See related blog by Iskander and Vance.
Mental Health From the Perspective of Primary Care Residents: A Pilot Survey

ABSTRACT
Objective: Primary care physicians are increasingly providing psychiatric care in the United States. Unfortunately, there is limited learning opportunity or exposure to psychiatry during their residency training. This survey was conducted to assess primary care resident interaction with mental health professionals and their satisfaction, knowledge, preference, and comfort with the delivery of mental health care in primary health care settings.
Method: On the basis of available published literature, a 20-question survey was formulated. Following receipt of the institutional review board’s approval, these questions were sent via e-mail in February 2012 to internal and family medicine residents (N = 108) at 2 teaching hospitals in southwest Virginia. Analysis of the electronically captured data resulted in a response rate of 32%. Descriptive analysis was used to examine the results.
Results: The responses were equally divided among male and female residents and family medicine and internal medicine residents. There were several interesting findings from the survey. No correlations were noted between the gender of residents, type or location of the medical school, or having had a psychiatric rotation during residency and the reported comfort level treating patients with psychiatric illness or the desire to see psychiatric patients in the future. A positive correlation was found between the residents’ training level and their belief about the percentage of mental health providers who have mental health problems.
Conclusions: The current training model to acclimate primary care residents to the field of mental health appears to have major limitations. Results of this pilot survey can serve as a guide to conduct prospective, multicenter studies to identify and improve psychiatric training for primary care residency programs.
Prim Care Companion CNS Disord 2014;16(4):doi:10.4088/PCC.14m01662
© Copyright 2014 Physicians Postgraduate Press, Inc.
Submitted: March 26, 2014; accepted May 13, 2014.
Published online: August 28, 2014.
Corresponding author: Joseph W. Iskandar, DO, Child and Adolescent Fellow in Psychiatry, Carilion Clinic, Virginia Tech Carilion School of Medicine, 2017 S. Jefferson St, Roanoke, VA 24014 ([email protected]).
The National Prescription Audit Plus in 20011 reported that the total number of psychotropic medication prescriptions issued by primary care physicians increased by 48% compared to 1996. Moreover, they prescribed approximately 80% of all anxiolytic prescriptions, 65% of all antidepressant prescriptions, and 20% of all antipsychotic prescriptions written in the United States. Despite the provision by primary care physicians of this volume of care to psychiatric patients, most residency training programs for primary care physicians provide little or no formal instruction in psychiatry. While family medicine requires mental and behavioral health training for its residents (minimal of 4-week rotation), internal medicine does not.2 As a result, a study showed that roughly 50% of all psychiatric cases presenting in primary care go unrecognized.3
METHOD
Design
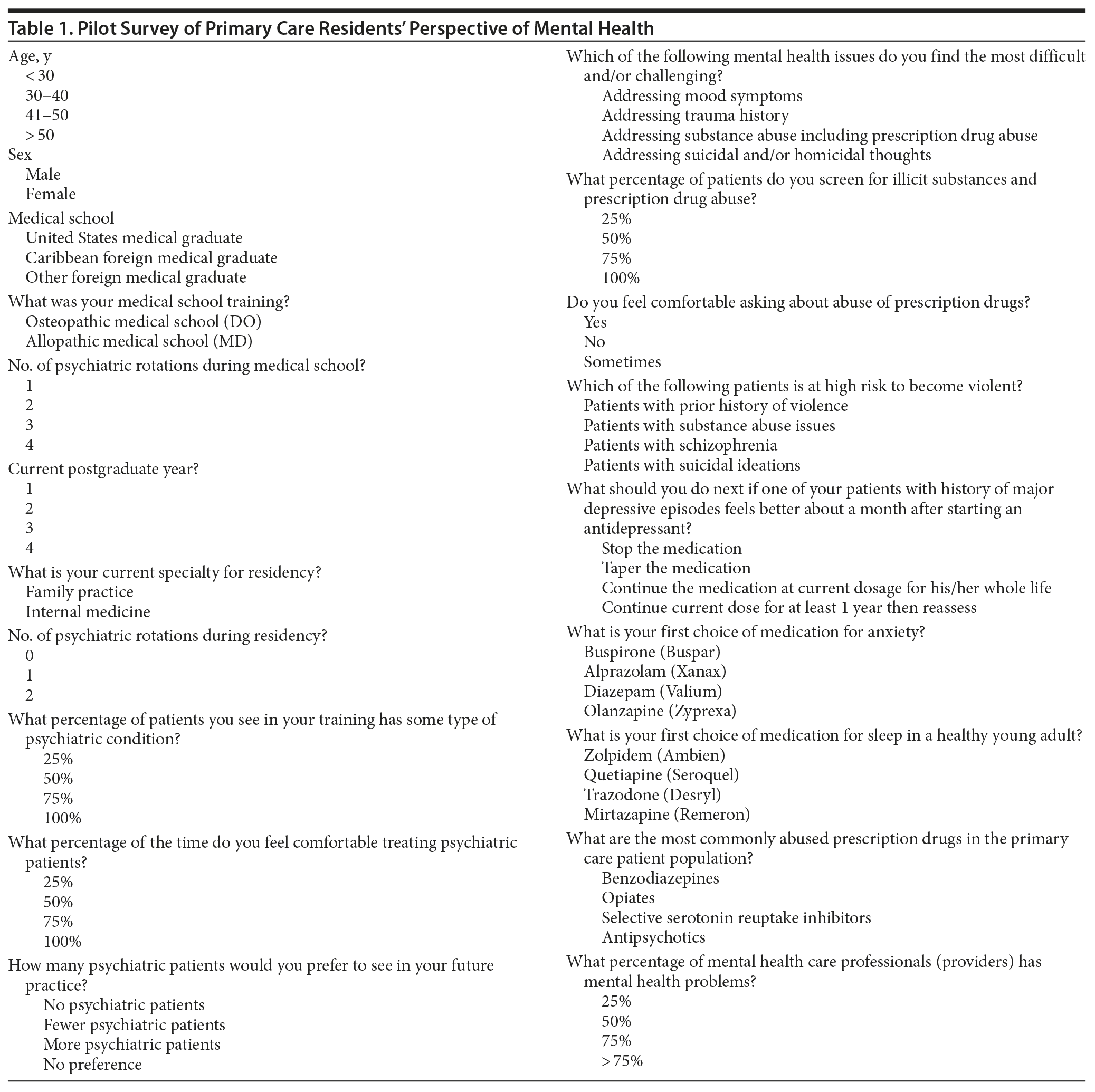
On the basis of evidence-based practice, a 20-question survey was formulated. The survey’s questions were designed to gather anonymous information about primary care residents’ demographics, training, comfort level seeing patients with mental illness, basic psychiatric knowledge, and attitudes toward mental health professionals. Following receipt of the institutional review board’s approval, these questions were transformed into an electronic form, and an electronic link was sent via e-mail in February 2012. Descriptive analysis was used to study the results. The survey questions are provided in Table 1.
Participating Sites
The survey was conducted at 2 teaching hospitals in southwest Virginia: Carilion Clinic—Virginia Tech Carilion School of Medicine Residency Programs, Roanoke (the family medicine program is allopathic and osteopathic; however, the internal medicine program is allopathic only) and Lewis Gale Medical Center Residency Programs, Salem (the family medicine and internal medicine programs are osteopathic).
Participants
The study included 2 family medicine residency programs (n = 45) and 2 internal medicine residency programs (n = 63.) The 2 family medicine residency programs and 1 internal medicine residency program (n = 16) incorporate a 4-week rotation in psychiatry; however, 1 internal medicine residency program (n = 47) does not provide any formal training in psychiatry.
RESULTS
The overall response rate was 32%, with 34 residents completing the survey. These responses were equally divided among male and female residents and between family medicine and internal medicine residents. Respondents were 60% osteopathic compared to 40% allopathic.
No correlations were noted between the gender of residents, type or location of the medical school, or having had a psychiatric rotation during residency and the reported comfort level treating patients with psychiatric illness or the desire to see psychiatric patients in the future. Half of the respondents (50%) reported feeling comfortable treating patients with psychiatric illness only 25% of the time, although 70% reported that 50% of their current patients have some type of psychiatric condition.

- The current training model to acclimate primary care residents to the field of mental health appears to have major limitations.
- Better integration and collaboration between primary care residency programs and psychiatric services are needed to improve the outcome.
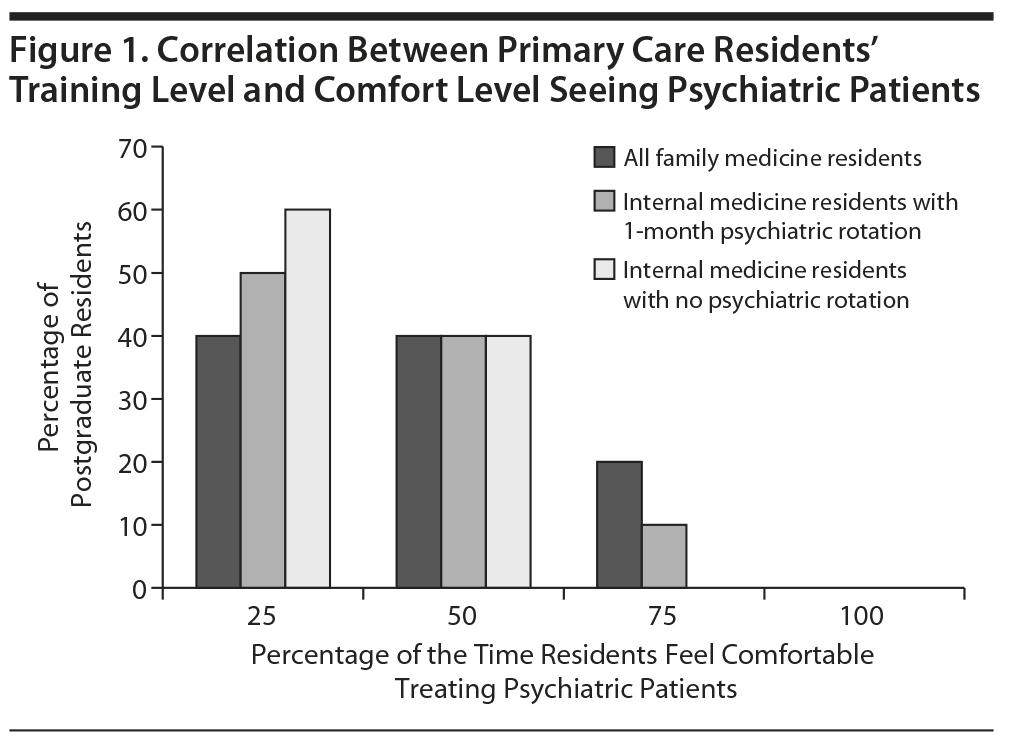
The internal medicine residents who had a 1-month rotation in psychiatry reported a minor increase in comfort level treating psychiatric patients compared to internal medicine residents who did not have a psychiatric rotation, but they did not report an increase in the desire to see psychiatric patients in their future practice. The correlation between the residents’ training level and comfort level seeing psychiatric patients is presented in Figure 1. There was no correlation between resident training level and preference to see psychiatric patients in future practice. When respondents were asked for their preference to see mental health patients in their future practice, 60% reported the preference to see fewer, 30% reported the preference to see no mental health patients, and 10% reported no preference.
Overall, 67% of the respondents demonstrated adequate basic knowledge to manage common psychiatric problems, and 90% of respondents reported feeling comfortable discussing prescription drug abuse with their patients. However, some gender differences were noted in specific mental health assessment skills. Among female residents, 59% accurately predicted patients at risk of violence compared to only 35% of male residents. On the other hand, 47% of female residents found it difficult or challenging to address suicidal or homicidal thoughts with patients compared to 24% of male residents.
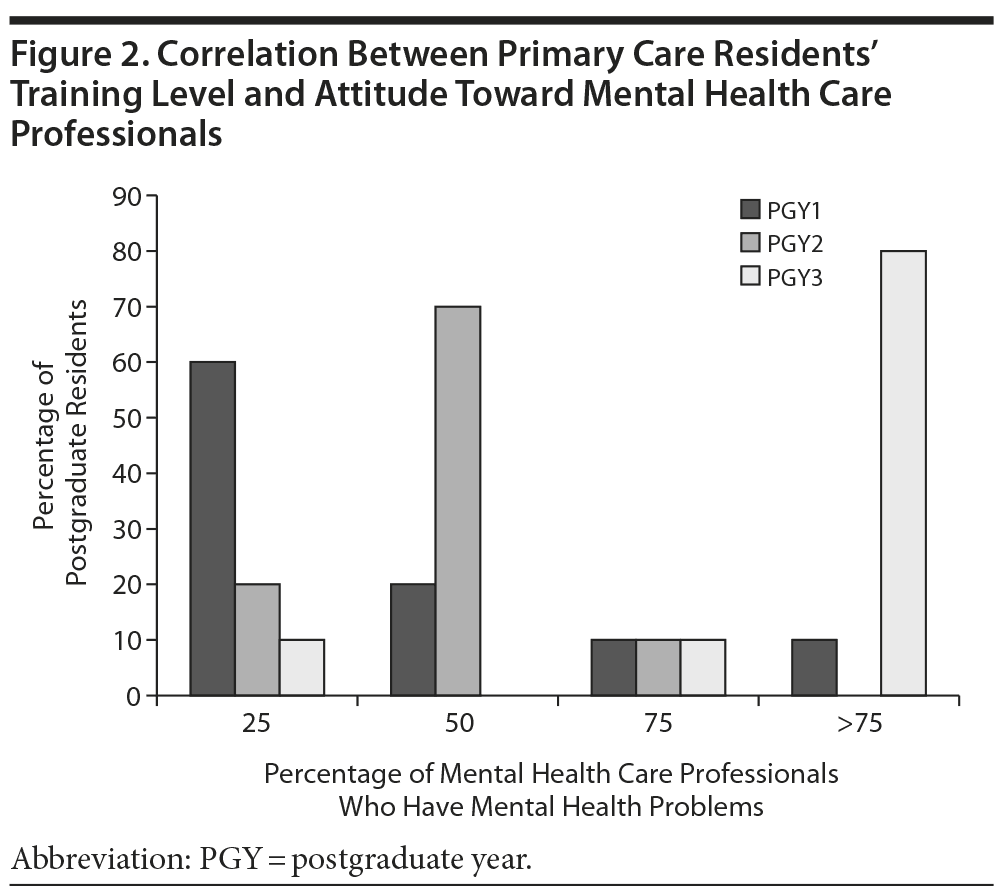
A positive correlation was found between the residents’ training level and their belief about the percentage of mental health providers who have mental health problems. Only 60% of postgraduate year 1 and 70% of year 2 residents reported a belief that 25% and 50% of mental health providers, respectively, may have mental health problems, but 80% of year 3 residents reported having a suspicion that more than 75% of mental health providers were likely to have mental health problems (Figure 2).
DISCUSSION
To the best of our knowledge, this is the first pilot survey focusing on the effects of psychiatric training on issues beyond the knowledge base of primary care residents, including their attitudes toward psychiatric patients and providers. Despite the study limitations, the survey results identify interesting observations.
The female primary care residents demonstrated better skills to assess violence risk factors compared to their male counterparts. This difference may be attributed to their vigilance in navigating the environment and their awareness of any potential physical threats while encountering a patient. A study of physician gender differences in general and cancer-specific prevention attitudes and practices showed that female gender predicted more discussion of violence prevention compared to male gender.4 On the other hand, our study demonstrates that female primary care residents struggle significantly more with addressing suicidal or homicidal thoughts with patients compared to male primary care residents (47% vs 24%, respectively). This finding is consistent with an online survey of 195 practicing primary care physicians in which female physicians reported lower self-perceived competency in the assessment and treatment of suicidality.5
Our study showed that primary care residents have extensive exposure to mental illness in the patients they see. They also demonstrated having adequate knowledge to manage common psychiatric symptoms. However, they report low comfort levels in seeing patients with mental illness in spite of frequently encountering mental illness in their patients. These results are consistent with those of multiple previous studies. Lack of adequate formal psychiatric training has been reported to be the main reason for this occurrence. It has been documented that primary care residents perceive that they are not receiving sufficient training in psychiatry.6-8 Furthermore, two-thirds of primary care residency training directors believe that their residents are not receiving sufficient training in psychiatry.7 In a national survey focusing on psychiatric training in primary care residency programs, 63% of respondents indicated that there is a need for more psychiatric exposure during training.8 The medical field’s reluctance to improve and/or increase psychiatric training in primary care resident programs is multifactorial and beyond the purpose of this study. It is encouraging that our study suggests that there is a mild increase in the level of reported comfort seeing patients with mental illness in the internal medicine residents who had 1 month of psychiatric rotation.
The stigma of and discrimination against mental illness has been acknowledged universally across cultures and settings including the workplace, general medical doctor’s offices, and psychiatric hospitals.9,10 This study confirms these findings, noting that a majority of primary care physician trainees have little interest in treating mental illness in their future practices. Perhaps more interesting was the finding that primary care residents perceive that most mental health providers suffer from mental health problems. To our knowledge, no previous evidence has been found to address this problematic attitude of primary care physicians toward their colleagues who provide treatment for patients with mental illness. It is concerning that our study showed an increase in this perception among primary care residents with increasing level of training. This finding could be explained by multiple factors that should be further investigated. Increasing exposure of trainees to psychiatric treatment during primary care residency training should lead to strengthened communication between primary care physicians and mental health providers, while improving the care provided for patients with mental illness.11,12
CONCLUSION
The current training model to acclimate primary care residents to the field of mental health appears to have major limitations, especially when we look at their reported comfort in treating patients with psychiatric illness and their attitude toward mental health patients as well as professionals specialized in mental health. Results of this pilot survey can serve as a guide to conduct prospective, multicenter studies to identify and improve psychiatric training for primary care residency programs. Improved training will not only help meet the need in mental health shortage areas but will also provide care coordination between primary care physicians and mental health professionals, while treating one of the most vulnerable patient populations.
Drug names: alprazolam (Xanax, Niravam, and others), diazepam (Diastat, Valium, and others), mirtazapine (Remeron and others), olanzapine (Zyprexa and others), quetiapine (Seroquel and others), zolpidem (Ambien, Edluar, and others).
Author affiliations: Departments of Child and Adolescent Psychiatry (Drs Iskandar and Vance) and Psychiatry (Drs Sharma and Mingoia), Carilion Clinic, Virginia Tech Carilion School of Medicine, Roanoke; Department of Family Medicine, Lewis Gale Medical Center, Salem (Dr Alishayev); and Department of Psychiatry, University of Virginia School of Medicine, Charlottesville (Dr Ali), Virginia.
Potential conflicts of interest: None reported.
Funding/support: None reported.
REFERENCES
1. IMS Health. National Prescription Audit Plus Moving Annual Total (MAT), 2001.
2. Hemming P, Loeb D. Internal medicine residents’ inadequate preparation in mental health. SGIM Forum. 2013;36(12):10-11.
3. Lieberman JA. The use of antipsychotics in primary care. Prim Care Companion J Clin Psychiatry. 2003;5(suppl 3):3-8.
4. Ramirez AG, Wildes KA, Nסpoles-Springer A, et al. Physician gender differences in general and cancer-specific prevention attitudes and practices. J Cancer Educ. 2009;24(2):85-93. PubMed doi:10.1080/08858190802664396
5. Graham RD, Rudd MD, Bryan CJ. Primary care providers’ views regarding assessing and treating suicidal patients. Suicide Life Threat Behav. 2011;41(6):614-623. PubMed doi:10.1111/j.1943-278X.2011.00058.x
6. Smith RC, Laird-Fick H, D’ Mello D, et al. Addressing mental health issues in primary care: an initial curriculum for medical residents. Patient Educ Couns. 2014;94(1):33-42. PubMed doi:10.1016/j.pec.2013.09.010
7. Primary care residents not getting sufficient training in psychiatry. Psychiatric News. October 6, 2000. http://psychnews.org/pnews/00-10-06/primary.html. Accessed May 30, 2014.
8. Chin HP, Guillermo G, Prakken S, et al. Psychiatric training in primary care medicine residency programs: a national survey. Psychosomatics. 2000;41(5):412-417. PubMed doi:10.1176/appi.psy.41.5.412
9. Kapungwe A, Cooper S, Mayeya J, et al; Mental Health and Poverty Project Research Programme Consortium. Attitudes of primary health care providers towards people with mental illness: evidence from two districts in Zambia. Afr J Psychiatry (Johannesbg). 2011;14(4):290-297. PubMed
10. Corrigan PW. Don’ t call me nuts: an international perspective on the stigma of mental illness. Acta Psychiatr Scand. 2004;109(6):403-404. PubMed doi:10.1111/j.1600-0047.2004.00316.x
11. Kates N, Craven MA, Crustolo AM, et al. Sharing care: the psychiatrist in the family physician’s office. Can J Psychiatry. 1997;42(9):960-965. PubMed
12. Lucena RJ, Lesage A. Family physicians and psychiatrists: qualitative study of physicians’ views on collaboration. Can Fam Physician. 2002;48:923-929. PubMed