Prim Care Companion CNS Disord 2021;23(3):20l02811
To cite: Bhatt K, Yoo J, Bridges A. Ketamine-induced manic episode. Prim Care Companion CNS Disord. 2021;23(3):20l0811.
To share: https://doi.org/10.4088/PCC.20l02811
© Copyright 2021 Physicians Postgraduate Press, Inc.
aKeck School of Medicine of USC, Los Angeles, California
bLAC+USC Medical Center, Department of Psychiatry, Los Angeles, California
*Corresponding author: Amber Bridges, MD, LAC+USC Medical Center Department of Psychiatry, Augustus Hawkins Mental Health Center, 1720 E 120th St, Los Angeles, CA 90059 ([email protected]).
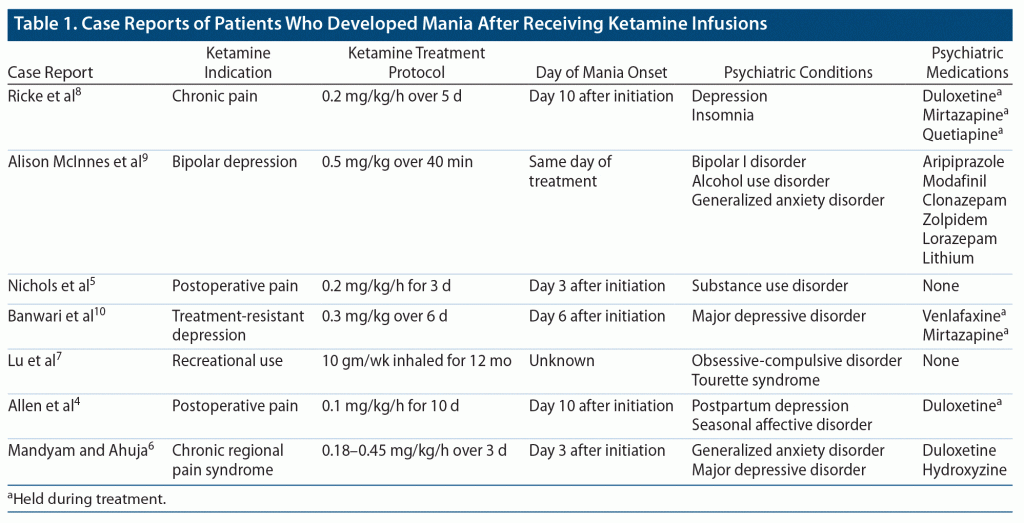
Ketamine has emerged as a promising treatment for patients with unipolar and bipolar depression, particularly for those with acute suicidality.1–3 However, there may be a rare, serious side effect. Currently, there are 7 case reports4–10 of individuals who developed mania after receiving ketamine infusions. These cases include patients who received ketamine in both inpatient and outpatient settings at subanesthetic and anesthetic doses and one who used ketamine recreationally4–10 (Table 1). Here, we report a case of a patient who received ketamine infusions, resulting in induction of a manic episode.
Case Report
Mr A is a 23-year-old White man (weight: 154 lb) with a history of polysubstance abuse, bipolar I disorder, and posttraumatic stress disorder (PTSD) who was admitted to the psychiatric hospital for a manic episode with psychotic features. Approximately 5 weeks before admission, a provider recommended ketamine to treat his bipolar depression and PTSD. Mr A received 6 ketamine infusions over 14 days at 0.5 mg/kg. He reported undergoing full psychiatric evaluation before his first infusion but was not reevaluated before subsequent infusions. He was not taking a mood stabilizer or other psychotropic medications at that time.
Mr A reported that his depressive symptoms, specifically hopelessness and agitation, immediately improved after his first ketamine infusion. His mood became increasingly elevated with subsequent infusions. By the final infusion, Mr A felt he had “reached a euphoric state.” He developed grandiose delusions and reckless behavior leading to a 5-day inpatient psychiatric hospitalization. He was discharged with oral olanzapine, which he never took.
Over the next 3 weeks, Mr A continued to decompensate with escalating recklessness and impulsive behaviors, including a sudden trip across the country, risky sex, excessive spending, and drug use that likely exacerbated his mania. He did not report or display cognitive impairment. He was hospitalized again with a diagnosis of bipolar mania with psychotic features and was stabilized on lithium 1,200 mg per day and aripiprazole 15 mg per day, achieving full remission after 3 weeks. Mr A did not to develop recurrence of depressive symptoms after stabilization. It is important to note that other factors, particularly drug use, may have contributed to this patient’s mania. However, the timeline of events suggests that ketamine infusions triggered the onset of manic symptoms, which secondarily led to drug use and other risky behaviors.
Discussion
Although research1,2 indicates that ketamine is effective in treating bipolar depression and associated suicidality, there are few data about the risk of inducing mania. Of note, participants in these studies were maintained on mood-stabilizing medications during ketamine treatment, which may have played a protective role against manic induction.
This case shares important commonalities with other case reports that may be valuable in identifying patients at risk for ketamine-induced mania. First, in previous case reports,4–10 patients had documented histories of 1 or more psychiatric illnesses. Given that bipolar disorder can present with a variety of clinical features, these patients may have had atypical presentations that were misdiagnosed as different psychiatric conditions or presentations that were masked by more salient features of comorbid psychiatric diagnoses. Second, apart from 1 case report,9 no patient was known to be taking mood stabilizers at the time of manic induction. As mentioned previously, mood stabilizers may be protective against ketamine-induced mania. Thus, multiple psychiatric illnesses and lack of mood stabilizers may be risk factors for ketamine-induced mania.
This is the eighth documented case report, to our knowledge, demonstrating the potential for ketamine-induced mania. Further studies are needed to explore the phenomenon of ketamine-induced mania. Therefore, we recommend that treatment with ketamine be used with caution and the understanding that mania is a possible outcome when administered for psychiatric or medical therapy.
Published online: May 13, 2021.
Potential conflicts of interest: None.
Funding/support: None.
Patient consent: Verbal consent was obtained from the patient to publish this case report, and all personal identifiers were removed to protect patient anonymity.
References (10)

- Zarate CA Jr, Brutsche NE, Ibrahim L, et al. Replication of ketamine’s antidepressant efficacy in bipolar depression: a randomized controlled add-on trial. Biol Psychiatry. 2012;71(11):939–946. PubMed CrossRef
- Vande Voort JL, Ballard ED, Luckenbaugh DA, et al. Antisuicidal response following ketamine infusion is associated with decreased nighttime wakefulness in major depressive disorder and bipolar disorder. J Clin Psychiatry. 2017;78(8):1068–1074. PubMed CrossRef
- Kraus C, Rabl U, Vanicek T, et al. Administration of ketamine for unipolar and bipolar depression. Int J Psychiatry Clin Pract. 2017;21(1):2–12. PubMed CrossRef
- Allen ND, Rodysill BR, Bostwick JM. A report of affective switching associated with ketamine: the case of ketamine-induced mania is not closed. Bipolar Disord. 2019;21(2):176–178. PubMed CrossRef
- Nichols SD, Bulman M, Tisher A, et al. A case of possible iatrogenic ketamine-induced mania in a patient being treated for postoperative pain. Psychosomatics. 2016;57(5):543–546. PubMed CrossRef
- Mandyam MC, Ahuja NK. Ketamine-induced mania during treatment for complex regional pain syndrome. Pain Med. 2017;18(10):2040–2041. PubMed CrossRef
- Lu YY, Lin CH, Lane HY. Mania following ketamine abuse. Neuropsychiatr Dis Treat. 2016;12:237–239. PubMed
- Ricke AK, Snook RJ, Anand A. Induction of prolonged mania during ketamine therapy for reflex sympathetic dystrophy. Biol Psychiatry. 2011;70(4):e13–e14. PubMed CrossRef
- Alison McInnes L, James-Myers MB, Turner MS. Possible affective switch associated with intravenous ketamine treatment in a patient with bipolar I disorder. Biol Psychiatry. 2016;79(9):e71–e72. PubMed CrossRef
- Banwari G, Desai P, Patidar P. Ketamine-induced affective switch in a patient with treatment-resistant depression. Indian J Pharmacol. 2015;47(4):454–455. PubMed CrossRef
Enjoy this premium PDF as part of your membership benefits!