ABSTRACT
Objective: To evaluate the knowledge and attitudes of Iraqi dermatologists regarding understanding, diagnosing, and treating psychocutaneous disorders.
Methods: An online survey questionnaire was randomly distributed among Iraqi dermatologists through Google Forms in August 2020. The dermatologists were asked to provide information on their understanding of psychodermatology, referral patterns, level of comfort in managing psychocutaneous disorders, awareness of community resources, and interest in learning more about psychodermatology.
Results: Of 200 distributed questionnaires, 61 were returned. The most common psychocutaneous disorder seen was acne, followed by alopecia areata and vitiligo. About half of the participants reported being neutral about their comfort level in treating psychocutaneous disorders, and approximately half had no formal training in psychodermatology. Almost 60% of participants did not know of any community resources, and three-quarters were willing to seek educational activities on psychodermatology.
Conclusions: The study results revealed that Iraqi dermatologists have significant gaps in knowledge, training, and treatment of psychocutaneous disorders. The survey findings reveal the importance of addressing the training needs of young physicians, including dermatologists, psychiatrists, and primary care physicians, in relation to the psychological component of skin diseases.
Prim Care Companion CNS Disord 2022;24(2):21m03077
To cite: Altaha L, Jafferany M, Khan A. Psychocutaneous medicine in Iraq: current status and recommendations. Prim Care Companion CNS Disord. 2022;24(2):21m03077.
To share: https://doi.org/10.4088/PCC.21m03077
© Copyright 2022 Physicians Postgraduate Press, Inc.
aCenter of Dermatology, Medical City, Baghdad, Iraq
bCentral Michigan University College of Medicine, Medical Education Partners, Saginaw, Michigan
cUniversity of California Los Angeles, Los Angeles, California
*Corresponding author: Mohammad Jafferany, MD, Central Michigan University College of Medicine, 3201 Hallmark Ct, Saginaw, MI 48603 ([email protected]).
From an embryologic standpoint, both the skin and nervous system share a common origin. The association between skin disease and psychological manifestations has long been discussed and well documented of late. In a multicenter European study,1 a close link among depression, anxiety, and skin disease was demonstrated. The well-documented link between the emotional state of the patient and skin disease provides evidence that skin has its own stress response. The hypothalamic-pituitary axis perpetuating stress response with increased cortisol levels compromises the skin barrier function and thus reduces epidermal hydration and disrupts mitochondrial DNA synthesis and repair.2 Several studies3–6 from different parts of the world have demonstrated lack of awareness among dermatologists about the basic concept of psychodermatology. It is important to understand that skin conditions themselves cause anxiety, sadness, and feelings of embarrassment and humiliation in individuals irrespective of the severity or type.7 Many invisible psychiatric conditions are easily missed due to suboptimal treatment of the visible skin condition.8 Incorporation of a psychodermatology curriculum in dermatology or psychiatry residency programs is still lacking.9,10 The mind-skin connection has been studied for many years. The last 2 decades have seen the development of new research areas revealing the connection between the skin and mind and how they are interconnected.11 Patients with psychocutaneous disorders generally refuse mental health resources due either to stigma associated with mental illness or poor insight about the acceptance of the psychological component associated with their disease. The objective of this study was to evaluate the knowledge and attitudes of Iraqi dermatologists regarding understanding, diagnosing, and treating psychocutaneous disorders. This is the first study, to our knowledge, on practice patterns and knowledge among Iraqi dermatologists and the third from the Middle East.3,4
METHODS
We conducted a survey of Iraqi dermatologists using an internet survey to evaluate the knowledge, awareness, practice patterns, and training needs of Iraqi dermatologists. The study was approved by the Center of Dermatology, Medical City, Baghdad, Iraq and was adherent to the Helsinki declaration. Informed consent was signed by all respondents.
Sample
An online survey questionnaire developed by one of the authors (M.J.) was randomly distributed among Iraqi dermatologists in social media groups in August 2020. The names and e-mail addresses of Iraqi dermatologists were obtained from dermatology social media groups on WhatsApp and LinkedIn. Some surveys were also sent by mail to those who did not respond to the online questionnaire. All respondents were practicing dermatologists in different settings such as university, ministry of health, or private practice.
Inclusion and Exclusion Criteria
All practicing dermatologists in different practice settings across the country were included in this study. Of the returned questionnaires, 41 were excluded from the study due to being incomplete.
Instrument
The survey questionnaire consists of questions related to dermatologists’ cognizance, practice pattern, and training needs regarding psychodermatologic disorders. Survey responses were kept anonymous and confidential except for a tracking number to count surveys.
Measures
To assess knowledge and awareness of psychodermatologic issues in the sample, respondents self-reported the percentage of patients seen with psychocutaneous disorders and knowledge of common dermatologic disorders. Practice patterns were assessed with a question on comfort level in treating patients with psychocutaneous complaints and referral patterns to psychiatrists/psychologists. Finally, to assess training needs among the study sample, respondents reported level of interest in continuing medical education (CME) activities. Respondents could select a single response choice for all questions in the analysis except for questions regarding dermatologic disorders with a psychological component and interest in CME activities, for which respondents could select more than one response choice.
Statistical Analysis
All collected data were entered and analyzed using SPSS software (IBM, Armonk, New York) to manage and analyze quantitative data. We conducted univariate analysis of demographic characteristics, knowledge, awareness, practice patterns, and training needs of the sample. Multivariate ordinary least squares regressions were conducted to assess factors that influenced percentage of patients seen with psychocutaneous disorders and the number of common dermatologic disorders seen by the dermatologists. In each of the multivariate regression models, we controlled for sociodemographic characteristics of the sample such as age, level of training, years of experience, and geographic location.
RESULTS
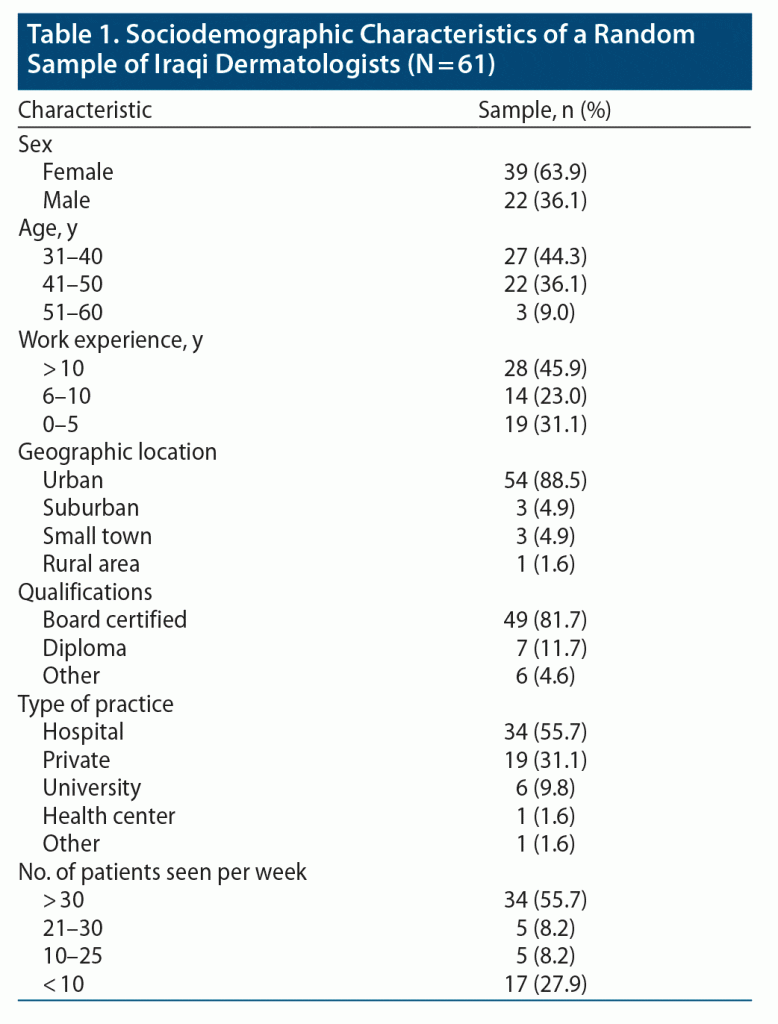
A total of 200 questionnaires were distributed, 102 were returned, and 61 were found to be eligible for the study. The majority of survey respondents were young dermatologists, and only 9% were aged > 60 years. More than 60% of participants were female. Almost half of the survey respondents had work experience > 10 years. Also, 88.5% of respondents were geographically located in urban areas. More than 80% had board certification. More than half of the participants were practicing in hospital settings, and one-third were in private practice. Table 1 shows detailed demographic data of the survey respondents.
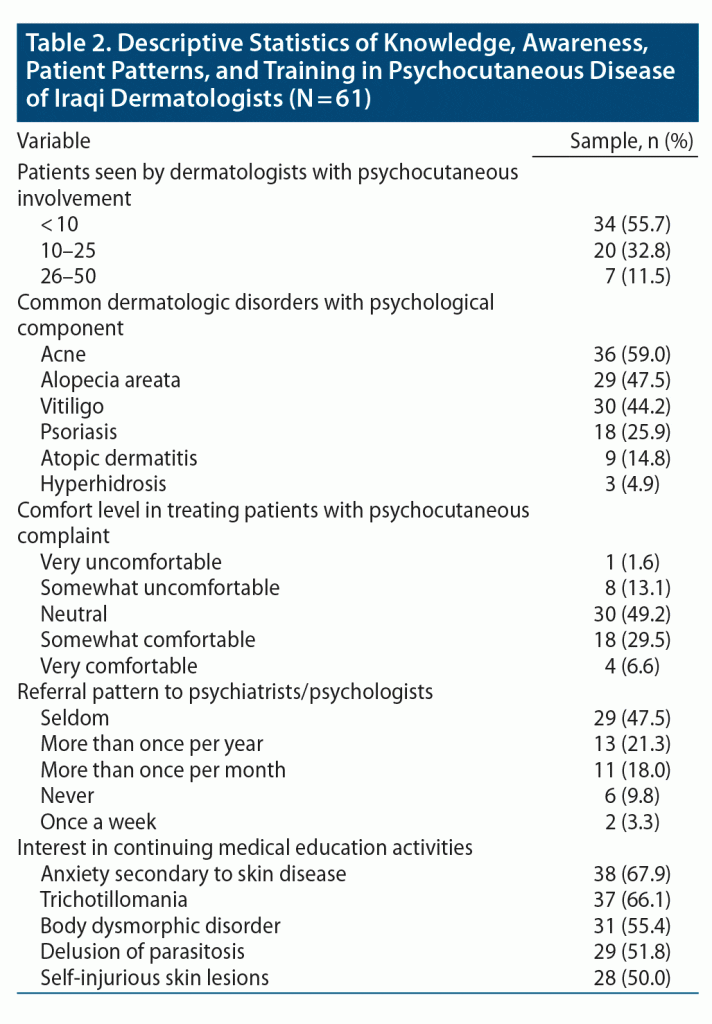
Table 2 shows the percentage of dermatologists seeing patients with psychocutaneous disorders. Acne, alopecia, and vitiligo were the 3 most common psychocutaneous disorders seen by dermatologists in our study. Regarding comfort level in treating psychocutaneous disorders, almost half of the survey respondents reported being neutral, and about one-third reported being somewhat comfortable. Only a small percentage (6.6%) was very comfortable seeing patients with psychocutaneous disorders. Almost half of dermatologists reported occasionally referring patients to psychiatrists, and approximately 10% reported never referring any patient to psychiatrists.
More than one-third (44%) of dermatologists had no formal training in psychodermatology, and 11% reported attending psychodermatology didactics. Only half of the survey respondents reported having some knowledge of community resources and psychodermatology educational websites. About three-quarters (74%) of participants showed interest in receiving CME about psychodermatology; 21.3% were indecisive about receiving CME activities. Three respondents (4.9%) were not interested in receiving CME. The area in which dermatologists were most interested in receiving CME was anxiety secondary to skin disease, followed by trichotillomania and body dysmorphic disorder.
DISCUSSION
The study results show that Iraqi dermatologists see a significant number of patients with psychodermatologic disorders, but they lack proper training and CME activities. Also, 44% had no formal training in psychodermatology. Dermatologists in our study had a noticeable disparity in knowledge and proper understanding and treatment of psychocutaneous disorders. The findings of our study are in contrast with other similar studies from different parts of the world, which is possibly related to geographic and cultural factors. Half of the participants reported no awareness of any community resources or informational websites that could be helpful for their patients or even increase their knowledge. The disparities were also identified in areas related to referral patterns. Lack of formal training and skepticism of some dermatologists regarding receiving educational activities on psychodermatology appear to be causing concerns, particularly in relation to awareness of psychodermatology in Iraq.
The estimated prevalence of psychiatric comorbidity in the outpatient dermatology setting is about 30%.5 Common psychocutaneous disorders seen in our study were acne, alopecia areata, and vitiligo. This finding is different from other studies conducted in different parts of the world including from the same region (ie, United Arab Emirates and Iran).3,4 This difference could be explained by the specific geographic location, weather, local customs, and culture. In a Turkish study,6 dermatologists reported hyperhidrosis, atopic dermatitis, and vitiligo as the prevailing psychocutaneous disorders, while studies3,4 from Iran and the United Arab Emirates both reported acne, alopecia areata, and vitiligo to be the prevalent psychocutaneous disorders. The latter 2 studies are from neighboring countries, confirming the geographic and cultural factors associated with this region. Kuhn et al5 reported 42% of dermatologists were comfortable diagnosing and treating psychocutaneous disorders. However, in our study only 6% reported being very comfortable with seeing and diagnosing patients with psychocutaneous disorders, and about 44% had no formal training in psychodermatology, indicating a significant gap in knowledge. This knowledge gap could be explained by the generalized lack of psychodermatology resources in the region. Our study has numerous limitations, and the results cannot be generalized, as the survey respondents were mostly from urban areas and did not include many dermatologists who work in remote and rural areas of the country. The responses of survey participants could be biased secondary to the lack of knowledge of dermatologists about psychodermatology. There were several open-ended questions, and respondents’ free text answers might have produced information bias.
CONCLUSION
Our findings strongly indicate the need to add didactics in residency programs and establish formal training opportunities for dermatologists, psychiatrists, and primary care physicians. Residency training programs should emphasize the psychological component associated with skin disease in their curriculum to better train young physicians. Regular CME events on psychodermatology and implementation of dermatology/psychiatry/primary care liaison clinics could be of enormous help in the long-term management of patients with psychocutaneous disorders. Our survey findings are of paramount importance in addressing the training needs of young physicians including dermatologists, psychiatrists, and primary care physicians in relation to the psychological component of skin diseases.
Submitted: July 19, 2021; accepted October 11, 2021.
Published online: April 21, 2022.
Relevant financial relationships: None.
Funding/support: None.
References (11)

- Dalgard FJ, Gieler U, Tomas-Aragones L, et al. The psychological burden of skin diseases: a cross-sectional multicenter study among dermatological out-patients in 13 European countries. J Invest Dermatol. 2015;135(4):984–991. PubMed CrossRef
- Picard M, McEwen BS. Psychological stress and mitochondria: a systematic review. Psychosom Med. 2018;80(2):141–153. PubMed CrossRef
- Osman OT, Souid AK, Al-Mugaddam F, et al. Attentiveness of dermatologists in the Middle East to psychocutaneous medicine. Prim Care Companion CNS Disord. 2017;19(2):10.4088/PCC.16m02080. PubMed CrossRef
- Handjani F, Saki N, Emad N, et al. Psychodermatology in Iran: a survey on knowledge, awareness, and practice patterns in Iranian dermatologists. Dermatol Ther (Heidelb). 2020;33(6):e14009. PubMed CrossRef
- Kuhn H, Mennella C, Magid M, et al. Psychocutaneous disease: clinical perspectives. J Am Acad Dermatol. 2017;76(5):779–791. PubMed CrossRef
- Ocek T, Kani AS, Baş A, et al. Psychodermatology: knowledge, awareness, practicing patterns, and attitudes of dermatologists in Turkey. Prim Care Companion CNS Disord. 2015;17(2):10.4088/PCC.14m01628. PubMed CrossRef
- Jafferany M. Psychodermatology: a guide to understanding common psychocutaneous disorders. Prim Care Companion J Clin Psychiatry. 2007;9(3):203–213. PubMed CrossRef
- Shenoi SD, Prabhu S, Nirmal B, et al. Our experience in a psychodermatology liaison clinic at Manipal, India. Indian J Dermatol. 2013;58(1):53–55. PubMed CrossRef
- Jafferany M, Vander Stoep A, Dumitrescu A, et al. The knowledge, awareness, and practice patterns of dermatologists toward psychocutaneous disorders: results of a survey study. Int J Dermatol. 2010;49(7):784–789. PubMed CrossRef
- Chung WL, Ng SS, Koh MJ, et al. A review of patients managed at a combined psychodermatology clinic: a Singapore experience. Singapore Med J. 2012;53(12):789–793. PubMed
- Azambuja RD, Universidade de Brasília, Brazil. The need of dermatologists, psychiatrists and psychologists joint care in psychodermatology. An Bras Dermatol. 2017;92(1):63–71. PubMed CrossRef
Enjoy this premium PDF as part of your membership benefits!