ABSTRACT
Objective: Novel approaches are needed to assist rural primary care physicians (PCPs) in caring for older patients living with depression and pain who are at an elevated suicide risk. To refine and improve a model of care (PREDICTOR: Pharmacy Identification and Primary Care Intervention of Older Adults at Risk for Suicide), we conducted qualitative interviews with rural PCPs about (1) caring for seniors with depression, pain, and suicidality and (2) their favored procedures for working with psychiatric consultants and the professional characteristics desired in an effective consultant.
Methods: The study utilized a best-practice approach (including double coding) for qualitative interviews with 10 PCPs practicing in rural Pennsylvania. PCPs were interviewed about 3 themes related to caring for older adults with depression, pain, and suicidal ideation and working with psychiatric consultants. The study was conducted from January 2019 to May 2019.
Results: Four primary themes emerged from the interviews. (1) Rural PCPs become comfortable managing depression in older adults out of necessity, but desire collaboration on more complex mental health care. (2) Comorbid depression and pain are universally described as related through a vicious cycle in older adults. (3) Rural PCPs experience varying comfort with prescribing opioids for pain management in older patients, but most prefer not to prescribe opioids, and some refuse to do so. (4) PCPs endorsed the PREDICTOR remote consultation model as potentially beneficial to themselves and their older patients, but strongly desired that the consultant work with them as collaborators and for a collegial professional relationship with the mental health specialist.
Conclusions: Rural PCPs are comfortable with remote consultation for older patients living with depression but desire collegial relationships with these consultants, supporting a collaborative approach. We describe explicit plans for implementing these findings as we refine PREDICTOR, in efforts to promote PCP practice change.
Prim Care Companion CNS Disord 2021;23(2):20m02725
To cite: Karp JF, Hamm ME, Cameron F, et al. Improving effective mental health consultation for rural older adults living with depression and pain: learning from the experiences of rural primary care physicians. Prim Care Companion CNS Disord. 2021;23(2):20m02725.
To share: https://doi.org/10.4088/PCC.20m02725
© Copyright 2021 Physicians Postgraduate Press, Inc.
aDepartment of Psychiatry, University of Pittsburgh School of Medicine, Pittsburgh, Pennsylvania
bCenter for Interventions to Enhance Community Health, University of Pittsburgh, Pittsburgh, Pennsylvania
cDepartment of Psychiatry, College of Medicine, University of Arizona, Tucson, Arizona
dQualitative, Evaluation, and Stakeholder Engagement Research Services, University of Pittsburgh School of Medicine, Pittsburgh, Pennsylvania
eKlingensmith’s Drug Stores, Ford City, Pennsylvania
‡Both Drs Karp and Hamm should be considered co-first authors.
*Corresponding author: Jordan F. Karp, MD, Department of Psychiatry, University of Pittsburgh School of Medicine, Western Psychiatric Hospital, 3811 O’Hara St, Pittsburgh, PA 15213 ([email protected]).
Rates of suicide are higher in older adults than any other age group.1 This is particularly true in rural areas, wherein rates of suicidal ideation among patients receiving telemental health care are approximately 40% for all ages,2 complicated by limited access to mental health specialists.3 The actual contributors to this age-related heightened risk are medical and psychiatric comorbidities, psychosocial challenges and social isolation, and cognitive changes.4–7 Foremost among these modifiable risk factors are pain and depression.8,9 The lifetime prevalence of suicidal ideation among patients with chronic pain is 20%,10 and among older adults who die by suicide, the most prevalent chronic conditions are depression (odds ratio [OR] = 6.44), bipolar disorder (OR = 9.20), and severe pain (OR = 7.52).11 A focus on screening and intervention for older adults with depression and chronic pain in rural areas may reduce suicide.
However, the current system for identifying rural patients at risk of suicide and taking action in primary care settings is broken. For example, while most older patients receive care for depression and pain in primary care,12,13 51% of older adults who complete suicide visited their primary care physician (PCP) within 4 weeks.5,11,14 This finding indicates that systematic screening and risk reduction techniques may not be consistently implemented. In rural areas, patients are sicker,15 which may interfere with the time PCPs can devote to screening and treating neuropsychiatric conditions and preventing suicide. As PCPs adjust to the increased practice of telemedicine in response to the coronavirus disease 2019 (COVID-19) pandemic, and the reduced frequency with which patients are currently seeing their PCP because of social distancing, the routine screening and management of depression and associated risks for suicide by PCPs may not be routinely implemented. Novel approaches to screen for depression and pain by trusted health professionals who have relatively regular telephonic and in-person contact with patients should be considered.
Mental health screening in community pharmacies may be a strategy to identify older adults with depression and pain who are at elevated suicide risk, since patients who are prescribed opioid analgesics for chronic pain must present to the pharmacy at least every month to collect their prescription. Thirty-nine percent of adults aged 65 years and older are prescribed ≥ 5 medications,16 and this is especially true for those living with depression and chronic pain,17 which may indicate additional trips to the pharmacy throughout the month. These pharmacy trips present frequent opportunities for screening and possible referral.
Once identified, these complex older adults are best managed in primary care using a multidisciplinary approach that includes mental health consultation and physician education in behavioral health clinical best practices18,19 along with care coordination.20 Intervention studies utilizing this approach for older adults in primary care settings have shown encouraging results in reducing symptoms of depression, pain, and suicidal ideation.21–24 While there are a variety of remote telehealth models available to assist rural PCPs in the care of older patients with these conditions (eg, ECHO [Extension for Community Health Outcomes],25 telepsychiatry), blending pharmacy identification, remote assessment by a mental health clinician, and focused consultation recommendations provided to both patient and PCP is a unique care approach for rural areas to identify patients at risk and improve outcomes.
We named this rural pharmacy screening and intervention approach PREDICTOR: Pharmacy Identification and Primary Care Intervention of Older Adults at Risk for Suicide. Part of the clinical model development was to qualitatively assess rural PCPs to (1) ascertain attitudes to caring for older adults with depression, pain, and suicidal ideation; (2) determine favored procedures for receiving clinical consultation and identify professional characteristics that PCPs desire in an effective consultant; and (3) use this feedback to refine the PREDICTOR model of screening and intervention. This article describes these qualitative surveys and how we used the results of these surveys to refine our model of remote consultation and collaboration with rural PCPs to improve the care of these complex patients.
METHODS
Overview
These qualitative interviews were the initial part of our treatment development project, as we assessed clinical support needs and refined our consultation model. Rural and suburban PCPs were interviewed about the 3 themes (described previously) related to caring for older adults with depression, pain, and suicidal ideation and working with psychiatric consultants. We followed best practice for qualitative interviews, coding, and analysis, and these interviews were all led by an experienced qualitative researcher (M.E.H.). The University of Pittsburgh Institutional Review Board approved all research procedures as well as our obtaining recorded verbal consent, which was provided by all participants. The study was conducted from January 2019 to May 2019.
Recruitment
Rural PCPs who sent prescriptions to our partnering community pharmacies were targeted via direct letter (n = 111). If agreeable, the interviewer contacted the PCP first via e-mail and then, if necessary, via phone to coordinate the interview. Ten interviews were selected because of the high likelihood of achieving thematic saturation.26 Recruitment continued until we completed interviews with 10 PCPs (each from a different practice) practicing in rural southwest and central Pennsylvania, and the qualitative interviewer rated a high level of confidence that thematic saturation had been reached.
Interview Guide Development and Data Collection
The interview was developed in an iterative fashion using expert stakeholders from geriatric psychiatry, primary care, geriatric medicine, community pharmacy practice, and an anthropologist with expertise in formative evaluation of behavioral and programmatic interventions and qualitative methodology. Given the experience of the interviewer (M.E.H.) and the consensus from stakeholders, we did not pilot the interview prior to commencing the project.
All interviews were conducted by phone by the same experienced qualitative methodologist (M.E.H.). Interviews lasted approximately 30 minutes and followed a semistructured interview guide, ensuring that participants were asked the same questions, but allowing for individualized follow-up at the interviewer’s discretion to more deeply probe our areas of interest. The questions asked in the guide (Supplementary Appendix 1) addressed treatment of depression, suicidal ideation, and chronic pain both individually and as comorbidities in rural older adults, barriers and facilitators to care in the PCP’s practice area, and what could be done to improve care. Following these general practice questions, interviewees were given a brief description of the proposed PREDICTOR approach to remote consultation and asked whether they thought this would help in the care of these challenging older patients and how they would like the remote consultation implemented. Interviews were audio recorded and subsequently transcribed verbatim, with any identifying details such as name or exact practice location redacted. PCPs provided verbal consent prior to initiating the interviews and were compensated $100.
Analysis
Analysis followed established principles for conducting a thematic analysis, including transcription of verbal data, familiarization with the data through close reading of transcripts, generating initial codes, refining those codes, searching coded data for themes, and then refining those themes though further review of the data.27 The interviewer inductively generated a qualitative codebook based on the interview content via a process sometimes known as “editing,” in which an analyst reads through available data searching for meaningful segments of text that highlight important concepts.28 This codebook was then applied to all 10 transcripts by the original interviewer and an additional coder who also had prior qualitative research experience (F.C.). All coding disagreements were adjudicated by the 2 coders to full agreement. The interviewer/primary coder then summarized the data and generated themes, which were then checked for accuracy and expanded by reviewing the codes relevant to each theme. Themes were shared with and corroborated by the secondary coder and then presented to the larger research team of content experts for discussion as a form of investigator triangulation.
RESULTS
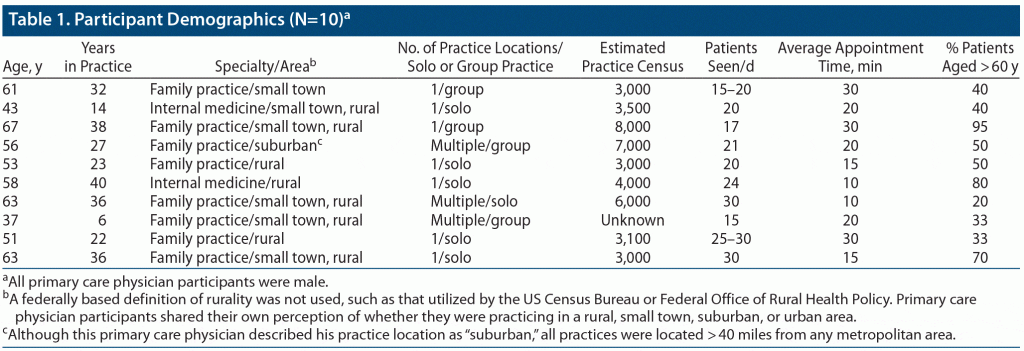
Ten rural PCPs participated in the interviews (Table 1). All were male with an average of 27 years of experience in family or internal medicine in small towns and rural settings. A median of 45% of the practice populations were older than 60 years of age. Four primary themes from the interviews are described. Table 2 lists representative quotes for each theme.
Theme 1: Rural PCPs Are Comfortable Managing Depression in Older Adults Out of Necessity, But Desire Collaboration on More Complex Mental Health Care
All PCPs interviewed were comfortable treating and managing depression in older patients. This comfort was borne out of familiarity and necessity. Depression is common in their patients, and a lack of available specialty psychiatric care in their areas resulted in PCPs learning more than they otherwise might have about how to independently manage late-life depression. All PCPs had encountered suicidal ideation enough to know what to do if a patient became suicidal, although at that point they cease to manage care on their own and refer to any available service, including emergency departments, psychiatric hospitals, and psychiatric specialists, depending on what is geographically available. However, nearly half felt they lacked adequate emergency services, and one noted that in the winter, the mountainous terrain could make transit out of the community to reach an emergency department for a suicidal patient especially treacherous. Of those with access to emergency services, almost all noted a lack of personal relationship with psychiatric providers that made coordinated care difficult. The PCPs were uncomfortable managing depression on their own if a patient’s depression proved to be treatment resistant or complicated by bipolar disorder or psychosis.
Nearly all PCPs engaged in routine, universal depression screening. Several universally screened for suicidality as well, but it was more common to screen for suicide among patients who were depressed or expressed suicidal thoughts in the past. Despite their general comfort managing depression, the providers frequently described a desire for a psychiatrist colleague with whom they could collaborate on depression care. Some had previously had such a collegial relationship, but their psychiatric colleagues had retired or closed practice, while others had always experienced a dearth of psychiatric collaborators in their areas. PCPs described rarely receiving communication from psychiatrists who do see their patients, possibly due to HIPAA concerns but also because they felt these providers were too busy to send a report and because they might rotate in and out of the community frequently if they were hospital affiliated. Collaborative relationships were described as lightening the burden of mental health care on PCPs and improving patient care.
Theme 2: Comorbid Pain and Depression in Late Life Are Universally Described by Rural PCPs as Related Through a Vicious Cycle
PCPs described chronic pain as ubiquitous in their older patients, and all described chronic pain and depression as interacting with each other in a vicious cycle. Metaphors used to describe that cycle included “chicken and egg” and the notion that depression and pain are “two sides of the same coin.” Some providers regarded this vicious cycle as physiologic (ie, they described older depressed patients as being physiologically sensitized to pain or “chronic pain affecting levels of neurotransmitters, leading to depression.” Others regarded the vicious cycle as being more circumstantial in nature—ie, if one is depressed, they will focus more on the pain, and if one is in pain, they will be less active, leading to isolation and depression. PCPs occasionally viewed chronic pain as “psychosomatic” in patients who either held stigma toward mental health or whose social networks held such stigmatic beliefs. This was described as mental pain manifesting as physical pain. This physical pain could more easily be expressed to their PCP, who could then acknowledge and treat it.
Most interviewees preferred to treat comorbid pain and depression in these older adults simultaneously, stating that treating them as unlinked conditions is ineffective. Some used treatment of chronic pain as a gateway to treating depression for older patients who held more stigma toward mental health. In such cases, PCPs would address pain first, and then convince patients that the pain was wearing them out and causing depression, and that treating both simultaneously might yield greater success. In addition to using duloxetine (an antidepressant approved by the US Food and Drug Adminsitration for both depression and several pain conditions), PCPs described other treatments for chronic pain including physical therapy, support groups and pets, acetaminophen, non–steroidal anti-inflammatory drugs (NSAIDS), gabapentin, opioids, and, rarely, medical marijuana and cannabidiol (CBD).
Theme 3: Rural PCPs Experience Varying Comfort With Prescribing Opioids for Pain Management in Older Patients, But Most Prefer Not to Prescribe Opioids, and Some Refuse to Do So
Providers were split about opioid prescribing in the context of the current epidemic. A minority of providers felt that in the current climate, they were “demonized” for prescribing opioids, and that older patients prescribed opioids long term were likewise now stigmatized. These providers felt that either older patients do not experience addiction, and thus do not contribute to the crisis, or that it was unfair to older patients who had no other options for controlling pain, citing as examples patients who described that if their pain could not be controlled they would not want to live.
Most providers, however, described avoiding opioids given the current crisis. Some noted that it had become more cumbersome to prescribe opioids due to restrictions from the state and insurance companies. These providers may prescribe a limited number of opioids for acute pain, but none for chronic pain, and some refused to prescribe them for chronic pain even for those patients whose chronic pain failed to respond to any other treatments. Others were even more conservative and simply refused to prescribe opioids at all; incoming patients on existing opioid regimens were told that they would need to find another provider or be referred to pain management if they wished to continue opioids. Providers who refused to prescribe opioids took this approach because of personal experiences with patients who overdosed, had requested opioids for nonanalgesic or euphoria-inducing use, had diverted medications, or the PCP was concerned about geriatric-specific adverse events such as delirium and falls.
Regardless of their personal opioid prescribing practices, providers noted that treating older patients with chronic pain without opioids is challenging since some comorbid conditions made the use of acetaminophen and NSAIDS unsafe. Physical therapy was discussed as a useful, but limited, treatment due to cost and travel. A few providers explored medical marijuana and CBD (medical marijuana was legalized in Pennsylvania in 2016), although a drawback was relatively high costs due to lack of insurance coverage. PCPs described pain management clinics as often unpleasant for their older patients because they felt like they were viewed as “drug addicts” in the clinics.
Theme 4: Rural PCPs Endorsed the PREDICTOR Consultation Model as Potentially Useful to Themselves and Their Older Patients, But Strongly Desired That the PREDICTOR Team Work With Them as Collaborators
Providers interviewed were nearly universally positive in response to the description of the PREDICTOR approach, which included (1) pharmacy-based screening for older patients with pain and/or depression and case identification as a method to efficiently identify at-risk patients via a frequently accessed and highly-trusted community pharmacist when picking up prescriptions, (2) remote patient consultation about depression and pain management by a mental health clinician, and (3) receipt of the report with specific treatment recommendations. Earlier in the interview, some providers identified teleconsult as a potential means of addressing the provider shortage and long wait times that make accessing psychiatric care in their areas so difficult. Some participants felt that PREDICTOR could reduce individual risk and professional burden of caring for older patients’ psychiatric and pain problems: PCPs would not be the only physician responsible for the patient. Others thought they might improve their own clinical skills in providing high-quality late-life psychiatric and pain care.
However, providers’ vision of potential benefit of PREDICTOR was heavily grounded in the prerequisite that interactions with the remote psychiatrists be relational and promote collaborative care. Provided that the consultation permits them to develop the collegial and collaborative relationship with psychiatrists, they were enthusiastic about participating and thought that their patients could benefit. Providers said that they would feel comfortable accepting recommendations made through the remote consultations, although several cautioned that they would implement them only if they “agreed with” the recommendation. This caveat about buy-in reinforced the need for remote psychiatrists to be aware of current practice patterns of rural PCPs and to be prepared to offer clinical education about best practice for these conditions.
Providers were nearly unanimous in wanting to receive written correspondence from the remote consultants. Written correspondence was preferred to telephonic physician-to-physician communication because it could be referred to repeatedly and because it provided documentation. Providers wanted the option for a phone call follow-up if clarification was needed, and they viewed such calls as a way to establish and maintain a relationship with the consultant.
DISCUSSION
In this qualitative study of rural PCPs’ experiences with and approaches to treating depression, pain, and suicidality in older adults, we found that PCPs have become comfortable managing depression due to a dearth of mental health services in their areas, but that they desire collaborators when managing more severe mental health conditions. Rural PCPs identify comorbid depression and chronic pain as linked through a vicious cycle, endorse discomfort with the prescription of opioids to treat pain (whether that discomfort is driven by current restrictions on prescribing or by desire to avoid opioids because of geriatric-specific concerns), and describe being challenged by the lack of other analgesic options for older adults. Furthermore, rural PCPs are comfortable with remote consultation to improve the care of their older patients living with depression and pain, but desire collegial relationships with these consultants that support a collaborative approach to ongoing care.
While most all PCPs said they routinely screened for depression and even suicide in their older patients, the elevated rates of depression, suicide, and pain in rural seniors29–31 suggest that (1) the PCPs may overestimate their consistency in screening for and treating these conditions or (2) the treatments offered (eg, dose, duration, follow-up) by these rural PCPs do not sufficiently match the patient’s diagnoses and clinical needs. Both possibilities support the novelty and clinical effectiveness of the PREDICTOR model of screening and identification in rural community pharmacies with subsequent remote consultation to provide more thorough mental health and pain evaluation and geriatric-specific treatment recommendations (made especially relevant given the coronavirus pandemic and need for older patients to access screening and treatment via unique providers). In retrospect, it would have been ideal to include more questions about how to better integrate primary care and pharmacy settings and survey the PCPs about additional ways to harmonize care between these 2 clinical sites.
While there are a handful of qualitative studies surveying rural PCPs about the care of depression in both older32 and younger adults,33 and no qualitative studies of rural PCPs’ attitudes toward caring for older adults living with pain, to our knowledge this is the first qualitative study of rural PCPs about their attitudes toward (1) caring for older patients living with these comorbid conditions and (2) the professional characteristics they desire in an effective consultant. PCPs reported a lack of any collegial relationships with local psychiatric services, making care coordination difficult, and that they were dismayed by rarely receiving written communication from psychiatrists who see their patients. We observed that PCPs (1) feel comfortable accepting recommendations that were made through the remote consultations, (2) prefer to receive written treatment recommendations (as opposed to physician-to-physician phone consultations) about their patients, and (3) envisioned that the best relationship they could have with remote consultants is one that is “relational and geared towards collaborative care of patients.” The IMPACT (collaborative care of late-life depression)34 and PROSPECT (collaborative care to reduce late-life suicide and depression)35 projects both support the clinical benefit of this approach. PREDICTOR attempts to expand collaborative care for depression and pain by shifting case identification from the PCP practice to customers at rural community pharmacies, potentially increasing scalability and the chance to capture a greater number of at-risk patients.
These findings replicate those of a recent qualitative survey36 of urban and rural PCPs to better understand reasons for poor uptake of a telephone-based intervention for neuropsychiatric conditions. In that study,36 PCPs desired greater integration of the mental health specialist into their practice. While the PCPs appreciated expert psychiatric recommendations, they rarely changed their practices, and this practice change was negatively influenced by the limited relationship between the mental health specialists and PCPs. Another qualitative study (this of mental health and social service workers) in rural Australia reinforced the notion that the most significant barrier to improving rural mental health across the life span was the lack of communication at the individual, case management, and organizational levels.37 It appears that clinical trust and a “professional friendship” between PCPs and mental health consultants is essential for PCPs and may be necessary for them to consistently implement the clinical recommendations provided by remote psychiatric consultations.
It is a limitation that all participants were men (by virtue of who responded to our outreach, not as an intentional sampling strategy), and all were drawn from the same region. It is possible that providers of different racial, ethnic, or gender backgrounds or from different rural regions (ie, different states that have a unique local culture of prescribing opioids, recreational marijuana laws, or different blend of family practice versus internal medicine providers) would have highlighted different issues or had different opinions. Future studies should seek a more diverse sample of PCPs. It should also be acknowledged that the self-selected PCPs who participated may reflect a subset of clinicians agreeable to being interviewed; a larger, more systematic assessment may have yielded other opinions.
These replicated observations are precisely the sort of information we hoped to obtain as we develop and test the PREDICTOR model of care. Indeed, the goals of qualitative work in medicine are to ascertain the lived experiences of a specific population about a topic that may improve care. Qualitative interviews provide the groundwork for developing, refining, implementing, and testing interventions and models of care. Using the data obtained from this qualitative project, and in the spirit of iterative intervention development, we have refined the PREDICTOR model in the following ways. First, as part of the written consultation, we explicitly state to PCPs that (1) we view our roles as collaborators in the care of these rural older patients, but ultimately the PCP remains the physician of record and care resides with the PCP; (2) these are clinical recommendations for the PCP to consider, and if they disagree with any or are uncomfortable implementing a suggestion, we would like the opportunity to discuss other treatment options; (3) we are available to the PCP to provide ongoing clinical decision support and are available for “curbside consults” by e-mail or phone; and (4) we will provide regular opportunities for clinical education via planned webinars to further develop trust and professional relationships between our clinical research team and these rural PCPs.
Community pharmacies are a trusted clinical space at which patients from many different PCP offices visit on a regular basis to pick up prescriptions. Given the lack of a common electronic medical record (of note, none of the PCP participants shared an electronic medical record system with us), screening at community pharmacies based on prescription status and then providing decision support to the prescribing PCPs may be more efficient than trying to screen from a variety of disconnected PCP practices. As we move forward with testing PREDICTOR on a larger scale, the lack of a shared electronic medical record across primary care practices will require implementation of creative communication solutions to assure PCPs receive remote mental health consultations in a consistently useful manner.
Submitted: September 22, 2020; accepted September 29, 2020.
Published online: March 18, 2021.
Potential conflicts of interest: Dr Karp has received medication supplies for investigator-initiated trials from Pfizer and Indivior within the last 5 years, has received compensation from Otsuka for development and presention of a webinar from Otsuka (disease state, not product focused), and serves as an advisor to NightWare and Aifred Health. Drs Karp and Reynolds receive compensation from American Association for Geriatric Psychiatry for service on the editorial board of The American Journal of Geriatric Psychiatry. Dr Reynolds has received research support from the National Institutes of Health (NIH), the Patient Centered Outcomes Research Institute, the Center for Medicare and Medicaid Services, the American Foundation for Suicide Prevention, the Brain and Behavior Research Foundation, and the Commonwealth of Pennsylvania and BristolMeyerSquib and Pfizer have provided pharmaceutical supplies for his NIH-sponsored research. Drs Hamm, Maher, and Kincman; Ms Cameron and Mr Lightfoot report no conflicts of interest related to the subject of this article.
Funding/support: This project was supported by Grant SRG-0-200-17 awarded to Dr Karp from the American Foundation for Suicide Prevention.
Role of the sponsor:The funder had no role in the design and conduct of the study; collection, management, analysis, and interpretation of data; or preparation, review, or approval of the manuscript.
Disclaimer: The content is solely the responsibility of the authors and does not necessarily represent the official views of the American Foundation for Suicide Prevention.
Supplementary material: See accompanying pages.
Clinical Points
- Rural primary care physicians (PCPs) describe comorbid depression and pain as related through a vicious cycle in older adults.
- Rural PCPs value remote geriatric mental health consultation but desire a relational approach that supports collaborative care.
- PCPs prefer written correspondence (versus physician-to-physician calls) with the option for a phone call follow-up if clarification is needed.
References (37)

- Raue PJ, Ghesquiere AR, Bruce ML. Suicide risk in primary care: identification and management in older adults. Curr Psychiatry Rep. 2014;16(9):466. PubMed CrossRef NLM
- Tarlow KR, Johnson TA, McCord CE. Rural status, suicide ideation, and telemental health: risk assessment in a clinical sample. J Rural Health. 2019;35(2):247–252. PubMed CrossRef NLM
- Fiske A, Gatz M, Hannell E. Rural suicide rates and availability of health care providers. J Community Psychol. 2005;33(5):537–543. CrossRef
- Hawton K, van Heeringen K. Suicide. Lancet. 2009;373(9672):1372–1381. PubMed CrossRef NLM
- Lapierre S, Erlangsen A, Waern M, et al; International Research Group for Suicide among the Elderly. A systematic review of elderly suicide prevention programs. Crisis. 2011;32(2):88–98. PubMed CrossRef NLM
- Gujral S, Dombrovski AY, Butters M, et al. Impaired executive function in contemplated and attempted suicide in late life. Am J Geriatr Psychiatry. 2014;22(8):811–819. PubMed CrossRef NLM
- Gujral S, Ogbagaber S, Dombrovski AY, et al. Course of cognitive impairment following attempted suicide in older adults. Int J Geriatr Psychiatry. 2016;31(6):592–600. PubMed CrossRef NLM
- Cheatle MD. Depression, chronic pain, and suicide by overdose: on the edge. Pain Med. 2011;12(suppl 2):S43–S48. PubMed CrossRef NLM
- Pfeiffer PN, Kim HM, Ganoczy D, et al. Treatment-resistant depression and risk of suicide. Suicide Life Threat Behav. 2013;43(4):356–365. PubMed CrossRef NLM
- Tang NKY, Crane C. Suicidality in chronic pain: a review of the prevalence, risk factors and psychological links. Psychol Med. 2006;36(5):575–586. PubMed CrossRef NLM
- Juurlink DN, Herrmann N, Szalai JP, et al. Medical illness and the risk of suicide in the elderly. Arch Intern Med. 2004;164(11):1179–1184. PubMed CrossRef NLM
- Breuer B, Cruciani R, Portenoy RK. Pain management by primary care physicians, pain physicians, chiropractors, and acupuncturists: a national survey. South Med J. 2010;103(8):738–747. PubMed CrossRef NLM
- Hall CA, Reynolds-Iii CF. Late-life depression in the primary care setting: challenges, collaborative care, and prevention. Maturitas. 2014;79(2):147–152. PubMed CrossRef NLM
- Luoma JB, Martin CE, Pearson JL. Contact with mental health and primary care providers before suicide: a review of the evidence. Am J Psychiatry. 2002;159(6):909–916. PubMed CrossRef NLM
- Weeks WB, Kazis LE, Shen Y, et al. Differences in health-related quality of life in rural and urban veterans. Am J Public Health. 2004;94(10):1762–1767. PubMed CrossRef NLM
- Kantor ED, Rehm CD, Haas JS, et al. Trends in prescription drug use among adults in the united states from 1999–2012. JAMA. 2015;314(17):1818–1831. PubMed CrossRef NLM
- Sergi G, De Rui M, Sarti S, et al. Polypharmacy in the elderly: can comprehensive geriatric assessment reduce inappropriate medication use? Drugs Aging. 2011;28(7):509–518. PubMed CrossRef NLM
- Kok RM, Reynolds CF 3rd. Management of depression in older adults: a review. JAMA. 2017;317(20):2114–2122. PubMed CrossRef NLM
- Zalsman G, Hawton K, Wasserman D, et al. Suicide prevention strategies revisited: 10-year systematic review. Lancet Psychiatry. 2016;3(7):646–659. PubMed CrossRef NLM
- Parekh AK, Goodman RA, Gordon C, et al; HHS Interagency Workgroup on Multiple Chronic Conditions. Managing multiple chronic conditions: a strategic framework for improving health outcomes and quality of life. Public Health Rep. 2011;126(4):460–471. PubMed CrossRef NLM
- Gallo JJ, Morales KH, Bogner HR, et al. Long term effect of depression care management on mortality in older adults: follow-up of cluster randomized clinical trial in primary care. BMJ. 2013;346:f2570. PubMed CrossRef NLM
- Alexopoulos GS, Reynolds CF 3rd, Bruce ML, et al; PROSPECT Group. Reducing suicidal ideation and depression in older primary care patients: 24-month outcomes of the PROSPECT study. Am J Psychiatry. 2009;166(8):882–890. PubMed CrossRef NLM
- Unützer J, Tang L, Oishi S, et al; IMPACT Investigators. Reducing suicidal ideation in depressed older primary care patients. J Am Geriatr Soc. 2006;54(10):1550–1556. PubMed CrossRef NLM
- Dobscha SK, Corson K, Perrin NA, et al. Collaborative care for chronic pain in primary care: a cluster randomized trial. JAMA. 2009;301(12):1242–1252. PubMed CrossRef NLM
- Scott JD, Unruh KT, Catlin MC, et al. Project ECHO: a model for complex, chronic care in the Pacific Northwest region of the United States. J Telemed Telecare. 2012;18(8):481–484. PubMed CrossRef NLM
- Namey E, et al. Evaluating bang for the buck:a cost-effectiveness comparison between individual interviews and focus groups based on thematic saturation levels. Am J Eval. 2016;37(3):425–440. CrossRef
- Braun V, Clarke V. Using thematic analysis in psychology. Qual Res Psychol. 2006;3(2):77–101. CrossRef
- Crabtree BF, Miller WL. Doing qualitative research. 2nd ed. Thousand Oaks, CA: SAGE Publishing; 1999.
- Bell RA, Smith SL, Arcury TA, et al. Prevalence and correlates of depressive symptoms among rural older African Americans, Native Americans, and Whites with diabetes. Diabetes Care. 2005;28(4):823–829. PubMed CrossRef NLM
- 30. Dahlhamer J, Lucas J, Zelaya C, et al. Prevalence of chronic pain and high-impact chronic pain among adults—United States, 2016. MMWR Morb Mortal Wkly Rep. 2018;67(36):1001–1006. PubMed CrossRef NLM
- Ivey-Stephenson AZ, Crosby AE, Jack SPD, et al. Suicide trends among and within urbanization levels by sex, race/ethnicity, age group, and mechanism of death—United States, 2001–2015. MMWR Surveill Summ. 2017;66(18):1–16. PubMed CrossRef NLM
- Fuller J, Oster C, Dawson S, et al. Improving the network management of integrated primary mental healthcare for older people in a rural Australian region: protocol for a mixed methods case study. BMJ Open. 2014;4(9):e006304. PubMed CrossRef NLM
- Colon-Gonzalez MC, McCall-Hosenfeld JS, Weisman CS, et al. “Someone’s got to do it”—primary care providers (PCPs) describe caring for rural women with mental health problems. Ment Health Fam Med. 2013;10(4):191–202. PubMed NLM
- Unützer J, Katon W, Callahan CM, et al; IMPACT Investigators. Improving Mood-Promoting Access to Collaborative Treatment. Collaborative care management of late-life depression in the primary care setting: a randomized controlled trial. JAMA. 2002;288(22):2836–2845. PubMed CrossRef NLM
- Bruce ML, Ten Have TR, Reynolds CF 3rd, et al. Reducing suicidal ideation and depressive symptoms in depressed older primary care patients: a randomized controlled trial. JAMA. 2004;291(9):1081–1091. PubMed CrossRef NLM
- Sunderji N, Ion A, Zhu A, et al. Challenges in conducting research on collaborative mental health care: a qualitative study. CMAJ Open. 2019;7(2):E405–E414. PubMed CrossRef NLM
- Sweeney P, Kisely S. Barriers to managing mental health in Western Australia. Aust J Rural Health. 2003;11(4):205–210. PubMed CrossRef NLM
Enjoy this premium PDF as part of your membership benefits!