Objective: Long-acting injectable (LAI) antipsychotic medications are employed universally for the treatment of schizophrenia. This study retrospectively assessed the variables that factor into an individual’s adherence to LAIs.
Methods: The data sample was obtained from the adult ambulatory services of a large general hospital mental health center located in Elizabeth, New Jersey. Reports were run in November 2015 to identify patients who had received at least 1 LAI between January 1, 2014, and October 14, 2015. In September 2016, an additional report was run to collect follow-up data. The sample included 120 women and 178 men, ranging in age from 18-81 years, who received at least 1 LAI during a 23-month period. A hazard analysis for single-decrement, nonrepeatable events was used to assess the risk of discontinuation of LAIs during the study period. Separate χ2 analyses were conducted to assess differences in discontinuation rates for sociodemographic variables, program type variables, type of long-acting medication, and time effects.
Results: The cumulative continuation rate across the study period was 73%. Main effect differences were found in continuation rates for program type (χ22 = 10.252, P = .006), LAI type (χ25 = 23.365, P < .000), and prescribed frequency of LAI (χ22 = 7.622, P = .022). In addition, multiple time-dependent effect differences were found. No significant main effect results were found for LAI continuation rates and patient age (χ23 = 3.689, P = .297), sex (χ21 = 0.904, P = .342), race (χ23 = 5.785, P = .123), or enrollment in involuntary outpatient commitment (χ21 = 2.989, P = .084).
Conclusions: The findings of the current research suggest that medication type, frequency of medication appointments, and program type may be key in increasing and maintaining LAI adherence.

CME Background
Articles are selected for credit designation based on an assessment of the educational needs of CME participants, with the purpose of providing readers with a curriculum of CME articles on a variety of topics throughout each volume. Activities are planned using a process that links identified needs with desired results.
To obtain credit, read the article, correctly answer the questions in the Posttest, and complete the Evaluation.
CME Objective
After studying this article, you should be able to:
‘ ¢ Find ways to support medication adherence for patients with schizophrenia
Accreditation Statement
The CME Institute of Physicians Postgraduate Press, Inc., is accredited by the Accreditation Council for Continuing Medical Education to provide continuing medical education for physicians.
Credit Designation
The CME Institute of Physicians Postgraduate Press, Inc., designates this journal-based CME activity for a maximum of 1.0 AMA PRA Category 1 Creditâ„¢. Physicians should claim only the credit commensurate with the extent of their participation in the activity.
Note: The American Academy of Physician Assistants (AAPA) accepts certificates of participation for educational activities certified for AMA PRA Category 1 Creditâ„¢ from organizations accredited by ACCME or a recognized state medical society. Physician assistants may receive a maximum of 1.0 hour of Category I credit for completing this program.
Date of Original Release/Review
This educational activity is eligible for AMA PRA Category 1 Creditâ„¢ through February 28, 2019. The latest review of this material was February 2017.
Financial Disclosure
All individuals in a position to influence the content of this activity were asked to complete a statement regarding all relevant personal financial relationships between themselves or their spouse/partner and any commercial interest. The CME Institute has resolved any conflicts of interest that were identified. In the past year, Larry Culpepper, MD, MPH, Editor in Chief, has been a consultant for Allergan, Ironshore, Lundbeck, Shire, and Sunovion; has been a stock shareholder of M-3 Information; and has received royalties from UpToDate and Oxford University Press. No member of the CME Institute staff reported any relevant personal financial relationships. Faculty financial disclosure appears at the end of the article.
Long-Acting Injectable Antipsychotics for Schizophrenia:
Sociodemographic Characteristics and Treatment Adherence
ABSTRACT
Objective: Long-acting injectable (LAI) antipsychotic medications are employed universally for the treatment of schizophrenia. This study retrospectively assessed the variables that factor into an individual’s adherence to LAIs.
Methods: The data sample was obtained from the adult ambulatory services of a large general hospital mental health center located in Elizabeth, New Jersey. Reports were run in November 2015 to identify patients who had received at least 1 LAI between January 1, 2014, and October 14, 2015. In September 2016, an additional report was run to collect follow-up data. The sample included 120 women and 178 men, ranging in age from 18-81 years, who received at least 1 LAI during a 23-month period. A hazard analysis for single-decrement, nonrepeatable events was used to assess the risk of discontinuation of LAIs during the study period. Separate χ2 analyses were conducted to assess differences in discontinuation rates for sociodemographic variables, program type variables, type of long-acting medication, and time effects.
Results: The cumulative continuation rate across the study period was 73%. Main effect differences were found in continuation rates for program type (χ22 = 10.252, P = .006), LAI type (χ25 = 23.365, P < .000), and prescribed frequency of LAI (χ22 = 7.622, P = .022). In addition, multiple time-dependent effect differences were found. No significant main effect results were found for LAI continuation rates and patient age (χ23 = 3.689, P = .297), sex (χ21 = 0.904, P = .342), race (χ23 = 5.785, P = .123), or enrollment in involuntary outpatient commitment (χ21 = 2.989, P = .084).
Conclusions: The findings of the current research suggest that medication type, frequency of medication appointments, and program type may be key in increasing and maintaining LAI adherence.
Prim Care Companion CNS Disord 2017;19(1):16m02005
https://doi.org/10.4088/PCC.16m02005
© Copyright 2017 Physicians Postgraduate Press, Inc.
aDepartment of Psychiatry and Behavioral Health, bAdult Outpatient Unit, cPsychiatry Residency Program, and dDepartment of Psychology, Trinitas Regional Medical Center, Elizabeth, New Jersey
ePsychiatry Residency Program, Seton Hall University, South Orange, New Jersey
fSchool of Medicine, Saint George’s University, Grenada, West Indies
*Corresponding author: Essie Larson, PhD, 654 E. Jersey St, Elizabeth, NJ 07206 ([email protected]).
Long-acting injectable (LAI) antipsychotic medications for the treatment of schizophrenia have been described as one of the most potentially useful strategies for enhancing adherence1 and being “highly efficacious,”2(p1263) “an attractive treatment option,”3(p1249) and “an important advance in the treatment of schizophrenia.”4(p1003) Two of a number of primary advantages reported in the literature for LAIs are verifiable medication delivery and immediate recognition of medication nonadherence,5 which are both significant problems in treating schizophrenia.6 Yet, utilization remains low.2
LAIs are said to have an image problem complicated by the tendency to use LAIs as a last resort.7 While anecdotal explanations point to patient resistance to accepting LAIs, prescriber hesitation7 and ambivalence8 are viewed as contributing to the low utilization. The utilization of LAIs needs to be understood in actual practice without the biases inherent in patient clinical trials. For reasons not clearly understood, many patients with schizophrenia are not offered the option of an LAI until after several relapses when a chronic course is unlikely to be reversed.2
Limited data are available on the sociodemographic characteristics or service utilization patterns of LAI continuers or discontinuers. A longer duration of previous antipsychotic medication treatment years (10.5) was associated with discontinuation of an LAI for patients with schizophrenia.9 Age was not associated with continuation in 2 studies10,11 or being prescribed an LAI,12 but older patients were associated with continuation in other studies.13-16 Sex was not associated with being prescribed an LAI12 or continuing on an LAI,10 but males were associated with continuation in another study.16 Racial minorities were found more likely to be prescribed an LAI than nonminority patients.12 In reference to program status, outpatient status was associated with continuing on an LAI in 2 studies.11,13 Continuing on an LAI was associated with inpatient status in 1 study16 and with an outpatient compulsory treatment program in another.11
The purpose of the current research is to retrospectively assess the role of several sociodemographic variables, type of long-acting medication, and program type in LAI adherence. The study sought to test variables related to continuation of LAI treatment in an effort to identify LAI consumers who are more likely to continue taking an LAI as well as to identify needed services and supports to enhance adherence rates. Furthermore, salient variables related to continuation may assist providers in making the decision of when and if a patient is a candidate for an LAI.
METHODS
Setting
Trinitas Regional Medical Center (TRMC) operates a large comprehensive community mental health center in Elizabeth, New Jersey. The adult ambulatory services are located across the street from the acute psychiatric emergency and psychiatric inpatient services. Elizabeth is a low-income and ethnically diverse (Hispanic: 59.5%, black: 21.1%, and white: 18.2%) community. Clinic patients are primarily unemployed and on supplemental security income/social security disability (Medicaid, Medicare, or both), with no more than a high school education. Approximately 10% are undocumented aliens. Clinic patients are predominately from Elizabeth and surrounding communities.
Data
The current research used data gathered from TRMC’s electronic medical record (EMR) system. Reports were run in November 2015 to identify patients who had received at least 1 LAI between January 1, 2014, and October 14, 2015. In September 2016, an additional report was run to collect follow-up data. At the time of the initial EMR report, a sample of 300 patients aged ≥ 18 years was identified. For each of the identified patients, demographic data (ie, age, sex, race) and information on clinical services received during the study period (ie, program type, involuntary outpatient commitment [IOC] status, date of first LAI given during the study period, total number of injections received during the study period, and LAIs used) were collected. When the final EMR report was run, additional data were collected on the date each identified patient received their last injection and the date of last mental health clinical contact for services of any kind with TRMC. The resulting data set identified LAI discontinuers and continuers.
Dependent Variables
Time. The 23-month study period was subdivided into six 3-month intervals: 0-3, 4-7, 8-11, 12-15, 16-19, and 20-23 months.

- Long-acting injectable (LAI) antipsychotics should not be the last resort for treating schizophrenia.
- Many patients are adherent with LAIs when treated at an outpatient level of care.
- Current research suggests that patients are more adherent with LAIs dosed monthly compared to twice a month.
Adherence. Adherence was assessed in terms of continuation and discontinuation of LAIs. An LAI discontinuer is defined as any patient who received no additional injections at TRMC after October 14, 2015.
Independent Variables
Sex. Patients were divided into male and female subgroups.
Age. Patients were divided into 4 subgroups on the basis of their age at the time of the initial EMR report: 18-30, 31-45, 46-60, and > 61 years.
Race: Patients were categorized into 4 groups: white, black, Hispanic, and other.
IOC participation. Patients were categorized into 2 groups: those who were involved in the IOC services at any point during the 23-month study period and those who were not.
Program type. Patients were categorized into 3 mutually exclusive groups: adult outpatient unit, higher level of care, and multiple. Patients in the adult outpatient unit group received only traditional ambulatory outpatient services (ie, medication management, weekly group therapy, occasional individual therapy) during the time they were receiving LAI injections. The adult outpatient unit is a psychiatric unit and does not treat patients with substance use as a primary diagnosis. Patients in the higher level of care group received only more intensive ambulatory services (ie, acute partial hospital, co-occurring partial hospital, substance abuse partial care, and treatment linkage and coordination partial care) during the time they were receiving LAI injections. Patients in the multiple levels of care group received traditional ambulatory outpatient services and more intensive ambulatory services, often switching back and forth, during the time they were receiving LAI injections.
LAI type. All patients were categorized into 6 mutually exclusive groups on the basis of LAI(s) they received during the entire length of the study period: haloperidol, risperidone, fluphenazine, paliperidone palmitate, aripiprazole, and multiple. The last category included all patients who received more than 1 type of LAI during the study period.
Prescribed frequency of LAI. Patients were categorized into 3 mutually exclusive groups on the basis of the prescribed frequency of the LAI: twice a month, monthly, and multiple. Individuals who were prescribed risperidone, fluphenazine, or biweekly haloperidol were in the biweekly group. Patients who received monthly haloperidol, paliperidone palmitate, and aripiprazole were in the monthly group. The multiple category included all patients who received more than 1 type of LAI during the study period.
Sample
After a visual review of the data on the initial 300 patients, 2 patients were removed from statistical analysis because they were the only patients who received an olanzapine injection for the full length of the study. The final analyzed sample of 298 included 120 women and 178 men, ranging in age from 18 to 81 years (mean [SD] = 43 [14.917] years). Age distribution was positively skewed (0.26) and negatively kurtotic (-0.88). Breakdown by patient-identified racial group was 43.0% white, 48.3% black, 3.7% Hispanic, and 5.0% other. Of the 298 patients, 115 discontinued receiving LAIs at some point during the 23-month study period. Of the 115 who discontinued, 54 continued receiving services at TRMC after the 23-month study period. The remaining 61 were right censored due to lost contact.
Statistics Used
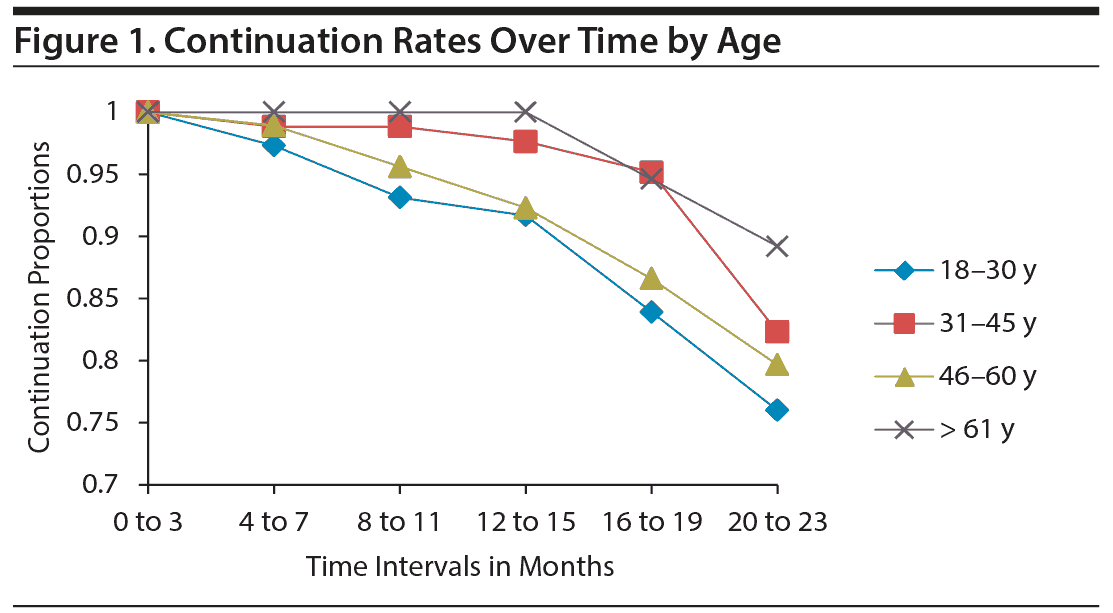
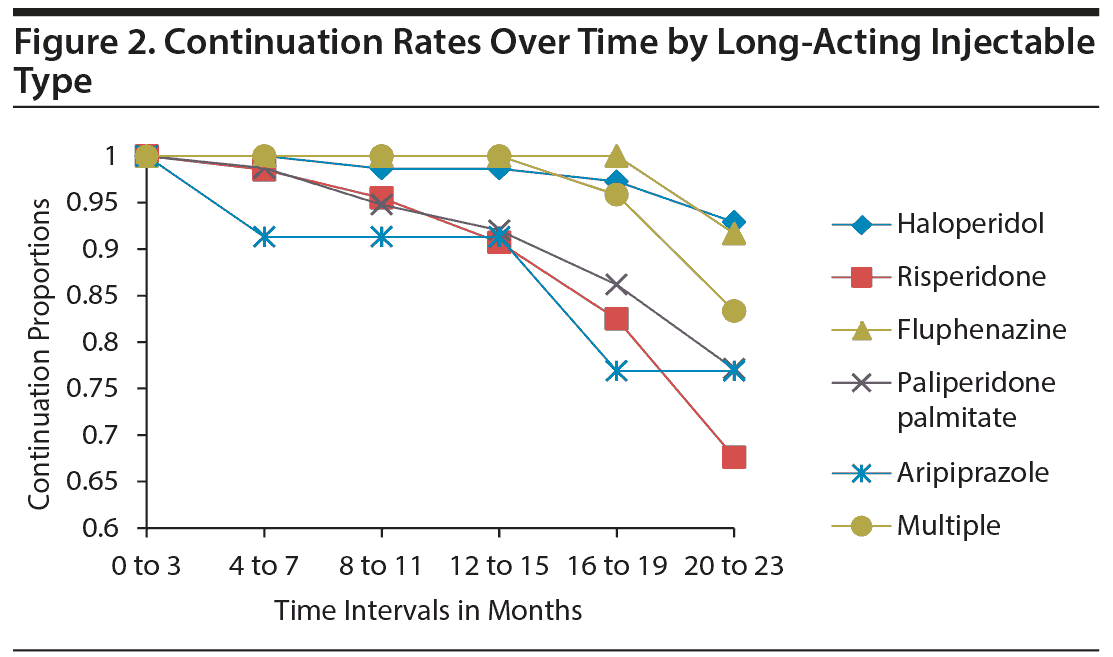
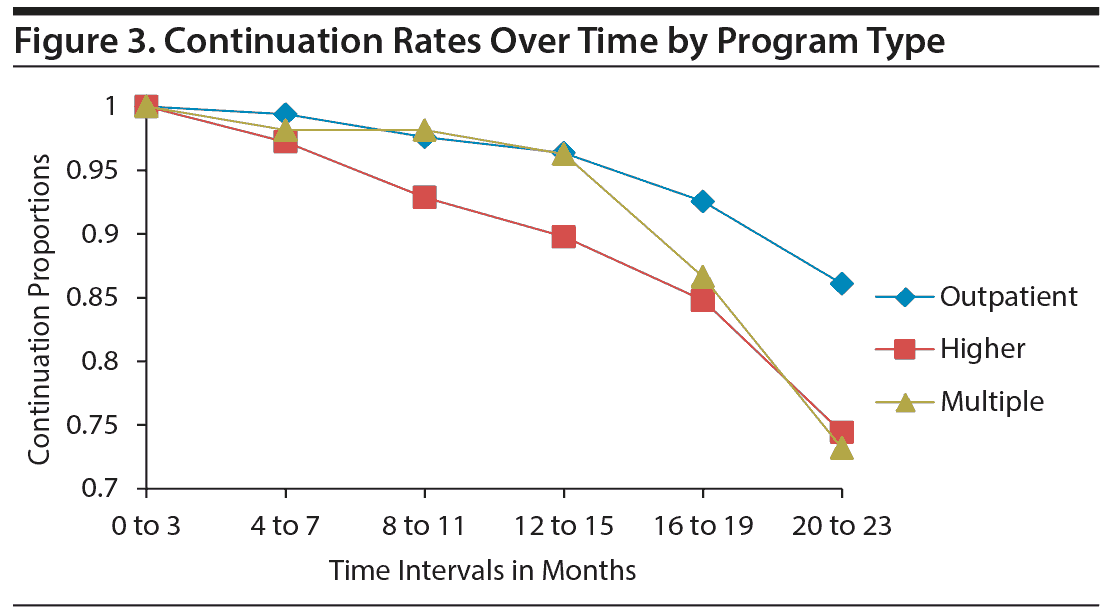
A hazard analysis for single-decrement, nonrepeatable events was used to assess the risk of discontinuation of LAIs over the study period. Graphs of hazard rates by groups were used for exploratory analyses before χ2 tests were completed to assess subgroup differences. The assumption of proportionality was met for subgroups of the independent variables sex, race, IOC status, and prescribed frequency of LAI. However, the exploratory analyses did reveal time-dependent effects between the subgroups for the independent variables of age (Figure 1), LAI used (Figure 2), and program type (Figure 3).
RESULTS
Hazard Analyses
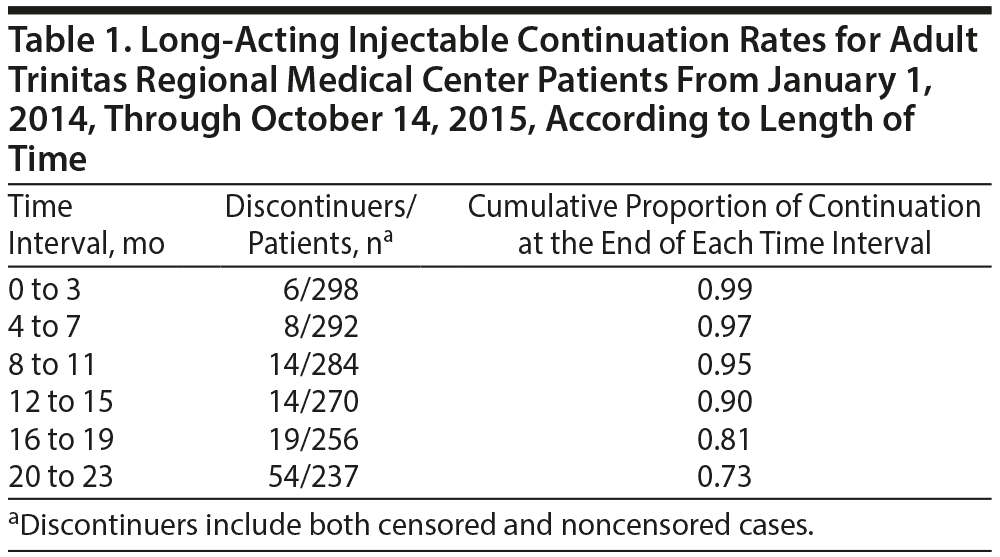
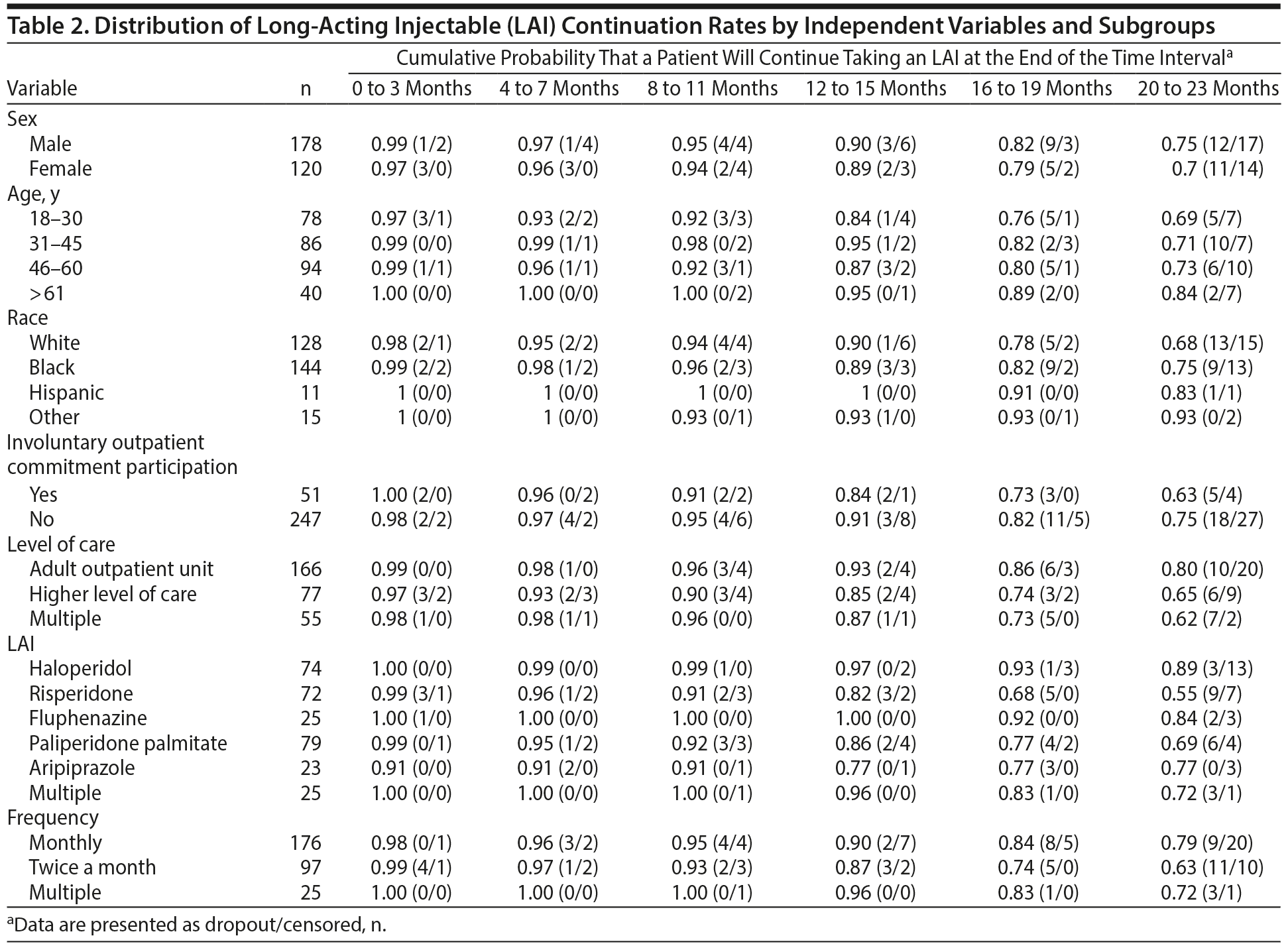
Across all patients, the cumulative LAI continuation rate at the end of the 23-month study period was 0.73 or 73%. The highest proportion of discontinuation occurred within the 16- to 19-month interval (Table 1). A summary of the hazard analysis results for independent variable subgroup continuation rates can be found in Table 2.
Subgroup Comparisons
Sex. No significant differences were found for LAI continuation rates of males and females overall (χ21 = 0.904, P = .342, n = 298) or at any specific time intervals.
Age. No significant differences were found for continuation rates of the different age groups overall (χ23 = 3.689, P = .297, n = 298). However, significant time-dependent effect differences were found between the aged 18 to 30 years subgroup (Pt = 0.839) compared to the aged 31 to 45 years subgroup (Pt = 0.952) for the time interval 16 to 19 months (χ21 = 4.874, P = .027, n = 164).
Race. No significant differences were found for LAI continuation rates between racial subgroups overall (χ23 = 5.785, P = .123, n = 298) or at any specific time intervals.
IOC participation. No significant differences were found for continuation rates of IOC and non-IOC patients either overall (χ21 = 2.989, P = .084, n = 298) or at any specific time intervals.
Program type. Significant differences were found for continuation rates of patients in different levels of care (χ22 = 10.252, P = .006, n = 298). Specifically, post hoc analyses indicated that continuation rates differed between the outpatient subgroup (Pt = 0.801) and both the higher level of care subgroup (Pt = 0.653, χ21 = 6.158, P = .013, n = 243) and the multiple levels of care subgroup (Pt = 0.618, χ21 = 7.431, P = .006, n = 221). Also, significant time-dependent effect differences were found between the outpatient subgroup (Pt = 0.861) and the multiple levels of care subgroup (Pt = 0.732) at the 20- to 23-month time interval (χ21 = 4.025, P = .045, n = 188).
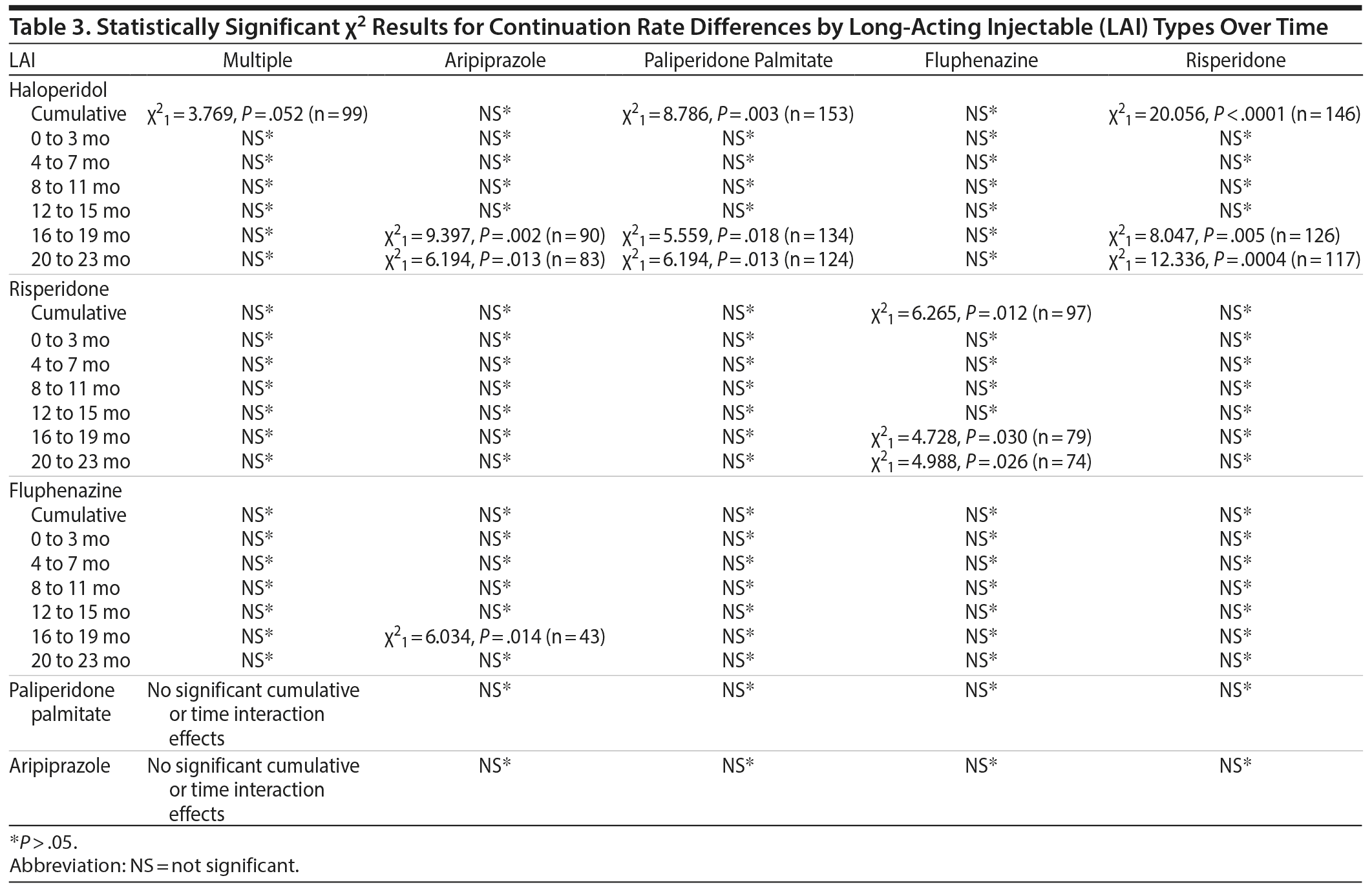
LAI type. Significant differences were found for continuation rates of patients receiving different LAIs (χ25 = 23.365, P < .000, n = 298). The multiple significant results of post hoc analyses for different LAIs and time-dependent effect differences are summarized in Table 3.
In addition, exploratory analyses conducted after the hazard analysis indicated a significant difference between the mean (SD) ages for individuals prescribed haloperidol (46.2 [15.04]) and risperidone (41.3 [15.27], t144 = −1.952, P = .05).
Prescribed frequency of LAI. Significant differences were found for continuation rates of patients receiving different prescribed frequencies of LAIs (χ22 = 7.622, P = .022, n = 298). Specifically, post hoc analyses indicated that continuation rates differed between the monthly subgroup (Pt = 0.787) and the biweekly subgroup (Pt = 0.633, χ21 = 7.483, P = .006, n = 273). There were no significant differences between the monthly and multiple subgroups (Pt = 0.725, χ21 = 0.484, P = .486, n = 201) or between the biweekly and multiple subgroups (χ21 = 0.729, P = .393, n = 122). No significant time-dependent effect differences were found.
DISCUSSION
The results indicating higher levels of adherence for the adult outpatient unit subgroup compared to the higher level of care and multiple levels of care subgroups were consistent with previous research.11,13 This finding may be surprising to those who believe that with increased frequency of contact and more “supportive” services in place, patients will show higher levels of medication adherence. While it is accurate that higher levels of care often do include more patient-prescriber contact, more clinical support and contact with therapists, more face-to-face monitoring, and more psychoeducation, other variables may intervene and lead to lower levels of LAI adherence in higher levels of care. Patients in higher levels of care may have greater symptom severity, which could make LAI adherence less likely. Also, the need to focus on the acuity of the patient’s clinical presentation at a higher level of care may limit the time spent by clinicians/prescribers “prepping” patients (eg, introducing LAIs, explaining LAIs, building rapport). This prepping may be crucial in the initial stages of LAI treatment to build commitment while bioavailability is being reached.
Highly significant differences were found in adherence between different LAIs. The highest rate of adherence across all LAI types was found for haloperidol compared to the second-generation LAIs. Several possible hypotheses for the higher adherence rates for haloperidol can be identified. First, it is possible that patients find the medication to be more effective and therefore continue to take it. Second, the significant difference found between the mean ages for individuals prescribed haloperidol and risperidone suggests a possible age/prescribed medication interaction in the current research. Finally, because the current research looked at only a circumscribed amount of time, it is possible that individuals who were taking haloperidol during the study period had already been stabilized on the LAI by the beginning date of the study, whereas patients who were prescribed risperidone began taking LAIs for the first time during the current study and therefore had not been stabilized. This finding warrants additional research, particularly relative to cost differences.17
There are several explanations for the higher rates of adherence among those receiving monthly injections compared to biweekly injections. One possibility is that the difference may be reflective of the patient’s physical or emotional discomfort at receiving more frequent injections. Another possibility could be the increased time commitment of attending biweekly injections. A third possible explanation could be related to prescriber bias. If certain patients are placed on biweekly injections because of the severity of their symptoms, those patients also may not be adherent as previously discussed.
Regarding time-dependent effect differences, the results suggest that across all variables, continuation rates are similar until patients reach the 12- to 15-month interval. After this time, it is more likely that patients will discontinue on the basis of age, LAI type, and level of care. This finding suggests that once patients have reached at least a year of LAI use, additional steps may need to be taken to ensure continued adherence. The lack of an association between continuation rates overall and the measured sociodemographic variables, age, sex, and race is consistent with other published studies.10-12
Finally, high LAI continuation rates were found in our sample. This finding is striking given the more commonly reported levels of nonadherence found in those being treated for schizophrenia.6 While we can begin to hypothesize from the current results about which variables may be associated with continuation of an LAI, a more controlled study will allow for more validity and predictive power of the significant findings.
Strengths, Limitations, and Directions for Future Research
Strengths. The study assessed adherence without the biases that are often present in formalized clinical trials. Instead, this study looked at adherence within the context of a “real-world” community mental health setting. Research in such a setting does not allow for inflated adherence rates due to monetary reinforcers for study participation and consistent reminder calls. Furthermore, because the majority of patients who come to TRMC have limited financial resources and other socioeconomic stressors, it provides an ideal setting to study adherence in underserved, inner-city populations. Finally, the use of a hazard analysis in the current study allowed for a more in-depth review of the interactions between adherence rates, time, and other variables.
Limitations. The current study provides only a retrospective analysis of a defined timeframe and a nonrandomized population. The findings cannot necessarily be generalized to the wider population of patients being treated with LAIs. The data that were analyzed, while dependable, did not allow for a thorough review of key variables such as relapses, hospitalizations, reasons for missed appointments, reasons for dropout/discontinuations, or patient perceptions of receiving LAIs. Also, some patients who attend higher levels of care do so just until they are stabilized and then return to private providers for continued medication monitoring. Because the current study was archival and did not follow up on patients who were “censored” in the hazard analysis, the results did not account for potential follow through with LAIs at other facilities. Finally, as quantified severity of symptoms and objective accuracy of diagnoses were not considered in the present study, potential impact of these variables on the results cannot be adequately assessed.
Directions for future research. In light of the current findings and limitations of this study, future research looking at variables such as prescriber-patient relationships, prescriber biases about LAIs, the amount and quality of the education on LAIs presented to the patient prior to and upon initiation, acuity of symptoms, and patient reasons for discontinuation will be essential.
Results that indicated the highest level of discontinuation occurred between 16 and 19 months suggest a need for research on the factors arising around this time period that lead to drops in adherence. Future research on adherence may want to use hazard analyses to further assess the interactions between length of time from beginning an LAI and relevant variables.
Finally, while age itself did not have a significant relationship with adherence, age was potentially related to type of LAI prescribed. Understanding these interactions between age and LAI type and even age and length of time on an LAI may help practitioners use different strategies to ensure adherence at each age.
CONCLUSION
It is crucial that we find ways to support medication adherence for patients with schizophrenia. This study has identified a cohort of highly adherent patients with schizophrenia, receiving a noncoercive, outpatient level of care, being treated with LAIs. It is likely that as the health care system moves to higher-quality, lower-cost solutions, LAIs could play a key role in increasing adherence and decreasing relapses.
Submitted: June 20, 2016; accepted November 3, 2016.
Published online: February 23, 2017.
Disclosure of off-label usage: The authors have determined that, to the best of their knowledge, no investigational information about pharmaceutical agents that is outside US Food and Drug Administration-approved labeling has been presented in this article.
Drug names: aripiprazole (Abilify), haloperidol (Haldol and others), olanzapine (Zyprexa and others), paliperidone palmitate (Sustenna), risperidone (Risperdal and others).
Financial disclosure: Dr McCreath is a consultant to Janssen and serves on the speakers or advisory boards for Otsuka and Alkermes. Drs Larson, Bharatiya, Weiss, and Lozovatsky and Mr Labanieh have no personal affiliations or financial relationships with any commercial interest to disclose relative to the article.
Funding/support: None.
Find more articles on this and other psychiatry and CNS topics:
The Journal of Clinical Psychiatry
The Primary Care Companion for CNS Disorders
REFERENCES
1. Kane JM. Review of treatments that can ameliorate nonadherence in patients with schizophrenia. J Clin Psychiatry. 2006;67(suppl 5):9-14. PubMed
2. Heres S. Long-acting injectable antipsychotics: an underutilized treatment option. J Clin Psychiatry. 2014;75(11):1263-1265. PubMed doi:10.4088/JCP.14com09541
3. Sajatovic M, Levin J, Ramirez LF, et al. Prospective trial of customized adherence enhancement plus long-acting injectable antipsychotic medication in homeless or recently homeless individuals with schizophrenia or schizoaffective disorder. J Clin Psychiatry. 2013;74(12):1249-1255. PubMed doi:10.4088/JCP.12m08331
4. Keith SJ, Pani L, Nick B, et al. Practical application of pharmacotherapy with long-acting risperidone for patients with schizophrenia. Psychiatr Serv. 2004;55(9):997-1005. PubMed doi:10.1176/appi.ps.55.9.997
5. Kane JM, Kishimoto T, Correll CU. Non-adherence to medication in patients with psychotic disorders: epidemiology, contributing factors and management strategies. World Psychiatry. 2013;12(3):216-226. PubMed doi:10.1002/wps.20060
6. Lacro JP, Dunn LB, Dolder CR, et al. Prevalence of and risk factors for medication nonadherence in patients with schizophrenia: a comprehensive review of recent literature. J Clin Psychiatry. 2002;63(10):892-909. PubMed doi:10.4088/JCP.v63n1007
7. Waddel L, Taylor M. Attitudes of patients and mental health staff to antipsychotic long acting injections: systematic review. Br J Psychiatry. 2009;195:42-50.
8. Weiden PJ, Roma RS, Velligan DI, et al. The challenge of offering long-acting antipsychotic therapies: a preliminary discourse analysis of psychiatrist recommendations for injectable therapy to patients with schizophrenia. J Clin Psychiatry. 2015;76(6):684-690. PubMed doi:10.4088/JCP.13m08946
9. Takaesu Y, Kishimoto T, Murakoshi A, et al. Factors associated with discontinuation of aripiprazole treatment after switching from other antipsychotics in patients with chronic schizophrenia: a prospective observational study. Psychiatry Res. 2016;236:71-74. PubMed doi:10.1016/j.psychres.2015.12.030
10. Williams R, Chandrasena R, Beauclair L, et al. Risperidone long-acting injection in the treatment of schizophrenia: 24-month results from the electronic Schizophrenia Treatment Adherence Registry in Canada. Neuropsychiatr Dis Treat. 2014;10:417-425. PubMed
11. Wheeler A, Vanderpyl J, Carswell C, et al. One-year treatment continuation in patients prescribed risperidone long-acting injection in New Zealand: a retrospective study. Clin Schizophr Relat Psychoses. 2012;6(2):61-68. PubMed doi:10.3371/CSRP.6.2.3
12. Aggarwal NK, Rosenheck RA, Woods SW, et al. Race and long-acting antipsychotic prescription at a community mental health center: a retrospective chart review. J Clin Psychiatry. 2012;73(4):513-517. PubMed doi:10.4088/JCP.11m07161
13. Taylor DM, Young C, Patel MX. Prospective 6-month follow-up of patients prescribed risperidone long-acting injection: factors predicting favourable outcome. Int J Neuropsychopharmacol. 2006;9(6):685-694. PubMed doi:10.1017/S1461145705006309
14. Taylor D, Atkinson J, Fischetti C, et al. A prospective 6-month analysis of the naturalistic use of aripiprazole—factors predicting favourable outcome. Acta Psychiatr Scand. 2007;116(6):461-466. PubMed doi:10.1111/j.1600-0447.2007.01102.x
15. Peuskens J, Olivares JM, Pecenak J, et al. Treatment retention with risperidone long-acting injection: 24-month results from the Electronic Schizophrenia Treatment Adherence Registry (e-STAR) in six countries. Curr Med Res Opin. 2010;26(3):501-509. PubMed doi:10.1185/03007990903488670
16. Ye W, Ascher-Svanum H, Tanji Y, et al. Predictors of continuation with olanzapine during the 1-year naturalistic treatment of patients with schizophrenia in Japan. Patient Prefer Adherence. 2011;5:611-617. PubMed doi:10.2147/PPA.S26002
17. Rosenheck RA, Leslie DL, Sint KJ, et al. Cost effectiveness of long acting injectable paliperidone palmitate versus haloperidol decanoate in the maintenance treatment of schizophrenia. Psychiatr Serv. 2016;67(10):1124-1130. PubMed doi:10.1176/appi.ps.201500447
Enjoy this premium PDF as part of your membership benefits!