Bipolar disorder, while commonly encountered in the primary care setting, is often misdiagnosed or undiagnosed. In the DSM-IV-TR, patients could be diagnosed as being in a mixed state only if they had concurrent manic and depressive symptoms; while this occurs in some patients, many more experience subsyndromal mixed symptoms that would disqualify a “mixed state” diagnosis. The recently released DSM-5 attempts to capture this large proportion of patients with subsyndromal mixed symptoms with the inclusion of the “mixed specifier.” The presence of such subsyndromal mixed symptoms has significant implications for both diagnosis and treatment. For those presenting with major depressive disorder with subsyndromal manic symptoms, clinicians must be vigilant for the development of full-blown bipolar disease. In treating this group, selective serotonin reuptake inhibitors and serotonin-norepinephrine reuptake inhibitors remain first-line therapy, but augmentation with other therapies is often required. If a diagnosis of bipolar disorder is confirmed and the patient is experiencing a depressive phase, traditional antidepressants should be avoided. For those presenting with mania and mixed depressive symptoms, treatment with a combination of atypical antipsychotics and mood stabilizers is best.
This CME activity is expired. For more CME activities, visit CMEInstitute.com.
Find more articles on this and other psychiatry and CNS topics:
The Journal of Clinical Psychiatry
The Primary Care Companion for CNS Disorders

CME Background
Articles are selected for credit designation based on an assessment of the educational needs of CME participants, with the purpose of providing readers with a curriculum of CME articles on a variety of topics throughout each volume. Activities are planned using a process that links identified needs with desired results.
To obtain credit, read the article, correctly answer at least 70% of the questions in the Posttest, and complete the Evaluation. The Posttest and Evaluation are available at http://www.cmeinstitute.com/activities/Pages/default.aspx#cmefrompcc.
CME Objective
After studying this article, you should be able to:
• Diagnose and treat patients with a manic/hypomanic or major depressive episode with a mixed features specifier
Accreditation Statement
The CME Institute of Physicians Postgraduate Press, Inc., is accredited by the Accreditation Council for Continuing Medical Education to provide continuing medical education for physicians.
Credit Designation
The CME Institute of Physicians Postgraduate Press, Inc., designates this journal-based CME activity for a maximum of 1.0 AMA PRA Category 1 Creditâ„¢. Physicians should claim only the credit commensurate with the extent of their participation in the activity.
Note: The American Academy of Physician Assistants (AAPA) accepts certificates of participation for educational activities certified for AMA PRA Category 1 Creditâ„¢ from organizations accredited by ACCME or a recognized state medical society. Physician assistants may receive a maximum of 1.0 hour of Category I credit for completing this program.
Date of Original Release/Review
This educational activity is eligible for AMA PRA Category 1 Creditâ„¢ through April 30, 2017. The latest review of this material was March 2014.
Financial Disclosure
All individuals in a position to influence the content of this activity were asked to complete a statement regarding all relevant personal financial relationships between themselves or their spouse/partner and any commercial interest. The CME Institute has resolved any conflicts of interest that were identified. In the past year, Larry Culpepper, MD, MPH, Editor in Chief, has been a consultant for Forest, Lundbeck, Merck, Sunovion, and Takeda. No member of the CME Institute staff reported any relevant personal financial relationships. Faculty financial disclosure appears with the article.
Mixed Specifier for Bipolar Mania and Depression: Highlights of DSM-5 Changes and Implications for Diagnosis and Treatment in Primary Care
ABSTRACT
Bipolar disorder, while commonly encountered in the primary care setting, is often misdiagnosed or undiagnosed. In the DSM-IV-TR, patients could be diagnosed as being in a mixed state only if they had concurrent manic and depressive symptoms; while this occurs in some patients, many more experience subsyndromal mixed symptoms that would disqualify a “mixed state” diagnosis. The recently released DSM-5 attempts to capture this large proportion of patients with subsyndromal mixed symptoms with the inclusion of the “mixed specifier.” The presence of such subsyndromal mixed symptoms has significant implications for both diagnosis and treatment. For those presenting with major depressive disorder with subsyndromal manic symptoms, clinicians must be vigilant for the development of full-blown bipolar disease. In treating this group, selective serotonin reuptake inhibitors and serotonin-norepinephrine reuptake inhibitors remain first-line therapy, but augmentation with other therapies is often required. If a diagnosis of bipolar disorder is confirmed and the patient is experiencing a depressive phase, traditional antidepressants should be avoided. For those presenting with mania and mixed depressive symptoms, treatment with a combination of atypical antipsychotics and mood stabilizers is best.
Prim Care Companion CNS Disord 2014;16(2):doi:10.4088/PCC.13r01599
© Copyright 2014 Physicians Postgraduate Press, Inc.
Submitted: October 13, 2013; accepted November 11, 2013.
Published online: April 17, 2014.
Corresponding author: Jia Hu, MD, Mood Disorders Psychopharmacology Unit, University of Toronto, 399 Bathurst St, MP 9-325, Toronto, Ontario MST 258 Canada ([email protected]).
Bipolar disorder is a debilitating yet common illness, with lifetime prevalence estimates in the United States of 1.0% for bipolar I and 1.1% for bipolar II.1 While frequently encountered in the primary care setting, bipolar disorder can be particularly challenging to diagnose. For example, it is reported that only 20% of individuals with bipolar disorder presenting to their primary care provider are correctly diagnosed within the first year,2 with an average time from onset of clinically significant symptoms to the establishment of the correct diagnosis ranging from 5 to 10 years.3 The diagnostic delay in bipolar disorder is associated with greater symptomatic burden, decreased quality of life,4 higher economic costs, increased health care service utilization, and increased risk for self-harm and suicidality.2,5
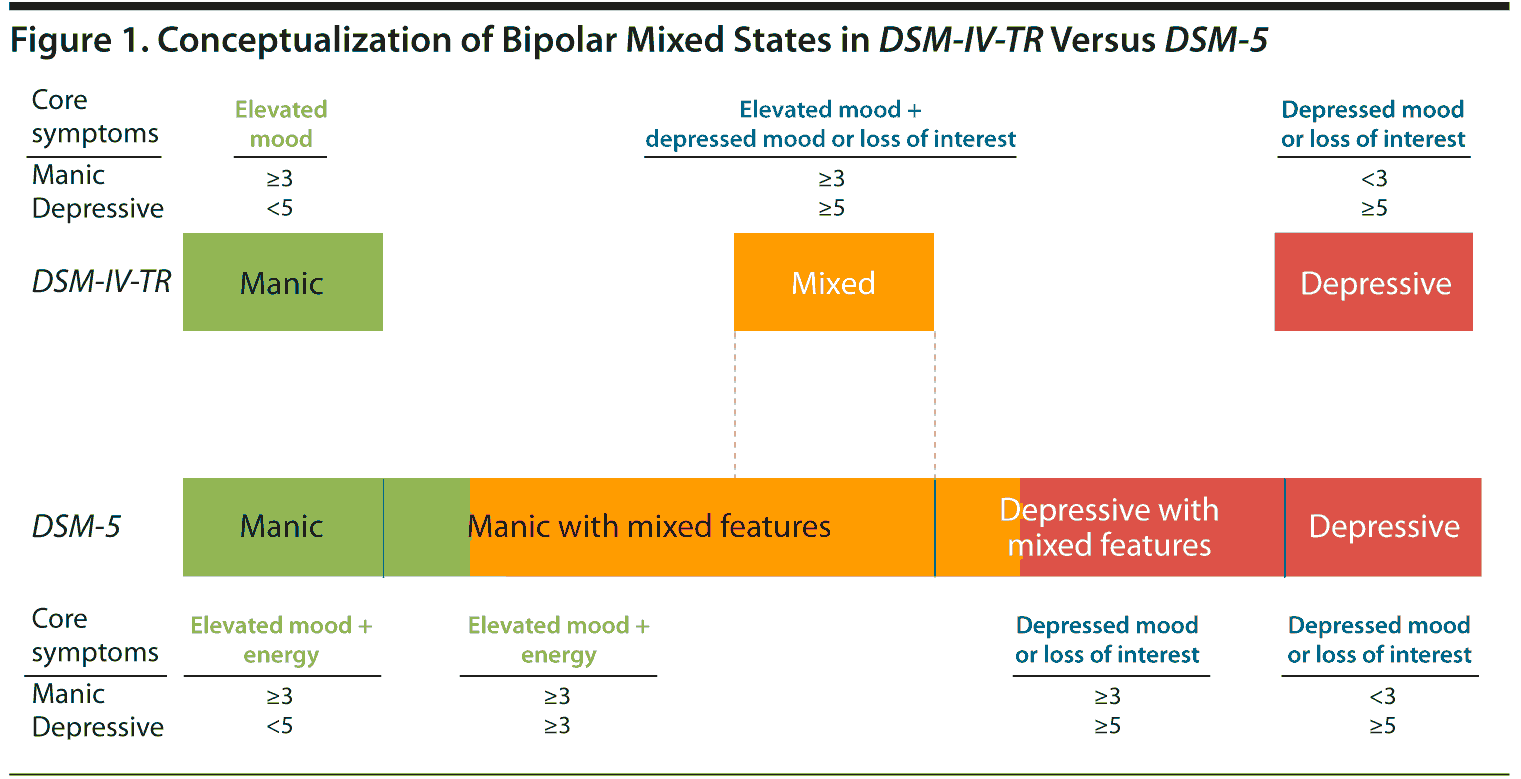
One significant contributor to diagnostic delay in bipolar disorder is the heterogeneous presentation, wherein affected individuals frequently present without classic manic symptoms. For example, a common clinical presentation of bipolar disorder is the “mixed state”: the contemporaneous presence of both manic and depressive symptoms. The DSM-5 has defined mixed states very differently from the categorical concurrence of syndrome mania and depression that appeared in the DSM-IV-TR. In the latter, one could be in a mixed state only if they met full criteria for a major depressive and a manic episode for ≥ 1 week—a definition that did not allow for the significant percentage of patients with subsyndromal mixed states. Such a narrow definition of a mixed state presentation has contributed to the misdiagnosis and consequently inappropriate treatment (ie, initiation with antidepressant rather than mood-stabilizing agents) of those with bipolar disorder.6,7 In an effort to improve identification and proper differentiation of mood disorders, the DSM-5, released in May 2013, proposed the inclusion of a “mixed features” specifier that takes into account the existence of subsyndromal, yet clinically significant, mixed states.
SUMMARY OF THE MIXED FEATURES SPECIFIER
Manic or Hypomanic Episode With Mixed Features
The DSM-5 criteria for both manic and hypomanic episodes remain the same as the DSM-IV-TR criteria with a few significant revisions. The phrase “abnormally and persistently increased energy and activity” has been added as a criteria A symptom. This edit in essence narrowed the definition for mania and hypomania. Furthermore, a manic or hypomanic episode that emerges during antidepressant treatment but persists at a fully syndromal level beyond the physiologic effect of the treatment is sufficient evidence to diagnose a manic or hypomanic episode. To qualify as having a manic or hypomanic episode with mixed features, one must also have at least 3 of the symptoms during the majority of the days of the current or most recent episode of mania/hypomania:

- Bipolar disorder is often undiagnosed, and patients will often present with subsyndromal mixed states.
- It is important to ask patients with major depressive disorder if they have manic symptoms, as this symptom has significant diagnostic and therapeutic implications.
- Atypical antipsychotics and mood-stabilizing agents can be helpful in the treatment of both depression with mixed symptoms and mania with mixed symptoms.
- Prominent dysphoria or depressed mood as indicated by either subjective report (eg, feels sad or empty) or observation made by others (eg, appears tearful).
- Diminished interest or pleasure in all, or almost all, activities (as indicated by either subjective account or observation made by others).
- Psychomotor retardation nearly every day (observable by others, not merely subjective feelings of being slowed down).
- Fatigue or loss of energy.
- Feeling of worthlessness or excessive or inappropriate guilt (not merely self-reproach or guilt about being sick).
- Recurrent thoughts of death (not just fear of dying), recurrent suicidal ideation without a specific plan, or a suicide attempt or a specific plan for committing suicide.8(pp 149,150)
For patients who meet full criteria for both a manic and depressive episode simultaneously (the DSM-IV-TR mixed episode definition), the diagnosis should be manic episode with mixed features.
Depressive Episode With Mixed Features
There are no changes in the DSM-5 from the DSM-IV-TR definition of a major depressive episode. To be diagnosed as having a major depressive episode with mixed features, one must also have at least 3 of the manic or hypomanic symptoms during the majority of days of the current or most recent episode of depression:
- Elevated, expansive mood.
- Inflated self-esteem or grandiosity.
- More talkative than usual or pressure to keep talking.
- Flight of ideas or subjective experience that thoughts are racing.
- Increase in energy or goal-directed activity (socially, at work or school, or sexually).
- Increased or excessive involvement in activities that have a high potential for painful consequences (eg, engaging in unrestrained buying sprees, sexual indiscretions, or foolish business investments).
- Decreased need for sleep (feeling rested despite sleeping less than usual, to be contrasted with insomnia).8(p150)
The DSM-5 explicitly states that mixed features associated with a major depressive episode have been found to be a significant risk factor for the development of bipolar I or II disorder and that such features should be noted in planning and monitoring the response to treatment. Ultimately, the changes from the DSM-IV-TR to the DSM-5 represent a shift in the conceptualization of bipolar disorder from one of discrete categories (ie, depressed, manic) to a more commonly encountered dimensional spectrum of symptomatology (Figure 1).
IMPLICATIONS FOR DIAGNOSIS
Bipolar disorder is often misdiagnosed as major depressive disorder; several studies have reported that approximately 25%-50% of patients presenting to a health care provider in primary care with a major depressive episode may have bipolar disorder.9,10 survey11 conducted of 4,192 patients diagnosed with bipolar disorder found 69% were previously misdiagnosed and that a mean number of 4 physicians were consulted before the appropriate diagnosis was made. Delay in diagnosis is also a significant problem—in the same survey, approximately one-third of patients waited up to a mean of 10 years before the correct diagnosis was made.11
It is vital that primary care practitioners consider bipolar disorder in the differential when patients present with depressive symptoms. The introduction of the mixed features specifier acknowledges the existence of highly prevalent subsyndromal mixed states not captured in the DSM-IV-TR and can contribute to the detection of bipolar disorder. For instance, studies have shown that up to 40% of major depressive episodes are accompanied by 1 or more hypomanic symptoms.12 By explicitly acknowledging that mixed features are prevalent, primary care practitioners should endeavor to identify manic symptoms in all patients that present with a major depressive episode.
Patients found to have mixed symptoms while depressed warrant closer monitoring and follow-up. While those with a major depressive episode with mixed features are still considered to have major depressive disorder and not bipolar disorder, the presence of subsyndromal manic symptoms is a phenotypic indicator for the later declaration of syndromal bipolar disorder. A 2009 study13 that screened patients initially diagnosed with major depressive disorder for the presence of manic symptoms reported that each additional manic symptom led to a 24% increased chance of a diagnosis of bipolar disorder. Mixed symptoms should not be considered pathognomonic of bipolar disorder, but instead represent a risk factor that must be considered in conjunction with other clinical features. Furthermore, the presence of mixed symptoms in major depressive disorder tends to be associated with rapid cycling, increased suicidality (61% more than those without any mixed symptoms), and a greater incidence of substance abuse.14
IMPLICATIONS FOR TREATMENT
It is generally recognized that patients with a mixed presentation tend to have a poorer response to pharmacotherapy than do those with pure episodes and that combination therapy is often required in such patients.15 It is important for primary care practitioners to recognize that those with mixed states are often more therapeutically challenging, as this can inform the choice and duration of medications and will also guide when a referral to psychiatry will be made. Patients with mania and mixed depressive symptoms have an increased risk of developing subsequent affective episodes. Similarly, patients with primarily depressive bipolar disorder with mixed manic symptoms are more likely to have more complex illness presentation, unfavorable course and outcome, and a poorer treatment course. The challenges in treating patients with mixed states are further complicated by the risk of mood-switching from the need to treat both manic and depressive symptoms. Medications designed to treat primarily manic symptoms can increase the risk of switching to depression.16 Similarly, antidepressant medications can induce a switch to mania in patients with depression.17
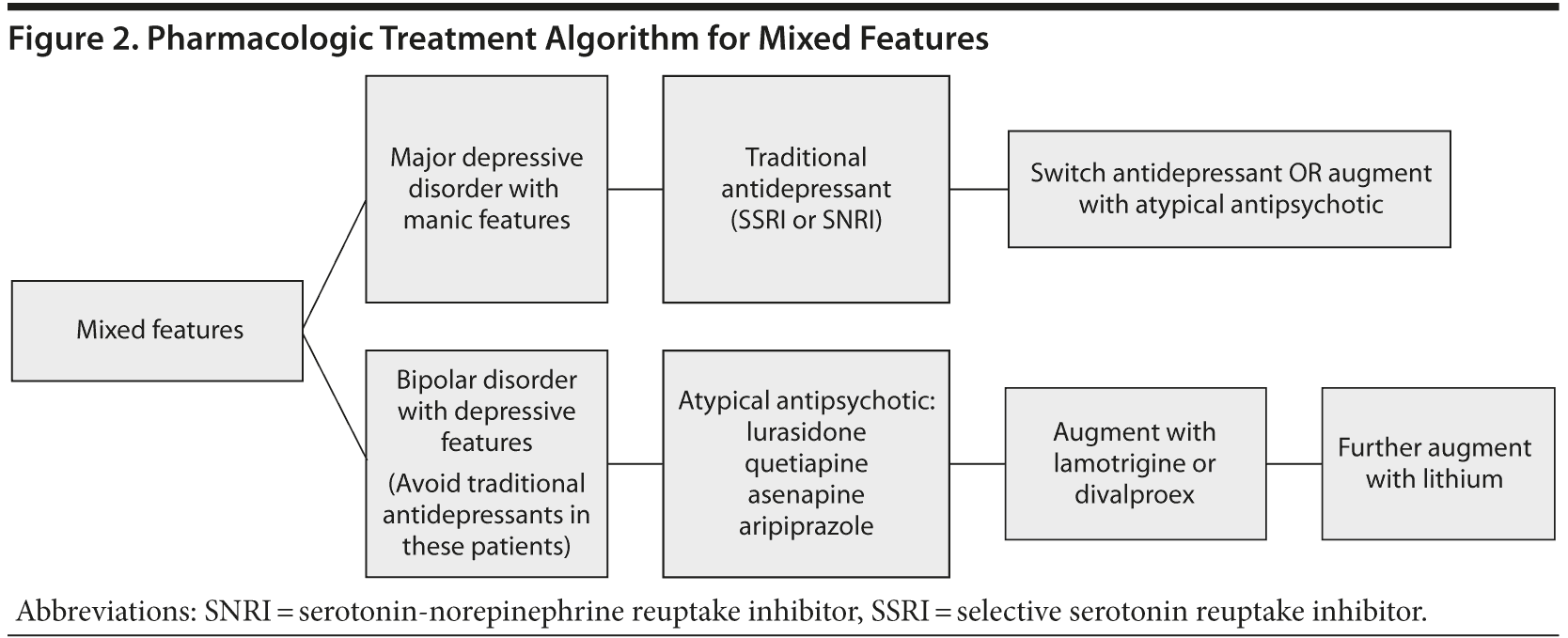
While many guidelines exist for the treatment of bipolar disorder as described in the DSM-IV-TR (eg, Canadian Network for Mood and Anxiety Treatments guidelines in Canada [www.canmat.org/guides.php] and National Institute for Health and Care Excellence guidelines in the United Kingdom [http://guidance.nice.org.uk/CG38/Guidance]), there are no evidence-based guidelines that specifically address the new DSM-5-defined mixed specifier. In general, the treatments for bipolar disorder versus major depressive disorder with mixed symptoms remain discrete but overlap to some extent. For the latter group, current guidelines still recommend antidepressant monotherapy with a selective serotonin reuptake inhibitor (SSRI) or a serotonin-norepinephrine reuptake inhibitor (SNRI). However, many adults with major depressive disorder receiving first-line antidepressant therapy do not achieve remission, inviting the need for a next-step treatment strategy. It is noted that, of the augmentation strategies available, the atypical antipsychotics such as aripiprazole or quetiapine have the largest evidence base in combination with an SSRI and SNRI.
For patients with bipolar disorder and mixed symptoms, atypical antipsychotics (Table 1) are the most effective agents.18 A post hoc analysis suggested that asenapine may in fact be superior to olanzapine in the treatment of mania with depressive features, particularly as the severity of the depressive features increased.18 In the event atypical antipsychotics are insufficient, traditional mood stabilizers such as divalproex or lamotrigine may be considered. Those with bipolar disorder in a depressive phase should not be treated with traditional antidepressants, as their use can trigger a manic switch. All such patients should also ideally receive appropriate psychotherapy (Figure 2).
CONCLUSIONS
Bipolar disorder is commonly encountered in the primary care setting, providing an opportunity for timely diagnosis and introduction of coordinated multimodality treatment. A limitation of the DSM-IV-TR-defined bipolar mixed states was the insufficient characterization of mixed features. By including the mixed specifier, the DSM-5 acknowledges the existence of dimensional mixed states, a change that has significant implications for both diagnosis and treatment. From a diagnostic perspective, these changes reinforce the importance of considering bipolar disorder when someone presents with primarily depressive symptoms. Moreover, those patients with depression and mixed features are at higher risk for more serious illness, concomitant substance use disorders, and developing bipolar disorder and should therefore be monitored more closely.
While no specific treatment guidelines exist for those with the DSM-5-defined mixed specifier, clinicians must recognize the risk of unintentional therapeutic harm when using antidepressant monotherapy in patients with major depressive disorder and a mixed specifier. In such patients, first-line therapy remains an SSRI or an SNRI, but clinicians must be vigilant for bipolar disorder and therapeutic worsening. For those with mania and mixed symptoms, it would be prudent to avoid antidepressant monotherapy and to instead use an atypical antipsychotic or a mood-stabilizing agent.
Drug names: aripiprazole (Abilify), asenapine (Saphris), carbamazepine (Carbatrol, Equetro, and others), divalproex (Depakote and others), haloperidol (Haldol and others), lamotrigine (Lamictal and others), lithium (Lithobid and others), lurasidone (Latuda), olanzapine (Zyprexa and others), paliperidone (Invega), quetiapine (Seroquel), risperidone (Risperdal and others), ziprasidone (Geodon).
Disclosure of off-label usage: The authors have determined that, to the best of their knowledge, no investigational information about pharmaceutical agents that is outside US Food and Drug Administration-approved labeling has been presented in this article.
Author affiliations: Mood Disorders Psychopharmacology Unit, University of Toronto, Toronto, Ontario, Canada.
Potential conflicts of interest: Dr McIntyre has received grant/research support from Eli Lilly, Janssen-Ortho, Shire, AstraZeneca, Pfizer, Lundbeck, Stanley Medical Research Institute, NARSAD, and National Institute of Mental Health; is a member of the advisory boards for AstraZeneca, Bristol-Myers Squibb, France Foundation, GlaxoSmithKline, Janssen-Ortho, Eli Lilly, Organon, Lundbeck, Pfizer, Shire, and Merck; is a member of the speakers’ bureaus for Janssen-Ortho, AstraZeneca, Eli Lilly, Lundbeck, Merck, and Pfizer; and has received honoraria for CME activities from AstraZeneca, Bristol-Myers Squibb, France Foundation, i3 CME, CME Outfitters, Optum Health, Merck, Eli Lilly, and Pfizer. Drs Hu and Mansur have no personal affiliations or financial relationships with any commercial interest to disclose relevant to the article.
Funding/support: None reported.
REFERENCES
1. Merikangas KR, Jin R, He JP, et al. Prevalence and correlates of bipolar spectrum disorder in the world mental health survey initiative. Arch Gen Psychiatry. 2011;68(3):241-251. PubMed doi:10.1001/archgenpsychiatry.2011.12
2. Hirschfeld RM, Lewis L, Vornik LA. Perceptions and impact of bipolar disorder: how far have we really come? results of the national depressive and manic-depressive association 2000 survey of individuals with bipolar disorder. J Clin Psychiatry. 2003;64(2):161-174. PubMed doi:10.4088/JCP.v64n0209
3. Baethge C, Tondo L, Bratti IM, et al. Prophylaxis latency and outcome in bipolar disorders. Can J Psychiatry. 2003;48(7):449-457. PubMed
4. Gazalle FK, Andreazza AC, Ceresér KM, et al. Clinical impact of late diagnose of bipolar disorder. J Affect Disord. 2005;86(2-3):313-316. PubMed doi:10.1016/j.jad.2005.01.003
5. Stang PE, Frank C, Kalsekar A, et al. The clinical history and costs associated with delayed diagnosis of bipolar disorder. MedGenMed. 2006;8(2):18. PubMed
6. Kupfer DJ, Angst J, Berk M, et al. Advances in bipolar disorder: selected sessions from the 2011 International Conference on Bipolar Disorder. Ann N Y Acad Sci. 2011;1242:1-25.
7. McElroy SL. Understanding the complexity of bipolar mixed episodes. J Clin Psychiatry. 2008;69(2):e06. PubMed doi:10.4088/JCP.0208e06
8. American Psychiatric Association. Diagnostic and Statistical Manual of Mental Disorders, Fifth Edition. Arlington, VA: American Psychiatric Association; 2013.
9. Angst J. Do many patients with depression suffer from bipolar disorder? Can J Psychiatry. 2006;51(1):3-5. PubMed
10. Ghaemi SN, Sachs GS, Chiou AM, et al. Is bipolar disorder still underdiagnosed? are antidepressants overutilized? J Affect Disord. 1999;52(1-3):135-144. PubMed doi:10.1016/S0165-0327(98)00076-7
11. Nusslock R, Frank E. Subthreshold bipolarity: diagnostic issues and challenges. Bipolar Disord. 2011;13(7-8):587-603. PubMed doi:10.1111/j.1399-5618.2011.00957.x
12. Fiedorowicz JG, Endicott J, Leon AC, et al. Subthreshold hypomanic symptoms in progression from unipolar major depression to bipolar disorder. Am J Psychiatry. 2011;168(1):40-48. PubMed doi:10.1176/appi.ajp.2010.10030328
13. Goldberg JF, Perlis RH, Bowden CL, et al. Manic symptoms during depressive episodes in 1,380 patients with bipolar disorder: findings from the STEP-BD. Am J Psychiatry. 2009;166(2):173-181. PubMed doi:10.1176/appi.ajp.2008.08050746
14. Gonzסlez-Pinto A, Barbeito S, Alonso M, et al. Poor long-term prognosis in mixed bipolar patients: 10-year outcomes in the Vitoria prospective naturalistic study in Spain. J Clin Psychiatry. 2011;72(5):671-676. PubMed doi:10.4088/JCP.09m05483yel
15. Popovic D, Reinares M, Goikolea JM, et al. Polarity index of pharmacological agents used for maintenance treatment of bipolar disorder. Eur Neuropsychopharmacol. 2012;22(5):339-346. PubMed doi:10.1016/j.euroneuro.2011.09.008
16. Baldessarini RJ, Faedda GL, Offidani E, et al. Antidepressant-associated mood-switching and transition from unipolar major depression to bipolar disorder: a review. J Affect Disord. 2013;148(1):129-135. PubMed doi:10.1016/j.jad.2012.10.033
17. McIntyre RS, Yoon J. Efficacy of antimanic treatments in mixed states. Bipolar Disord. 2012;14(suppl 2):22-36. PubMed doi:10.1111/j.1399-5618.2012.00990.x
18. McIntyre RS, Tohen M, Berk M, et al. DSM-5 mixed specifier for manic episodes: evaluating the effect of depressive features on severity and treatment outcome using asenapine clinical trial data. J Affect Disord. 2013;150(2):378-383. PubMed doi:10.1016/j.jad.2013.04.025