Objective: To determine if symptoms of social anxiety are distinct from negative symptoms of schizophrenia.
Method: Fifty-three patients with schizophrenia or schizoaffective disorder (diagnosed per DSM-IV criteria) and 37 healthy controls were examined with the Liebowitz Social Anxiety Scale (LSAS) for social anxiety disorder and for the severity of social anxiety. The Positive and Negative Syndrome Scale (PANSS) and the Chapman scales for physical and social anhedonia were also administered. Data were collected from 2005 to 2010 from inpatient and outpatient research centers at the New York State Psychiatric Institute, New York.
Results: Social anxiety disorder was elevated more than 10-fold in schizophrenia patients than in controls (37.7% of patients vs 2.9% of controls, P ≤ .001). Social anxiety and social fear were unrelated to the PANSS with few exceptions. A family history of psychosis was also a significant independent predictor of social anxiety as measured by LSAS total (P = .004) and the social fear subscale (P = .007).
Conclusions: These data confirm social anxiety disorder as a prominent comorbid disorder in patients with schizophrenia. Future studies should focus on treatment trials of this phenomenon. Social anxiety cannot be explained by the negative symptomatology of the disease. This study suggests that a family history of psychosis is a significant predictor of social anxiety.
Frequent Comorbidity and Predictors of Social Anxiety in Persons With Schizophrenia: A Retrospective Cohort Study
ABSTRACT
Objective: To determine if symptoms of social anxiety are distinct from negative symptoms of schizophrenia.
Method: Fifty-three patients with schizophrenia or schizoaffective disorder (diagnosed per DSM-IV criteria) and 37 healthy controls were examined with the Liebowitz Social Anxiety Scale (LSAS) for social anxiety disorder and for the severity of social anxiety. The Positive and Negative Syndrome Scale (PANSS) and the Chapman scales for physical and social anhedonia were also administered. Data were collected from 2005 to 2010 from inpatient and outpatient research centers at the New York State Psychiatric Institute, New York.
Results: Social anxiety disorder was elevated more than 10-fold in schizophrenia patients than in controls (37.7% of patients vs 2.9% of controls, P ≤ .001). Social anxiety and social fear were unrelated to the PANSS with few exceptions. A family history of psychosis was also a significant independent predictor of social anxiety as measured by LSAS total (P = .004) and the social fear subscale (P = .007).
Conclusions: These data confirm social anxiety disorder as a prominent comorbid disorder in patients with schizophrenia. Future studies should focus on treatment trials of this phenomenon. Social anxiety cannot be explained by the negative symptomatology of the disease. This study suggests that a family history of psychosis is a significant predictor of social anxiety.
Prim Care Companion CNS Disord 2015;17(5):doi:10.4088/PCC.15m01799
© Copyright 2015 Physicians Postgraduate Press, Inc.
aDepartment of Psychiatry, New York University School of Medicine, New York, New York
bLieber Center for Research in Schizophrenia, Columbia University, New York, New York
cDepartment of Psychiatry, Institute for Social and Psychiatric Initiatives (InSPIRES), New York University School of Medicine, New York, New York
dNew York State Psychiatric Institute, New York
*Corresponding author: Dolores Malaspina, MD, MSPH, Institute for Social and Psychiatric Initiatives, New York University School of Medicine, 500 1st Ave, NBV 22N14, New York, NY 10016 ([email protected]).
Schizophrenia remains a chronic and disabling condition in about 1% of the world’s population.1 The heterogeneous nature of the symptoms found in schizophrenia pose a unique challenge for clinicians.
Per the DSM-5, social fear is a marked or persistent anxiety in unfamiliar situations, despite an individual recognizing this fear as excessive or unreasonable. Social anxiety disorder, encompassing social fear, is easily measured using the Liebowitz Social Anxiety Scale (LSAS),2 a clinician-administered assessment of self-reported symptoms of fear and avoidance. Social anxiety disorder is a prevalent comorbid disorder in samples of schizophrenia patients; rates of 8%,3 11%,4 17%,5,6 18%,7 and 36%8 have been reported, and a large meta-analysis found a prevalence of 15%.9 Social anxiety disorder is also a significant predictor of functional outcome, leading to an increase in both the frequency and lethality of suicide attempts over a lifetime, more past substance/alcohol abuse disorders, poorer social adjustment, and lower quality of life.8 Research has found social anxiety to be treatable in patients with schizophrenia.10 Of note, the DSM-5 now includes psychiatric comorbidity in schizophrenia as independent diagnoses for which appropriate treatment should be initiated. In earlier versions of the DSM, other domains of psychopathology were included with a hierarchical diagnosis of schizophrenia.
Avolition and asociality comprise 1 domain of the negative symptoms associated with schizophrenia and are also important predictors of functional outcome.11 One theory that has only been weakly addressed in the field is the possibility that social fear is a crucial component of the impaired drive and sociability in persons with schizophrenia.12,13 Most current theories focus instead on reward-processing abnormalities.14 The relationship between negative symptoms and social anxiety remains unclear.8,10,13
Additionally, predictors of social fear and anxiety in schizophrenia patients are scant in the literature. Previous studies have shown that negative symptoms, self-stigma, and self-esteem were predictive of social anxiety prospectively in outpatients.13 One study15 suggested that social anxiety in patients with schizophrenia may be medication-induced. Studies also have shown that social anxiety is associated with a lower subjective quality of life,16 higher levels of insight and avoidance behavior,8 impaired flexibility of abstract thought,17 social anhedonia, and negative affect.12 Beyond these associations, it has been suggested that severe anxiety reflects the existence of a particular subtype of schizophrenia that results in fundamentally different outcomes and treatment implications.18 Delineating subtypes within schizophrenia (ie, schizophrenia with comorbid social anxiety disorder) and characterizing dimensions that exist beyond it is of particular interest to researchers in order to develop focused treatments.19
In this study, we assessed 3 a priori hypotheses. First, we propose that persons with schizophrenia do exhibit significant levels of social fear. Second, we hypothesize that social fear in schizophrenia cannot be explained by negative symptoms. Third, we explore different predictors that are related to increased social fear in schizophrenia.
METHOD
Participants
A total of 53 patients with DSM-IV schizophrenia or schizoaffective disorder, hereafter referred to as schizophrenia patients, were recruited from inpatient and outpatient research centers at the New York State Psychiatric Institute, New York, and provided informed consent for this institutional review board–approved study. All patients were clinically stable for at least 1 month with no changes in medication.
A total of 37 healthy controls were recruited from postings at the medical center and through Internet advertisements and had completed sufficient testing to be included. Sex distribution did not differ between the 2 groups. Patients and controls were excluded if they were pregnant or taking oral contraceptives, had any substance dependence disorder, or had a history of epilepsy or a major head injury requiring medical treatment. All assessments were completed by trained clinicians with a master’s degree or higher. All patients and controls were recruited to participate in an R01 study to examine social function in schizophrenia. Data were collected from 2005 to 2010.
Assessments
The Diagnostic Interview for Genetic Studies20 was used to determine the current and lifetime psychiatric diagnoses in addition to demographic information about sex, age, and education in all of the study participants, including the control subjects.
The LSAS comprises 4 individual subscales: social fear, social avoidance, performance fear, and performance avoidance. A total score ≥ 60 is used as a threshold for diagnosing social anxiety disorder.21 Participants are asked by a clinician to rate the degree of fear and avoidance they have or hypothetically would have felt performing 24 different social and performance actions in the past week.
The 30-item Positive and Negative Syndrome Scale (PANSS)22 is a rating instrument to evaluate the presence/absence and severity of positive, negative, and general psychopathology of schizophrenia. Additionally, the 5 symptom factors derived from the PANSS using the pentagonal model (PANSS 5-Factors)23 were used to assess clinical symptoms because of their superiority in delineating dysthymic symptoms from negative symptoms. The factor analysis of the PANSS includes 25 of the 30 PANSS items that are grouped into 5 categories: positive symptoms, such as delusions and unusual thought; negative symptoms, such as emotional and social withdrawal; dysthymic mood symptoms, such as anxiety and depression; activation symptoms, such as hostility, impulsivity, and poor rapport; and autistic preoccupation symptoms, such as poor attention, preoccupation, and disturbed volition.
The self-report Chapman scales for physical and social anhedonia24 include 101 items that measure the inability to experience pleasure from normally pleasurable social stimuli (eg, communicating and being with other people) and physical stimuli (eg, touching, eating, and smell).
Family history was obtained blind to patient information using the Family Interview for Genetic Studies.25 At least 1 immediate family member provided information about psychiatric symptoms in all first- and second-degree family members so that the schizophrenia patients could be identified as either having a family history (familial) or not having a family history (sporadic). The familial patients each had a first- or second-degree relative with a chronic nonaffective psychosis, and sporadic patients had no family members with psychosis.
Trained research and clinical staff carried out all procedures, diagnostic interviews, and symptom assessments with high interrater reliability. The reliability for DSM-IV diagnoses using the Diagnostic Interview for Genetic Studies was κ = 0.95 and for individual symptoms was κ = 0.80. Reliability was assessed using live and videotaped interviews, which were then corated for all scales used. Staff members agreed on all diagnoses.
Data Analysis
All data and forms were checked for errors and consistency prior to data entry. Form-fill databases were created, data were entered and verified using the SIR Database Management Software (SIR 2002, SIR Pty Ltd, Terrey Hills, Australia), and data analyses were performed using IBM/SPSS Version 21 (IBM Corp, Armonk, New York). During data analysis, we examined the descriptive statistics (means and standard deviations) and distributions of all measures whether continuous or categorical to identify key features (nonnormal distribution, outliers, skewness) that might impact inferential methods. Age and education level were examined using analysis of variance to assess for possible group membership (patients and controls) and sex (male and female) effects. Education level was also examined using the χ2 statistic. Age at psychotic symptom onset was examined between the male and female schizophrenia patients using the t test statistic. The analyses of the LSAS scales and the Chapman anhedonia scales were performed using multivariate analysis of covariance (ANCOVA) assessing for the main effects of diagnostic group, sex, and their interaction. The LSAS total (the total of the 4 subscales) was analyzed using ANCOVA. The healthy controls reported minimal PANSS symptoms, thus the PANSS scales and symptom items were only examined for sex differences within the schizophrenia group using multivariate ANCOVA for the scales and Student t test for the symptom items.
Correlation coefficients were calculated by examining the association between the LSAS total, the LSAS social fear subscale, and the PANSS 5-Factors among the schizophrenia patients as a group and then separately by sex. The clinical symptoms reported by healthy controls were minimal and not examined. As a final integrative procedure, we performed several multiple regression analyses of the LSAS total and social fear subscale on the PANSS 5-Factors as well as the individual PANSS symptom items. We were specifically interested in identifying the specific negative PANSS symptom factors and symptom items that were the most salient in predicting social anxiety and fear. Although we conducted multiple tests, we did not implement a Bonferroni-adjusted level of significance given that we had a hypothesis that looked specifically at negative symptoms and that our meaningful findings were already significant at P < .01.
RESULTS
Demographic Measures
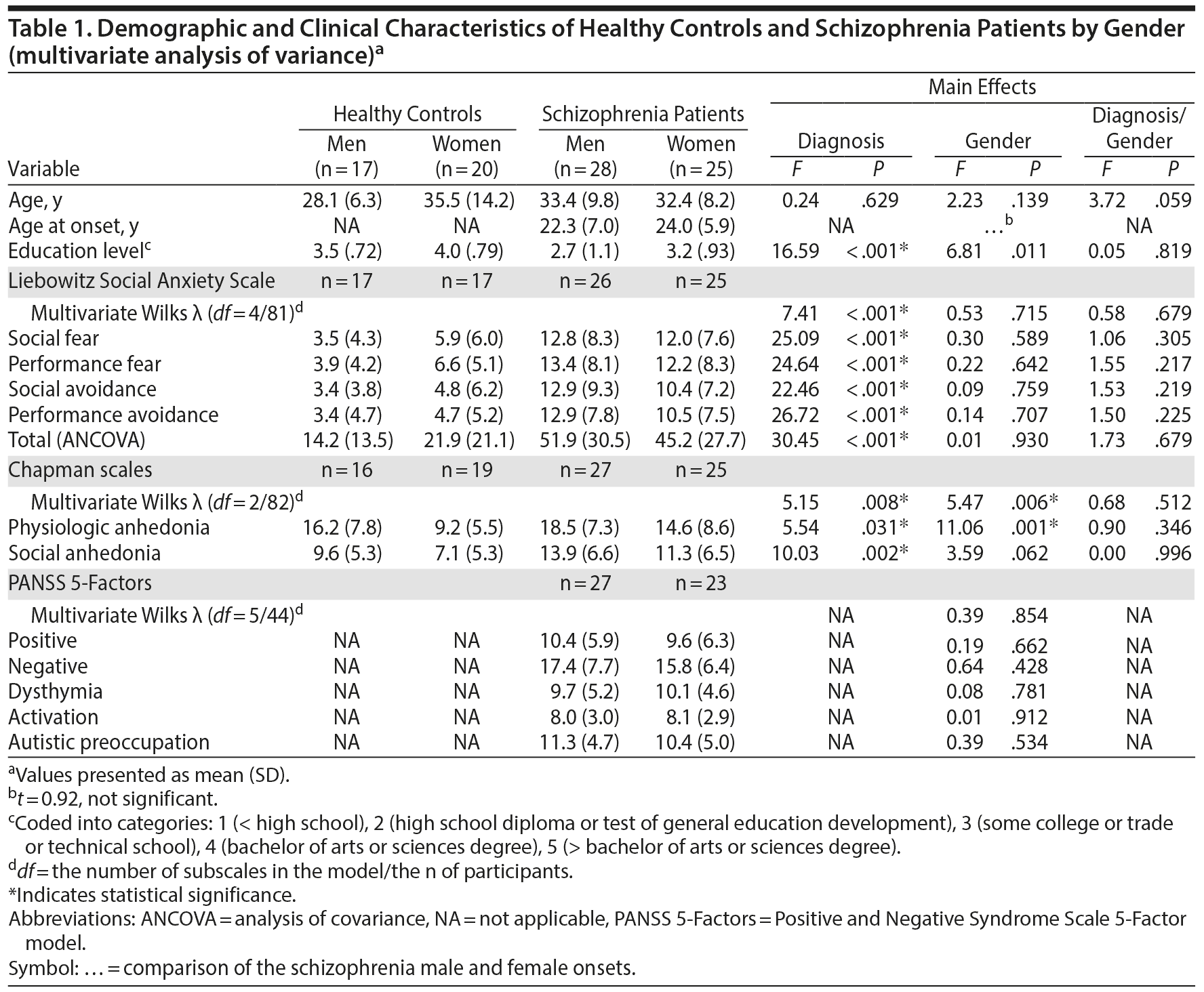
Preliminary analyses (Table 1) showed that age did not significantly differ by either diagnosis or sex; however, there were significant diagnosis and sex effects for education level (P < .001). The schizophrenia patient group was significantly less educated than controls (P < .001), and females were more educated than males, with no significant interaction of the 2 factors. Age at illness onset did not differ between the male and female schizophrenia patients.
Social Anxiety and Anhedonia
in Schizophrenia Patients
The multivariate ANCOVA of the LSAS yielded a highly significant Wilks λ (P < .001) for schizophrenia patients compared to controls, and this encompassed the 4 subscales: social and performance fear and social and performance avoidance (P < .001 for all between-group comparisons). All schizophrenia patient scores were significantly greater than controls (P < .001). The LSAS total was also significantly higher among the schizophrenia patients (P < .001). There were no significant sex effects nor was there a significant diagnosis by sex interaction term. On the basis of our cutoff score, significantly more schizophrenia patients than controls qualified for a diagnosis of social anxiety disorder (37.7% vs 2.9%, respectively, χ2 = 14.11, P ≤ .001).The multivariate ANCOVA results of the Chapman social and physical anhedonia scales revealed a significant Wilks λ for both diagnosis of schizophrenia (P = .008) and sex (P = .006), with no significant interaction. Significant between-group effects for diagnosis were present for physical (P = .031) and social (P = .002) anhedonia ratings, and a significant sex effect was present for physical (P = .001) but not social anhedonia. The schizophrenia patients exhibited higher levels of both physical and social anhedonia than controls, and the males exhibited higher levels of physical anhedonia than females.
Social Anxiety and the PANSS
The controls exhibited minimal PANSS symptoms, and these are not presented. The PANSS 5-Factors and individual PANSS symptom items were examined for sex effects within the schizophrenia group, and none were significant.
We were specifically interested in examining the associations between the LSAS total as well as the social fear subscale and the PANSS symptom factors. There were no significant correlations for schizophrenia patients or within male schizophrenia patients exclusively. However, significant correlations were revealed in the female schizophrenia patient group between the PANSS dysthymia factor and the social fear subscale (r = 0.485, n = 23, P = .019), the social avoidance subscale (r = 0.527, n = 23, P = .010), and the LSAS total (r = 0.423, n = 23, P = .044). The first 2 correlations differed significantly (Fisher R to Z, P = .037 and P = .025, respectively) from the male schizophrenia patients.
Multiple Regression Analyses
We performed several multiple regressions separately using LSAS total and the social fear subscale as outcomes. These regressions were performed in 2 steps. First, we entered current age, sex, onset of psychotic symptoms, and family history of psychosis into the model, followed in the second step by the PANSS 5-Factors symptoms and the Chapman anhedonia scales. In separate regressions, the PANSS symptom items were entered during the second step.
Our first regression examined which of the PANSS 5-Factors symptoms, in addition to the Chapman anhedonia scales, were related to the LSAS total. Family history (t = 3.06, P = .004) and higher social anhedonia (t = 3.87, P ≤ .001) were both significantly associated with higher LSAS total, while the negative factor was not. We also looked at the relationship between the individual PANSS symptom items and the LSAS total and again found a positive family history to be a significant predictor (t = 3.69, P = .001), while the only negative symptom items associated were higher “difficulty in abstract thinking” (t = 3.413, P = .002) and lower “blunted affect” (t = −2.34, P = .024). Additionally, when looking at the relationship between the PANSS 5-Factors symptoms and the Chapman anhedonia scales using the social fear subscale instead of LSAS total as our outcome, we found again that family history (t = 2.81, P = .007) and social anhedonia (t = 3.63, P = .001) were significantly associated, while the negative factor was not. There were no individual negative PANSS symptom items that were significant predictors of the social fear subscale as well. Positive family history was again significant (t = 3.44, P = .001).
DISCUSSION
This study had 3 main findings. First, there was an increased rate of social anxiety disorder, social anxiety, and social fear in schizophrenia patients compared to controls. Second, the PANSS negative symptoms, with the exception of lower blunted affect and higher difficulty in abstract thinking, did not predict social anxiety. Third, a family history of psychosis was a significant predictor of social anxiety.
Although other studies have included the LSAS to assess social anxiety in schizophrenia patients,4,8,17,26 our study is the first to use it to calculate a prevalence rate of the disorder. Our prevalence rate (37.7%) is at the higher end of the 8.2%–36.3% range previously reported using the Diagnostic Interview for Genetic Studies or Structured Clinical Interview for DSM Disorders (SCID).3–9 This variety of rates is likely due to the different diagnostic instruments used or differences in the patient population.10 However, our rate is most similar to the only study to assess the validity of the LSAS as compared to the SCID in determining social anxiety disorder (36.3% compared to our rate of 37.7%).8 Our higher rate of detection may be attributed to the higher sensitivity of the LSAS in picking up specific social anxiety traits not otherwise assessed, consistent with previous literature suggesting that instruments in addition to the SCID increase the prevalence rate of anxiety disorders.9 Dimensionally, social anxiety was also significantly higher for patients than controls. Thus, patients with schizophrenia do have social fear, and to a degree that amounts to a comorbid clinical diagnosis.
Our results also demonstrate that negative symptoms are unable to account for social anxiety. The negative factor from the PANSS 5-Factors and the total negative symptom measure from the PANSS were not correlated to and did not predict social anxiety, aside from the individual symptoms blunted affect, in which patients actually exhibited a decreased blunted affect, and difficulty in abstract thinking, which was the only negative symptom item that was elevated in patients. Given that we considered negative symptoms using both the traditional PANSS and the 5-factor grouping method in addition to individually considering each symptom, this finding appears to be reliable. Additionally, no negative symptoms using the PANSS and the PANSS 5-Factors predicted the specific social fear subscale. Social anxiety and fear were thus not explained by negative symptoms, confirming results from previous literature8 and further attesting to the use of the LSAS to reliably pick up social anxiety. Differences in treatment response for social anxiety symptoms and negative symptoms have been demonstrated.15 However, there are no formalized guidelines for the treatment of social anxiety in patients with schizophrenia.
Our multivariate regressions reveal that by far the strongest predictor of social anxiety and social fear is a family history of psychosis. It is well known that there is a familial contribution to the development of schizophrenia; however, its use to determine a discrete subset of patients remains an area of active research and controversy.19,27 Clinical differences between familial and sporadic subtypes of patients with schizophrenia have been demonstrated in the past,28 including higher levels of negative symptoms in familial subtypes29 and more treatment-resistant negative symptoms than in their sporadic counterparts.30
The increased rate of both social anxiety disorder and greater negative symptoms in familial patients begs the question of whether there is a common genetic vulnerability leading to these 2 distinct phenomena. There may be a pleiotropic effect stemming from this vulnerability, leading to both more severe negative symptoms and the development of increased social anxiety. One other noteworthy finding is the lack of association between positive symptoms and social anxiety, confirming previous results8 and refuting articles that have reported otherwise.4,17,31
An important limitation to our study is the high likelihood of bias during recruitment. Patients with social anxiety disorder would naturally be less likely to agree to a long and socially interactive assessment. Thus, our study most likely underestimates the prevalence of social anxiety disorder in patients and controls. Although we only assessed the presence of social anxiety disorder based on LSAS scores > 61, this approach is a validated screen for social anxiety disorder.2,8 A cutoff of 60 has also been used to classify the disorder.21
Other limitations of our study include the heterogeneity of our sample in diagnosis, recruitment site, and medications used. Our sample includes schizophrenia and schizoaffective diagnoses, inpatients and outpatients, and persons taking a variety of medications. It is impossible to exclude the emergence of social anxiety due to medication use, which has occurred in previous studies.26 Differences in medication regimens may play a role in our findings, given that patients with a familial etiology are considered more treatment resistant. A major strength of our study was the use of stringent criteria to assess family history, which required the presence of chronic nonaffective psychoses in first- or second-degree relatives, increasing the validity of our family history findings. An important alternate hypothesis is the role of family history as an environmental stressor that subsequently produces social dysfunction and negative symptoms rather than functioning as a genetic vulnerability.
In conclusion, our findings point to the importance of familial etiology in explaining some of the symptom variability found in schizophrenia. It is especially important to delineate subtypes within schizophrenia when assessing effective treatments in subpopulations, given the heterogeneity of the disease. Additionally, this study supports the use of the LSAS to detect social anxiety symptoms, as well as its use as a reliable and sensitive measure of social anxiety. Social anxiety disorder is a prevalent and comorbid disorder in patients with schizophrenia that further studies must focus on to both characterize and treat.
Submitted: February 9, 2015; accepted May 1, 2015.
Published online: September 3, 2015.
Potential conflicts of interest: None reported.
Funding/support: This work was supported by the National Institute of Mental Health (R01MH066428 and 5K24MH001699-10).
Role of the sponsor:The sponsor played no role in the design and conduct of the study; collection, management, analysis, and interpretation of data; or preparation, review, or approval of the manuscript.
REFERENCES
1. Insel TR. Rethinking schizophrenia. Nature. 2010;468(7321):187–193. doi:10.1038/nature09552 PubMed
2. Heimberg RG, Horner KJ, Juster HR, et al. Psychometric properties of the Liebowitz Social Anxiety Scale. Psychol Med. 1999;29(1):199–212. doi:10.1017/S0033291798007879 PubMed
3. Goodwin RD, Amador XF, Malaspina D, et al. Anxiety and substance use comorbidity among inpatients with schizophrenia. Schizophr Res. 2003;61(1):89–95. doi:10.1016/S0920-9964(02)00292-X PubMed
4. Mazeh D, Bodner E, Weizman R, et al. Comorbid social phobia in schizophrenia. Int J Soc Psychiatry. 2009;55(3):198–202. doi:10.1177/0020764008093447 PubMed
5. Cosoff SJ, Hafner RJ. The prevalence of comorbid anxiety in schizophrenia, schizoaffective disorder and bipolar disorder. Aust N Z J Psychiatry. 1998;32(1):67–72. doi:10.3109/00048679809062708 PubMed
6. Braga RJ, Mendlowicz MV, Marrocos RP, et al. Anxiety disorders in outpatients with schizophrenia: prevalence and impact on the subjective quality of life. J Psychiatr Res. 2005;39(4):409–414. doi:10.1016/j.jpsychires.2004.09.003 PubMed
7. Cassano GB, Pini S, Saettoni M, et al. Multiple anxiety disorder comorbidity in patients with mood spectrum disorders with psychotic features. Am J Psychiatry. 1999;156(3):474–476. PubMed
8. Pallanti S, Quercioli L, Hollander E. Social anxiety in outpatients with schizophrenia: a relevant cause of disability. Am J Psychiatry. 2004;161(1):53–58. doi:10.1176/appi.ajp.161.1.53 PubMed
9. Achim AM, Maziade M, Raymond E, et al. How prevalent are anxiety disorders in schizophrenia? a meta-analysis and critical review on a significant association. Schizophr Bull. 2011;37(4):811–821. doi:10.1093/schbul/sbp148 PubMed
10. Braga RJ, Petrides G, Figueira I. Anxiety disorders in schizophrenia. Compr Psychiatry. 2004;45(6):460–468. doi:10.1016/j.comppsych.2004.07.009 PubMed
11. Wittorf A, Wiedemann G, Buchkremer G, et al. Prediction of community outcome in schizophrenia 1 year after discharge from inpatient treatment. Eur Arch Psychiatry Clin Neurosci. 2008;258(1):48–58. doi:10.1007/s00406-007-0761-z PubMed
12. Blanchard JJ, Mueser KT, Bellack AS. Anhedonia, positive and negative affect, and social functioning in schizophrenia. Schizophr Bull. 1998;24(3):413–424. doi:10.1093/oxfordjournals.schbul.a033336 PubMed
13. Lysaker PH, Yanos PT, Outcalt J, et al. Association of stigma, self-esteem, and symptoms with concurrent and prospective assessment of social anxiety in schizophrenia. Clin Schizophr Relat Psychoses. 2010;4(1):41–48. doi:10.3371/CSRP.4.1.3 PubMed
14. Strauss GP, Waltz JA, Gold JM. A review of reward processing and motivational impairment in schizophrenia. Schizophr Bull. 2014;40(suppl 2):S107–S116. doi:10.1093/schbul/sbt197 PubMed
15. Pallanti S, Quercioli L, Rossi A, et al. The emergence of social phobia during clozapine treatment and its response to fluoxetine augmentation. J Clin Psychiatry. 1999;60(12):819–823. doi:10.4088/JCP.v60n1203 PubMed
16. Kumazaki H, Kobayashi H, Niimura H, et al. Lower subjective quality of life and the development of social anxiety symptoms after the discharge of elderly patients with remitted schizophrenia: a 5-year longitudinal study. Compr Psychiatry. 2012;53(7):946–951. doi:10.1016/j.comppsych.2012.03.002 PubMed
17. Lysaker PH, Hammersley J. Association of delusions and lack of cognitive flexibility with social anxiety in schizophrenia spectrum disorders. Schizophr Res. 2006;86(1–3):147–153. doi:10.1016/j.schres.2006.05.014 PubMed
18. Lysaker PH, Salyers MP. Anxiety symptoms in schizophrenia spectrum disorders: associations with social function, positive and negative symptoms, hope and trauma history. Acta Psychiatr Scand. 2007;116(4):290–298. doi:10.1111/j.1600-0447.2007.01067.x PubMed
19. Bergen SE, O’Dushlaine CT, Lee PH, et al; International Schizophrenia Consortium, Swedish Schizophrenia Consortium. Genetic modifiers and subtypes in schizophrenia: investigations of age at onset, severity, sex and family history. Schizophr Res. 2014;154(1–3):48–53. doi:10.1016/j.schres.2014.01.030 PubMed
20. Nurnberger JI Jr, Blehar MC, Kaufmann CA, et al. Diagnostic Interview for Genetic Studies: rationale, unique features, and training. NIMH Genetics Initiative. Arch Gen Psychiatry. 1994;51(11):849–859, discussion 863–864. doi:10.1001/archpsyc.1994.03950110009002 PubMed
21. Rytwinski NK, Fresco DM, Heimberg RG, et al. Screening for social anxiety disorder with the self-report version of the Liebowitz Social Anxiety Scale. Depress Anxiety. 2009;26(1):34–38. doi:10.1002/da.20503 PubMed
22. Kay SR, Fiszbein A, Opler LA. The Positive and Negative Syndrome Scale (PANSS) for schizophrenia. Schizophr Bull. 1987;13(2):261–276. doi:10.1093/schbul/13.2.261 PubMed
23. White L, Harvey PD, Opler L, et al; The PANSS Study Group. Empirical assessment of the factorial structure of clinical symptoms in schizophrenia: a multisite, multimodel evaluation of the factorial structure of the Positive and Negative Syndrome Scale. Psychopathology. 1997;30(5):263–274. doi:10.1159/000285058 PubMed
24. Chapman LJ, Chapman JP, Raulin ML. Scales for physical and social anhedonia. J Abnorm Psychol. 1976;85(4):374–382. doi:10.1037/0021-843X.85.4.374 PubMed
25. Maxwell ME. Family Interview for Genetic Studies (FIGS): Manual for FIGS. Bethesda, MD: Clinical Neurogenetics Branch, Intramural Research Program, National Institute of Mental Health; 1992.
26. Pallanti S, Quercioli L, Pazzagli A. Social anxiety and premorbid personality disorders in paranoid schizophrenic patients treated with clozapine. CNS Spectr. 2000;5(9):29–43. PubMed
27. Roy MA, Crowe RR. Validity of the familial and sporadic subtypes of schizophrenia. Am J Psychiatry. 1994;151(6):805–814. doi:10.1176/ajp.151.6.805 PubMed
28. Keefe RS, Mohs RC, Losonczy MF, et al. Characteristics of very poor outcome schizophrenia. Am J Psychiatry. 1987;144(7):889–895. doi:10.1176/ajp.144.7.889 PubMed
29. Galderisi S, Maj M, Mucci A, et al. Historical, psychopathological, neurological, and neuropsychological aspects of deficit schizophrenia: a multicenter study. Am J Psychiatry. 2002;159(6):983–990. doi:10.1176/appi.ajp.159.6.983 PubMed
30. Malaspina D, Goetz RR, Yale S, et al. Relation of familial schizophrenia to negative symptoms but not to the deficit syndrome. Am J Psychiatry. 2000;157(6):994–1003. doi:10.1176/appi.ajp.157.6.994 PubMed
31. Penn DL, Hope DA, Spaulding W, et al. Social anxiety in schizophrenia. Schizophr Res. 1994;11(3):277–284. doi:10.1016/0920-9964(94)90022-1 PubMed
Enjoy this premium PDF as part of your membership benefits!


