Objective: Alcohol-related seizures are acute symptomatic seizures most frequently associated with alcohol withdrawal. However, little is known about the phenotypic characteristics of patients with alcohol-related seizures. This study evaluated the clinical features and personality traits of alcohol use disorder patients with alcohol-related seizures.
Methods: This comparative correlational study assessed the clinical and psychological covariates of alcohol-related seizures. A total of 144 alcohol-dependent patients were recruited from an alcoholism unit from January 2017 to January 2019 and divided into 2 subgroups: alcohol-dependent patients reporting alcohol-related seizures and alcohol-dependent patients with no history of alcohol-related seizures.
Results: The alcohol-related seizures subgroup significantly started to abuse (F = 4.1, P = .019) and depend (F = 0.12, P = .008) on alcohol at an earlier age and had more alcohol detoxification episodes (F = 4.4, P = .048), a higher degree of alcohol dependence severity (F = 0.30, P = .009), and a more frequent family history of alcoholism (χ2 = 4.9, P = .026). These patients also had lower levels of openness to experience (F = 4.0, P = .029) after adjustment for current age, age at onset of alcohol misuse and dependence, severity of alcohol dependence level, number of previous alcohol detoxifications, and family history.
Conclusions: The findings will help clinicians better understand this subgroup of patients and highlight the importance of considering personality traits and other clinical features when tailoring treatment for these individuals.
ABSTRACT
Objective: Alcohol-related seizures are acute symptomatic seizures most frequently associated with alcohol withdrawal. However, little is known about the phenotypic characteristics of patients with alcohol-related seizures. This study evaluated the clinical features and personality traits of alcohol use disorder patients with alcohol-related seizures.
Methods: This comparative correlational study assessed the clinical and psychological covariates of alcohol-related seizures. A total of 144 alcohol-dependent patients were recruited from an alcoholism unit from January 2017 to January 2019 and divided into 2 subgroups: alcohol-dependent patients reporting alcohol-related seizures and alcohol-dependent patients with no history of alcohol-related seizures.
Results: The alcohol-related seizures subgroup significantly started to abuse (F = 4.1, P = .019) and depend (F = 0.12, P = .008) on alcohol at an earlier age and had more alcohol detoxification episodes (F = 4.4, P = .048), a higher degree of alcohol dependence severity (F = 0.30, P = .009), and a more frequent family history of alcoholism (χ2 = 4.9, P = .026). These patients also had lower levels of openness to experience (F = 4.0, P = .029) after adjustment for current age, age at onset of alcohol misuse and dependence, severity of alcohol dependence level, number of previous alcohol detoxifications, and family history.
Conclusions: The findings will help clinicians better understand this subgroup of patients and highlight the importance of considering personality traits and other clinical features when tailoring treatment for these individuals.
Prim Care Companion CNS Disord 2019;21(6):19m02501
To cite: Câmara Pestana P, Novais F, Ismail F, et al. Are patients with alcohol-related seizures a specific subgroup? Prim Care Companion CNS Disord. 2019;21(6):19m02501.
To share: https://doi.org/10.4088/PCC.19m02501
© Copyright 2019 Physicians Postgraduate Press, Inc.
aPsychiatric and Mental Health Service of Santa Maria Hospital, Lisbon, Portugal
*Corresponding author: Pedro Câmara Pestana, MD, Psychiatric and Mental Health Service of Santa Maria Hospital, Avenida Professor Egas Moniz, 1649-035 Lisbon, Portugal ([email protected]).
Alcohol consumption is one of the leading preventable risk factors for population health worldwide.1 Alcohol use disorder (AUD, DSM-5 criteria) is a common medical problem related to the misuse of alcohol.
Alcohol-related seizures are acute seizures related to alcohol consumption. Although acute intoxication may precipitate seizures,2 alcohol-related seizures are most frequently associated with alcohol withdrawal,3 occurring in up to 30% of patients experiencing alcohol withdrawal4 as a rebound phenomenon after abrupt cessation of prolonged intoxication.2 The withdrawal symptoms typically occur within 8 hours of stopping heavy or prolonged drinking, reach maximal intensity on day 2, and resolve by day 4 to 5.5 Severe withdrawal occurs in about 5% of patients and can also induce delirium tremens, wherein generalized tonic-clonic seizures, postictal confusion, and disorientation are more obvious signs of severe withdrawal.5
Seizures can be defined as transient signs and symptoms due to abnormal, excessive, or synchronous neuronal activity in the brain. They comprise a broader spectrum of clinical manifestations rather than a specific disease entity,5 as several diseases can lead to clinical seizures, namely febrile states and nonepileptic physiologic events such as alcohol and sedative deprivation. If not appropriately treated, alcohol abuse can cause status epilepticus in 9%–25% of patients, and this condition may be these patients’ first presentation.2 Alcohol abuse is also a major risk factor for epilepsy, which is overrepresented in those dependent on alcohol.2
Although alcohol-related seizures are common and dangerous manifestations of AUD, the literature seems to show reduced interest in this occurrence. Studies are scarce and focus primarily on the electrophysiology, pathophysiology, and clinical management of alcohol-related seizures,2 and little is known about the phenotypic characteristics of these patients. A few studies6,7 have attempted to risk stratify patients at risk for alcohol-related seizures, while others explored the clinical course of AUD8 or the potential associations between alcohol-related seizures and depression, age, and mild cognitive impairment.9,10 In this regard, Lesch et al11 argue that patients with alcohol-related seizures but without epilepsy are physiologically vulnerable to relapse and craving. In fact, alcohol is commonly used as “self-medication” to prevent withdrawal symptoms.12
These observations raise further questions. Could these patients be vulnerable from a psychological point of view, for instance, in terms of personality functioning? As far as we know, no studies have assessed the potential association between alcohol-related seizures and personality traits, as only the association between epilepsy and personality traits has been explored.13,14 Therefore, we aimed to evaluate the clinical features and personality traits of AUD patients with alcohol-related seizures.
METHODS
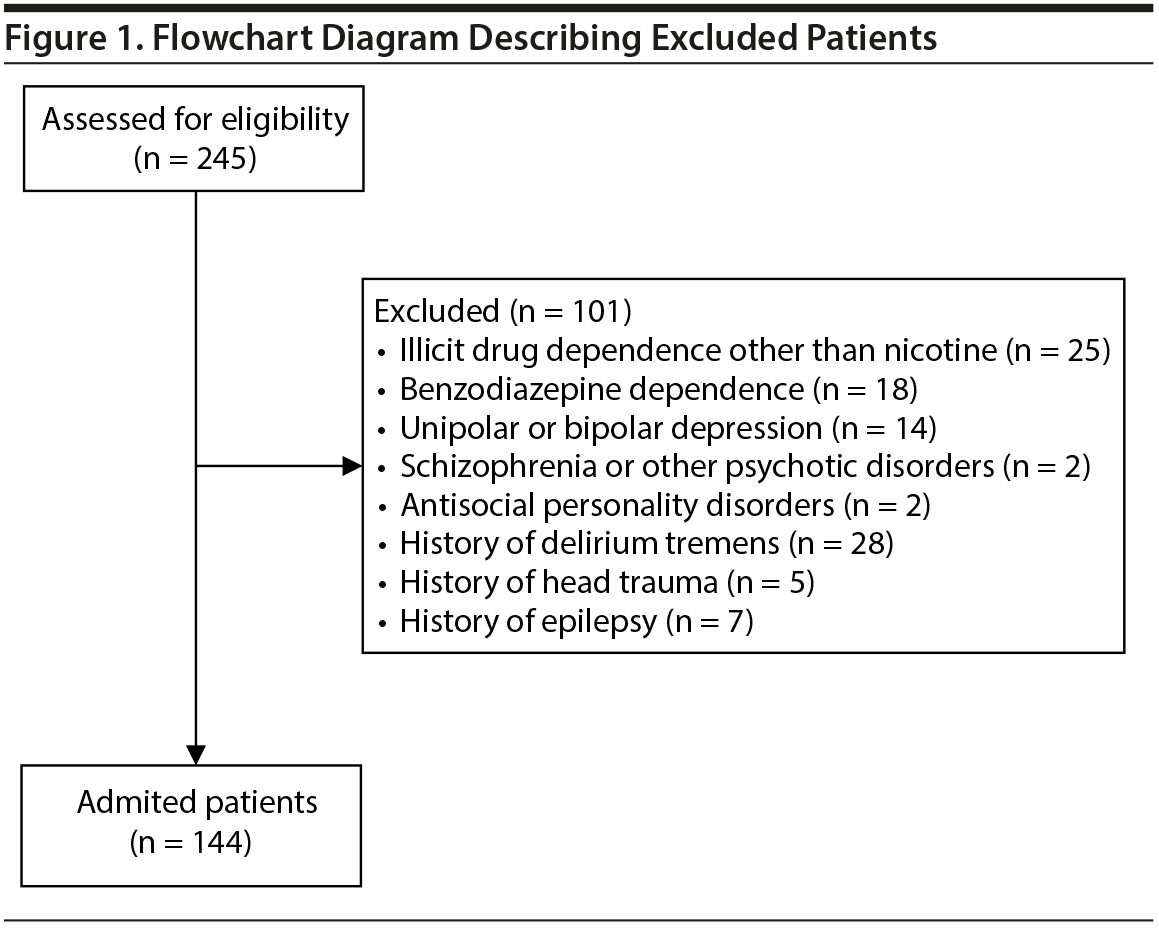
A comparative correlational study was designed and approved by the local ethics board of the Academic Medical Center of Lisbon, Lisbon, Portugal. Participants were recruited from the alcoholism unit of the Psychiatric Service of Santa Maria University Hospital in Lisbon, Portugal, and the initial sample comprised 245 patients. Clinical and sociodemographic information was collected from January 2017 to January 2019 at hospital admission with a standardized clinical interview adapted to alcoholic patients. Clinical conditions that could interact with the study analysis were carefully evaluated, particularly psychiatric comorbidity. All enrolled subjects underwent a screening procedure that involved the semistructured Mini-International Neuropsychiatric Interview.15 Patients were excluded if they met criteria for illicit drug dependence other than nicotine (n = 25), benzodiazepine dependence (n = 18), unipolar or bipolar depression (n = 14), other psychiatric disorders such as schizophrenia or other psychotic disorders (n = 2), antisocial personality disorders (n = 2), history of delirium tremens (n = 28), history of head trauma (n = 5), or history of epilepsy (n = 7). Other exclusion criteria were < 18 years of age, state of intoxication (alcoholic or other) during the assessment, and marked cognitive deficit or mental retardation. A total of 144 patients remained in the study and provided informed consent (Figure 1).
Measures
Semistructured interview for alcohol-dependent patients. This interview explores patients’ sociodemographic and drinking information and has been used in several other studies.16,17
Seizure assessment. Seizures were documented on self or collateral history and then confirmed using clinical records from emergency services and neurologic consultations.
Mini Neuropsychiatric Interview (MINI). The MINI is a short structured diagnostic interview created to assess 17 psychiatric disorders. It takes approximately 15 minutes to complete and can be easily incorporated into clinical practice.15 The MINI is available in almost 30 languages, including Portuguese.18
Quantity-frequency (QF) method. The QF formula was used to compute the mean number of drinking days over a typical week and the mean number of drinks consumed per day. The QF drinking variable was then calculated as the product result of those measures into the mean number of standard drinks per week. In abstinence cases, patients were asked about the last week of alcohol consumption before they stopped drinking alcohol.
Severity Alcohol Dependence Questionnaire (SADQ). The SADQ is a self-administered questionnaire developed to measure alcohol dependence severity.19 The questionnaire is divided into 5 sections, namely frequency of alcohol consumption, physical withdrawal symptoms, affective withdrawal symptoms, speed of onset of withdrawal symptoms, and relief drinking.
NEO Five-Factor Inventory (NEO-FFI). The NEO-FFI is a reduced version of the NEO Personality Inventory.20 It provides a comprehensive overview of emotional, interpersonal, attitudinal, and motivational styles, reporting on the 5 personality factors of openness, conscientiousness, extraversion, agreeableness, and neuroticism. The Portuguese version of the NEO-FFI has been validated by Bertoquini and Pais-Ribeiro.21
Statistical Analysis
The normal distribution of the psychometric measures was confirmed using the Kolmogorov-Smirnov test. Parametric methods were used to calculate numerical relations among variables. Sex-based distributions of baseline sociodemographic and drinking data were assessed using χ2 and student t tests. Pearson correlation test was applied to continuous variables. A preliminary exploratory analysis was conducted before all variables were investigated separately within the 2 cohorts. Finally, assuming a significant interaction between some of the variables, 1-way analysis of covariance (ANCOVA) was performed to assess whether the subgroup differences of the dependent variable (alcoholic seizures) were attributable to covariate factors. All categorical variables were dummy coded (eg, women received code 0 and men received code 1; negative family history of alcoholism received code 0 and positive family history received code 1). Data were analyzed using the Statistical Package for Social Sciences software (SPSS Version 21.0, IBM Corp, Armonk, New York). Statistical significance was defined at P < .05.
RESULTS
Sociodemographic and
Clinical Characteristics of the Sample
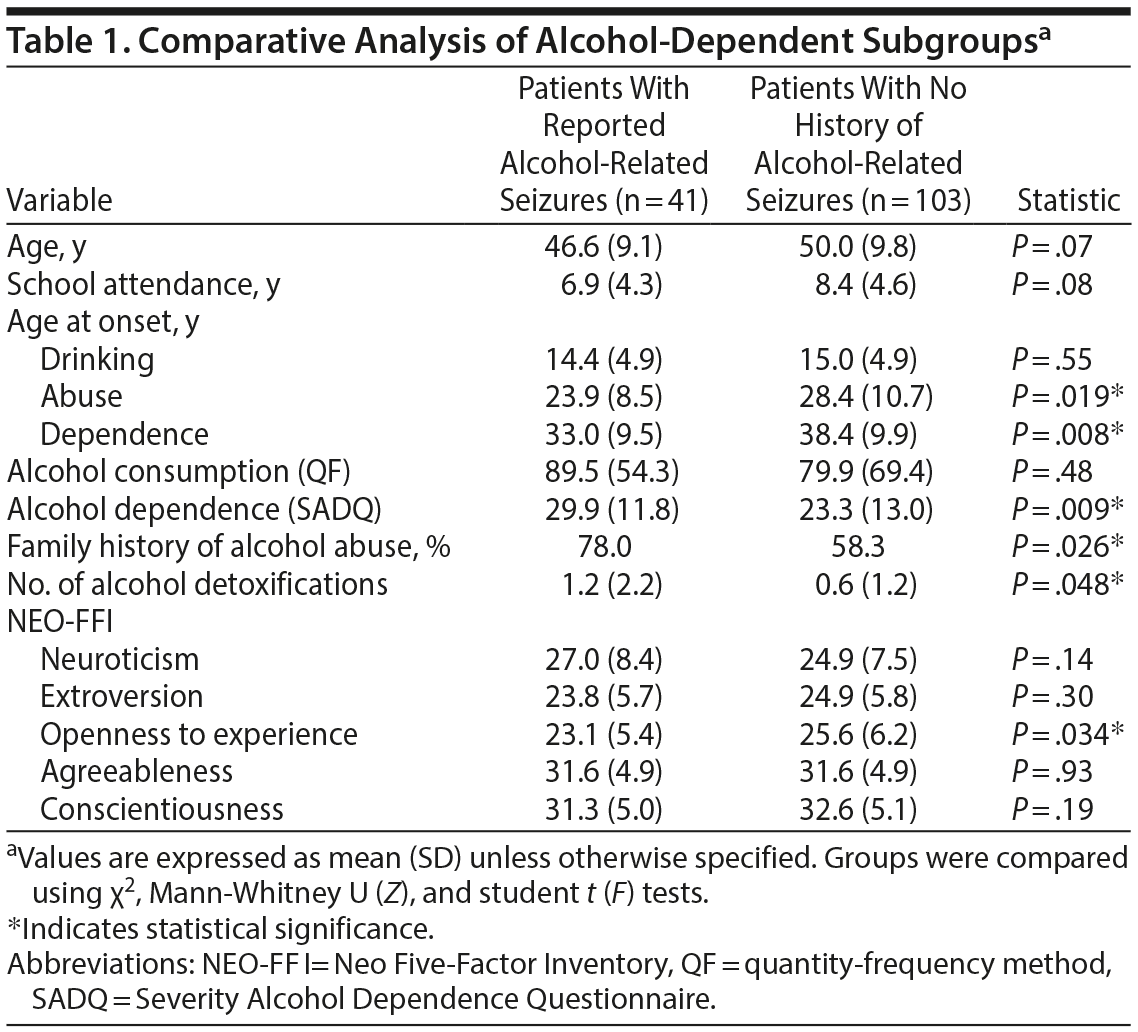
The sample comprised 144 alcohol-dependent patients: 113 (78.5%) men and 31 (21.5%) women. There were no significant differences between groups by sex (P > .05). The cohorts were composed of 41 alcohol-dependent patients with alcohol-related seizures (28.5% of the sample) and 103 alcohol-dependent patients without seizures (71.5%) (Table 1). Age of the patients ranged from 28 to 68 years, with a mean of 49.0 years (SD = 9.8). The sample was white; 56.3% were married or lived in marital union, while 13.9% were single and 27.8% were separated or divorced. The patients had attended school for a mean of 7.9 years (SD = 4.6); 14.6% were nonqualified workers, 32.6% were employed, 29.9% were unemployed, and 22.9% were retired.
With regard to alcohol use, the mean ages were 14.8 for drinking onset (SD = 4.9), 27.0 for excessive alcohol use (SD = 10.3), and 36.8 for alcohol dependence (SD = 10.0). More than half of the sample had a family history of alcoholism (0.9%). Alcoholic seizures were reported in 28.5% of the patients, and 38.2% had a history of detoxification (mean = 0.78, SD = 1.6). The mean severity of alcohol dependence (SADQ score) was 25.1 (SD = 13.0). Regarding nicotine use, the mean number of cigarettes smoked per day was 24.8 (SD = 12.1), and the mean age of nicotine use onset was 15.3 years (SD = 3.0). Of the alcohol-dependent patients, 77.3% reported being alcohol free (16.1 weeks on average) and 26.7% reported being currently in a drinking period. The mean number of standard drinks per week was 82.8 (QF method). Male patients started to abuse alcohol earlier in their lives than females (P < .05). No other significant differences were found.
Correlates of Alcohol-Related Seizures
Compared to the alcohol-dependent group without seizures, patients in the alcohol-related seizures subgroup started to abuse (F = 4.1, P = .019) and depend (F = 0.12, P = .008) on alcohol at a significantly earlier age. They also had a higher number of previous alcohol detoxifications (F = 4.4, P = .048), degree of alcohol dependence severity (F = 0.30, P = .009), and family history of alcoholism (χ2 = 4.9, P = .026).
Personality Covariates of Craving
Each NEO-FFI temperament factor was separately correlated with sociodemographic and clinical features. Openness to experience negatively correlated with age (r2 = −0.18, P = .037) and neuroticism directly correlated with the SADQ score (r2 = 0.25, P = .005). No other significant associations were found.
Group comparison revealed statistically significant differences in NEO–FFI dimensions. Following an ANCOVA, corrected Bonferroni comparison tests showed that patients with alcohol-related seizures had lower levels of openness to experience (F = 4.0, P = .029) after controlling for factors such as current age (P = .11), age at onset of alcohol misuse (P = .84) and dependence (P = .71), severity of alcohol dependence level (P = .56), number of previous alcohol detoxifications (P = .21), and positive history of AUD in the family (P = .12).
DISCUSSION
Our results show that the alcohol-related seizures subgroup started to abuse and depend on alcohol at a significantly earlier age than alcohol-dependent patients without seizures. These patients also had a higher number of previous alcohol detoxifications, a higher degree of alcohol dependence severity, and more frequent family history of AUD. Moreover, these patients revealed lower levels of openness to experience.
Our study confirms previous findings documenting the relation between alcohol-related seizures and a long-term alcohol dependence history,4 probably involving kindling, a process in which the brain, following repeated subthreshold electrical stimulations in the past, is likely to progressively demonstrate more severe motor overactivity.6 The higher alcohol dependence severity in patients with a family history of AUD is in line with the alcoholic phenotype defined as type 1, wherein alcohol-related seizures and family history are both relevant diagnostic criteria.16,22
Regarding personality traits, openness to experience is a crucial trait linked to a broad range of cognitive-affective styles such as a preference for novel experiences, curiosity, and creativity.23 A positive relationship between openness, creativity, and bipolar disorder has been reported.24 However, higher levels of openness to experience, strongly related with the sensation-seeking construct, have also been associated with a higher risk of substance use and addiction.25 Indeed, a study26 found that openness to experience was an important predictor of multiple substance use in alcohol-dependent outpatients. On the other hand, low levels of openness to experience seem to be linked with increased odds of reducing alcohol consumption and preferring abstinence.27
Our study showed that the alcohol-related seizure subgroup had lower levels of openness to experience. More restrictions in daily activity or functioning and communication problems have been observed in patients with alcohol-related seizures9 and may suggest that, at least partially, lower levels of openness to experience may be a consequence of the condition. Additionally, it has been demonstrated that epilepsy-related factors, including early age at onset and higher seizure frequency, significantly impact personality traits.13 Some hypotheses have been proposed to explain these associations, namely the psychosocial impact of continued seizures during the development of personality and self-identity.28 Although it is known that personality traits are relatively stable during the lifespan, they may change due to environmental influences. For instance, the use of alcohol itself has been associated with personality trait changes in adulthood.29 The continued negative impact of the experience of a seizure, acting as a “punitive sign,” may render individuals less prone to experiment according to the model of Cloninger.30 Moreover, the direct effect of epileptic activity in temporal and frontal lobes may contribute to these traits,14 as positive associations have been established between openness to experience, increased mesocortical connectivity,23 and decreased myelination in the brain imaginative network and regions related to motivational state.24
However, we also consider that less openness to experience might constitute a premorbid personality trait. Therefore, as lower levels of openness to experience seem to be protective,27 other risk factors may be more predictive of the development of alcohol dependence in the alcohol-related seizures subgroup. On the other hand, according to the Lesch alcoholism typology,12 the alcohol-related seizure subgroup, defined as type 1, seems to have an increased biological vulnerability characterized by more severe abstinence symptoms, more intense craving, and a potentially higher genetic load. These individuals may be particularly prone to develop dependence at earlier ages and have a higher degree of dependence severity due to this important biological vulnerability. Thus, personality factors in these patients become less important as risk factors for the disease.
Regarding the relationship between personality and treatment approaches, the possibility that personality traits may affect the utilization, course, and effectiveness of various treatments of mental disorders has been investigated.31 Notably, a few studies8,12,32 indicate that personality traits should be considered when refining treatment programs, arguing that interventions matched to relevant personality traits may improve treatment outcomes for substance misusers.32
Thus, our findings may have some relevant clinical implications, namely reinforcing the importance of personality trait assessment before alcohol detoxification admission, not only as part of an alcohol-related seizure risk-stratification strategy together with the personal and family history of alcohol use, but also as a way to refine the treatment program.
The present study had several limitations. We recognize the sample size was relatively small, and we were unable to obtain electroencephalographic (EEG) confirmation of seizures for every patient. However, the diagnosis of a seizure is clinical, which means that these well-established data may in themselves be enough for diagnosis, as EEG and imaging only provide supplementary information to support the diagnosis. In other words, the presence of epileptiform activity in EEG and imaging is suggestive but not enough to establish the diagnosis without the convincing clinical presentation of seizures. Considering that patients frequently cannot recall seizures, we sought a collateral history from seizure observers. We also recognized that our choice of exclusion criteria, namely illicit drug dependence, unipolar or bipolar depression, or history of delirium tremens, may have limited the characterization of some components of the alcohol-related seizure subgroup phenotype. However, since alcohol-related seizures could be extensively influenced by multiple conditions, for this analysis we decided to increase the homogeneity of our sample and, consequently, data reliability. Future studies, including the variables we opted to exclude with a subsequent sensitivity analysis, could add information to the study of the alcohol-related seizure phenotype. Since not only seizures but also changes in alcohol consumption could lead to changes in personality traits over time,14,29 it would be interesting to perform a personality assessment after alcohol abstinence or after the last alcohol-related seizure to clarify the consistency of our findings. Finally, despite the excluded criteria and controlled variables, personality can also be affected by other difficult-to-quantify environmental factors.
In conclusion, our results indicate that AUD patients with alcohol-related seizures are a specific subgroup of alcohol-dependent patients. These findings will help clinicians better understand and characterize this subgroup of patients and highlight the importance of considering personality traits and these clinical features not only as a part of an alcohol-related seizure risk-stratification strategy but also when tailoring treatment for these individuals.
Submitted: June 18, 2019; accepted July 31, 2019.
Published online: November 7, 2019.
Potential conflicts of interest: Dr Câmara Pestana reports nonfinancial support outside the submitted work from Janssen-Cilag Farmacêutica, Lundbeck Portugal-Produtos Farmacêuticos Lda, Servier Portugal-Especialidades Farmacêuticas Lda, and Sanofi-Produtos Farmacêuticos Lda. Drs Novais, Ismail, and Pombo report no potential conflicts of interest related to the subject of this article.
Funding/support: None.
Acknowledgments: The authors thank Liliana Sousa Nanji, MD, MSc (St Vincent’s Hospital, Melbourne, Australia), for assistance with the critical review of the manuscript. Dr Sousa Nanji reports no conflicts of interest related to the subject of this article.
REFERENCES
1. Global Status Report on Alcohol and Health 2018. World Health Organization website. https://apps.who.int/iris/bitstream/handle/10665/274603/9789241565639-eng.pdf?ua=1. Accessed September 26, 2019.
2. Hillbom M, Pieninkeroinen I, Leone M. Seizures in alcohol-dependent patients: epidemiology, pathophysiology and management. CNS Drugs. 2003;17(14):1013–1030. PubMed CrossRef
3. Beghi E, Carpio A, Forsgren L, et al. Recommendation for a definition of acute symptomatic seizure. Epilepsia. 2010;51(4):671–675. PubMed CrossRef
4. Victor M, Brausch C. The role of abstinence in the genesis of alcoholic epilepsy. Epilepsia. 1967;8(1):1–20. PubMed CrossRef
5. Arciniegas DB, Yudofsky SC, Hales RE, eds. The American Psychiatric Association Publishing Textbook of Neuropsychiatry and Clinical Neurosciences. 6th Edition. Washington, DC: American Psychiatry Association Publishing; 2018.
6. Eyer F, Schuster T, Felgenhauer N, et al. Risk assessment of moderate to severe alcohol withdrawal—predictors for seizures and delirium tremens in the course of withdrawal. Alcohol Alcohol. 2011;46(4):427–433. PubMed CrossRef
7. Rathlev NK, Ulrich A, Fish SS, et al. Clinical characteristics as predictors of recurrent alcohol-related seizures. Acad Emerg Med. 2000;7(8):886–891. PubMed CrossRef
8. Pombo S, da Costa NF, Figueira ML, et al. Multidimensional alcoholism typologies: could they guide clinical practice? results from a 3-month prospective study. Int J Psychiatry Clin Pract. 2015;19(2):137–147. PubMed CrossRef
9. Gutmane E, Suna N, Tomilova A, et al. Alcohol-related seizures may be associated with more severe depression, alcohol dependence syndrome, and more pronounced alcohol-related problems. Epilepsy Behav. 2019;91:81–85. PubMed CrossRef
10. Ishii N, Terao T, Araki Y, et al. Repeated seizures in an elderly patient with alcohol dependence and mild cognitive impairment. BMJ Case Rep. 2013;2013:bcr2013201575. PubMed CrossRef
11. Lesch OM, Walter H. Wetschka, et al. Alcohol and Tobacco: Medical and Sociological Aspects of Use, Abuse and Addiction. New York, NY: Springer Wein New York; 2011.
12. Schlaff G, Walter H, Lesch OM. The Lesch alcoholism typology—psychiatric and psychosocial treatment approaches. Ann Gastroenterol. 2011;24(2):89–97. PubMed
13. Wang X, Lv Y, Zhang W, et al. Cognitive impairment and personality traits in epilepsy: characterization and risk factor analysis. J Nerv Ment Dis. 2018;206(10):794–799. PubMed CrossRef
14. Pizzi AM, Chapin JS, Tesar GE, et al. Comparison of personality traits in patients with frontal and temporal lobe epilepsies. Epilepsy Behav. 2009;15(2):225–229. PubMed CrossRef
15. Sheehan DV, Lecrubier Y, Sheehan KH, et al. The Mini-International Neuropsychiatric Interview (M.I.N.I.): the development and validation of a structured diagnostic psychiatric interview for DSM-IV and ICD-10. J Clin Psychiatry. 1998;59(suppl 20):22–33. PubMed
16. Pombo S, Lesch OM. The alcoholic phenotypes among different multidimensional typologies: similarities and their classification procedures. Alcohol Alcohol. 2009;44(1):46–54. PubMed CrossRef
17. Pombo S, Figueira ML, da Costa NF, et al. The burden of cyclothymia on alcohol dependence. J Affect Disord. 2013;151(3):1090–1096. PubMed CrossRef
18. Amorim P, Guterres T. MINI Entrevista Neuropsiquiátrica Internacional.Versão Portuguesa 4.4. Copyright Version. 1996.
19. Stockwell T, Murphy D, Hodgson R. The Severity of Alcohol Dependence Questionnaire: its use, reliability and validity. Br J Addict. 1983;78(2):145–155. PubMed CrossRef
20. Costa PT, McCrae RR. Revised Neo Personality Inventory (NEO PI-R) and Neo Five-Factor Inventory (Neo-FFI) : Professional Manual. Odessa, FL: PAR; 1992.
21. Bertoquini V, Pais Ribeiro J. Estudo de formas muito reduzidas do modelo dos cinco factores da personalidade. Psychologica. 2006;43:193–210.
22. Lesch OM, Dietzel M, Musalek M, et al. The course of alcoholism: long-term prognosis in different types. Forensic Sci Int. 1988;36(1–2):121–138. PubMed CrossRef
23. Passamonti L, Terracciano A, Riccelli R, et al. Increased functional connectivity within mesocortical networks in open people. Neuroimage. 2015;104:301–309. PubMed CrossRef
24. Yasuno F, Kudo T, Yamamoto A, et al. Significant correlation between openness personality in normal subjects and brain myelin mapping with T1/T2-weighted MR imaging. Heliyon (Lond). 2017;3(9):e00411. PubMed CrossRef
25. Turiano NA, Whiteman SD, Hampson SE, et al. Personality and substance use in midlife: conscientiousness as a moderator and the effects of trait change. J Res Pers. 2012;46(3):295–305. PubMed CrossRef
26. Novais F, Pombo S, Ismail F. Predictors of multiple substance use in alcohol dependence: the role of personality. J Addict Res Ther. 2016;7(1):258.
27. Hakulinen C, Elovainio M, Batty GD, et al. Personality and alcohol consumption: pooled analysis of 72,949 adults from eight cohort studies. Drug Alcohol Depend. 2015;151:110–114. PubMed CrossRef
28. Wilson SJ, Wrench JM, McIntosh AM, et al. Personality development in the context of intractable epilepsy. Arch Neurol. 2009;66(1):68–72. PubMed CrossRef
29. Hakulinen C, Jokela M. Alcohol use and personality trait change: pooled analysis of six cohort studies. Psychol Med. 2019;49(2):224–231. PubMed CrossRef
30. Cloninger CR, Svrakic DM, Przybeck TR. A psychobiological model of temperament and character. Arch Gen Psychiatry. 1993;50(12):975–990. PubMed CrossRef
31. Hopwood CJ, Quigley BD, Grilo CM, et al. Personality traits and mental health treatment utilization. Pers Ment Health. 2008;2(4):207–217. PubMed CrossRef
32. Staiger PK, Kambouropoulos N, Dawe S. Should personality traits be considered when refining substance misuse treatment programs? Drug Alcohol Rev. 2007;26(1):17–23. PubMed CrossRef
Enjoy this premium PDF as part of your membership benefits!