The Psychiatric Consultation Service at Massachusetts General Hospital sees medical and surgical inpatients with comorbid psychiatric symptoms and conditions. During their twice-weekly rounds, Dr Stern and other members of the Consultation Service discuss diagnosis and management of hospitalized patients with complex medical or surgical problems who also demonstrate psychiatric symptoms or conditions. These discussions have given rise to rounds reports that will prove useful for clinicians practicing at the interface of medicine and psychiatry.

Intrusive-Destructive Behaviors:
Novel Behavioral Presentations of Patients With Co-Occurring Tourette Syndrome, Obsessive-Compulsive Disorder, and Attention-Deficit/Hyperactivity Disorder

LESSONS LEARNED AT THE INTERFACE OF MEDICINE AND PSYCHIATRY
The Psychiatric Consultation Service at Massachusetts General Hospital sees medical and surgical inpatients with comorbid psychiatric symptoms and conditions. During their twice-weekly rounds, Dr Stern and other members of the Consultation Service discuss diagnosis and management of hospitalized patients with complex medical or surgical problems who also demonstrate psychiatric symptoms or conditions. These discussions have given rise to rounds reports that will prove useful for clinicians practicing at the interface of medicine and psychiatry.
Prim Care Companion CNS Disord 2021;23(1):20f02670
To cite: Greenberg E, Petriceks AH, Stern TA. Intrusive-destructive behaviors: novel behavioral presentations of patients with co-occurring Tourette syndrome, obsessive-compulsive disorder, and attention-deficit/hyperactivity disorder. Prim Care Companion CNS Disord. 2021;23(1):20f02670.
To share: https://doi.org/10.4088/PCC.20f02670
© Copyright 2021 Physicians Postgraduate Press, Inc.
aDepartment of Psychiatry, Massachusetts General Hospital, Boston, Massachusetts
bHarvard Medical School, Boston, Massachusetts
*Corresponding author: Erica Greenberg, MD, Department of Psychiatry, Massachusetts General Hospital, Fruit St, Boston, MA 02114 ([email protected]).
Have you ever wondered why people act impulsively or compulsively? Have you ever been unsure whether certain behaviors are under someone’s control? Have you ever been frustrated when seemingly logical strategies to help change behaviors and emotional states are less effective than you had hoped? If you have, then these vignettes and the following discussion may prove useful by providing insights into intrusive-destructive behaviors (IDBs), a newly characterized construct.
Case Vignette 1
A 15-year-old girl with Tourette syndrome (TS), obsessive-compulsive disorder (OCD), and attention-deficit/hyperactivity disorder (ADHD) arrived for an initial visit with a new primary care physician. She had been receiving treatment for these conditions off and on since the age of 8 years and through hard work had managed to reduce the frequency of her obsessive thoughts, compulsive behaviors, and complex motor and vocal tics. However, she described a behavior that had recently begun to interfere with her life. Several months ago, her parents purchased an expensive tablet for her. While reflecting on the value and meaning of this gift, she realized how terrible it would be if she were to break the tablet. Shortly thereafter, she experienced an intrusive image of herself biting and cracking the tablet’s glass cover. Despite (or perhaps because of) her belief that this would be “the worst thing ever,” she became stuck on the image and unable to put it out of her mind. Although she “absolutely” did not want to damage the tablet, the more she tried to push away the image, the more powerful it became—an all-consuming inner tension/turmoil that could only be relieved through biting into and cracking the tablet’s screen. In explaining how it broke, she told her parents that she had accidentally dropped the tablet, and they bought her a new one. The thoughts and behaviors recurred, and she broke 2 additional tablets.
How should her primary care physician understand this new behavior in light of her known (neuro) psychiatric conditions? Is this a tic (as part of TS), a compulsion (as part of OCD), an impulsive behavior (as seen in ADHD), bad behavior, or something else?
Case Vignette 2
An 11-year-old boy, accompanied by his mother, met with his primary care physician. One year ago, he was diagnosed with OCD, adding to his long-standing preexisting diagnoses of TS and ADHD (with executive dysfunction). His primary OCD symptom is “taboo thoughts,” wherein he experiences intrusive images of stabbing his father with a kitchen knife. This thought mortifies him. He now refuses to go in the kitchen because he is worried he will pick up a knife and act out his fear. He has never harmed his father and has no desire to do so. When he experiences these thoughts, they lead to severe fear and anxiety. His mother brought him to the doctor because of “ringing in his ears.” At first, the boy was reluctant to share any information regarding when or how this developed. However, after some coaxing, he described that it came from turning the volume on his headphones all the way to the top until he “feels a pop” in his ears. He states that he does not want to do this, but he feels he needs to. He recently saw a movie where a character’s ear drums burst after being exposed to an extremely loud noise, and this behavior began shortly thereafter. He describes that whenever he begins listening to music with his headphones, he develops an intrusive image of turning the volume to the top and wincing from the pain. Although he tries to resist, he develops a growing sense of intolerable distress and tension and a feeling that if he does not turn the volume to the top, he will “explode/go crazy.” To reduce the internal distress, he acts on the urge and impulsively raises the volume until he feels a pop, which simultaneously relieves the inner tension, but also causes severe pain.
What led this patient to feel like he had to increase the volume to unsafe levels? And how, if at all, can his physician address the problem?
What Are Intrusive-Destructive Behaviors?
In descriptive terms, IDBs occur when one feels simultaneously compelled to and unable to stop oneself from acting out the “worst” or “greatest negative” possible action in a particular situation. IDBs involve combinations of feelings, urges, and actions. Mechanistically, they begin with an intrusive thought-urge that is particular to one’s environment and exquisitely distressing because acting on it would result in negative consequences or problematic outcomes (eg, yelling “fire” in a crowded movie theater). The potential action in mind is often quick or brief in nature, followed by perseveration or inability to shift away from the thought, crowding out other thoughts and becoming the sole focus. Simultaneously, there is a growing sense of inner distress and turmoil associated with resisting that thought-urge. The growing distress builds to a need, or drive, to alleviate that internal tension through impulsively “letting go” and engaging in the behavior. By relieving the intrusive urge, the individual experiences the resulting negative, yet paradoxically satisfying, consequence. The behavior is then inadvertently reinforced by the extent of the negative consequence, such that the greater the magnitude of the effect or reaction, the greater the urge to repeat. Subjectively, individuals with IDBs often report that the behavior must be commensurate with the degree of potential negative impact. For example, an individual with IDBs would not feel satisfied or experience the same relief from whispering “fire” or yelling “water!” in a crowded movie theater as he or she would from yelling “fire!”
The phenomenon of feeling compelled to act out socially inappropriate behavior despite awareness of negative implications was first described in a population of individuals with TS in the early 1990s.1 In seeking to further understand these urges and disinhibition-complex behaviors in those with TS, Kurlan et al2 developed a scale to characterize the presence, features, and impact of non-obscene socially inappropriate (NOSI) behaviors.1 (This is in contrast to coprolalia and copropraxia, which are “obscene” verbalizations and behaviors, respectively.) NOSI behaviors in TS include engaging in socially inappropriate insults, comments, or actions toward family members, familiar individuals, or strangers. In both NOSI behaviors and IDBs, there is an underlying inability to refrain from “deliberately” acting out undesired behaviors. IDBs expand on the concept of NOSI behaviors in that IDBs also include acts directed solely toward the self or self-sabotage behaviors (eg, turning the dial to maximum volume or, as per one patient, tripping oneself when on a breakaway in a soccer match).
Who Is at Risk for Intrusive-Destructive Behaviors? Who Is at Risk for Intrusive Thoughts, Impulsive Behaviors, and Compulsions?
Characterizations of IDBs evolved from working and speaking with children and adolescents who have tic disorders (eg, TS) and associated OCD, ADHD with executive dysfunction, or additional impulsive-compulsive spectrum disorders. Tics are brief, repetitive movements or sounds that are partially suppressible, but only with significant effort on the part of those who experience them.3,4 Tics are often preceded by “premonitory urges” or the sensation of a mounting inner tension that is temporarily relieved by the tic. Suppressing a tic is often compared to holding back a sneeze or a yawn or not scratching an itch. TS is characterized by the presence of more than 1 motor tic and at least 1 vocal tic (not necessarily concurrent) for at least 1 year with onset prior to 18 years of age.3 Tics can be simple (ie, involving 1 muscle group) or complex (ie, involving multiple muscle groups or coordinated movements that appear deliberate) and can be motor or vocal. Some individuals with TS experience “self-harm tics”—complex tics that may involve, for example, punching oneself.
OCD is characterized by the presence of recurrent, intrusive, unwanted, or disturbing thoughts, images, or urges (obsessions) and repetitive behaviors and mental acts (compulsions) aimed at reducing the anxiety and distress associated with those obsessions or according to rigidly applied rules. A subset of individuals with OCD suffer from “aggressive obsessions,” wherein they experience upsetting intrusive thoughts of harming others, often followed by compulsive checking to make sure they have not caused harm.
A TS-OCD hybrid phenomenon is referred to as “Tourettic OCD” (or Tourettic compulsions). These behaviors have elements of both tics and compulsions. Examples include a compulsive-appearing behavior (tapping 3 times) in response to a more tic-like “just-right” premonitory sensation or having a tic-like movement secondary to an intrusive obsessive thought (aptly named a “ticculsion” by one individual).
ADHD is a childhood-onset neuropsychiatric disorder associated with impulsivity in the context of prominent inattention or hyperactivity. Executive functioning refers to the integrative cognitive processes that allow for effective problem-solving in novel situations. About 90% of youth with ADHD demonstrate evidence of executive dysfunction, specifically in the realms of impaired inhibition (disinhibition), working memory, and organization and planning.5,6
IDBs are conceptualized as a hybrid of TS and OCD symptoms atop an overlay of disinhibition (inability to stop, eg, “faulty brakes”) and impulsivity. Impulsivity (reward-seeking), an often prominent symptom in ADHD, is characterized by failing to inhibit behaviors motivated by reward or pleasure. Compulsivity (harm-avoiding), in contrast, is characterized by failing to suppress behaviors aimed to relieve a negative feeling state.7-9
From a biological perspective, there is significant overlap between the genetic factors and neurocircuitry underlying TS, OCD, and ADHD with executive dysfunction and other impulsive-compulsive spectrum conditions (eg, trichotillomania, binge-eating disorder, etc).10-13 In individuals with TS, about half have co-occurring OCD, half have co-occurring ADHD, and one-third have both OCD and ADHD.12,13 Certain individuals with TS, often those with the TS/OCD/ADHD triad, demonstrate a genetic “disinhibition endophenotype,” which is characterized by increased rates of coprophenomena (coprolalia and copropraxia), NOSI behaviors, and obsessive urges to offend or be destructive.14,15 As such, one might expect that IDBs would also be associated with this particular TS phenotype. Further exploration will be important.
- When a child or adolescent presents with new-onset problematic behaviors, which appear to be both simultaneously deliberate and upsetting, clinicians should conduct an assessment for intrusive-destructive behaviors (IDBs).
- A behavioral treatment consideration in IDBs should include reducing the magnitude of the potential negative consequence or reaction to the IDB.
- Pharmacologic management in IDBs may include interventions similar to those used in treating tics and other impulsive-compulsive spectrum disorders, such as α2 agonists, stimulants, serotonergic agents, and dopamine antagonists.
TS, OCD, ADHD, and other impulsive-compulsive spectrum conditions are also all associated with dysregulated cortico-striatal-thalamo-cortical (CSTC) neurocircuitry.16 CSTC circuitry is responsible for the regulation of cognitive, motor, and affective processes.16 When disrupted, one would see dysregulation in cognitive (ADHD/executive functioning), motor (tics), and affective realms (OCD). While there are currently no epidemiologic or neuroimaging studies thus far, we believe that IDBs would be associated with CSTC circuitry dysregulation as well.
Interestingly, when NOSI behaviors were first described in the early 1990s, they were found to be associated with severe TS symptoms (particularly coprophenomena) and impulse control disorders (ie, ADHD and conduct disorder).1 It was not until more recently that increased premonitory urges, as measured by the Premonitory Urge to Tic Scale, were also noted to be more commonly associated with NOSI behaviors.17 As such, one would predict that IDBs are also associated with severe tics, OCD symptoms, ADHD/impulse control disorders, and increased premonitory urges.
Chronic tic disorders (including TS) are believed to affect approximately 2% to 3% of individuals.18 Studies evaluating NOSI phenomena in adults found that up to 60% of individuals with TS experience NOSI urges, and approximately 30% engage in NOSI behaviors.2,19 In studies by Kurlan et al2 and Eddy and Cavanna,19 rates of NOSI behavior tended to decline with age. Therefore, the rates may be even greater in a child/adolescent population.2,19 Eddy and Cavanna19 postulated that increased self-consciousness and increased awareness/intolerance of distress contribute to NOSI behavior. The self-consciousness aspect in particular may be associated with increased rates of IDBs in youth.
When Might These Symptoms Present? What Is the Clinical Course?
TS, childhood-onset OCD, and ADHD are all neurodevelopmental conditions that typically emerge by middle to late childhood or early adolescence.4,20-22 Given the overlap, IDBs are very likely to first present during one’s late childhood or early adolescent years as well. Although TS, OCD, and ADHD symptoms may persist into adulthood, they typically improve through late adolescence and into early adulthood. This improvement may reflect the developmental trajectory of frontostriatal (including CSTC) networks, which continue to develop into early adulthood.23
Regarding the clinical course of TS, OCD, and ADHD, the prognosis is generally positive. Tics tend to improve once one enters late adolescence, pediatric-onset OCD has a moderately favorable prognosis compared to adult-onset OCD, and while ADHD is indeed a chronic condition, certain ADHD symptoms tend to wane as one gets older.24,25 It is possible that IDBs would follow a similar course, with some reduction in rate and severity with age, though this would be an important area of future study.
How Might These Symptoms Present?
Particularly when a patient is not yet working with a psychiatrist, those with IDBs are likely to arrive at a primary care office with their parents or guardian, with all parties voicing concern about certain confusing behaviors. Some time may have elapsed since the behaviors first arose, during which the family may have attempted to understand and address the behaviors. If this is the case, one might expect them to arrive in the clinic emotionally exhausted from weeks and months of uncertainty, seeking answers. Or, they may be seeking a referral to a psychiatrist or other behavioral specialist. Nonetheless, primary care providers should think about IDBs when a child, adolescent, or young adult presents with confusing behaviors in the context of tics, OCD, ADHD, and impulsive or compulsive behavioral disorders.
What Is the Differential Diagnosis for Intrusive-Destructive Behaviors?18,24,26-36
Tic disorders. Tics are classified by their complexity (simple or complex) and form (motor or vocal).3,31 Simple motor tics are characterized by brief contractions of 1 muscle group, most commonly of the eyes, nose, head, or shoulders. Simple vocal tics are similar, but require a brief contraction of pharyngeal, laryngeal, and respiratory muscles to produce sounds, such as sniffing or throat-clearing. Complex tics entail a broader range of motor and vocal phenomena, typically including multiple muscle groups and vocalizations. Complex tics often appear coordinated and purposeful (eg, shoulder shrug and neck jerk simultaneously, speaking specific words in a stereotyped way out of context). Tics are known to wax and wane over time and to jump from location to location. Tics typically increase in frequency and intensity in the setting of certain internal/external-modifying factors (eg, anxiety, boredom, TV watching, homework) and decrease with certain internal/external-modifying factors (eg, intense focus, calmness, playing an instrument, playing a sport).
Beginning at around age 10, individuals commonly report that the tics are preceded by premonitory urges or sensations of a mounting inner tension temporarily relieved by a specific movement or vocalization (the tic). These urges are frequently likened to a bad itch or the feeling before a sneeze. Those with tic disorders often find that they can temporarily suppress the tic (like one might try to suppress a sneeze or a yawn) until the building discomfort of the premonitory urge necessitates release. As such, the phenomena of tics are considered somewhere between voluntary and involuntary, and their suppression may depend on a patient’s level of stress, anxiety, and focus.3 The level of suppression may also depend on one’s “capacity to inhibit” neurophysiologically.37
Tics and IDBs are similarly preceded by uncomfortable premonitory sensations or urges that lead to the specific movements, vocalizations, or behaviors. Both can cause physical harm (eg, complex tics involving punching oneself, poking one’s eyes). Both can also be characterized by a complex sequence of actions, although in IDBs, the behaviors are perhaps even more deliberate appearing—such as biting an expensive glass tablet or turning a dial to increase volume.
While tics and IDBs are both associated with a release of tension or distress, there is a clear distinguishing cognitive element to IDBs, as the behavior follows conscious anxiety about the “worst possible” action in a specific circumstance. In IDBs, it is often the case that the greater the potential negative consequence of the action, the more difficult it is to tolerate the discomfort and suppress the behavior. This contributes to the uniquely situational nature of IDBs. IDBs arise within a given context and therefore manifest most frequently in situations in which the behavior will generate a high negative impact. In contrast, tics are purposeless and arise across a variety of circumstances irrespective of the greater social or contextual impact. If the inciting situation is altered in some way, or never comes about, the IDB may dissipate or not occur in the first place.
Clinicians differentiating between IDBs and complex tics should pay close attention to the patient’s experience prior to, during, and after the behavior. If the behavior demonstrates an obsessive, cognitive component—with intrusive, inappropriate thoughts or ideas leading to anxiety and distress and requiring action to alleviate the discomfort—then it is more likely to be consistent with an IDB. As one might imagine, certain behaviors may involve elements of both complex tics and IDB-specific features. Using coprolalia as an example: coprolalia may worsen in church secondary to increased anxiety around long periods of idle sitting (typical for tics) and because foul language is specifically more prohibited in religious institutions (IDB related). However, differentiating and better understanding the contributions of both may be helpful for treatment-related purposes.
OCD and OCRDs. Categorized in the Diagnostic and Statistical Manual of Mental Disorders, Fifth Edition (DSM-5) as part of the obsessive-compulsive and related disorders (OCRDs) chapter, OCD is diagnosed through the presence of obsessions, compulsions, or both, which are time consuming (at least 1 hour/day) and distressing or interfering with daily functioning.31 Individuals with OCD often have insight, which means that despite knowing that their compulsions (eg, tapping 4 times to prevent an accident from happening) are irrational, they feel compelled to perform them to rid themselves of anxiety, disgust, or “not just rightness.” The compulsions are to ensure that the theoretical bad outcomes of their obsessions do not occur. Additional common features of OCD include difficulty tolerating uncertainty, pervasive doubt, and difficulty trusting one’s experiences (eg, “Did I lock the door?”). Patients will often go to great lengths to try to resolve any doubt or uncertainty, as tolerating it can feel unbearable.
Research has differentiated the most consistent OCD symptom factors into 4 subgroups: (1) symmetry, (2) forbidden thoughts, (3) cleaning/contamination, and (4) hoarding (now a separate diagnosis), which provide an adequate framework for adults as well as children and adolescents.22,38 Symmetry symptoms include obsessions regarding symmetry, evenness, and not just rightness and associated compulsions that often involve repeating, counting, or ordering until it feels “just right.” It is important to note that the symmetry subtype is more associated with co-occurring tic disorders. This coheres with current understandings, given that the not-just-right feeling is often experienced as similar to the premonitory urges in tics. Forbidden thoughts refer to intrusive obsessions of aggressive, religious, sexual, or somatic nature. A common example is having an intrusive thought of stabbing a loved one with a knife. Individuals with this type of OCD find these thoughts extremely disturbing and upsetting. The associated compulsions may include “checking” what they think or feel when in close proximity to knives, repetitively seeking reassurance from a loved one (eg, asking repeatedly “Are you sure I won’ t?”), or sometimes avoiding sharp objects all together.
There are several factors that differentiate IDBs from the forbidden thought OCD subtype. In contrast to IDBs, in forbidden thought OCD, the sufferer does not act on the feared thoughts.39 Additionally, obsessions are not necessarily environmentally context dependent. One with OCD might have more intrusive images about stabbing someone when in close proximity to a knife, but the thoughts will be experienced regardless of the setting. In contrast, in IDBs, the disturbing force of these intrusive thought-urges derives from (in patient terms) “the worst possible thing” one could do in a specific situation. The IDB thoughts arise, to a large degree, because of particular contexts and are given salience by the magnitude of their undesirable effects.
When clinicians are differentiating between OCD symptoms and IDBs, they should inquire into the specific nature of the thoughts and sensations that precede the unwanted behaviors. If a patient describes their compulsive behaviors as self-sabotaging—eg, biting the tablet because of the degree to which it will prevent social networking, be an expensive loss, or upset their parents—it is more consistent with an IDB. If on the other hand they report biting the tablet because they feel if they “don’ t bite on glass, something bad may happen to my family,” that would be more consistent with typical OCD. If individuals experience the need to bite on the glass because when they see glass, they feel an irresistible just-right urge/inner tension that can only be relieved through biting onto it, that would be more consistent with a Tourettic compulsion.
Nonsuicidal self-injury. Because patients with IDB are distinguished, in part, by their specifically self-sabotaging behavior, it is important to distinguish their symptoms from nonsuicidal self-injury (NSSI), which is defined by deliberate, nonsuicidal “destruction of bodily tissue . . . for purposes not socially sanctioned.”40
Several factors differentiate NSSI from IDB, though the 2 are not mutually exclusive. IDBs need not be directed at the patient’s self, and if they are, they need not be physical or specifically injurious. Furthermore, IDBs do not arise from negative feelings or thoughts that may characterize severe mood states or inter/intrapersonal turmoil (more associated with NSSI) but rather from obsessional urges regarding the actions themselves, which then generate anxiety or distress until the actions are performed. Additionally, in IDBs, the action is conceptually ego-dystonic (separate from self), while in NSSI, the actions may be ego-syntonic (consistent with one’s goals) and occur in the context of mood dysregulation.41 Whether there is an independent association between IDBs and specific mood or mood dysregulation disorders is unknown, though at present, the association appears to be more with impulsive-compulsive spectrum disorders.40,42 Table 1 provides an overview of the prevalence, onset, presentation, and prognosis of IDBs and related diagnoses.
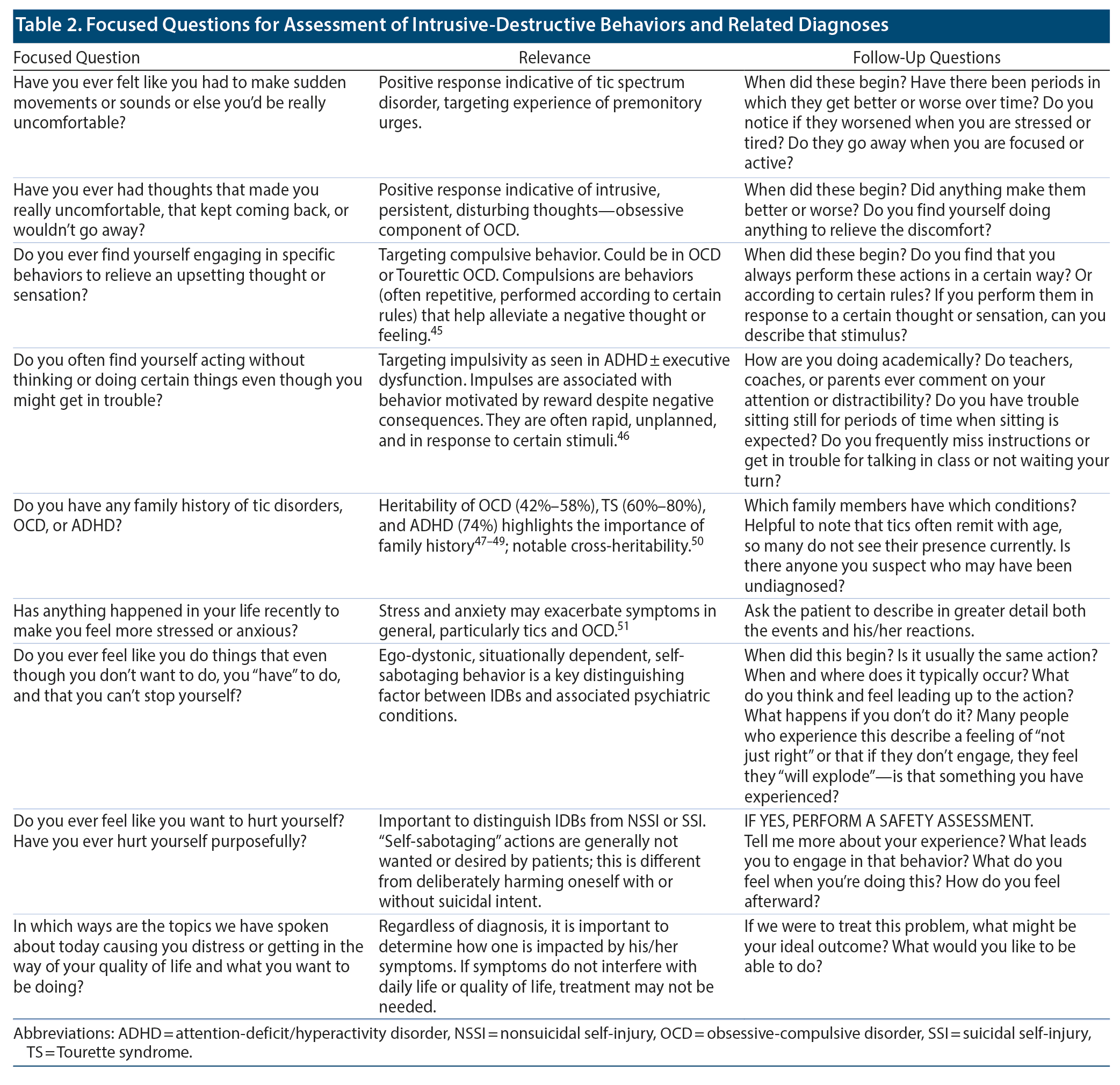
How Do You Assess for Intrusive-Destructive Behaviors?43-48
When a child or adolescent presents with new, confusing, or self-destructive behaviors that appear both deliberate and, at the same time, undesired, clinicians should assess for IDBs. Clinicians should consider this diagnosis especially in those who are known or suspected to have any combination of tics/TS, OCD, or ADHD with executive dysfunction, as well as any other disorders on the impulsive-compulsive spectrum, as thus far that is the population in which IDBs have been observed. Given that IDBs involve a hybrid of tic, OCD, and ADHD/impulsivity symptoms, the clinician should evaluate for those symptoms, as one would not expect to see IDBs without current or previous tic, OCD, or ADHD/impulsivity symptoms.
When assessing the patient, it would be helpful to give examples of defining features of those syndromes, as patients often do not realize that there are tics beyond coprolalia, OCD symptoms beyond excessive hand washing, or ADHD symptoms beyond hyperactivity. Clinicians should also evaluate for recent psychosocial changes (eg, new teacher at school, recent divorce) that may increase stress, and as such, exacerbate symptoms, as well as histories of any other neurologic and neurodevelopmental abnormalities. Given the overlapping genetics and heritability patterns of tics/TS, OCD, and ADHD, it would also be prudent to ask about the family history of those conditions.11,13
While the cause of TS and associated conditions remains unknown, the most likely etiology is a combination of multiple genetic and environmental factors. That said, a very small percentage of individuals are believed to develop TS or OCD secondary to an autoimmune process known as either pediatric autoimmune neuropsychiatric disorder associated with strep (PANDAS) or pediatric acute-onset neuropsychiatric syndrome (PANS).50 Regarding recognizing and treating IDBs, it is extremely unlikely that one would see IDBs independent of the development of other symptoms more clearly associated with PANS/PANDAS, and as such, one does not need to consider PANS/PANDAS when specifically evaluating for or treating IDBs.
When assessing for IDBs, interviews should focus specifically on the content, context, and self-understanding of the patient’s behaviors. Questions could include “Do you ever feel like you have to do things you don’ t want to, but can’ t stop yourself?” and “What do you feel/experience if you don’ t act?” It can be very helpful to try to validate the patient’s experience with statements such as “I work with a number of other individuals who describe what you’ re describing.” Providing specific examples of other IDBs may help patients to better characterize their own experiences, as well as provide validation that they are not alone. Table 2 provides focused questions for assessment of IDBs and related diagnoses.
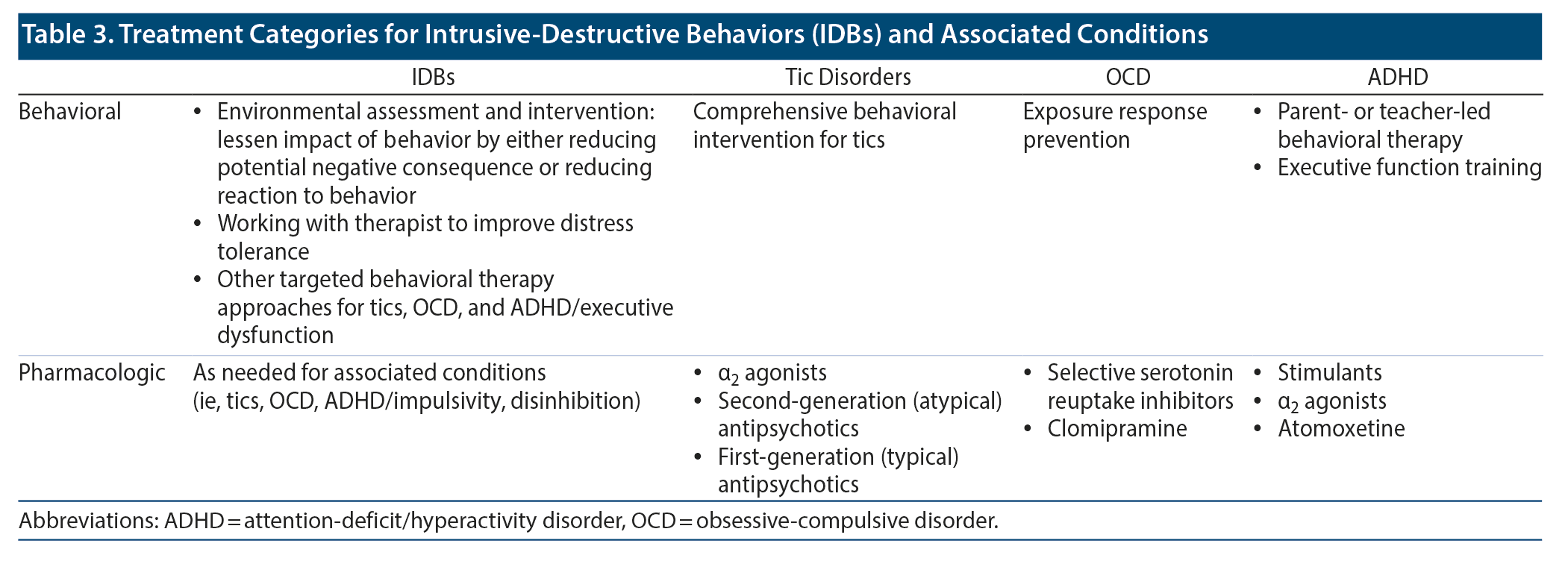
How Do You Treat Intrusive-Destructive Behaviors?
As a broad principle, clinicians should ensure that individuals with IDBs with coexisting tics, OCD, or ADHD are treated for those primary diagnoses. While the full range of treatments for these conditions is beyond the scope of this article, general approaches to each will be described, followed by IDB-specific interventions.
TS treatment is divided into behavioral and pharmacologic modalities. The AAN-recommended first-line behavioral treatment for tics is called comprehensive behavioral intervention for tics (CBIT).50,51 The protocol focuses on habit-reversal training and functional assessment and interventions to reduce exacerbating factors or situations.51 Tics are addressed one at a time, although strategies may generalize as the treatment progresses. Pharmacologic treatment for TS is divided into 3 tiers based on potential benefit and side effects.52 The first tier includes α2 agonists such as guanfacine and clonidine, the second tier includes atypical neuroleptics such as aripiprazole and risperidone, and the third tier includes first-generation antipsychotics such as haloperidol and pimozide.51
Treatment for OCD is also divided into behavioral and pharmacologic interventions. Behavioral treatment is typically composed of exposure and response prevention therapy, a specialized form of cognitive-behavioral therapy (CBT). The most effective pharmacologic treatments for OCD include serotonergic agents, namely selective serotonin reuptake inhibitors (SSRIs) and clomipramine, a highly serotonergic tricyclic antidepressant (TCA).
Stimulants are the treatment of choice in children and adolescents with diagnosed ADHD and associated impulsivity.21,27,53 Children between 6 and 11 years of age should be provided with behavioral therapy and, preferably, US Food and Drug Administration-approved medications such as methylphenidate-based stimulants.21 Adolescents between the ages of 12 and 18 years should be provided with either medications alone or medications alongside behavioral therapy.53 While typically less effective than stimulants, α agonists are also commonly used to treat ADHD symptoms, particularly hyperactivity and impulsivity.
While there is a lack of pharmacologic treatment options that specifically target disinhibition/dysregulation, certain off-label neuroleptic agents, such as lamotrigine, may have some positive benefit on stabilizing behavior and cognition/executive function and could be judiciously considered.54,55
Presently, there are no formal treatments for IDBs. Given that these behaviors are most likely associated with the same dysregulated neurocircuitry and associated neurotransmitters as seen in other CSTC-related conditions, one might hypothesize that IDBs would benefit from the same medication(s) used to target the associated disorders (for example, any combination of stimulants, α agonists, SSRIs, and dopamine antagonists for ADHD, ADHD/tics, OCD, and tics, respectively). Kurlan et al2 similarly hypothesized that medications targeting tics or impulsivity might be beneficial for NOSI behaviors. However, it is prudent to try behavioral treatment strategies first.
The functional assessment/intervention component of CBIT may yield some particularly helpful behavioral strategies. Given that a common trigger of IDBs is the magnitude for potential negative outcome/reaction, one strategy would include modifying the environment to reduce this magnitude. Intriguingly, when the potential negative consequence of the intrusive thought-urges are externally limited, the behaviors often attenuate and ultimately cease as the individual no longer experiences the compulsive urge.
For instance, when the patient who felt intrusive urges to turn the volume all the way up was instructed to wear ear plugs under the headphones (mitigating the potential for physical damage), the behavior abated. When the teen who would bite her tablet was given a much less expensive model, her urges reduced, and the behavior eventually abated. Given that these patients describe having decreased ability to tolerate the inner discomfort when the stakes are felt to be higher, limiting the negative consequences may help reduce the inner tensions and, as such, the behaviors. In another sense, the locus of control is pulled completely outside the patient, perhaps resulting in some relief. (Of note, a goal over time would be to work with a therapist to learn how to better tolerate and cope with distressing feelings and sensations.)
Individuals with IDBs often describe these behaviors as being “quick” or “impulsive” and not fully within their control. Given this, an additional strategy could include adding in an external stop-gap, which gives the patient time to “catch himself/herself” and potentially walk away. An example is giving the patient who bites her tablet a dental device or retainer to wear when using her tablet. While the “magnetic drive” of the IDB may still override the patient’s will to not bite the tablet, this extra step of having to first take the device out of one’s mouth may provide enough distraction to disrupt the IDB and allow for a cognitive shift. One may also try suggesting that the patient do something akin to the behavior, but less destructive (eg, increasing the volume to the half-way point). However, those with IDBs often describe that it simply does not satisfy the urge and that it is those externally imposed boundaries that are most helpful.
Given that the behaviors in IDBs (eg, turning earphones to maximum volume) may lead to medical complications, primary care providers who care for these patients should also assess for additional physical signs and symptoms and, if necessary, refer to proper specialists (eg, otolaryngology).
Finally, because tic disorders, OCD, and ADHD (regardless if co-occurring IDBs) are associated with various learning disorders and worsened academic experience and achievement, practitioners should ask these patients how they are performing academically.56-58 It is often helpful and important to refer to neuropsychological testing and work with the school to ensure the patient receives the appropriate accommodations (eg, 504, individualized education plan) as necessary. Table 3 includes an overview of treatment categories for IDBs and related conditions.
Why Is It Important to Recognize This Disorder?
Like many individuals suffering from TS, OCD, or ADHD, patients with IDBs often experience profound distress not only with the destructive behaviors, but also with the social and interpersonal ramifications. They often describe feelings of shame and remorse, and they are often confused about the nature of their behaviors. As such, they are unlikely to bring these behaviors up despite the detrimental consequences. Beyond the psychosocial discomfort engendered by these behaviors, there is also a genuine danger to the physical health of patients with IDBs and, depending on the behavior, those around them. When characterizing factors associated with NOSI behaviors in a TS population, Eddy and Cavanna19 found that individuals with NOSI behaviors had significantly worse quality of life compared to those without NOSI behaviors. The behaviors not infrequently led to arguments, and in at least a few cases, to legal trouble and physical confrontations.19 Kurlan et al2 were additionally concerned that this was actually a “common manifestation of TS,” most likely with substantial negative functional impact on individuals who experience it. Given the similarity, one would be similarly concerned about those who experience IDBs.
Ultimately, clinicians should be aware of IDBs, including the presentations and risk factors, so that they may more easily identify patients who require more specific interventions. Timely, effective, and creative interventions could provide immense relief for these patients who are weighed down even further by these peculiar and damaging behaviors.
Conclusion
IDBs are characterized by acting in exquisitely undesirable ways in specific environments or situations. An individual experiences an intrusive or unwanted thought-urge (analogous to obsessions in OCD) that, if acted upon, would lead to a particular negative outcome. This thought-urge then becomes increasingly pervasive in their mind, along with a growing sensation of intolerable inner distress (similar to tic-like premonitory urges in TS) often commensurate with the magnitude of the potential negative outcome. Though the true desire is not to act, the individual experiences an inability to tolerate the distress of resisting and inhibiting and often impulsively lets go. This abrupt action resolves any uncertainty about one’s ability to continue resisting and results in a deeply upsetting, albeit temporarily satisfying, outcome. The greater the potential magnitude of negative consequence, the greater the internal distress, and the more difficult it is to resist. IDBs appear to be a symptom hybrid of typically coexisting conditions including TS, OCD, and ADHD with executive dysfunction and are most likely associated with CSTC dysfunction and difficulties with impulsivity, compulsivity, dysregulation, and disinhibition. IDBs are phenomenologically similar to NOSI behaviors but also include a possible self-sabotage component wherein the destructive behavior is directed toward oneself. Following the IDB, patients typically experience remorse, shame, and confusion. Pharmacologic treatments for IDBs should target the underlying associated impulsive-compulsive conditions (eg, TS, OCD, ADHD). Novel and creative behavioral treatment techniques that center around reducing the impact of IDBs may be helpful.
Submitted: May 11, 2020; accepted August 7, 2020.
Published online: January 21, 2021.
Potential conflicts of interest: Dr Stern is an employee of the Academy of Consultation-Liaison Psychiatry (as editor of Psychosomatics). Dr Greenberg and Mr Petriceks report no conflicts of interest related to the subject of this article.
Funding/support: None.
Acknowledgments: The authors thank Mary Colvin, PhD, for her assistance in reviewing and editing this article. Dr Colvin reports no conflicts of interest.
Patient consent: The 2 case vignettes described are a mix of fictional and real accounts. Consent/assent was received from the appropriate parties for the real accounts, and information has been de-identified to protect anonymity.
REFERENCES
1.Cohen AJ, Leckman JF. Sensory phenomena associated with Gilles de la Tourette’s syndrome. J Clin Psychiatry. 1992;53(9):319-323. PubMed
2.Kurlan R, Daragjati C, Como PG, et al. Non-obscene complex socially inappropriate behavior in Tourette’s syndrome. J Neuropsychiatry Clin Neurosci. 1996;8(3):311-317. PubMed CrossRef
3.Swain JE, Leckman JF. Tourette syndrome and tic disorders: overview and practical guide to diagnosis and treatment. Psychiatry (Edgmont). 2005;2(7):26-36. PubMed
4.Diangosing tic disorders. Centers for Disease Control and Prevention. 2019. Accessed February 15, 2020. https://www.cdc.gov/ncbddd/tourette/diagnosis.html
5.Otterman DL, Koopman-Verhoeff ME, White TJ, et al. Executive functioning and neurodevelopmental disorders in early childhood: a prospective population-based study. Child Adolesc Psychiatry Ment Health. 2019;13(1):38. PubMed CrossRef
6.Kofler MJ, Irwin LN, Soto EF, et al. Executive functioning heterogeneity in pediatric ADHD. J Abnorm Child Psychol. 2019;47(2):273-286. PubMed CrossRef
7.Hollander E, Wong CM. Obsessive-compulsive spectrum disorders. J Clin Psychiatry. 1995;56(suppl 4):3-6, discussion 53-55. PubMed
8.Franklin ME, Kratz HE, Freeman JB, et al; Accreditation Task Force of The Canadian Institute for Obsessive Compulsive Disorders. Cognitive-behavioral therapy for pediatric obsessive-compulsive disorder: empirical review and clinical recommendations. Psychiatry Res. 2015;227(1):78-92. PubMed CrossRef
9.Palumbo D, Kurlan R. Complex obsessive compulsive and impulsive symptoms in Tourette’s syndrome. Neuropsychiatr Dis Treat. 2007;3(5):687-693. PubMed
10.Stewart SE, Illmann C, Geller DA, et al. A controlled family study of attention-deficit/hyperactivity disorder and Tourette’s disorder. J Am Acad Child Adolesc Psychiatry. 2006;45(11):1354-1362. PubMed CrossRef
11.Mathews CA, Grados MA. Familiality of Tourette syndrome, obsessive-compulsive disorder, and attention-deficit/hyperactivity disorder: heritability analysis in a large sib-pair sample. J Am Acad Child Adolesc Psychiatry. 2011;50(1):46-54. PubMed CrossRef
12.Hirschtritt ME, Lee PC, Pauls DL, et al; Tourette Syndrome Association International Consortium for Genetics. Lifetime prevalence, age of risk, and genetic relationships of comorbid psychiatric disorders in Tourette syndrome. JAMA Psychiatry. 2015;72(4):325-333. PubMed
13.Hirschtritt ME, Darrow SM, Illmann C, et al. Genetic and phenotypic overlap of specific obsessive-compulsive and attention-deficit/hyperactive subtypes with Tourette syndrome. Psychol Med. 2018;48(2):279-293. PubMed CrossRef
14.Darrow SM, Hirschtritt ME, Davis LK, et al; Tourette Syndrome Association International Consortium for Genetics. Identification of two heritable cross-disorder endophenotypes for tourette syndrome. Am J Psychiatry. 2017;174(4):387-396. PubMed CrossRef
15.Hirschtritt ME, Darrow SM, Illmann C, et al; Tourette Syndrome Association International Consortium for Genetics (TSAICG). Social disinhibition is a heritable subphenotype of tics in Tourette syndrome. Neurology. 2016;87(5):497-504. PubMed CrossRef
16.Jahanshahi M, Obeso I, Rothwell JC, et al. A fronto-striato-subthalamic-pallidal network for goal-directed and habitual inhibition. Nat Rev Neurosci. 2015;16(12):719-732. PubMed CrossRef
17.Reese HE, Scahill L, Peterson AL, et al. The premonitory urge to tic: measurement, characteristics, and correlates in older adolescents and adults. Behav Ther. 2014;45(2):177-186. PubMed CrossRef
18.Scharf JM, Miller LL, Mathews CA, et al. Prevalence of Tourette syndrome and chronic tics in the population-based Avon Longitudinal Study of Parents and Children cohort. J Am Acad Child Adolesc Psychiatry. 2012;51(2):192-201.e5. PubMed CrossRef
19.Eddy CM, Cavanna AE. On being your own worst enemy: an investigation of socially inappropriate symptoms in Tourette syndrome. J Psychiatr Res. 2013;47(9):1259-1263. PubMed CrossRef
20.Wolraich ML, Hagan JF, Allan C, et al. Clinical practice guideline for the diagnosis, evaluation, and treatment of ADHD in children and adolescents. Pediatrics. 2015;144(4):54-54.
21.Sharma A, Couture J. A review of the pathophysiology, etiology, and treatment of attention-deficit hyperactivity disorder (ADHD). Ann Pharmacother. 2014;48(2):209-225. PubMed CrossRef
22.Conelea CA, Walther MR, Freeman JB, et al. Tic-related obsessive-compulsive disorder (OCD): phenomenology and treatment outcome in the Pediatric OCD Treatment Study II. J Am Acad Child Adolesc Psychiatry. 2014;53(12):1308-1316. PubMed CrossRef
23.Arain M, Haque M, Johal L, et al. Maturation of the adolescent brain. Neuropsychiatr Dis Treat. 2013;9:449-461. PubMed
24.Stewart SE, Geller DA, Jenike M, et al. Long-term outcome of pediatric obsessive-compulsive disorder: a meta-analysis and qualitative review of the literature. Acta Psychiatr Scand. 2004;110(1):4-13. PubMed CrossRef
25.Mick E, Faraone S, Biederman J, et al. The course and outcome of attention-deficit/hyperactivity disorder. Prim Psychiatry. 2004;11(7).
26.Knight T, Steeves T, Day L, et al. Prevalence of tic disorders: a systematic review and meta-analysis. Pediatr Neurol. 2012;47(2):77-90. PubMed CrossRef
27.Pliszka S; AACAP Work Group on Quality Issues. Practice parameter for the assessment and treatment of children and adolescents with attention-deficit/hyperactivity disorder. J Am Acad Child Adolesc Psychiatry. 2007;46(7):894-921. PubMed CrossRef
28.Klonsky ED, Victor SE, Saffer BY. Nonsuicidal self-injury: what we know, and what we need to know. Can J Psychiatry. 2014;59(11):565-568. PubMed CrossRef
29.Leckman JF, Zhang H, Vitale A, et al. Course of tic severity in Tourette syndrome: the first two decades. Pediatrics. 1998;102(1 pt 1):14-19. PubMed CrossRef
30.Taylor S. Early versus late onset obsessive-compulsive disorder: evidence for distinct subtypes. Clin Psychol Rev. 2011;31(7):1083-1100. PubMed CrossRef
31.Franklin ME, Harrison JP, Benavides KL. Obsessive-compulsive and tic-related disorders. Child Adolesc Psychiatr Clin N Am. 2012;21(3):555-571. PubMed CrossRef
32.Visser SN, Danielson ML, Bitsko RH, et al. Trends in the parent-report of health care provider-diagnosed and medicated attention-deficit/hyperactivity disorder: United States, 2003-2011. J Am Acad Child Adolesc Psychiatry. 2014;53(1):34-46.e2. PubMed CrossRef
33.Cipriano A, Cella S, Cotrufo P. Nonsuicidal self-injury: a systematic review. Front Psychol. 2017;8:1946. PubMed CrossRef
34.Bloch MH, Leckman JF. Clinical course of Tourette syndrome. J Psychosom Res. 2009;67(6):497-501. PubMed CrossRef
35.Barbaresi WJ, Colligan RC, Weaver AL, et al. Mortality, ADHD, and psychosocial adversity in adults with childhood ADHD: a prospective study. Pediatrics. 2013;131(4):637-644. PubMed CrossRef
36.Turner BJ, Austin SB, Chapman AL. Treating nonsuicidal self-injury: a systematic review of psychological and pharmacological interventions. Can J Psychiatry. 2014;59(11):576-585. PubMed CrossRef
37.Greenberg E, Essa A, Scharf JM. Tricky “ticcy” case: tics/tourette syndrome with co-occuring OCD. In: Hauptman AJ, Salpekar JA, eds. Pediatric Neuropsychiatry. Cham, Switzerland: Springer; 2019.
38.Bloch MH, Landeros-Weisenberger A, Rosario MC, et al. Meta-analysis of the symptom structure of obsessive-compulsive disorder. Am J Psychiatry. 2008;165(12):1532-1542. PubMed CrossRef
39.Veale D, Freeston M, Krebs G, et al. Risk assessment and management in obsessive-compulsive disorder. Adv Psychiatr Treat. 2009;15(5):332-343. CrossRef
40.Zetterqvist M. The DSM-5 diagnosis of nonsuicidal self-injury disorder: a review of the empirical literature. Child Adolesc Psychiatry Ment Health. 2015;9(1):31. PubMed CrossRef
41.Glenn CR, Klonsky ED. Nonsuicidal self-injury disorder: an empirical investigation in adolescent psychiatric patients. J Clin Child Adolesc Psychol. 2013;42(4):496-507. PubMed CrossRef
42.Gratz KL, Dixon-Gordon KL, Chapman AL, et al. Diagnosis and characterization of DSM-5 nonsuicidal self-injury disorder using the Clinician-Administered Nonsuicidal Self-Injury Disorder Index. Assessment. 2015;22(5):527-539. PubMed CrossRef
43.Grant JE, Potenza MN. Compulsive aspects of impulse-control disorders. Psychiatr Clin North Am. 2006;29(2):539-551, x. PubMed CrossRef
44.Moeller FG, Barratt ES, Dougherty DM, et al. Psychiatric aspects of impulsivity. Am J Psychiatry. 2001;158(11):1783-1793. PubMed CrossRef
45.Faraone SV, Larsson H. Genetics of attention deficit hyperactivity disorder. Mol Psychiatry. 2019;24(4):562-575. PubMed CrossRef
46.Pauls DL, Fernandez TV, Mathews CA, et al. The inheritance of Tourette disorder: a review. J Obsessive Compuls Relat Disord. 2014;3(4):380-385. PubMed CrossRef
47.Hudziak JJ, Van Beijsterveldt CEM, Althoff RR, et al. Genetic and environmental contributions to the Child Behavior Checklist Obsessive-Compulsive Scale: a cross-cultural twin study. Arch Gen Psychiatry. 2004;61(6):608-616. PubMed CrossRef
48.Lin H, Katsovich L, Ghebremichael M, et al. Psychosocial stress predicts future symptom severities in children and adolescents with Tourette syndrome and/or obsessive-compulsive disorder. J Child Psychol Psychiatry. 2007;48(2):157-166. PubMed CrossRef
49.Spinello C, Laviola G, Macrì S. Pediatric autoimmune disorders associated with streptococcal infections and Tourette’s Syndrome in preclinical studies. Front Neurosci. 2016;10:310. PubMed CrossRef
50.Piacentini J, Woods DW, Scahill L, et al. Behavior therapy for children with Tourette disorder: a randomized controlled trial. JAMA. 2010;303(19):1929-1937. PubMed CrossRef
51.Pringsheim T, Okun MS, Müller-Vahl K, et al. Practice guideline recommendations summary: treatment of tics in people with Tourette syndrome and chronic tic disorders. Neurology. 2019;92(19):896-906. PubMed CrossRef
52.McNaught KSP, Mink JW. Advances in understanding and treatment of Tourette syndrome. Nat Rev Neurol. 2011;7(12):667-676. PubMed CrossRef
53.Wolraich M, Brown L, Brown RT, et al; Subcommittee on Attention-Deficit/Hyperactivity Disorder; Steering Committee on Quality Improvement and Management. ADHD: clinical practice guideline for the diagnosis, evaluation, and treatment of attention-deficit/hyperactivity disorder in children and adolescents. Pediatrics. 2011;128(5):1007-1022. PubMed CrossRef
54.Boylan LS, Devinsky O, Barry JJ, et al. Psychiatric uses of antiepileptic treatments. Epilepsy Behav. 2002;3(5S):54-59. PubMed CrossRef
55.Meador KJ, Baker GA. Behavioral and cognitive effects of lamotrigine. J Child Neurol. 1997;12(suppl 1):S44-S47. PubMed CrossRef
56.Piacentini J, Bergman RL, Keller M, et al. Functional impairment in children and adolescents with obsessive-compulsive disorder. J Child Adolesc Psychopharmacol. 2003;13(suppl 1):S61-S69. PubMed CrossRef
57.Claussen AH, Bitsko RH, Holbrook JR, et al. Impact of Tourette syndrome on school measures in a nationally representative sample. J Dev Behav Pediatr. 2018;39(4):335-342. PubMed CrossRef
58.Loe IM, Feldman HM. Academic and educational outcomes of children with ADHD. J Pediatr Psychol. 2007;32(6):643-654. PubMed CrossRef
This PDF is free for all visitors!