-item Hopkins Symptom Checklist Depression Scale: psychometric properties in primary care patients with minor depression or dysthymia. Int J Psychiatry Med. 2004;34(1):37-50. PubMed doi:10.2190/U1B0-NKWC-568V-4MAK
58. Katon W, Rutter C, Ludman EJ, et al. A randomized trial of relapse prevention of depression in primary care. Arch Gen Psychiatry. 2001;58(3):241-247. PubMed doi:10.1001/archpsyc.58.3.241
59. Hunkeler EM, Katon W, Tang L, et al. Long term outcomes from the IMPACT randomised trial for depressed elderly patients in primary care. BMJ. 2006;332(7536):259-263. PubMed doi:10.1136/bmj.38683.710255.BE
60. Hamilton M. A rating scale for depression. J Neurol Neurosurg Psychiatry. 1960;23(1):56-62. PubMed doi:10.1136/jnnp.23.1.56
61. Simon GE, Katon WJ, Lin EH, et al. Cost-effectiveness of systematic depression treatment among people with diabetes mellitus. Arch Gen Psychiatry. 2007;64(1):65-72. PubMed doi:10.1001/archpsyc.64.1.65
62. Katon WJ, Un×¼tzer J. Pebbles in a pond: NIMH grants stimulate improvements in primary care treatment of depression. Gen Hosp Psychiatry. 2006;28(3):185-188. PubMed doi:10.1016/j.genhosppsych.2006.01.004
63. Rubenstein L, Chaney EF, Williams J, et al. Collaborative treatment for depression. VA Practice Matters. 2004;9:1-6.
64. Institute for Clinical Systems Improvement. DIAMOND Fact Sheet. http://www.icsi.org/health_care_redesign_/diamond_35953/diamond_fact_sheet/. Updated August 5, 2009. Accessed October 22, 2010.
65. Depression Care Recognition Program. Bridges to Excellence. http://www.bridgestoexcellence.org/Content/ContentDisplay67b2.html?ContentID=44. Accessed January 19, 2011.
66. de Brantes F, Rosenthal MB, Painter M. Building a bridge from fragmentation to accountability: the Prometheus Payment model. N Engl J Med. 2009;361(11):1033-1036. doi: 10.1056/NEJMp0906121 PubMed