Objective: To gain insight into the current prevalence of tobacco consumption in various forms among female psychiatric inpatients and their visiting female relatives in Mumbai, India.
Methods: In this cross-sectional study, survey questionnaires were administered to 127 female inpatients and 110 of their visiting female relatives from July to October 2016. A total of 100 patients and 108 of their relatives completed responses. Additionally, a modified version of the Fagerström Test for Nicotine Dependence was incorporated into the survey to assess the level of nicotine dependence, with higher scores corresponding to higher levels of dependence.
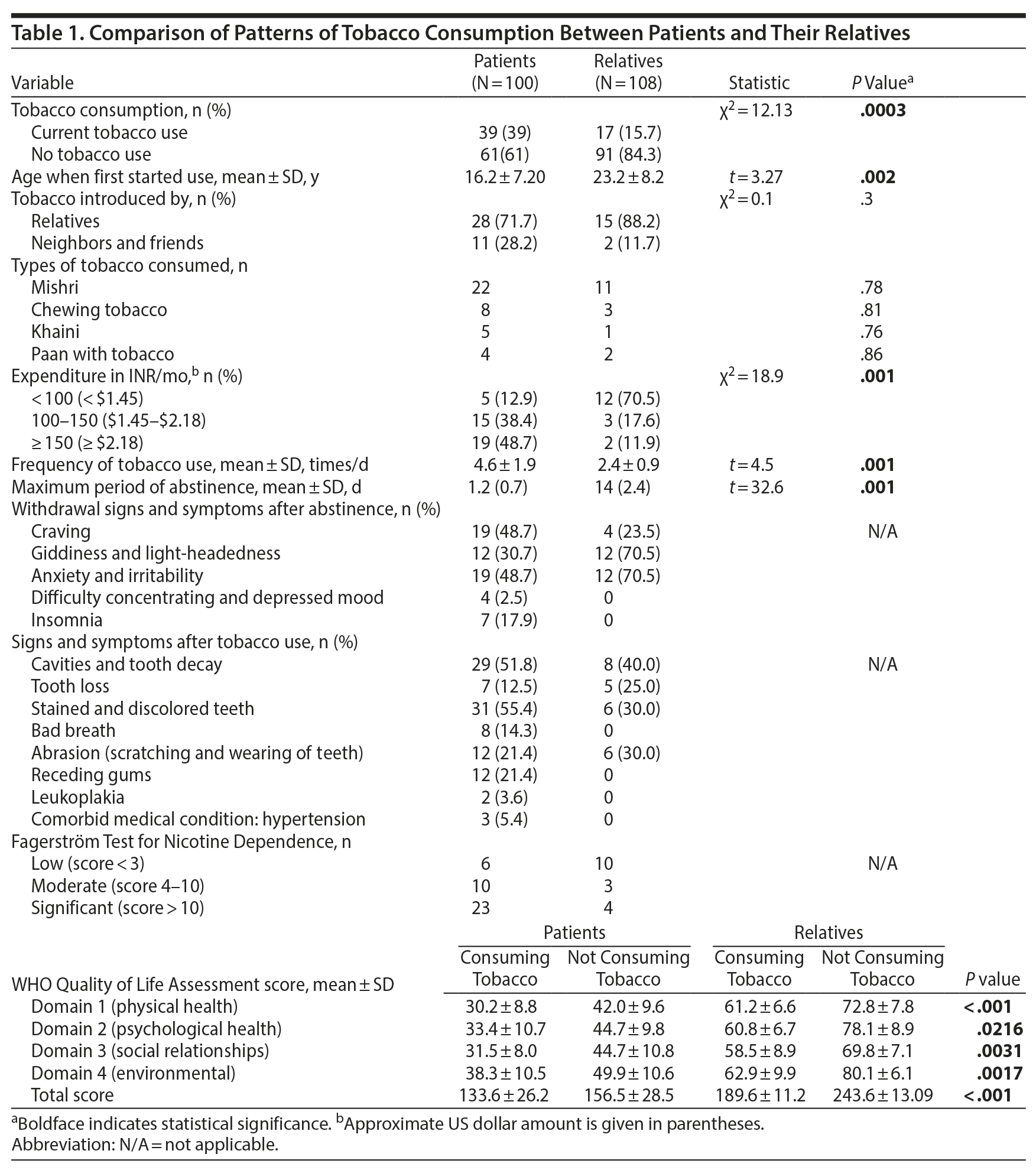
Results: The rates of tobacco use were higher in the patients than in their relatives (χ2Â =Â 12.13, PÂ =Â .0003). Patients had shorter periods of abstinence and lower World Health Organization Quality of Life Assessment parameters.
Conclusions: This study sheds light on certain data that may be utilized for future health programs and in the development of treatment plans for women with mental illness.’ ‹’ ‹
Trends of Tobacco Consumption Among Women Admitted to and Visiting the Psychiatric Inpatient Unit of a Tertiary Care Center in Mumbai:
A Cross-Sectional Study

ABSTRACT
Objective: To gain insight into the current prevalence of tobacco consumption in various forms among female psychiatric inpatients and their visiting female relatives in Mumbai, India.
Methods: In this cross-sectional study, survey questionnaires were administered to 127 female inpatients and 110 of their visiting female relatives from July to October 2016. A total of 100 patients and 108 of their relatives completed responses. Additionally, a modified version of the Fagerström Test for Nicotine Dependence was incorporated into the survey to assess the level of nicotine dependence, with higher scores corresponding to higher levels of dependence.
Results: The rates of tobacco use were higher in the patients than in their relatives (χ2 = 12.13, P = .0003). Patients had shorter periods of abstinence and lower World Health Organization Quality of Life Assessment parameters.
Conclusions: This study sheds light on certain data that may be utilized for future health programs and in the development of treatment plans for women with mental illness.
Prim Care Companion CNS Disord 2019;21(3):18m02422
To cite: Sharma P, Virani S, Mitra S, et al. Trends of tobacco consumption among women admitted to and visiting the psychiatric inpatient unit of a tertiary care center in Mumbai: a cross-sectional study. Prim Care Companion CNS Disord. 2019;21(3):18m02422.
To share: https://doi.org/10.4088/PCC.18m02422
© Copyright 2019 Physicians Postgraduate Press, Inc.
aDepartment of Psychiatry, Lokmanya Tilak Medical College, Sion, Mumbai
bDepartment of Psychiatry, Maimonides Medical Center, Brooklyn, New York
cDepartment of Psychiatry, Bronxcare Health System, Bronx, New York
dDepartment of Psychiatry, Nassau University Medical Center, East Meadow, New York
*Corresponding author: Souparno Mitra, MD, Department of Psychiatry, Bronxcare Health System, 1276 Fulton Ave, Bronx, NY 10456 ([email protected]).
Widespread tobacco consumption is known to result in poor health outcomes and significant economic loss, as corroborated by the US Surgeon General’s report in 2014.1 Per a report from the World Health Organization (WHO),2 approximately 80% of the world’s 1.1 billion smokers live in low- and middle-income countries. Low-income countries, as defined by the World Bank,3 are countries with a gross national income less than $995. Middle-income countries are those with a gross national income less than $12,055. In 2015, it was also noted that the poorest countries were the worst hit by the growing number of deaths from tobacco consumption and stifling economic development.4 It has been theorized that in lower-income Asian and African countries, underreporting and lack of reliable data often lead to underestimation of the magnitude of the issue.5 The pattern of tobacco use in India especially has not been well studied over the past decade, particularly in relation to the demographic characteristics of its vast population.6 Researchers7reported in 2005 that compared to men, Indian women were much less likely to smoke tobacco (3.4% vs 33.3%), chew tobacco (13.0% vs 29.0%), and use tobacco in both forms (15.5% vs 50.2%). According to WHO estimates reported in 2006,8 194 million men and 45 million women use tobacco in smoke or smokeless form in India. Specifically, this estimate consisted of 68.9 million smokers (users of cigarettes, beedi, hookahs, cigars, and pipes), 163.7 million smokeless users (chewing smokeless tobacco), and 42.3 million users of both products.8 Tobacco is available in smokeless form for consumption in India mainly by chewing as paan masala, mawa, khaini, mishri, gul, bajjar, lal dant manjan, and gudhaku. Paan masala is a commercial preparation containing areca nut, slaked lime, catechu, and condiments with or without powdered tobacco.9 Mawa is prepared by mixing small pieces of areca nut, processed tobacco, and slaked lime. Khaini is a mixture of sun-dried tobacco and slaked lime that is widespread in Maharashtra and several states of north India. Mishri is a roasted, powdered preparation made by baking tobacco on a hot metal plate until it is uniformly black. Gul is a pyrolyzed tobacco product used as a dentifrice in the eastern part of India. Bajjar is dry snuff (also known as tapkeer) applied commonly by women in Gujarat on the teeth and gums. Lal dant manjan is a dentifrice10—a red-colored tooth powder containing tobacco. Gudhaku is a paste made of tobacco and molasses.11
According to a report from the Centre for Addiction and Mental Health,12 people diagnosed with a psychiatric disorder or a substance use disorder are 2 to 4 times more likely to smoke than those in the general population. Smoking has been reported to be 2 to 3 times more prevalent among people with mental illness compared with the general population in Australia, the United States, and the United Kingdom.13,14 When assessed by psychiatric diagnoses, smoking prevalence is particularly high (almost 5-fold greater) among those with schizophrenia, bipolar disorder, posttraumatic stress disorder (PTSD), and alcohol/illicit drug use disorders. Up to 88% of people with schizophrenia and 82.5% of people with bipolar disorder smoke.15 Furthermore, studies16 have reported that smoking cessation is known to have a positive impact on mood and improve the quality of life. To glean some insight into the current prevalence of tobacco consumption in various forms, we conducted a cross-sectional study of female patients and their visiting female relatives at an inpatient psychiatric unit at one of the largest tertiary care centers in Mumbai, India. In this article, we discuss how the results from our study compare with those of previous studies and the general population and point out the implications for the individual’s quality of life and in the broader context of clinical practice.
METHODS
Introduction
Survey questionnaires were administered to 127 female patients admitted to the inpatient psychiatric unit and 110 of their visiting female relatives in 2016. A total of 100 patients and 108 of their relatives completed responses. The study was approved by the hospital ethics committee, and written informed consent was obtained prior to participation in the study.

- Tobacco consumption among women in India is underreported and underestimated due to sociocultural barriers.
- Physicians should incorporate screening for tobacco consumption in the treatment of all patients with mental illness.
- Screening for tobacco consumption should be comprehensive as well as culturally sensitive, and smoking policies should be standardized for inpatient psychiatric units.
Selection of Study Groups
The study was conducted from July to October 2016. All female patients admitted to the inpatient psychiatric unit with a diagnosed DSM-5 psychiatric condition were considered for the study. As healthy controls, female relatives who visited these patients were also requested to participate if they were willing. All patients irrespective of their caste, socioeconomic status, geographical region, or insurance status were given the opportunity to participate in the study.
New patients admitted to the psychiatric unit were administered the questionnaire after they were stabilized. Psychotic and delusional patients were stabilized and, once found to be lucid, were asked to participate in the study.
Setting
Patients were chosen from the inpatient psychiatry unit of a tertiary care hospital. The tertiary care hospital had no restrictions for admissions on any grounds. All patients admitted to the unit were given the opportunity to participate in the study. On the unit, patients had access to tobacco and tobacco products as provided by their visitors. The unit had common areas wherein patients could smoke if they wished. However, most patients chewed tobacco and continued to do so in their rooms.
Measures
We designed a questionnaire to assess the participants’ past and current patterns of tobacco consumption via various measures such as frequency, quantity, form, amount of money spent, health hazards experienced if any, and symptoms of withdrawal. These questions are provided in Figure 1. The questionnaire was administered by the medical staff assisting in translation and interpretation of questions.
Additionally, a modified version of the Fagerström Test for Nicotine Dependence17 was incorporated into the survey to assess the level of nicotine dependence, with higher scores corresponding to higher levels of dependence. Specifically, the modifications comprised redefining the focus of 6 of the scale items to assess the number of tins or pouches of tobacco chewed per week, time of first use, difficulty refraining from chewing, frequency of use, and chewing when ill. Finally, over a period of 2 weeks prior to survey administration, questions from the WHO Quality of Life Assessment18 were utilized to assess experiences related to physical, psychological, and social relationships and the environment as well as overall quality of life and general health. Physical signs of tobacco use were assessed by the duty medical officer of the unit after patients had responded to the questionnaire.
Data Analysis
Data obtained from both groups were analyzed using the Statistical Package for the Social Sciences (SPSS; IBM Corp, Armonk, New York) and compared to draw conclusions. The two groups were compared for statistically significant differences as shown in Table 1.
RESULTS
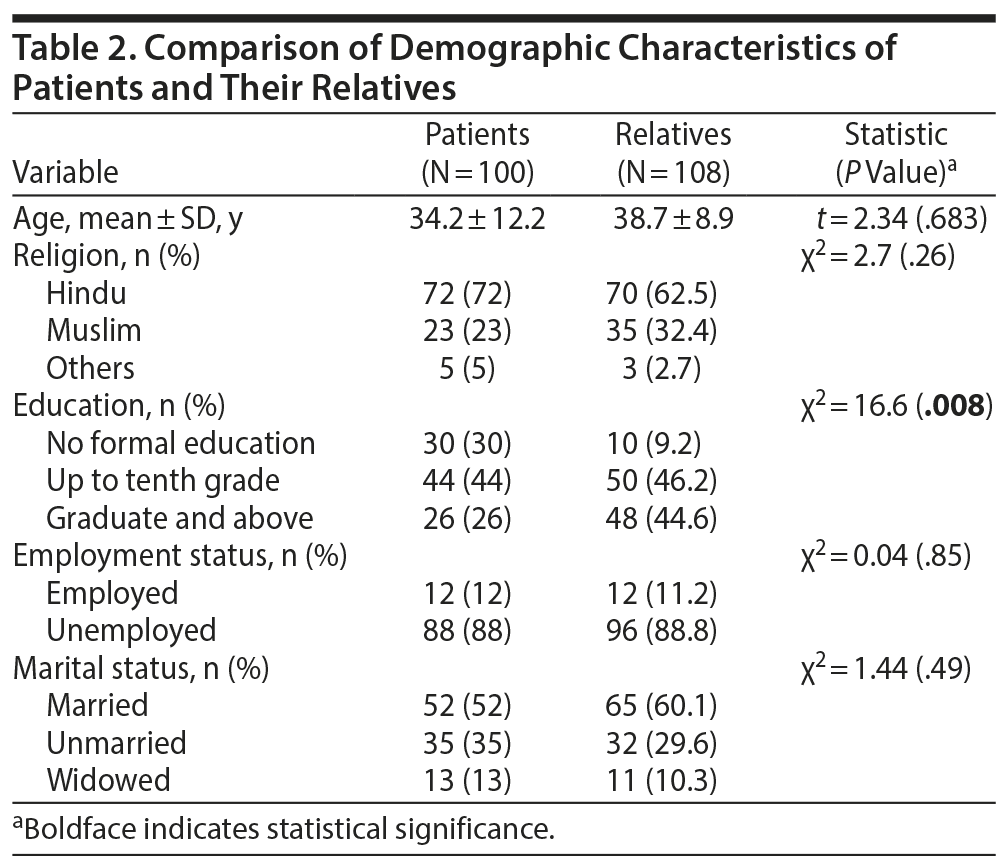
Demographic characteristics of the patient and relative groups are compared in Table 2. The female patients and their female relatives differed significantly on education levels, but both groups were comparable on other demographic parameters. The most common psychiatric diagnoses of the patients included schizophrenia and other psychotic disorders (40%), major depressive disorder (36%), bipolar disorder (10%), alcohol use disorder (3%), conversion disorder (6%), and major neurocognitive disorders (5%), with some having dual diagnoses.
The rates of tobacco use were higher in patients than their relatives (χ2 = 12.13, P = .0003). The study also showed shorter periods of abstinence (t = 32.6, P = .001) and lower levels of education (χ2 = 16.6, P = .008) among patients versus their relatives. Patients had lower WHO Quality of Life Assessment parameters (total score: 133.6 ± 26.2 among patients who are smokers versus 243.6 ± 13.09 among relatives who were nonsmokers, P < .001) and greater consumption amounts (t = 4.5, P = .001) compared to their relatives.
Patients and their relatives differed significantly (P = .002) in the age at onset of tobacco consumption. Smokeless tobacco was found to be popular, and, interestingly, none of the patients or their relatives used tobacco in the form of cigarettes, beedi, or hookah. Significantly more patients compared to their female relatives were addicted to nicotine.
DISCUSSION
This study sheds light on certain data that may be utilized for future health programs and development of treatment plans for women with mental illness. The statistics found in this study are higher than the rates of tobacco usage reported in the Global Adult Tobacco Survey.19 This higher rate may be due to the differences in local characteristics of the patients in our study compared to that of the population studied in the Global Adult Tobacco Survey. Studies20 have shown associations between socioeconomic status and tobacco use, and this may, in part, contribute to the rates found in our study. Studies have also found that self-reporting of tobacco, especially among youth in India, has low sensitivity.
Screening for tobacco use, especially among this patient population, is a necessity, as the association between mental illness and tobacco-related morbidity and mortality is well researched.21,22 Inpatient units may develop smoke-free policies or designated smoking areas to enable patients with nicotine use disorder to manage their nicotine addiction.
Potential limitations of the study include the use of a single-point source and the lack of universal smoking policies for patients admitted to the unit. This study indicates a need for well-validated studies to estimate the accurate epidemiology of nicotine use among not just female patients but all patients with mental illness in India. The results of these studies will enable psychiatrists to gauge the prevalence of comorbid mental illness and nicotine use and develop comprehensive treatment plans.
Submitted: December 12, 2018; accepted February 4, 2019.
Published online: May 2, 2019.
Potential conflicts of interest: None.
Funding/support: None.
REFERENCES
1. US Department of Health and Human Services. The Health Consequences of Involuntary Exposure to Tobacco Smoke: A Report of the Surgeon General. Atlanta, GA: US Department of Health and Human Services, Centers for Disease Control and Prevention, Coordinating Center for Health Promotion, National Center for Chronic Disease Prevention and Health Promotion, Office on Smoking and Health; 2006
2. World Health Organization. Research for International Tobacco Control. WHO Report on the Global Tobacco Epidemic, 2008: the MPOWER Package. World Health Organization; 2008.
3. World Bank. World Bank Country and Lending Groups. World Bank Atlas Method. World Bank website. https://datahelpdesk.worldbank.org/knowledgebase/articles/906519-world-bank-country-and-lending-groups. Accessed April 4, 2019.
4. Boutayeb A, Boutayeb S. The burden of non communicable diseases in developing countries. Int J Equity Health. 2005;4(1):2. PubMed CrossRef
5. Khattab A, Javaid A, Iraqi G, et al; BREATHE Study Group. Smoking habits in the Middle East and North Africa: results of the BREATHE study. Respir Med. 2012;106(suppl 2):S16-S24. PubMed CrossRef
6. Gajalakshmi V, Peto R, Kanaka TS, et al. Smoking and mortality from tuberculosis and other diseases in India: retrospective study of 43,000 adult male deaths and 35,000 controls. Lancet. 2003;362(9383):507-515. PubMed CrossRef
7. Chandra PS, Carey MP, Carey KB, et al. Prevalence and correlates of tobacco use and nicotine dependence among psychiatric patients in India. Addict Behav. 2005;30(7):1290-1299. PubMed CrossRef
8. Reddy KS, Gupta PC. Tobacco Control in India. New Delhi, India: Ministry of Health and Family Welfare, Government of India; 2004.
9. Shimkhada R, Peabody JW. Tobacco control in India. Bull World Health Organ. 2003;81(1):48-52. PubMed
10. Agrawal SS, Ray RS. Nicotine contents in some commonly used toothpastes and toothpowders: a present scenario. J Toxicol. 2012;2012:237506. PubMed
11. Neufeld KJ, Peters DH, Rani M, et al. Regular use of alcohol and tobacco in India and its association with age, gender, and poverty. Drug Alcohol Depend. 2005;77(3):283-291. PubMed CrossRef
12. The Centre for Addiction and Mental Health. Mental Illness & Smoking. Key Messages for Health Care Providers and Policy Makers. https://www.nicotinedependenceclinic.com/English/teach/SiteAssets/Pages/Smoking-Fact-Sheets2/Mental%20Illness%20and%20Smoking%20Fact%20Sheet%20for%20Healthcare%20Providers.pdf. Accessed April 3, 2019.
13. Pirie K, Peto R, Reeves GK, et al; Million Women Study Collaborators. The 21st century hazards of smoking and benefits of stopping: a prospective study of one million women in the UK. Lancet. 2013;381(9861):133-141. PubMed CrossRef
14. Bunnell RE, Agaku IT, Arrazola RA, et al. Intentions to smoke cigarettes among never-smoking US middle and high school electronic cigarette users: National Youth Tobacco Survey, 2011-2013. Nicotine Tob Res. 2015;17(2):228-235. PubMed CrossRef
15. Weaver TL, Etzel JC. Smoking patterns, symptoms of PTSD and depression: preliminary findings from a sample of severely battered women. Addict Behav. 2003;28(9):1665-1679. PubMed CrossRef
16. Taylor G, McNeill A, Girling A, et al. Change in mental health after smoking cessation: systematic review and meta-analysis. BMJ. 2014;348(1):g1151. PubMed CrossRef
17. Heatherton TF, Kozlowski LT, Frecker RC, et al. The Fagerström Test for Nicotine Dependence: a revision of the Fagerstrom Tolerance Questionnaire. Br J Addict. 1991;86(9):1119-1127. PubMed CrossRef
18. Group TW. The World Health Organization Quality of Life Assessment (WHOQOL): development and general psychometric properties. Soc Sci Med. 1998;46(12):1569-1585. PubMed CrossRef
19. World Health Organization. GATS 2: Global Adult Tobacco Survey Fact Sheet/India 2016-2017. https://www.who.int/tobacco/surveillance/survey/gats/GATS_India_2016-17_FactSheet.pdf. Accessed April 3, 2019.
20. Corsi DJ, Subramanian SV. Divergent socio-economic gradients in smoking by type of tobacco use in India. Int J Tuberc Lung Dis. 2014;18(1):122-124. PubMed CrossRef
21. Bandiera FC, Anteneh B, Le T, et al. Tobacco-related mortality among persons with mental health and substance abuse problems. PLoS One. 2015;10(3):e0120581. PubMed CrossRef
22. Mendelsohn CP, Kirby DP, Castle DJ. Smoking and mental illness: an update for psychiatrists. Australas Psychiatry. 2015;23(1):37-43. PubMed CrossRef
Please sign in or purchase this PDF for $40.00.