Objective: To examine the quality of a broad range of life domains using both quantitative and qualitative methodologies.
Method: Forty-eight individuals seeking inpatient treatment for an eating disorder (mean age = 29.8 years, female = 100%, white = 96.4%) from 2007 to 2009 completed the Quality of Life Inventory (QOLI) and the Eating Disorder Examination Questionnaire; a medical chart review confirmed diagnosis and treatment history. Patients diagnosed with anorexia nervosa (n = 24) and bulimia nervosa (n = 24) were compared. Body mass index (kg/m2), treatment history, number of comorbid psychiatric conditions, and eating disorder severity were used to predict quality of life. Finally, an inductive content analysis was performed on qualitative QOLI responses to contextualize the quantitative findings.
Results: Participants with anorexia nervosa, compared to those with bulimia nervosa, reported significantly less satisfaction with the domain of relatives (F1,46 = 5.35; P = .025); no other significant group differences were found. The only significant predictor of QOLI global score was number of previous treatments (F1,41 = 8.67; P = .005; R2 = 0.175). Content analysis of qualitative data yielded complementary findings to the quantitative data; interesting group differences emerged for satisfaction with health with implications for measuring quality of life domains.
Conclusions: Across several life domains, individuals seeking treatment for anorexia nervosa and bulimia nervosa appear to have similar levels of satisfaction, as evidenced by numeric and descriptive responses. Satisfaction with relatives, however, appears to differ between groups and suggests a specific target for intervention among patients in treatment for anorexia nervosa (eg, a family-based intervention such as the Maudsley approach). The use of quantitative and qualitative assessments, such as the QOLI, provides more clinically meaningful, contextualized information about quality of life than traditional self-report assessments alone.
Quantitative and Qualitative Analysis of the
Quality of Life of Individuals With Eating Disorders
ABSTRACT
Objective: To examine the quality of a broad range of life domains using both quantitative and qualitative methodologies.
Method: Forty-eight individuals seeking inpatient treatment for an eating disorder (mean age = 29.8 years, female = 100%, white = 96.4%) from 2007 to 2009 completed the Quality of Life Inventory (QOLI) and the Eating Disorder Examination Questionnaire; a medical chart review confirmed diagnosis and treatment history. Patients diagnosed with anorexia nervosa (n = 24) and bulimia nervosa (n = 24) were compared. Body mass index (kg/m2), treatment history, number of comorbid psychiatric conditions, and eating disorder severity were used to predict quality of life. Finally, an inductive content analysis was performed on qualitative QOLI responses to contextualize the quantitative findings.
Results: Participants with anorexia nervosa, compared to those with bulimia nervosa, reported significantly less satisfaction with the domain of relatives (F1,46 = 5.35; P = .025); no other significant group differences were found. The only significant predictor of QOLI global score was number of previous treatments (F1,41 = 8.67; P = .005; R2 = 0.175). Content analysis of qualitative data yielded complementary findings to the quantitative data; interesting group differences emerged for satisfaction with health with implications for measuring quality of life domains.
Conclusions: Across several life domains, individuals seeking treatment for anorexia nervosa and bulimia nervosa appear to have similar levels of satisfaction, as evidenced by numeric and descriptive responses. Satisfaction with relatives, however, appears to differ between groups and suggests a specific target for intervention among patients in treatment for anorexia nervosa (eg, a family-based intervention such as the Maudsley approach). The use of quantitative and qualitative assessments, such as the QOLI, provides more clinically meaningful, contextualized information about quality of life than traditional self-report assessments alone.
Prim Care Companion CNS Disord
2015;17(2):doi:10.4088/PCC.14m01667
© Copyright 2015 Physicians Postgraduate Press, Inc.
Submitted: April 26, 2014; accepted January 27, 2015.
Published online: April 30, 2015.
Corresponding author: Lauren O. Pollack, MA, Department of Psychology, University of Missouri–Kansas City, 5030 Cherry St, Kansas City, MO, 64110 ([email protected]).
Quality of life is important to assess in individuals with eating disorders because it provides information about how an individual is experiencing his or her eating disorder, serves as a proxy for assessing quality of care and clinical effectiveness, and has come to influence insurance reimbursement decisions for medical care.1,2 Quality of life measures can also aid clinical practice3 by giving patients the opportunity to communicate how their disease or disorder affects other aspects of their life, broadening the perspective from disorder symptoms to life domains. Together, patients and practitioners can identify and prioritize other problems. These measures can also be helpful to evaluate treatment progress and outcome.3
Individuals diagnosed with anorexia nervosa and bulimia nervosa have considerably impaired quality of life in comparison to healthy individuals.2,4–9 Similarities and differences in the quality of life of individuals with anorexia nervosa compared to those with bulimia nervosa, however, are less clear. Some studies have found that patients with anorexia nervosa report worse quality of life than patients with bulimia nervosa. For example, Abraham et al10 found that inpatients with anorexia nervosa reported worse quality of life on the Quality of Life for Eating Disorders compared to those with bulimia nervosa. Keilen and colleagues11 found the same pattern using a generic quality of life measure (Nottingham Health Profile). Other studies have found the opposite pattern, such that individuals with bulimia nervosa report worse quality of life than those with anorexia nervosa. For example, Muñoz and colleagues12 found that individuals with bulimia nervosa reported worse quality of life on all domains of the Health Related Quality of Life for Eating Disorders. Mond and colleagues4 found similar results using a generic quality of life questionnaire (World Health Organization Brief Quality of Life Assessment Scale). Finally, others found no difference between eating disorder diagnostic groups using a generic health-related quality of life questionnaire (Medical Outcomes Study 36-item Short-Form Health Survey9,13,14) and an eating disorder–specific quality of life questionnaire (Eating Disorders Quality of Life15).
Independent of diagnosis, correlates of quality of life among individuals with eating disorders have been explored. For example, Bamford and Sly16 found that eating disorder severity (derived from global Eating Disorder Examination Questionnaire [EDEQ] scores) and body mass index (BMI), but not duration of eating disorder, were significant predictors of worse quality of life. Additionally, psychiatric comorbidity was found to contribute to worse quality of life in individuals with an eating disorder.17 Gonzalez-Pinto and colleagues17 found that irrespective of specific comorbid disorder, psychiatric comorbidity negatively impacted aspects of quality of life.
Contradictory and complex results with respect to eating disorder diagnosis and correlates may be related to the way in which quality of life is measured. Numerous quality of life measures exist, including generic, health-related, and eating disorder–specific quality of life measures. Each type of measure includes advantages and disadvantages; generic quality of life measures are advantageous because they permit comparisons across disease states and fulfill clinical utility of identifying how a disease or disorder broadly impacts various aspects of life. A recent study by Mitchison and colleagues18 found support for use of a generic quality of life measure, the Medical Outcomes Study 12-item Short-Form Health Survey, as a valid measure of quality of life impairment in patients with anorexia nervosa. The Quality of Life Inventory (QOLI) is a generic quality of life measure that allows for the collection of both quantitative and qualitative data for 16 life domains.19 This measure offers some advantages over other generic quality of life measures. The QOLI considers the importance of each life domain as well as the individual’s satisfaction with it, yielding weighted scores for each domain and an average global score. The measure also allows individuals to write comments about each domain, producing complimentary qualitative data. This feature addresses the main weakness of generic quality of life measures, which is that they are not sensitive to specific symptoms, because individuals are able to write about their specific symptoms and experiences. A notable strength of integrating qualitative and quantitative data using a mixed-methods approach is that quantitative data may be contextualized by thorough investigation of patients’ perspectives. Previous studies on quality of life and eating disorders have not used weighted measures that consider the importance of a domain, nor have they used measures that solicit qualitative data. Given some of the mixed findings in the literature, this approach may add insight or clarification to some of these findings.
Thus, this study aims to add to the literature on quality of life and eating disorders by assessing life domains that have not been evaluated previously and by providing a richer descriptive explanation of quality of life impairments. The QOLI was selected because it comprehensively assesses a variety of life domains that are not captured using eating disorder–specific quality of life measures, and it allows individuals to further explain in writing their self-reported numeric ratings for each domain. In addition, to our knowledge, no data about use of the QOLI with an eating disorder population have been published. The QOLI scores for the anorexia nervosa and bulimia nervosa groups will be compared, and the association of eating disorder symptoms, previous treatments, number of comorbid disorders, and BMI to QOLI scores will be examined. Finally, a content analysis of qualitative data will be performed to better understand why quality of life across several life domains is impaired for individuals with an eating disorder from a first-person perspective. On the basis of the literature reviewed, we predict there will be no significant differences on global quality of life for the anorexia nervosa and bulimia nervosa groups; however, we hypothesize that there will be differences in the domains of relatives and friends.11 We also hypothesize that BMI and comorbidity will be significantly related to global QOLI, consistent with previous studies.
METHOD
Participants and Recruitment
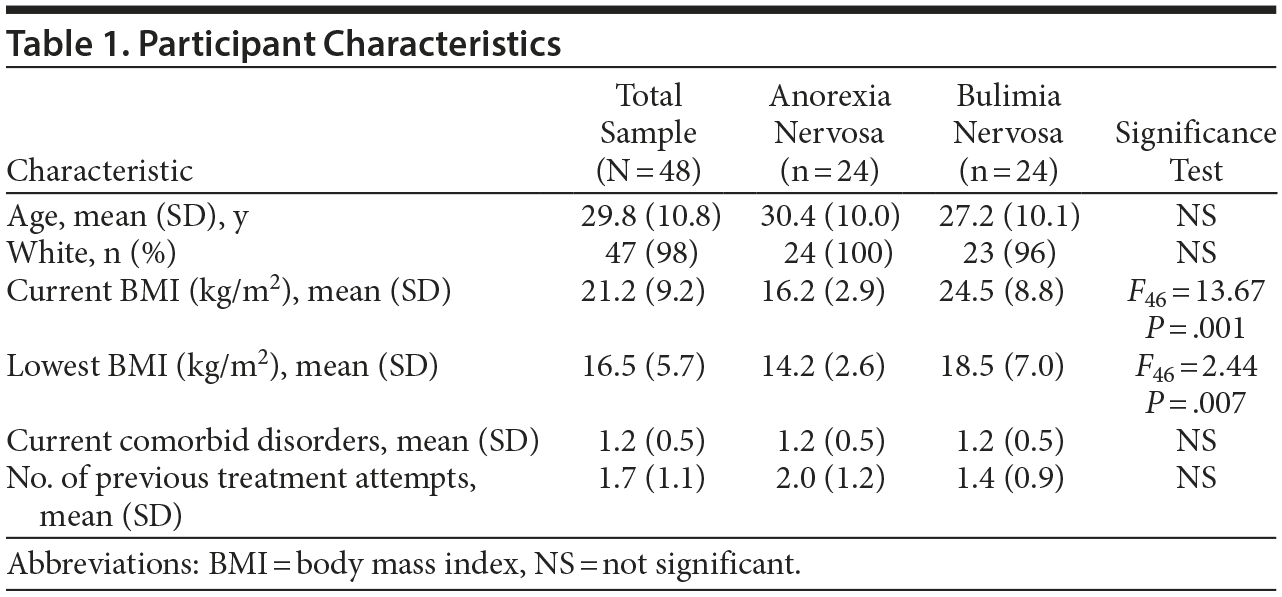
These data were collected as part of a larger study examining general eating disorder symptoms, treatment history, and caregiver experiences among patients admitted to an inpatient eating disorder treatment unit within a community hospital. Eligible participants included all males and females consecutively admitted to the treatment unit from 2007 to 2009. The unit intake coordinator informed 141 patients about the study during their intake assessment; 52 patients provided consent and/or assent (in the case of minors) for participation and completed all measures. Self-report measures were administered by psychology doctoral student research assistants. Table 1 presents participant characteristics; 2 males and 2 individuals diagnosed with an eating disorder not otherwise specified were removed from the sample for analyses. This study was approved by the Institutional Review Board at the University of Missouri–Kansas City.
Measures
Patient medical records. Patient medical records were reviewed by psychology doctoral student research assistants to obtain eating disorder diagnosis according to the DSM-IV-TR, age, ethnicity, other psychiatric diagnoses, and current BMI. Research assistants obtained supplemental information about eating disorder treatment history (ie, number of previous treatments) and self-reported lowest BMI from participants at the time self-report measures were administered.
EDE-Q. The EDE-Q20 is a 28-item self-report questionnaire based on the Eating Disorder Examination Interview. The EDE-Q demonstrates acceptable to excellent internal consistency (Cronbach α = 0.70–0.95).21,22 In the current study, the Cronbach α for the global score was 0.89, indicating good reliability. This measure was used as an index of eating disorder severity in the regression analysis predicting global QOLI scores.
Quality of Life. The QOLI23 assesses satisfaction across 16 life domains. For each domain, an importance and satisfaction score is obtained and multiplied to yield a weighted score. The global score, an indication of overall satisfaction with quality of life, is the average of each domain. The QOLI also permits the test taker to write about specific problems that interfere with satisfaction in each domain in an open-ended format, thereby contextualizing quantitative self-report responses. Finally, the QOLI was selected to meet the needs of the larger multi-aim study, which included evaluating caregiver quality of life. The QOLI demonstrates acceptable to good internal consistency (Cronbach α = 0.77–0.89) in various samples.19 In the current study, the Cronbach α was 0.74, indicating acceptable reliability.
Statistical Analyses
Quantitative analyses. A 1-way analysis of variance with Bonferroni correction for multiple comparisons was conducted to compare the mean QOLI global and domain scores for participants with anorexia nervosa and bulimia nervosa. To predict global quality of life scores, a stepwise regression analysis with backward elimination was conducted to determine whether the variables of BMI, eating disorder severity, comorbidity, treatment history, or eating disorder diagnosis were associated with global QOLI scores. Eating disorder severity was quantified by the EDE-Q global score.
Qualitative analysis. A conventional inductive content analysis was performed on written responses. The purpose of content analysis is to systematically and objectively describe and enhance understanding of the data by analyzing the written responses. The outcome of the analysis is condensed themes or categories derived from the data.24,25 An inductive analytic approach permits themes to emerge from the data, moving from specific to general. In contrast, a deductive approach applies themes previously described in the literature to the data, moving from general to specific.24 Given the dearth of qualitative data describing quality of life of individuals with eating disorders, an inductive approach was chosen.
On the basis of the guidelines of Elo and Kyngäs,25 we completed the following steps for data analysis: first, all written responses were typed and compiled. To develop a coding scheme for participant responses to each domain, 3 trained raters read all written responses and developed a list of prominent themes. The raters discussed these themes, and a final list of themes for each domain was reached by consensus. Coders then reread and coded responses based on the final coding list. The final code(s) for each response was determined by the consensus of the 3 coders, and discrepancies were resolved through discussion and consensus of at least 2 coders. Finally, the data were summarized quantitatively according to the frequency of each theme.
RESULTS
Quantitative Results
The mean (SD) EDE-Q global score was 4.44 (1.30), and the QOLI global score was 0.10 (1.54). There was no statistically significant difference between the anorexia nervosa and bulimia nervosa groups on global QOLI scores. Relatives was the only overall domain for which there was a statistically significant difference between groups (F1,46 = 5.35; P = .025), such that patients with anorexia nervosa reported significantly worse satisfaction (lower scores). For the backward elimination regression analysis, the only statistically significant predictor of quality of life retained in the final model was number of previous treatments (F1,41 = 8.67; P = .005; R2 = 0.175). Specifically, as the number of previous treatments increased, global QOLI scores decreased.
Qualitative Results
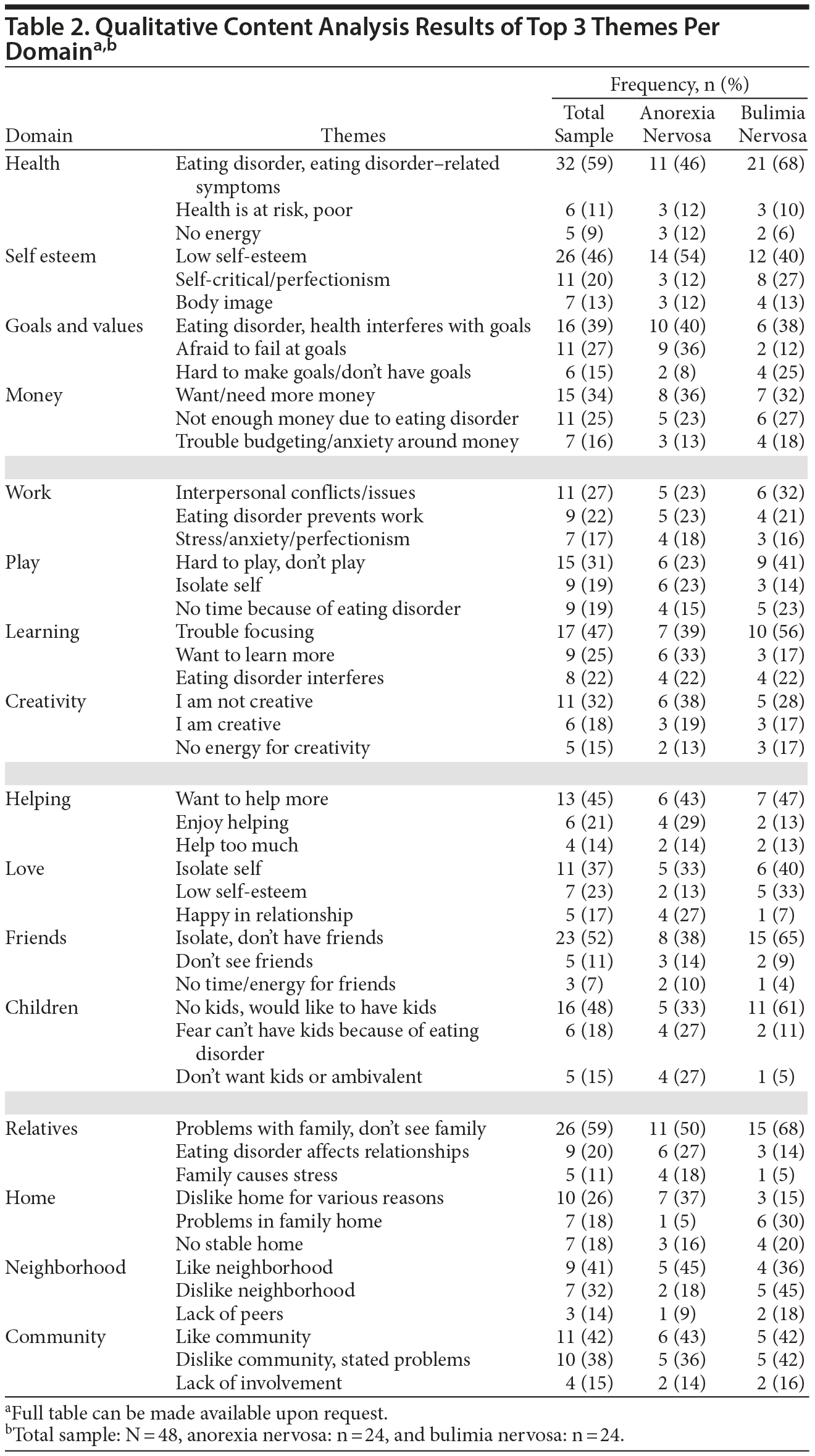
The results of the qualitative content analysis are presented in Table 2. Percent agreement of intercoder reliability was calculated to be 93.75%, therefore acceptable. The top 3 themes for each domain on the QOLI are presented for the entire sample and broken down by eating disorder diagnosis. There was no significant difference in the response rate for each group. Diagnostic group differences for which the most frequently cited theme differed in prevalence by > 10% included health, self-esteem, play, learning, friends, children, relatives, and home. For the health domain, the majority of participants viewed their eating disorder as impairing their quality of life. Consistent with quantitative analysis, this theme was endorsed more frequently by patients diagnosed with bulimia nervosa. For self-esteem, the most prevalent theme was having low self-esteem, and 54% of patients with anorexia nervosa endorsed this theme compared with 40% of patients with bulimia nervosa. For play, the most prevalent theme was having difficulty or not engaging in relaxation, fun, or leisure activities. More patients with bulimia nervosa endorsed this theme (41% for bulimia nervosa versus 23% for anorexia nervosa). For learning, the most common theme was difficulty focusing, endorsed by 56% of patients with bulimia nervosa and 39% of patients with anorexia nervosa. Isolation and lack of friends was the most common theme for the domain of friends, endorsed more frequently by patients with bulimia nervosa. For the children domain, the most prevalent theme written about was not having kids but wanting to have them. This theme was more frequently endorsed by patients with bulimia nervosa (61%) than anorexia nervosa (33%). More patients with anorexia nervosa (37%) than bulimia nervosa (15%) wrote about dissatisfaction with their home environment.
DISCUSSION
The purpose of this study was to evaluate satisfaction of life domains that have not been evaluated previously in this population and to contextualize these quantitative evaluations through an inductive content analysis of complimentary qualitative data. The literature has been mixed in terms of differences in quality of life for individuals with anorexia nervosa versus bulimia nervosa. The current results support previous research, which suggests that patients with anorexia nervosa and bulimia nervosa have similar levels of quality of life4,26; however, a few interesting differences emerged. First, of those who thought their health was important, there was no significant difference of life satisfaction for participants with anorexia nervosa and bulimia nervosa. The qualitative responses, however, suggest that concern about eating disorder symptoms in relation to health is more prevalent among patients with bulimia nervosa (68% endorsed this theme) versus patients with anorexia nervosa (46% endorsed this theme). These findings highlight the importance of considering whether a person views a domain as important and what aspects of it are relevant to his or her quality of life, in addition to assessing satisfaction with it. In fact, a recently published eating disorder–specific quality of life measure, the Eating Disorders Well Being Questionnaire,27 assesses both intensity and subjective relevance of distress, which is an improvement upon previous eating disorder–specific quality of life measures.
When comparing the weighted scores for the 16 QOLI domains, the only statistically significant difference that emerged were for the domain of relatives. This finding supports that of Keilen and colleagues,11 who found that patients with anorexia nervosa reported significantly worse quality of life in social relationships and home life compared to patients with bulimia nervosa. Interestingly, the qualitative responses regarding family relationships only partially supported the quantitative responses. Specifically, 68% of patients with bulimia nervosa wrote about problems with their family compared with 50% of patients with anorexia nervosa. Additionally, 14% of patients with bulimia nervosa wrote about having supportive family/relatives, whereas only 5% of responses from patients with anorexia nervosa described supportive family/relatives. Family support specifically seems to contribute to overall greater satisfaction on the relatives domain, carrying more absolute weight in the positive direction than family problems carry in the negative direction. This finding also speaks to the value of family-based therapy, which is a supported treatment for anorexia nervosa.
Contrary to our hypothesis, the only significant predictor of QOLI global score was the number of previous treatments. Previous research supports associations of BMI, comorbidity, particular eating disorder symptoms, and eating disorder severity with quality of life.6,16,17,28–32 There are several considerations for interpreting these results. First, we wondered whether number of previous treatments might be positively associated with comorbidity or eating disorder severity. However, post hoc correlation analyses among these variables were not significant, suggesting there is a unique association between treatment history and quality of life. Another consideration is that there may truly be no association between quality of life and BMI, comorbid disorders, and eating disorder severity in this sample. More generally, discrepancies between the current findings and existing literature may also be attributed to the use of different types of quality of life measures, ie, generic versus disease specific. Another consideration in failing to replicate past findings is that the current inpatient sample may be more ill than previous study samples. The current sample was hospitalized and presumably experienced loss of autonomy while in that environment and suffered more serious health complications compared to outpatient samples.
To help contextualize the quantitative findings, the qualitative portion of the QOLI provided valuable information. Eating disorder–specific themes emerged for 12 of the 16 domains. The domains of helping, love, friends, and home did not include any eating disorder–specific themes. However, the most common theme for love was isolating oneself, which may be indirectly related to the eating disorder. Isolation was also a prominent theme for the domain of friends, and several participants indicated that they do not see their family for the domain of relatives. Collectively, these responses suggest that the patients do not have a lot of supportive relationships with friends or family, and this may have negative implications for eating disorder treatment. Many wrote about problems with focus or concentration and negative impact on domains of learning, work, and goals and values, which also may have negative treatment implications. Collectively, these results support the recommendation by de la Rie and colleagues14 to assess patient views on quality of life qualitatively in addition to administering standardized quality of life measures.
Although this study yielded important information about quality of life in several life domains, some limitations should be noted. The sample is homogenous in terms of race and gender, so results cannot be generalized to other racial or ethnic groups or males. This sample was severely ill, being hospitalized for their eating disorder, so results cannot be generalized to less ill people. Furthermore, homogeneity in terms of disorder severity may have limited the ability to detect significant differences between groups. In addition, this sample may contain a selection bias, as patients completed questionnaires voluntarily; patients did not receive financial compensation. Further, we do not know why 63% of the patients approached for this study chose not to participate, which limits generalizability to other samples. Finally, all data were collected at 1 time point, so one cannot determine a causal association between eating disorder symptoms and QOLI scores; the results and conclusions presented are only correlational in nature.
Nevertheless, this was the first study to evaluate the QOLI in an eating disorder sample. Because the QOLI assesses 16 different domains, some of which are not included in other quality of life measures, these results revealed new information about how people with an eating disorder perceive and experience these domains. This was also the first study to present both quantitative and qualitative data about quality of life, allowing for more detailed explanation of numeric responses. Results were in line with some previous findings that indicate no significant difference in overall quality of life between inpatients with anorexia nervosa and bulimia nervosa, with the exception of the domain relatives. Results did not support a direct association between BMI, comorbid disorders, or eating disorder severity and global QOLI scores. Finally, the QOLI may be a useful measure to administer to an eating disorder population in the future and particularly informative to eating disorder treatment.
Author affiliations: Department of Psychology, University of Missouri–Kansas City, Kansas City (Mss Pollack and McCune and Dr Lundgren); and Centennial Peaks Hospital, St Louisville, Colorado (Dr Mandal).
Potential conflicts of interest:None reported.
Funding/support:None reported.
Previous presentation: These data were presented as a poster at the International Conference on Eating Disorders; May 2–4, 2013; Montreal, Quebec, Canada.
Acknowledgments: The authors thank Alyssa LaMarr, BA, Amanda Lopez, BA, and Carrie Spresser, PhD (all were affiliated with University of Missouri–Kansas City at the time of the study), for their work on data collection and analysis. Dr Spresser and Mss Lamarr and Lopez report no conflicts of interest related to the subject of this article.
REFERENCES
1. Engel SG, Adair CE, Las Hayas C, et al. Health-related quality of life and eating disorders: a review and update. Int J Eat Disord. 2009;42(2):179–187. doi:10.1002/eat.20602 PubMed
2. Jenkins PE, Hoste RR, Meyer C, et al. Eating disorders and quality of life: a review of the literature. Clin Psychol Rev. 2011;31(1):113–121. doi:10.1016/j.cpr.2010.08.003 PubMed
3. Higginson IJ, Carr AJ. Measuring quality of life: using quality of life measures in the clinical setting. BMJ. 2001;322(7297):1297–1300. doi:10.1136/bmj.322.7297.1297 PubMed
4. Mond JM, Hay PJ, Rodgers B, et al. Assessing quality of life in eating disorder patients. Qual Life Res. 2005;14(1):171–178. doi:10.1007/s11136-004-2657-y PubMed
5. Doll HA, Petersen SE, Stewart-Brown SL. Eating disorders and emotional and physical well-being: associations between student self-reports of eating disorders and quality of life as measured by the SF-36. Qual Life Res. 2005;14(3):705–717. doi:10.1007/s11136-004-0792-0 PubMed
6. Johnson JG, Spitzer RL, Williams JB. Health problems, impairment and illnesses associated with bulimia nervosa and binge eating disorder among primary care and obstetric gynecology patients. Psychol Med. 2001;31(8):1455–1466. doi:10.1017/S0033291701004640 PubMed
7. Mond J, Hay P, Rodgers B, et al. Quality of life impairment in a community sample of women with eating disorders. Aust N Z J Psychiatry. 2012;46(6):561–568. doi:10.1177/0004867411433967 PubMed
8. Sy R, Ponton K, De Marco P, et al. Quality of life in anorexia nervosa: a review of the literature. Eat Disord. 2013;21(3):206–222. doi:10.1080/10640266.2013.779176 PubMed
9. Winkler LA-D, Christiansen E, Lichtenstein MB, et al. Quality of life in eating disorders: a meta-analysis. Psychiatry Res. 2014;219(1):1–9. doi:10.1016/j.psychres.2014.05.002 PubMed
10. Abraham SF, Brown T, Boyd C, et al. Quality of life: eating disorders. Aust N Z J Psychiatry. 2006;40(2):150–155. doi:10.1080/j.1440-1614.2006.01762.x PubMed
11. Keilen M, Treasure T, Schmidt U, et al. Quality of life measurements in eating disorders, angina, and transplant candidates: are they comparable? J R Soc Med. 1994;87(8):441–444. PubMed
12. Muñoz P, Quintana JM, Las Hayas C, et al. Assessment of the impact of eating disorders on quality of life using the disease-specific, Health-Related Quality of Life for Eating Disorders (HeRQoLED) questionnaire. Qual Life Res. 2009;18(9):1137–1146. doi:10.1007/s11136-009-9542-7 PubMed
13. Padierna A, Quintana JM, Arostegui I, et al. The health-related quality of life in eating disorders. Qual Life Res. 2000;9(6):667–674. doi:10.1023/A:1008973106611 PubMed
14. de la Rie S, Noordenbos G, Donker M, et al. The patient’s view on quality of life and eating disorders. Int J Eat Disord. 2007;40(1):13–20. doi:10.1002/eat.20338 PubMed
15. Bamford B, Sly R. Exploring quality of life in the eating disorders. Eur Eat Disord Rev. 2010;18(2):147–153. doi:10.1002/erv.975 PubMed
16. Bamford BH. Assessing quality of life in the eating disorders: the HeRQoLED-S. Expert Rev Pharmacoecon Outcomes Res. 2010;10(5):513–516. doi:10.1586/erp.10.47 PubMed
17. González-Pinto A, Inmaculada F, Cristina R, et al. Purging behaviors and comorbidity as predictive factors of quality of life in anorexia nervosa. Int J Eat Disord. 2004;36(4):445–450. doi:10.1002/eat.20058 PubMed
18. Mitchison D, Hay P, Engel S, et al. Assessment of quality of life in people with severe and enduring anorexia nervosa: a comparison of generic and specific instruments. BMC Psychiatry. 2013;13(1):284. doi:10.1186/1471-244X-13-284 PubMed
19. Frisch MB, Cornell J, Villanueva M, et al. Clinical validation of the Quality of Life Inventory: a measure of life satisfaction for use in treatment planning and outcome assessment. Psychol Assess. 1992;4(1):92–101. doi:10.1037/1040-3590.4.1.92
20. Fairburn CG, Beglin SJ. Assessment of eating disorders: interview or self-report questionnaire? Int J Eat Disord. 1994;16(4):363–370. PubMed
21. Peterson CB, Crosby RD, Wonderlich SA, et al. Psychometric properties of the Eating Disorder Examination Questionnaire: factor structure and internal consistency. Int J Eat Disord. 2007;40(4):386–389. doi:10.1002/eat.20373 PubMed
22. Aardoom JJ, Dingemans AE, Slof Op’t Landt MC, et al. Norms and discriminative validity of the Eating Disorder Examination Questionnaire (EDE-Q). Eat Behav. 2012;13(4):305–309. doi:10.1016/j.eatbeh.2012.09.002 PubMed
23. Frisch MB. Manual and Treatment Guide for the Quality of Life Inventory (QOLI). Minneapolis, MN: National Computer Systems; 1994.
24. Hsieh HF, Shannon SE. Three approaches to qualitative content analysis. Qual Health Res. 2005;15(9):1277–1288. doi:10.1177/1049732305276687 PubMed
25. Elo S, Kyngäs H. The qualitative content analysis process. J Adv Nurs. 2008;62(1):107–115. doi:10.1111/j.1365-2648.2007.04569.x PubMed
26. Sanftner JL. Quality of life in relation to psychosocial risk variables for eating disorders in women and men. Eat Behav. 2011;12(2):136–142. doi:10.1016/j.eatbeh.2011.01.003 PubMed
27. Castellini G, Fioravanti G, Ravaldi C, et al. The Eating Disorders Well Being Questionnaire (EDwell): a new measure of quality of life in eating disorders. Eat Weight Disord. 2013;18(1):11–22. doi:10.1007/s40519-013-0002-6 PubMed
28. Hay P. Quality of life and bulimic eating disorder behaviors: findings from a community-based sample. Int J Eat Disord. 2003;33(4):434–442. doi:10.1002/eat.10162 PubMed
29. Latner JD, Vallance JK, Buckett G. Health-related quality of life in women with eating disorders: association with subjective and objective binge eating. J Clin Psychol Med Settings. 2008;15(2):148–153. doi:10.1007/s10880-008-9111-1 PubMed
30. Vallance JK, Latner JD, Gleaves DH. The relationship between eating disorder psychopathology and health-related quality of life within a community sample. Qual Life Res. 2011;20(5):675–682. doi:10.1007/s11136-010-9799-x PubMed
31. Mond J, Rodgers B, Hay P, et al. Disability associated with community cases of commonly occurring eating disorders. Aust N Z J Public Health. 2004;28(3):246–251. doi:10.1111/j.1467-842X.2004.tb00703.x PubMed
32. Cook BJ, Hausenblas HA. Eating disorder-specific health-related quality of life and exercise in college females. Qual Life Res. 2011;20(9):1385–1390. doi:10.1007/s11136-011-9879-6 PubMed
Enjoy this premium PDF as part of your membership benefits!


