ABSTRACT
Objective: To determine the etiologies of epilepsy in a cohort of patients using the International League Against Epilepsy 2017 classification system and to determine frequencies of preventable causes and their clinical characteristics.
Methods: Epileptic patients in neurology clinics at a tertiary care hospital were prospectively recruited from June 1, 2018, to November 30, 2018. Patients were divided according to their respective etiologic categories. Traumatic brain injury, stroke, hypoxic-ischemic encephalopathy, and central nervous system infections were considered preventable etiologies.
Results: A total of 160 patients were included in the study. Of these patients, 61 had epilepsy of unknown etiology, while among the remaining 99 patients in whom etiology could be identified, traumatic brain injury was the most frequent overall cause with 17 (17.2%) cases. Frequencies in other etiologies were genetic (idiopathic generalized epilepsy): n = 14, stroke: n = 13, hypoxic-ischemic encephalopathy: n = 13, cerebral tumors: n = 10, mesial temporal sclerosis: n = 9, cortical malformation: n = 7, and other structural pathologies: n = 5. Other rarer causes (including central nervous system infections) had less than 5 patients each. When the preventable etiologies were grouped, they formed 46 of 99 patients (46.5%) with identifiable etiology. Seizure control was mostly satisfactory in the total sample (126/160 [78.8%]), including patients with preventable etiologies, of whom 50% were on polytherapy.
Conclusions: Epilepsies with preventable etiologies are common in our clinics. Studies are needed in other centers to identify epilepsy etiologies and confirm our findings, which may help determine better strategies for primary prevention of epilepsy.
Prim Care Companion CNS Disord 2021;23(6):20m02904
To cite: Khuda IE, Aljaafari D, Zeeshan MA, et al. Preventable etiologies of epilepsies in Saudi Arabia: a tertiary care experience. Prim Care Companion CNS Disord. 2021;23(6):20m02904.
To share: https://doi.org/10.4088/PCC.20m02904
© Copyright 2021 Physicians Postgraduate Press, Inc.
aDepartment of Neurology, College of Medicine, Imam Abdul Rahman Bin Faisal University, King Fahd University Hospital, Dammam, Saudi Arabia
bDepartment of Medical Education, College of Medicine, Imam Abdul Rahman Bin Faisal University, Dammam, Saudi Arabia
*Corresponding author: Danah Aljaafari, MD, Department of Neurology, College of Medicine, Imam Abdul Rahman Bin Faisal University, 2835 King Faisal Rd, Dammam 34212, Saudi Arabia ([email protected]).
Epilepsy is a common chronic neurologic disorder. According to World Health Organization data, approximately 50 million people are suffering from epilepsy worldwide.1 In Saudi Arabia, its prevalence is 6.54/1,000 population.2
Epilepsy is a chronic condition that requires treatment for many years, with some patients requiring lifelong therapy.3 The burden of epilepsy thus has a potential long-term impact on financial and health care resources; moreover, there are significant effects of epilepsy on the personal and social lives of patients.4
In the last few years, the International League Against Epilepsy (ILAE) has improved epilepsy definitions and classifications.5,6 In 2017, ILAE published a new classification system for seizures and epilepsy, which has reduced the inconsistencies and deficiencies in seizure classification strategies used previously.6,7 In 2018, ILAE’s task force for primary prevention of epilepsy published a systematic review8 that reinforced the concept of primary prevention of epilepsy, which is otherwise a subject that is largely ignored. This task force considered traumatic brain injury (TBI), stroke, perinatal brain insults (hypoxic ischemic encephalopathy [HIE]), and central nervous system (CNS) infections as preventable etiologies of epilepsy.8 All of these preventable epilepsies are due to a remote cerebral insult and thus constitute a group of disorders that are sometimes called remote symptomatic epilepsies.
We used the 2017 ILAE classification system by identifying the seizure type first, followed by syndromic diagnosis, if possible, and detecting the etiologies in a cohort of our patients. We further grouped the etiologies of epilepsy that were preventable according to the ILAE task force guidelines for epilepsy prevention and evaluated their frequencies. We also evaluated clinical characteristics for all the etiologies, which included demographic profiles, electroencephalographic (EEG) features, seizure control, the requirement of polytherapy, and the antiepileptic drugs used in different etiologies.
METHODS
This prospective cross-sectional study was approved by the institutional review board of the tertiary care hospital wherein it was conducted. The patients visiting neurology clinics during a 6-month period (June 1, 2018, to November 30, 2018), irrespective of their race or nationality, were prospectively included in the study. After applying the inclusion and exclusion criteria, eligible patients were ≥ 12 years of age and had an established diagnosis of epilepsy for at least 1 year. After providing informed consent, the patients’ demographic details, EEG characteristics, seizure control, use of antiepileptic drugs, and requirement of monotherapy or polytherapy were also recorded. All the cases were reviewed, evaluated, and investigated further (if necessary) by a consultant epileptologist to determine their eligibility for the study, etiology of epilepsy, and clinical characteristics. The details were entered into a predesigned data collection tool.
All the patients were classified according to the ILAE 2017 classification system, depending on the seizure type, syndrome, and etiology.6,7 Patients with TBI, stroke, HIE, or CNS infections were grouped as having preventable etiologies. Their characteristics were determined individually as a component of the group as well as a whole group of preventable etiologies. For details of operational definitions, see Supplementary Table 1.
Inclusion Criteria
Inclusion criteria included all consecutive patients with a diagnosis of epilepsy aged ≥ 12 years who visited the epilepsy clinic during the study period.
Exclusion Criteria
Exclusion criteria included epileptic patients aged < 12 years, those with acute symptomatic seizures, those with incomplete workup, and those in whom epilepsy could not be classified.
Statistical Analysis
All the categorical variables were evaluated by 2*2 contingency tables, using odds ratio (OR) with 95% confidence intervals and χ2 or Fisher exact test to generate P values (significant if P < .05). Continuous variables are presented as medians with minimum and maximum values. All data were analyzed by SPSS version 21.0 (SPSS Inc, IBM Corp, Armonk, New York).
RESULTS
A total of 172 consecutive patients were considered, and after applying the inclusion and exclusion criteria, 160 patients were eligible for the study. The median age was 29 years (range, 12–76 years), with a male to female ratio of 1:1. There were 22 patients in the adolescent age group (aged 12–18 years), while 138 patients were adults (aged ≥ 19 years).
Frequencies of Different Seizure Types
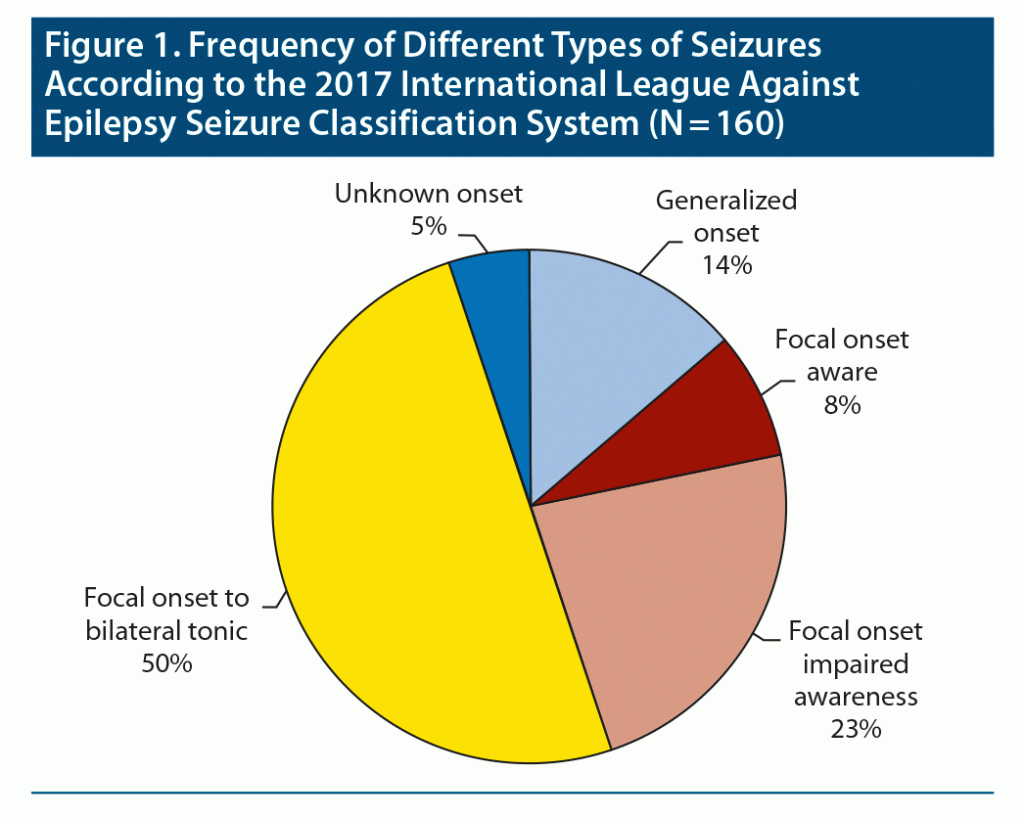
Of 160 patients, 130 (81.3%) had focal onset seizures, while 22 (13.8%) had generalized onset and 8 (5%) had unknown onset seizures. Among the focal onset seizures, the focal to bilateral tonic-clonic seizures were the most frequent type in 80 of 130 patients (61.5%). Focal impaired awareness seizures were present in 37 of 130 (28.4%) patients, and focal aware seizures were present in 13 of 130 (10%) patients (Figure 1).
Frequency Distribution in Syndromes and Etiologic Categories
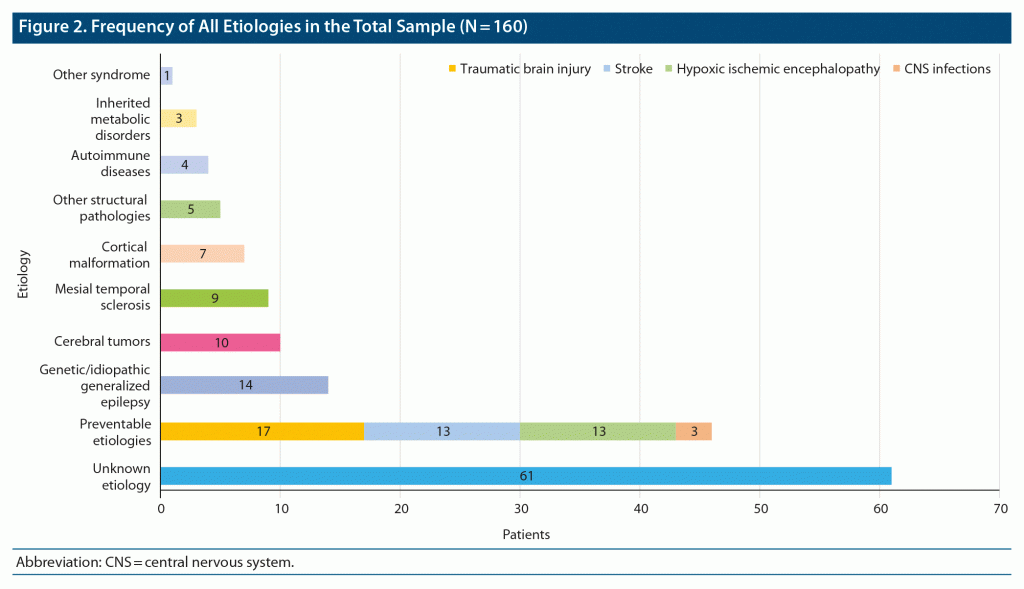
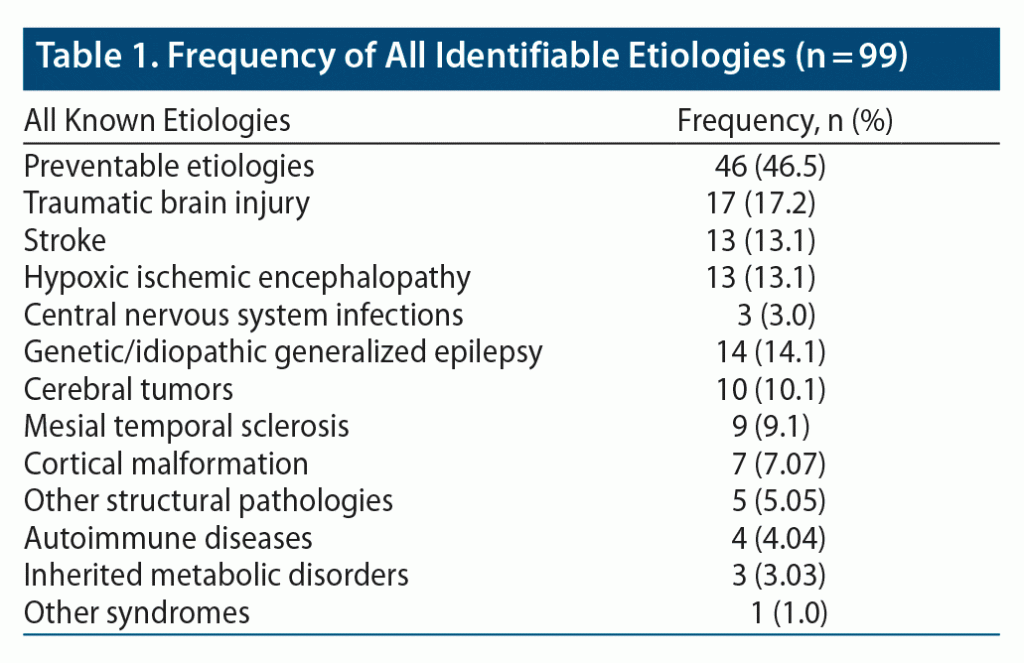
Of the 160 patients, 61 (38%) had no identifiable cause for their seizures. Of the remaining 99 patients with a diagnosed etiology, TBI was most common with 17 patients or 17% of all the identifiable causes. Genetic/idiopathic generalized epilepsy (IGE) syndrome was the second most common identifiable cause with 14 of 99 cases, followed by stroke and HIE, each having 13 of 99 patients. Cerebral tumors were found in 10 of 99 identifiable epileptic cases. Other etiologies included mesial temporal sclerosis (9 of 99 patients), cortical malformation (7 of 99 patients), and other structural pathologies (5 of 99 patients). Other rarer causes (including CNS infections) had less than 5 patients each (Figure 2, Table 1). Among the patients with IGE syndromes, 7 had juvenile myoclonic epilepsy, 5 had epilepsy with generalized tonic-clonic seizures alone, and 1 patient each had childhood and juvenile absence epilepsy.
When all the preventable etiologies were grouped irrespective of age (consisting of TBI, stroke, HIE, and CNS infections), they totaled 46 cases or 46.5% of all the 99 identifiable causes (see Figure 2, Table 1). TBI was the most frequent cause, comprising 37% (17/46) of the preventable epilepsy group (see Figure 2).
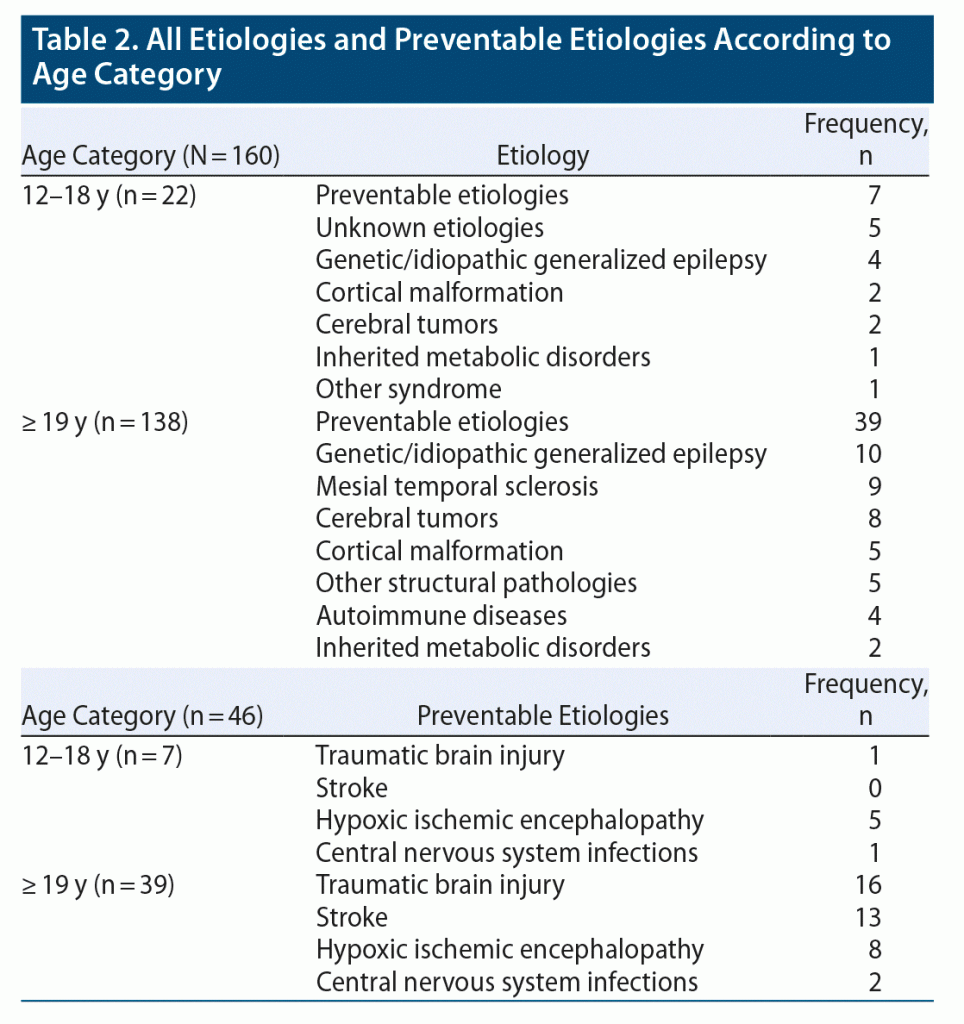
When the adolescent (12–18 years age group) patients were considered separately, the preventable etiology group had the highest frequency with 7/22 patients, consisting mostly of the HIE etiology (5 of 7 patients), while there were no poststroke epilepsy cases (Table 2).
In adult patients, the preventable epilepsy group again had the largest proportion (39/82, 47.5%) of identifiable causes comprised mainly of TBI etiology (16/39, 41%) (see Table 2).
Demographic Profiles of Different Categories
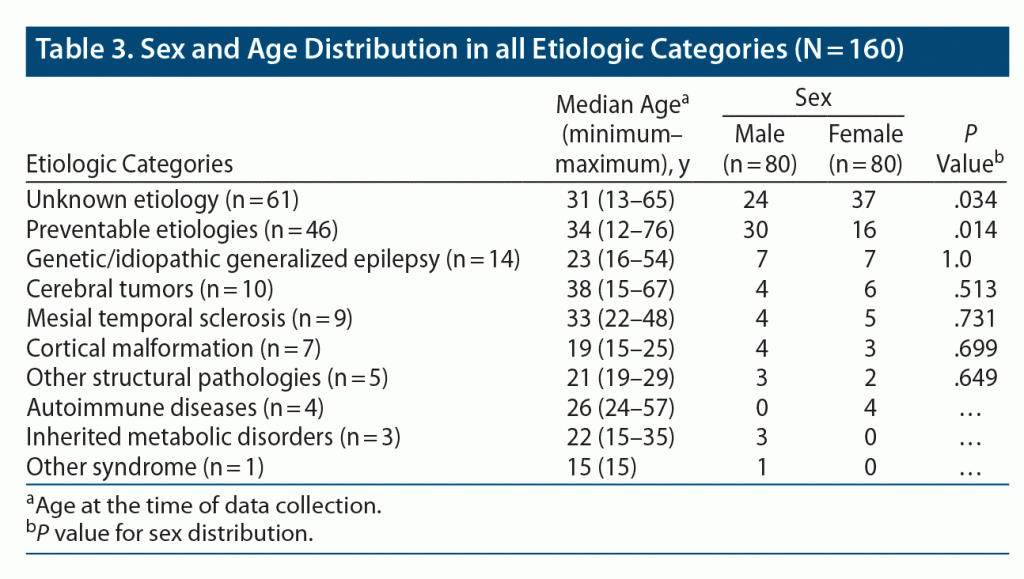
The sex and age distribution among different etiologic categories was similar (Table 3) with a few exceptions. The group of epilepsies with preventable etiologies had a significantly higher frequency of male sex (P = .014) due to higher male frequency in its component TBI, HIE, and CNS infection etiologies, while poststroke epilepsy had an equal distribution by sex. The unknown etiology category had a significant number of female patients (P = .034). The 3 patients with epilepsies due to inherited metabolic disorders were male, and the 4 patients with autoimmune epilepsy were female (see Table 3).
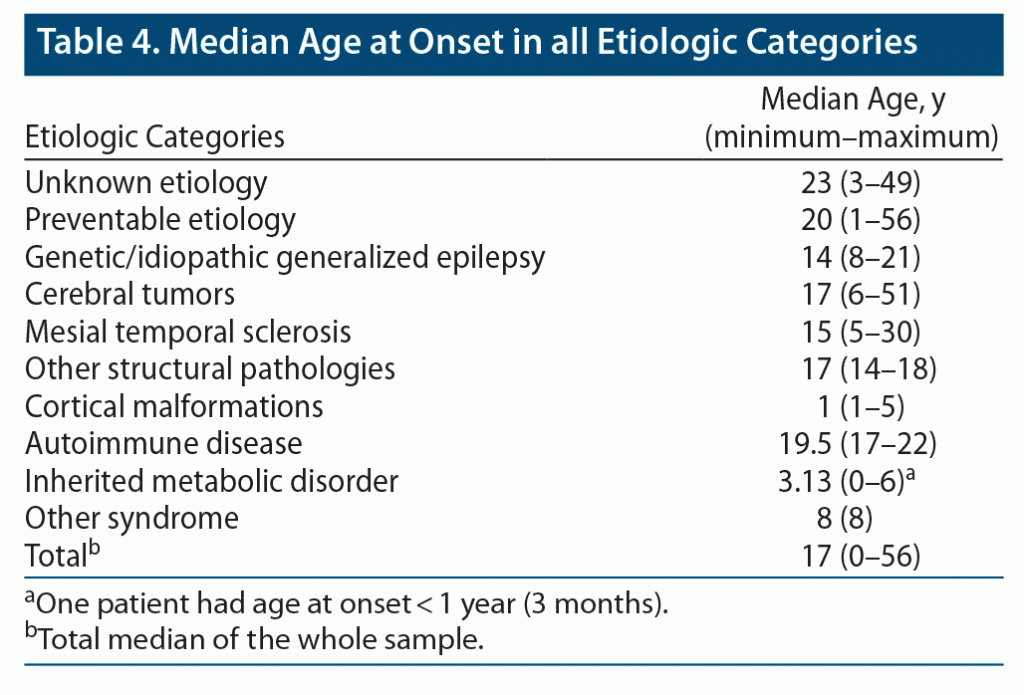
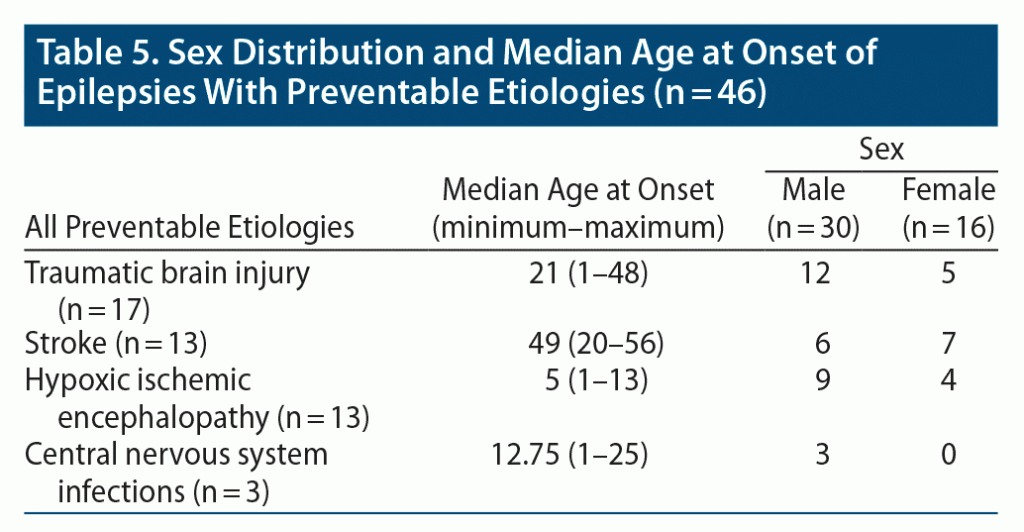
The median age at onset of epilepsy with preventable etiologies was 20 (range, 1–56) years (Table 4). For epilepsies post-TBI and stroke, the median age at onset of epileptic seizures was 21 (range, 1–48) years and 49 (range, 20–56) years, respectively (Table 5).
Seizure Control in Different Etiology Categories
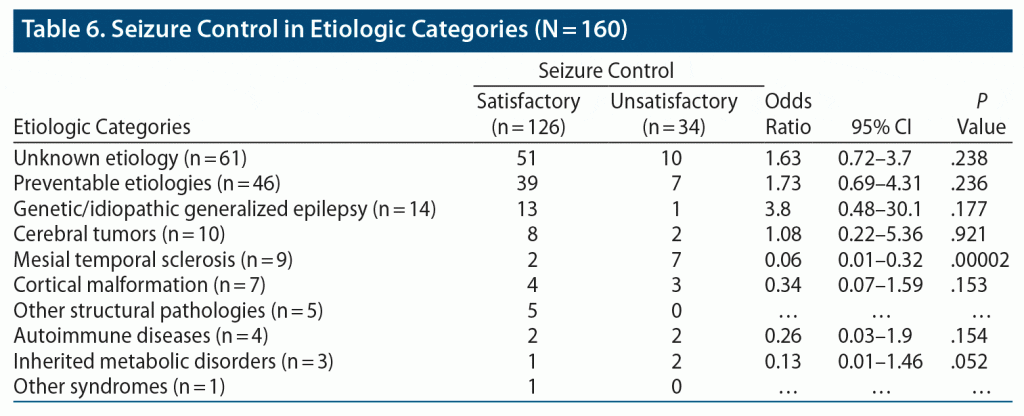
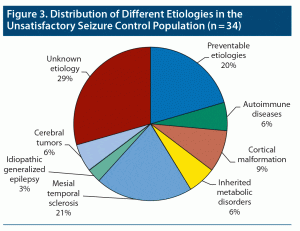
Overall seizure control in the total sample was largely satisfactory (126/160, 78.8%), except for 34 patients who had unsatisfactory seizure control. Patients with mesial temporal sclerosis had significantly lower frequency of satisfactory seizure control (2/9; OR = 0.06; 95% CI, 0.01–0.32; P < .001). Patients with inherited metabolic disorders, which had a very low prevalence, also had a lower proportion of satisfactory seizure control that nearly reached statistical significance (Table 6). Those with autoimmune epilepsy and cortical malformation had an almost equal proportion of satisfactory and unsatisfactory seizure control. Among patients with preventable epilepsies, 85% of the patients (39/46; OR = 1.73; 95% CI, 0.69–4.31; P = .236) had satisfactory seizure control. However, among the 34 patients with unsatisfactory seizure control, 7 (20%) had preventable etiologies (Figure 3).
Epileptiform Discharges on Routine EEG
A total of 155 patients underwent routine EEG, of whom only 74 (47.7%) had epileptiform discharges. In the preventable etiologies group, epileptiform activities were present in 15 of 44 (21%) patients, which was significantly lower compared to the rest of the sample (OR = 0.46; 95% CI, 0.22–0.94; P =.032).
Type of Antiepileptic Drug Therapy
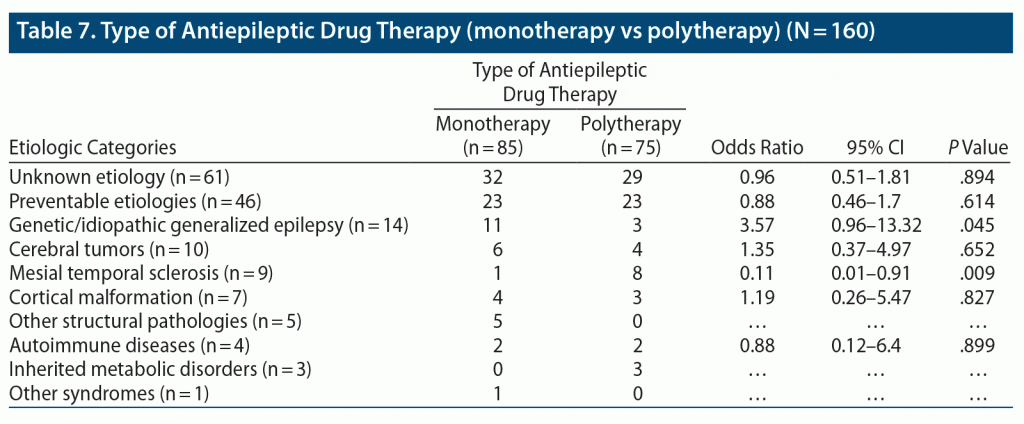
Among the total sample, 85 (53%) patients were on monotherapy (Table 7). Monotherapy and polytherapy use were of almost equal proportions across different etiologic categories, except for IGE and mesial temporal sclerosis. Monotherapy was favored in IGE; however, it did not reach statistical significance, with a low sample size (95% CI, 0.96–13.2). Monotherapy was least preferred for patients with mesial temporal sclerosis, who were mostly on polytherapy, with a statistically significant difference (OR = 0.11; 95% CI, 0.01–0.91; P = .009).
Antiepileptic Drugs Used in Monotherapy Among Different Etiologies
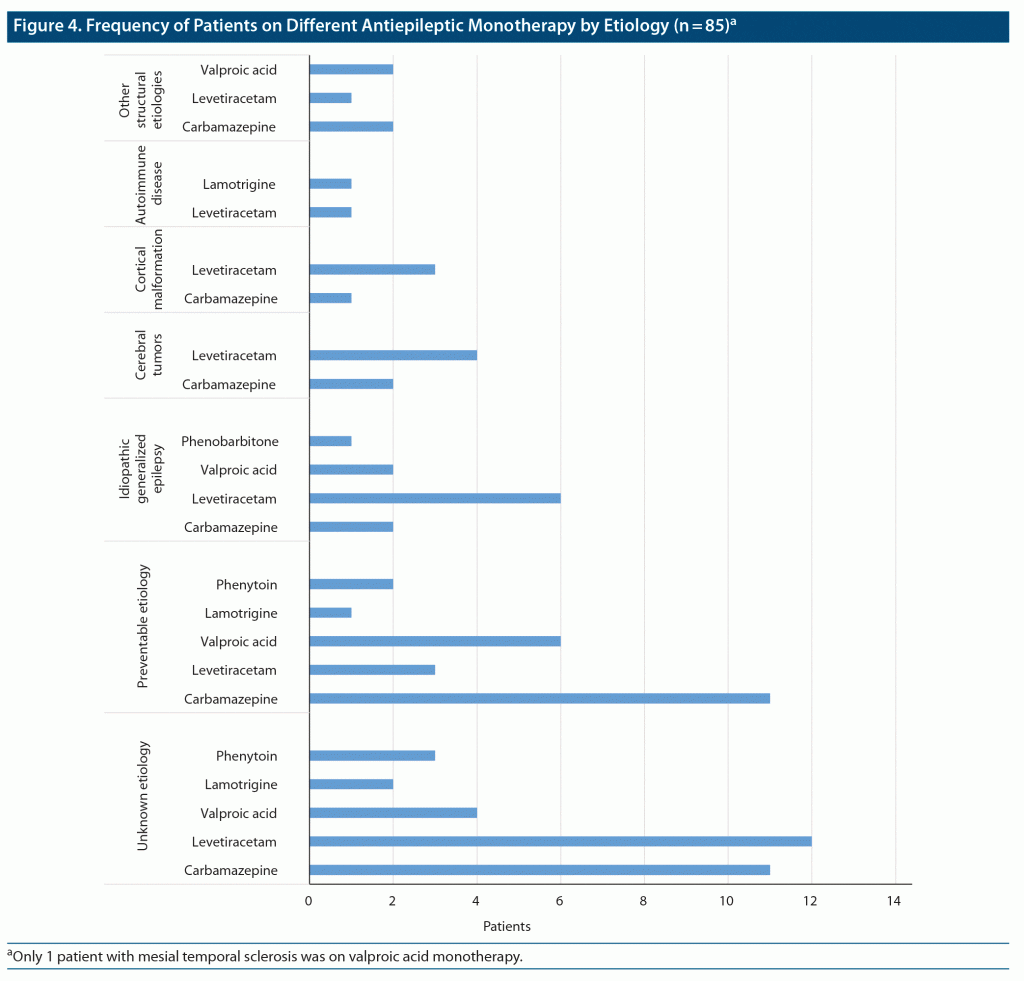
In the preventable etiologies group, only 23 (50%) patients were on monotherapy. Among these patients, the most prescribed drug was carbamazepine, which was used in 11 of 23 patients, followed by valproic acid, which was used in 6 of 23 patients. In patients with IGE, 11 (78.5%) were on monotherapy and levetiracetam was the most used (6/11), followed by valproic acid and carbamazepine, which were each used in 2 of 11 patients. Levetiracetam was also the predominant antiepileptic drug used in patients with cerebral tumors (4/6) and in the unknown etiology category (12/32), followed by carbamazepine in these etiologies (11/32) (Figure 4).
DISCUSSION
Our study showed some notable findings. Among the identifiable causes, the group with preventable etiologies (defined per the ILAE task force guidelines) had the highest proportion of patients with TBI, which was the most frequent identifiable cause in adult epileptic patients. Overall, TBI was the most common preventable cause of epilepsy, followed by stroke, HIE, and CNS infections. A meta-analysis by Thurman et al8 demonstrated a difference in the proportions of various types of preventable epilepsies according to the income status of countries. TBI and infectious etiology were shown to be more common in low-income countries. In high-income countries, stroke was a more frequent cause. Although Saudi Arabia is classified as a high-income country, our results demonstrated a combination of characteristics from both low- and high-income nations. Thus, there was a high prevalence of TBI and a very low frequency of CNS infections in the etiologic profile of our epileptic patients. The most common reason for TBI in our patients was road traffic accidents. The reason for a very low infectious etiology may be attributed to better living conditions, health, and hygiene among Saudi patients. Furthermore, the finding that adolescent epilepsy patients have a higher HIE etiology may refer to the need for better antenatal care of pregnant mothers in our communities.
Nearly one-third of our patients (38%) had epilepsy of unknown etiology despite going through adequate investigations including EEG, a 3 tesla MRI scan, and autoimmune testing and other workups when indicated. This finding is consistent with many studies9–13 that have demonstrated that etiology remains unclear in a significant number of epilepsy patients.
The median age at onset of epilepsy after TBI was 21 (range, 1–48) years, with a predominant male sex distribution, which emphasizes that young males need more education and awareness about road traffic safety, as road traffic accidents were the most common cause of TBI in our patients. However, a plausible explanation for the male predominance is that females had been prohibited to drive in Saudi Arabia until June 2018.14 Unfortunately, our data show that many victims of TBI that leads to chronic epilepsy are in the prime of their lives.
Seizure control was satisfactory in most patients, including those with preventable epilepsies. The only exception was epilepsy due to mesial temporal sclerosis, which had a statistically significant odds of unsatisfactory seizure control. However, mesial temporal sclerosis is less common than unknown and preventable etiologies, which both formed half of the unsatisfactory seizure control group of our patients (see Figure 3). Therefore, despite the better odds of satisfactory seizure control, preventable epilepsies still affect a sizable proportion of patients with unsatisfactory seizure control because of their high prevalence.
Almost half of our patients were on polytherapy. Epilepsies with preventable etiologies were no different, with a similar proportion of polytherapy. However, there were a couple of exceptions. Mesial temporal sclerosis, being the most refractory type of epilepsy, required polytherapy much more frequently, while IGE mostly required monotherapy. The use of polytherapy would understandably increase drug-related morbidity, including side effect profiles, drug interactions, and financial burden.
A routine EEG (which included activation procedures as per our departmental policy) does not seem to be a useful procedure for the detection of epileptiform discharges in epileptic patients. Our finding that there was a much lower sensitivity for EEG epileptiform activity in patients with preventable epilepsies was statistically significant when compared with all the other known and unknown etiologies. The reason for this low sensitivity is unknown and needs to be confirmed by more studies. Sleep EEG obtained by sleep deprivation, or a home-based ambulatory (including sleep) EEG recording, may be a better choice for such patients in cases in which an EEG recording is needed to make important clinical decisions.15
In patients with preventable epilepsies, clinicians still tend to favor older-generation drugs, including carbamazepine and valproic acid. Carbamazepine is used perhaps because of the focal nature of seizures in this type of epilepsy. It is interesting to note that levetiracetam was the preferred choice in patients with IGE and epilepsies with unknown etiology. Perhaps this preference indicates the broad-spectrum profile of levetiracetam that makes it useful.
Our study, apart from shedding light on a few important features of epilepsies according to their etiologies, also emphasizes the burden of epilepsies in our clinics that could have been prevented. The primary prevention of epilepsy is even more relevant at present, as recently there have been many advances in treating critically ill patients (including stroke, TBI, birth injuries, and CNS infections) with effective interventions. The increased effectiveness and availability of better management strategies for these conditions, resulting in increased survival of patients, may paradoxically put them at increased risk of developing chronic epilepsy.8 Thus, we believe that it is important to consider primary prevention strategies for epilepsies and to develop interventions targeting epileptogenesis.
This is the first study carried out in Saudi Arabia, to the best of our knowledge, that identified the proportion of preventable causes of epilepsy by diagnosing etiology using the 2017 ILAE classification system. Studies based on previous classification systems have lacked uniformity in definitions of different seizure types and etiologies, while the classifications themselves have been controversial.16 Compared to the previous classification, the latest system has been shown to have improvements, as well as better consistency in classifying different seizure types.17
Limitations and Strengths
Our results show a substantial proportion of preventable epilepsies in our patient population of a tertiary (level 3 epilepsy center) health care setting. However, we do not have evidence of similar proportions in the general population. Given the administrative structure of the study center/hospital, the patient sample is largely representative of Saudi nationals, as we believe the immigrant/expatriate population has a low representation in our clinics. As the services in this hospital are not limited by pay, we believe that our study sample may have represented all socioeconomic groups. Furthermore, some of the etiologic categories had a low number of cases, so their statistical significance could not be reliably evaluated. Therefore, we would recommend larger single or multicenter studies to evaluate epilepsy etiologies and outcomes using 2017 ILAE classifications. Moreover, we believe that this study sheds light on an important unmet need in epilepsy care from a public health perspective in Saudi Arabia that needs to be explored further.
CONCLUSIONS
Epilepsies with preventable etiologies constitute a substantial proportion of epilepsies among Saudi patients. Although seizure control in most of these epilepsies is satisfactory, they still put the patients at risk of polytherapy, drug interactions, psychological trauma, and social stigma. Effective primary prevention targeting these etiologies can thus be very useful.
Submitted: December 29, 2020; accepted March 21, 2021.
Published online: December 9, 2021.
Potential conflicts of interest: None.
Funding/support: None.
Acknowledgments: The authors acknowledge and express their sincere gratitude to Khurum H. Khan, MD (University College London Hospitals, NHS Foundation Trust), for revising the manuscript and giving his valuable suggestions, and the following undergraduate medical students from the College of Medicine, Imam Abdul Rahman Bin Faisal University, Saudi Arabia, for their contribution in data collection and hard work in carrying out this research project: Modhi Alajmi, MBBS; Amira Alolyani, MBBS; Sara Al Arhain, MBBS; Ashwaq Alanazi, MBBS; and Sara Al Mohammed Salem, MBBS. The acknowledged individuals report no conflicts of interest related to the subject of this article.
Supplementary material: See accompanying pages.
CLINICAL POINTS
- Preventable etiologies form a sizable proportion of epilepsy etiologies in Saudi patients.
- The most common preventable etiology of epilepsy is traumatic brain injury in adults.
- Primary prevention strategies may have a potential to reduce epilepsy burden in the Saudi population.
References (17)

- de Boer HM, Moshé SL, Korey SR, et al. ILAE/IBE/WHO Global Campaign Against Epilepsy: a partnership that works. Curr Opin Neurol. 2013;26(2):219–225. PubMed CrossRef
- al Rajeh S, Bademosi O, Ismail H, et al. A community survey of neurological disorders in Saudi Arabia: the Thugbah Study. Neuroepidemiology. 1993;12(3):164–178. PubMed CrossRef
- Beghi E, Giussani G, Sander JW. The natural history and prognosis of epilepsy. Epileptic Disord. 2015;17(3):243–253. PubMed CrossRef
- Altowayan R, Aloqaily H, Almutairi A, et al. Level of awareness and attitudes toward epilepsy in Qassim, Saudi Arabia: a cross-sectional study. Epilepsy Behav. 2019;90:66–69. PubMed CrossRef
- Fisher RS, Acevedo C, Arzimanoglou A, et al. ILAE official report: a practical clinical definition of epilepsy. Epilepsia. 2014;55(4):475–482. PubMed CrossRef
- Fisher RS, Cross JH, French JA, et al. Operational classification of seizure types by the International League Against Epilepsy: position paper of the ILAE Commission for Classification and Terminology. Epilepsia. 2017;58(4):522–530. PubMed CrossRef
- Scheffer IE, Berkovic S, Capovilla G, et al. ILAE classification of the epilepsies: position paper of the ILAE Commission for Classification and Terminology. Epilepsia. 2017;58(4):512–521. PubMed CrossRef
- Thurman DJ, Begley CE, Carpio A, et al. The primary prevention of epilepsy: a report of the Prevention Task Force of the International League Against Epilepsy. Epilepsia. 2018;59(5):905–914. PubMed CrossRef
- Hernández-Ronquillo L, Adams S, Ballendine S, et al. Epilepsy in an elderly population: classification, etiology and drug resistance. Epilepsy Res. 2018;140:90–94. PubMed CrossRef
- Aaberg KM, Surén P, Søraas CL, et al. Seizures, syndromes, and etiologies in childhood epilepsy: the International League Against Epilepsy 1981, 1989, and 2017 classifications used in a population-based cohort. Epilepsia. 2017;58(11):1880–1891. PubMed CrossRef
- Fiest KM, Sauro KM, Wiebe S, et al. Prevalence and incidence of epilepsy: a systematic review and meta-analysis of international studies. Neurology. 2017;88(3):296–303. PubMed CrossRef
- Chipaux M, Szurhaj W, Vercueil L, et al; GRENAT Group. Epilepsy diagnostic and treatment needs identified with a collaborative database involving tertiary centers in France. Epilepsia. 2016;57(5):757–769. PubMed CrossRef
- Besocke AG, Rosso B, Cristiano E, et al. Outcome of newly diagnosed epilepsy in older patients. Epilepsy Behav. 2013;27(1):29–35. PubMed CrossRef
- Saudi Arabia: Royal Decree Allows Women to Be Issued Driving Licenses October 3, 2017. Accessed November 30, 2021. loc.gov/law/foreign-news/article/saudi-arabia-royal-decree-allows-women-to-be-issued-driving-licenses/
- Thomaides TN, Kerezoudi EP, Chaudhuri KR, et al. Study of EEGs following 24-hour sleep deprivation in patients with posttraumatic epilepsy. Eur Neurol. 1992;32(2):79–82. PubMed CrossRef
- Panayiotopoulos CP. The new ILAE report on terminology and concepts for the organization of epilepsies: critical review and contribution. Epilepsia. 2012;53(3):399–404. PubMed CrossRef
- Gao H, Sander JW, Xiao Y, et al. A comparison between the 1981 and 2017 International League Against Epilepsy classification of seizure types based on an outpatient setting. Epileptic Disord. 2018;20(4):257–264. PubMed CrossRef
Enjoy this premium PDF as part of your membership benefits!