Prim Care Companion CNS Disord 2021;23(3):20cr02880
To cite: Motamedi N, Riahinezhad A, Korenis P. Impact of COVID-19 on a patient with depression and suicidal ideation. Prim Care Companion CNS Disord. 2021;23(3):20cr02880.
To share: https://doi.org/10.4088/PCC.20cr02880
© Copyright 2021 Physicians Postgraduate Press, Inc.
aBronxCare Health System, Icahn School of Medicine at Mount Sinai, Bronx, New York
*Corresponding author: Neda Motamedi, MD, BronxCare Health System, 1276 Fulton Ave, Bronx, NY 10456 ([email protected]).
The coronavirus disease 2019 (COVID-19) pandemic is caused by the novel coronavirus severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2) that predominantly affects the respiratory system. In addition to the physical impact, COVID-19 can have serious effects on people’s mental health.1 There is increasing evidence that SARS-CoV-2 can be neuroinvasive, resulting in neuropsychiatric complications.2 SARS-CoV utilizes 2 pathways to manifest in a neuropsychiatric form: direct and indirect. The direct pathway is infection via hematogenous and neural pathways, while the indirect way includes hypoxia, immune injury, and hypercoagulability. These pathways can cause viral encephalopathy, infection, toxic encephalopathy, and acute cerebrovascular disease. A wide range of psychological outcomes has been observed during the virus outbreak at the individual, community, national, and international levels. Especially at the individual level, people are more likely to experience the fear of getting sick or dying, feeling helpless, and being stereotyped by others.3
Case Report
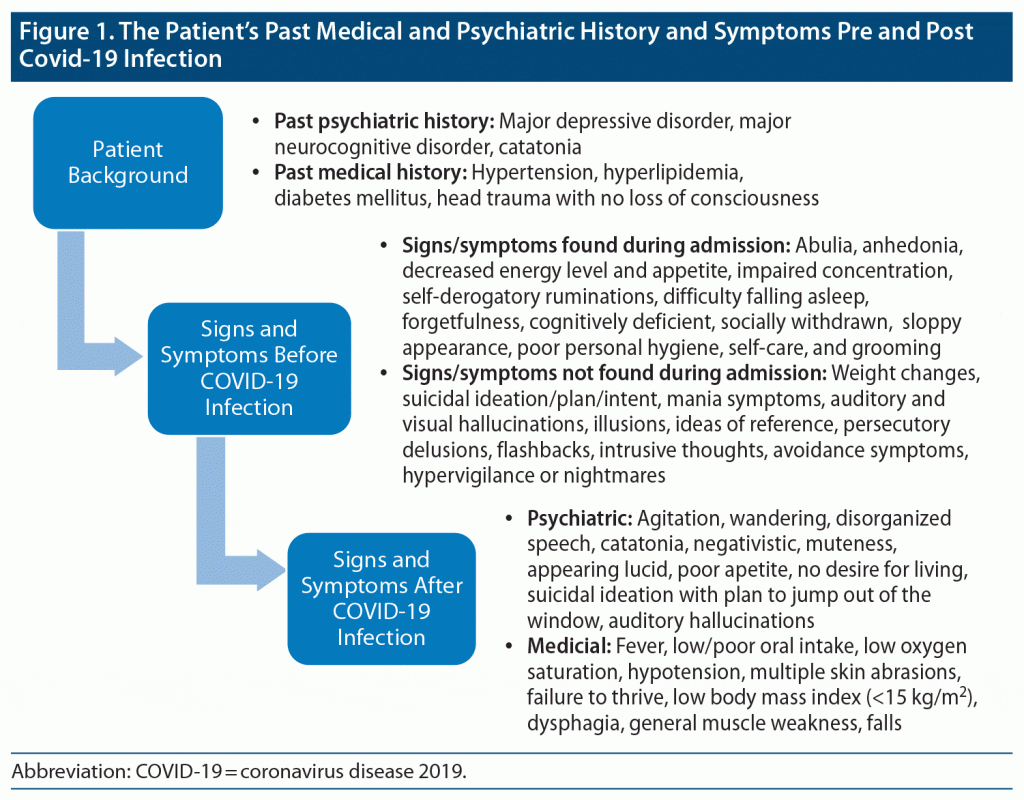
The patient is a 70-year-old Hispanic man with past psychiatric and medical history, as shown in Figure 1, who was admitted to the psychiatry inpatient unit for worsening depression and poor self-care in the context of medication noncompliance. The current episode of depression started 1 year ago when he started feeling depressed and guilty with no identified precipitant. His clinical presentation at the time of admission is also shown in Figure 1. The patient was started on 2 antidepressants, as he had a history of treatment-resistant symptoms (selective serotonin reuptake inhibitor, serotonin-norepinephrine reuptake inhibitor), as well as an atypical antipsychotic for augmentation. While on the unit, his depression and activities of daily living (ADLs) gradually were improving; however, he developed fever, was found to be COVID-19 positive, and was transferred to a COVID inpatient psychiatry unit. He was started on medication for COVID-19 management, and his psychotropic medication was continued in the isolation unit.
He required support to manage his ADLs. He had unsteady gait, severe muscle weakness, and confusion. He was a fall risk and was placed on constant observation. His depression worsened, and his presentation changed to symptoms and signs shown in Figure 1.
He was transferred to the medical unit for further management of failure to thrive and was subsequently admitted. A nutrition consult was placed, and the patient was started on a caloric supplement and intravenous fluid. Gastroenterology was consulted for possible percutaneous endoscopic gastrostomy tube placement, which was not recommended because he was able to maintain his vitals and his laboratory tests were unremarkable. He appeared to have become more delirious and stopped eating and drinking. He was transferred back to the psychiatry unit when medically cleared.
During his battle with COVID-19, not only did his depression worsen and he stopped eating and drinking, but he also stopped having any desire to live and would spend his days begging for death and would scream out loud about being tortured with life. He claimed he was hearing voices telling him to jump out of the window. The treatment team recalled the hopelessness particularly at a point when his body mass index fell below 15 kg/m2 due to poor oral intake and failure to thrive. He continued to refuse to eat, and his weight was 100 lb, which was life threatening.
Team work with patient care technicians, physical therapists, nursing staff, and physicians as well as continuation of care (ie, spoon feeding, assisted bathing, coordinating FaceTime calls with his daughter) increased his motivation and desire to live. As a result, he eventually stopped reporting hopelessness, helplessness, suicidal ideation, and auditory hallucinations.
He was successfully discharged, and his weight increased to 134 lb. The follow-up plan after discharge was determined as weekly outpatient visits for 2 weeks, then every other week for 2 months, and then every month. The patient’s family was involved in his discharge to develop a safety plan, and they were educated about medication compliance and the suicide risk factor.
Discussion
The prevalence rates of stress, anxiety, and depression as a result of the pandemic in the general population are 29.6%, 31.9%, and 33.7%, respectively. In the current crisis, it is vital to identify individuals prone to psychological disorders from various groups and at different layers of populations so that with appropriate psychological strategies, techniques, and interventions, the general population’s mental health will be preserved and improved.4 Recent studies5 have revealed an association between medical history and increased anxiety and depression caused by the spread of COVID-19. Previous research has shown that medical history and chronic illnesses are associated with increased psychiatric distress levels.6,7 People who have a history of medical problems and are also suffering from poor health may feel more vulnerable to a new disease.8 Suicidal ideation was elevated during the COVID-19 pandemic; approximately twice as many respondents reported serious consideration of suicide in the previous 30 days than did adults in the United States in 2018, referring to the previous 12 months (10.7% versus 4.3%, respectively).9 In the present case, COVID-19 not only caused medical comorbidity such as pneumonia, hypoxia, hypotension, general weakness, dysphasia, failure to thrive, and pressure ulcer but also worsened depression, leading the patient to stop eating and drinking and to develop suicidal ideation specifically with a plan to jump out of the window. So, being aware of patients’ backgrounds and needs and having appropriate strategies and adequate screening methods for treatment of high-risk patients can decrease the rate of suicide and save lives. Family access to mental health services, family education, and family support can help to prevent suicide during the COVID-19 crisis as well. Multidisciplinary management and team work played key roles in treatment of our patient with severe depression and suicidal ideation and saved his life.
Published online: May 27, 2021.
Potential conflicts of interest: None.
Funding/support: None.
Meeting presentation: This report will be presented at the 2022 American Psychiatric Association Meeting; May 21–25, 2022; New Orleans, Louisiana.
Patient consent: The patient provided consent to publish the case report, and information has been de-identified to protect anonymity.
References (9)

- Huang Y, Zhao N. Generalized anxiety disorder, depressive symptoms and sleep quality during COVID-19 epidemic in China. a web-based cross sectional survey. Psychiatry Res. 2020;288:112954.
- Troyer EA, Kohn JN, Hong S. Are we facing a crashing wave of neuropsychiatric sequelae of COVID-19? neuropsychiatric symptoms and potential immunologic mechanisms. Brain Behav Immun. 2020;87:34–39. PubMed CrossRef
- Hall RC, Hall RC, Chapman MJ. The 1995 Kikwit Ebola outbreak: lessons hospitals and physicians can apply to future viral epidemics. Gen Hosp Psychiatry. 2008;30(5):446–452. PubMed CrossRef
- Salari N, Hosseinian-Far A, Jalali R, et al. Prevalence of stress, anxiety, depression among the general population during the COVID-19 pandemic: a systematic review and meta-analysis. Global Health. 2020;16(1):57. PubMed CrossRef
- Mazza C, Ricci E, Biondi S, et al. A Nationwide survey of psychological distress among Italian people during the COVID-19 pandemic: immediate psychological responses and associated factors. Int J Environ Res Public Health. 2020;17(9):3165. PubMed CrossRef
- Wang C, Pan R, Wan X, et al. Immediate psychological responses and associated factors during the initial stage of the 2019 coronavirus disease (COVID-19) epidemic among the general population in China. Int J Environ Res Public Health. 2020;17(5):1729. PubMed CrossRef
- Holmes EA, O’Connor RC, Perry VH, et al. Multidisciplinary research priorities for the COVID-19 pandemic: a call for action for mental health science. Lancet Psychiatry. 2020;7(6):547–560. PubMed CrossRef
- Hatch R, Young D, Barber V, et al. Anxiety, depression and post traumatic stress disorder after critical illness: a UK-wide prospective cohort study. Crit Care. 2018;22(1):310. PubMed CrossRef
- Substance Abuse and Mental Health Services Administration. Key substance use and mental health indicators in the United States: results from the 2018 National Survey on Drug Use and Health. SAMHSA website. https://store.samhsa.gov/product/key-substance-use-and-mental-health-indicators-in-the-united-states-results-from-the-2018-national-survey-on-Drug-Use-and-Health/PEP19-5068.
Enjoy this premium PDF as part of your membership benefits!