Objective: Although depression is common among homeless mothers, little progress has been made in testing treatment strategies for this group. We describe pilot test results of an adapted collaborative care model for homeless mothers with depression.
Method: We conducted a pilot intervention study of mothers screening positive for depression in 2 randomly selected shelter-based primary care clinics in New York over 18 months in 2010-2012. Study participants completed a psychosocial, health, and mental health assessment at baseline, 3 months, and 6 months.
Results: One-third of women screened positive for depression (123 of 328 women). Sixty-seven women (63.2% of the eligible sample) enrolled in the intervention. At 6 months, compared to usual-care women, intervention group women were more likely to be receiving depression treatment (40.0% vs 5.9%, P = .01) and antidepressant medication (73.3% vs 5.9%, P = .001, respectively) and had more primary care physician and care manager visits at both 3 months (74.3% vs 53.3%, P = .009 and 91.4% vs 26.7%, P < .001, respectively) and 6 months (46.7% vs 23.5%, P = .003 and 70% vs 17.7%, P = .001, respectively). More women in the intervention group compared to usual-care women reported ≥ 50% improvement in depression symptoms at 6 months (30% vs 5.9%, P = .07).
Conclusions: This pilot study found that implementing an adapted collaborative care intervention was feasible in a shelter-based primary care clinic and had promising results that require further testing.
Trial Registration: ClinicalTrials.gov identifier: NCT02723058

CME Background
Articles are selected for credit designation based on an assessment of the educational needs of CME participants, with the purpose of providing readers with a curriculum of CME articles on a variety of topics throughout each volume. Activities are planned using a process that links identified needs with desired results.
To obtain credit, read the article, correctly answer the questions in the Posttest, and complete the Evaluation.
CME Objective
After studying this article, you should be able to:
‘ ¢ Engage homeless women with major depressive disorder in treatment using a collaborative care model
Accreditation Statement
The CME Institute of Physicians Postgraduate Press, Inc., is accredited by the Accreditation Council for Continuing Medical Education to provide continuing medical education for physicians.
Credit Designation
The CME Institute of Physicians Postgraduate Press, Inc., designates this journal-based CME activity for a maximum of 1.0 AMA PRA Category 1 Creditâ„¢. Physicians should claim only the credit commensurate with the extent of their participation in the activity.
Note: The American Academy of Physician Assistants (AAPA) accepts certificates of participation for educational activities certified for AMA PRA Category 1 Creditâ„¢ from organizations accredited by ACCME or a recognized state medical society. Physician assistants may receive a maximum of 1.0 hour of Category I credit for completing this program.
Date of Original Release/Review
This educational activity is eligible for AMA PRA Category 1 Creditâ„¢ through April 30, 2018. The latest review of this material was April 2016.
Financial Disclosure
All individuals in a position to influence the content of this activity were asked to complete a statement regarding all relevant personal financial relationships between themselves or their spouse/partner and any commercial interest. The CME Institute has resolved any conflicts of interest that were identified. In the past year, Larry Culpepper, MD, MPH, Editor in Chief, has been a consultant for Forest, Lundbeck, Merck, Shire, Takeda, and Elsevier Press; has been a stock shareholder of M3 My Mood Monitor; and has received royalties from UpToDate and Oxford University Press. No member of the CME Institute staff reported any relevant personal financial relationships. Faculty financial disclosure appears at the end of the article.
Managing Depression Among Homeless Mothers:
Pilot Testing an Adapted Collaborative Care Intervention
ABSTRACT
Objective: Although depression is common among homeless mothers, little progress has been made in testing treatment strategies for this group. We describe pilot test results of an adapted collaborative care model for homeless mothers with depression.
Method: We conducted a pilot intervention study of mothers screening positive for depression in 2 randomly selected shelter-based primary care clinics in New York over 18 months in 2010-2012. Study participants completed a psychosocial, health, and mental health assessment at baseline, 3 months, and 6 months.
Results: One-third of women screened positive for depression (123 of 328 women). Sixty-seven women (63.2% of the eligible sample) enrolled in the intervention. At 6 months, compared to usual-care women, intervention group women were more likely to be receiving depression treatment (40.0% vs 5.9%, P = .01) and antidepressant medication (73.3% vs 5.9%, P = .001, respectively) and had more primary care physician and care manager visits at both 3 months (74.3% vs 53.3%, P = .009 and 91.4% vs 26.7%, P < .001, respectively) and 6 months (46.7% vs 23.5%, P = .003 and 70% vs 17.7%, P = .001, respectively). More women in the intervention group compared to usual-care women reported ≥ 50% improvement in depression symptoms at 6 months (30% vs 5.9%, P = .07).
Conclusions: This pilot study found that implementing an adapted collaborative care intervention was feasible in a shelter-based primary care clinic and had promising results that require further testing.
Trial Registration: ClinicalTrials.gov identifier: NCT02723058
Prim Care Companion CNS Disord 2016;18(2):doi:10.4088/PCC.15m01907
© Copyright 2016 Physicians Postgraduate Press, Inc.
aFamily Medicine and Community Health, University of Massachusetts Medical School, Worcester
bCare for the Homeless, New York, New York
cPreventive and Behavioral Medicine, University of Massachusetts Medical School, Worcester
*Corresponding author: Linda Weinreb, MD, Family Medicine and Community Health, University of Massachusetts Medical School, 55 Lake Ave North, Worcester, MA 01655 ([email protected]).
Homeless mothers are more vulnerable to major depressive disorder (MDD) than comparable groups of impoverished mothers, with rates in community studies approaching 50%.1-3 While depression may not predispose poor mothers to homelessness, and in fact, may be a consequence of homelessness,4 it can interfere with mothers’ capacity to care for children and to successfully pursue education and employment. Depression may also contribute to difficulties in overcoming homelessness.5 Although primary care offers an ideal venue to identify and manage depression among women who commonly fail to receive needed mental health services, we are unaware of rigorously tested primary care-based treatment strategies that address the needs of homeless mothers with depression.
Among homeless women with symptoms suggestive of depression, less than one-third received mental health services during the prior year,6 reinforcing the need to identify and engage women in primary care. Additionally, homeless mothers with mental health issues report conflict between meeting the needs of their children and managing their own illnesses, which creates a barrier to treatment participation.7 There is good evidence that women with mental health disorders seek care more commonly in primary care settings compared to specialty treatments.8,9 Further, homeless mothers with depression often have trauma histories that are accompanied by physical health conditions, resulting in high levels of medical care utilization and increasing the likelihood that they can be identified in primary care settings.9
The collaborative care model offers an effective treatment approach for depression in primary care.10,11 While tested with diverse patient populations, it has not been adapted for and tested with homeless mothers. In this article, we provide information on a sample of homeless mothers receiving primary care and report results on a pilot test and feasibility findings of a new intervention, the Integrated Care Model for Homeless Mothers (ICMHM), adapted from the collaborative care model to address unique aspects of care for homeless mothers who screened positive for depression during a shelter-based primary care visit.
METHOD
Study Setting and Recruitment
The study was conducted at 2 randomly selected and then assigned (one to intervention and one to usual care) primary care clinics based in family residence shelters in Queens and Bronx, New York (ClinicalTrials.gov identifier: NCT02723058). The design took advantage of the way in which homeless families were assigned on a rotating basis from a central registry to shelters in New York City, which controlled for possible bias in populations among different shelters.
All women entering the 2 shelters over 18 months in 2010-2012 were targeted for screening using the 9-item Patient Health Questionnaire (PHQ-9).12,13 Shelter policies required new shelter residents to visit the primary care clinic to review basic health information. The vast majority of women complied, and at least 90% also received the depression screening questionnaire. Women who screened positive for possible MDD (score ≥ 10 on the PHQ-9) and who met criteria for the intervention study (aged ≥ 18 years, not pregnant, not currently receiving depression treatment, and not currently psychotic) were asked if they would be willing to talk to the research coordinator about study enrollment. The research coordinator made an appointment at the shelter within 1 week to explain the study. Whether or not they consented to study enrollment, any woman who screened positive for depression was provided an appointment with the primary care physician (PCP) and with the care manager to initiate depression treatment following the intervention model and to address any other health care needs. At the usual-care site, women who screened positive for depression also were provided appointments with the PCP who initiated treatment as usual, which could include antidepressant medication and recommendation for psychotherapy outside the clinic. Women in the usual-care group received general case management services that were available to all families receiving health services at the clinic. These services included, for example, assistance with obtaining public benefits, linking with community resources for family activities, outside mental health or substance use services, and meeting children’s educational needs.

- Implementing a collaborative care model for depression in homeless shelter-based primary care clinics helps engage hard-to-reach and high-risk women in depression treatment by improving session completion and medication use.
- Without proactive outreach and regular monitoring, high-risk women will receive fewer treatment services.
- While multiple comorbidities and daily living stressors make it difficult for women to achieve positive clinical outcomes, this pilot model appears to help more women achieve clinically significant improvement.
Intervention
The intervention consisted of a collaborative care model14,15 modified to address the needs of homeless mothers. The collaborative care model principles of leadership engagement, proactive outreach by case managers, enhanced patient self-management, systems redesign, and use of clinical decision-making tools were incorporated into the intervention design. Leadership engagement involved training of the organization chief executive officer and clinical leaders, who provided commitment and support for universal depression screening and modification of PCP and existing case manager roles to implement the collaborative care model. The organization redesigned clinic systems at the intervention site (eg, implementation of universal screening processes) and made modifications to clinical decision tools (eg, adding fields and tracking capacity to the existing electronic medical record to be used to monitor depression symptom improvement). An existing case manager increased hours and was trained to become the depression care manager. The care manager was provided training and written materials to implement depression psychoeducation and facilitate patient goal setting and self-management, as well as proactive, scheduled outreach to patients to monitor symptom change. Training was also provided to the PCP, including collaborating with the care manager to implement outreach, regular symptom monitoring, review of patient self-management, and treatment modifications. Further modifications of prior collaborative care model interventions included (1) incorporating a treatment engagement interview at the beginning of treatment conducted by the care manager, (2) having the care manager address basic needs (eg, obtaining public assistance, food stamps, and clothing that many homeless families require) and children’s needs (eg, diapers; Special Supplemental Nutrition Program for Women, Infants, and Children; clothing; school evaluations or placements) that might interfere with women’s ability to focus on depression treatment, and (3) simultaneously addressing mental health comorbidities (eg, addressing substance use problems or posttraumatic stress disorder through collaboration with other providers or consultation with the clinic’s consulting psychiatrist).
Training and Supervision
Four hours of initial training were provided to all staff at the intervention clinic and 20 hours to the care manager who was a master’s level trained mental health clinician. Three subsequent 2-hour team training sessions were provided over the next 18 months. We completed weekly case supervision calls with the care manager and PCP and monthly calls with a supervising psychiatrist. Calls were designed to determine fidelity in PCP and care manager encounters to recommended collaborative care model components. A fidelity checklist reviewed the basic elements of the collaborative care model to be implemented in patient encounters (eg, symptom assessment, review of self-management and update of patient goal setting, medication compliance if applicable, and treatment modifications when necessary) and was completed on the list of active cases reviewed at each call. Fidelity to the components was uniformly high in almost all encounters, and, typically, components were skipped only if the patient was in crisis and the encounter needed to focus on the proximal issues to the exclusion of depression monitoring. The care manager also periodically provided taped recordings of engagement interviews for more focused clinical supervision using an evaluation guideline developed by Grote et al.16
Implementation
After a positive PHQ-9 screen, both the PCP and the care manager met with the patient to do intake and treatment planning sessions and determine if there were other health, mental health, or support issues to address. The care manager’s role was to obtain a psychosocial history, identify unmet basic needs, and implement a treatment engagement interview. The initial case management session was modeled after the patient engagement work of Grote et al16 and focused on allowing the patient to tell her history, identify concerns about and barriers to depression treatment, and participate in treatment and self-management decisions.
The PCP assessed depression in the context of other health care needs and initiated treatment planning, which included regular meetings with the care manager, prescribing medication, potential for outside psychotherapy referral, and follow-up. The PCP was the primary prescriber for antidepressant medications unless the team decided that the consulting psychiatrist needed to monitor patients with comorbidities or multiple medications. Referrals to community-based counseling and substance abuse programs were made when deemed appropriate and the patient was willing to initiate outside services. Guidance on addressing comorbidities was provided to the PCP and care manager during training and through psychiatric supervision. Weekly or biweekly outreach was conducted for 6-8 weeks followed by as-needed visits or check-ins for 6 months to support follow-through with treatment recommendations. Periodic PHQ-9 reassessment measured treatment progress.
Study Method
At the baseline interview, the research coordinator obtained informed consent and completed an interview that collected information about demographic characteristics, housing, employment, income, insurance status, and stressful life events and administered standardized mental and physical health measures. The research coordinator contacted participants again 3 months and 6 months after baseline to readminister mental and physical health measures and to obtain feedback on their relationship with the care manager and PCP. Attempts to contact participants for follow-up study data collection were made repeatedly to those residing in the shelter and those who had left the shelter for up to 2 months after the last follow-up time point.
Measures
The depression screening measure, the PHQ-9,12,17,18 was utilized to determine primary eligibility for the study, with a score ≥ 10 triggering referral for study participation. The Hopkins Depression Symptom Checklist-Depression Scale 2019,20 was used to confirm depression symptoms at baseline and to document the primary outcome of reduction in depressive symptoms at follow-up. A score ≥ 0.75 indicates presence of depressive symptoms; a score ≥ 1.75 indicates moderate to severe depression.21
Additional measures used to evaluate comorbidities and possible confounders included the Posttraumatic Diagnostic Scale22 to determine stress related to violence and other threatening events at baseline, the 10-item Drug Abuse Screening Test23,24 to ascertain misuse of prescription or street drugs and the Alcohol Use Disorders Identification Test-Consumption25 to screen for comorbid alcohol use problems at baseline and follow-up, the Medical Outcomes Study 8-item Short-Form Health Survey (SF-8)26 to ascertain general physical and mental health at baseline and follow-up, and the 7-item Generalized Anxiety Disorder scale27 to identify generalized anxiety at baseline and follow-up.
The quality of the relationship with the PCP was measured by the 15-item Patient Reactions Assessment.28 The quality of the relationship with the care manager was measured using the Helping Alliance Questionnaire.29 Finally, data on visits to the care manager and PCP for both groups and on antidepressant medication use were recorded in the clinical electronic medical record and extracted and analyzed at the end of the study.
Analysis
Data were analyzed using Stata/MP software version 12.1 (StataCorp LP, College Station, Texas). Differences between intervention and usual-care groups for categorical variables were quantified using a χ2 statistic and a Fisher exact test statistic for those with cell counts < 5. A t test was used to test the differences in continuous measures when the distribution of the measure was approximately normal, and a Wilcoxon rank-sum test was used when the distribution was skewed. Significant predictors of the continuous Hopkins Symptom Checklist depression score and the dichotomous indicator of 50% improvement in the depression score by end of follow-up were explored using multivariable linear and logistic regression models.
Rates of follow-up at 6 months were similar in both groups, but a significant number of women were lost to follow-up. Demographic, physical, and mental health baseline characteristics were similar between those who completed the study and those who did not. Those who experienced physical violence from someone they did not know (23.9% vs 50.0%) and those with an increased number of traumatic exposures (2.6 vs 3.5) were more likely to be lost to follow-up. All women who completed a 6-month visit were included in the analysis.
RESULTS
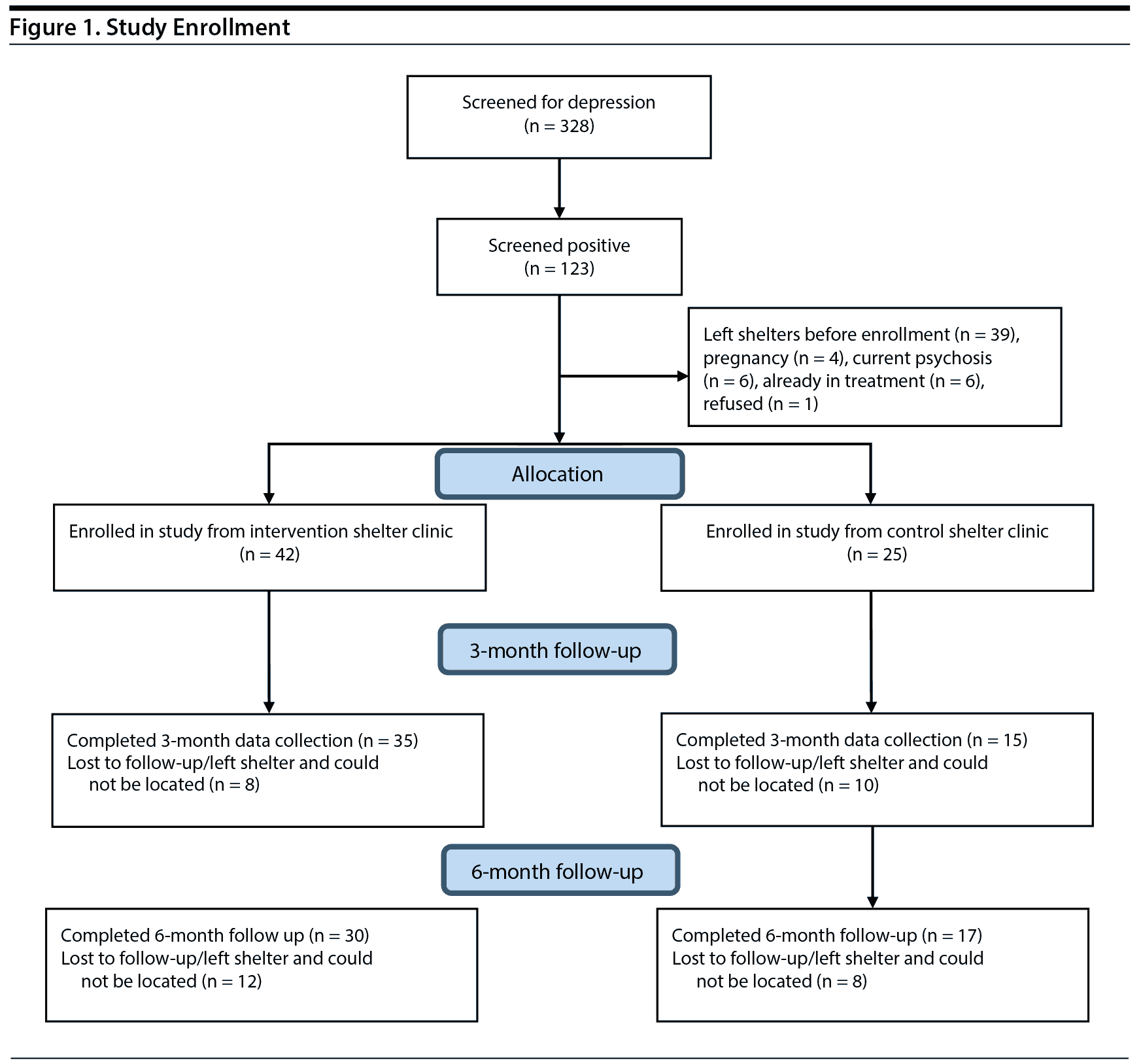
A total of 328 women were screened. This number represents over 90% of all mothers entering the shelters during this time period. The mean PHQ-9 score for all screened was 8.2 (SD = 6.6). Over one-third of women (37.5%) screened positive with a PHQ score ≥ 10. Of the 123 women who screened positive, 39 left the shelters before the study could be explained and additional information collected. This was because city policy was to provide temporary shelter while final determination for longer-term shelter was investigated. If women were not deemed eligible for publicly funded shelter (eg, they had some type of prior shelter violation), they were discharged quickly. Additionally, 17 women did not meet other study criteria after meeting with the study coordinator, and 67 eligible women (63.2%) completed the baseline interview. Of the 17 women who met with the study coordinator, only 1 refused to enroll in the study, 4 were ineligible due to pregnancy, 6 had evidence of active psychoses, and 6 were already involved in ongoing mental health treatment. Figure 1 shows the sample from screening through enrollment and follow-up.
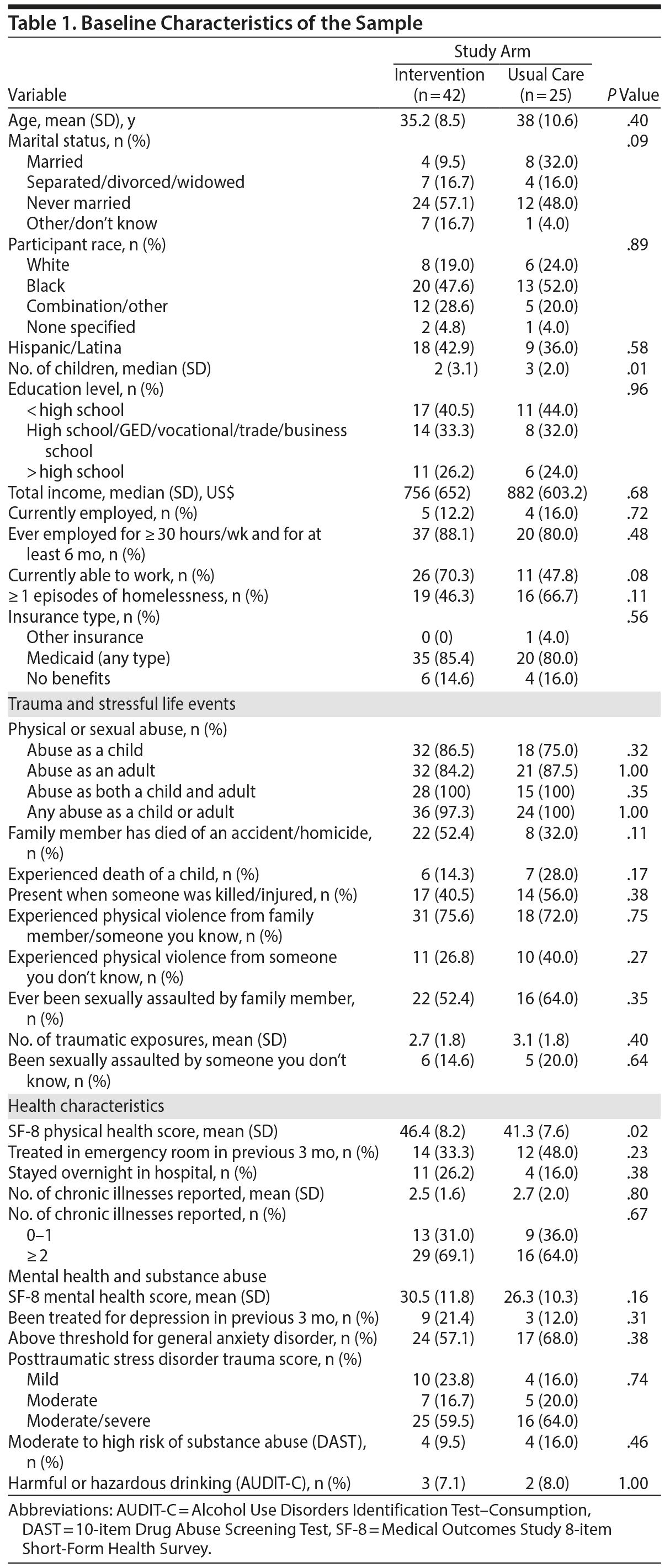
Table 1 presents baseline characteristics of the sample by study condition. Women in both conditions were similar in all characteristics except for number of children (P = .01) and SF-8 physical health score (P = .02). Women were on average 36 years of age (intervention: 35.2 years, usual care: 38 years); 52.2% had been homeless before. The majority of women were on Medicaid (intervention: 85.4%, usual care: 80%). Almost 100% of women in both groups reported a past history of childhood or adulthood abuse (intervention: 97.3%, usual care: 100%). Women reported an average of 3 chronic illnesses (intervention: 2.5, usual care: 2.7).
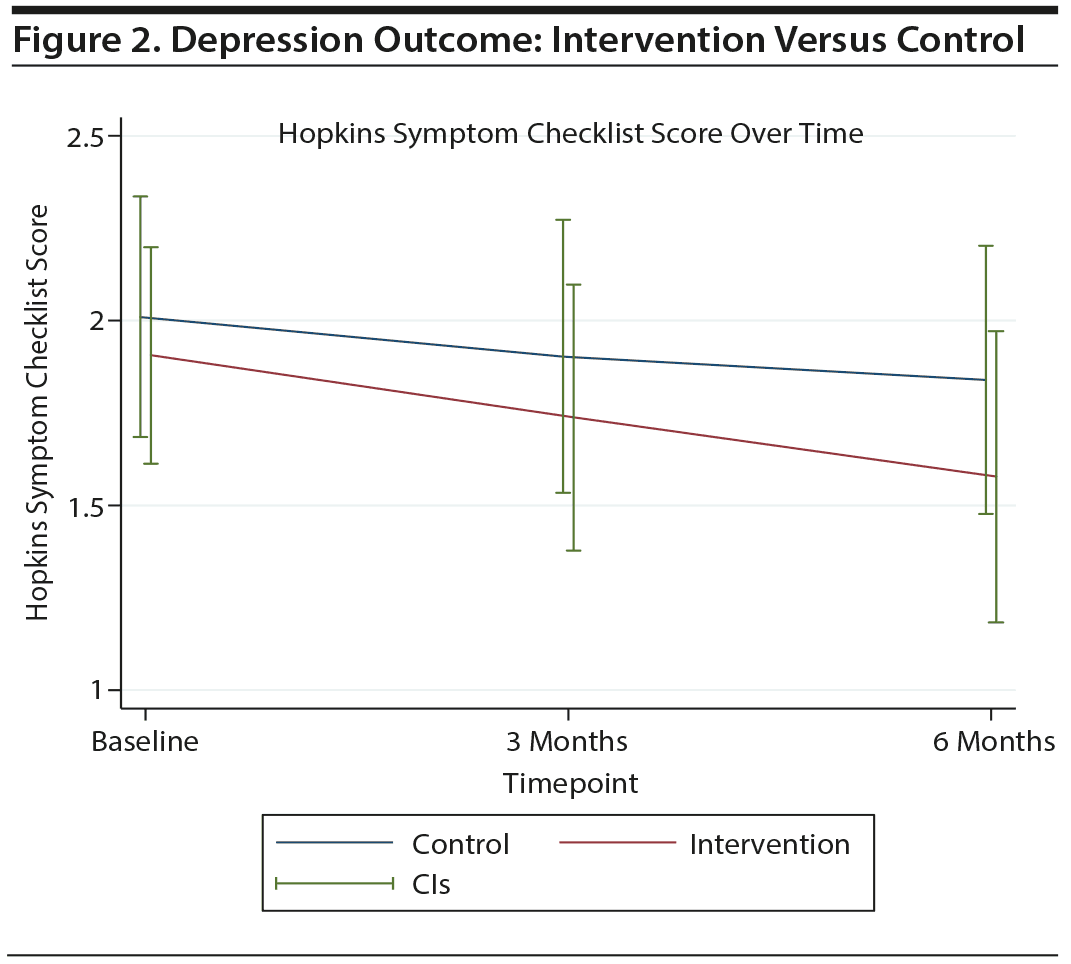
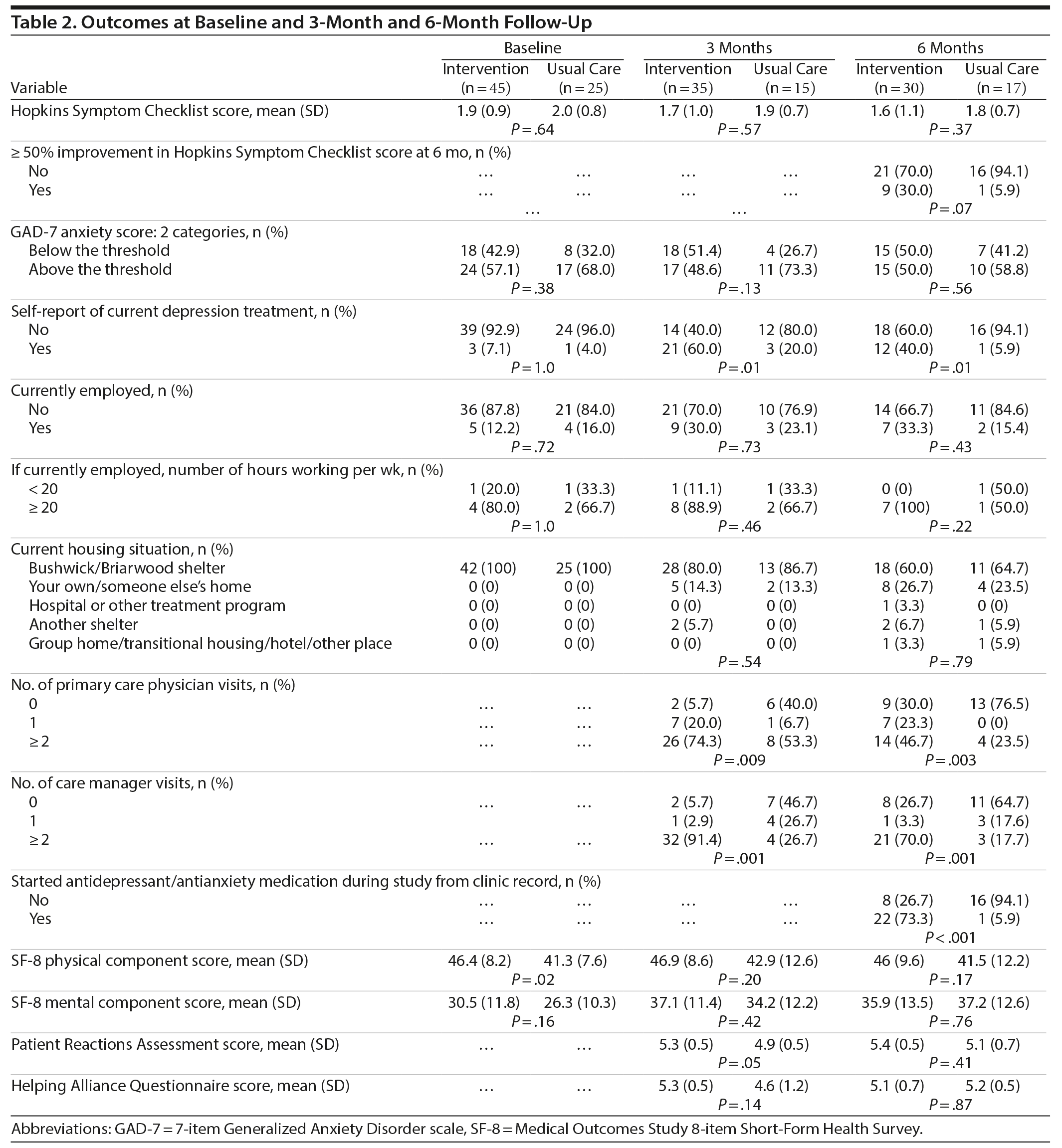
We observed a significant drop in the continuous depression score for all women by the end of follow-up (−0.27, 95% CI = −0.50 to −0.05, P = .02 for time trend) (Figure 2). Table 2 presents outcome measures at baseline and follow-up by study condition. There were no significant differences detected between study groups in the continuous depression outcome measure at follow-up; however, the difference in the proportion of women achieving ≥ 50% improvement in depression symptoms at 6 months approached significance (intervention: 30%, usual care: 5.9%, P = .07). Self-report of receiving current depression treatment differed significantly between groups at 3 months (intervention: 60%, usual care: 20%, P = .01) and 6 months (intervention: 40%, usual care: 5.9%, P = .01). Women in the intervention group also had significantly more PCP and care manager visits at both 3-month (74.3% vs 53.3% with ≥ 2 PCP visits, P = .009; 91.4% vs 26.7% with ≥ 2 care manager visits, P < .001, respectively) and 6-month (46.7% vs 23.5% with ≥ 2 PCP visits, P = .003, respectively); 70% vs 17.7% with ≥ 2 care manager visits, P = .001, respectively) follow-up than women in the control group. Further, by 6-month follow-up, 73.3% of women in the intervention group had been prescribed an antidepressant medication compared to 5.9% of women in the usual-care group (P ≤ .001).
There were no significant differences between groups in anxiety, mental or physical health functioning, the Patient Reactions Assessment, or the Helping Alliance Questionnaire at follow-up. Our modeling of continuous depression outcome and 50% improvement including variables such as age, baseline depression scores, baseline anxiety, baseline general health, number of care manager and PCP visits, use of medication, and intervention condition revealed that only baseline depression and anxiety scores predicted 6-month depression scores for the continuous variable. There were no significant predictors of 50% improvement in depression score, but, similar to the bivariate outcome, the intervention condition was close to marginally significant controlling for baseline characteristics in predicting improvement (P = .103).
In terms of employment, at 6-month follow-up, 33% of intervention group mothers reported working currently compared to 12% at baseline. There was little change in baseline and follow-up employment status among the usual-care group (16% and 15%, respectively). In terms of housing status, at 6-month follow-up, both groups had similar situations in terms of housing with more than half of women still in shelters (intervention: 66% vs usual care: 70%).
DISCUSSION
This study provides information on depression rates and associated comorbidities among homeless mothers receiving primary care. A recent review30 highlighted the dated nature of the homeless families’ literature and the need for current research to guide the public health community. Despite high levels of reported depression among homeless mothers, little progress has been made in developing and testing treatment strategies that target this group.31 To our knowledge, this study is the first in the scientific literature to test the feasibility of, and report pilot results from, a treatment study for homeless mothers with depression.
Over one-third of the mothers receiving primary care in our study screened positive for depression. While this represents a lower rate than older studies,3 it is 2-4 times the rate of comparable low-income women attending public-sector health care settings.32,33 Not surprisingly, depression was accompanied by high rates of mental health and physical health comorbidities and recent medical hospitalization. Almost all women had multiple traumatic exposures, a factor that has been commonly associated with depression34 and has been described as common among homeless mothers.3,35 Our findings highlight the importance of primary care settings recognizing and addressing these conditions together.
Despite high rates of depression, less than 20% of mothers in our study had received recent depression treatment. Our findings concur with prior research describing that the majority of homeless mothers with depression symptoms do not receive treatment.3,6 Numerous barriers contribute to why homeless mothers fail to seek mental health treatment including prior negative experiences with the health care system,30,35 stigma,36 fear of child welfare intervention,7 and mothers’ belief that a change in life circumstances would relieve their depression rather than treatment.37 Therefore, targeting homeless mothers for depression screening in less stigmatizing primary care settings, including shelter-based primary care clinics, has the potential to more readily engage women and address their multiple medical and mental health issues.
Overall, we found few differences in primary or secondary outcomes between intervention and usual-care participants. However, the difference in the proportion of women achieving at least a 50% improvement in depression symptoms at 6 months, a commonly used measure of treatment improvement,38 approached significance among intervention group women. Additionally, the intervention appeared to better engage women to participate in treatment. Compared to women in the usual-care group, intervention participants were significantly more likely to be receiving depression treatment at 3- and 6-month follow-up, were more likely to be receiving antidepressant medication, and had more visits with the care manager and PCP. While this small pilot study did not have the power to demonstrate significant mean depression score differences between intervention and control women at 6-month follow-up, there was some evidence that more intervention women improved by a clinically significant degree. It is possible that improvement in depression outcomes may have been detected with a larger sample or longer follow-up period. It is also possible that our intervention was not intensive enough to show differences given that women in the usual-care group were also linked with a PCP who provided depression treatment and had access to case management services.
While there is good evidence that counseling and medication treatment improve depression outcomes,21 considerable effort is still needed to successfully engage low-income, ethnically diverse women with depression treatment. The ICMHM utilized components that may have contributed to the observed improvements in treatment participation in the intervention group. The ICMHM adapted an engagement approach developed by Grote et al16 designed to engage and retain low-income women in care by conducting a session at the outset of depression treatment that aims to build trust and address women’s concerns and resistance to depression treatment. This session, which was condensed to 20 minutes and conducted by a care manager rather than a therapist as in Grote’s study, enabled the care team to proactively address concerns that might limit mothers’ participation in care. It is also possible that other aspects of the model, including addressing children’s unmet needs and blending depression care with managing basic needs, supported mothers in the intervention group to participate more actively in care.
We did not detect significant differences in housing or employment, although there was a trend for intervention women to more likely be working at follow-up. There were no detectable differences in housing status at follow-up. Past studies39,40 suggest that homeless families’ characteristics, including depression, may have less bearing on the entry to and exit from shelter compared to policy, program, and resource factors. Nevertheless, it is critical to identify effective ways to address depression among homeless mothers given its common occurrence and associated adverse consequences for mothers and their children.
This pilot study found that implementing an adapted collaborative care model was feasible in a shelter-based primary care clinic. Heightened awareness about the importance of identifying depression, training on the use of the screening measure, and buy-in by leadership facilitated more routine intervention. While engagement in depression care was significantly improved for the intervention women compared to usual care, there still remained barriers to fully implementing the collaborative care model that may explain the lack of strong differences between the 2 groups. For example, compliance with follow-up visits was often prevented by shelter rules that required women’s attendance at mandatory meetings and housing search efforts. Some families were also discharged abruptly, making continuity and a long enough period of care difficult to achieve. Procedures to routinely collaborate between the shelter and health care teams did not appear to be in place, although communication on behalf of specific families did occur at times. Strengthening communication between health care providers and shelter staff might allow for the modification of shelter requirements so mothers can attend needed health visits. Clinics may need to offer flexible hours during the weekend or evening when mothers may have fewer conflicts that interfere with appointments. When possible, alerting the health providers to an upcoming discharge from the shelter would allow them to create a bridge to a health setting in the family’s new community or neighborhood. Building effective linkages between homeless health care programs and community health care programs may allow for improvements in care continuity. Given that many homeless families may move to housing in a different geographic area than where sheltered, coordinating needed services for depression may be necessary across not only health care sites but also with other types of community settings.41
Our study is limited in that the sample size is small and we do not have data on those who refused screening or did not complete the baseline interview. Also, our results may only generalize to urban areas with similar shelter eligibility criteria.
Health care reform, the emergence of patient-centered medical homes, and a growing evidence base suggesting that behavioral health and primary care services can be effectively integrated offer important opportunities to more effectively serve homeless mothers. The Affordable Care Act provides funding that encourages states and health providers to develop innovative health care models for high-risk populations. Untreated depression may interfere with mothers’ ability to care for their children, successfully pursue employment and education, and maintain housing. Unaddressed mental health needs may also interfere with the success of current federal homeless policies to facilitate rapid rehousing. The adapted collaborative care model appears promising as an approach to address the significant need for depression treatment among homeless mothers. This feasibility study provides important information to use in refining the intervention to improve access to depression treatment for a hard-to-reach high-risk population.
Submitted: November 10, 2015; accepted January 29, 2016.
Published online: April 21, 2016.
Disclosure of off-label usage: The authors have determined that, to the best of their knowledge, no investigational information about pharmaceutical agents that is outside US Food and Drug Administration-approved labeling has been presented in this article.
Financial disclosure: Drs Weinreb, Upshur, and Reed and Mss Fletcher-Blake and Frisard have no personal affiliations or financial relationships with any commercial interest to disclose relative to the article.
Funding/support: This research was supported by a grant from the National Institute of Mental Health (R34MH085881).
Role of the sponsor: The funding agency played no role in the design and conduct of the study; collection, management, analysis, and interpretation of data; or preparation, review, or approval of the manuscript.
Acknowledgments: The authors thank the Care for the Homeless service delivery team for their participation in the study, Karen Johnson, PhD (Columbia University, School of Social Work, New York, New York) for her effort in conducting the research field operation, and Carol Caton, PhD (Columbia University, Department of Psychiatry, New York, New York) from Columbia Homelessness Prevention Center for her conceptual contributions to the study and contribution to the field operation supervision. They also thank Nancy Grote, PhD (University of Washington, School of Social Work, Seattle, Washington) for her conceptual contribution to the study and Wayne Katon, MD (University of Washington Medical School, Department of Psychiatry and Behavioral Sciences, Seattle, Washington [deceased]) who contributed to the conceptualization and implementation of the study and will be deeply missed. None of the acknowledged individuals report conflicts of interest related to the subject of this article.
Find more articles on this and other psychiatry and CNS topics:
The Journal of Clinical Psychiatry
The Primary Care Companion for CNS Disorders
REFERENCES
1. Bassuk EL, Buckner JC, Perloff JN, et al. Prevalence of mental health and substance use disorders among homeless and low-income housed mothers. Am J Psychiatry. 1998;155(11):1561-1564. PubMed doi:10.1176/ajp.155.11.1561
2. Bassuk EL, Weinreb LF, Buckner JC, et al. The characteristics and needs of sheltered homeless and low-income housed mothers. JAMA. 1996;276(8):640-646. PubMed doi:10.1001/jama.1996.03540080062031
3. Weinreb LF, Buckner JC, Williams V, et al. A comparison of the health and mental health status of homeless mothers in Worcester, Mass: 1993 and 2003. Am J Public Health. 2006;96(8):1444-1448. PubMed doi:10.2105/AJPH.2005.069310
4. Bogard CJ, McConnell JJ, Gerstel N, et al. Homeless mothers and depression: misdirected policy. J Health Soc Behav. 1999;40(1):46-62. PubMed doi:10.2307/2676378
5. Rog D, Buckner J. Homeless Families and Children. Presented at: Toward Understanding Homelessness: The 2007 National Symposium on Homelessness Research; March 1-2, 2007; Washington, DC. https://aspe.hhs.gov/legacy-page/2007-national-symposium-homelessness-research-homeless-families-and-children-146546. Accessed January 14, 2014.
6. Zima BT, Wells KB, Benjamin B, et al. Mental health problems among homeless mothers: relationship to service use and child mental health problems. Arch Gen Psychiatry. 1996;53(4):332-338. PubMed doi:10.1001/archpsyc.1996.01830040068011
7. Nicholson J, Sweeney EM, Geller JL. Mothers with mental illness, I: the competing demands of parenting and living with mental illness. Psychiatr Serv. 1998;49(5):635-642. PubMed doi:10.1176/ps.49.5.635
8. Norquist GS, Regier DA. The epidemiology of psychiatric disorders and the de facto mental health care system. Annu Rev Med. 1996;47:473-479. PubMed doi:10.1146/annurev.med.47.1.473
9. Weinreb L, Nicholson J, Williams V, et al. Integrating behavioral health services for homeless mothers and children in primary care. Am J Orthopsychiatry. 2007;77(1):142-152. PubMed doi:10.1037/0002-9432.77.1.142
10. Thota AB, Sipe TA, Byard GJ, et al; Community Preventive Services Task Force. Collaborative care to improve the management of depressive disorders: a community guide systematic review and meta-analysis. Am J Prev Med. 2012;42(5):525-538. PubMed doi:10.1016/j.amepre.2012.01.019
11. Community Preventive Services Task Force. Recommendation from the community preventive services task force for use of collaborative care for the management of depressive disorders. Am J Prev Med. 2012;42(5):521-524. PubMed doi:10.1016/j.amepre.2012.01.010
12. Kroenke K, Spitzer RL, Williams JB. The PHQ-9: validity of a brief depression severity measure. J Gen Intern Med. 2001;16(9):606-613. PubMed doi:10.1046/j.1525-1497.2001.016009606.x
13. Kroenke K, Spitzer RL. The PHQ-9: a new depression and diagnostic severity measure. Psychiatr Ann. 2002;32(9):509-521. doi:10.3928/0048-5713-20020901-06
14. Bodenheimer T, Wagner EH, Grumbach K. Improving primary care for patients with chronic illness: the chronic care model, part 2. JAMA. 2002;288(15):1909-1914. PubMed doi:10.1001/jama.288.15.1909
15. Bodenheimer T, Wagner EH, Grumbach K. Improving primary care for patients with chronic illness. JAMA. 2002;288(14):1775-1779. PubMed doi:10.1001/jama.288.14.1775
16. Grote NK, Zuckoff A, Swartz H, et al. Engaging women who are depressed and economically disadvantaged in mental health treatment. Soc Work. 2007;52(4):295-308. PubMed doi:10.1093/sw/52.4.295
17. Spitzer RL, Kroenke K, Williams JB. Validation and utility of a self-report version of PRIME-MD: the PHQ primary care study. Primary Care Evaluation of Mental Disorders. Patient Health Questionnaire. JAMA. 1999;282(18):1737-1744. PubMed doi:10.1001/jama.282.18.1737
18. Löwe B, Un×¼tzer J, Callahan CM, et al. Monitoring depression treatment outcomes with the Patient Health Questionnaire-9. Med Care. 2004;42(12):1194-1201. PubMed doi:10.1097/00005650-200412000-00006
19. Derogatis LR, Lipman RS, Covi L. SCL-90: an outpatient psychiatric rating scale—preliminary report. Psychopharmacol Bull. 1973;9(1):13-28. PubMed
20. Williams JW Jr, Stellato CP, Cornell J, et al. The 13- and 20-item Hopkins Symptom Checklist Depression Scale: psychometric properties in primary care patients with minor depression or dysthymia. Int J Psychiatry Med. 2004;34(1):37-50. PubMed doi:10.2190/U1B0-NKWC-568V-4MAK
21. Katon W, Robinson P, Von Korff M, et al. A multifaceted intervention to improve treatment of depression in primary care. Arch Gen Psychiatry. 1996;53(10):924-932. PubMed doi:10.1001/archpsyc.1996.01830100072009
22. Foa EB, Cashman L, Jaycox L, et al. The validation of a self-report measure of posttraumatic stress disorder: the Posttraumatic Diagnostic Scale. Psychol Assess. 1997;9(4):445-451. doi:10.1037/1040-3590.9.4.445
23. Skinner HA. The Drug Abuse Screening Test. Addict Behav. 1982;7(4):363-371. PubMed doi:10.1016/0306-4603(82)90005-3
24. Yudko E, Lozhkina O, Fouts A. A comprehensive review of the psychometric properties of the Drug Abuse Screening Test. J Subst Abuse Treat. 2007;32(2):189-198. PubMed doi:10.1016/j.jsat.2006.08.002
25. Bradley KA, DeBenedetti AF, Volk RJ, et al. AUDIT-C as a brief screen for alcohol misuse in primary care. Alcohol Clin Exp Res. 2007;31(7):1208-1217. PubMed doi:10.1111/j.1530-0277.2007.00403.x
26. Ware JE, Kosinski M, Dewey JE, et al. How to Score and Interpret Single-Item Health Status Measures: A Manual for User of the SF-8 Health Survey. Lincoln, RI: Quality Metric Inc.; 2001.
27. Spitzer RL, Kroenke K, Williams JB, et al. A brief measure for assessing generalized anxiety disorder: the GAD-7. Arch Intern Med. 2006;166(10):1092-1097. PubMed doi:10.1001/archinte.166.10.1092
28. Galassi JP, Schanberg R, Ware W. The Patient Reactions Assessment: a brief measure of the quality of the patient-provider medical relationship. Psychol Assess. 1992;4(3):346-351. doi:10.1037/1040-3590.4.3.346
29. Luborsky L, McLellan AT, Woody GE, et al. Therapist success and its determinants. Arch Gen Psychiatry. 1985;42(6):602-611. PubMed doi:10.1001/archpsyc.1985.01790290084010
30. Grant R, Gracy D, Goldsmith G, et al. Twenty-five years of child and family homelessness: where are we now? Am J Public Health. 2013;103(suppl 2):e1-e10. PubMed doi:10.2105/AJPH.2013.301618
31. Bassuk EL, Beardslee WR. Depression in homeless mothers: addressing an unrecognized public health issue. Am J Orthopsychiatry. 2014;84(1):73-81. PubMed doi:10.1037/h0098949
32. Miranda J, Azocar F, Komaromy M, et al. Unmet mental health needs of women in public-sector gynecologic clinics. Am J Obstet Gynecol. 1998;178(2):212-217. PubMed doi:10.1016/S0002-9378(98)80002-1
33. Miranda J, Green BL, Krupnick JL, et al. One-year outcomes of a randomized clinical trial treating depression in low-income minority women. J Consult Clin Psychol. 2006;74(1):99-111. PubMed doi:10.1037/0022-006X.74.1.99
34. Connelly CD, Baker-Ericzen MJ, Hazen AL, et al. A model for maternal depression. J Womens Health (Larchmt). 2010;19(9):1747-1757. PubMed doi:10.1089/jwh.2009.1823
35. Weinreb L, Goldberg R, Perloff J. Health characteristics and medical service use patterns of sheltered homeless and low-income housed mothers. J Gen Intern Med. 1998;13(6):389-397. PubMed doi:10.1046/j.1525-1497.1998.00119.x
36. Castaldelli-Maia JM, Scomparini LB, Andrade AG, et al. Perceptions of and attitudes toward antidepressants: stigma attached to their use—a review. J Nerv Ment Dis. 2011;199(11):866-871. PubMed doi:10.1097/NMD.0b013e3182388950
37. Gowen LK. You’ d be depressed too: treatment acceptability among mothers who are economically disadvantaged. Focal Point. 2008;22(2):17-19.
38. Katon W, Von Korff M, Lin E, et al. Collaborative management to achieve treatment guidelines. impact on depression in primary care. JAMA. 1995;273(13):1026-1031. PubMed doi:10.1001/jama.1995.03520370068039
39. Weinreb L, Rog DJ, Henderson KA. Exiting shelter: an epidemiological analysis of barriers and facilitators for families. Soc Serv Rev. 2010;84(4):597-614. PubMed doi:10.1086/657108
40. Culhane D, Metraux S, Park JM, et al. Testing a typology of family homelessness based on patterns of public shelter utilization in four US jurisdictions: implications for policy and program planning. Housing Policy Debate. 2007;18(1):1-28. doi:10.1080/10511482.2007.9521591
41. Miranda J, Ong MK, Jones L, et al. Community-partnered evaluation of depression services for clients of community-based agencies in under-resourced communities in Los Angeles. J Gen Intern Med. 2013;28(10):1279-1287. PubMed doi:10.1007/s11606-013-2480-7
Enjoy this premium PDF as part of your membership benefits!