Prevalence and Correlates of Clinically Significant Depressive Symptoms in an Urban Hospital Emergency Department
CME Background
Articles are selected for credit designation based on an assessment of the educational needs of CME participants, with the purpose of providing readers with a curriculum of CME articles on a variety of topics throughout each volume. Activities are planned using a process that links identified needs with desired results.
To obtain credit, read the material and go to PSYCHIATRIST.COM to complete the Posttest and Evaluation online.
CME Objective
After studying this article, you should be able to:
- Identify emergency department patients with clinically significant depressive symptoms and facilitate their referral and treatment
Accreditation Statement
The CME Institute of Physicians Postgraduate Press, Inc., is accredited by the Accreditation Council for Continuing Medical Education to provide continuing medical education for physicians.
Credit Designation
The CME Institute of Physicians Postgraduate Press, Inc., designates this educational activity for a maximum of 1.5 AMA PRA Category 1 Creditsâ„¢. Physicians should only claim credit commensurate with the extent of their participation in the activity.
Date of Original Release/Review
This educational activity is eligible for AMA PRA Category 1 Credit through April 30, 2013. The latest review of this material was March 2010.
Financial Disclosure
All individuals in a position to control the content of this CME activity were asked to complete a statement regarding all relevant personal financial relationships between themselves or their spouse/partner and any commercial interest. The CME Institute has resolved any conflicts of interest that were identified. In the past 3 years, Larry Culpepper, MD, MPH, Editor in Chief, has been a consultant and a member of the advisory boards for AstraZeneca, Cephalon, Forest, Pfizer, Wyeth, Eli Lilly, Takeda, Merck, Neurocrine, sanofi, Bristol-Myers Squibb, and Otsuka and has been a member of the speakers panels for Forest, Wyeth, and Pfizer. No member of the CME Institute staff reported any relevant personal financial relationships. Faculty financial disclosure appears at the end of the article.
Background: In hospital settings, depression is an underdetected, undertreated, but prevalent and interfering illness that is associated with significant disability, morbidity, and mortality. A general hospital emergency department (ED) setting may be well suited to identify individuals with clinically significant depressive symptoms, facilitating their referral and treatment.
Method: Cross-sectional data of adult ED patients in a general hospital enrolling in a human immunodeficiency virus (HIV) screening study between February 2007 and March 2008 were analyzed. Data included demographic factors, the Center for Epidemiologic Studies Depression Scale (CES-D), alcohol and substance use history, sexual risk taking, and brief medical history. The primary outcome was a dichotomous measure of self-reported clinically significant depressive symptoms. Patients who scored ≥ 16 on the CES-D were considered to screen positive for depressive symptoms.
Results: Of the 3,262 patients enrolled in the screening trial, 2,588 (79%) completed the survey between February 2007 and March 2008. Among these, 1,945 (75%) completed the psychosocial assessment battery; 596 (31%) survey completers screened positive for clinically significant depressive symptoms. In a multivariable model, female sex (RR = 1.36; 95% CI, 1.16-1.57), being unemployed (RR = 1.61; 95% CI, 1.32-1.93), and lower annual income (RR from 1.73 to 2.24) were associated with increased rates of clinically significant depressive symptoms (CES-D score ≥ 16). Clinically significant depressive symptoms were more often present in patients who screened positive for alcohol dependence (RR = 1.48; 95% CI, 1.19-1.78), individuals reporting current smoking (RR = 1.39; 95% CI, 1.17-1.62), those with a prior psychiatric disorder diagnosis (RR = 2.20; 95% CI, 1.80-2.57) or history of hypertension (RR = 1.47; 95% CI, 1.18-1.79), and those who reported ever having sex with an HIV-infected partner (RR = 1.58; 95% CI, 1.08-2.09).
Conclusions: This study identified a high frequency of undiagnosed clinically significant depressive symptoms among ED patients and highlights several new demographic and clinical correlates of such symptoms. Screening for and diagnosis of clinical depression in the ED setting introduces important opportunities for acute care providers and for the health care system as a whole.
Prim Care Companion J Clin Psychiatry 2010;12(2):e1-e11
© Copyright 2010 Physicians Postgraduate Press, Inc.
Submitted: March 24, 2009; accepted June 9, 2009.
Published online: April 8, 2010 (doi:10.4088/PCC.09m00817gry).
Corresponding author: Matthew J. Mimiaga, ScD, MPH, Department of Psychiatry, Harvard Medical School, Massachusetts General Hospital, 1 Bowdoin Square, 7th Floor, Boston, MA 02114 ([email protected]).
Although effective treatments for depression exist, including antidepressant medications (eg, selective serotonin reuptake inhibitors, tricyclic antidepressants, and monoamine oxidase inhibitors) and specific psychosocial or psychotherapeutic approaches (eg, behavioral activation, cognitive-behavioral therapy, and interpersonal psychotherapy),1 depression remains substantially underdiagnosed and undertreated. An estimated 30%-50% of patients who suffer from depression go unrecognized and therefore cannot access effective treatment.2,3 Routine screening for depression among adults has been found to improve the identification of patients with depression.4
While efforts have been made to increase awareness of depression in outpatient primary medical settings,3,5-7 less attention has been paid to screening for depression in emergency departments (EDs) in urban hospital settings. Research has documented both the need and desire for preventive health care measures to be initiated or provided as part of ED care, especially among patients without primary physicians.8-12 Emergency departments often serve as a primary or only source of health care for at-risk populations. Specifically, the uninsured, the homeless, the mentally ill, the economically disadvantaged, the elderly, the chronically ill, many ethnic/racial minorities, immigrants, and refugees13-20 are populations that may be at high risk for untreated, but treatable, psychiatric comorbidity. Consequently, for many individuals, the ED may be a rare opportunity to increase the availability of psychiatric services and address depression on a wider scale.
Clinical Points
- Although effective treatments for depression exist, including antidepressant medications (eg, selective serotonin reuptake inhibitors, tricyclic antidepressants, and monoamine oxidase inhibitors) and specific psychosocial or psychotherapeutic approaches (eg, behavioral activation, cognitive-behavioral therapy, and interpersonal psychotherapy), depression remains substantially underdiagnosed and undertreated.
- Screening for clinical depression in the emergency department (ED) setting introduces important opportunities for acute care providers and for the health care system as a whole.
- Screening for depression in the ED setting may increase the recognition and diagnosis of depression, and, when integrated with a commitment to provide coordinated and prompt follow-up of diagnosis and treatment, clinical outcomes could potentially improve.
Emergency room-initiated interventions for depression would require prevalence data in order to more optimally provide appropriate staffing for triage and/or treatment and to aid in sample size calculations for the testing of future randomized controlled intervention trials in this setting. Emergency department interventions would benefit from identification of risk factors associated with clinically significant depressive symptoms, allowing for better prioritization of ED resources. Although the presence of risk factors alone cannot distinguish depressed from nondepressed patients, identifying risk factors for depression may provide valuable information to optimize ED interventions to reach those adults at highest risk. Accordingly, we sought to determine the frequency and risk factors associated with clinically significant depressive symptoms among adult ED patients presenting for care and enrolled in an ED-based human immunodeficiency virus (HIV) screening study at an urban general hospital in Boston, Massachusetts.
METHOD
Study Site
The Brigham and Women’s Hospital (BWH) is an urban general hospital and a 747-bed teaching affiliate of Harvard Medical School in Boston, Massachusetts. The ED staff at BWH sees over 56,000 patients annually, 48% of whom are white, 25% black, and 20% Hispanic. The median age of ED patients is 44 years; approximately 60% are female.
Patient Eligibility
This study was conducted within the National Institutes of Health-funded Universal Screening for HIV Infection in the Emergency Room (USHER) Trial.21 Data for this analysis were collected between February 2007 and March 2008.
Patient eligibility criteria for USHER were (1) aged 18-75 years old; (2) clear mental status (oriented to time, situation, person, and place and no signs of delirium, psychosis, or other mental impairment) and an Emergency Severity Index (ESI) score of 3, 4, or 5 on a scale of 1 (most severe) to 5 (least severe); (3) fluent in English or Spanish; (4) not currently in prenatal care; and (5) not known to be HIV infected.22-24 Participants included 2,588 adult ED patients enrolled in the USHER study. The study has been approved by the BWH Partners Human Research Committee and is overseen by a Data Safety and Monitoring Board. All participants completed an informed consent process.
Study Instruments
Participants completed a self-administered questionnaire available by either paper/pencil or audio computer-assisted self-interview, which included data along the following domains.
Demographics. We requested the following information: patient age, race/ethnicity, gender, education level (divided into 5 categories: graduate/professional degree, college degree, some college, high school degree/general education development [GED], and less than a high school degree), employment status, and annual income.
Depression. Depressive symptoms in the prior week were assessed with the Center for Epidemiologic Studies Depression Scale (CES-D), a validated survey of clinically significant distress as a marker for clinical depression (coefficient α = .90, Cronbach’s α = .89).25-27 The 20 items were scored on a 4-point Likert scale from 0 to 3.
Substance abuse. Current potential alcohol dependence was assessed using the Alcohol Use Disorders Identification Test.28 Total scores of 8 or more are recommended as indicators of hazardous and harmful alcohol use, as well as possible alcohol dependence.28 Patients indicated whether they had ever used drugs in the past (including heroin, cocaine/crack, speed, Oxycontin, poppers, marijuana, lysergic acid diethylamide, Ecstasy, and crystal methamphetamine). Patients were also asked whether they currently smoked, defined as actively smoking at least 1 cigarette per day.
Comorbidities. Patients indicated whether they had ever had a chronic disease diagnosis, including hypertension, diabetes, asthma, cancer, heart disease, stroke, psychiatric disorder, or other. Because psychiatric disorder and hypertension have been associated with depressive symptoms, they were analyzed as distinct categories. Since the same observations were coded as missing for all the chronic diseases in our questionnaire, we created a hierarchical categorical variable for the psychiatric disorder and hypertension comorbidities for modeling purposes. Participants were classified as having psychiatric disorder (with or without hypertension), hypertension alone, not having either disease, or missing. For less frequently reported chronic diseases, we created a summative score and classified patients as having 0, 1, or 2 or more (for diabetes, asthma, cancer, heart disease, stroke, or other).
Sexual behavior. Patients were asked their total number of sexual partners in the 3 months prior to study enrollment, as well as whether they had ever knowingly had sex with an HIV-infected partner.
HIV infection and sexually transmitted infections. Patients indicated whether they had ever been tested for HIV infection and were asked whether they ever had a history of 1 or more viral (herpes simplex virus, human papillomavirus, hepatitis B virus, or hepatitis C virus) and/or bacterial sexually transmitted infections (STIs) (chlamydia, gonorrhea, or syphilis). Patients’ current basic knowledge about HIV infection was also assessed using the validated HIV Knowledge Questionnaire (HIV-KQ-18).29
Analytic Process
Primary outcome. The primary outcome is a dichotomous measure of self-reported clinically significant depressive symptoms. Patients who scored 16 or greater on the CES-D were considered to screen positive for depressive symptoms.25 Because some research has recognized a CES-D score of 27 or greater as indicative of severe depression, we conducted replication analyses using 27 as a secondary outcome (see sensitivity analysis below).30-32
Missing data on primary outcome. For participants who answered all 20 questions, a summative score was created from all 20 CES-D responses. For those patients who answered 16 to 19 of the 20 questions (at least 75%), a score was imputed by summing the score for the questions to which they responded. That score was then divided by the number of answered questions and multiplied by 20 to equalize the scale with those who answered all the questions. Patients answering fewer than 16 questions had their score set to missing.33,34
Data analyses. First, we used a complete case analysis with respect to our primary outcome yielding usable data on 1,945 patients. The initial USHER questionnaire was designed to look at correlates of HIV risk and HIV testing history; we used all of these data to look at depression because we felt they had overlapping constructs. All data collected as part of the USHER assessment were utilized: demographics, chronic disease diagnosis, current and prior substance use, sexual risk, and HIV testing and STI history were examined for their association with depressive symptoms. Unadjusted relative risks (RRs) and their 95% CIs were calculated to examine associations between predictor variables and depressive symptoms. Multivariable logistic regression was performed to adjust for potential confounding. The odds ratios and their 95% CIs were converted to relative risks.35 This procedure is recommended to obtain unbiased estimates of relative risks when the outcome event is common (10% or more).33,34,36
Second, we examined the impact of missing data on results of multivariable analyses. There were 2 sources of missing data for the outcome. The first originated from those patients who did not fill out the self-administered questionnaire at all. To better understand the impact of these missing data, we compared demographics collected for all enrolled patients (age, gender, and race/ethnicity) stratified by whether or not they answered the questionnaire. The second type of missing data was resultant from those patients who filled out the questionnaire but did not answer at least 75% of the questions on the CES-D section of the questionnaire, not allowing for ascertainment of the primary outcome. We examined the impact of such missing data by stratifying the patients who filled out the questionnaire into 3 groups: (1) those with depressive symptoms, (2) those without depressive symptoms, and (3) those with a missing value for depressive symptoms. We then compared this 3-level variable across all other variables described above to see if there were any distributional differences. For all analyses, we included a missing category for the predictors of interest due to a large amount of missing values for some of these variables.
Lastly, we performed 3 sensitivity analyses. We used the more stringent definition of depressive symptoms (CES-D score ≥ 27) to define the outcome of depressive symptoms. The second sensitivity analysis looked at the impact of missing data for our primary outcome of having depressive symptoms (CES-D score ≥ 16). This analysis was performed by assuming that participants with missing data for the primary outcome either did or did not have depressive symptoms. The third sensitivity analysis examined all participants with a missing value for the outcome of clinically significant depressive symptoms who were assumed to not have clinically significant depressive symptoms (CES-D scale score ≥ 16). SAS statistical software version 9.1 (Cary, North Carolina) was used to perform each analysis.
RESULTS
Cohort Description
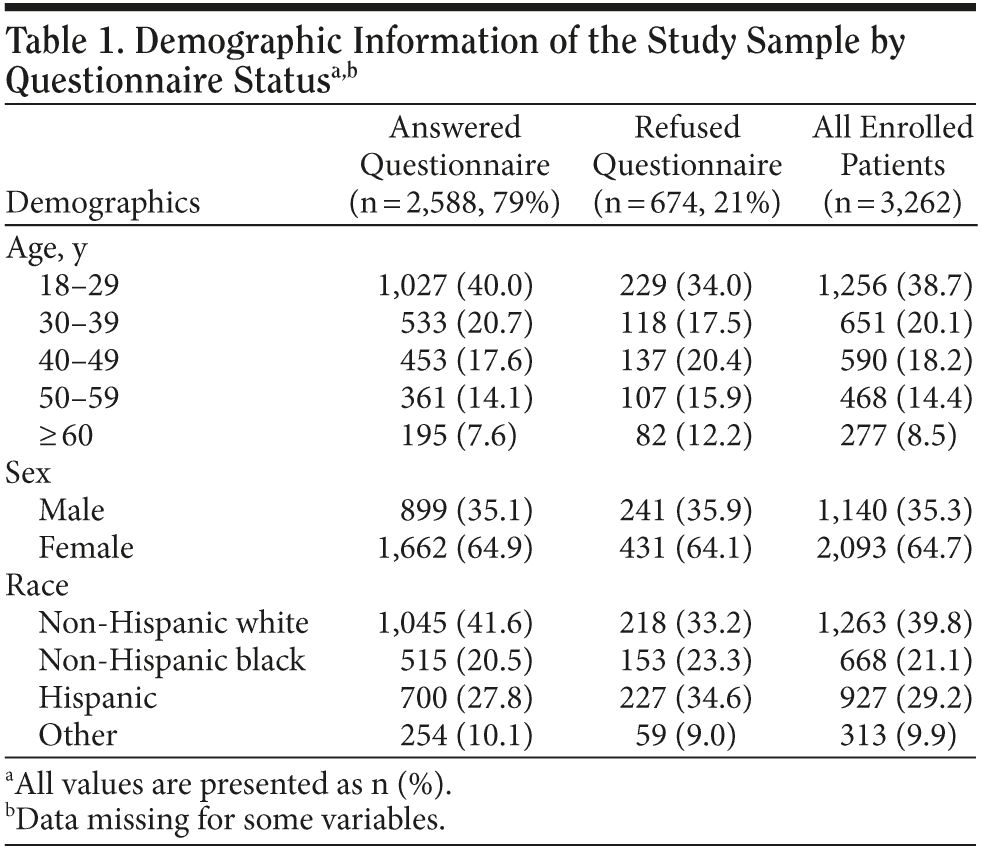
Between February 2007 and March 2008, 3,262 patients enrolled in USHER; of whom, 2,588 (79%) agreed to answer a comprehensive survey about HIV infection and 1,945 (75%) completed the psychosocial assessment battery. Demographic characteristics (age, gender, and race/ethnicity) were similar between study participants who completed or refused the questionnaire (Table 1).
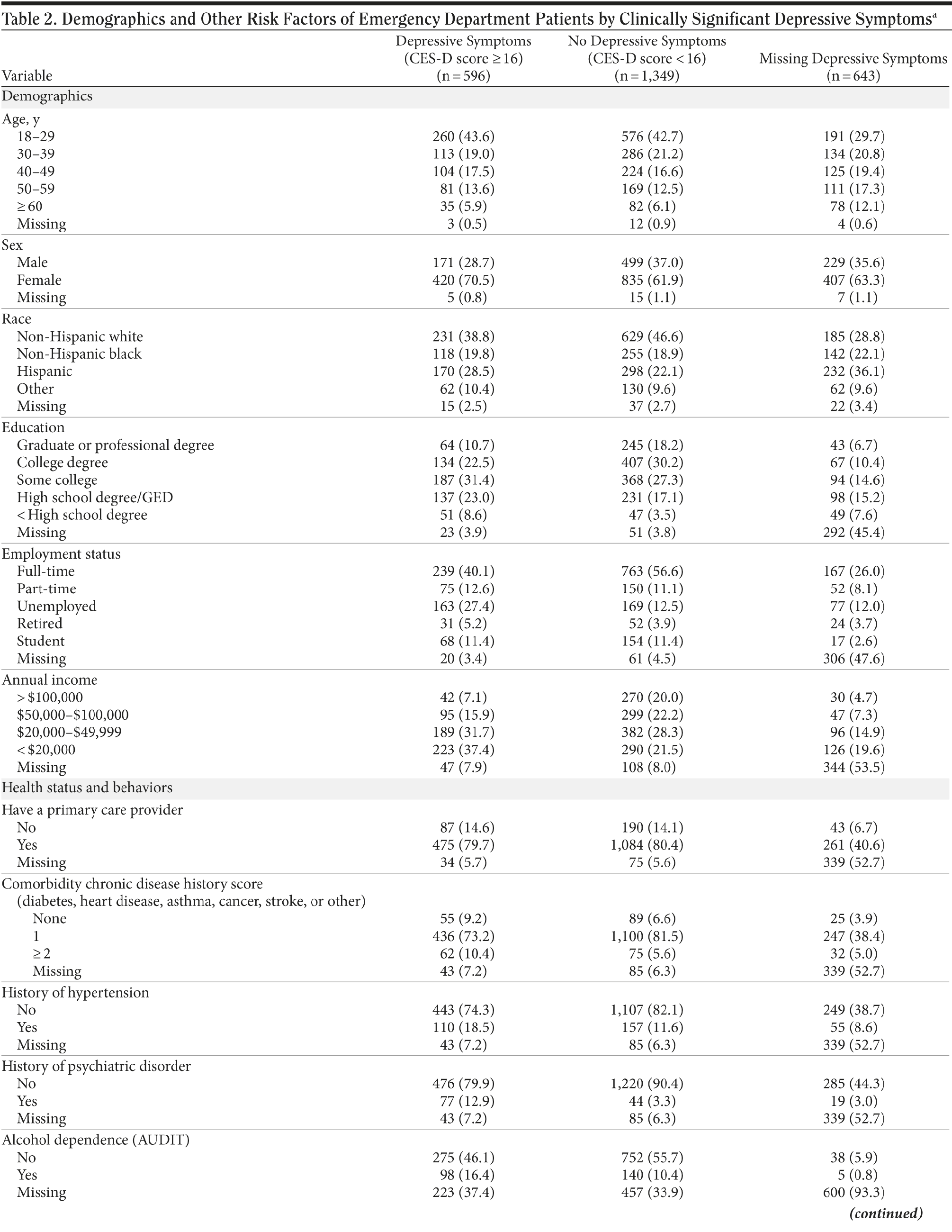
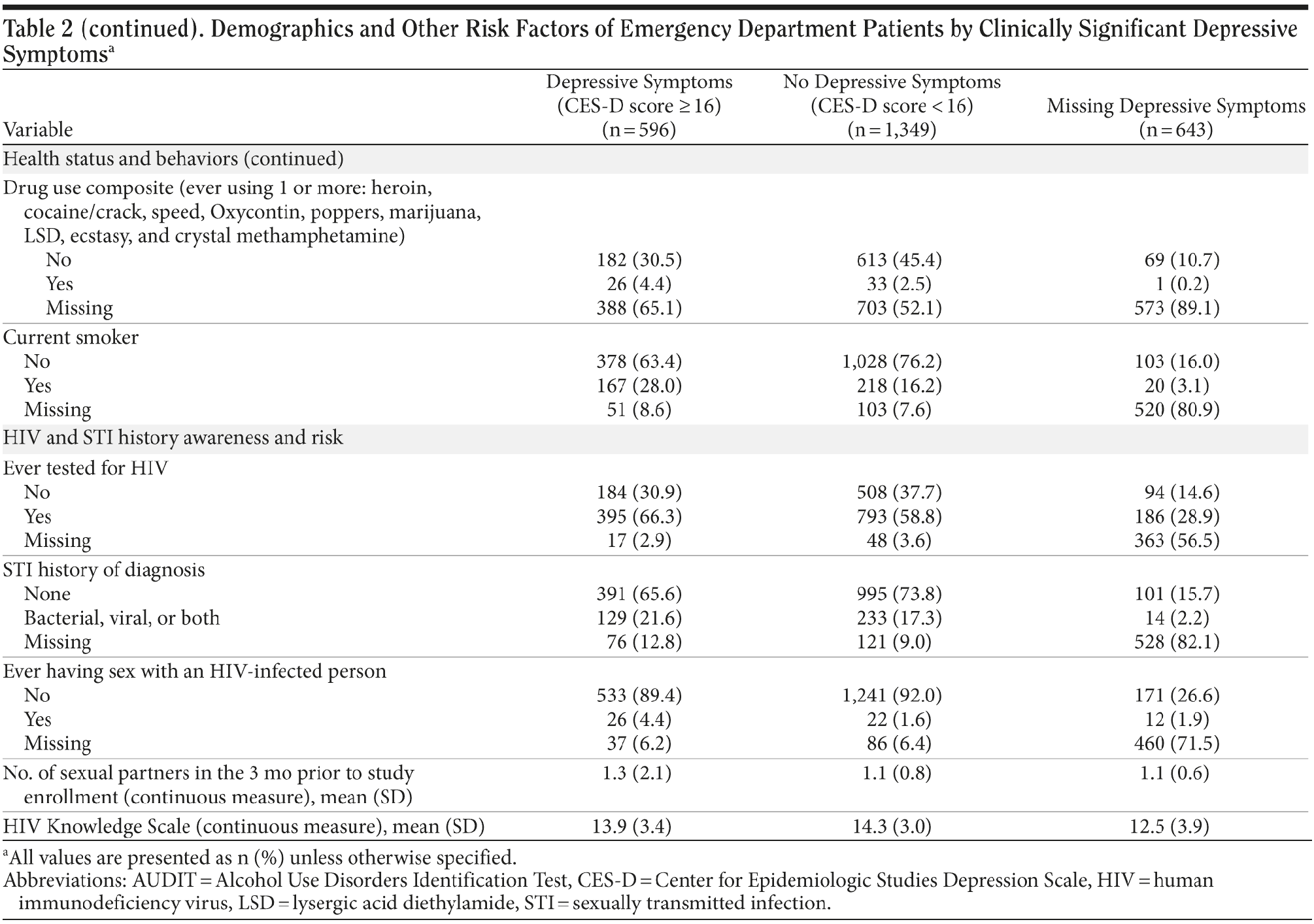
Of 1,945 patients with complete or imputed CES-D data, 596 (31%) screened positive for clinically significant depressive symptoms (CES-D score ≥ 16), and 203 (10%) screened positive for severe depressive symptoms (CES-D score ≥ 27). Six percent of all participants self-reported being previously diagnosed with a psychiatric disorder. Of those with depressive symptoms, 44% were < 30 years of age, 70% were female, 65% had completed at least some college, 40% were fully employed, and 84% had at least 1 comorbidity. Demographics and other characteristics of the study sample for those with and without clinically significant depressive symptoms are outlined in Table 2A and Table 2B.
Bivariate Analyses: Primary Outcome (CES-D score ≥ 16)
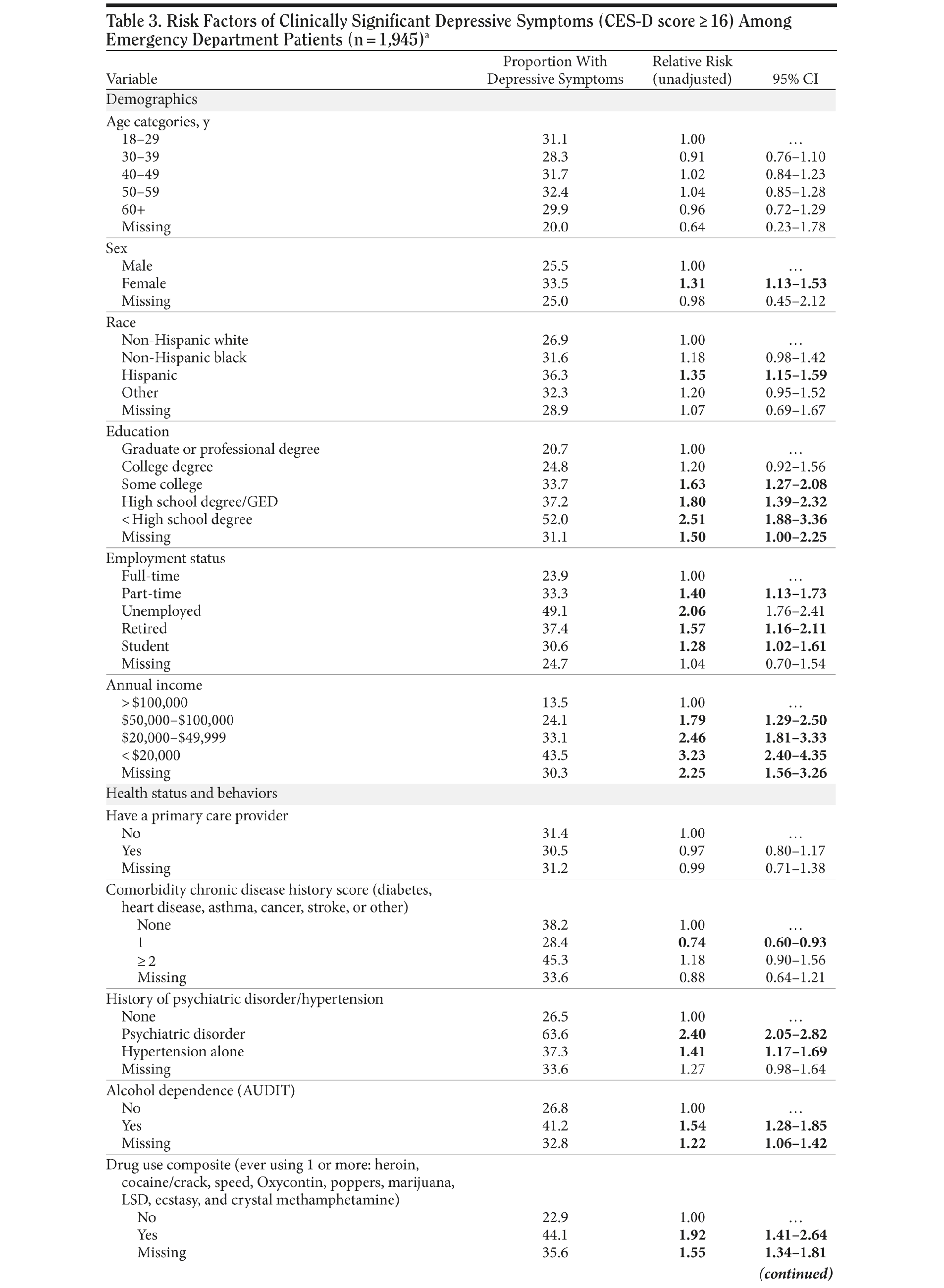
Demographic characteristics statistically significantly associated with increased depressive symptoms in bivariate analyses were female gender, Hispanic ethnicity, lower educational attainment, less than fulltime employment, lower annual income, and history of a psychiatric disorder or hypertension (Table 3A and Table 3B).
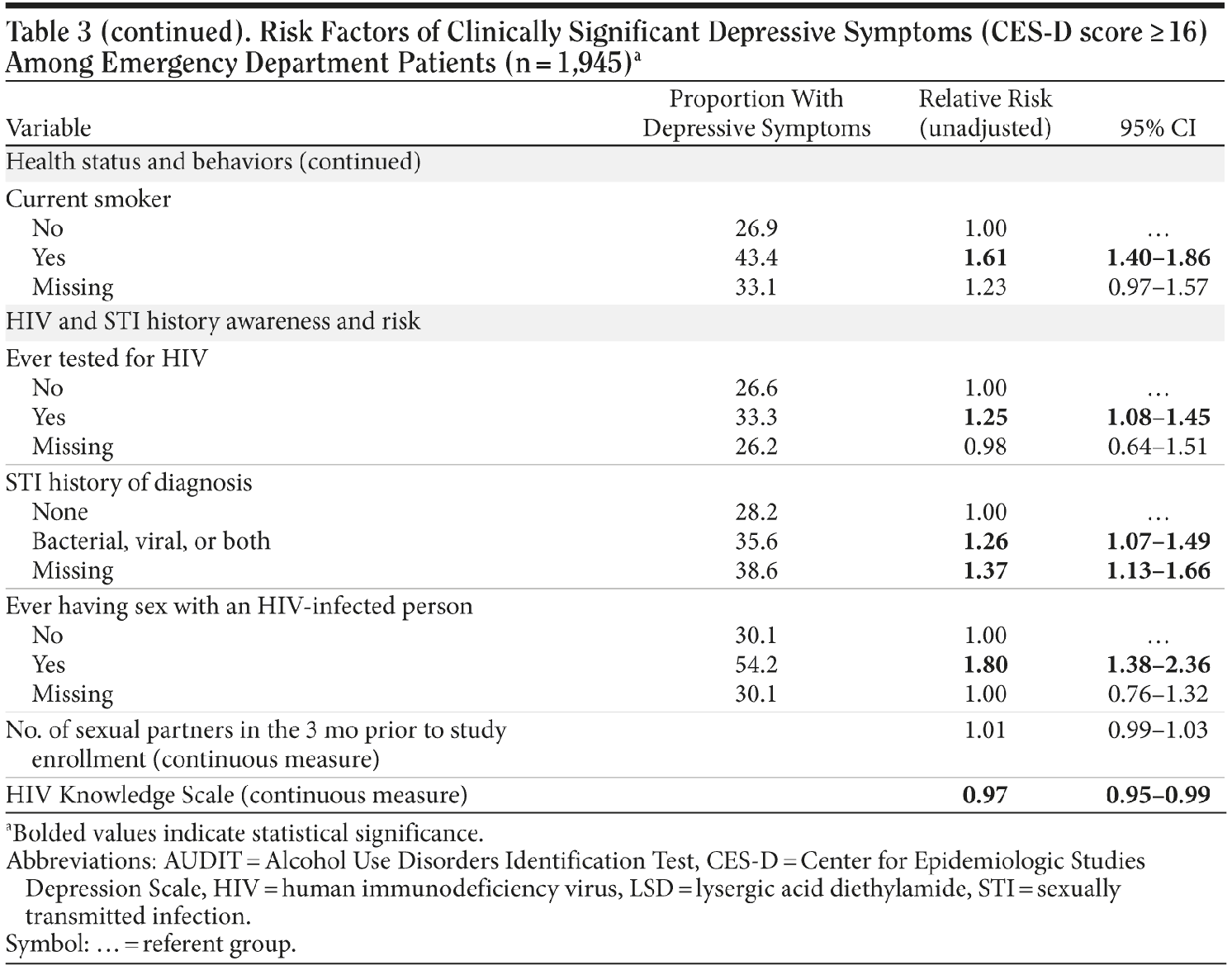
Among behavioral factors collected, alcohol dependence, active tobacco use, and use of illicit substances were significantly associated with higher rates of clinically significant depressive symptoms (Table 3A and Table 3B).
Those who reported prior history of HIV testing, a previous STI diagnosis, and having had sex with a known HIV-infected person in the past were more likely to report clinically significant depressive symptoms. Finally, participants with higher levels of HIV knowledge were less likely to have clinically significant depressive symptoms (Table 3A and Table 3B).
Results of Multivariable Analyses for Primary Outcome (CES-D score ≥ 16)
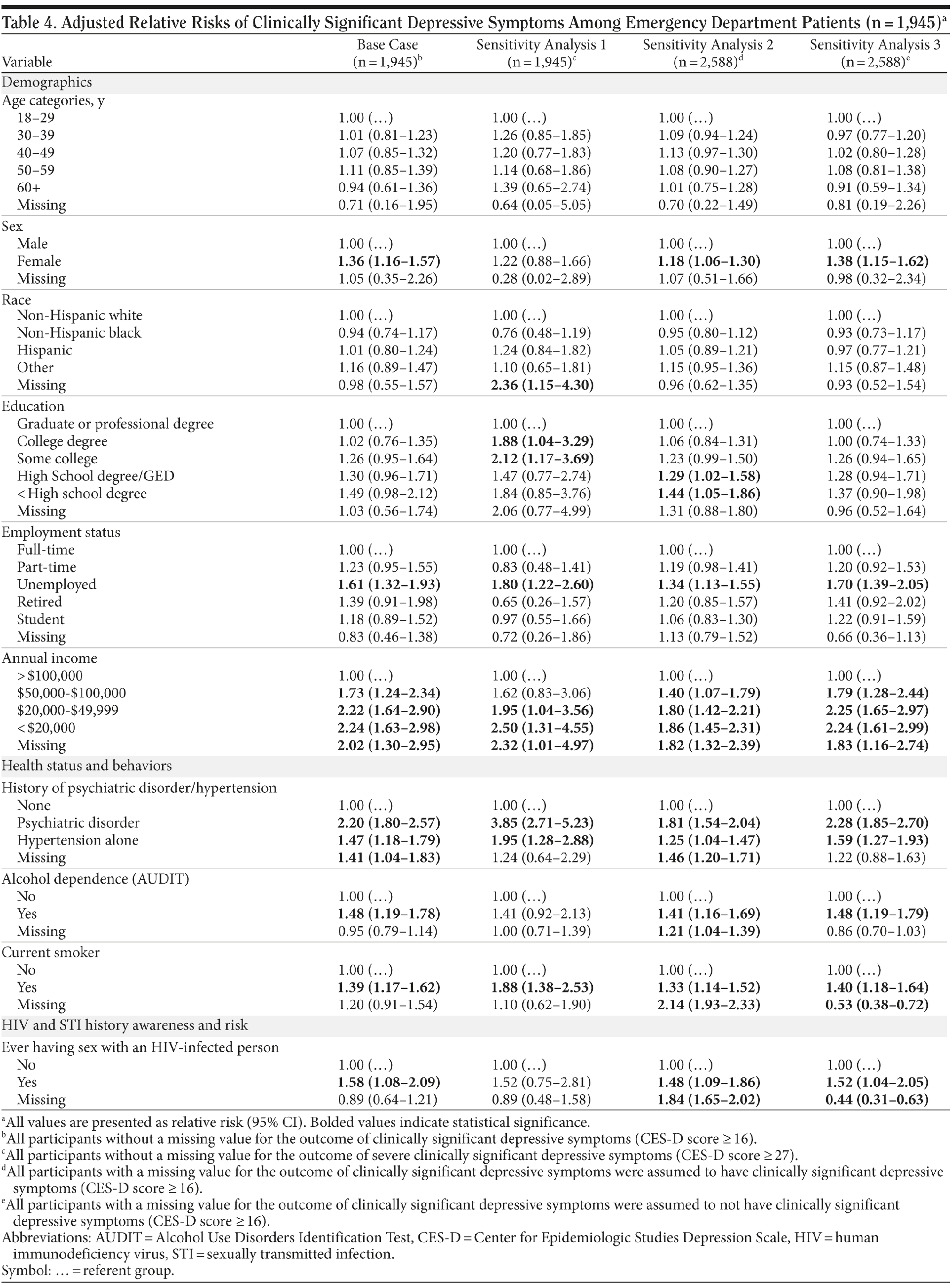
In multivariable analyses, using data from 1,945 participants who completed the questionnaire, nearly all demographic, clinical, and behavioral factors identified in the bivariate analyses exhibited independent positive associations with higher rates of clinically significant depressive symptoms. These included female sex, being unemployed, lower annual income, history of hypertension or psychiatric disorder, alcohol dependence, current smoking, and history of self-reported sex with an HIV-infected person (Table 4). In contrast to bivariate analyses, Hispanic ethnicity and lower educational attainment failed to show a statistically significant association.
Sensitivity Analyses
Sensitivity analysis 1 (CES-D score ≥ 27). Using the CES-D threshold score of ≥ 27 as indicative of severe depressive symptoms, results of multivariable analyses demonstrated similar magnitude of association with education, employment, and annual income. Several factors exhibited a somewhat stronger association. Current tobacco use increased the likelihood of severe depressive symptoms (RR = 1.88; 95% CI, 1.38-2.53), history of hypertension increased the risk of severe depressive symptoms (RR = 1.95; 95% CI, 1.28-2.88), and previous history of psychiatric disorder almost doubled the risk of severe depressive symptoms (RR = 3.85; 95% CI, 2.71-5.23).
Sensitivity analyses 2 and 3 (CES-D score ≥ 16). Results from the sensitivity analyses examining the impact of missing data on the primary outcome were concordant with the base-case analysis (Table 4).
DISCUSSION
Almost one third (31%) of a sample of adults in an urban general hospital ED screened positive for clinically significant depressive symptoms and 10% screened positive for severe depression. The rates of severe depression are consistent with community estimates for prevalence of major depressive disorder (6.6%; 95% CI, 5.9-7.3; 13.1-14.2 million US adults).37
Findings suggest that depressive symptoms are common and may often be overlooked in the ED and urgent care setting, and, hence, recent efforts to increase awareness of depression in outpatient medical settings may be warranted in EDs as well.3,5 Useful and practical screening tools (like the CES-D) that can be administered by physicians or self-administered by patients represent a strategy for identifying depressed patients and linking them into needed treatment and care.
Consistent with prior research, female patients, individuals with lower educational attainment, and those with current alcohol dependence were more likely to screen positive for having clinically significant depressive symptoms.6,7,38-42 Recent studies have linked hypertension and depression, though many indicate that the depression predates and leads to the hypertensive diagnosis.43-46 We demonstrated a clinically important and statistically significant association between history of hypertension and clinically significant depressive symptoms. Due to the cross-sectional nature of our study, however, we cannot examine directionality. Patients with a self-reported history of psychiatric disorder were significantly more likely to have clinically significant depressive symptoms. However, only 6% of all participants self-reported being previously diagnosed with a psychiatric disorder, and, notably, 31% of the total sample screened positive for clinically significant depressive symptoms. These results suggest potentially new identifiable cases that may have been overlooked in the ED due to lack of screening.
Although the benefits of psychiatric care are generally well regarded, health care in the ED setting remains dominated by the primary mission—a focus on acute care; substantial gaps in the delivery of effective preventive care, including identification of depression, in the United States remain.25,47,48 Many barriers to the provision of preventive care interventions exist in emergent and urgent care settings. One of the most important barriers is likely prioritization of acuity—in an ED setting, the acute problem is the focus of the encounter. A second barrier is time constraints. The ED setting has periods of time when multiple individuals present simultaneously requiring emergent attention. Thus, it is critical to keep encounters associated with depression screening as time limited as possible. Finally, as per any health behavior intervention, inadequate provider knowledge in prevention, skepticism about effectiveness of preventive services, and lack of evidence-based prevention practices would be barriers because these would decrease motivation to provide such care services. Patients feeling unwell may also be primarily interested in attention to their chief complaint.3,49
It is critical to note that across-the-board depression screening in the ED will face considerable challenges of linkage to care. Screening is only the first step in the process. As recommended by the US Preventive Services Task Force,48 a positive screen should be followed up with a thorough assessment of depression. Individuals identified as depressed require outpatient follow-up and possibly treatment with mental health professionals. Previous research on HIV testing efforts in ED settings has demonstrated substantial loss to follow-up after a positive screening test result, despite vigorous efforts to contact patients by telephone and mail, and lack necessary protocols and supporting infrastructure to accommodate a large number of positive screening results.50
Despite these barriers, a screening approach to depression is likely to be feasible in the ED setting because many general hospitals are already staffed with psychiatric providers, including PhD-level and/or MD-level clinicians and Master’s -level social workers, who are available for consultation and can be used for follow-up assessment and referral. Modifications in hospital protocols may also be effective in reducing the number of patients lost to follow-up. Two recent studies have shown case management approaches to be effective in improving treatment engagement and outcomes for depressed women seeking mental health care and in linking ED patients with substance abuse treatment.11,51 However, more research on mental health treatment linkage interventions is needed.
The data presented here should be interpreted in the context of the following limitations. First, because these data are cross-sectional, causation cannot be established. Second, participants were part of an ED HIV screening study (ie, they were willing to participate and were potentially less sick than those not willing to participate), thus introducing potential biases and reduced generalizability of findings across all urban general hospital ED patients. Because the CES-D measures symptoms in the past week, it is possible the elevated clinically significant depressive symptoms could be due to short-term reactions to the acute medical problem that brought them into the ED.
Third, screening positive for depressive symptoms is not synonymous to a depression diagnosis. There is also limited evidence on how well screening for depression works when clinicians do not have tools to help improve diagnosis and treatment and allow appropriate follow-up. Clinical practices that screen for depression should have systems in place to ensure that those patients who screen positive receive follow-up for diagnosis and treatment. Despite its potential shortcomings, the potential benefits to screening for depression in the ED setting are substantial, including early diagnosis and treatment.3
The amount of missing data and its impact on our findings cannot be ignored. We were only able to ascertain the outcome of interest for 60% of the enrolled participants and 75% of those who agreed to participate in the survey. Those who agreed to the survey were similar demographically with respect to age and gender; however, those of Hispanic ethnicity were more likely to not participate. This difference potentially could lead to biased estimates within our sample, and, as such, it is possible that differences in clinically significant depressive symptoms by racial/ethnic group exist, but this was not observed in our sample. Finally, due to the high prevalence of alcohol dependence found in the current sample (19%) and its association to increased clinically significant depressive symptoms,52 urban general hospital EDs might also consider a brief alcohol screening assessment and triaging positive screens into appropriate treatment services.
This study points to the potential utility of screening for mental health problems such as depression in the ED setting. The high frequency of clinically significant depressive symptoms among ED patients raises several important concerns for acute care providers and for the health care system as a whole. It is possible that screening will increase the recognition and diagnosis of depression and, when integrated with a commitment to provide coordinated and prompt follow-up of diagnosis and treatment, clinical outcomes could potentially improve.
Disclosure of off-label usage: The authors have determined that, to the best of their knowledge, no investigational information about pharmaceutical agents that is outside US Food and Drug Administration−approved labeling has been presented in this article.
Author affiliations: Department of Psychiatry, Harvard Medical School/Massachusetts General Hospital and The Fenway Institute, Fenway Health (Drs Mimiaga and Safren); Department of Orthopedic Surgery (Mr Reichmann and Dr Losina), Department of Emergency Medicine (Dr Arbelaez), Department of Medicine/Division of Infectious Disease (Dr Walensky), Brigham and Women’s Hospital; Department of Medicine, Divisions of Infectious Disease and General Medicine, Massachusetts General Hospital (Dr Walensky); Department of Biostatistics, Boston University School of Public Health (Mr Reichmann and Dr Losina); and Center for AIDS Research, Harvard Medical School (Drs Safren, Losina, and Walensky), Boston Massachusetts.
Financial disclosure: Drs Mimiaga, Safren, Losina, Arbelaez, and Walensky and Mr Reichmann have no personal affiliations or financial relationships with any commercial interest to disclose relative to the article.
Funding/support: This research was funded by the National Institute of Mental Health (R01 MH073445, R01 MH65869) and the Doris Duke Charitable Foundation, Clinical Scientist Development Award (Dr Walensky).
Disclaimer: The content is solely the responsibility of the authors and does not necessarily represent the official views of the National Institutes of Health.
Acknowledgment: The authors would like to acknowledge the co-investigators and staff of the USHER Trial including Carrie Braverman, LICSW; Susan Larrabee, LICSW; Regina Mikulinsky; Paul Sax, MD; and Elizabeth Wright, PhD. These individuals report no financial or other affiliations relevant to the subject of this article. We would like to thank the faculty and staff of the Brigham and Women’s Hospital Emergency Department for their participation in the USHER Trial, the emergency service assistants and focus group members, and the HIV testing counselors.
This CME activity is expired. For more CME activities, visit cme.psychiatrist.com.
Find more articles on this and other psychiatry and CNS topics:
The Journal of Clinical Psychiatry
The Primary Care Companion for CNS Disorders
REFERENCES
1. Dimidjian S, Hollon SD, Dobson KS, et al. Randomized trial of behavioral activation, cognitive therapy, and antidepressant medication in the acute treatment of adults with major depression. J Consult Clin Psychol. 2006;74(4):658-670. PubMed doi:10.1037/0022-006X.74.4.658
2. Simon GE, VonKorff M. Recognition, management, and outcomes of depression in primary care. Arch Fam Med. 1995;4(2):99-105. PubMed doi:10.1001/archfami.4.2.99
3. US Preventive Services Task Force. Screening for depression: recommendations and rationale. Ann Intern Med. 2002;136(10):760-764. PubMed
4. Pignone MP, Gaynes BN, Rushton JL, et al. Screening for depression in adults: a summary of the evidence for the US Preventive Services Task Force. Ann Intern Med. 2002;136(10):765-776. PubMed
5. Schade CP, Jones ER Jr, Wittlin BJ. A ten-year review of the validity and clinical utility of depression screening. Psychiatr Serv. 1998;49(1):55-61. PubMed
6. Boudreaux ED, Clark S, Camargo CA Jr. Mood disorder screening among adult emergency department patients: a multicenter study of prevalence, associations and interest in treatment. Gen Hosp Psychiatry. 2008;30(1):4-13. PubMed doi:10.1016/j.genhosppsych.2007.09.006
7. Boudreaux ED, Cagande C, Kilgannon H, et al. A prospective study of depression among adult patients in an urban emergency department. Prim Care Companion J Clin Psychiatry. 2006;8(2):66-70. PubMed doi:10.4088/PCC.v08n0202
8. Rhodes KV, Gordon JA, Lowe RA. Preventive care in the emergency department, pt 1: clinical preventive services: are they relevant to emergency medicine? Society for Academic Emergency Medicine Public Health and Education Task Force Preventive Services Work Group. Acad Emerg Med. 2000;7(9):1036-1041. PubMed
9. Zun LS, Downey L. Adult health screening and referral in the emergency department. South Med J. 2006;99(9):940-948. PubMed doi:10.1097/01.smj.0000224130.29337.19
10. Starfield B. Primary Care: Balancing Health Needs, Services, and Technology. New York, NY: Oxford University Press; 1998.
11. Bernstein E, Bernstein J, Levenson S. Project ASSERT: an ED-based intervention to increase access to primary care, preventive services, and the substance abuse treatment system. Ann Emerg Med. 1997;30(2):181-189. PubMed doi:10.1016/S0196-0644(97)70140-9
12. Rodriguez RM, Kreider WJ, Baraff LJ. Need and desire for preventive care measures in emergency department patients. Ann Emerg Med. 1995;26(5):615-620. PubMed doi:10.1016/S0196-0644(95)70014-5
13. Bazargan M, Bazargan S, Baker RS. Emergency department utilization, hospital admissions, and physician visits among elderly African American persons. Gerontologist. 1998;38(1):25-36. PubMed
14. Billings J, Parikh N, Mijanovich T. Emergency Department Use in New York City: A Substitute for Primary Care? New York, NY: Commonwealth Fund Publications; 2000.
15. Blanchard JC, Haywood YC, Scott C. Racial and ethnic disparities in health: an emergency medicine perspective. Acad Emerg Med. 2003;10(11):1289-1293. PubMed doi:10.1111/j.1553-2712.2003.tb00615.x
16. Burt CW, Arispe IE. Characteristics of emergency departments serving high volumes of safety-net patients: United States, 2000. Vital Health Stat 13. 2004;13(155):1-16.
17. Hadley J, Cunningham P. Availability of safety net providers and access to care of uninsured persons. Health Serv Res. 2004;39(5):1527-1546. PubMed doi:10.1111/j.1475-6773.2004.00302.x
18. Kunen S, Niederhauser R, Smith PO, et al. Race disparities in psychiatric rates in emergency departments. J Consult Clin Psychol. 2005;73(1):116-126. PubMed doi:10.1037/0022-006X.73.1.116
19. McCaig L, Burt CW. National Hospital Ambulatory Medical Care Survey: 2003 Emergency Department Summary, Advance Data From Vital and Health Statistics. Hyattsville, MD: National Center for Health Statistics; 2005.
20. McCusker J, Karp I, Cardin S, et al. Determinants of emergency department visits by older adults: a systematic review. Acad Emerg Med. 2003;10(12):1362-1370. PubMed doi:10.1111/j.1553-2712.2003.tb00011.x
21. National Institute of Mental Health (NIMH). Two approaches to routine HIV testing in a hospital emergency department. Available http://www.clinicaltrials.gov/ct2/show/NCT00502944?term=usher&rank=6.
22. Wuerz RC, Travers D, Gilboy N, et al. Implementation and refinement of the Emergency Severity Index. Acad Emerg Med. 2001;8(2):170-176. PubMed doi:10.1111/j.1553-2712.2001.tb01283.x
23. Wuerz RC, Milne LW, Eitel DR, et al. Reliability and validity of a new five-level triage instrument. Acad Emerg Med. 2000;7(3):236-242. PubMed doi:10.1111/j.1553-2712.2000.tb01066.x
24. Eitel DR, Travers DA, Rosenau AM, et al. The Emergency Severity Index triage algorithm version 2 is reliable and valid. Acad Emerg Med. 2003;10(10):1070-1080. PubMed doi:10.1111/j.1553-2712.2003.tb00577.x
25. US Department of Health and Human Services. CES-D Scale. Bethesda, MD: Department of Health and Human Services & National Institute of Health; 2004.
26. Hann D, Winter K, Jacobsen P. Measurement of depressive symptoms in cancer patients: evaluation of the Center for Epidemiological Studies Depression Scale (CES-D). J Psychosom Res. 1999;46(5):437-443. PubMed doi:10.1016/S0022-3999(99)00004-5
27. Radloff LS. The CES-D scale: a self-report depression scale for research in the general population. Appl Psychol Meas. 1977;1(3):385-401. doi:10.1177/014662167700100306
28. Barbor TF, Higgins-Biddle JC, Saunders JB, et al. The Alcohol Use Disorders Identification Test (AUDIT): Guidelines for Use in Primary Care. 2nd ed. Geneva, Switzerland: World Health Organization; 2001.
29. Carey MP, Schroder KE. Development and psychometric evaluation of the brief HIV Knowledge Questionnaire. AIDS Educ Prev. 2002;14(2):172-182. PubMed doi:10.1521/aeap.14.2.172.23902
30. Zich JM, Attkisson CC, Greenfield TK. Screening for depression in primary care clinics: the CES-D and the BDI. Int J Psychiatry Med. 1990;20(3):259-277. PubMed
31. Ensel WM. Measuring depression: the CES-D scale. In: Lin N, Dean A, Ensel W, eds. Social Support, Life Events, and Depression. New York, NY: Academic Press; 1986.
32. Geisser ME, Roth RS, Robinson ME. Assessing depression among persons with chronic pain using the Center for Epidemiological Studies-Depression Scale and the Beck Depression Inventory: a comparative analysis. Clin J Pain. 1997;13(2):163-170. PubMed doi:10.1097/00002508-199706000-00011
33. Zou G. A modified poisson regression approach to prospective studies with binary data. Am J Epidemiol. 2004;159(7):702-706. PubMed doi:10.1093/aje/kwh090
34. Greenland S. Model-based estimation of relative risks and other epidemiologic measures in studies of common outcomes and in case-control studies. Am J Epidemiol. 2004;160(4):301-305. PubMed doi:10.1093/aje/kwh221
35. Zhang J, Yu KF. What’s the relative risk? a method of correcting the odds ratio in cohort studies of common outcomes. JAMA. 1998;280(19):1690-1691. PubMed doi:10.1001/jama.280.19.1690
36. McNutt LA, Wu C, Xue X, et al. Estimating the relative risk in cohort studies and clinical trials of common outcomes. Am J Epidemiol. 2003;157(10):940-943. PubMed doi:10.1093/aje/kwg074
37. Kessler RC, Berglund P, Demler O, et al. National Comorbidity Survey Replication. The epidemiology of major depressive disorder: results from the National Comorbidity Survey Replication (NCS-R). JAMA. 2003;289(23):3095-3105. PubMed doi:10.1001/jama.289.23.3095
38. Kessler RC, McGonagle KA, Zhao S, et al. Lifetime and 12-month prevalence of DSM-III-R psychiatric disorders in the United States: results from the National Comorbidity Survey. Arch Gen Psychiatry. 1994;51(1):8-19. PubMed
39. Dohrenwend BP, Dohrenwend BS. Social Status and Psychological Disorder: A Causal Inquiry. New York, NY: Wiley; 1969.
40. Dohrenwend BS, Dohrenwend BP. Stressful Life Events: Their Nature and Effects. New York, NY: Wiley; 1974.
41. Kumar A, Clark S, Boudreaux ED, et al. A multicenter study of depression among emergency department patients. Acad Emerg Med. 2004;11(12):1284-1289. PubMed doi:10.1111/j.1553-2712.2004.tb01915.x
42. Whooley MA, Kiefe CI, Chesney MA, et al. CARDIA Study. Depressive symptoms, unemployment, and loss of income: The CARDIA Study. Arch Intern Med. 2002;162(22):2614-2620. PubMed doi:10.1001/archinte.162.22.2614
43. Wells KB. The role of depression in hypertension-related mortality. Psychosom Med. 1995;57(5):436-438. PubMed
44. Jonas BS, Franks P, Ingram DD. Are symptoms of anxiety and depression risk factors for hypertension? longitudinal evidence from the National Health and Nutrition Examination Survey I Epidemiologic Follow-up Study. Arch Fam Med. 1997;6(1):43-49. PubMed doi:10.1001/archfami.6.1.43
45. Davidson K, Jonas BS, Dixon KE, et al. Do depression symptoms predict early hypertension incidence in young adults in the CARDIA study? Coronary Artery Risk Development in Young Adults. Arch Intern Med. 2000;160(10):1495-1500. PubMed doi:10.1001/archinte.160.10.1495
46. Meyer CM, Armenian HK, Eaton WW, et al. Incident hypertension associated with depression in the Baltimore Epidemiologic Catchment area follow-up study. J Affect Disord. 2004;83(2-3):127-133. PubMed doi:10.1016/j.jad.2004.06.004
47. Centers for Disease Control and Prevention (CDC). The Power of Prevention: Reducing the Health and Economic Burden of Chronic Disease. Atlanta, GA: Department of Health and Human Services, Centers for Disease Control and Prevention; 2003.
48. Woolf SH, Atkins D. The evolving role of prevention in health care: contributions of the US Preventive Services Task Force. Am J Prev Med. 2001;20(suppl 3):13-20. PubMed doi:10.1016/S0749-3797(01)00262-8
49. US Department of Health and Human Services. Healthy People 2010. Understanding and Improving Health and Objectives for Improving Health. 2nd ed. 2 vols. Washington, DC: Government Printing Office; 2000.
50. Brown J, Shesser R, Simon G, et al. Routine HIV screening in the emergency department using the new US Centers for Disease Control and Prevention Guidelines: results from a high-prevalence area. J Acquir Immune Defic Syndr. 2007;46(4):395-401. PubMed doi:10.1097/QAI.0b013e3181582d82
51. Miranda J, Azocar F, Organista KC, et al. Treatment of depression among impoverished primary care patients from ethnic minority groups. Psychiatr Serv. 2003;54(2):219-225. PubMed doi:10.1176/appi.ps.54.2.219
52. Davidson KM, Ritson EB. The relationship between alcohol dependence and depression. Alcohol Alcohol. 1993;28(2):147-155. PubMed