Prim Care Companion CNS Disord 2022;24(3):20cr02885
To cite: Silva-dos-Santos A, Costa S, Moitinho M. Transdermal fentanyl–induced seizures: case report and literature review. Prim Care Companion CNS Disord. 2022;24(3):20cr02885.
To share: https://doi.org/10.4088/PCC.20cr02885
© Copyright 2022 Physicians Postgraduate Press, Inc.
aNOVA Medical School, NOVA University of Lisbon, Lisbon, Portugal
bDepartment of Psychiatry, Hospital de Vila Franca de Xira, Vila Franca de Xira, Portugal
cDepartment of Neurology, Hospital de Vila Franca de Xira, Vila Franca de Xira, Portugal
dCentro Hospitalar Universitário de Lisboa Central, Lisbon, Portugal
*Corresponding author: Amílcar Silva-dos-Santos, MD, Department of Psychiatry, Hospital de Vila Franca de Xira, Estrada Carlos Lima Costa, n° 2, Vila Franca de Xira, 2600-009, Portugal ([email protected]).
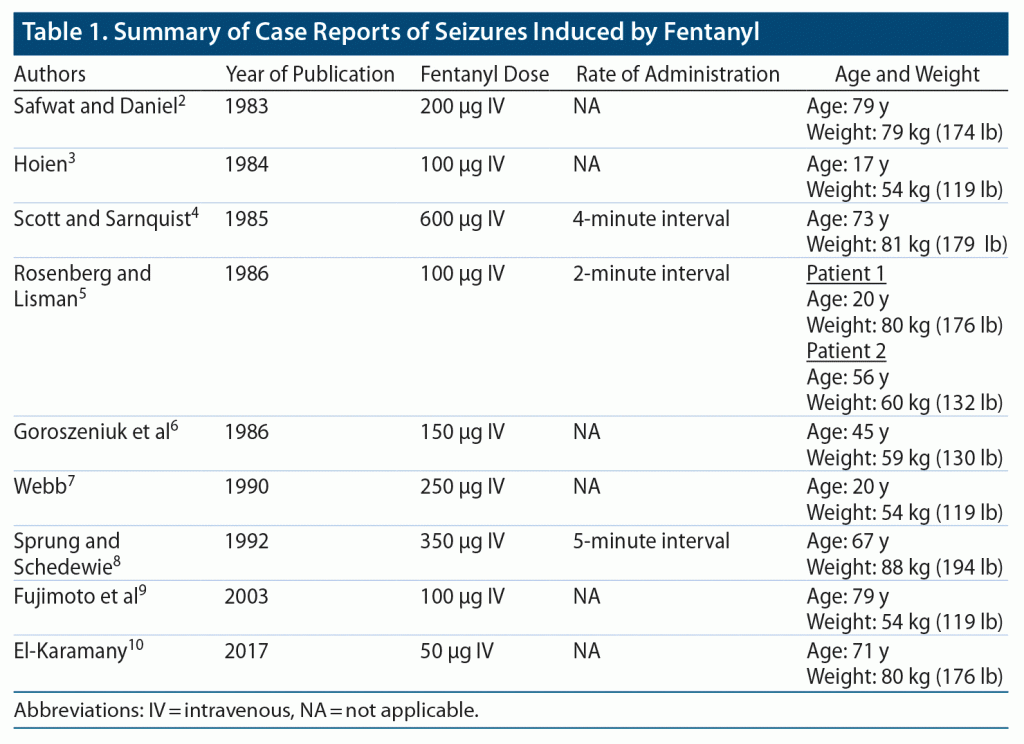
Fentanyl is a well-known opioid used in general anesthesia and pain management.1 Although opioids have anticonvulsant properties, they might have proconvulsant effects. Seizures caused by fentanyl are rare. As of this writing, only a few cases have been reported in humans (Table 12–10), namely in the setting of general anesthesia.2,8,11 Seizures after the administration of fentanyl in association with other drugs (such as lidocaine) have been reported in the literature.11
Case Report
Here, we report a case of seizure that occurred in a 46-year-old man treated in an ambulatory setting for chronic neuropathic back pain related to previous lumbar surgery. The patient’s medications included oral acetaminophen 1,000 mg and diazepam 5 mg, both if needed. A few hours after the first application of a fentanyl transdermal patch (50 µg), the patient was brought to the emergency department (ED) due to involuntary facial and limb movements. Upon his arrival, besides the Glasgow Coma Scale12 score of 11, his physical examination, laboratory workup, and neuroimaging results were within normal limits (Supplementary Material Topic 1). The neurologic examination revealed erratic involuntary movements of the 4 limbs, not rhythmic, uncoordinated, without tongue biting or sphincter incontinence. The movements lasted a few seconds with impaired awareness. Seizure onset and frequency were unknown.
After regaining consciousness, he had spasmodic speech without aphasia, with preserved oral comprehension and writing and reading abilities. The differential diagnoses included (1) epileptic seizures, (2) psychogenic nonepileptic seizures, (3) stroke, and (4) syncope. Stroke was ruled out due to the absence of focal or cortical signs as well as the normal computed tomography scan. Syncope was ruled out since the patient had no hemodynamic changes and his electrocardiogram was within normal limits. A psychiatric assessment was required due to the hypothesis of psychogenic nonepileptic seizures/conversion disorder (functional neurologic symptom disorder), with attacks or seizures (F44.5 according to DSM-5 criteria). The patient recalled a similar episode after treatment with tramadol. Moreover, there was no significant psychiatric symptom, psychosocial context suggesting psychological stress, or history of psychiatric medication. A final hypothesis of seizure induced by a substance or medication was considered. A literature search retrieved a few case reports of fentanyl-induced seizures, including 1 published in 2003 describing such a phenomenon after a 7-day fentanyl treatment in small doses with phenytoin.8
The definitive diagnosis was motor epileptic seizures with unknown onset (Supplementary Material Topic 2 provides the updated International League Against Epilepsy 2017 classification of epilepsy) induced by fentanyl. Hence, the psychiatrist decided to treat the patient with intravenous valproic acid (15 mg/kg in 30 minutes). The patient improved suddenly after approximately 20 minutes, with no specific symptom improvement pattern as seen in other conditions,13 and was discharged with oral valproic acid 1,000 mg once a day. One week later, in the outpatient clinic, he was asymptomatic. Three months later, he was reexamined and discharged since he remained symptom free.
Discussion
This is the first report, to our knowledge, to describe fentanyl-induced seizures in ambulatory care, rather than in the context of preoperative general anesthesia (as previously described in the literature). The exact mechanisms underlying seizures caused by fentanyl are not understood. However, these types of seizures are more likely to originate in the subcortical areas, which would not be detectable by surface electrodes. No electroencephalography was performed at the ED, which would reveal a pattern of drug-induced seizures.14 Scott and Sarnquist4 proposed that seizures can result from myoclonic movements due to the depression of inhibitory neurons or possibly that the abnormal movements might exacerbate muscular rigidity caused by even small doses of fentanyl. This report reminds psychiatrists and physicians to be aware of drug-induced seizures (namely related to opioids such as fentanyl, as in the current case).
Published online: June 16, 2022.
Relevant financial relationships: None.
Funding/support: None.
Patient consent: The patient signed informed consent, and information has been de-identified to protect anonymity.
Supplementary material: See accompanying pages.
References (14)

- Kuip EJM, Zandvliet ML, Koolen SLW, et al. A review of factors explaining variability in fentanyl pharmacokinetics; focus on implications for cancer patients. Br J Clin Pharmacol. 2017;83(2):294–313. PubMed CrossRef
- Safwat AM, Daniel D. Grand mal seizure after fentanyl administration. Anesthesiology. 1983;59(1):78. PubMed CrossRef
- Hoien AO. Another case of grand mal seizure after fentanyl administration. Anesthesiology. 1984;60(4):387–388. PubMed CrossRef
- Scott JC, Sarnquist FH. Seizure-like movements during a fentanyl infusion with absence of seizure activity in a simultaneous EEG recording. Anesthesiology. 1985;62(6):812–814. PubMed CrossRef
- Rosenberg M, Lisman SR. Major seizure after fentanyl administration: two case reports. J Oral Maxillofac Surg. 1986;44(7):577–579. PubMed CrossRef
- Goroszeniuk T, Albin M, Jones RM. Generalized grand mal seizure after recovery from uncomplicated fentanyl-etomidate anesthesia. Anesth Analg. 1986;65(9):979–981. PubMed CrossRef
- Webb MD. Seizure-like activity during fentanyl anesthesia: a case report. Anesth Prog. 1990;37(6):306–307. PubMed
- Sprung J, Schedewie HK. Apparent focal motor seizure with a jacksonian march induced by fentanyl: a case report and review of the literature. J Clin Anesth. 1992;4(2):139–143. PubMed CrossRef
- Fujimoto T, Nishiyama T, Hanaoka K. Seizure induced by a small dose of fentanyl. J Anesth. 2003;17(1):55–56. PubMed CrossRef
- El-Karamany M. Case study and review article: epilepsy-like movements induced by fentanyl analgesia. Egypt J Intern Med. 2017;29(2):86–90. CrossRef
- Hsieh XX, Hsu YC, Cherng CH, et al. Grand mal seizure induced by low-dose fentanyl and lidocaine in a young child. Acta Anaesthesiol Taiwan. 2015;53(3):105–108. PubMed CrossRef
- Sternbach GL. The Glasgow Coma Scale. J Emerg Med. 2000;19(1):67–71. PubMed CrossRef
- Silva-Dos-Santos A, Venda D, Sales MB, et al. Bottom-up neuroanatomical pattern of symptom remission in melancholic depression after electroconvulsive therapy: a case report and literature review. Psychogeriatrics. 2021;21(2):252–254. PubMed CrossRef
- Silva-Dos-Santos A. The hypothesis of connecting two spinal cords as a way of sharing information between two brains and nervous systems. Front Psychol. 2017;8:105. PubMed CrossRef
Enjoy this premium PDF as part of your membership benefits!