Prim Care Companion CNS Disord 2022;24(6):22cr03268
To cite: Valido R, Caldas F, Ferreira P. Severe catatonia following sudden withdrawal of quetiapine. Prim Care Companion CNS Disord. 2022;24(6):22cr03268.
To share: https://doi.org/10.4088/PCC.22cr03268
© 2022 Physicians Postgraduate Press, Inc.
aHospital Magalhães Lemos, Porto, Portugal
*Corresponding author: Rodrigo Valido, MD, Hospital de Magalhães Lemos, Rua Professor Álvaro Rodrigues, 4149-003 Porto, Portugal ([email protected]).
Catatonia is a syndrome characterized by psychomotor abnormalities. It is hypothesized to be associated with γ-aminobutyric acid (GABA) hypoactivity and involves functional alterations between the basal ganglia, thalamus, and cortex.1–3 First-line treatments are benzodiazepines or electroconvulsive therapy (ECT).1,2 Dopamine-blocking drugs should be avoided, as they can worsen or precipitate catatonia.1,2 We present a case depicting the development of severe catatonia after stopping quetiapine. Withdrawal catatonia is an uncommon condition with onset shortly after stopping a drug, primarily associated with benzodiazepines and clozapine.2
Case Report
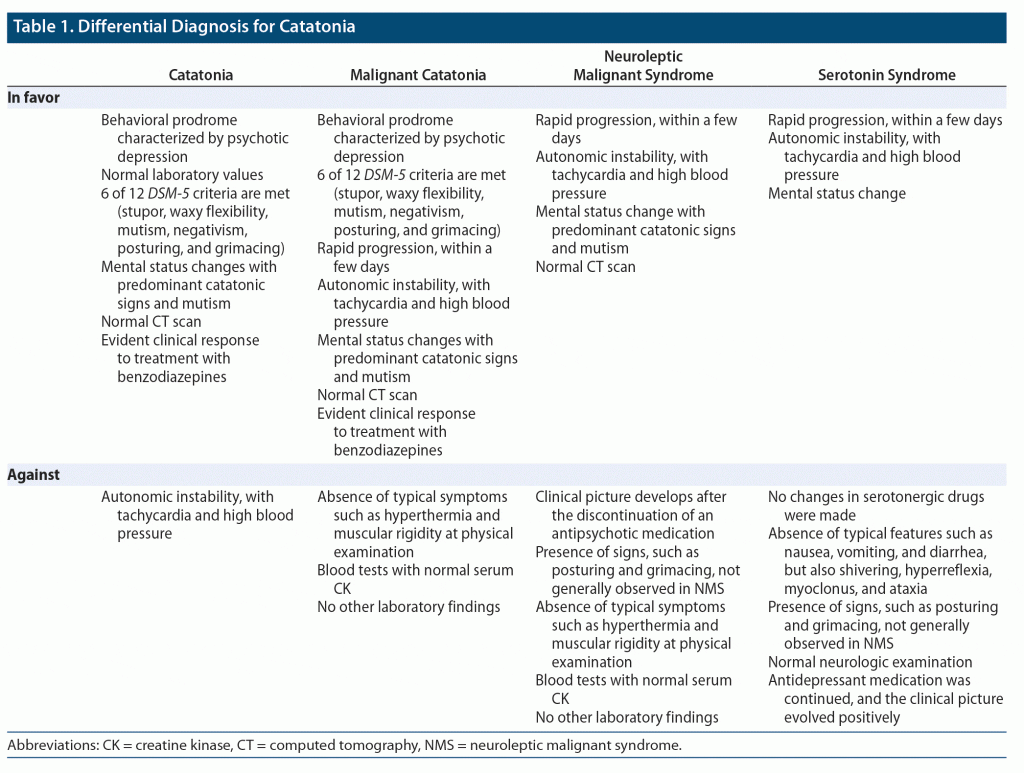
We present the case of a 66-year-old woman treated in the inpatient unit for severe psychotic depression. She was previously diagnosed with recurrent depressive disorder and had a prior hospitalization because of psychotic depression. We established a history of psychotic symptoms for 3 months, characterized by delusions of ruin and somatic concerns, concomitant with a severely depressed mood and anhedonia. On the 28th day of combined treatment with escitalopram (20 mg) plus quetiapine (600 mg), she developed intolerable side effects, namely severe lower limb edema and drowsiness. Upon evaluation, the internist physician advised the discontinuation of quetiapine. We discontinued quetiapine within 3 days, using low-dose olanzapine (5 mg/d) to prevent withdrawal symptoms. She developed a sudden catatonic syndrome 3 days later, scoring 28 points on the Bush-Francis Catatonia Rating Scale (BFCRS).4 Beyond the classic symptoms of extreme hypoactivity, nonresponse to painful stimuli, no speech, negativism, rigidity, waxy flexibility, and refusal to eat or drink, she presented autonomic instability, namely hypertension and tachycardia. We did not find alterations during the physical and neurologic examination. She required urgent intubation for nutritional support and the utilization of a urinary catheter due to acute urinary retention. She stayed under close monitoring. We excluded major medical precipitants, namely metabolic, infectious, or neurologic conditions, and all ancillary examination results were within normal limits (Table 1). Finally, we considered a differential diagnosis between neuroleptic malignant syndrome, serotonin syndrome, and malignant or severe catatonia, depicted in Table 1, and established a diagnosis of severe catatonia. At this point, we suspended olanzapine. ECT was not readily available. Treatment with clonazepam 1 mg (titrated to 8 mg) was started, with a significant improvement in overall symptoms on the first day, as her BFCRS score decreased from 28 to 20 points. One week later, the patient still presented psychomotor retardation, and the delusional ideas of somatic concerns emerged once more. We decided to introduce clozapine, slowly titrated to 100 mg/d, with excellent clinical response. On day 15, she improved significantly, presenting with only mild psychomotor retardation and no psychotic features. Her BFCRS score decreased to 0 points.
Discussion
Withdrawal symptoms associated with quetiapine, such as agitation, dysphoria, insomnia, and hypertension, have been previously reported.5 Still, to our knowledge, this is the first report of withdrawal catatonia due to quetiapine discontinuation. Withdrawal catatonia is mainly described with benzodiazepines and clozapine.1,2 Both medications are used as treatments for catatonia, suggesting the occurrence of “rebound” catatonia when discontinuing medications used to treat it. This phenomenon is possibly comparable to the emergence of psychosis after antipsychotic withdrawal, which is mainly associated with clozapine and occurs in approximately 20% of treatment-resistant patients who suddenly discontinue it.6 This may be related to the supersensitivity of dopamine receptors and cholinergic, serotonergic, and GABAergic systems.1,2,6 Similar to clozapine, quetiapine has a rapid dissociation from the D2 receptor and complex multireceptor interaction.7 There is some evidence that dopamine D2 receptor blockage is related to causing or worsening catatonia syndrome.6 We speculate that olanzapine initiation or the olanzapine plus quetiapine withdrawal could have worsened the catatonia features in this case. There are successful reports of quetiapine being used to treat schizophrenia with catatonic stupor.8 A combined effect of quetiapine and benzodiazepines is described in the treatment of catatonia.8 The etiology of withdrawal catatonia is not fully understood, and further research is required to understand the role that quetiapine may play in it.
Published online: December 29, 2022.
Relevant financial relationships: None.
Funding/support: None.
Previous presentation: This case was previously presented at the European Congress of Psychiatry Virtual Congress; July 4–7, 2020.
Patient consent: Consent was received from the patient to publish the case report, and information has been de-identified to protect anonymity.
ORCID: Rodreigo Valido: https://orcid.org/0000-0001-9114-0487
References (8)

- Edinoff AN, Kaufman SE, Hollier JW, et al. Catatonia: clinical overview of the diagnosis, treatment, and clinical challenges. Neurol Int. 2021;13(4):570–586. PubMed CrossRef
- Lander M, Bastiampillai T, Sareen J. Review of withdrawal catatonia: what does this reveal about clozapine? Transl Psychiatry. 2018;8(1):139. PubMed CrossRef
- Yeh AW, Lee JW, Cheng TC, et al. Clozapine withdrawal catatonia associated with cholinergic and serotonergic rebound hyperactivity: a case report. Clin Neuropharmacol. 2004;27(5):216–218. PubMed CrossRef
- Bush G, Fink M, Petrides G, et al. Catatonia. I. Rating scale and standardized examination. Acta Psychiatr Scand. 1996;93(2):129–136. PubMed CrossRef
- Monahan K, Cuzens-Sutton J, Siskind D, et al. Quetiapine withdrawal: a systematic review. Aust N Z J Psychiatry. 2021;55(8):772–783. PubMed CrossRef
- Moncrieff J. Does antipsychotic withdrawal provoke psychosis? Review of the literature on rapid onset psychosis (supersensitivity psychosis) and withdrawal-related relapse. Acta Psychiatr Scand. 2006;114(1):3–13. PubMed CrossRef
- Bastiampillai T, Woo WWL, Chan SKW, et al. Why does clozapine cause increased rebound psychosis and catatonia, compared to quetiapine? Aust N Z J Psychiatry. 2022;56(1):98. PubMed CrossRef
- Yoshimura B, Hirota T, Takaki M, et al. Is quetiapine suitable for treatment of acute schizophrenia with catatonic stupor? A case series of 39 patients. Neuropsychiatr Dis Treat. 2013;9:1565–1571. PubMed CrossRef
Enjoy this premium PDF as part of your membership benefits!