Objective: To expand knowledge during the coronavirus disease 2019 (COVID-19) pandemic with regard to suicide prevention among the elderly population by providing recommendations for interview strategies using 3 suicide theories.
Methods: Two hypothetical geriatric suicide cases (1 low lethality and 1 high lethality) are presented and categorized according to 3 suicide theories: interpersonal theory of suicide, three-step theory of suicide, and hopelessness theory of depression.
Results: In crisis intervention, the clinician’s interview must match the intrinsic belief of the suicide attempter to enable engagement and rapport. Use of different aspects of the 3 suicide theories can be useful but are dependent on the emergent nature of the attempt.
Conclusion: The need for identification and treatment of those with mental health issues, especially among the elderly population, and collaborative multidiscipline management teams is increasing during the current global pandemic. Specific interview strategies are needed when engaging with elderly suicidal patients. Suicide prevention in elderly patients is worthy of strong public attention.
ABSTRACT
Objective: To expand knowledge during the coronavirus disease 2019 (COVID-19) pandemic with regard to suicide prevention among the elderly population by providing recommendations for interview strategies using 3 suicide theories.
Methods: Two hypothetical geriatric suicide cases (1 low lethality and 1 high lethality) are presented and categorized according to 3 suicide theories: interpersonal theory of suicide, three-step theory of suicide, and hopelessness theory of depression.
Results: In crisis intervention, the clinician’s interview must match the intrinsic belief of the suicide attempter to enable engagement and rapport. Use of different aspects of the 3 suicide theories can be useful but are dependent on the emergent nature of the attempt.
Conclusion: The need for identification and treatment of those with mental health issues, especially among the elderly population, and collaborative multidiscipline management teams is increasing during the current global pandemic. Specific interview strategies are needed when engaging with elderly suicidal patients. Suicide prevention in elderly patients is worthy of strong public attention.
Prim Care Companion CNS Disord 2020;22(5):20nr02676
To cite: Chou HC, Tzeng DS, Lin SL. Suicide and the elderly during the COVID-19 pandemic: an overview of different suicide theories. Prim Care Companion CNS Disord. 2020;22(5):20nr02676.
To share: https://doi.org/10.4088/PCC.20nr02676
© Copyright 2020 Physicians Postgraduate Press, Inc.
aDepartment of Psychiatry, Kaohsiung Armed Forces General Hospital, Kaohsiung City, Taiwan
bInstitute of Undersea and Hyperbaric Medicine, National Defense Medical Center, Taipei, Taiwan
cCollege of Pharmacy and Biotechnology, Tajen University, Pingtung, Taiwan
dGraduate Institute of Medical Science, College of Health Science, Chang Jung Christian University, Tainan, Taiwan
eDepartment of Psychiatry, Kaohsiung Armed Forces, General Hospital Pingtung Branch, Pingtung, Taiwan
fDepartment of Electrical Engineering, I-Shou University, Kaohsiung City, Taiwan
*Corresponding author: Shang-Lun Lin, MS, No.2, Zhongzheng 1st Rd, Lingya Dist, Kaohsiung City 80284, Taiwan ([email protected]).
Imagine a possible scene during the coronavirus disease 2019 (COVID-19) crisis. When a young man goes home experiencing extreme fatigue, his elderly father, who suspected his son to have COVID-19, cut his radial artery. With the exception of attempting to stop the bleeding, what else could his son have done in that moment? What conversation could be used to quickly build a rapport to relieve the man’s mental anguish, stop the suicide attempt, and prevent the recurrence of suicide? This scene indicates 3 challenges with regard to suicide prevention in the geriatric population during the COVID-19 pandemic. First, in most countries, adults over age 65 years have the highest suicide rate.1 In the United States, the annual suicide death rate of senior citizens is > 27 per 100,000 in men and > 4 per 100,000 in women.2 Second, many individuals have underlying psychiatric disorders but may not seek help. A psychological autopsy revealed that 95% of suicide victims had a psychiatric disorder; however, 87% had not sought mental health treatment.3 Third, physicians may find it difficult to convey all the verbal and nonverbal messages, including the tenets of empathy, partnership, respect, support, legitimization, and compassion, to an elderly patient who has attempted suicide.4 Also, emergent psychiatric consultation is not always available in all medical institutions.
Although it is impossible to identify all individuals who may attempt suicide, it is important to understand factors that may increase the likelihood, especially during the COVID-19 crisis. Therefore, in this article, we demonstrate the possible intrinsic beliefs associated with 2 geriatric suicide cases and provide recommended interview techniques according to 3 main suicide theories. Given the limited government budgets for mental health services, the aim of this article is to quickly expand knowledge with regard to suicide prevention during the COVID-19 pandemic, especially among the elderly population.
METHODS
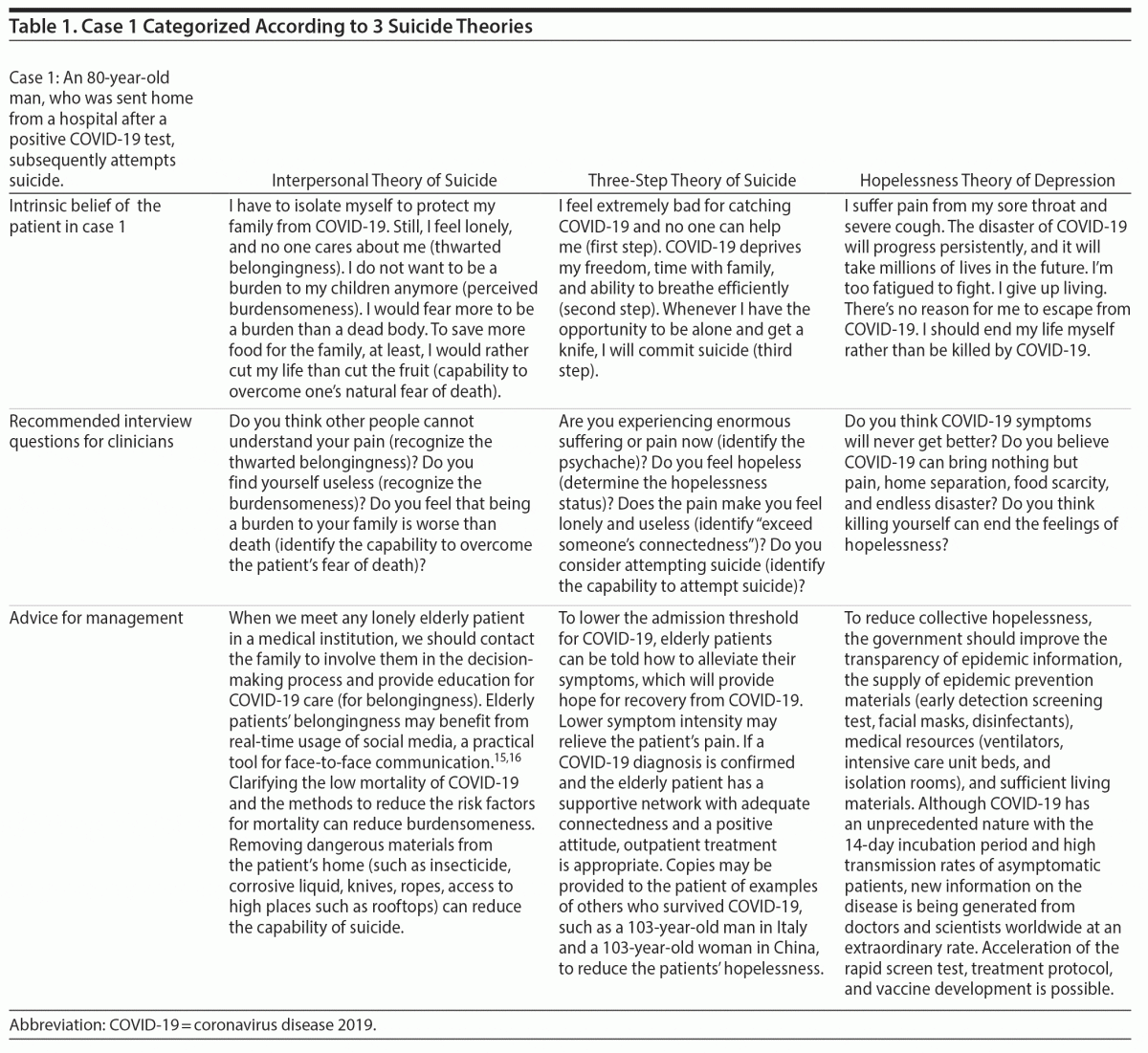
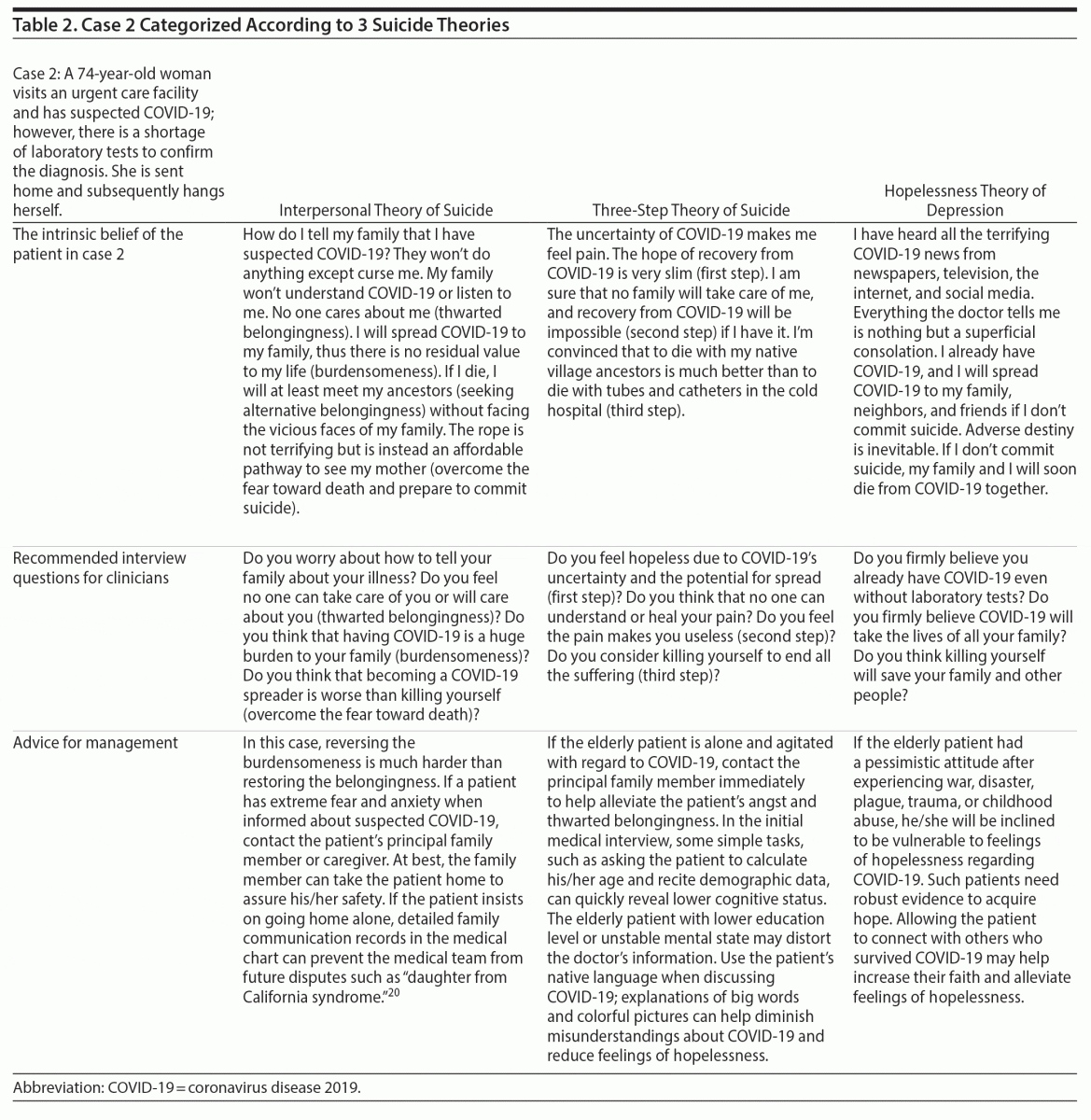
Three main suicide theories were applied in this analysis: interpersonal theory of suicide (IPT),5 three-step theory of suicide (TST),6 and hopelessness theory of depression (HTD),7 given that they are widely cited, concise, and practical8 to convert into interview sentences. Two hypothetical geriatric suicide cases (case 1 as an example of low lethality, case 2 as an example of high lethality) are presented to illustrate use of the 3 theories. The 2 cases were categorized using the 3 suicide theories by the possible intrinsic beliefs of the individuals, recommended interview questions for clinicians, and advice for management. An explanation of the 3 suicide theories used in this analysis is as follows.
Interpersonal Theory of Suicide
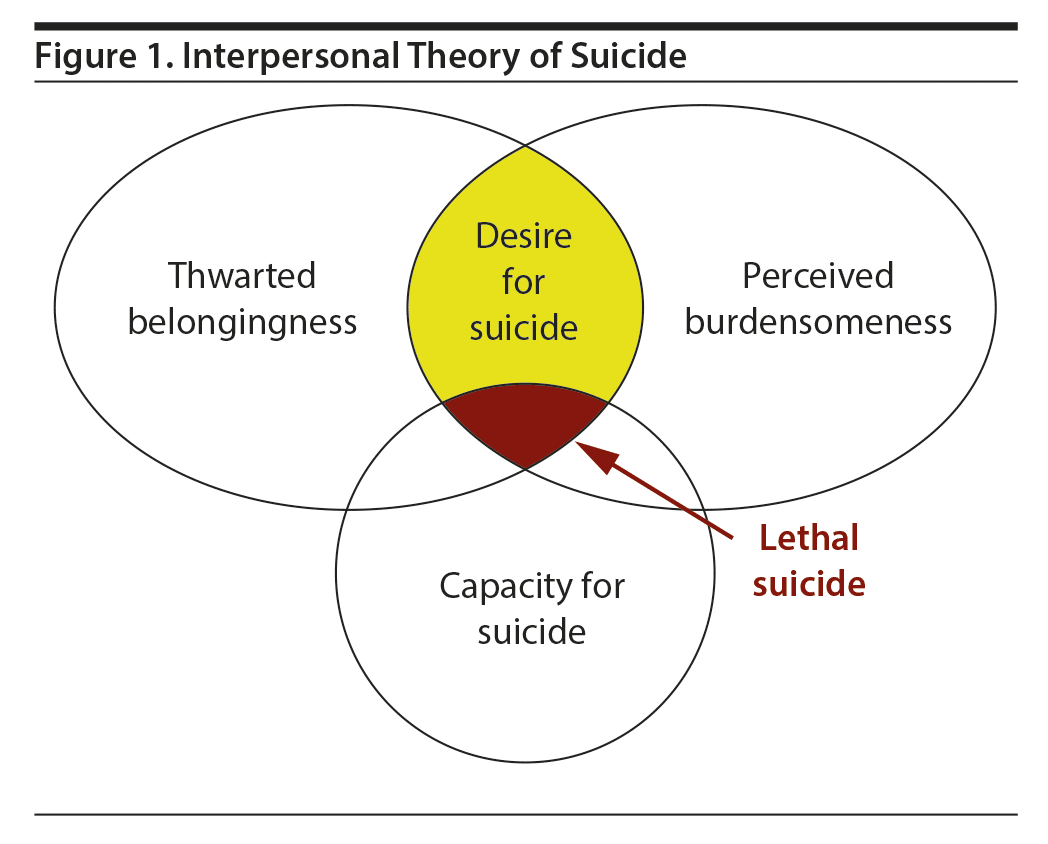
IPT (Figure 1) states that the combination of thwarted belongingness and perceived burdensomeness induces suicidal ideation. When suicidal ideation becomes stable and unchanging, active suicidality emerges. The simultaneous existence of the capability for suicide and strong suicidal desire provokes suicide attempts. The main variables of the capability for suicide include pain tolerance and ability to overcome the fear of death.
Three-Step Theory of Suicide
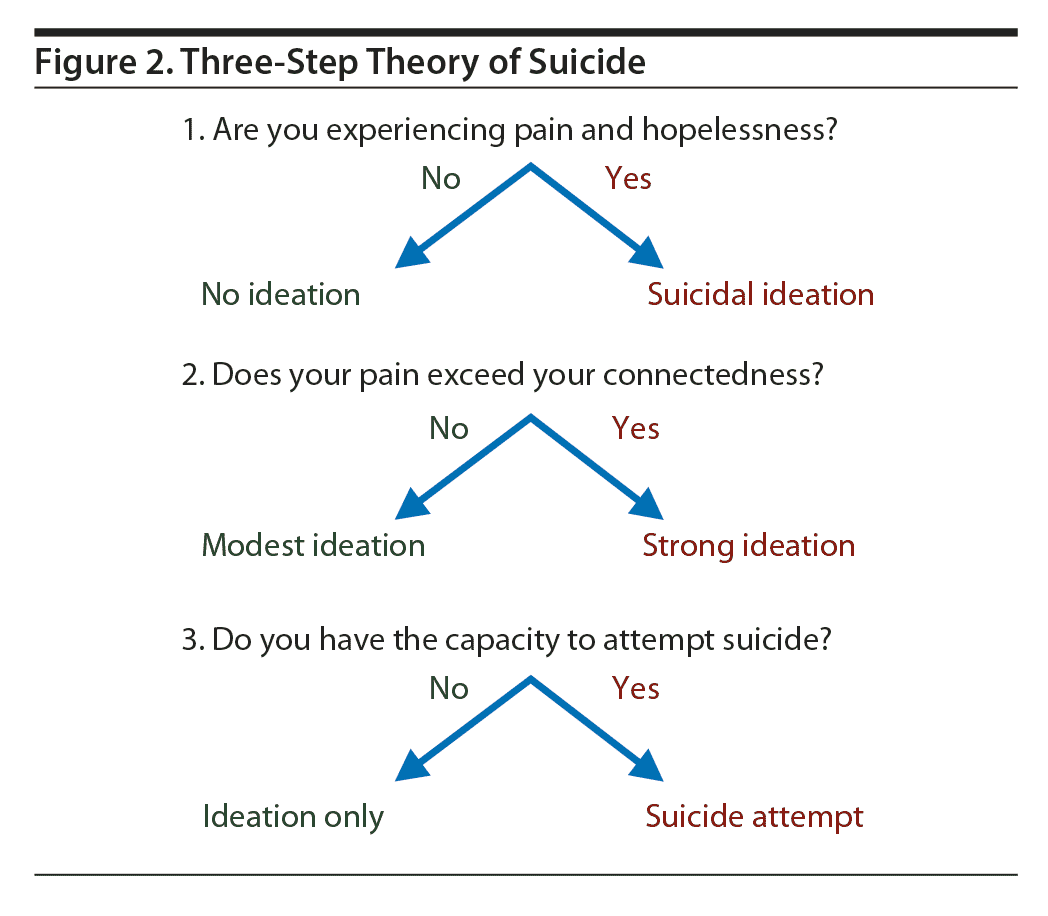
In the first step of TST, the presence of pain and hopelessness induces suicidal ideation (Figure 2). In the second step, the suicidal ideation will increase if there is a lack of sufficient connectedness. Adequate connectedness includes sufficient belongingness and “lack of burdensomeness” (ie, any sense of meaning or purpose for living or valued roles). In the third step, an individual with active suicidal ideation and the capacity for suicide will attempt suicide. The capability for suicide originates from a sense of fearlessness toward death, tolerance of physical pain, and practice of actions or plans.
Hopelessness Theory of Depression
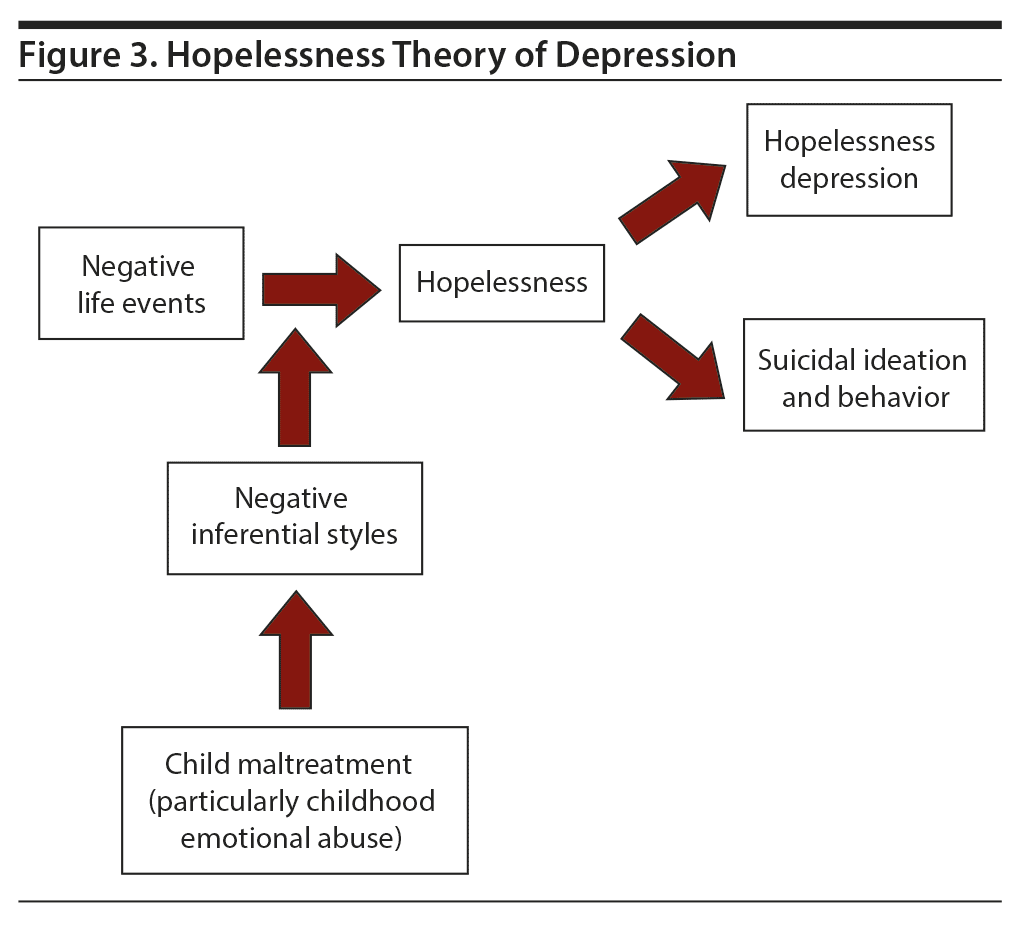
HTD (Figure 3) indicates that childhood maltreatment produces negative inferential styles, which cause people to negatively self-blame and view any challenges or difficulties as global and stable derivations of negative results. Negative inferential styles accelerate one’s view of adverse life events with a hopeless status. Hopelessness situations induce hopelessness depression plus suicidal ideation and attempts. Reciprocally speaking, positive inferential styles indicate that events are incidental and transitional derivations of proper endings or blessings.
RESULTS
Elderly COVID-19 patients often have comorbidities such as type 2 diabetes mellitus, cardiovascular disease, and pulmonary illness, which increase mortality risk.9 Hence, COVID-19 often precipitates preexisting burdensomeness. Geriatric individuals’ lower fear of death compared to younger patients makes suicide prevention more difficult in the elderly population.
Consideration of suicide-related variables in the firstline interview is an ideal way to investigate potential for suicide with adequate validity and reliability. However, such an interview will be too lengthy for non–mental health clinicians to carry out if too many suicide theory variables are considered. Currently, as the medical system is on the verge of collapse due to COVID-19, a thorough and lengthy interview may not only exhaust medical resources but also increase the risk of infection for interviewers. Here, we chose to use variables from only 3 suicide theories; however, there are other theories that could be considered such as the fluid vulnerability theory,10 integrated motivational-volitional model,11 borderline personality disorder theory,12 and Durkheim’s suicidology.13 The literature provides transgender, cross-cultural, and transnational support for the generalizability of the 3 main suicide theories7,14 used in this article.
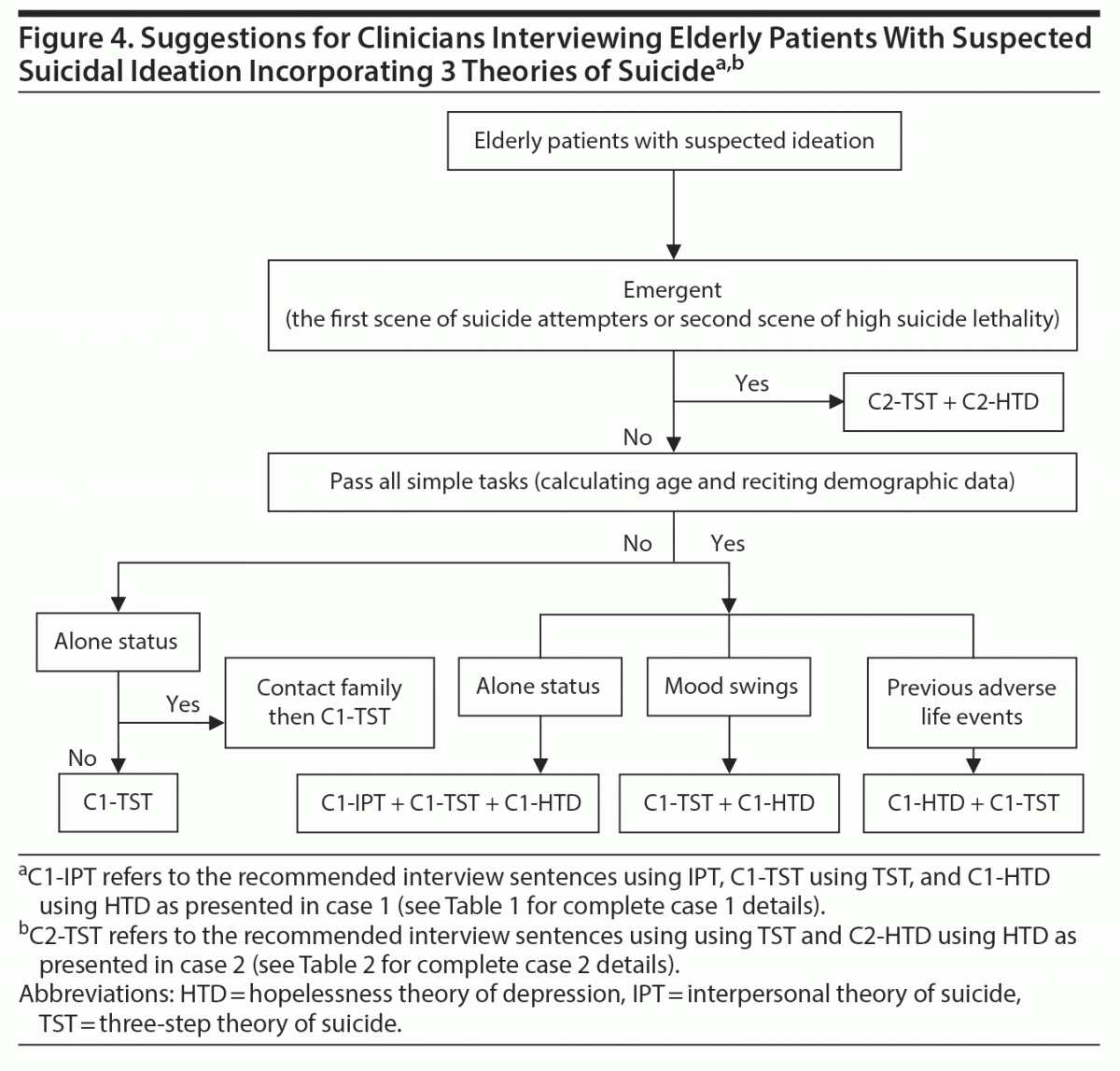
In crisis intervention, the effectiveness of the engagement and rapport depends on how close the clinician’s interview is to the exact intrinsic belief of the suicide attempter. The core precondition of IPT is the destruction of the interpersonal relationship, of TST is the psychache, and of HTD is the negative inferential style toward previous life events. Therefore, we provide some suggestions for clinicians in Figure 4.
Figure 4 shows possible scenarios for both cases according to the 3 suicide theories. Thus, C1-IPT refers to the recommended interview sentences for clinicians using IPT, C1-TST refers to using TST, and C1-HTD refers to using HTD per case 1 (see Table 1 for complete case 1 details). C2-IPT refers to the recommended interview sentences for clinicians using IPT, C2-TST refers to using TST, and C2-HTD refers to using HTD per case 2 (see Table 2 for complete case 2 details). The definition of emergent in Figure 4 refers to the first scene of suicide attempters or the second scene of high lethality. If first responders to a suicide attempt are emergency medical technicians, police officers, or doctors or nurses in ambulances, the interview must be terse with more profound empathy. In such conditions, interview by C2-TST + C2-HTD is adequate. The second step of C2-TST covers the main content of C2-IPT. Development of rapport through early identification of the psychache may lower the patient’s resistance to admitting negative inferential style.
In the nonemergent circumstance, assessment of the simple tasks of basic calculation and remote memory can clarify the impairment of cognition, which usually limits the attention to lengthy interview, distorts the interview sentences, and exaggerates the pessimistic attitude toward events. In C1-TST, the sentences related to psychache and hopelessness can cover the concept of negative inferential style in C1-HTD, and the sentences of connectedness can cover the concepts of belongingness and burdensomeness in C1-IPT. Hence, use of C1-TST is adequate for the geriatric patient with suspected cognitive impairment. C1-IPT may not be necessary because geriatric patients with caregivers often have sufficient belongingness. If the patient is alone, contacting the primary caregiver can not only prevent “daughter from California syndrome” (when a long-lost relative suddenly arrives at the hospital and insists that the medical team pursue aggressive life-prolonging interventions) but also ensure the patient’s safety when he/she returns home. For individuals who are alone but not cognitively impaired, use of C1-IPT + C1-TST + C1-HTD may be adequate. For individuals with mood swings, use of C1-TST + C1-HTD can quickly establish empathy for the psychache, allowing for exploration of the pessimistic thoughts. C1-HTD + C1-TST fits the subgroup of patients with life events (eg, domestic violence, bullying, life-threatening events such as surgeries and wars, and long-term morbidity of multiple illnesses). Such a population with negative inferential style usually has a Omega sign or Veraguth’s fold, low and slow pitch, monotonous vocabulary and tone, and down-deviation of sight and body axis. However, for an experienced clinician familiar with body language, use of C1-TST and C2-TST is adequate for most clinical settings. Adjustment of the intensity of nonverbal language facilitates advanced empathy and engagement.
COVID-19 patients have a broad spectrum of presentation, from asymptomatic to sepsis and multiple organ failure. Studies17–19 have shown the negative influence of mental disorders on the mortality and recovery of sepsis patients. If we screen, diagnose, and treat mental disorders in patients with COVID-19, they may benefit from lower mortality and faster recovery. Hence, collaborative teams, including infectious disease and respiratory specialists and psychiatrists, are needed globally.
Elderly patients who prepare to attempt suicide are usually already experiencing mental health issues. In medical interviews, elderly individuals often need more respect and empathy than younger patients. Thus, if interviewers take the time to understand their mental distress, elderly patients will benefit from the empathy and therapeutic alliance, as well as the new belongingness resulting from the doctor-patient relationship. Receipt of immediate symptom relief from health care providers may restore the patient’s faith in the medical field and facilitate hope. After treating the psychiatric illness, health care providers should encourage the patient to live for family and unfinished work to enhance connectedness, pain tolerance, and the desire to live.
If the medical system is overloaded due to COVID-19, omission of extensive interviews may be necessary. In such a circumstance, we recommend routinely executing a 1-minute screen using the 5-item Brief Symptom Rating Scale (BSRS-5)21 and previous suicide attempt history. The BSRS-5 was developed with adequate validity and reliability from the 50-item BSRS21–23 via thousands of study participants. The BSRS-5 has been widely used for screening suicidal ideation and psychiatric illness in schools, communities, and hospitals.22,23
CONCLUSION
This article, to our knowledge, is the first to focus on geriatric mental health to prevent suicide during the COVID-19 pandemic. The need for identification and treatment of those with mental health issues, especially among the elderly population, and collaborative multidiscipline management teams is increasing during the current global pandemic. Suicide prevention in elderly patients is worthy of strong public attention.
Clinical Points
- Specific suicide prevention interview strategies may improve patient health care, promote willingness to seek mental health resources, and prevent the stigma effect.
- The need for identification and treatment of those with mental health issues, especially among the elderly population, and collaborative multidiscipline management teams is increasing during the COVID-19 pandemic.
Received: May 16, 2020.
Published online: October 22, 2020.
Potential conflicts of interest: None.
Funding/support: None.
Acknowledgments: The article pays tribute to the mental health experts of Kaohsiung Armed Forces General Hospital.
REFERENCES
1. Preventing suicide: A global imperative. World Health Organization website. https://www.who.int/mental_health/suicide-prevention/world_report_2014/en/. 2014.
2. Curtin SC, Warner M, Hedegaard H. Increase in suicide in the United States, 1999–2014. NCHS Data Brief. 2016;(241):1–8. PubMed
3. Leavey G, Rosato M, Galway K, et al. Patterns and predictors of help-seeking contacts with health services and general practitioner detection of suicidality prior to suicide: a cohort analysis of suicides occurring over a two-year period. BMC Psychiatry. 2016;16(1):120. PubMed CrossRef
4. Fifield PY. Confidence And Connectedness: A Mixed Methods Study On Patients Managing Co-Occuring Physical And Behavioral Health Conditions [dissertation]. Biddeford, Maine: University of New England; 2015.
5. Van Orden KA, Witte TK, Cukrowicz KC, et al. The interpersonal theory of suicide. Psychol Rev. 2010;117(2):575–600. PubMed CrossRef
6. Dhingra K, Klonsky ED, Tapola V. An empirical test of the three-step theory of suicide in UK university students. Suicide Life Threat Behav. 2019;49(2):478–487. PubMed CrossRef
7. Liu RT, Kleiman EM, Nestor BA, et al. The hopelessness theory of depression: a quarter-century in review. Clin Psychol (New York). 2015;22(4):345–365. PubMed CrossRef
8. Klonsky ED, May AM, Saffer BY. Suicide, suicide attempts, and suicidal ideation. Annu Rev Clin Psychol. 2016;12(1):307–330. PubMed CrossRef
9. Weiss P, Murdoch DR. Clinical course and mortality risk of severe COVID-19. Lancet. 2020;395(10229):1014–1015. PubMed CrossRef
10. Rudd MD. Fluid vulnerability theory: a cognitive approach to understanding the process of acute and chronic suicide risk. In: Ellis TE, ed. Cognition and Suicide: Theory, Research, and Therapy. 2006:355–368.
11. Dhingra K, Boduszek D, O’Connor RC. A structural test of the integrated motivational-volitional model of suicidal behaviour. Psychiatry Res. 2016;239:169–178. PubMed CrossRef
12. Lieb K, Zanarini MC, Schmahl C, et al. Borderline personality disorder. Lancet. 2004;364(9432):453–461. PubMed CrossRef
13. Durkheim E. Suicide: A Study in Sociology. 2nd edition. Oxford, United Kingdom: Routledge; 2005.
14. Klonsky ED, Saffer BY, Bryan CJ. Ideation-to-action theories of suicide: a conceptual and empirical update. Curr Opin Psychol. 2018;22:38–43. PubMed CrossRef
15. Bekalu MA, McCloud RF, Viswanath K. Association of social media use with social well-being, positive mental health, and self-rated health: disentangling routine use from emotional connection to use. Health Educ Behav. 2019;46(2 suppl):69–80. PubMed CrossRef
16. Chen Y-RR, Schulz PJ. The effect of information communication technology interventions on reducing social isolation in the elderly: a systematic review. J Med Internet Res. 2016;18(1):e18. PubMed CrossRef
17. Ribe AR, Vestergaard M, Katon W, et al. Thirty-day mortality after infection among persons with severe mental illness: a population-based cohort study in Denmark. Am J Psychiatry. 2015;172(8):776–783. PubMed CrossRef
18. Davydow DS, Ribe AR, Pedersen HS, et al. The association of unipolar depression with thirty-day mortality after hospitalization for infection: a population-based cohort study in Denmark. J Psychosom Res. 2016;89:32–38. PubMed CrossRef
19. Prescott HC, Angus DC. Enhancing recovery from sepsis: a review. JAMA. 2018;319(1):62–75. PubMed
20. Molloy DW, Clarnette RM, Braun EA, et al. Decision making in the incompetent elderly: “the daughter from California syndrome.” J Am Geriatr Soc. 1991;39(4):396–399. PubMed CrossRef
21. Lin S-L, Wu S-L, Huang H-T, et al. Can a 10-minute questionnaire identify significant psychological issues in patients with temporomandibular joint disease? J Oral Maxillofac Surg. 2017;75(9):1856–1865. PubMed CrossRef
22. Lee M-B, Liao S-C, Lee Y-J, et al. Development and verification of validity and reliability of a short screening instrument to identify psychiatric morbidity. J Formos Med Assoc. 2003;102(10):687–694. PubMed
23. Lung FW, Lee MB; F-W L. The five-item Brief-Symptom Rating Scale as a suicide ideation screening instrument for psychiatric inpatients and community residents. BMC Psychiatry. 2008;8(1):53. PubMed CrossRef
Enjoy this premium PDF as part of your membership benefits!