Prim Care Companion CNS Disord 2022;24(6):22cr03388
To cite: Fournier O, Sanders E, Fetter JC. Low COVID-19 immunoglobulin G titers following vaccination and breakthrough infection in patients taking clozapine. Prim Care Companion CNS Disord. 2022;24(6):22cr03388.
To share: https://doi.org/10.4088/PCC.22cr03388
© 2022 Physicians Postgraduate Press, Inc.
aGeisel School of Medicine at Dartmouth, Lebanon, New Hampshire
bDartmouth Hitchcock Medical Center, Lebanon, New Hampshire
cNew Hampshire Hospital, Concord, New Hampshire
*Corresponding author: Jeffrey C. Fetter, MD, Geisel School of Medicine at Dartmouth, New Hampshire Hospital, 36 Clinton St, Concord, NH 03301 ([email protected]).
Severe mental illness (SMI) is associated with an increased risk of coronavirus disease 2019 (COVID-19) infection and an increased risk of morbidity and mortality.1–3 These risks exist even when controlling for comorbid conditions such as obesity and smoking; mental illness itself seems to mediate the impact of COVID-19 on patients with SMI.4
Clozapine is an important medication for the treatment of patients with SMI, being the only medication indicated for treatment-resistant schizophrenia and carrying additional benefits for suicidal thinking specifically.5 It is the only medication associated with reduced overall mortality in severe schizophrenia.6 An association between clozapine and secondary antibody deficiency has been observed. In a convenience sample, patients taking clozapine and clozapine-naive patients were compared for total immunoglobulin and immunoglobulin G (IgG) antibodies to several vaccine antigens, and subjects taking clozapine were found to have significantly lower antibody levels and required more antibiotics for clinically significant infections.7 Other studies8–10 have also shown an increased risk of pneumonia, inflammation, and antibiotic use in clozapine-treated patients.
If clozapine use were to decrease the effectiveness of COVID-19 vaccines, then this finding could have significant clinical implications for the care of these patients who are already at elevated risk for morbidity and mortality from this disease. As the 2022 Omicron wave began on the East Coast, the medical team at a state psychiatric hospital implemented a screening IgG antibody test for severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2) to identify potential candidates for Evusheld (tixagevimab and cilgavimab) among our patients prescribed clozapine. In these cases, we employed the ARUP Laboratories (Salt Lake City, Utah) semiquantitative chemiluminescent immunoassay, which detects antibodies against the spike protein receptor-binding domain that develop in response to vaccination and natural infection.11 Here, we present the cases of 2 patients who were both vaccinated and had breakthrough infections yet demonstrated markedly decreased antibody responses during this testing sweep.
Case 1
Mr A is a white man in his 20s with a history of schizoaffective disorder bipolar type, suicide attempts, violence, substance use disorder (marijuana, alcohol, ingesting “catnip”), tobacco use, posttraumatic stress disorder (PTSD), and attention-deficit/hyperactivity disorder (ADHD). He was psychiatrically admitted for suicidal and homicidal threats after engaging in arson. He displayed poor insight, grandiosity, delusional thinking, and extreme paranoia; reported auditory and visual hallucinations; and was seen responding to internal stimuli. He failed multiple antipsychotics and mood stabilizers, so clozapine was started 3 months into his admission to treat his psychosis and suicidal ideation. Clozapine was titrated up to 400 mg over the following 3 months with resolution of his hallucinations and mania. He was also prescribed lithium carbonate 1,500 mg/d, gabapentin 600 mg/d, melatonin 3 mg at night, vitamin D3 2,000 IU/d, glycopyrrolate 1 mg as needed for drooling, and pantoprazole 40 mg/d. He had chronic neutrophilic leukocytosis thought to be related to his lithium and clozapine, with an average leukocyte count of 11.09 × 109/L and an average absolute neutrophil count of 8.13 × 109/L during his admission. He also suffered from poor dentition and received a single course of amoxicillin 500 mg 3 times/d shortly before the COVID infection.
Mr A received the Johnson & Johnson (J&J) COVID-19 vaccine 6 months into his admission and declined multiple offers for a Moderna booster. Nine months into the admission, he tested positive for COVID-19 via a BinaxNOW nasal antigen test (Abbott, Chicago, Illinois). He was isolated for 10 days. On night 1 of his infection, he developed chills, hypotension (88/54 mm Hg), tachycardia (137 bpm), and hypoxia (87%), which increased to 94% on recheck; his blood pressure improved without intervention other than encouraging fluid intake. His highest temperature was 99°F. He also reported a sore throat and occasional cough. On day 10 of infection, his measured COVID-19 IgG (anti-spike) was positive, though lower than expected at 31.07 index value.
Case 2
Ms B is a white woman in her 40s with a history of major depressive disorder with psychotic features, who was involuntarily admitted for treatment-resistant depression with a recent suicide attempt by overdose. Other diagnoses included PTSD, ADHD, a remote subdural hematoma leading to a seizure disorder and mild cognitive impairment, as well as cocaine, opioid, and benzodiazepine use disorders in sustained remission. Her admission was complicated by bilateral otitis externa, a right ear abscess of the pinna that was positive for methicillin-resistant staphylococcus aureus, right mid-lung pneumonia treated with ceftriaxone and azithromycin, and a coronary artery bypass graft. Psychotropic medications included venlafaxine extended release 225 mg/d, buspirone 20 mg twice/d, prazosin 3 mg at bedtime, vitamin D3 2,000 IU/d, vitamin B12 500 mcg/d, and clozapine 200 mg at bedtime. Oxcarbazepine 600 mg twice/d and levetiracetam 750 mg twice/d were her anticonvulsants, and she also received metoprolol 12.5 mg twice/d, metformin extended release 500 mg at night, rosuvastatin 40 mg at night, and aspirin 81 mg/d. The clozapine was started at an outside hospital 6 months before admission, targeting suicidal behavior and psychotic symptoms. During the current admission, clozapine 600 mg/d was titrated down to 200 mg by the fourth month of hospitalization due to side effects. She received the J&J COVID-19 vaccine 2 months into the admission and repeatedly declined offers to receive a Moderna booster. Five months into the admission, she tested positive for COVID-19 via BinaxNOW. She was isolated for 10 days. She experienced a few days of myalgias, pharyngitis, rhinitis, a productive cough, and a temporary loss of taste and smell but remained afebrile. After 2 days of symptoms, her COVID-19 IgG titer was lower than expected at 1.1 index value. After she tested positive for COVID-19, her ear abscess worsened, and she was started on topical mupirocin ointment and a 5-day course of amoxicillin, followed by a 5-day course of prednisone 40 mg/d a month later when she developed facial hives thought to be a reaction to the topical mupirocin. The Supplementary Material provides additional laboratory results.
Discussion
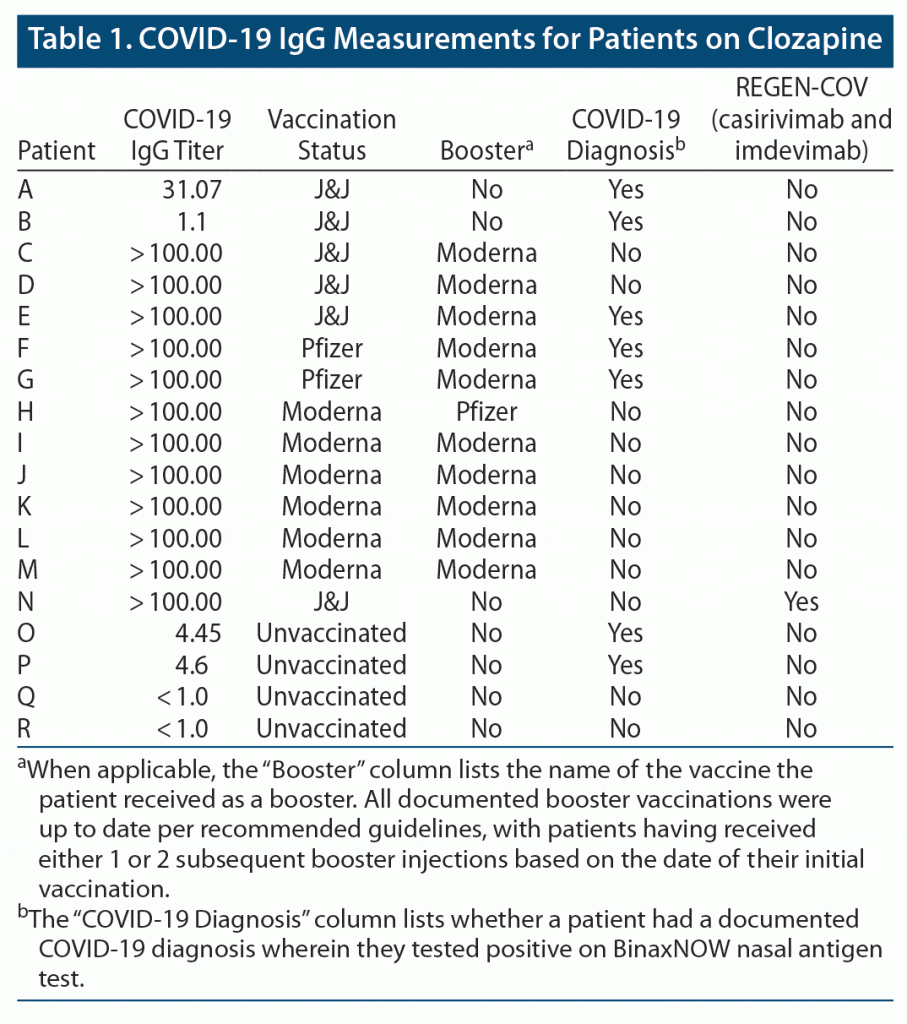
Anti–SARS-CoV-2 IgG levels for these patients were much lower than expected for being both vaccinated and infected with the virus. Although a positive result is ≥ 1.00 index value and there are no current recommendations for assessing vaccine response11 given limitations in inferring immunity, we are concerned that the patients who only received the J&J vaccine and no booster had lower levels compared to other boosted patients. As seen in Table 1, 11 vaccinated and boosted patients on clozapine during this period (Delta predominant) had a COVID-19 IgG measurement > 100 index value, including 3 patients who received an initial J&J vaccine followed by a Moderna booster. Only 3 of these 11 patients had a documented COVID-19 infection. One other patient, who had the single J&J vaccine, no booster, and never tested positive for COVID-19, received Regeneron’s postexposure prophylactic REGEN-COV (casirivimab and imdevimab) administration and had an antibody level > 100 index value. The only other clozapine patients who had COVID-19 IgG levels < 100 index value were 4 unvaccinated patients; 2 were diagnosed with COVID-19 during this outbreak (IgG levels of 4.45 and 4.6 index value), and the other 2 never tested positive (IgG level < 1 index value).
The antibiotics and steroids for Ms B’s ear infection and facial rash were started after the IgG level was measured, so we do not believe it affected the results in any way. Her repeated need for antibiotics suggests some degree of immune suppression from clozapine, as she did not have these symptoms prior to taking clozapine.
Our findings suggest that clozapine may blunt the immune response to vaccination against SARS-CoV-2, as well as post-illness antibody protection. We suggest that mRNA vaccines should be considered as preferred to the J&J vaccine, as no unexpectedly low titers were seen in those who received an mRNA vaccination. Clozapine patients should be strongly encouraged to receive a booster of an mRNA vaccine, especially those living in congregate settings, such as state hospitals and correctional facilities. Prophylactic monoclonal antibody treatment also appeared to boost immune response.
If further studies confirm a risk of COVID-19 immune failure for patients on clozapine, it may be indicated to routinely monitor levels of anti–SARS-CoV-2 antibody after vaccination and screen for histories of recurrent infections to determine which patients are candidates for preexposure prophylaxis with Evusheld (tixagevimab and cilgavimab).
Received: September 4, 2022.
Published online: November 15, 2022.
Relevant financial relationships: None.
Funding/support: None.
Patient consent: Consent was received from the patients to publish the reports, and information has been de-identified to protect anonymity.
Supplementary material: See accompanying pages.
References (11)

- Yang H, Chen W, Hu Y, et al. Pre-pandemic psychiatric disorders and risk of COVID-19: a UK biobank cohort analysis. Lancet Healthy Longev. 2020;1(2):e69–e79. PubMed CrossRef
- Maripuu M, Bendix M, Öhlund L, et al. Death associated with coronavirus (COVID-19) infection in individuals with severe mental disorders in Sweden during the early months of the outbreak-an exploratory cross-sectional analysis of a population-based register Study. Front Psychiatry. 2021;11:609579. PubMed CrossRef
- Wang Q, Xu R, Volkow ND. Increased risk of COVID-19 infection and mortality in people with mental disorders: analysis from electronic health records in the United States. World Psychiatry. 2021;20(1):124–130. PubMed CrossRef
- Mazereel V, Van Assche K, Detraux J, et al. COVID-19 vaccination for people with severe mental illness: why, what, and how? Lancet Psychiatry. 2021;8(5):444–450. PubMed CrossRef
- Owen MJ, Sawa A, Mortensen PB. Schizophrenia. Lancet. 2016;388(10039):86–97. PubMed CrossRef
- Tiihonen J, Lönnqvist J, Wahlbeck K, et al. 11-year follow-up of mortality in patients with schizophrenia: a population-based cohort study (FIN11 study). Lancet. 2009;374(9690):620–627. PubMed CrossRef
- Ponsford M, Castle D, Tahir T, et al. Clozapine is associated with secondary antibody deficiency. Br J Psychiatry. 2018;214(2):1–7. PubMed CrossRef
- Landry P, Benaliouad F, Tessier S. Increased use of antibiotics in clozapine-treated patients. Int Clin Psychopharmacol. 2003;18(5):297–298. PubMed CrossRef
- Nielsen J, Foldager L, Meyer JM. Increased use of antibiotics in patients treated with clozapine. Eur Neuropsychopharmacol. 2009;19(7):483–486. PubMed CrossRef
- de Leon J, Ruan CJ, Verdoux H, et al. Clozapine is strongly associated with the risk of pneumonia and inflammation. Gen Psychiatr. 2020;33(2):e100183. PubMed CrossRef
- COVID-19 IgG (Spike). Semi-Quantitative by CIA | ARUP Laboratories Test Directory. ARUP Laboratories website. Accessed July 27, 2022. https://ltd.aruplab.com/Tests/Pub/3003648?_ga=2.85060313.1167336289.1659060410-111487192.1659060410
Enjoy this premium PDF as part of your membership benefits!