ABSTRACT
Objective: To assess the extent to which articles examining telepsychiatry after the start of the COVID-19 pandemic provided racial and sociodemographic characteristics for people receiving audiovisual (video) versus audio-only telepsychiatry.
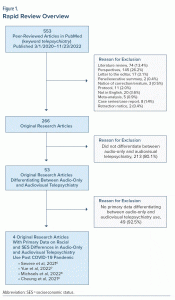
Data Sources, Study Selection, and Data Extraction: We employed the keyword telepsychiatry and screened all peer-reviewed articles in PubMed published from March 1, 2020, until November 23, 2022, prior to the federal government’s announcement of the impending end to the COVID-19 public health emergency. We retrieved and reviewed the full-text articles of 553 results for potential inclusion, of which 266 were original research articles.
Results: We found that 106 of 553 articles had any mention of differences between audio-only and audiovisual telepsychiatry. Twenty-nine of 553 articles described potential socioeconomic differences in the distribution of people receiving audio-only versus audiovisual telepsychiatry, and 20 of 553 described potential racial/ethnic differences. Among research articles, most (213/266) did not differentiate between videoconferencing and audio-only/telephone-based telehealth services. A total of 4 research articles provided racial and sociodemographic characteristics of individuals who received audio-only versus audiovisual telepsychiatry services during the COVID-19 pandemic, all of which were conducted in relatively small regional samples that could not be generalized to the US as a whole.
Conclusions: Overall, this analysis underscores that empirical data are lacking on racial and sociodemographic distribution of audio-only versus audiovisual telepsychiatry services since the COVID-19 pandemic.
Prim Care Companion CNS Disord 2023;25(6):23r03563
Author affiliations are listed at the end of this article.
Telepsychiatry use has surged in the United States (US) during the coronavirus disease 2019 (COVID-19) public health emergency.1,2 Although telemedicine was initially intended to include video and audio access nationwide, it has been observed that many patients from racially oppressed communities did not have access to video technology.3 While many medical specialties have successfully used telemedicine during the COVID-19 pandemic, there are unique challenges facing the application of telemedicine in psychiatry, a specialty that relies heavily on types of communication such as those related to signs and symptoms obtained from history, including from collateral sources and visual observations of nonverbal cues. In non-psychiatric specialties, in California, for example, a high proportion of telehealth appointments among minoritized patients have been audio-only visits during the pandemic,2 but we continue to lack summative data on whether psychiatry can be practiced effectively via telephone.
To address this gap in research, we conducted a rapid review of all articles examining telepsychiatry since the start of the COVID-19 pandemic. We sought to identify articles with primary data on the racial and sociodemographic distribution of people receiving audiovisual versus audio-only telepsychiatry from March 2020 to November 2022, prior to the federal government’s announcement of the impending end to the COVID-19 public health emergency.
METHODS
Rapid reviews can be defined as a type of knowledge synthesis in which the steps of a systematic review are streamlined to produce evidence in a shortened time frame.4 They are well suited for time-sensitive and dynamic topics, such as the evolution of telehealth during the COVID-19 pandemic.
Our search employed the keyword telepsychiatry and screened all peer-reviewed articles in PubMed and MEDLINE, including case reports, case series, qualitative studies, systematic reviews, meta-analyses, position papers, observational studies, and randomized controlled trials, published from March 1, 2020, until November 23, 2022. Because our rapid review was focused on patient–mental health clinician interactions via telehealth during the COVID-19 pandemic, we excluded studies of telehealth services such as remote monitoring, mobile application development, and mHealth (mobile health) interventions. One reviewer (K.Y.X.) conducted the literature search, reviewing full texts and extracting data on racial/ethnic demographics and outcomes, which were reviewed together with a second author (T.R.B.). Disagreements regarding study eligibility were resolved via discussion, with the reviewers erring on the side of inclusion. To capture as many eligible articles as possible, the search strategy was executed twice, first on November 10, 2022, when the Biden Administration announced impending restrictions to telehealth access, and again on November 23, 2022. As a rapid review, our protocol was not registered on the International Prospective Register of Systematic Reviews (PROSPERO). Institutional review board approval was not required for this analysis.
Study eligibility criteria were defined based on the population, intervention, comparison, and outcome (PICO) framework.5 The population was adults and/or children receiving telepsychiatry services during the COVID-19 pandemic. The intervention was treatment services delivered via either type of live telehealth service (audiovisual versus audio-only telephone services). We were interested in comparing distribution of audiovisual versus audio-only telephone services between people of different racial/ethnic backgrounds. As shown in Figure 1, we retrieved and individually reviewed the full text of 553 articles for potential inclusion.
RESULTS
Our search employed the keyword telepsychiatry and screened all peer-reviewed articles in PubMed published from March 1, 2020, until November 23, 2022. We retrieved and reviewed the full-text articles of all 553 results for potential inclusion.
Overall, only 106 articles (of 553; 19.2%) had any mention of differences between audio-only and audiovisual telepsychiatry. Twenty-nine articles (of 553; 5.2%) provided descriptive commentary on potential socioeconomic differences in the distribution of people receiving audio-only versus audiovisual telepsychiatry, whereas 20 (of 553; 3.6%) provided descriptive commentary on potential racial/ethnic differences.
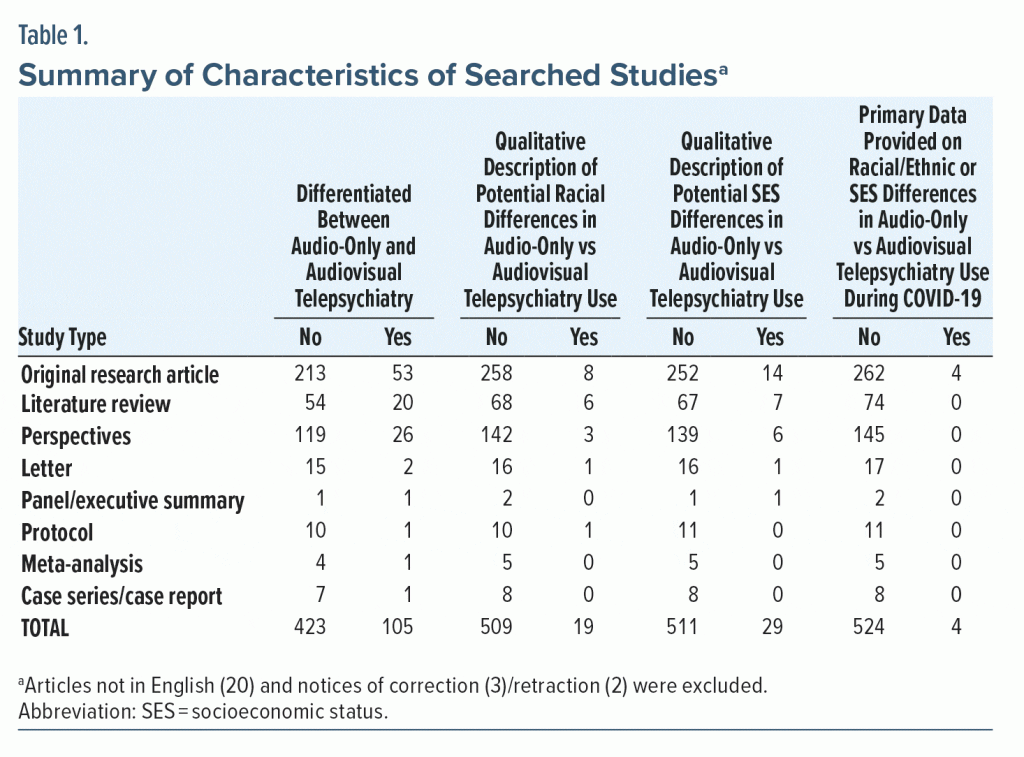
As shown in Table 1, we subsequently sought to identify original research articles containing empirical, primary data from the COVID-19 epidemic illuminating potential racial/ethnic and sociodemographic differences in individuals receiving audio-only versus audiovisual telepsychiatry. We eliminated many publications, such as perspectives (145 articles), literature reviews (74 articles), panel/executive summaries (2 articles), protocols (11 articles), case series (8 articles), and letters to the editor (17 articles), as they did not include original, primary data collected during the COVID-19 pandemic. Articles not published in English were excluded (20 articles). Meta-analyses (5 articles) employing data preceding COVID-19 were also not included.
Among all research studies, most (213 articles) did not differentiate between audiovisual and audio-only/telephone-based services. Of the 53 research articles that differentiated between audio-only and audiovisual telepsychiatry, we excluded 49 studies that did not report demographic and/or racial data for people receiving audiovisual versus audio-only/telephone-based services. This resulted in a total of 4 articles,6–9 summarized in Figure 1, providing racial and socioeconomic/demographic characteristics of individuals who received audio-only versus audiovisual telepsychiatry services during the COVID-19 pandemic. All studies were observational, with 3 based on patient self-report (survey) and 1 based on review of physician case logs. No studies provided national data, used administrative claim data, or contained data after the first wave of the COVID-19 pandemic.
DISCUSSION
Amid the cries of racial unrest coinciding with the initial COVID-19 outbreak, the year 2020 was commonly described as “unprecedented” in the US, meaning “unparalleled; never previously done, known, or experienced.”10 However, deeply entrenched racial inequities and harrowing conditions in historically marginalized communities, in reality, have been known and experienced long before the US went into lockdown. Repeatedly throughout history, public health catastrophes in the US have amplified structural racism,11 which then too remains unheeded or invisible in the aftermath. Consider the case of Hurricane Katrina, before which policymakers failed to maintain levees surrounding low-income communities in Louisiana, culminating in levee failures, heavy flooding, and a disproportionate burden of death in Black, Indigenous, and People of Color (BIPOC) communities after the storm. Even though Hurricane Katrina culminated in an overhauling of the US emergency preparedness infrastructure, the sordid role of structural racism in shaping tumult in New Orleans was usually absent from public discourse in the storm’s wake,12 a lesson seemingly unheard.
As we reviewed, the majority of the recent literature base has not consistently differentiated between audiovisual and audio-only telepsychiatry, nor has it examined sufficiently those very variables that would illuminate the extent of inequities in receipt of care during the pandemic. While telehealth presented a potential to mitigate existing inequities in health care access, there is reason to believe that the rollout of telepsychiatry may also perpetuate racist structures in mental health care, and this study illustrates that empirical data to help policymakers develop antiracist interventions are largely missing. Previous studies have found that over 40% of adult Medicare beneficiaries were found to lack access to a desktop or laptop computer with high-speed internet, with a similar percentage lacking access to a smartphone with wireless data necessary for video telemedicine appointments.13 Although efforts have been made in recent years to increase access to affordable broadband, the numbers of individuals accessing affordable connectivity programs are low.14,15 In comparison to higher–socioeconomic status non-Hispanic White patients who have been able to use video conferencing for medical appointments during the pandemic, a high proportion of telehealth appointments among people from socioeconomically and racially oppressed communities have been audio-only visits.2 In analyses of California’s federal qualified health centers, encompassing a population of historically marginalized patients, audio-only visits were found to constitute more than 90% of all telemedicine visits from March 2020 to August 2020.2 A recent analysis showed that in the setting of Veterans Affairs buprenorphine treatment, older patients who were male, Black, non–service connected, or experiencing housing instability were less likely to receive audiovisual compared with telephone-only telehealth.16 Whether these figures are generalizable to outpatient telepsychiatry in particular warrants further research.
While telepsychiatry can be conceptualized as a promising opportunity for improved treatment access, it simultaneously can come with significant risks for minoritized patients. For instance, while audio-only telemedicine has removed visual cues from patient encounters, implicit bias may still resonate and persist in the form of linguistic profiling, defined as racial discrimination based on auditory cues. Research has shown that those who lack fluency in mainstream standard American English, such as BIPOC patients, are prone to unequal access to essential social services when they seek these resources through telephone encounters,17 which can exacerbate diagnostic bias and stigma in mental status examinations. Amid the high burden of medical comorbidity caused by structural racism,18,19 difficulty in obtaining physical examination information may also result in missed diagnoses of treatable disease,20 with several studies revealing that video or in-person visits are associated with fewer medication errors, higher accuracy of initial diagnosis, and improved patient satisfaction.21,22 Nevertheless, studies have also revealed that many patients have preferred audio-only telemental health over audio/video telemental health, rooted in concerns about providers viewing their home settings and family members, amid a lack of trust.23 It also has been noted that patients with a history of trauma may find the virtual physical examination—and the greater degree of privacy and choice over their dress and environments at home—to be empowering.24 However, the complex reasons for patients’ preferences for audio-only versus audio/video telepsychiatry during the COVID-19 pandemic have not been thoroughly characterized and warrant further research. Furthermore, it remains unclear the extent to which audiovisual and audio-only telepsychiatry differ in terms of long-term health outcomes, and—amid the current endemic of structural racism—the distribution of racial and demographic characteristics between people receiving audiovisual and audio-only telepsychiatry services is poorly characterized.
To understand how telepsychiatry’s rollout truly exposed structures that maintain inequitable systems and sustain differential access to quality care, essential descriptive data on racial and sociodemographic characteristics of people receiving telepsychiatry are sorely needed. In addition, given that the majority of ambulatory mental health care is provided by primary care, future studies should evaluate the racial and sociodemographic characteristics of people receiving telemental health via telephone versus video in primary care settings.25,26 Moreover, even as there has been no shortage of health equity articles in the last 2 years,27 this rapid review underscores that empirical scholarship is severely lacking on racial and sociodemographic distribution of audio-only versus audiovisual telepsychiatry services since the COVID-19 pandemic. Following the US federal government’s end of the COVID-19 public health emergency, this rapid review raises concern that opportunities to study and gather primary data on the racist structures impacting telemedicine rollout appear to have been missed.
Article Information
Published Online: November 2, 2023. https://doi.org/10.4088/PCC.23r03563
© 2023 Physicians Postgraduate Press, Inc.
Submitted: May 16, 2023; accepted July 26, 2023.
To Cite: Brown TR, Xu KY, Glowinski AL. Structural racism and lessons not heard: a rapid review of the telepsychiatry literature during the COVID-19 public health emergency. Prim Care Companion CNS Disord. 2023;25(6):23r03563.
Author Affiliations: Division of Child and Adolescent Psychiatry, UCLA Semel Institute for Neuroscience and Human Behavior, Los Angeles, California (Brown); Department of Psychiatry, Washington University School of Medicine, St Louis, Missouri (Xu); UCSF Child, Teen and Family Center and Children Benioff Hospitals; UCSF/UCB Schwab Dyslexia and Cognitive Diversity Center; UCSF Department of Psychiatry and Behavioral Sciences, UCSF Weill Institute for Neurosciences, San Francisco, California (Glowinski).
Corresponding Author: Tashalee R. Brown, MD, PhD, UCLA Psychiatry House Staff Office, 760 Westwood Plaza, Suite B7-357, Los Angeles, CA 90024 ([email protected]).
Relevant Financial Relationships: The authors declare no financial interests. None of the authors have financial relationships with organizations that may have an interest in this work.
Funding/Support: Effort for authors was supported by National Institutes of Health (NIH R25 MH112473, Dr Brown and Dr Xu; NIH T32 DA015035, Dr Xu; NIH K12 DA041449, Dr Xu). Effort was also supported in part by the American Psychiatric Association Foundation’s SAMHSA Minority Fellowship program (#H79SM080388, Dr Brown) and the American Psychiatric Association Psychiatric Research Fellowship (Dr Xu). The contents of this publication are solely the responsibility of the authors and do not necessarily represent the official views of the Department of Health and Human Services, American Psychiatric Association, or American Psychiatric Association Foundation. Mention of trade names, commercial practices, or organizations does not imply endorsement by the US Government.
Role of the Funders/Sponsors: The funding sources had no role in the study design, implementation, or interpretation of results.
CLINICAL POINTS
- Very little research has evaluated potential racial and sociodemographic disparities in the use of audio-only versus video telepsychiatry.
- When reading literature on the effectiveness of telepsychiatry, clinicians should be mindful of potentially limited generalizability to marginalized patient populations.
References (27)

- Uscher-Pines L, Sousa J, Jones M, et al. Telehealth use among safety-net organizations in california during the COVID-19 pandemic. JAMA. 2021;325(11):1106–1107. PubMed CrossRef
- Uscher-Pines L, Jones M, Sousa J, et al. The doctor will call me maybe: the uncertain future of audio-only visits and why we need them to address disparities. Health Aff. 2021.
- Ye S, Kronish I, Fleck E, et al. Telemedicine expansion during the COVID-19 pandemic and the potential for technology-driven disparities. J Gen Intern Med. 2021;36(1):256–258. PubMed CrossRef
- WHO. Rapid reviews to strengthen health policy and systems: a practical guide. 2017. Accessed November 1, 2022. https://ahpsr.who.int/publications/i/item/2017-08-10-rapid-reviews-to-strengthen-health-policy-and-systems-a-practical-guide
- Eriksen MB, Frandsen TF. The impact of patient, intervention, comparison, outcome (PICO) as a search strategy tool on literature search quality: a systematic review. J Med Libr Assoc. 2018;106(4):420–431. PubMed CrossRef
- Severe J, Tang RQ, Horbatch F, et al. Factors influencing patients’ initial decisions regarding telepsychiatry participation during the COVID-19 pandemic: telephone-based survey. JMIR Form Res. 2021;5(1):e27357. PubMed CrossRef
- Yue H, Mail V, DiSalvo M, et al. Patient preferences for patient portal-based telepsychiatry in a safety net hospital setting during COVID-19: cross-sectional study. JMIR Form Res. 2022;6(1):e33697. PubMed CrossRef
- Michaels TI, Singal S, Marcy P, et al. Post-acute college student satisfaction with telepsychiatry during the COVID-19 pandemic. J Psychiatr Res. 2022;151:1–7. PubMed CrossRef
- Cheung SG, Capote J, Fan W, et al. Pilot assessment of patient and provider characteristics associated with satisfactory consultation-liaison telepsychiatry encounters. J Acad Consult Liaison Psychiatry. 2021;62(6):582–587. PubMed CrossRef
- Oxford English Dictionary. Oxford University Press; 2020.
- Ezell JM, Griswold D, Chase EC, et al. The blueprint of disaster: COVID-19, the Flint water crisis, and unequal ecological impacts. Lancet Planet Health. 2021;5(5):e309–e315. PubMed CrossRef
- O’Brien LT, Blodorn A, Nelson JC, et al. Understanding white Americans’ perceptions of racism in hurricane Katrina-related events. Group Process Intergroup Relat. 2009;12(4):431–444. CrossRef
- Roberts ET, Mehrotra A. Assessment of disparities in digital access among medicare beneficiaries and implications for telemedicine. JAMA Intern Med. 2020;180(10):1386–1389. PubMed CrossRef
- Galperin H. A failed regulatory remedy? an empirical examination of affordable broadband plan obligations. Int J Commun. 2022:16.
- Affordable Connectivity Program (ACP) Enrollment and Claims Tracker. Universal Service Administrative Co. https://www.usac.org/about/affordable-connectivity-program/acp-enrollment-and-claims-tracker/. 2023.
- Frost MC, Zhang L, Kim HM, et al. Use of and retention on video, telephone, and in-person buprenorphine treatment for opioid use disorder during the COVID-19 pandemic. JAMA Netw Open. 2022;5(10):e2236298. PubMed CrossRef
- Wisniewski JM, Walker B. Association of simulated patient race/ethnicity with scheduling of primary care appointments. JAMA Netw Open. 2020;3(1):e1920010. PubMed CrossRef
- Luck AN, Preston SH, Elo IT, et al. The Unequal Burden of the Covid-19 Pandemic: Capturing Racial/Ethnic Disparities in US Cause-Specific Mortality. Ssm-Popul Hlth; 2022:17.
- Khazanchi R, Evans CT, Marcelin JR. Racism, not race, drives inequity across the COVID-19 continuum. JAMA Netw Open. 2020;3(9):e2019933. PubMed CrossRef
- Romanick-Schmiedl S, Raghu G. Telemedicine - maintaining quality during times of transition. Nat Rev Dis Primers. 2020;6(1):45. PubMed CrossRef
- Serper M, Nunes F, Ahmad N, et al. Positive early patient and clinician experience with telemedicine in an academic gastroenterology practice during the COVID-19 pandemic. Gastroenterology. 2020;159(4):1589–1591.e4. PubMed CrossRef
- Rush KL, Howlett L, Munro A, et al. Videoconference compared to telephone in healthcare delivery: a systematic review. Int J Med Inform. 2018;118:44–53. PubMed CrossRef
- Reese RJ, Conoley CW, Brossart DF. The attractiveness of telephone counseling: an empirical investigation of client perceptions. J Couns Dev. 2006;84(1):54–60. CrossRef
- Gerber MR, Elisseou S, Sager ZS, et al. Trauma-informed telehealth in the COVID-19 era and beyond. Fed Pract. 2020;37(7):302–308. PubMed CrossRef
- Olfson M, Kroenke K, Wang S, et al. Trends in office-based mental health care provided by psychiatrists and primary care physicians. J Clin Psychiatry. 2014;75(3):247–253. PubMed CrossRef
- Rotenstein LS, Edwards ST, Landon BE. Adult primary care physician visits increasingly address mental health concerns. Health Aff (Millwood). 2023;42(2):163–171. PubMed CrossRef
- Lett E, Adekunle D, McMurray P, et al. Health equity tourism: ravaging the justice landscape. J Med Syst. 2022;46(3):17. PubMed CrossRef
Enjoy this premium PDF as part of your membership benefits!