Because this piece does not have an abstract, we have provided for your benefit the first 3 sentences of the full text.
Have you ever been confronted by a patient who appeared angry? Have you ever feared for your safety while with a patient? Have you wondered how you could have approached or managed an apparently angry individual? If you have, then the following case vignettes and discussion of angry patients in the hospital setting should prove useful.
Evaluation and Treatment of the Angry Patient
Have you ever been confronted by a patient who appeared angry? Have you ever feared for your safety while with a patient? Have you wondered how you could have approached or managed an apparently angry individual? If you have, then the following case vignettes and discussion of angry patients in the hospital setting should prove useful.
case VIGNETTES
Case 1
Mr A, a 92-year-old black man with a history of poorly controlled type 2 diabetes mellitus (complicated by end-stage renal disease on hemodialysis and a right below-the-knee amputation), was admitted to the emergency department from the dialysis clinic with pseudomonas bacteremia. Mr A became enraged when he was told that he needed hospital admission. He felt that this was an attempt to take his money and that it was not a strategy to improve his health; he maintained that he felt fine and that if intravenous (IV) antibiotics were required, he could receive them at the dialysis clinic. When the emergency department physician attempted to do a physical examination of his leg stump, Mr A began to yell, and he swung his crutch at the physician. He bellowed, “The infection is in my blood. There is no need to examine any other part of me!”
How could the emergency department staff have handled Mr A’s worsening aggression?
Case 2
Ms B, a 43-year-old woman with chronic abdominal pain, arrived at her first visit with a new primary care physician. She felt that her prior doctors had not adequately addressed her pain or completed a thorough workup. She was convinced that she had Crohn’s disease and was angry because her physicians had not agreed with her diagnosis. After the new physician took a history and determined that Crohn’s disease was unlikely, Ms B became agitated and declared, “No one listens to me. I know my body better than all of you.”
How could or should the physician have proceeded?
WHAT IS ANGER?
Anger is a negative emotional state that is generally accompanied by physiologic arousal and antagonistic thoughts directed toward a person or object viewed as the cause of an adverse event.1 Manifestations of anger range from mild irritation to out-of-control rage.2 Anger can also be suppressed, such as when directed inward toward the self, or it can be directed at others in the form of confrontations or aggressive behavior.3
WHY IS IT IMPORtANT TO
RECOGNIZE ANGER IN OTHERS?
Recognizing patient anger is important for keeping health care providers safe. Among psychiatric patients, anger is one of the strongest predictors of aggression.4 Although uncommon, extreme instances of violence directed at health care providers do occur. In 2010, Warren Davis shot his mother’s orthopedic surgeon before killing his mother and himself after he learned that back surgery had left his mother paralyzed.5 In 2014, a strikingly similar situation occurred at Sacred Heart Hospital in Cebu City, Philippines, when a wheelchair-bound patient, who was upset about not being able to walk after spinal surgery, shot and killed his orthopedic surgeon before killing himself.6 In 2015, Stephen Pasceri shot and killed Dr Michael Davidson, a Brigham and Women’s Hospital cardiologist, who Mr Pasceri believed inappropriately prescribed his mother an antiarrhythmic agent, which he was convinced had contributed to her death.7 According to police reports, prior to walking out to meet Mr Pasceri, Dr Davidson stated to a colleague, “Watch this, he’ll probably shoot me.” While it is impossible to know whether Dr Davidson really believed Mr Pasceri to be capable of violence, his statement might betray an unconscious awareness that a particular person has the capacity for violence. While extreme acts of violence are uncommon, violent crimes in health care institutions have increased significantly in recent years.8
Recognizing patient anger is also necessary for ensuring patient safety. Partially in response to the increase in violent incidents, in 2014, 52% of medical centers in a national survey reported that they allowed security guards to carry guns.9 The increased presence of guns in hospitals has resulted in the injury and death of several agitated patients. In August 2015, a 26-year-old student, Alan Pean, who had been admitted for bipolar disorder, nearly died when 2 off-duty police officers shot him in the chest.10 Psychiatric patients appear to be particularly at risk. In January 2016, a Central Lynchburg General Hospital security officer in Lynchburg, Virgina, shot Jonathan Warner, a patient with bipolar disorder, 4 times after he became angry and took the officer’s taser. Jonathan Warner was left paralyzed from the waist down.11
Beyond physical harm, there are other consequences of failure to identify and appropriately respond to angry patients. Anger disrupts the doctor-patient relationship and can cause patients to miss appointments, to be less adherent with their medications, and to develop overall worse health outcomes.12,13
Additionally, anger contributes to many malpractice lawsuits. When physicians and hospitals address patient anger by admitting mistakes and apologizing, the rate of malpractice lawsuits declines.14 Since lawsuits decline when physicians apologize, it is reasonable to surmise that such suits are often driven more by anger than the actual outcome.
HOW CAN ONE RECOGNIZE THAT
A PATIENT IS ANGRY?
Individuals vary in how they manifest anger, and a single individual may express anger differently depending on the situation. Physical signs of anger include glowering eyes, knitted brows, pursed lips, slightly opened mouth, facial flushing, a tense jaw, or adopting an aggressive stance.15 Behavioral manifestations of aggression include yelling, swearing, becoming quiet, or changing from one’s baseline behavior. Some patients may not provide overt signs of anger but passively demonstrate their anger through their actions, such as noncompliance with medical treatment.
In the health care setting, anger can be described as falling on a 6-pronged continuum16:
- Calm and nonthreatening: A patient may be frustrated but fail to show overt signs of agitation.
- Verbally agitated: A patient may say, “This is ridiculous. I can’t believe I have been sitting in here for 45 minutes,” as he or she paces while waiting for a physician who is running late.
- Verbally hostile: A patient may shift from offering phrases of discontent to unkind phrases, eg, “This doctor is incompetent and this entire practice is a sham.”
- Verbally threatening: A patient may demand an apology or threaten to sue.
- Physically threatening: A patient may take a fighter’s stance and make a fist.
- Physically violent: A patient may attempt to injure providers.
Patients in phase 1 of the continuum are capable of thinking logically and responding appropriately. Providers can employ the techniques discussed in the following section to keep patients in or redirect them to this phase.
HOW CAN ONE PREDICT WHO IS AT INCREASED RISK OF BECOMING AGGRESSIVE?
There is no paper-and-pencil tool that can accurately identify which patients will become violent during a given hospitalization. However, some tools can help predict which patients are at higher risk for aggression. McNiel and Binder’s17 checklist is one such instrument; it contains 5 domains (eg, history of aggression within 2 weeks of admission). The checklist has a 25% improvement over chance at identifying which patients will become physically assaultive. While such checklists are helpful, they are far from perfect. For example, McNiel and Binder’s17 checklist has a 67.9% false positive rate at detecting those at risk of becoming physically violent.
Research to identify patient aggression risk factors is ongoing. In a preliminary study4 of 200 psychiatric inpatients, researchers found that the most reliable predictors of patient aggression were younger age, shorter length of illness, hostility, depression, and difficulty in delaying gratification.
HOW CAN AN ANGRY PATIENT BE HANDLED?
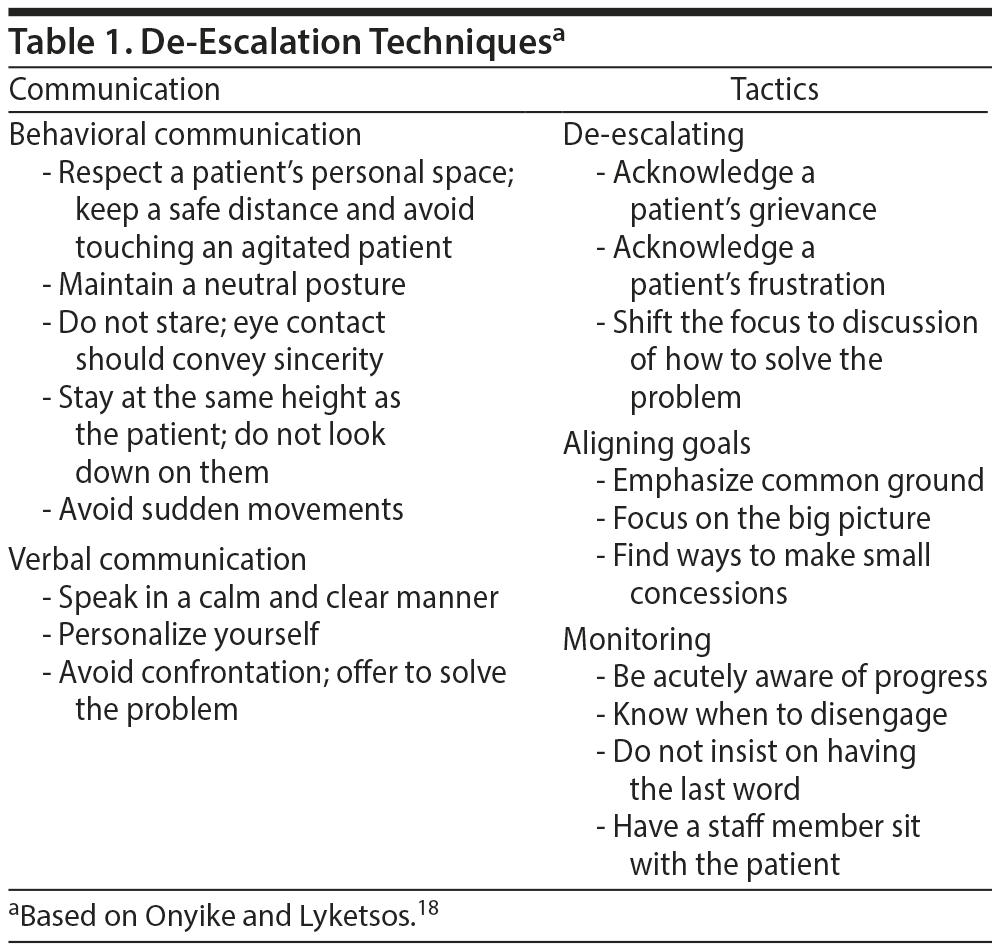
In the case of the severely agitated patient, first and foremost, safety of the environment (eg, checking for weapons using hand or metal detectors and conducting a room search with security) must be assured.18 In all cases, physicians should employ verbal de-escalation techniques, as outlined in Table 1. When de-escalation techniques fail, physical and verbal restraints may be required in the acute setting. Additional policies may be used at a systemic level to increase safety, and physicians should be aware of the policies at their institutions. Institutional policies should include a mechanism for alerting staff about escalating patients and guidelines for calling security. For a more complete list of protective measures, see Table 2.

WHAT IS THE DIFFERENTIAL
DIAGNOSIS FOR ANGER IN AN ADULT?
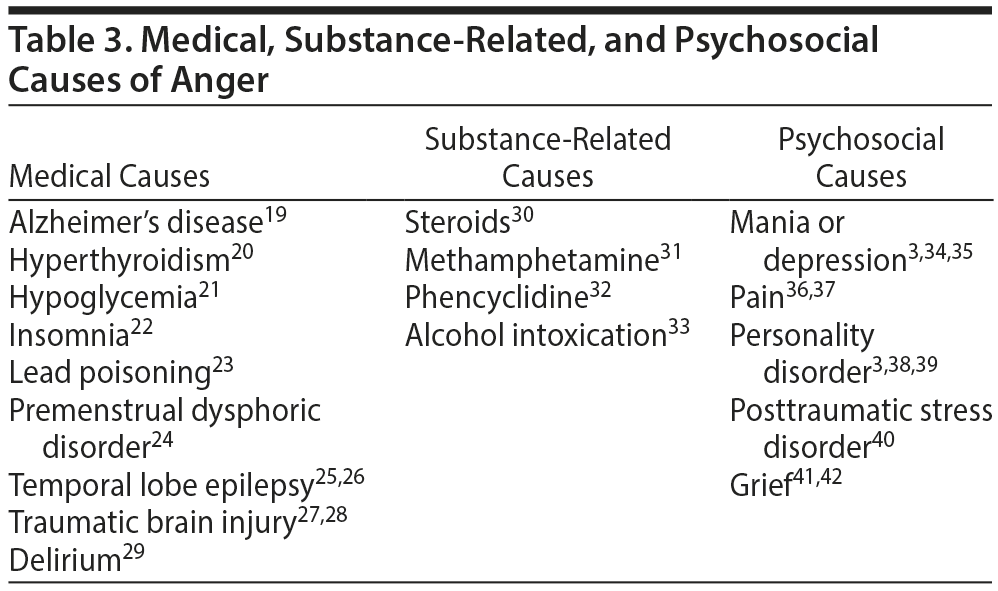
While anger is a normal emotional response to certain situations, in other circumstances, it can be maladaptive or an indication of an underlying medical, substance-related, or psychosocial condition (Table 3). When anger is a symptom of one of these diagnoses, it is important to treat the underlying condition.
WHAT CAUSES ANGER IN HEALTH CARE SETTINGS?
While correlates of anger need to be considered, it is also important to recognize and address the origin of anger. Unfortunately, not all patients are able to correctly identify the root cause of their anger.43 People can often quickly and accurately identify the immediate triggers of anger, but they are less proficient at recognizing the larger contextual landscape from which the anger arises. For example, a patient may be able to identify the immediate frustration that set them off, such as a delayed surgery, but be less proficient at understanding other predisposing factors to anger, such as the stress of the surgery itself and concern over one’s general health. This shortsighted understanding of the causes of anger has been termed the proximity bias.44 Due to this bias, it is important for health care providers to explore with patients the root cause of their anger.
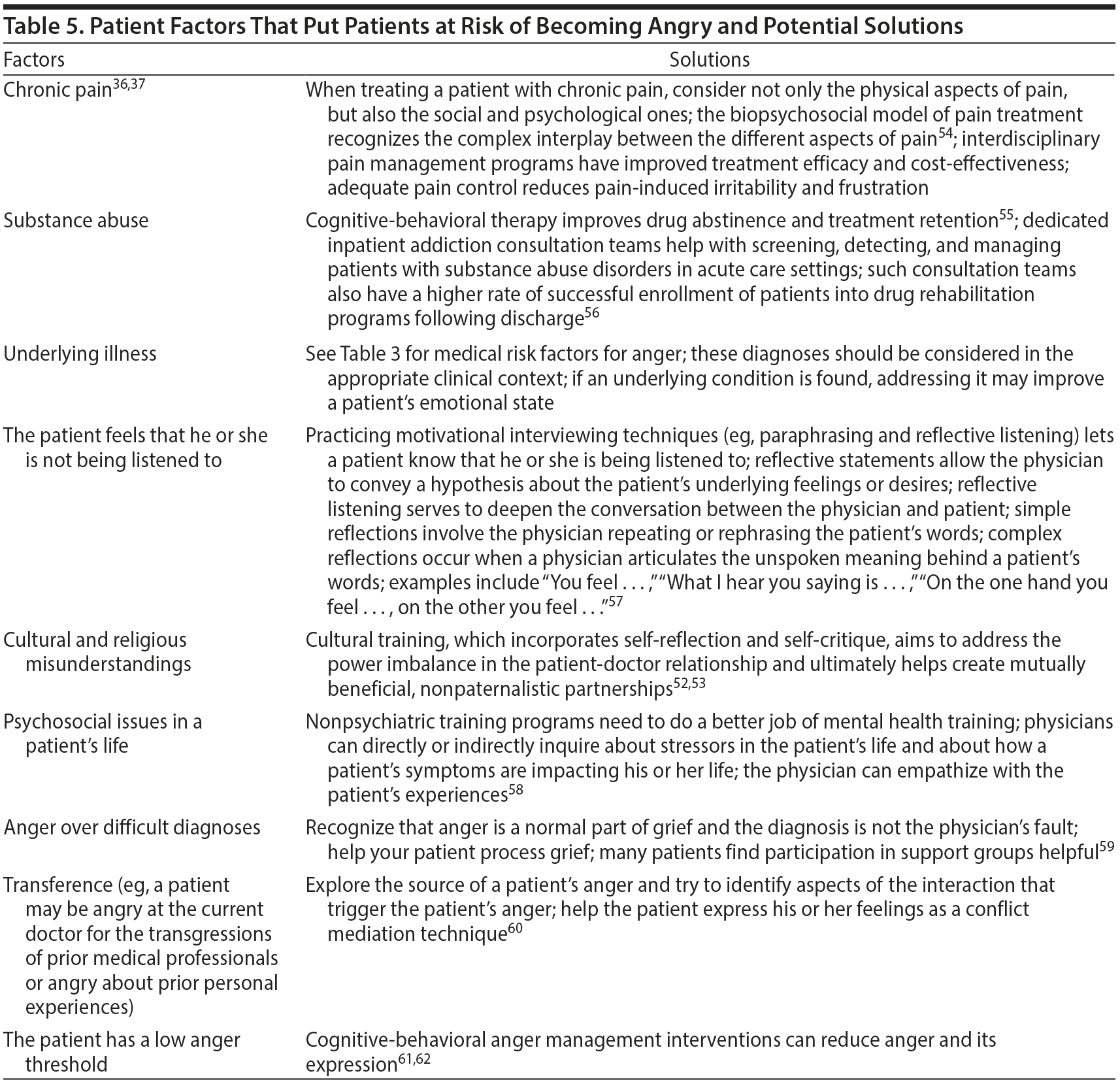
Common provider, patient, and systemic factors that regularly cause anger in health care settings and their corresponding solutions are presented in Tables 4–6. Physicians and hospitals can attempt to prevent patient anger by addressing each of these causative factors. For example, physicians can attempt to prevent the development of patient anger by improving communication and bedside manner and minimizing significant delays, while hospitals can similarly work to minimize the cost of care and to improve efficiency in patient care.


CASE DISCUSSION
The case of Mr A (vignette 1) illustrates how misunderstandings and distrust can set the stage for patient anger. Mr A’s deep distrust of the health care system was evident in his assumption that the system was trying to make money off of him and his care. He believed that he was admitted to the hospital so he could receive IV antibiotics, something that he could get at his hemodialysis center. He did not understand that the main purpose of admitting him was to discover the cause of his bacteremia. He similarly did not understand why the emergency department physician was attempting to do a physical examination. He felt that his problem had already been diagnosed. The purpose of the physical examination was to identify the source of the pseudomonas bacteremia, as well as whether he had any pressure ulcers on his right leg stump or left foot. Unfortunately, Mr A rapidly progressed along the anger continuum from calm and nonthreatening to physically violent before the physician could explain the rationale behind the hospitalization and the examination. When patients become physically violent, physicians’ must first ensure their own safety and the safety of other patients and staff. Hospital security can accompany the physician to see the patient so they are on the scene if required. In the case of Mr A, the physician should first use de-escalation techniques to try to calm him down. The physician should speak calmly and maintain a neutral posture at a safe distance from Mr A, always remaining between the patient and the door. From this position, the physician can acknowledge Mr A’s frustration and align their goals by telling Mr A that the physician also wants to get him home as soon as possible but wants to make sure that when he goes home he is safe and won’t become so ill that he ends up needing to be in the hospital for a longer period of time. If verbal de-escalation fails to calm Mr A down and he remains assaultive, physical or chemical restraints may be necessary.
In Mr A’s case, once the reasoning behind the admission was explained, he agreed to stay in the hospital overnight. He was also willing to compromise with his physicians, and while he continued to refuse to have his stump examined, he did consent to X-rays and computed tomographic imaging, which helped diagnose a soft tissue infection on his stump. He was treated and discharged.
The case of Ms B (vignette 2), which occurs in a primary care setting, describes a situation in which the patient disagrees with her doctors about her diagnosis and treatment plan. The patient feels that her health care providers are not listening to her. Given the benefit of being in a nonacute environment, the new physician could start by affirming that the patient does know her body best, thus acknowledging the patient’s own beliefs and making her feel listened to. The physician could then explain that they need to work together as a team to discover what is causing her abdominal pain. By carefully explaining why the symptoms that Ms B reported do not fit with the diagnosis of Crohn’s disease, the physician demonstrates that he or she paid attention to Ms B’s symptoms and why Crohn’s disease is unlikely. The physician could explore why Ms B is fixated on Crohn’s disease as a diagnosis and address the underlying concern or need. Perhaps the patient feels that her friends and family think she is making up her symptoms and she desperately wants a “real” diagnosis to prove them wrong. Or, the patient might have remote experience with a friend or family member who has that same diagnosis. The physician can then address this concern head-on as well as explore any underlying proximity biases that may be propagating Ms B’s anger.
Patients are unique, and strategies that work with one patient in a particular situation may not work with a different patient or slightly different situation. Thus, the primary purpose of our discussion is to provide tools to equip physicians with strategies to recognize subtle warning signs of brewing anger, minimize impulsive response to patient anger, and consider secondary causes of anger.
CONCLUSION
As our vignettes intended to illustrate, anger compromises patient care. Anger is manifest in multiple ways and for a variety of reasons and can occasionally become dangerous. Therefore, it is important for physicians to recognize when a patient is angry, determine the cause of the anger, and implement de-escalation techniques to improve care.
REFERENCES
1. Novaco RW. Aggression. In: Friedman H, ed. Encyclopedia of Mental Health. San Diego, CA: Academic Press; 1998:13.
2. Spielberger CD, Jacobs G, Russell JS, et al. Assessment of anger: the State-Trait Anger Scale. In: Butcher JN, Spielberger CD, eds. Advances in Personality Assessment, vol 2. Hillside, NJ: Erlbaum; 1983:159–187.
3. Lubke GH, Ouwens KG, de Moor MH, et al. Population heterogeneity of trait anger and differential associations of trait anger facets with borderline personality features, neuroticism, depression, attention-deficit/hyperactivity disorder (ADHD), and alcohol problems. Psychiatry Res. 2015;230(2):553–560. doi:10.1016/j.psychres.2015.10.003 PubMed
4. Kay SR, Wolkenfeld F, Murrill LM. Profiles of aggression among psychiatric patients, II: covariates and predictors. J Nerv Ment Dis. 1988;176(9):547–557. doi:10.1097/00005053-198809000-00008 PubMed
5. Friedman E. Johns Hopkins Hospital: gunman shoots doctor, then kills self and mother. September 16, 2010. ABC News Web site. http://abcnews.go.com/US/shooting-inside-baltimores-johns-hopkins-hospital/story?id=11654462. Accessed May 16, 2016.
6. Aragon C. Surgeon dies after being shot by patient. Cebu City, Philippines. July 24, 2014. Cebu Daily News Web site. http://cebudailynews.inquirer.net/37094/patient-kills-doctor-then-self-in-clinic. Accessed May 16, 2016.
7. Allen E. Fury entered here. Boston, MA. March 8, 2015. The Boston Globe Web site. https://www.bostonglobe.com/metro/2015/03/08/fury-entered-here-what-led-shooting-brigham-and-women-doctor-jan/14mg6ma0UcTQ4nQXAzuU5I/story.html. Accessed May 16, 2016.
8. Healthcare crime survey. IHSS Foundation Web site. http://ihssf.org/PDF/2015crimesurvey.pdf. Accessed February 23, 2016.
9. Weapons use among hospital security personnel. IHSS Foundation Web site. http://ihssf.org/PDF/weaponsuseamonghosptial
securitypersonnel2014.pdf. Accessed February 23, 2016.
10. Rosenthal E. When the hospital fires the bullet. The New York Times. February 14, 2016: A1.
11. Hospital patient shot in altercation with security officer in Lynchburg. Richmond Times Dispach Web site. http://www.richmond.com/news/virginia/article_d6995e4d-4818-5c37-84a3-08b73cfec418.html. Accessed February 23, 2016.
12. Gordon C, Beresin EV. The doctor-patient relationship. In: Stern TA, Fava M, Wilens TE, et al, eds. Massachusetts General Hospital Comprehensive Clinical Psychiatry. 2nd ed. Philadelphia, PA: Elsevier Health Sciences; 2016:1–7.
13. Ong LML, de Haes JC, Hoos AM, et al. Doctor-patient communication: a review of the literature. Soc Sci Med. 1995;40(7):903–918. doi:10.1016/0277-9536(94)00155-M PubMed
14. Kraman SS, Hamm G. Risk management: extreme honesty may be the best policy. Ann Intern Med. 1999;131(12):963–967. doi:10.7326/0003-4819-131-12-199912210-00010 PubMed
15. Alschuler CF, Alschuler AS. Developing healthy responses to anger: the counselor’s role. J Couns Dev. 1984;63(1):26–29. doi:10.1002/j.1556-6676.1984.tb02674.x
16. Wilder SS, Sorensen C, eds. Essentials of Aggression Management in Health Care. London, UK: Pearson; 2001:51–58.
17. McNiel DE, Binder RL. Screening for risk of inpatient violence. Law Hum Behav. 1994;18(5):579–586. doi:10.1007/BF01499176
18. Onyike CU, Lyketsos CG. Aggression and violence. In Levenson JL and Wulsin L. The American Psychiatric Publishing Textbook of Psychosomatic Medicine: Psychiatric Care of the Medically Ill. Arlington, VA: American Psychiatric Publishing, Inc; 2011:161–168.
19. Lyketsos CG, Lopez O, Jones B, et al. Prevalence of neuropsychiatric symptoms in dementia and mild cognitive impairment: results from the cardiovascular health study. JAMA. 2002;288(12):1475–1483. doi:10.1001/jama.288.12.1475 PubMed
20. Stern RA, Robinson B, Thorner AR, et al. A survey study of neuropsychiatric complaints in patients with Graves’ disease. J Neuropsychiatry Clin Neurosci. 1996;8(2):181–185. doi:10.1176/jnp.8.2.181 PubMed
21. Gonder-Frederick LA, Clarke WL, Cox DJ. The emotional, social, and behavioral implications of insulin-induced hypoglycemia. Semin Clin Neuropsychiatry. 1997;2(1):57–65. PubMed
22. Baum KT, Desai A, Field J, et al. Sleep restriction worsens mood and emotion regulation in adolescents. J Child Psychol Psychiatry. 2014;55(2):180–190. doi:10.1111/jcpp.12125 PubMed
23. Rajan P, Kelsey KT, Schwartz JD, et al. Lead burden and psychiatric symptoms and the modifying influence of the δ-aminolevulinic acid dehydratase (ALAD) polymorphism: the VA Normative Aging Study. Am J Epidemiol. 2007;166(12):1400–1408. doi:10.1093/aje/kwm220 PubMed
24. Epperson CN, Steiner M, Hartlage SA, et al. Premenstrual dysphoric disorder: evidence for a new category for DSM-5. Am J Psychiatry. 2012;169(5):465–475. doi:10.1176/appi.ajp.2012.11081302 PubMed
25. van Elst LT, Woermann FG, Lemieux L, et al. Affective aggression in patients with temporal lobe epilepsy: a quantitative MRI study of the amygdala. Brain. 2000;123(pt 2):234–243. doi:10.1093/brain/123.2.234 PubMed
26. Bear D, Levin K, Blumer D, et al. Interictal behaviour in hospitalised temporal lobe epileptics: relationship to idiopathic psychiatric syndromes. J Neurol Neurosurg Psychiatry. 1982;45(6):481–488. doi:10.1136/jnnp.45.6.481 PubMed
27. Neumann D, Malec JF, Hammond FM. The association of negative attributions with irritation and anger after brain injury. Rehabil Psychol. 2015;60(2):155–161. doi:10.1037/rep0000036 PubMed
28. Saban KL, Hogan NS, Hogan TP, et al. He looks normal but . . . challenges of family caregivers of veterans diagnosed with a traumatic brain injury. Rehabil Nurs. 2015;40(5):277–285. doi:10.1002/rnj.182 PubMed
29. Martins S, Fernandes L. Delirium in elderly people: a review. Front Neurol. 2012;3:101. doi:10.3389/fneur.2012.00101 PubMed
30. Su TP, Pagliaro M, Schmidt PJ, et al. Neuropsychiatric effects of anabolic steroids in male normal volunteers. JAMA. 1993;269(21):2760–2764. doi:10.1001/jama.1993.03500210060032 PubMed
31. Lederer K, Fouche JP, Wilson D, et al. Frontal white matter changes and aggression in methamphetamine dependence. Metab Brain Dis. 2016;31(1):53–62. doi:10.1007/s11011-015-9775-9 PubMed
32. McCarron MM, Schulze BW, Thompson GA, et al. Acute phencyclidine intoxication: incidence of clinical findings in 1,000 cases. Ann Emerg Med. 1981;10(5):237–242. doi:10.1016/S0196-0644(81)80047-9 PubMed
33. Steele CM, Josephs RA. Alcohol myopia: its prized and dangerous effects. Am Psychol. 1990;45(8):921–933. doi:10.1037/0003-066X.45.8.921 PubMed
34. Mitchell PB, Loo CK, Gould BM. Diagnosis and monitoring of bipolar disorder in general practice. Med J Aust. 2010;193(suppl 4):S10–S13. PubMed
35. Fava M. Depression with anger attacks. J Clin Psychiatry. 1998;59(suppl 18):18–22.
36. Fernandez E, Turk DC. The scope and significance of anger in the experience of chronic pain. Pain. 1995;61(2):165–175. doi:10.1016/0304-3959(95)00192-U PubMed
37. Okifuji A, Turk DC, Curran SL. Anger in chronic pain: investigations of anger targets and intensity. J Psychosom Res. 1999;47(1):1–12. doi:10.1016/S0022-3999(99)00006-9 PubMed
38. Gardner DL, Leibenluft E, O’Leary KM, et al. Self-ratings of anger and hostility in borderline personality disorder. J Nerv Ment Dis. 1991;179(3):157–161. doi:10.1097/00005053-199103000-00008 PubMed
39. Peters JR, Geiger PJ, Smart LM, et al. Shame and borderline personality features: the potential mediating role of anger and anger rumination. Personal Disord. 2014;5(1):1–9. doi:10.1037/per0000022 PubMed
40. Ehlers A, Clark DM. A cognitive model of posttraumatic stress disorder. Behav Res Ther. 2000;38(4):319–345. doi:10.1016/S0005-7967(99)00123-0 PubMed
41. Patistea E, Makrodimitri P, Panteli V. Greek parents’ reactions, difficulties and resources in childhood leukaemia at the time of diagnosis. Eur J Cancer Care (Engl). 2000;9(2):86–96. doi:10.1046/j.1365-2354.2000.00204.x PubMed
42. Kübler-Ross E, Wessler S, Avioli LV. On death and dying. JAMA. 1972;221(2):174–179. doi:10.1001/jama.1972.03200150040010 PubMed
43. Robins S, Novaco RW. Systems conceptualization and treatment of anger. J Clin Psychol. 1999;55(3):325–337. doi:10.1002/(SICI)1097-4679(199903)55:3<325::AID-JCLP5>3.0.CO;2-O PubMed
44. Novaco RW. Clinicians ought to view anger contextually. Behav Change. 1993;10:208–218.
45. Tabler NG. Dealing with a medical mistake: should physicians apologize to patients? Med Econ. 2013;90(21):36–38, 38. PubMed
46. Opinion 8.121—ethical responsibility to study and prevent error and harm. AMA Web site. http://www.ama-assn.org/ama/pub/physician-resources/medical-ethics/code-medical-ethics/opinion8121.page. Accessed February 17, 2016.
47. Bonvicini KA, Perlin MJ, Bylund CL, et al. Impact of communication training on physician expression of empathy in patient encounters. Patient Educ Couns. 2009;75(1):3–10. doi:10.1016/j.pec.2008.09.007 PubMed
48. Fallowfield L, Jenkins V. Communicating sad, bad, and difficult news in medicine. Lancet. 2004;363(9405):312–319. doi:10.1016/S0140-6736(03)15392-5 PubMed
49. McCord RS, Floyd MR, Lang F, et al. Responding effectively to patient anger directed at the physician. Fam Med. 2002;34(5):331–336. PubMed
50. Neill RA, Mainous AG 3rd, Clark JR, et al. The utility of electronic mail as a medium for patient-physician communication. Arch Fam Med. 1994;3(3):268–271. doi:10.1001/archfami.3.3.268 PubMed
51. Leong SL, Gingrich D, Lewis PR, et al. Enhancing doctor-patient communication using email: a pilot study. J Am Board Fam Pract. 2005;18(3):180–188. doi:10.3122/jabfm.18.3.180 PubMed
52. Tervalon M, Murray-García J. Cultural humility versus cultural competence: a critical distinction in defining physician training outcomes in multicultural education. J Health Care Poor Underserved. 1998;9(2):117–125. doi:10.1353/hpu.2010.0233 PubMed
53. Beach MC, Price EG, Gary TL, et al. Cultural competence: a systematic review of health care provider educational interventions. Med Care. 2005;43(4):356–373. doi:10.1097/01.mlr.0000156861.58905.96 PubMed
54. Gatchel RJ, McGeary DD, McGeary CA, et al. Interdisciplinary chronic pain management: past, present, and future. Am Psychol. 2014;69(2):119–130. doi:10.1037/a0035514 PubMed
55. Dutra L, Stathopoulou G, Basden SL, et al. A meta-analytic review of psychosocial interventions for substance use disorders. Am J Psychiatry. 2008;165(2):179–187. doi:10.1176/appi.ajp.2007.06111851 PubMed
56. Fuller MG, Diamond DL, Jordan ML, et al. The role of a substance abuse consultation team in a trauma center. J Stud Alcohol. 1995;56(3):267–271. doi:10.15288/jsa.1995.56.267 PubMed
57. Douaihy A, Kelly TM, Gold MA, eds. Motivational Interviewing: A Guide for Medical Trainees. New York, NY: Oxford University Press; 2015:43.
58. Teo AR, Du YB, Escobar JI. How can we better manage difficult patient encounters? J Fam Pract. 2013;62(8):414–421. PubMed
59. Spiegel D, Bloom JR, Yalom I. Group support for patients with metastatic cancer: a randomized outcome study. Arch Gen Psychiatry. 1981;38(5):527–533. doi:10.1001/archpsyc.1980.01780300039004 PubMed
60. Lazoritz S. Dealing with angry patients. Physician Exec. 2004;30(3):28–31. PubMed
61. Linkh DJ, Sonnek SM. An application of cognitive-behavioral anger management training in a military/occupational setting: efficacy and demographic factors. Mil Med. 2003;168(6):475–478. PubMed
62. Henwood KS, Chou S, Browne KD. A systematic review and meta-analysis on the effectiveness of CBT informed anger management. Aggress Violent Behav. 2015;25:280–292. doi:10.1016/j.avb.2015.09.011
63. Satterfield JM, Hughes E. Emotion skills training for medical students: a systematic review. Med Educ. 2007;41(10):935–941. doi:10.1111/j.1365-2923.2007.02835.x PubMed
64. Laidlaw TS, MacLeod H, Kaufman DM, et al. Implementing a communication skills programme in medical school: needs assessment and programme change. Med Educ. 2002;36(2):115–124. doi:10.1046/j.1365-2923.2002.01069.x PubMed
65. Halbesleben JRB, Rathert C. Linking physician burnout and patient outcomes: exploring the dyadic relationship between physicians and patients. Health Care Manage Rev. 2008;33(1):29–39. doi:10.1097/01.HMR.0000304493.87898.72 PubMed
66. Irving JA, Dobkin PL, Park J. Cultivating mindfulness in health care professionals: a review of empirical studies of mindfulness-based stress reduction (MBSR). Complement Ther Clin Pract. 2009;15(2):61–66. doi:10.1016/j.ctcp.2009.01.002 PubMed
67. Krasner MS, Epstein RM, Beckman H, et al. Association of an educational program in mindful communication with burnout, empathy, and attitudes among primary care physicians. JAMA. 2009;302(12):1284–1293. doi:10.1001/jama.2009.1384 PubMed
LESSONS LEARNED AT THE INTERFACE
OF MEDICINE AND PSYCHIATRY
The Psychiatric Consultation Service at Massachusetts General Hospital (MGH) sees medical and surgical inpatients with comorbid psychiatric symptoms and conditions. During their twice-weekly rounds, Dr Stern and other members of the Consultation Service discuss diagnosis and management of hospitalized patients with complex medical or surgical problems who also demonstrate psychiatric symptoms or conditions. These discussions have given rise to rounds reports that will prove useful for clinicians practicing at the interface of medicine and psychiatry.
Drs Chipidza and Wallwork are interns in internal medicine at Massachusetts General Hospital, Boston. Dr Adams is a pulmonary/critical care fellow at UT Southwestern Medical Center, Dallas, Texas. Dr Stern is chief of the Avery D. Weisman Psychiatry Consultation Service at Massachusetts General Hospital and the Ned H. Cassem professor of psychiatry in the field of psychosomatic medicine/consultation at Harvard Medical School, Boston, Massachusetts.
Prim Care Companion CNS Disord 2016;18(3):doi:10.4088/PCC.16f01951
© Copyright 2016 Physicians Postgraduate Press, Inc.
Submitted: March 24, 2016; accepted April 28, 2016.
Published online: June 23, 2016.
Potential conflicts of interest: Dr Stern is an employee of the Academy of Psychosomatic Medicine, has served on the speaker’s board of Reed Elsevier, is a stock shareholder in WiFiMD (Tablet PC), and has received royalties from Mosby/Elsevier and the Massachusetts General Hospital Psychiatry Academy and McGraw Hill. Drs Chipidza, Wallwork, and Adams report no conflicts of interest related to the subject of this article.
Funding/support: None.
Corresponding author: Theodore A. Stern, MD, Department of Psychiatry, Massachusetts General Hospital, Fruit St, WRN 605, Boston, MA 02114
([email protected]).
Enjoy this premium PDF as part of your membership benefits!





