ABSTRACT
Objective: To examine the funding priorities of the National Institute of Mental Health (NIMH) since 2016 to assess whether NIMH was continuing to prioritize basic research at the expense of clinical research.
Methods: Six psychiatric disorders (schizophrenia, bipolar disorder, depression, anxiety disorders, eating disorders, autism) were assessed using 2 publicly available data sources (ClinicalTrials.gov and the National Institutes of Health Research, Condition, and Disease Categorization [RCDC]) to determine the degree of NIMH support for drug trials and research on these disorders in general since 2016.
Results: From 2017 through 2022, ClinicalTrials.gov lists just 1 drug trial each for schizophrenia and bipolar disorder. The RCDC database for 2016 through 2021 shows that NIMH support for research projects on schizophrenia and bipolar disorder decreased by 22% and 20%, respectively. During that time, Congress increased the budget of NIMH by 40%.
Conclusions: NIMH has continued to prioritize basic research over clinical trials, resulting in a steep decline in funding for possible treatments for the most serious and costly psychiatric diseases.
Prim Care Companion CNS Disord 2023;25(4):23m03486
Author affiliations are listed at the end of this article.
Schizophrenia and bipolar disorder, especially the more severe form of bipolar I, are among the most important and difficult to treat psychiatric diseases. These diagnoses cover the majority of seriously mentally ill individuals found among the homeless, in jails and prisons, and in nursing homes. A recent prevalence study1 of schizophrenia, based on Medicare and Medicaid data, estimated that 3.8 million Americans are affected. The National Institute of Mental Health (NIMH) claims that 2.5% of Americans, or 5.2 million people, have “serious bipolar disorder.”2 Together these diseases affect approximately 9 million Americans.
Schizophrenia and bipolar disorder are also among the most expensive diseases. The economic burden of schizophrenia in 2019 in the US was reported to be $343.2 billion, including $62.3 billion in direct health care costs.3 The economic burden of bipolar I disorder in 2015 was reported to be $202.1 billion, including $50.9 billion in direct health care costs.4 One reason for these high costs is the lack of effective treatments for many patients. Thus, together these 2 diseases cost the US $545 billion, which is 12 times greater than the $45 billion budget for the entire National Institutes of Health (NIH) and dwarfs the annual $2.2 billion budget of NIMH. In addition to humanitarian reasons, one might think that based on cost issues alone NIMH should prioritize research to improve the treatment of these diseases.
For the past quarter century such prioritization has not been the case. Traditionally, NIMH has divided its research portfolio approximately evenly between clinical research, designed to help individuals currently affected, and basic research, intended to develop better treatments for the future. That distribution began to change in 1996 when Harold Varmus, MD, a cancer researcher who was then the NIH director, recruited Steven Hyman, MD, to be the new director of NIMH. Dr Varmus told Dr Hyman that NIMH was “a mess” with a research portfolio that was “antiquated and incoherent.”5 It would be Dr Hyman’s job, Dr Varmus said, “to fix it,” using his training in molecular neurobiology and other scientific approaches.5 At that time, the Human Genome Project was also moving forward and promising to discover major genes that would lead to better treatments for most human diseases, including schizophrenia and bipolar disorder.
Between 1996 and 2001, Dr Hyman began to transfer funds from clinical research, including research on schizophrenia and bipolar disorder, to basic research projects, especially genetic studies. This transfer accelerated under Thomas Insel, MD, who became the NIMH director in 2002. In 2022, Dr Insel acknowledged that he had “bet big on genomics.”6 By 2015, the final year of Dr Insel’s NIMH tenure, he estimated that clinical research at NIMH had been reduced to 10% of the research portfolio.7
In 2016, Joshua Gordon, MD, was appointed to be the next NIMH director. Immediately following his appointment, research colleagues published op-eds in the New York Times7 and the Washington Post8 encouraging Dr Gordon to increase clinical research to achieve a more balanced portfolio. In 2018 and 2019, we conducted studies to ascertain whether Dr Gordon had done so.9,10 We found that there had been a 90% reduction in drug treatment trials for schizophrenia, bipolar disorder, and depression between 2006–2009 and 2016–2019.11 We also reported that between 2016 and 2019, NIMH decreased research projects on schizophrenia by 17.5% and on bipolar disorder by 25%. Thus, in the first 3 years of Dr Gordon’s tenure as NIMH director, there was no evidence that he was restoring a balanced research portfolio. We are now updating that assessment to include data covering 2020 to 2022.
METHODS
Two public databases were used to assess the NIMH research portfolio. ClinicalTrials.gov is a web-based resource managed by the National Library of Medicine. It was accessed on November 1, 2022, with the following specifications:
Advanced search
Name of the disease: eg, schizophrenia, bipolar disorder, depression, anxiety disorders, eating disorders, autism
Study type: interventional studies
Intervention/treatment: drug trial
Sponsor/collaborator: NIMH
Funder type: National Institutes of Health
Study start: from 01/01/2017 to 12/31/2022
The second database used in the study was the NIH Research, Condition, and Disease Categorization (RCDC) database mandated by Congress in 2008. This database lists all research projects funded by NIH for 309 diseases and conditions and was available through 2021. The project information includes an abstract, a statement on public health relevance, and the grant’s funding history.
RESULTS
ClinicalTrials.gov identified only 1 drug trial for schizophrenia funded by NIMH during the 6-year period from 2017 through 2022. This was a 2022 randomized clinical trial of clozapine to assess its effectiveness in preventing violent behavior. Similarly, ClinicalTrials.gov identified only one drug trial for bipolar disorder funded by NIMH for this period. This was a 2021 comparison of intramuscular ketamine versus midazolam for the treatment of suicidal patients seen in an emergency department. For the other drug trials, ClinicalTrials.gov identified 12 drug trials for the treatment of depression, 2 for the treatment of anxiety disorders, and none for the treatment of autism or eating disorders.
The RCDC database was used to assess the total number of research grants, the total amount spent on these grants, and that number as a percentage of the total NIMH budget for the years 2016 through 2021 for the same 6 psychiatric disorders. In 2016, NIMH funded 496 research grants on schizophrenia, which accounted for 13.9% of the total NIMH budget. The number of grants decreased over the following 5 years so that in 2021 NIMH funded only 389 schizophrenia grants, a decrease of 22%, accounting for only 10.1% of the total NIMH budget. The grants that were funded were shown in a previous study11 to be largely focused on basic brain research and unlikely to lead to clinical improvement. Similarly, the trajectory for NIMH-funded grants for bipolar disorder was also progressively downward. In 2016, NIMH funded 147 bipolar disorder grants, which accounted for 5.3% of the total NIMH budget; however, by 2021 the number of such grants had been reduced to 117, a reduction of 20%, accounting for only 4.2% of the total NIMH budget. In contrast to this downward trajectory, the number of NIMH-funded grants for depression increased from 592 to 676, an increase of 15%; anxiety disorders increased from 278 to 318, an increase of 14%; eating disorders increased from 47 to 63, an increase of 34%; and for autism there was no notable change, from 312 to 310.
DISCUSSION
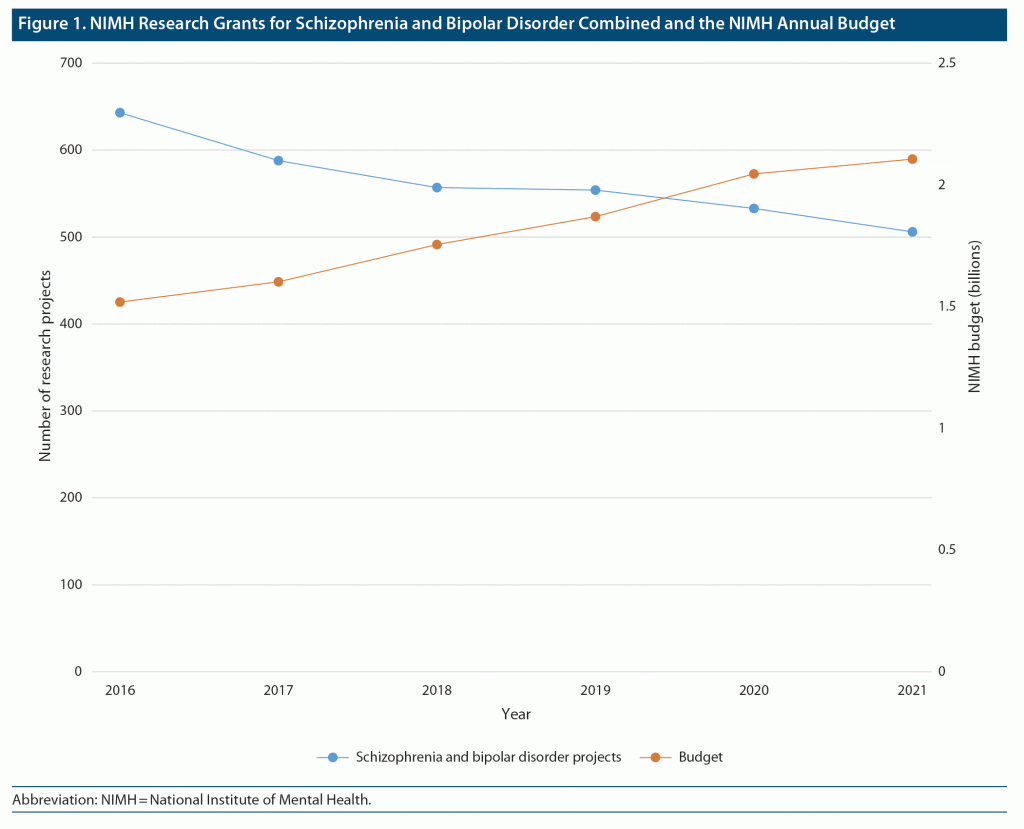
In this updated analysis for the NIMH research portfolio, the most striking finding is the decrease in funding for schizophrenia and bipolar disorder research in general, and specifically the almost complete failure to fund drug trials to improve the treatment of these diseases. Given that approximately 9 million Americans are affected, that these are among the most expensive diseases, and the obvious need for better treatments, such a failure is inexplicable. It should also be noted that this failure occurred during years in which Congress was giving NIMH among the largest budget increases the institute had ever received. Between 2016 and 2021, the NIMH budget increased from $1.5 billion to $2.1 billion, an increase of 40%. Indeed, as Figure 1 illustrates, it appears that the more money Congress gives to NIMH, the less research it does on schizophrenia and bipolar disorder.
There are additional reasons for NIMH to support more clinical research in general. A 2014 study by the RAND Corporation reported that “clinical research has had a larger impact on patient care than basic research has over the 20 years since the research was undertaken.”12(xiii) A 2022 analysis of NIMH’s failure to do adequate clinical research lists among its consequences “ignoring patient care, stifling clinical advancement, and impoverishing a rich area of intellectual endeavor.”13(e2) Of course there is clinical research that does not get done as clinical resources are shifted to basic studies. Among the promising clinical leads for developing better treatments for schizophrenia that NIMH has failed to adequately pursue, for example, are research on infectious and immune abnormalities, neurohormones, and the use of probiotics and other agents to modulate the microbiome and the gut-brain axis.
In his defense, Dr Gordon claims that investing heavily in basic research will ultimately lead to better treatments. In a summary of this approach, he cites the development of brexanolone, a drug recently approved for the treatment of postpartum depression, as a model but fails to mention that the interval between the basic research and the drug’s successful development was 35 years.14 As part of its basic research plan, NIMH has invested heavily in genetics research for more than 20 years with almost nothing therapeutically to show for it. Genetic linkage analysis findings could not be replicated.15 The results of candidate gene studies fared equally poorly, including more than 1,000 candidate genes for schizophrenia alone at a cost of approximately $250 million.16 These studies were followed by genome-wide association studies in hopes of identifying a few genes of major effect that could be targeted therapeutically. Instead, what has been found for schizophrenia, bipolar disorder, and depression are hundreds of genes of small effect and little chance of being targeted therapeutically.17
Basic research certainly has a place in the development of better medications, but it should not dominate the field. Dr Gordon’s plan, as exemplified in the NIMH Strategic Plan for Research for 2020–2024,18 continues to emphasize basic research, especially genetics and neural circuits.10 Dr Gordon’s plan was reinforced by Dr Insel, who recently suggested that NIMH should “double down on brain research.”6 It appears to be time for a public reexamination of the NIMH research portfolio.
Article Information
Published Online: August 1, 2023. https://doi.org/10.4088/PCC.23m03486
© 2023 Physicians Postgraduate Press, Inc.
Submitted: January 13, 2023; accepted March 15, 2023.
To Cite: Torrey EF, Simmons WW, Dailey L. The NIMH research portfolio: an update. Prim Care Companion CNS Disord. 2023;25(4):23m03486.
Author Affiliations: Stanley Medical Research Institute, Rockville, Maryland (Torrey, Simmons); Treatment Advocacy Center, Arlington, Virginia (Torrey, Dailey).
Corresponding Author: E. Fuller Torrey, MD, 6204 Ridge Drive, Bethesda, MD 20816 ([email protected]).
Relevant Financial Relationships: None.
Funding/Support: None.
Additional Information: The original data for the clinical trials dataset can be found at ClinicalTrials.gov. The original data for the NIH Research, Condition, and Disease database can be found at https://report.nih.gov/funding/categorical-spending#/.
Clinical Points
- The failure of the National Institute of Mental Health to support treatment trials research results in fewer treatment options for clinicians.
- The failure of the Human Genome Project to identify psychiatric genes of major effect that could be used to develop new treatments, as promised, has resulted in fewer treatment options for clinicians.
References (18)

- Mojtabai R. Estimating the prevalence of schizophrenia in the United States using the multiplier method. Schizophr Res. 2021;230:48–49. PubMed CrossRef
- National Institute of Mental Health. Bipolar disorder. Accessed June 29, 2023. https://www.nimh.nih.gov/health/statistics/bipolar-disorder
- Kadakia A, Catillon M, Fan Q, et al. The economic burden of schizophrenia in the United States. J Clin Psychiatry. 2022;83(6):22m14458. PubMed CrossRef
- Cloutier M, Greene M, Guerin A, et al. The economic burden of bipolar I disorder in the United States in 2015. J Affect Disord. 2018;226:45–51. PubMed CrossRef
- Hyman SE. Steven E. Hyman. Curr Biol. 2018;28(1):R6–R8. PubMed CrossRef
- Barry E. The “nation’s psychiatrist” takes stock, with frustration. New York Times. February 22, 2022. Accessed June 29, 2023. https://www.nytimes.com/2022/02/22/us/thomas-insel-book.html
- Markowitz JC. There is such a thing as too much neuroscience. New York Times. October 14, 2016. Accessed June 29, 2023. https://www.nytimes.com/2016/10/15/opinion/theres-such-a-thing-as-too-much-neuroscience.html
- Lewis-Fernandez R. In mental health research, NIH needs to focus less on tomorrow and more on today. The Washington Post. October 13, 2016. Accessed June 29, 2023. https://www.washingtonpost.com/opinions/in-mental-health-research-nih-needs-to-focus-less-on-tomorrow-and-more-on-today/2016/10/13/37d09d7a-5da4-11e6-9d2f-b1a3564181a1_story.html
- Torrey EF, Yolken RH, Lamb HR. NIMH drug trials for schizophrenia. J Clin Psychiatry. 2019;80(1):18com12597. PubMed CrossRef
- Torrey EF, Simmons WW, Hancq ES, et al. The continuing decline of clinical research on serious mental illnesses at NIMH. Psychiatr Serv. 2021;72(11):1342–1344. PubMed CrossRef
- Torrey EF, Knable MB, Rush AJ, et al. Using the NIH research, condition and disease categorization database for research advocacy: schizophrenia research at NIMH as an example. PLoS One. 2020;15(11):e0241062. PubMed CrossRef
- Wooding S, Pollitt A, Castle-Clarke S, et al. Mental Health Retrosight: Understanding the Returns From Research (Lessons From Schizophrenia): Policy Report. Santa Monica, CA: RAND Corporation; 2013.
- Markowitz JC, Milrod BL. Lost in translation: the value of psychiatric clinical trials. J Clin Psychiatry. 2022;83(6):22com14647. PubMed CrossRef
- Gordon JA. From neurobiology to novel medications: a principled approach to translation. Am J Psychiatry. 2019;176(6):425–427. PubMed CrossRef
- DeLisi LE. A critical overview of recent investigations into the genetics of schizophrenia. Curr Opin Psychiatry. 1999;12(1):29–39. CrossRef
- Sullivan PF. How good were candidate gene guesses in schizophrenia genetics? Biol Psychiatry. 2017;82(10):696–697. PubMed CrossRef
- Trubetskoy V, Pardiñas AF, Qi T, et al; Indonesia Schizophrenia Consortium; PsychENCODE; Psychosis Endophenotypes International Consortium; SynGO Consortium; Schizophrenia Working Group of the Psychiatric Genomics Consortium. Mapping genomic loci implicates genes and synaptic biology in schizophrenia. Nature. 2022;604(7906):502–508. PubMed CrossRef
- National Institute of Mental Health. NIMH Strategic Plan. Accessed June 29, 2023. https://www.nimh.nih.gov/about/strategic-planning-reports
This PDF is free for all visitors!