Objective: To assess insomnia and its health correlates among elderly primary care patients in India.
Methods: A multicenter, cross-sectional survey was administered to 1,770 elderly primary care patients from 71 government primary health centers in Kerala, India, from May to December 2016. Insomnia was evaluated using the Insomnia Severity Index. Basic demographics and information about medical illness were collected. Study instruments included the Patient Health Questionnaire-Somatic, Anxiety, and Depression Symptoms; Alcohol Use Disorders Identification Test; Fagerström Test for Nicotine Dependence; 12-item World Health Organization Disability Assessment Schedule; and World Health Organization Quality of Life-BREF.
Results: Valid responses were received from 1,574 (89%) patients, of whom the mean age was 68.6 years and 55.5% were women. Clinical insomnia was reported by 11.8%, whereas 30.4% had subclinical insomnia. Primary care attendees with subclinical as well as clinical insomnia had increased odds of being older and female and having chronic medical illness compared with those without insomnia. Patients with clinical insomnia had increased odds of common mental disorders (anxiety, depression, and somatization) and greater disability compared with the subclinical or no insomnia groups. Those with subclinical insomnia had poor satisfaction with life compared to those with no insomnia.
Conclusions: Insomnia in the elderly is frequent in primary care patients in India and has multiple negative health correlates. This study reiterates the need for more awareness with regard to detection and management of insomnia in the elderly population.
Insomnia Among Elderly Primary Care Patients in India
ABSTRACT
Objective: To assess insomnia and its health correlates among elderly primary care patients in India.
Methods: A multicenter, cross-sectional survey was administered to 1,770 elderly primary care patients from 71 government primary health centers in Kerala, India, from May to December 2016. Insomnia was evaluated using the Insomnia Severity Index. Basic demographics and information about medical illness were collected. Study instruments included the Patient Health Questionnaire-Somatic, Anxiety, and Depression Symptoms; Alcohol Use Disorders Identification Test; Fagerström Test for Nicotine Dependence; 12-item World Health Organization Disability Assessment Schedule; and World Health Organization Quality of Life-BREF.
Results: Valid responses were received from 1,574 (89%) patients, of whom the mean age was 68.6 years and 55.5% were women. Clinical insomnia was reported by 11.8%, whereas 30.4% had subclinical insomnia. Primary care attendees with subclinical as well as clinical insomnia had increased odds of being older and female and having chronic medical illness compared with those without insomnia. Patients with clinical insomnia had increased odds of common mental disorders (anxiety, depression, and somatization) and greater disability compared with the subclinical or no insomnia groups. Those with subclinical insomnia had poor satisfaction with life compared to those with no insomnia.
Conclusions: Insomnia in the elderly is frequent in primary care patients in India and has multiple negative health correlates. This study reiterates the need for more awareness with regard to detection and management of insomnia in the elderly population.
Prim Care Companion CNS Disord 2020;22(3):19m02581
To cite: Dahale AB, Jaisoorya TS, Manoj L, et al. Insomnia among elderly primary care patients in India. Prim Care Companion CNS Disord. 2020;22(3):19m02581.
To share: https://doi.org/10.4088/PCC.19m02581
© Copyright 2020 Physicians Postgraduate Press, Inc.
aDepartment of Psychiatry, National Institute of Mental Health and Neurosciences, Bangalore, India
bNational Health Mission Alappuzha, Kerala, India
cNational Health Mission Thiruvananthapuram, Kerala, India
dDepartment of Psychogeriatrics, Waitemata District Health Board, Takapuna, New Zealand
eDepartment of Psychiatry, University of Auckland, Auckland, New Zealand
fDepartment of Biostatistics, National Institute of Mental Health and Neurosciences, Bangalore, India
*Corresponding author: T. S. Jaisoorya, MD, MRCPsych, Department of Psychiatry, National Institute of Mental Health and Neurosciences, Bangalore, India 560 029 ([email protected]).
Insomnia is a common but underrecognized problem in the elderly population and is reported to have multiple negative health correlates.1 Physical conditions, including arthritis, musculoskeletal pain, chronic obstructive pulmonary disease, and cardiovascular problems, are reported at higher rates in individuals with insomnia. Those with insomnia also report increased rates of mental health issues, especially depressive and anxiety disorders.2,3 Insomnia in the elderly is associated with increased mortality, higher functional limitation, and impaired quality of life.4-6 The public health burden of insomnia is significant given greater odds of hospitalization, use of home health care services, and nursing home use.7
Annual incidence rates for insomnia symptoms in the elderly are reported to be around 5%,1 whereas the prevalence of insomnia in the general population is reported to be over 20%.3,8 Higher insomnia rates are reported among primary care attendees, with rates varying between 42% and 57%.9,10 Sociodemographic correlates such as older age, female sex, widowhood, and lower economic status have all been implicated in studies1,11-13 of insomnia, although with inconsistencies.
Existing Indian studies14-16 of insomnia among elderly subjects are few and utilize differing samples, with reported prevalence ranging from 20% to 59%. Further, correlates of insomnia among elderly subjects in India have only been reported in 1 study14 from a single institution, hence the findings have limited generalizability. In addition, it is increasingly recognized that cultural and geographical factors have a significant role in mediating expression of sleep problems.17 Hence, extension of findings from other countries and cultures may have limitations. India has the second largest elderly population in the world, thus addressing health care issues in this group is a priority.18
The objective of this study was to assess the prevalence of insomnia and its correlates among elderly patients presenting to primary care centers across the state of Kerala in south India. Kerala has seen an increase in life expectancy and low birth rates as result of an aging population. Currently, the state has the highest proportion of elderly individuals in the country (12.6% compared to the national average of 8.0%).19 Thus, Kerala was an ideal setting in which to screen elderly subjects for insomnia and its correlates.
This study reports partial findings of a larger study that assessed psychological problems among subjects attending primary care settings, and the methodology is a replication of a similar study done in an adult population by the same authors.20
METHODS
This study was a cross-sectional survey of elderly subjects (aged ≥ 60 years per the government of India definition) attending primary health centers (PHCs) in Kerala, India, from May to December 2016. Ethical clearance of the study was obtained from Government Medical College, Ernakulam, India.
Of the 825 PHCs across the state of Kerala, 71 were randomly selected for the survey. At least 25 consecutive elderly patients from each PHC were invited to participate. Subjects who had dementia, severe hearing, or visual impairment were excluded. A sample size of 1,537 was calculated for a 2-sided 95% confidence interval with a width of 4%, considering the expected prevalence of 20%.
The block public relations officers of the National Health Mission (Kerala), who had received prior training, administered the questionnaire. The block public relations officers have postgraduate degrees in social work and a supervisory role for implementation of public health programs of the PHCs. Subjects who provided informed consent were administered the questionnaire.
Sociodemographic profiles and information about chronic medical illness (eg, hypertension, diabetes mellitus, epilepsy, tuberculosis, chronic dermatologic conditions, asthma, arthritis) were collected using a checklist (self-report). In addition, insomnia and its correlates were evaluated using various structured tools.
Study Instruments
Insomnia Severity Index. Insomnia was evaluated with the Insomnia Severity Index (ISI).21 The ISI is a self-administered tool that assesses the nature, severity, and impact of insomnia in the previous 2 weeks. A score < 7 denotes no insomnia, 8-14 denotes subthreshold insomnia, 15-21 denotes clinical insomnia (moderate), and 22-28 denotes clinical insomnia (severe). In this study, elderly subjects with sleep disturbances were categorized on the basis of their ISI scores as having clinical insomnia (≥ 15) or subclinical insomnia (≤ 14).
Patient Health Questionnaire-Somatic, Anxiety, and Depression Symptoms. Occurrence and co-occurrence of depression, anxiety, and somatic symptoms are common in primary care. Hence, the Patient Health Questionnaire-Somatic, Anxiety, and Depression Symptoms,22 a validated and widely used instrument in primary care that assesses depression, generalized anxiety, somatization, and panic symptoms, was used to evaluate for mental disorders. Given their high prevalence in primary care and the community, the cluster of depression and anxiety disorders is defined as common mental disorders.23
Alcohol Use Disorders Identification Test. The Alcohol Use Disorders Identification Test (AUDIT)24 was used to assess alcohol use. The AUDIT is a 10-item screening instrument developed by the World Health Organization to evaluate alcohol consumption. The AUDIT has been validated for use in primary care. A score of 8 suggesting hazardous alcohol use was used as the cutoff for the study.
Fagerström Test for Nicotine Dependence. The Fagerström Test for Nicotine Dependence25 was used to assess the prevalence and severity of nicotine addiction. This instrument has been widely used and has excellent sensitivity, specificity, and validity in diagnosing nicotine dependence.

- Insomnia is a common concern in elderly primary care patients.
- Elderly patients with insomnia are more likely to have other health issues (physical or psychiatric), hence the need for a comprehensive geriatric assessment.
- Even subclinical insomnia can affect satisfaction with life in elderly primary care patients and thus should be addressed through sleep education and sleep hygiene.
World Health Organization Disability Assessment Schedule. Disability in the previous month due to functional impairment caused by health issues was assessed using the 12-item World Health Organization Disability Assessment Schedule.26
World Health Organization Quality of Life-BREF. Two items from the World Health Organization Quality of Life-BREF were used to briefly evaluate quality and satisfaction with life.27
Statistical Analysis
The statistical analysis was conducted with SPSS version 22 (IBM Inc, Armonk, New York).28 The prevalence of sleep disturbances and various subcategories was calculated. Sociodemographic variables, chronic medical illness, presence of mental disorders, quality of life, satisfaction with life, and disability were compared among subjects with no insomnia, subclinical insomnia, and clinical insomnia using univariate and multivariable binary logistic regression analysis (full model). Each mental disorder was assessed individually in the full model. A score test was conducted to assess the trends of odds across sleep categories. The results were reported as odds ratios and 95% confidence intervals. The tests were 2-tailed, and statistical significance was set at P < .05.
RESULTS
Of the 1,770 subjects invited to participate, 92 (5.2%) did not provide informed consent. The information given by 104 (5.8%) subjects had many missing responses, thus 1,574 (89%) subjects were included in the analysis.
Among the analyzed questionnaires, 774 (55.5%) were from women. The mean age of the subjects was 68.6 years (SD = 6.3 years, median = 67 years, range, 61-97 years). Sleep disturbances in the previous 2 weeks were reported by 665 (42.2%) subjects. Of those, 479 (30.4%) reported subclinical insomnia (ISI subgroups with no clinically significant insomnia [n = 203, 12.9%] and subthreshold insomnia [n = 276, 17.5%] were grouped together). Clinical insomnia was noted in 186 subjects (11.8%) (ISI subgroups of clinical insomnia: moderate [n = 139, 8.8%] and severe [n = 47, 3%] were grouped together). In subjects reporting sleep disturbances, duration of symptoms was > 6 months in 64.3%.
In the univariate analysis, significant differences were found between subjects with no insomnia and those with subclinical and clinical insomnia for all assessed variables except marital status, residence, and years of education (see Supplementary Table 1). When subjects with subclinical insomnia were compared with those with clinical insomnia, differences between living arrangement and employment were not significant (see Supplementary Table 1).
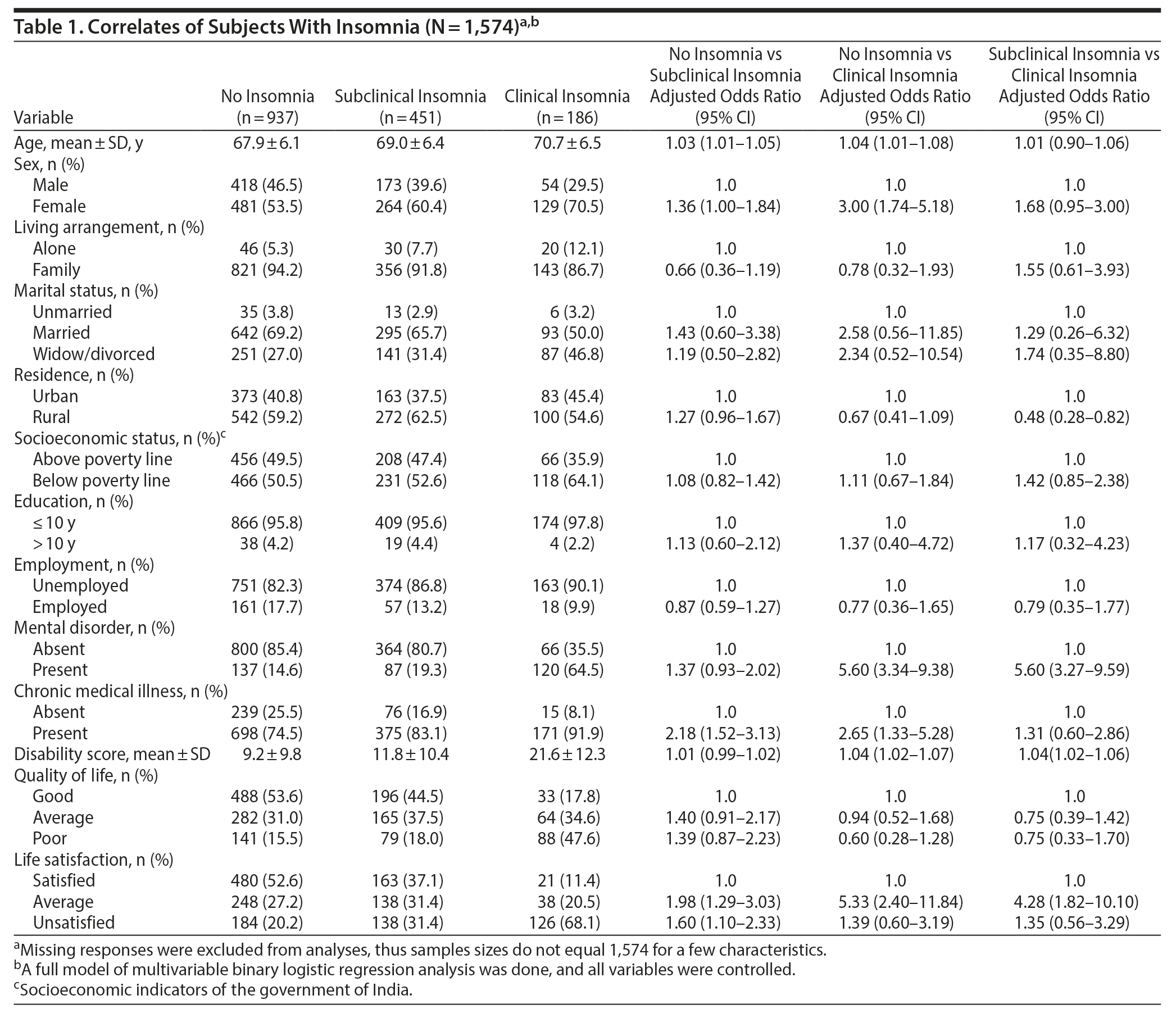
In the full multivariable analysis model, subjects with subclinical insomnia were more likely to be female and older and to have a chronic medical illness and poor life satisfaction compared to those with no insomnia. Those with clinical insomnia had increased odds of being female and older and of having medical and mental disorders and greater disability compared to those without insomnia. Subjects with clinical insomnia were more likely to have mental disorders and greater disability compared to those with subclinical insomnia (Table 1).
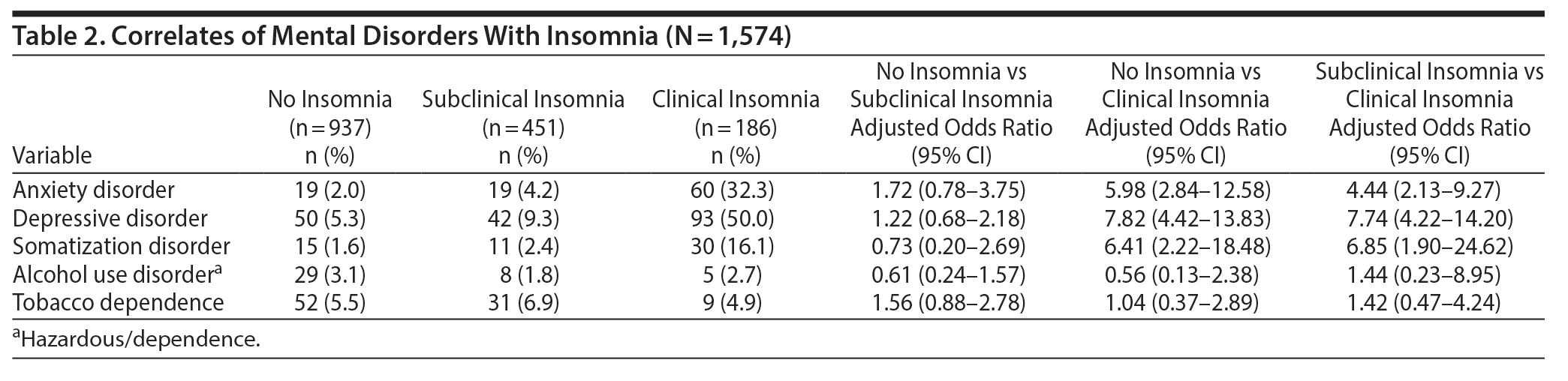
As mental disorders were analyzed individually, subjects with clinical insomnia were more likely to have anxiety, depression, and somatization compared to those with subclinical insomnia or no insomnia. Subjects with subclinical insomnia showed no higher risk for any of the mental disorders assessed in the survey compared to those with no insomnia (Table 2).
Trend analysis was conducted to examine whether there was a stepwise increase in associations over those with no insomnia, subclinical insomnia, or clinical insomnia. The score test showed a significant trend of odds across sleep categories for all assessed variables except place of residence and education.
DISCUSSION
In this study, 42.2% of the elderly primary care attendees reported sleep disturbances, of whom subclinical and clinical insomnia was reported by 30.4% and 11.8%, respectively. Although methodological approaches vary in previous research, including definitions of symptoms, assessment measures, and settings, the findings of our study are comparable with reported rates of 42%-57%.9,10 Further, despite varying sleep habits, climate, and culture, the broad overlap of prevalence rates with research from western Europe and North America suggests cultural universality of insomnia among the elderly population.29
The majority of our subjects with sleep disturbances (64%) had symptoms lasting more than 6 months. This finding replicates that of previous studies,9,30 which reported that insomnia had a chronic course in 40% to 70% of subjects over 1 to 20 years. The high rate of insomnia persistence should be addressed, as in addition to the numerous negative correlates of insomnia detailed earlier, there is initial evidence suggesting that persistent insomnia is correlated with increased mortality risk.31
Our older female subjects had higher risk of insomnia and subclinical insomnia similar to findings of most previous studies.11-13,29 Earlier studies11,13 proposed that aging itself leads to higher prevalence, with older adults having difficulty falling asleep, experiencing mid-sleep awakening, and having reduced sleep efficiencies. But, studies12,32 suggest that insomnia occurs consequent to the physical and mental health comorbidities of aging rather than aging itself. Female sex, as in our study, was previously reported as one of the most frequent demographic associations of insomnia among elderly people,12 although some studies11-13 have reported no association with sex. Although many factors, including depression and social isolation, have been proposed, the underlying mechanisms remain ill-defined. Among elderly subjects in our study, living arrangement, marital status, place of residence, socioeconomic status, education, and employment did not correlate with insomnia. Many of these factors were examined previously with inconsistent findings, suggesting that the expression of insomnia may be mediated by a complex interaction of sociodemographic, medical, and psychological factors, and individual sociodemographic factors may not have independent effects.12,29
Despite that it may not be possible to infer causality given the cross-sectional design of our study, subjects with clinical and subclinical insomnia had multiple negative correlates. Subclinical and clinical insomnia among our subjects was associated with self-reported chronic medical illness. Previous studies33,34 have reported association of insomnia with a range of diseases, including hypertension, cardiac diseases, cancer, neurologic disease, diabetes, asthma, and musculoskeletal pain. Although preliminary findings have shown associations between chronic medical illness and insomnia are mediated by psychological factors,35 in our subjects the association with insomnia and subthreshold insomnia remained robust even after controlling for common mental disorders.
In our subjects, a correlation was found between clinical insomnia, but not subclinical insomnia, and common mental disorders. When individual disorders were assessed separately, anxiety, depression, and somatization correlated only with clinical insomnia, suggesting that sleep disturbances that do not cross the diagnostic threshold may not be indicative of underlying mental disorders. Multiple studies,12,29,36 both prospective and cross-sectional, have reported that insomnia co-occurs with several mental illnesses, typically depression and anxiety. There is also increasing evidence that insomnia shares a bidirectional relationship with mental illness.2,3
Our subjects with clinical insomnia showed significantly higher disability compared to those with subthreshold insomnia and no insomnia, suggesting increasing severity is associated with greater disability. Although no differences with regard to disability were found between subjects with subclinical insomnia and normal sleepers, the subclinical insomnia group did indicate poor satisfaction with life. Similar findings were reported in prior studies.5,37 Multiple studies1,3,5 to date have reported on negative correlates among subjects with clinical insomnia/insomnia syndrome, but our findings suggest that elderly subjects with subsyndromal sleep disturbances may also have negative correlates, albeit to a lesser degree, that need to be addressed.
Studies9,10,38 of insomnia among elderly primary care patients are scarce, and few have examined multiple correlates and large populations. Ours is one of few and possibly the only study from a low- and middle-income country to report comprehensively on the correlates (both physical and mental) and disability experienced by a large sample of elderly primary care patients from a large number of centers.
The current study did have limitations. Assessment of chronic medical illness was by self-report and restricted to a limited number of medical conditions. Single-question evaluation of quality of life and life satisfaction may have been inadequate to evaluate these complex constructs. Many factors such as medications and stressful life events that might be independently related to insomnia were not examined. Our findings among elderly primary care patients from the state of Kerala may not be generalizable to other regions or settings.
Clinical and subclinical insomnia is frequent in elderly subjects receiving primary care in Kerala, India. Also, the association of insomnia with medical and psychiatric illnesses, with increased disability, indicates that it is an important health concern among elderly people. Yet, this common indicator of poor health has little public health priority in low- and middle-income countries like India. Thus, more needs to be done to increase awareness among all stake-holders, including health care personnel, policy makers, and the general population, leading to the adoption of effective measures to help those affected.
Submitted: December 16, 2019; accepted February 5, 2020.
Published online: May 21, 2020.
Potential conflicts of interest: Dr Radhakrishnan received financial support for writing chapters for BMJ Clinical Evidence and BMJ Best Practice. Drs Dahale, Jaisoorya, Manoj, Kumar, Thennarasu, and Varghese and Mr Gokul report no conflicts of interest related to the subject of this article.
Funding/support: Funding for this study was received from the National Health Mission, Kerala, India.
Role of the sponsor: The supporters had no role in the design, analysis, or interpretation of this study or publication of this manuscript.
Acknowledgments: The authors would like to acknowledge the block public relation officers of the National Health Mission, Kerala, India, who were involved in data collection.
Supplementary material: See accompanying pages.
REFERENCES
1. Foley DJ, Monjan A, Simonsick EM, et al. Incidence and remission of insomnia among elderly adults: an epidemiologic study of 6,800 persons over three years. Sleep. 1999;22(suppl 2):S366-S372. PubMed
2. Jansson-Fröjmark M, Lindblom K. A bidirectional relationship between anxiety and depression, and insomnia? a prospective study in the general population. J Psychosom Res. 2008;64(4):443-449. PubMed CrossRef
3. Kim J-M, Stewart R, Kim S-W, et al. Insomnia, depression, and physical disorders in late life: a 2-year longitudinal community study in Koreans. Sleep. 2009;32(9):1221-1228. PubMed CrossRef
4. Brassington GS, King AC, Bliwise DL. Sleep problems as a risk factor for falls in a sample of community-dwelling adults aged 64-99 years. J Am Geriatr Soc. 2000;48(10):1234-1240. PubMed CrossRef
5. Hidalgo JL, Gras CB, Garc×a YD, et al. Functional status in the elderly with insomnia. Qual Life Res. 2007;16(2):279-286. PubMed CrossRef
6. Schubert CR, Cruickshanks KJ, Dalton DS, et al. Prevalence of sleep problems and quality of life in an older population. Sleep. 2002;25(8):889-893. PubMed
7. Kaufmann CN, Canham SL, Mojtabai R, et al. Insomnia and health services utilization in middle-aged and older adults: results from the Health and Retirement Study. J Gerontol A Biol Sci Med Sci. 2013;68(12):1512-1517. PubMed CrossRef
8. Gureje O, Oladeji BD, Abiona T, et al. The natural history of insomnia in the Ibadan study of ageing. Sleep. 2011;34(7):965-973. PubMed CrossRef
9. Hohagen F, Kפppler C, Schramm E, et al. Prevalence of insomnia in elderly general practice attenders and the current treatment modalities. Acta Psychiatr Scand. 1994;90(2):102-108. PubMed CrossRef
10.Patelaros E, Argyriadou S. Investigation of insomnia among the elderly in primary care settings in Greece: the efficient collaboration of GPs and psychiatrists. Primary Care Mental Health. 2004;2(2):115-121.
11.Rediehs MH, Reis JS, Creason NS. Sleep in old age: focus on gender differences. Sleep. 1990;13(5):410-424. PubMed
12.Smagula SF, Stone KL, Fabio A, et al. Risk factors for sleep disturbances in older adults: evidence from prospective studies. Sleep Med Rev. 2016;25:21-30. PubMed CrossRef
13.Unruh ML, Redline S, An MW, et al. Subjective and objective sleep quality and aging in the sleep heart health study. J Am Geriatr Soc. 2008;56(7):1218-1227. PubMed CrossRef
14.Gambhir IS, Chakrabarti SS, Sharma AR, et al. Insomnia in the elderly—a hospital-based study from North India. J Clin Gerontol Geriatr. 2014;5(4):117-121. CrossRef
15.Suri JC. Sen MK, Ojha U, et al. Epidemiology of sleep disorders in the elderly—a questionnaire survey. Indian J Sleep Med. 2009;4(1):12-18. CrossRef
16.Roy S, Bhattacharjee A, Chakraborti C, et al. Prevalence of insomnia in urban population of West Bengal: a community-based cross-sectional study. Int J Med Public Health. 2015;5(4):293-296. CrossRef
17.Leger D, Poursain B. An international survey of insomnia: under-recognition and under-treatment of a polysymptomatic condition. Curr Med Res Opin. 2005;21(11):1785-1792. PubMed CrossRef
18.Government of India, Ministry of Statistics and Programme Implementation, Central Statistics Office. Elderly in India—Profile and Programmes 2016. Government of India, Ministry of Statistics and Programme Implementation website. http://mospi.nic.in/sites/default/files/publication_reports/ElderlyinIndia_2016.pdf. 2016. Accessed November 4, 2019.
19.Census of India 2011. Office of the Registrar General & Census Commissioner, India website. http://censusindia.gov.in/2011-Common/CensusData2011.html. 2011. Accessed October 13, 2019.
20.Jaisoorya TS, Dahale AB, Sunil KG, et al. Insomnia in primary care: a study from India. Sleep Health. 2018;4(1):63-67. PubMed CrossRef
21.Bastien CH, Valliרres A, Morin CM. Validation of the Insomnia Severity Index as an outcome measure for insomnia research. Sleep Med. 2001;2(4):297-307. PubMed CrossRef
22.Kroenke K, Spitzer RL, Williams JBW, et al. The Patient Health Questionnaire Somatic, Anxiety, and Depressive Symptom Scales: a systematic review. Gen Hosp Psychiatry. 2010;32(4):345-359. PubMed CrossRef
23.World Health Organization. Depression and Other Common Mental Disorders: Global Health Estimates. World Health Organization website. https://www.who.int/mental_health/management/depression/prevalence_global_health_estimates/en/. 2017. Accessed October 24, 2019.
24.Saunders JB, Aasland OG, Babor TF, et al. Development of the Alcohol Use Disorders Identification Test (AUDIT): WHO Collaborative Project on Early Detection of Persons with Harmful Alcohol Consumption, II. Addiction. 1993;88(6):791-804. PubMed CrossRef
25.Heatherton TF, Kozlowski LT, Frecker RC, et al. The Fagerström Test for Nicotine Dependence: a revision of the Fagerström Tolerance Questionnaire. Br J Addict. 1991;86(9):1119-1127. PubMed CrossRef
26.Ustün TB, Chatterji S, Kostanjsek N, et al; WHO/NIH Joint Project. Developing the World Health Organization Disability Assessment Schedule 2.0. Bull World Health Organ. 2010;88(11):815-823. PubMed CrossRef
27.Harper A, Power M, Orley J, et al; The WHOQOL Group. Development of the World Health Organization WHOQOL-BREF quality of life assessment. Psychol Med. 1998;28(3):551-558. PubMed CrossRef
28.IBM SPSS statistics for Windows, Version 22.0 [computer program]. Armonk, NY: IBM Corp; 2013.
29.Ohayon MM. Epidemiology of insomnia: what we know and what we still need to learn. Sleep Med Rev. 2002;6(2):97-111. PubMed CrossRef
30.Morphy H, Dunn KM, Lewis M, et al. Epidemiology of insomnia: a longitudinal study in a UK population. Sleep. 2007;30(3):274-280. PubMed
31.Parthasarathy S, Vasquez MM, Halonen M, et al. Persistent insomnia is associated with mortality risk. Am J Med. 2015;128(3):268-75.e2. PubMed CrossRef
32.Vitiello MV, Moe KE, Prinz PN. Sleep complaints cosegregate with illness in older adults: clinical research informed by and informing epidemiological studies of sleep. J Psychosom Res. 2002;53(1):555-559. PubMed CrossRef
33.Sivertsen B, Lallukka T, Salo P, et al. Insomnia as a risk factor for ill health: results from the large population-based prospective HUNT Study in Norway. J Sleep Res. 2014;23(2):124-132. PubMed CrossRef
34.Vgontzas AN, Liao D, Bixler EO, et al. Insomnia with objective short sleep duration is associated with a high risk for hypertension. Sleep. 2009;32(4):491-497. PubMed CrossRef
35.Vgontzas AN, Lin H-M, Papaliaga M, et al. Short sleep duration and obesity: the role of emotional stress and sleep disturbances. Int J Obes. 2008;32(5):801-809. PubMed CrossRef
36.Neckelmann D, Mykletun A, Dahl AA. Chronic insomnia as a risk factor for developing anxiety and depression. Sleep. 2007;30(7):873-880. PubMed CrossRef
37.Simon GE, VonKorff M. Prevalence, burden, and treatment of insomnia in primary care. Am J Psychiatry. 1997;154(10):1417-1423. PubMed CrossRef
38.Morgan K, Clarke D. Risk factors for late-life insomnia in a representative general practice sample. Br J Gen Pract. 1997;47(416):166-169. PubMed
This PDF is free for all visitors!