See related blog by Quinn.
A Review of Attention-Deficit/Hyperactivity Disorder in Women and Girls: Uncovering This Hidden Diagnosis

ABSTRACT
Objective: To describe the clinical presentation of attention-deficit/hyperactivity disorder (ADHD) in women and girls and factors influencing proper diagnosis and treatment.
Data Sources: A PubMed search was conducted in April 9, 2012 for English-language publications from the previous 10 years. Search terms included attention deficit hyperactivity disorder, attention deficit/hyperactivity disorder, ADHD, and AD/HD combined with gender, girls, females, women, continuity, discontinuity, gap, treatment, untreated, and lack of treatment.
Study Selection/Data Extraction: A total of 41 articles were reviewed for relevance. Reference lists from relevant articles were reviewed for additional publications; sources known to the authors were also included.
Results: Attitudes about ADHD among individuals with ADHD and knowledgeable informants (families, teachers, colleagues) vary on the basis of the diagnosed individual’s gender. The ADHD prevalence rates are higher among boys than girls. A low index of clinical suspicion exists for girls; their presentation is considered “subthreshold” because inattentiveness is more prominent than hyperactivity/impulsivity. Females with ADHD may develop better coping strategies than males to mask their symptoms. Lastly, anxiety and depression, common comorbidities in female patients with ADHD, can lead to missed or misdiagnosis. If not properly diagnosed and treated, girls with ADHD experience the same negative consequences as boys, including poor academic performance and behavioral problems. Unique issues related to hormonal effects on ADHD expression and treatment response are also experienced by women and girls.
Conclusions: Accurate ADHD diagnosis in women and girls requires establishing a symptom history and an understanding of its gender-specific presentation. Coexisting anxiety and depression are prominent in female patients with ADHD; satisfactory academic achievement should not rule out an ADHD diagnosis.
Prim Care Companion CNS Disord 2014;16(3):doi:10.4088/PCC.13r01596
© Copyright 2014 Physicians Postgraduate Press, Inc.
Submitted: October 9, 2013; accepted January 27, 2014.
Published online: May 15, 2014.
Corresponding author: Patricia O. Quinn, MD, National Center for Girls and Women With ADHD, 3268 Arcadia Pl, NW, Washington, DC 20015 ([email protected]).
Attention-deficit/hyperactivity disorder (ADHD) is a common neurobehavioral disorder characterized by a persistent pattern of inattention and/or hyperactivity-impulsivity.1 In the majority of cases, symptoms begin in childhood and continue to affect a person’s functioning well into adulthood. Gender differences have been reported in the prevalence rates of ADHD, with the published literature indicating that the prevalence of ADHD in boys is 2- to 9-fold higher than in girls in clinical samples and 2- to 3-fold higher in epidemiologic samples.2 These findings are consistent with the 3- to 16-fold higher prevalence of ADHD in boys than in girls across European countries as well.3
The prevalence of ADHD in adulthood appears to be more comparable between sexes than in childhood, with the estimated prevalence of adult ADHD being less than 2-fold higher in men versus women (5.4% vs 3.2%, respectively)4; however, women tend to be older than men when diagnosed with ADHD.5 In addition to differences in rates of diagnosis, the prevalence of ADHD medication use is lower in girls and women compared with boys and men.6 It behooves us, therefore, to understand whether the prevalence data from adult ADHD is incorrect or if childhood symptoms of ADHD are being missed in girls.
Multiple factors may contribute to the lack of ADHD diagnosis in girls during childhood, including differences in predominant symptoms (internalizing rather than externalizing) and subtype (inattentive rather than hyperactive)7; the presence of comorbid psychiatric disorders, including depression and anxiety,8,9 which are linked to internalizing ADHD symptoms; the presence of comorbid obsessive-compulsive disorder, often accompanied by perfectionistic behaviors,10 that might mitigate symptoms and delay diagnosis; the need for referral by others (parents and teachers) for treatment11 and the fact that referrals are made more often for boys than for girls12; and the tendency for relational (covert) aggression to be more prominent than overt aggression in girls13 and for physical aggression in girls with ADHD to be less prominent than in boys with ADHD.14
Taken together, the disparity in diagnosis of ADHD between sexes, the bias in treatment referral, and the reduced use of medication in female patients contribute to the underdiagnosis and undertreatment of ADHD in this population. To assist physicians and mental health professionals in their understanding of this disparity and to foster more successful recognition, diagnosis, and treatment of ADHD in women and girls, the present narrative review will (1) describe the unique presentation of ADHD in females and the factors contributing to this presentation, (2) identify the areas to investigate when assessing the possible presence of ADHD in women and girls, (3) describe the short-term and long-term consequences of untreated ADHD in females, and (4) provide strategies for accurate diagnosis of ADHD in women and girls.
METHOD
Articles cited in this review were identified via a search of PubMed conducted on April 9, 2012 that was limited to English-language articles published in the previous 10 years. The search terms included attention deficit hyperactivity disorder, attention deficit/hyperactivity disorder, ADHD, or AD/HD combined with the following general search terms: gender, girls, females, women, continuity, discontinuity, gap, treatment, untreated, and lack of treatment. A total of 41 articles were identified and reviewed for potential relevance to ADHD in women and girls. Reference lists from relevant articles were also reviewed for additional publications of relevance. Lastly, relevant sources known to the authors that were not obtained from the PubMed search or reference list review were also incorporated, including data related to self-esteem and peer relationships in women and girls with ADHD.
The Presentation of ADHD in Women and Girls
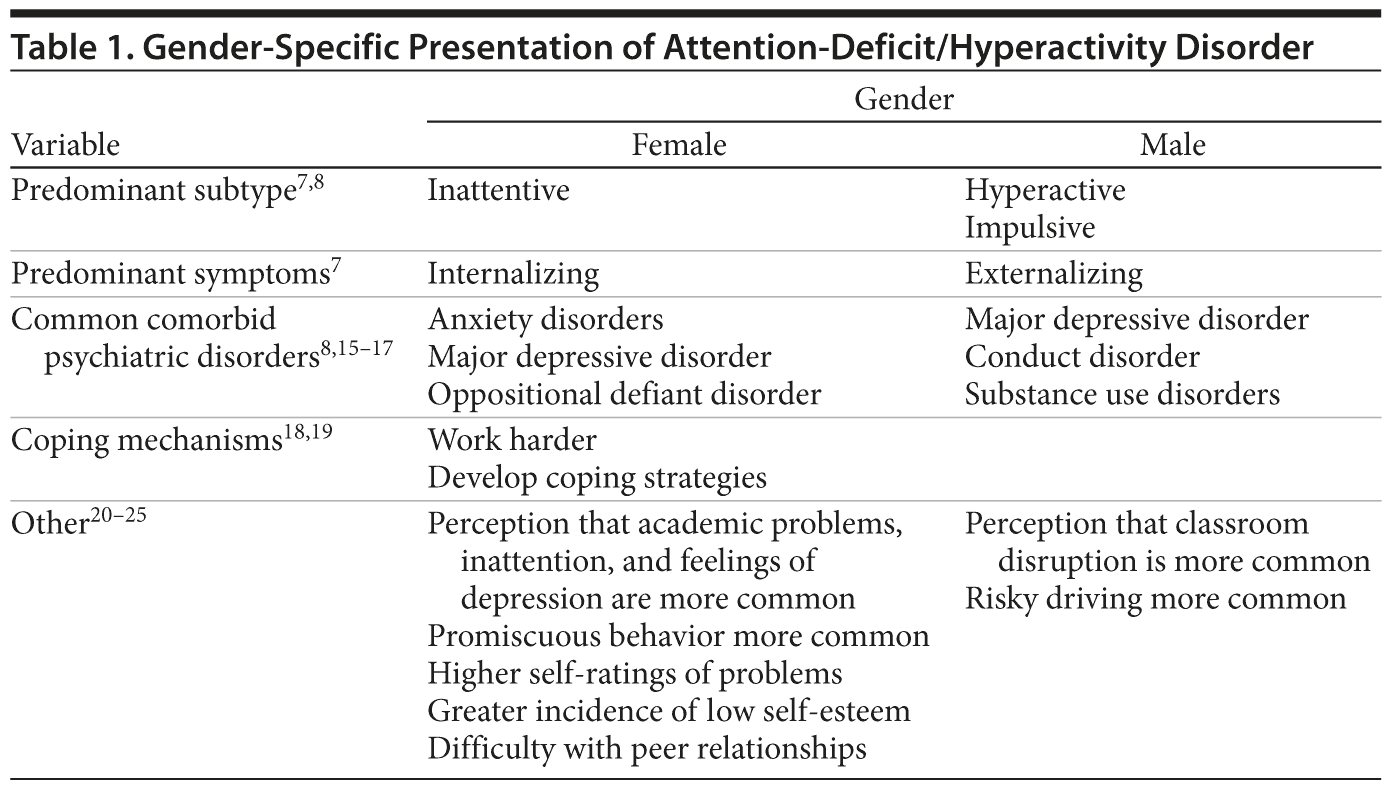
Several characteristics are unique to the expression of ADHD in women and girls. These characteristics include specific symptom presentation, greater incidence of low self-esteem and more difficulty with peer relationships, coexisting anxiety and affective disorders (including a higher incidence of treatment for major depression), and the development of coping strategies that mask underachievement and performance issues (Table 1).

- Women and girls with ADHD have a distinct symptom presentation, with internalizing symptoms (eg, inattentiveness) being more prominent than externalizing symptoms (eg, impulsiveness and hyperactivity). Their symptoms are more likely to be overlooked by knowledgeable informants, and they are less likely to be referred for diagnosis and treatment.
- Females with ADHD may develop better coping strategies than males with ADHD and, as a result, can better mask or mitigate the impact of their ADHD symptoms.
- Missed diagnosis of ADHD in women and girls may occur when anxiety or depression presents in association with ADHD because symptoms of ADHD may mistakenly be attributed to the coexisting condition.
- Greater awareness on the part of health care professionals regarding the specific symptom profile of ADHD in women and girls is necessary for proper diagnosis and treatment.
Although the core symptoms of ADHD as defined by the Diagnostic and Statistical Manual of Mental Disorders, Fourth Edition, Text Revision (DSM-IV-TR)26 criteria (inattentiveness, impulsivity, and hyperactivity) are the same for males and females, inattentiveness is generally more common than hyperactivity and impulsivity in girls with ADHD.3,7,8,27-29 As a generality, females have fewer symptoms as measured by DSM-IV-TR criteria but are just as impaired as males by these symptoms. In addition, for some time, it has been known that women and girls with ADHD are more likely to internalize symptoms and become anxious and depressed and suffer emotional dysregulation than men and boys with the disorder.28 Related to this concept, normative data for the ADHD Rating Scale-IV30 generally show lower thresholds for females than males.
Inattention is less likely to be observed by teachers because it is less disruptive in the classroom setting, and schoolwork is often completed in spite of the challenges noted previously. Because symptom severity contributes to the likelihood of referral for treatment,11 girls may be less likely to be diagnosed and receive treatment. A series of studies explored these problems as they relate to underdiagnosis for girls during childhood. One study confirmed that mothers felt that DSM-IV criteria for ADHD more accurately described boys than girls.31 In addition, girls who were overlooked by their teachers were seen by their parents as having ADHD characteristics,12 perhaps because parents compared their daughters with other girls, whereas teachers compared these same girls with their male classmates. A study published in 2009 explored disruptiveness as a factor for gender gap in referrals of girls.12 Because they are comparing these girls with their male counterparts, teachers may dismiss the less obvious signs of ADHD in girls instead of referring them for an ADHD evaluation. Findings indicate that teachers referred girls with ADHD alone less often than girls with ADHD and oppositional defiant disorder or boys with ADHD.12 Because of the delay in recognizing, diagnosing, and treating ADHD, girls who were referred were more likely to demonstrate more severe symptoms.12
Self-Esteem and Peer Relationships in Women and Girls With ADHD
Low self-esteem is more prominent in females with ADHD than in males with ADHD or non-ADHD female controls.22,23,32 In a population-based study of 10- to 11-year-old children, girls with ADHD scored lower than boys with ADHD on the mental well-being, relationship to parents, and relationship to others subscales on the “I Think I Am” scale of self-esteem.22 In another study of adolescents (aged 13-16 years), girls with ADHD reported more negative self-esteem than boys with ADHD and healthy controls on the Children’s Depression Inventory.23 Additionally, a survey reported that teachers believe that girls with ADHD are more embarrassed about their diagnosis than boys.20 Interestingly, higher levels of executive function deficits in girls are associated with lower peer acceptance,33 which could further contribute to diminished self-esteem in girls with ADHD who exhibit impaired executive function. Poorer self-esteem may persist past childhood,32 and self-esteem among adults with ADHD has been reported to be lower in women than in men.21 Research has confirmed these perceptions and highlighted the fact that women with ADHD struggle with a more negative self-image than do men with ADHD.21
Girls and women with ADHD also tend to be more impaired in social behaviors, peer functioning, and interpersonal relationships than female controls without ADHD.24,25,34 In one study that investigated friendship patterns among girls (aged 6-12 years) with and without ADHD who attended a summer camp,24 it was reported that girls with ADHD had fewer friends, less stable friendships, and more negative features (including conflicts) in their friendships than did girls without ADHD. Similarly, another study of children (aged 6-10 years) reported that boys and girls with ADHD exhibited impaired peer relationships compared with children without ADHD; however, the negative impact of conduct problems on peer relationships was the strongest in girls with ADHD.25 Difficulties in social interactions in girls with ADHD may stem from their choice of action in social situations; one study reported that to reach the same social goals, 6- to 12-year-old girls with ADHD are more likely to respond to hypothetical social vignettes with negative and/or aggressive actions than girls without ADHD.35 However, not all studies report strong gender differences in social impairment. At least one study reported that boys and girls with ADHD exhibited similar levels of impairment relative to children without ADHD on the “problem with peers” and “activity with peers” items of the Social Adjustment Inventory for Children and Adolescents.36
Common Psychological Comorbidities in Women and Girls With ADHD
Anxiety and affective disorders are common comorbidities in girls with ADHD8,9 and have been reported to persist into adulthood.15-17 Significantly higher lifetime prevalence rates were reported in girls (aged 6-18 years) with ADHD versus age-matched healthy controls for major depression (17% vs 1%, respectively) and multiple (ie, more than 2) anxiety disorders (34% vs 5%, respectively).8 Women with ADHD are also more likely to exhibit specific phobias and generalized anxiety disorder than men with ADHD.5 In an 11-year follow-up study, girls with symptoms of ADHD that persisted into adulthood had higher rates of conduct disorder and bipolar disorder than controls.16 Women with ADHD that was not diagnosed until adulthood were more likely to have a history of depression and anxiety than those without ADHD.32
Whether these comorbid disorders are independent of ADHD or develop as a consequence of untreated ADHD, their presence can decrease the likelihood that ADHD will be diagnosed.37,38 Female patients primarily exhibiting symptoms of inattentiveness tend to report low levels of arousal and may be diagnosed with dysthymia rather than ADHD, women exhibiting combined symptoms with high energy and impulsivity could be misdiagnosed with bipolar disorder, and girls presenting with anxiety or depressive symptoms may be treated for these disorders without ADHD ever being considered.39,40 In support of this latter notion that comorbidities can influence ADHD diagnosis, a nationwide survey reported that more young girls than young boys were treated with antidepressants before receiving treatment for ADHD (14% vs 5%),20 reinforcing the notion that pharmacotherapy in female patients tends to be targeted toward such non-ADHD conditions.
Perception of Symptom Presentation in Women and Girls With ADHD by Knowledgeable Informants
Knowledgeable informants (eg, families, teachers, colleagues) may be more likely to overlook ADHD symptoms in women and girls and are therefore less likely to refer them for diagnosis or treatment. A study published in 2009 explored the reasons for this gender gap in referrals for treatment by teachers of girls.12 In this study, parents and teachers read a series of vignettes that differed only in whether the name of a boy or girl was used. Both parents and teachers indicated that they were less likely to seek or recommend ADHD services when the vignette used a girl’s name.12 Another study reported that symptom severity had the greatest influence on referral for treatment for teachers,11 but that despite teachers viewing girls with ADHD as significantly more impaired than boys with ADHD, medication was considered as a treatment strategy less often for girls.11
The contribution of these various factors to the lack of ADHD diagnosis in girls is further supported by the perceptions of parents, educators, and the general public. As previously noted, mothers of girls with ADHD reported that DSM-IV criteria for ADHD more accurately described boys than girls.31 Consistent with this finding, in a survey of the general public and teachers, a substantial proportion held the belief that ADHD is more common in boys than girls and that girls are diagnosed later than boys because they suffer silently and do not act out as noticeably as do boys with ADHD.20 In the same survey, more girls than boys with ADHD reported that they were not currently receiving treatment for their ADHD.20
Circumstances That Suggest the Need to Investigate for ADHD in Women and Girls
When Other Family Members Have ADHD
The current consensus of expert opinion is that ADHD has no simple etiology; both genetic and environmental factors seem to play a role in the risk for ADHD.41 However, there is little doubt that ADHD shows a familial tendency, with a previously published review suggesting that having a first-degree relative with ADHD is associated with a 2- to 8-fold increased risk of ADHD.42 Twin studies indicate 76% heritability in ADHD, but none of the candidate genes studied to date fully account for the risk of ADHD, suggesting that heritability results from a combination of genetic variations and interactions.43 A review of the literature from 1997 to 2012 indicated that genetics and environment are not separate concepts, and the effect of genetic variants may be to increase sensitivity to environmental factors. In addition, the increased risk associated with a positive family history may also apply to comorbid behavioral problems, substance abuse, and affective disorders.44 It should be noted that a family history of documented or suspected ADHD should raise the clinical index of suspicion regardless of gender. However, in the case of a female patient presenting with behaviors characteristic of ADHD, it should serve as an indication that ADHD may be the primary condition rather than any other psychiatric disorder.
When Problems Arise in the Classroom
To address the problem of girls with ADHD not being referred for treatment by teachers and to prevent girls with ADHD from being overlooked in the classroom, it is important to screen girls who are not doing well or require extra help to succeed. In a retrospective analysis of young women (mean age of 19 years) diagnosed with ADHD as children, ADHD was recognized as contributing to impaired academic progress by the parent but not by the individual with ADHD.45 Lack of academic progress also resulted in an increased use of tutoring services, repeating of grades, and placement in special education classes for girls with ADHD compared with controls.8,15 Educational impairments were also reflected in lower rates of graduation from high school in girls with ADHD compared with non-ADHD controls.16
When Behavior Disorders and Problems With Relationships Appear
Oppositional defiant disorder and conduct disorder occur with greater frequency in girls with ADHD than in controls8,9 and could play a role in the problems with relationships (particularly with their mothers18) that are observed in girls with ADHD.8,9,27 Girls with ADHD tend also to engage in socially maladaptive behaviors such as aggression9 more often than healthy controls, which could contribute to problems with peer relationships. If problems in these areas develop, a girl should be referred for an evaluation for underlying ADHD rather than simply focusing on her behavioral issues.
When There Is Risky Sexual Behavior
Although risky sexual behavior and unplanned pregnancy are not typically examined as outcomes when ADHD is assessed using rating scales, they are risks associated with impulsivity. In a survey among teachers (grade 8 and above), more reported that they observed promiscuous behavior in girls with ADHD (44%) than in boys with the disorder (28%).20 In addition, a decreased likelihood of condom use during sexual encounters was reported in a sample of female college undergraduates with ADHD when compared with females without ADHD and males with ADHD46; however, this study did not report any differences in unplanned pregnancy rates between girls with and without ADHD, indicating that additional data are needed to more clearly define the relationship between ADHD and the risk of unintended pregnancy in girls and women with ADHD. In contrast, another study found that higher ADHD symptom scores in young women were associated with an increased likelihood of several high-risk sexual behaviors, except inconsistent condom use, and the acquisition of sexually transmitted diseases.47 A Finnish study found that girls with externalizing problems during childhood (eg, conduct problems and hyperactivity) have a significantly increased risk of becoming mothers before age 20 years.48
When Hormonal Fluctuations May Affect Functioning
It is also important to consider the role of neuroendocrine factors in the expression of ADHD symptoms in women and girls. Preclinical studies suggest that estrogen hormones play an important role in the development and plasticity of midbrain dopamine neurons.49 The neurobiology of dopaminergic function in ADHD is complex, but most data suggest a hypofunction of dopaminergic systems in adults with ADHD (see Del Campo et al50 for a recent review). To date, the interplay of endocrine factors with dopaminergic function in individuals with ADHD has received limited attention, yet there is clear evidence that endocrine systems interact with the central dopamine systems implicated in the etiology and expression of ADHD. A functional magnetic resonance imaging study in healthy women (mean age of 29 years) demonstrated correlations between ovarian steroids (estradiol and progesterone) and neural activity in the amygdala, hippocampus, and orbitofrontal cortex.51 Because these regions play key roles in decision-making and emotional and social behavior,51 it could be speculated that fluctuations in these hormones modulate the preexisting impairments in these behaviors observed in women with ADHD.
Sex differences in cortical and striatal dopamine release, as well as on cognitive function and sensation seeking, have been observed between healthy men (mean age of 28 years) and women (mean age of 25 years) in response to oral amphetamine; this effect was speculated to be related in part to gonadal hormones.52 The subjective euphoric and stimulating effects of oral amphetamine in healthy women (mean age of 25-26 years) have been reported to be greater during the follicular phase than the luteal phase of the menstrual cycle, with these effects being positively correlated with estradiol and negatively correlated with progesterone.53,54 Furthermore, transdermal estradiol administration had stimulating effects when administered alone and increased the stimulating effects of amphetamine, as measured by the Stimulant Sedative Questionnaire, in healthy young women (mean age of 23-26 years).55
The relationship between gonadal hormones and dopaminergic function has implications for women with ADHD. The differential response to stimulant drugs in the presence of estrogen suggests that ADHD medications may need to be titrated throughout the menstrual cycle for optimal symptom control.39 Premenstrual magnification of ADHD symptoms has been described in at least 1 case study39 and is an area worthy of future clinical research.
In addition to estrogen and progesterone, the role of thyroid hormone on ADHD symptoms should be considered. It has been shown that healthy 4-year-old children with thyroid-stimulating hormone levels in the high normal range had a higher risk of exhibiting ADHD symptoms, as did those with low free thyroxine levels.56 Given the higher incidence of thyroid disorders in women than in men57 and the growing evidence of the role of thyroid hormones in brain development and function,58 and a possible association with thyroid hormone receptor insensitivity,59 the role of thyroid hormones in the etiology and expression of ADHD in women and girls should be further examined.
Short-Term and Long-Term Consequences of Missed Diagnosis or Misdiagnosis of ADHD
The short-term effects of undiagnosed or undertreated ADHD in girls sets the stage for the range of academic and social problems during childhood and adolescence20 that have been briefly discussed previously. In addition, the symptomatology and functional impairments present during the formative years are likely to continue into adulthood.6,16,60 Women with ADHD continue to experience lower self-esteem and more anxiety than women without ADHD.32 These women tend to respond to life stressors with emotion and feel a lack of control over their situation,.28,32 which translates into difficulties in coping with home life,29 feelings of disorganization,61 somatization (including headaches, stomachaches),62 and/or sleep difficulties.28,63 As such, children and adolescents with recurrent complaints of headaches, stomachaches, or musculoskeletal pains without associated pathology should be screened for psychiatric disorders.64 Clinicians should also be aware that gender may affect the type of psychopathology associated with the somatic complaints.64
In addition, there is an economic cost associated with untreated ADHD that may not be fully appreciated until these women enter the workforce and assume responsibility for their own financial support. Overall, the behavioral problems associated with adult ADHD can lead to performance issues in the workplace that negatively affect the quality and quantity of work completed.65 Women with ADHD are also treated by mental health professionals more often than women without ADHD and spend more time in treatment,32 suggesting that medical costs are more substantial for these women.
Strategies for Accurate Diagnosis of ADHD in Women and Girls
Increased awareness among health care professionals that ADHD is an important medical issue in women and girls is critical for ensuring proper diagnosis and treatment. It has been suggested that women often seek help for their symptoms on their own,21 but they may not be aware that ADHD is responsible for the problems they are experiencing. Although female patients have been less likely to receive ADHD medications in the past, a review published by Cornforth and colleagues66 suggested that the efficacy and tolerability of ADHD medications is similar in male and female patients, and a review of outcomes from the Multimodal Treatment Study of Children With ADHD found that girls were more likely than boys to have favorable long-term (36 months) outcomes with ADHD medication.67 Growth rates in medication use suggest that the treatment of adult ADHD in women is increasing,6 possibly because of increased awareness of the presentation of ADHD symptoms in women and a subsequent diagnosis of ADHD.
Several factors play key roles in establishing an accurate ADHD diagnosis in women and girls. It is essential to establish a history of ADHD symptoms, with special attention to identifying past and current behaviors consistent with the characteristic presentation in female patients (eg, inattention, emotional reactivity, decreased self-esteem, academic difficulties, and risky behavior). Specific inquiries should be made to identify behaviors suggestive of comorbid anxiety and depression. Self-evaluation of functioning both at home and with peers should be encouraged, in addition to assessment of academic achievement and workplace success. Because girls may work hard to maintain classroom performance, satisfactory academic achievement does not rule out ADHD in girls. Parents may often be the first to report difficulties seen in the home that are missed or not present in school, particularly if the individual receives additional support in the home. Poor peer relationships, anxiety, or self-esteem issues and/or somatic complaints may be initial clues to the impact that ADHD symptoms are having on girls and women in school, at work, or at home.
CONCLUSIONS
Attention-deficit/hyperactivity disorder is an underdiagnosed and undertreated condition especially in women and girls, often being discounted in favor of other comorbid psychiatric disorders. In part, the underrecognition of ADHD in women and girls may be due to a symptom profile (ie, more inattentive and less hyperactive/impulsive than males) that is less likely to be disruptive in the class or in the workplace.20 Greater awareness on the part of health care professionals of the behavioral characteristics of ADHD in women and girls is necessary to uncover the disorder and adequately serve and treat this neglected patient population.
Author affiliations: National Center for Girls and Women With ADHD, Washington, DC (Dr Quinn); and Neuroscience Medical Strategy, Shire Development LLC, Wayne, Pennsylvania (Dr Madhoo).
Potential conflicts of interest: Dr Quinn has served as a consultant to BioBehavioral Diagnosis, McNeil, and Shire; has received honoraria from Noven and Shire; and has served on the speaker’s boards of BioBehavioral Diagnosis, McNeil, Noven, and Shire. Dr Madhoo is an employee of Shire Development LLC and is a stock shareholder in Shire.
Funding/support: Shire Development LLC provided funding to Complete Healthcare Communications, Inc (Chadds Ford, Pennsylvania) for support in writing and editing this manuscript.
Role of the sponsor: The authors exercised full editorial control and had final approval of the manuscript for submission. The content of this manuscript, the ultimate interpretation, and the decision to submit the manuscript for publication in The Primary Care Companion for CNS Disorders was made by the authors independently.
Acknowledgments: Under the direction of the authors, writing assistance was provided by Diane DeHaven-Hudkins, PhD, and Craig Slawecki, PhD, Complete Healthcare Communications, Inc (Chadds Ford, Pennsylvania), and was supported by Shire Development LLC. Drs DeHaven-Hudkins and Slawecki report no other conflicts of interest related to the subject of this article.
REFERENCES
1. American Psychiatric Association. Attention-deficit/hyperactivity disorder. In: Diagnostic and Statistical Manual of Mental Disorders, Fifth Edition. Washington, DC: American Psychiatric Association; 2013:59-61.
2. Nussbaum NL. ADHD and female-specific concerns: a review of the literature and clinical implications. J Atten Disord. 2012;16(2):87-100. PubMed doi:10.1177/1087054711416909
3. Novik TS, Hervas A, Ralston SJ, et al. Influence of gender on attention-deficit/hyperactivity disorder in Europe-ADORE. Eur Child Adolesc Psychiatry. 2006;(suppl 1):115-124.
4. Kessler RC, Adler L, Barkley R, et al. The prevalence and correlates of adult ADHD in the United States: results from the National Comorbidity Survey Replication. Am J Psychiatry. 2006;163(4):716-723. PubMed doi:10.1176/appi.ajp.163.4.716
5. Grevet EH, Bau CH, Salgado CA, et al. Lack of gender effects on subtype outcomes in adults with attention-deficit/hyperactivity disorder: support for the validity of subtypes. Eur Arch Psychiatry Clin Neurosci. 2006;256(5):311-319. PubMed doi:10.1007/s00406-006-0639-5
6. Castle L, Aubert RE, Verbrugge RR, et al. Trends in medication treatment for ADHD. J Atten Disord. 2007;10(4):335-342. PubMed doi:10.1177/1087054707299597
7. Gershon J. A meta-analytic review of gender differences in ADHD. J Atten Disord. 2002;5(3):143-154. PubMed doi:10.1177/108705470200500302
8. Biederman J, Faraone SV, Mick E, et al. Clinical correlates of ADHD in females: findings from a large group of girls ascertained from pediatric and psychiatric referral sources. J Am Acad Child Adolesc Psychiatry. 1999;38(8):966-975. PubMed doi:10.1097/00004583-199908000-00012
9. Hinshaw SP. Preadolescent girls with attention-deficit/hyperactivity disorder, 1: background characteristics, comorbidity, cognitive and social functioning, and parenting practices. J Consult Clin Psychol. 2002;70(5):1086-1098. PubMed doi:10.1037/0022-006X.70.5.1086
10. Arnold PD, Ickowicz A, Chen S, et al. Attention-deficit hyperactivity disorder with and without obsessive-compulsive behaviors: clinical characteristics, cognitive assessment, and risk factors. Can J Psychiatry. 2005;50(1):59-66. PubMed
11. Coles EK, Slavec J, Bernstein M, et al. Exploring the gender gap in referrals for children with ADHD and other disruptive behavior disorders. J Atten Disord. 2012;16(2):101-108. PubMed doi:10.1177/1087054710381481
12. Ohan JL, Visser TA. Why is there a gender gap in children presenting for attention-deficit/hyperactivity disorder services? J Clin Child Adolesc Psychol. 2009;38(5):650-660. PubMed doi:10.1080/15374410903103627
13. Ohan JL, Johnston C. Positive illusions of social competence in girls with and without ADHD. J Abnorm Child Psychol. 2011;39(4):527-539. PubMed doi:10.1007/s10802-010-9484-0
14. Abikoff HB, Jensen PS, Arnold LL, et al. Observed classroom behavior of children with ADHD: relationship to gender and comorbidity. J Abnorm Child Psychol. 2002;30(4):349-359. PubMed doi:10.1023/A:1015713807297
15. Biederman J, Faraone SV, Monuteaux MC, et al. Gender effects on attention-deficit/hyperactivity disorder in adults, revisited. Biol Psychiatry. 2004;55(7):692-700. PubMed doi:10.1016/j.biopsych.2003.12.003
16. Biederman J, Petty CR, O’ Connor KB, et al. Predictors of persistence in girls with attention-deficit/hyperactivity disorder: results from an 11-year controlled follow-up study. Acta Psychiatr Scand. 2012;125(2):147-156. PubMed doi:10.1111/j.1600-0447.2011.01797.x
17. Wilens TE, Biederman J, Faraone SV, et al. Presenting ADHD symptoms, subtypes, and comorbid disorders in clinically referred adults with ADHD. J Clin Psychiatry. 2009;70(11):1557-1562. PubMed doi:10.4088/JCP.08m04785pur
18. Quinn PO, Nadeau KG, Littman EB. Understanding Girls With AD/HD. Silver Spring, MD: Advantage Books; 1999.
19. Quinn P. 100 Questions & Answers About Attention Deficit Hyperactivity Disorder (ADHD) in Women and Girls. Burlington, MA: Jones & Bartlett Learning; 2010.
20. Quinn P, Wigal S. Perceptions of girls and ADHD: results from a national survey. MedGenMed. 2004;6(2):2. PubMed
21. Arcia E, Conners CK. Gender differences in ADHD? J Dev Behav Pediatr. 1998;19(2):77-83. PubMed doi:10.1097/00004703-199804000-00003
22. Ek U, Westerlund J, Holmberg K, et al. Self-esteem in children with attention and/or learning deficits: the importance of gender. Acta Paediatr. 2008;97(8):1125-1130. PubMed doi:10.1111/j.1651-2227.2008.00894.x
23. Rucklidge JJ, Tannock R. Psychiatric, psychosocial, and cognitive functioning of female adolescents with ADHD. J Am Acad Child Adolesc Psychiatry. 2001;40(5):530-540. PubMed doi:10.1097/00004583-200105000-00012
24. Blachman DR, Hinshaw SP. Patterns of friendship among girls with and without attention-deficit/hyperactivity disorder. J Abnorm Child Psychol. 2002;30(6):625-640. PubMed doi:10.1023/A:1020815814973
25. Mikami AY, Lorenzi J. Gender and conduct problems predict peer functioning among children with attention-deficit/hyperactivity disorder. J Clin Child Adolesc Psychol. 2011;40(5):777-786. PubMed doi:10.1080/15374416.2011.597089
26. American Psychiatric Association. Diagnostic and Statistical Manual of Mental Disorders. Fourth Edition, Text Revision. Washington, DC: American Psychiatric Association; 2000.
27. Elkins IJ, Malone S, Keyes M, et al. The impact of attention-deficit/hyperactivity disorder on preadolescent adjustment may be greater for girls than for boys. J Clin Child Adolesc Psychol. 2011;40(4):532-545. PubMed doi:10.1080/15374416.2011.581621
28. Robison RJ, Reimherr FW, Marchant BK, et al. Gender differences in 2 clinical trials of adults with attention-deficit/hyperactivity disorder: a retrospective data analysis. J Clin Psychiatry. 2008;69(2):213-221. PubMed doi:10.4088/JCP.v69n0207
29. Fedele DA, Lefler EK, Hartung CM, et al. Sex differences in the manifestation of ADHD in emerging adults. J Atten Disord. 2012;16(2):109-117. PubMed doi:10.1177/1087054710374596
30. DuPaul GJ, Power TJ, Anastopoulos AD, et al. ADHD Rating Scale-IV: Checklists, Norms, and Clinical Interpretation. New York, NY: Guilford Press; 1998.
31. Ohan JL, Johnston C. Gender appropriateness of symptom criteria for attention-deficit/hyperactivity disorder, oppositional-defiant disorder, and conduct disorder. Child Psychiatry Hum Dev. 2005;35(4):359-381. PubMed doi:10.1007/s10578-005-2694-y
32. Rucklidge JJ, Kaplan BJ. Psychological functioning of women identified in adulthood with attention-deficit/hyperactivity disorder. J Atten Disord. 1997;2(3):167-176. doi:10.1177/108705479700200303
33. Diamantopoulou S, Rydell AM, Thorell LB, et al. Impact of executive functioning and symptoms of attention-deficit/hyperactivity disorder on children’s peer relations and school performance. Dev Neuropsychol. 2007;32(1):521-542. PubMed doi:10.1080/87565640701360981
34. Young S, Heptinstall E, Sonuga-Barke EJ, et al. The adolescent outcome of hyperactive girls: self-report of psychosocial status. J Child Psychol Psychiatry. 2005;46(3):255-262. PubMed doi:10.1111/j.1469-7610.2004.00350.x
35. Thurber JR, Heller TL, Hinshaw SP. The social behaviors and peer expectation of girls with attention deficit hyperactivity disorder and comparison girls. J Clin Child Adolesc Psychol. 2002;31(4):443-452. PubMed
36. Greene RW, Biederman J, Faraone SV, et al. Social impairment in girls with ADHD: patterns, gender comparisons, and correlates. J Am Acad Child Adolesc Psychiatry. 2001;40(6):704-710. PubMed doi:10.1097/00004583-200106000-00016
37. Nadeau KG, Quinn PO. Rethinking DSM-IV. In: Nadeau KG, Quinn PO, eds. Understanding Women with ADHD. Silver Spring, MD: Advantage Books; 2002:2-19.
38. Nadeau KG, Quinn PO. Gender and history of ADHD: an unexamined gender bias. In: Quinn PO, Nadeau KG, eds. Gender Issues and ADHD: Research, Diagnosis, and Treatment. Silver Spring, MD: Advantage Books; 2002:2-19.
39. Quinn PO. Treating adolescent girls and women with ADHD: gender-specific issues. J Clin Psychol. 2005;61(5):579-587. PubMed doi:10.1002/jclp.20121
40. Waite R. Women and attention deficit disorders: a great burden overlooked. J Am Acad Nurse Pract. 2007;19(3):116-125. PubMed doi:10.1111/j.1745-7599.2006.00203.x
41. Sonuga-Barke EJ, Halperin JM. Developmental phenotypes and causal pathways in attention-deficit/hyperactivity disorder: potential targets for early intervention? J Child Psychol Psychiatry. 2010;51(4):368-389. PubMed doi:10.1111/j.1469-7610.2009.02195.x
42. Faraone SV, Mick E. Molecular genetics of attention-deficit/hyperactivity disorder. Psychiatr Clin North Am. 2010;33(1):159-180. PubMed doi:10.1016/j.psc.2009.12.004
43. Faraone SV, Perlis RH, Doyle AE, et al. Molecular genetics of attention-deficit/hyperactivity disorder. Biol Psychiatry. 2005;57(11):1313-1323. PubMed doi:10.1016/j.biopsych.2004.11.024
44. Thapar A, Cooper M, Eyre O, et al. What have we learnt about the causes of ADHD? J Child Psychol Psychiatry. 2013;54(1):3-16. PubMed doi:10.1111/j.1469-7610.2012.02611.x
45. Babinski DE, Pelham WE Jr, Molina BS, et al. Late adolescent and young adult outcomes of girls diagnosed with ADHD in childhood: an exploratory investigation. J Atten Disord. 2011;15(3):204-214. PubMed doi:10.1177/1087054710361586
46. Huggins SP, Rooney ME, Chronis-Tuscano A. Risky sexual behavior among college students with ADHD: is the mother-child relationship protective [published online ahead of print October 9, 2012]? J Atten Disord. 2012. PubMed doi:10.1177/1087054712459560
47. Hosain GM, Berenson AB, Tennen H, et al. Attention-deficit/hyperactivity symptoms and risky sexual behavior in young adult women. J Womens Health (Larchmt). 2012;21(4):463-468. PubMed doi:10.1089/jwh.2011.2825
48. Lehti V, Niemelä S, Heinze M, et al. Childhood predictors of becoming a teenage mother among Finnish girls. Acta Obstet Gynecol Scand. 2012;91(11):1319-1325. PubMed doi:10.1111/j.1600-0412.2012.01517.x
49. K×¼ppers E, Ivanova T, Karolczak M, et al. Estrogen: a multifunctional messenger to nigrostriatal dopaminergic neurons. J Neurocytol. 2000;29(5-6):375-385. PubMed doi:10.1023/A:1007165307652
50. Del Campo N, Chamberlain SR, Sahakian BJ, et al. The roles of dopamine and noradrenaline in the pathophysiology and treatment of attention-deficit/hyperactivity disorder. Biol Psychiatry. 2011;69(12):e145-e157. PubMed doi:10.1016/j.biopsych.2011.02.036
51. Dreher JC, Schmidt PJ, Kohn P, et al. Menstrual cycle phase modulates reward-related neural function in women. Proc Natl Acad Sci U S A. 2007;104(7):2465-2470. PubMed doi:10.1073/pnas.0605569104
52. Riccardi P, Zald D, Li R, et al. Sex differences in amphetamine-induced displacement of [(18)F]fallypride in striatal and extrastriatal regions: a PET study. Am J Psychiatry. 2006;163(9):1639-1641. PubMed doi:10.1176/appi.ajp.163.9.1639
53. Justice AJ, de Wit H. Acute effects of d-amphetamine during the follicular and luteal phases of the menstrual cycle in women. Psychopharmacology (Berl). 1999;145(1):67-75. PubMed doi:10.1007/s002130051033
54. White TL, Justice AJ, de Wit H. Differential subjective effects of d-amphetamine by gender, hormone levels and menstrual cycle phase. Pharmacol Biochem Behav. 2002;73(4):729-741. PubMed doi:10.1016/S0091-3057(02)00818-3
55. Justice AJ, de Wit H. Acute effects of estradiol pretreatment on the response to d-amphetamine in women. Neuroendocrinology. 2000;71(1):51-59. PubMed doi:10.1159/000054520
56. Alvarez-Pedrerol M, Ribas-Fitó N, Torrent M, et al. TSH concentration within the normal range is associated with cognitive function and ADHD symptoms in healthy preschoolers. Clin Endocrinol (Oxf). 2007;66(6):890-898. PubMed doi:10.1111/j.1365-2265.2007.02871.x
57. Vanderpump MP, Tunbridge WM, French JM, et al. The incidence of thyroid disorders in the community: a twenty-year follow-up of the Whickham survey. Clin Endocrinol (Oxf). 1995;43(1):55-68. PubMed doi:10.1111/j.1365-2265.1995.tb01894.x
58. Argumedo GS, Sanz CR, Olgu×n HJ. Experimental models of developmental hypothyroidism. Horm Metab Res. 2012;44(2):79-85. PubMed doi:10.1055/s-0031-1297941
59. Weiss RE, Tunca H, Knapple WL, et al. Phenotype differences of resistance to thyroid hormone in two unrelated families with an identical mutation in the thyroid hormone receptor beta gene (R320C). Thyroid. 1997;7(1):35-38. PubMed doi:10.1089/thy.1997.7.35
60. Rucklidge J, Brown D, Crawford S, et al. Attributional styles and psychosocial functioning of adults with ADHD: practice issues and gender differences. J Atten Disord. 2007;10(3):288-298. PubMed doi:10.1177/1087054706289942
61. Retz-Junginger P, Rösler M, Jacob C, et al. Gender differences in self- and investigator-rated psychopathology in adult attention-deficit/hyperactivity disorder. Atten Defic Hyperact Disord. 2010;2(2):93-101. PubMed doi:10.1007/s12402-010-0024-0
62. Graetz BW, Sawyer MG, Baghurst P. Gender differences among children with DSM-IV ADHD in Australia. J Am Acad Child Adolesc Psychiatry. 2005;44(2):159-168. PubMed doi:10.1097/00004583-200502000-00008
63. Rasmussen K, Levander S. Untreated ADHD in adults: are there sex differences in symptoms, comorbidity, and impairment? J Atten Disord. 2009;12(4):353-360. PubMed doi:10.1177/1087054708314621
64. Egger HL, Costello EJ, Erkanli A, et al. Somatic complaints and psychopathology in children and adolescents: stomach aches, musculoskeletal pains, and headaches. J Am Acad Child Adolesc Psychiatry. 1999;38(7):852-860. PubMed doi:10.1097/00004583-199907000-00015
65. de Graaf R, Kessler RC, Fayyad J, et al. The prevalence and effects of adult attention-deficit/hyperactivity disorder (ADHD) on the performance of workers: results from the WHO World Mental Health Survey Initiative. Occup Environ Med. 2008;65(12):835-842. PubMed doi:10.1136/oem.2007.038448
66. Cornforth C, Sonuga-Barke E, Coghill D. Stimulant drug effects on attention-deficit/hyperactivity disorder: a review of the effects of age and sex of patients. Curr Pharm Des. 2010;16(22):2424-2433. PubMed doi:10.2174/138161210791959827
67. Murray DW, Arnold LE, Swanson J, et al. A clinical review of outcomes of the multimodal treatment study of children with attention-deficit/hyperactivity disorder (MTA). Curr Psychiatry Rep. 2008;10(5):424-431. PubMed doi:10.1007/s11920-008-0068-4