Objective: To investigate the impact of reminder-focused positive psychiatry (RFPP) on attention-deficit/hyperactive disorder (ADHD) and posttraumatic stress disorder (PTSD) symptoms, vascular-function, inflammation and well-being of adolescents with comorbid ADHD and PTSD.
Methods: After obtaining informed-consent, 11 adolescents were randomized to RFPP (n = 5) or trauma-focused cognitive-behavioral therapy (TF-CBT) (n = 6). Eight participants (RFPP: n = 4, TF-CBT: n = 4) completed the twice-weekly intervention for a 6-week trial. The RFPP intervention was inclusive of positive psychiatry interventions on (1) traumatic reminders and (2) avoidance and negative cognition. Vascular function measured as temperature rebound, C-reactive protein, homocysteine, ADHD Swanson, Nolan, and Pelham (SNAP) Questionnaire, Clinician-Administered PTSD Scale for DSM-5-Child/Adolescent Version (CAPS-CA), and neuropsychiatric-measures were measured at baseline and 6 weeks. Subjects were followed for 12 months. The study was conducted from September 2016 to June 2018.
Results: A significant improvement in CAPS-CA, SNAP scores, and vascular function of both RFPP and TF-CBT groups was noted at follow-up, but was more-robust in the RFPP group (P < .05). At the sixth week, a significant increase in PERMA, gratitude, resilience, and Posttraumatic Growth Inventory scores and a significant decrease in homocysteine and C-reactive protein levels in the RFPP group, but not the TF-CBT group, were noted (P < .05). At 12-month follow-up, there was no psychiatry hospitalization or suicide ideation reported in either group. A continuation of significant improvement in CAPS-CA and SNAP scores in both groups was noted but was more robust in the RFPP group (P < .05). Similarly, a continuation of significant increase in PERMA, gratitude, resilience and Posttraumatic Growth Inventory scores was noted in the RFPP group but not in the TF-CBT group (P < .05).
Conclusions: RFPP is associated with improvement in core PTSD and ADHD symptoms, decrease in inflammation, and increase in well-being, vascular function, and posttraumatic growth, as well as a favorable long-term clinical outcome. This finding highlights the importance of the dual role of RFPP in addressing vulnerability symptoms as well as enhancing well-being in youth with comorbid ADHD and PTSD.
Trial Registration: ClinicalTrials.gov identifier: NCT04336072
ABSTRACT
Objective: To investigate the impact of reminder-focused positive psychiatry (RFPP) on attention-deficit/hyperactive disorder (ADHD) and posttraumatic stress disorder (PTSD) symptoms, vascular-function, inflammation and well-being of adolescents with comorbid ADHD and PTSD.
Methods: After obtaining informed-consent, 11 adolescents were randomized to RFPP (n = 5) or trauma-focused cognitive-behavioral therapy (TF-CBT) (n = 6). Eight participants (RFPP: n = 4, TF-CBT: n = 4) completed the twice-weekly intervention for a 6-week trial. The RFPP intervention was inclusive of positive psychiatry interventions on (1) traumatic reminders and (2) avoidance and negative cognition. Vascular function measured as temperature rebound, C-reactive protein, homocysteine, ADHD Swanson, Nolan, and Pelham (SNAP) Questionnaire, Clinician-Administered PTSD Scale for DSM-5–Child/Adolescent Version (CAPS-CA), and neuropsychiatric-measures were measured at baseline and 6 weeks. Subjects were followed for 12 months. The study was conducted from September 2016 to June 2018.
Results: A significant improvement in CAPS-CA, SNAP scores, and vascular function of both RFPP and TF-CBT groups was noted at follow-up, but was more-robust in the RFPP group (P < .05). At the sixth week, a significant increase in PERMA, gratitude, resilience, and Posttraumatic Growth Inventory scores and a significant decrease in homocysteine and C-reactive protein levels in the RFPP group, but not the TF-CBT group, were noted (P < .05). At 12-month follow-up, there was no psychiatry hospitalization or suicide ideation reported in either group. A continuation of significant improvement in CAPS-CA and SNAP scores in both groups was noted but was more robust in the RFPP group (P < .05). Similarly, a continuation of significant increase in PERMA, gratitude, resilience and Posttraumatic Growth Inventory scores was noted in the RFPP group but not in the TF-CBT group (P < .05).
Conclusions: RFPP is associated with improvement in core PTSD and ADHD symptoms, decrease in inflammation, and increase in well-being, vascular function, and posttraumatic growth, as well as a favorable long-term clinical outcome. This finding highlights the importance of the dual role of RFPP in addressing vulnerability symptoms as well as enhancing well-being in youth with comorbid ADHD and PTSD.
Trial Registration: ClinicalTrials.gov identifier: NCT04336072
Prim Care Companion CNS Disord 2020;22(5):19m02579
To cite: Ahmadi N, Chaudhry S, Salam T, et al. A randomized controlled feasibility trial of reminder-focused positive psychiatry in adolescents with comorbid attention-deficit/hyperactivity disorder and posttraumatic stress disorder. Prim Care Companion CNS Disord. 2020;22(5):19m02579.
To share: https://doi.org/10.4088/PCC.19m02579
© Copyright 2020 Physicians Postgraduate Press, Inc.
aDepartment of Psychiatry, David Geffen School of Medicine, University of California Los Angeles, Los Angeles, California
bDepartment of Psychiatry, Kern Medical, Bakersfield, California
*Corresponding author: Naser Ahmadi, MD, PhD, Department of Psychiatry, David Geffen School of Medicine, University of California Los Angeles, Olive View UCLA Medical Ctr, 1445 Olive View Dr, Sylmar, CA 91342 ([email protected]).
Attention-deficit/hyperactivity disorder (ADHD) and posttraumatic stress disorder (PTSD) are prevalent chronic comorbid neuropsychiatric disorders in adolescents. Compared to individuals without PTSD, a significantly higher rate of ADHD in adolescents with PTSD has been observed (16% vs 59%, respectively, P < .05).1 Furthermore, a strong association between the severity of ADHD and PTSD (r = 0.4, P < .05)2 has been reported, which is linked with higher levels of morbidity and dysfunction.3–5 PTSD is associated with increased neurovascular inflammation in adolescents, especially in those with ADHD.2–5
Traumatic reminders are core symptoms of PTSD that play a major role in the development and maintenance of PTSD and are more pronounced in those with comorbid PTSD and ADHD.6 The severity of reactivity to PTSD trauma reminders is associated with impaired cardiovascular function that directly predicts major adverse cardiovascular events.6
Positive psychiatry is the study of well-being, engagement, and optimal functioning and differs from traditional psychiatry in that it conceptualizes mental health as more than just the absence of mental illness. Positive psychiatry promotes well-being through optimal increase in positive psychosocial characteristics such as resilience, optimism, and posttraumatic growth.7 Studies8–10 have revealed the feasibility of positive psychiatry in youth, with positive outcomes, decreased youth depression, and increased long-term life satisfaction.
The main objective of this study is to explore the feasibility and impact of reminder-focused positive psychiatry (RFPP)—a tailored positive psychiatry intervention targeting PTSD’s traumatic reminders and related avoidance and negative affectivity—on core PTSD and ADHD symptoms as well as neuroinflammation, vascular function, well-being, and posttraumatic growth.
METHODS
Study Population
Eleven adolescents with documented PTSD and ADHD based on DSM-5 criteria from the UCLA-Kern Child and Adolescent Psychiatry Clinic, Bakersfield, California, were enrolled in the study. The participants were a mean ± SD age of 11 ± 3 years (range, 10–15 y), and 55% were female. They had no known medical disease, other psychiatric disorder, or substance use disorder. After obtaining informed consent from parents and informed assent from the adolescents, the participants were randomized to group therapy with RFPP (n = 5) or trauma-focused cognitive-behavioral therapy (TF-CBT) (n = 6) in a double-blind manner using numbered containers assigned to a computer-generated randomization chart by the nurse coordinator. All participants, personnel administering interventions, clinicians, and psychiatrists involved in the study were blinded to group assignment. All subjects were on the optimal dose of stimulant psychotropic medication, and none were on any other psychotropic medications. The study was conducted from September 2016 to June 2018.
Eight participants (RFPP: n = 4, TF-CBT: n = 4) completed the 6-week trial, which was inclusive of twice-weekly intervention sessions with adolescents with comorbid PTSD and ADHD and 4 intervention sessions with their parents. Vascular function, measured as temperature rebound by reactive hyperemia procedure using digital thermal monitoring, C-reactive protein (CRP), homocysteine, and neuropsychiatric questionnaires (ADHD Swanson, Nolan, and Pelham [SNAP] Questionnaire11; PERMA [positive emotion, engagement, relationships, meaning, and accomplishment]12; Gratitude Resentment and Appreciation Test13; Posttraumatic Growth Inventory14; Connor-Davidson Resilience Scale15; UCLA Trauma Reminder Inventory16; and Clinician-Administered PTSD Scale for DSM-5–Child/Adolescent Version [CAPS-CA]17) were measured at baseline and 6 weeks and at 12-month follow-up. The Cronbach α for the SNAP and CAPS-CA was 0.90 at baseline and 0.90 at postintervention.
Digital Thermal Monitoring of Vascular Function
Digital thermal monitoring of vascular function was measured in the morning in a quiet, dimmed room at a controlled ambient temperature of 23.5° to 25.0°C. Digital thermal monitoring was measured using thermal changes (temperature rebound) during the 5-minute arm cuff–induced reactive hyperemia procedure at the fingertip using an automated, operator-independent protocol (VENDYS, Endothelix, Houston, Texas).18 CRP and homocysteine levels were measured using the standard techniques.19
Acceptability
After the 6-week intervention, adolescents and parents were asked about overall satisfaction with treatment using the validated and reliable Client Satisfaction Questionnaire (CSQ-8).20 Our aim was a mean score above 20.00 (good–excellent) on the CSQ-8 (total scores can range from 8 to 32) and a mean of 4.00 (very valuable session) on the Session Feedback Questionnaire (SFQ) (total scores can range from 0 to 5).21
Feasibility
The feasibility goal was a ≥ 50% referred-to-enrolled rate, ≥ 70% intervention completion rate, and 70% 12-month follow-up rate.
Efficacy
Reactivity to trauma reminder was assessed with the UCLA Trauma Reminder Inventory and CAPS-CA. All measures demonstrated acceptable internal consistency.
Fidelity
The adherence and competence of therapists to the model was assessed by live observation, role play, and provider self-report and checklist. Sessions were observed or listened to as they were happening. Therapists demonstrated specific skills that might be used with a client generically and as applied to specific clinical cases required by the model. Therapists described in detail exactly what they did in the session and how the client responded and also completed checklists following the sessions.
Reminder-Focused Positive Psychiatry
RFPP group therapy was conducted by 2 therapists trained in positive psychiatry twice a week for 6 weeks. The focus of RFPP is on enhancing contextual discrimination and emotional regulation and promoting the use of adaptive coping strategies in response to trauma reminders, including recognizing reminders and shifting attention from intrusive memories during exposure to reminders to a focus on positive feelings, thoughts, goals, and choices. RFPP also includes exercises to deal with avoidance and psychological and physiologic reactivity associated with trauma reminders. RFPP is a trauma reminder–focused group treatment for both children with PTSD and their families. RFPP includes child/adolescent and parent components.
Child/adolescent component. Trauma reminders. This component focuses on exercises to enhance recognition of emotional constriction, associated adverse aggressive behavior, and social withdrawal and reduction of the reactivity to trauma reminders by promoting enhanced adaptive coping strategies through shifting attention. Participants receive instruction on how to shift their suffering during a trauma reminder to feelings of caring and kindness toward self, as well as behavioral interventions on how to bounce back from distress by enhancing emotion regulation and abilities to open new doors to the self, developing positive emotion by expressing gratitude to self and others, and encouraging social connectedness.
Avoidance and negative cognitions. This component consists of exercises to promote flexible thinking less influenced by traumatic expectations. The component includes antecedent behavior consequence skill-building exercises to promote increased self-understanding and enhanced coping strategies, exercises to enhance verbal emotional labeling and expression of physical reactions, and strategies to deal with setbacks and risky behavior and to promote posttraumatic constructive action and developmental progression. This component aims (1) to increase cognitive coping skills and impulse control by understanding the relation of activating events, beliefs, and consequences through compassionate thinking and by disputing distorted thoughts; (2) to increase flexible thinking by promoting personal growth through self-reflection and developmental progress using strength; (3) to increase passionate and purposeful interactions with others by improving positive attention toward self and increase positive feelings and interpersonal relationships; (4) to develop a habit of savoring in the present moment each day with touch to sensory input of happiness; and (5) to express emotional and physical reaction labeling and strategies to promote posttraumatic constructive progression by addressing common pitfalls and possible solutions.
Each child/adolescent component session lasted 75 minutes and consisted of 10 minutes of group skills education, 10 minutes of individual therapy with each participant, and group positive psychiatry combining the 2 main modules of traumatic reminders and avoidance and negative affectivity, followed by 5 minutes of wrap up. Using the UCLA Trauma Reminder Inventory, the 5 most prevalent traumatic reminders were identified in advance, and participants practiced RFPP interventions during the traumatic reminders and maintenance phase.
Parent component. This component includes psychological education using RFPP modules.
TF-CBT
Group therapy was conducted by 2 therapists trained in TF-CBT and was adapted to be delivered twice weekly for 6 weeks. The trauma narrative and processing components enabled the child to talk about memories individually and in groups. The final sessions focused on grief-specific elements. The structure of all sessions were as follows: (1) refreshments, (2) review the previous group activities, (3) teach new components, (4) assign homework, and (5) preview the next group.22
Statistical Analysis
All data were collected with no missing values. All continuous data are presented as mean ± SD, all categorical data are reported as a percentage or absolute number, and χ2 and t tests were used to assess differences between groups. Interrater reliability was assessed using the chance-corrected weighted κ statistic. A κ value of 0.81–1.00 was considered to indicate almost perfect agreement, 0.61–0.80 substantial agreement, 0.41–0.60 moderate agreement, 0.21–0.40 fair agreement, and 0.00–0.20 slight agreement. Mixed regression was employed to assess the change in ADHD and PTSD symptoms as well as inflammation, vascular function, and positive biopsychosocial trait in the RFPP and TF-CBT groups. Using multivariate mixed regression analyses, risk factor–adjusted improved vascular function, increased positive biopsychosocial trait, and inflammation in RFPP compared to TF-CBT were assessed. All statistical analyses were performed using SAS version 9.2 (SAS Institute Inc, Cary, North Carolina) and SPSS version 24 (SPSS Inc, Chicago, Illinois). This study was approved and overseen by the Institutional Review Board Committee of Kern Medical, Bakersfield, California, and the study was registered at ClinicalTrials.gov (identifier: NCT04336072).
RESULTS
Baseline Characteristics
The mean ± SD acceptability measured by the SFQ in the RFPP and TF-CBT groups was 4.5 ± 0.2 and 4.3 ± 0.3, respectively (P = .3). The mean CSQ-8 score in the RFPP and TF-CBT groups was 27.4 ± 2.6 and 23.3 ± 2.9, respectively (P = .02). From the 11 participants who completed the baseline visit and were randomized to conditions, 8 completed the postintervention assessment at 6 weeks (80% in the RFPP group and 67% in the TF-CBT group since the baseline visit), and 8 completed the 12-month follow-up assessment (100% in both groups since the postintervention visit). The mean attendance rate was 95.8% (range, 83%–100%) for the sessions. The interrater reliability between observer and therapists was 97% with κ of 0.92 (95% CI, 0.84–0.96) where the 2 raters made the exact same judgement with regard to the extent to which the item was delivered.
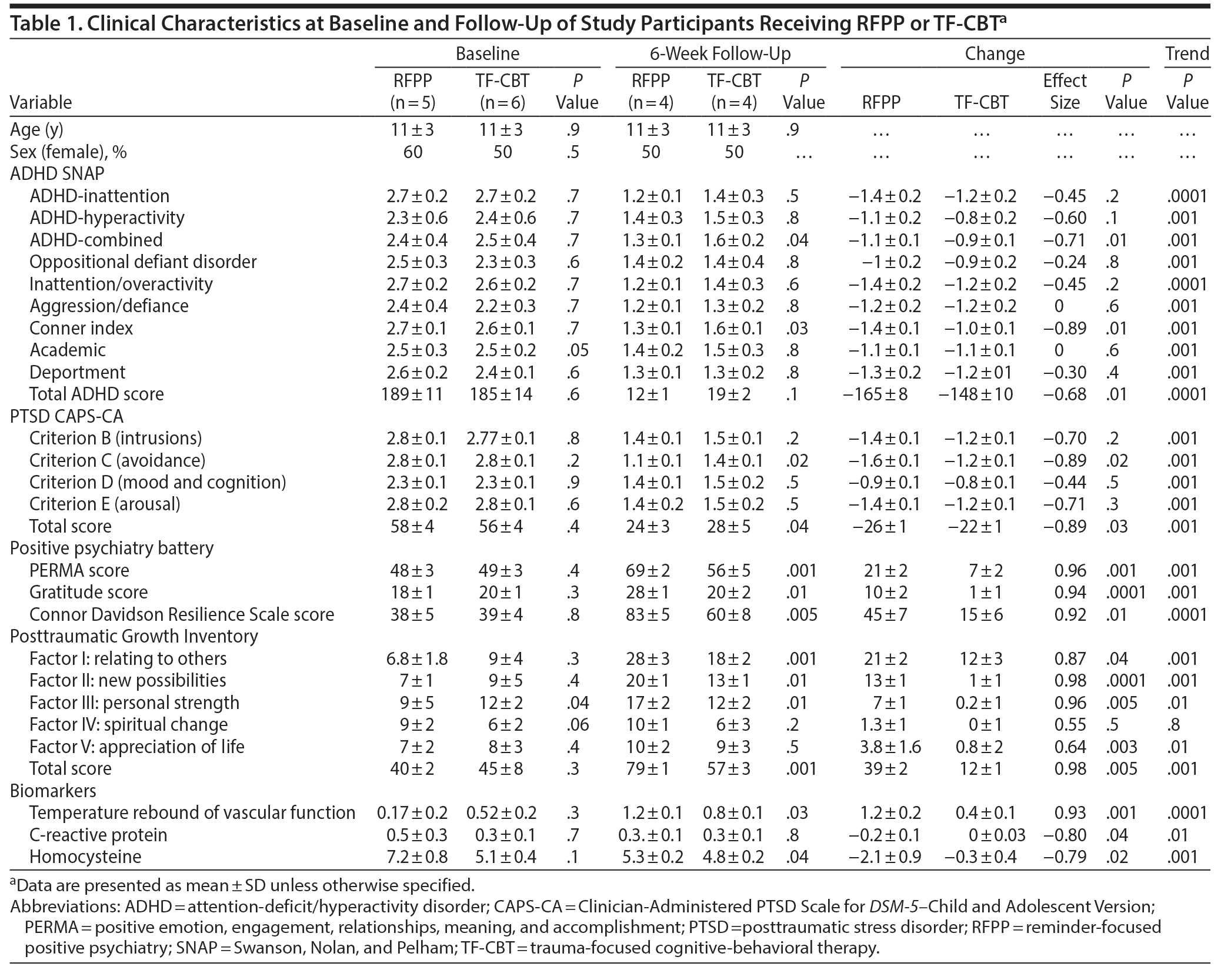
Demographics and conventional risk factors are presented in Table 1. There were no significant differences between groups in terms of age, sex, and baseline ADHD and PTSD symptoms. There was a significant inverse correlation between the severity of ADHD and PTSD symptoms at baseline with reduced PERMA score (r2 = 0.53, P = .001) and impaired vascular function (r2 = 0.67, P = .001). In addition, preserved vascular function at baseline directly correlated with higher levels of resilience, gratitude, and PERMA scores (P < .05). Furthermore, vascular function and PERMA scores were significantly lower in adolescents with a SNAP score > 40 and CAP score > 30 compared to those with SNAP scores of 28–40 and CAP scores of 16–30 (P < .05). Similarly, CRP and homocysteine levels were significantly higher in adolescents with a SNAP score > 40 and CAP score > 30 compared to those with SNAP scores of 28–40 and CAP scores of 16–30 (P < .05). In addition, severity of reactivity to PTSD trauma reminders was directly associated with impaired vascular function (r2 = 0.71, P = .001), higher levels of CRP (r2 = 0.32, P = .01), and lower resilience (r2 = 0.60, P = .001), gratitude (r2 = 0.63, P = .001), and PERMA (r2 = 0.58, P = .001) scores.
6-Week Outcomes
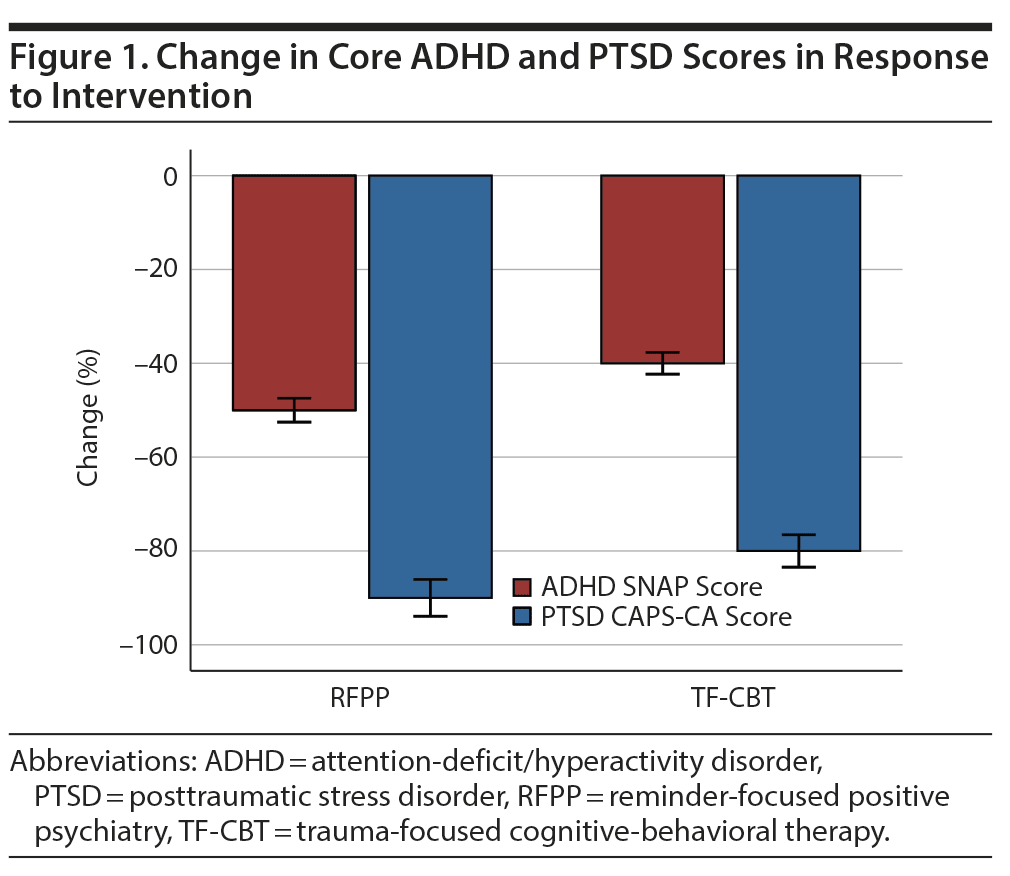
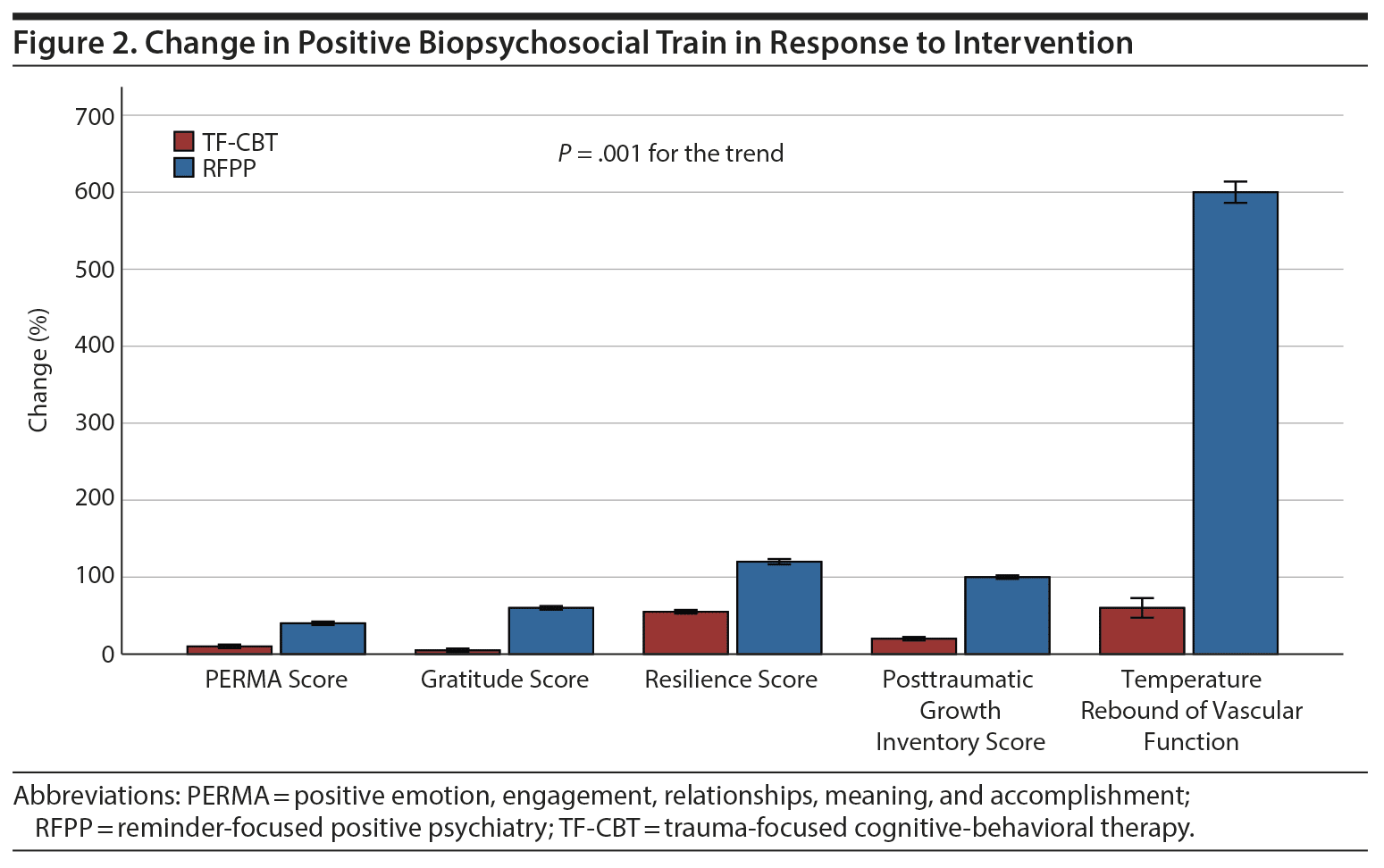
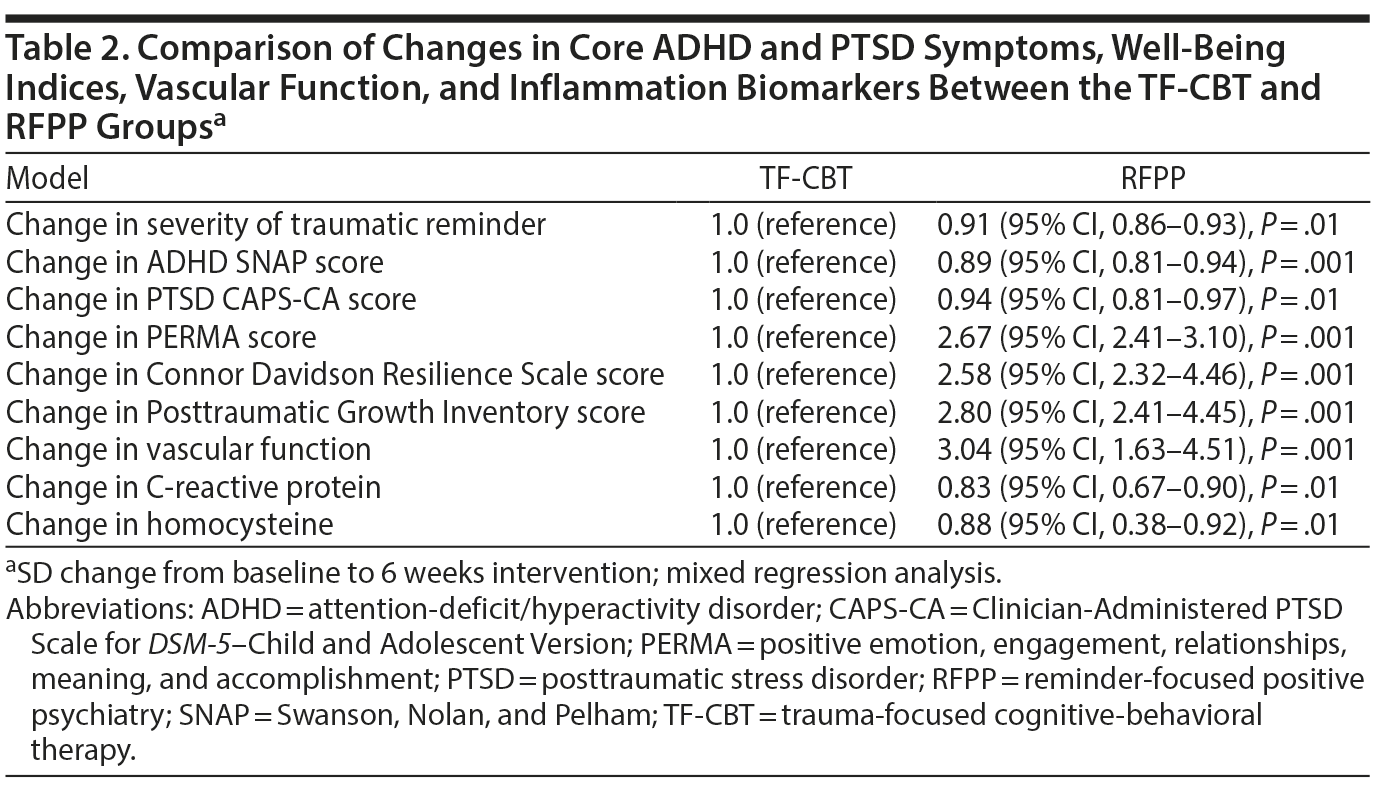
At 6-week follow-up, a significant improvement in CAPS-CA, SNAP (Figure 1), and vascular function in both the RFPP and TF-CBT groups was noted but was more robust in the RFPP group (Figure 2) (P < .05). At the sixth week, a significant decrease in homocysteine and CRP, as well as an increase in PERMA, gratitude, resilience, and posttraumatic growth scores in the RFPP group, but not in the TF-CBT group, was noted. Similarly, a significant relation was noted between decrease in CAPS and SNAP scores and increase in vascular function as well as decrease in homocysteine levels (Table 2).
At 6-week follow-up, a significant decrease in CAPS and SNAPS scores and severity of reactivity to PTSD trauma reminders in both groups was noted, which was significantly more robust in RFPP compared to TF-CBT (P < .05). In addition, a significant increase in vascular function and PERMA, gratitude, resilience, and posttraumatic growth scores and a decrease in CRP and homocysteine levels were observed in RFPP but not in TF-CBT (P < .01). The most prominent improvement of the positive biopsychosocial trait in response to RFPP was in resilience, gratitude, and posttraumatic growth with focus on positive connectedness, new possibilities, appreciation of life, personal strength, and relating to others (P < .05).
12-Month Outcomes
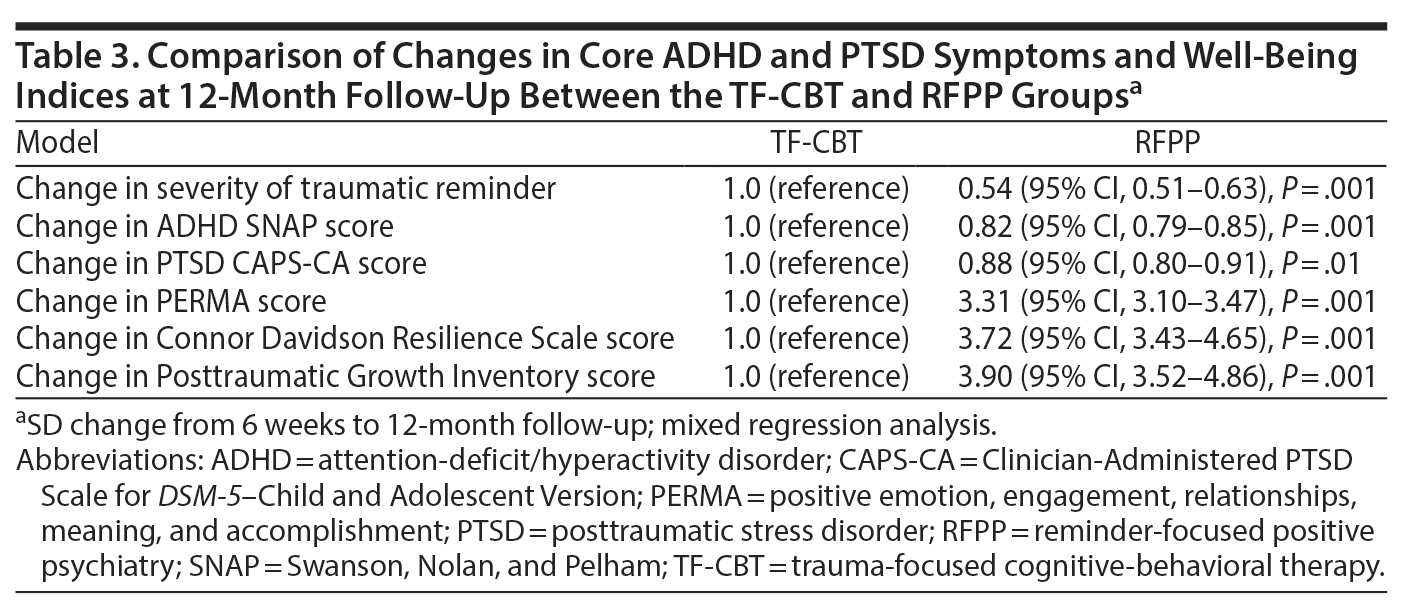
During the 12-month follow-up, no psychiatry hospitalization, suicide ideation, or recurrence of mental disorder in either group was observed. Furthermore, a continuation of decrease in CAPS-CA and SNAP scores in both groups was noted but was more prominent in RFPP (P < .05). Table 3 shows that RFPP, but not TF-CBT, was associated with sustained reduction of severity of reactivity to PTSD trauma reminders and improvement in PERMA, gratitude, resilience, and posttraumatic growth scores in RFPP (P < .05). Finally, at 1-year follow-up, the severity of reactivity to PTSD trauma reminders remained reduced in the RFPP group but not in the TF-CBT group (P < .05).
DISCUSSION
The present study supports several novel findings. (1) The severity of reactivity to PTSD trauma reminders and PTSD and ADHD symptoms is linked with impaired vascular function, increased inflammation, and lower levels of well-being, gratitude, and resilience. (2) RFPP was found to be highly feasible and acceptable for adolescents with PTSD and ADHD. (3) RFPP was associated with improvement in core PTSD and ADHD symptoms; decreased severity of reactivity to PTSD trauma reminders and inflammation; increased vascular function, well-being, and posttraumatic growth; and a favorable long-term clinical outcome. (4) There is a direct link between increased well-being, resilience, and posttraumatic growth and improvement in vascular function and inflammation in response to RFPP.
Prior studies1–5,23 revealed the severity of ADHD symptoms (ie, inattention, impulsivity, and emotional dysregulation) as a significant predictor of severity of PTSD symptoms, suggesting a heightened disruption to frontal-amygdala neurocircuitry as a common underlying mechanism of both disorders. In addition, PTSD and ADHD are associated with multiple medical and mental health disorders through alterations in inflammatory state and dysregulation of the hypothalamic-pituitary-adrenal (HPA) axis and impaired autonomic and vascular function.1–5,23–26
Many individuals with comorbid ADHD and PTSD continue to suffer despite US Food and Drug Administration–approved psychotropic medications—including antidepressants (sertraline and paroxetine), prazosin, and stimulants—and the Institute of Medicine–approved psychotherapy.27 Long-term outcomes with even the most intensive treatments, although significant, were modest and revealed persistent morbidities and disabilities for many individuals with PTSD with comorbid ADHD.27,28
Traditional psychotherapies for PTSD and ADHD are based on a deficit model, focusing on ameliorating their core symptoms.29,30 Furthermore, there is a significant dropout rate of 20%–75% in such interventions (ie, exposure or narrative therapy) due to re-experiencing the traumatic memories, negative affectivity, and deterioration of well-being.29,31
Recent studies32,33 of positive psychiatry revealed that higher levels of resilience, satisfaction with life, and gratitude were associated with lower PTSD symptoms. Vernon et al34 reported that gratitude, positive emotion, and proactive coping style were reversely associated with the severity of PTSD symptoms. Prior studies35,36 showed that self-compassion interventions (ie, self-kindness, common humanity, mindfulness) are associated with improvement of PTSD symptoms facilitated through decrease in self-judgement, isolation, and over identification as well as increase in self-kindness. Furthermore, studies29,31–33 demonstrate that posttraumatic growth is associated with a greater protection against the exacerbation of PTSD symptoms and development of PTSD. Similarly, mindfulness interventions show a superior efficacy in improving ADHD symptoms and executive control compared to treatment as usual inclusive of pharmacotherapy plus psychotherapy.34 The findings of the current study confirmed that of prior studies and is the first to provide evidence that RFPP intervention tailored to core clinical features of PTSD is highly acceptable and feasible and is associated with more robust reduction of core PTSD and ADHD symptoms compared to TF-CBT. RFPP was also associated with more prominent improvement of vascular function and inflammation as well as an increase in well-being and positive biopsychosocial traits.
RFPP focuses on enhancing contextual differentiation, emotion regulation, and adaptive coping strategies by shifting individuals’ attention from intrusive memories during traumatic reminders to meaningful reactions, feelings, thoughts, goals, and choices through self-compassion, gratitude, and resilience exercises. RFPP also promotes flexible thinking when confronted with avoidance and negative symptoms associated with traumatic reminders through positive perceptual-sensory input, pathfinding mindset with connectedness and empathy, self through savoring, compassionate antecedent behavior consequence skill building, engagement, and vitality exercises. These salutary effects have been associated with evidence of concomitant increase in vascular function, decrease of inflammation that correlates strongly with HPA axis normalization, significant reduction of PTSD and its related reminders, and reduced major adverse cardiovascular events.
Finally, while both interventions were associated with ADHD and PTSD sustained remission, RFPP, but not TF-CBT, is associated with sustained reduction of traumatic reminder severity and preserved well-being, connectedness, gratitude, resilience, and posttraumatic growth.
Clinical Application
The appreciation for a role of severity of reactivity to PTSD trauma reminders in worsening neurovascular inflammation and poor clinical outcome, especially in those with ADHD, has increased considering previous studies.37–43 The current study is the first to (1) make a direct association between RFPP and improvement of ADHD and PTSD symptoms; (2) provide evidence of improvement in well-being, positive coping skills, and resiliency in response to RFPP; and (3) note a sustained lower level of traumatic reminder severity and favorable clinical outcome in response to RFPP.
Study Limitations
Major limitations of this study include the small sample size and lack of double blinding. The raters of psychiatric measures and analysis were blinded to the study. Post hoc power analysis shows a power size of 0.90 to distinguish significant improvement in PTSD symptoms, vascular function, and well-being in response to RFPP, with bias of 1.3%. Although there were immense changes in PTSD and ADHD symptoms as well as physiologic measures in response to RFPP in this small sample-size study, bootstrapping analyses revealed less than 3.1% bias in estimating the change in core PTSD and ADHD symptoms and physiologic measures in response to RFPP after increasing the sample size to 10,000. Further prospective studies are needed to replicate the findings of this study and to evaluate the long-term effect of RFPP on ADHD and PTSD core symptoms and well-being.
CONCLUSIONS
The severity of PTSD and ADHD is associated with impaired vascular function, increased inflammation, and lower levels of well-being, gratitude, and resilience. RFPP is an acceptable and feasible trauma-informed reminder-focused intervention and is associated with improvement in PTSD and ADHD symptoms, an increase in well-being and vascular function, a reduction in inflammation, and favorable long-term clinical outcome. These findings highlight the importance of the dual role of RFPP in addressing vulnerable symptoms as well as enhancing well-being in youth with ADHD and PTSD.
Clinical Points
- Reminder-focused positive psychiatry (RFPP) is an acceptable and feasible intervention.
- Current evidence supports the improvement of attention-deficit/hyperactivity disorder (ADHD) and posttraumatic stress disorder (PTSD) symptoms and physiologic measures in response to RFPP.
- Using RFPP, clinicians can address symptoms of ADHD and PTSD, thereby enhancing the well-being of youth with such disorders.
Submitted: December 9, 2019; accepted April 20, 2020.
Published online: September 3, 2020.
Potential conflicts of interest: None.
Funding/support: This study was funded by the American Academy of Child and Adolescent Psychiatry Pilot Research Award.
Role of the sponsor: The American Academy of Child and Adolescent Psychiatry funded this pilot study and provided continuous mentorship throughout the award period.
Acknowledgments: We are grateful to the American Academy of Child and Adolescent Psychiatry for funding this study and providing a thorough mentorship for this pilot research award. Special thanks to Samantha Madziarski, MD; Chandan Samra, MD; and Farial Kosten, LCSW, as well as medical students Alex Dragic, MD, and Michelle Zamorano, MD, for their help during implementation of this pilot study. The acknowledged individuals report no conflicts of interest related to the subject of this article.
REFERENCES
1. Adams Z, Adams T, Stauffacher K, et al. The effects of inattentiveness and hyperactivity on posttraumatic stress symptoms: does a diagnosis of posttraumatic stress disorder matter ?[published online ahead of print April 16, 2015] J Atten Disord. 2015;1087054715580846. PubMed CrossRef
2. Biederman J, Petty CR, Spencer TJ, et al. Examining the nature of the comorbidity between pediatric attention deficit/hyperactivity disorder and post-traumatic stress disorder. Acta Psychiatr Scand. 2013;128(1):78–87. PubMed CrossRef
3. Mitchell RH, Goldstein BI. Inflammation in children and adolescents with neuropsychiatric disorders: a systematic review. J Am Acad Child Adolesc Psychiatry. 2014;53(3):274–296. PubMed CrossRef
4. Carpenter LL, Gawuga CE, Tyrka AR, et al. Association between plasma IL-6 response to acute stress and early-life adversity in healthy adults. Neuropsychopharmacology. 2010;35(13):2617–2623. PubMed CrossRef
5. Bücker J, Fries GR, Kapczinski F, et al. Brain-derived neurotrophic factor and inflammatory markers in school-aged children with early trauma. Acta Psychiatr Scand. 2015;131(5):360–368. PubMed CrossRef
6. Ahmadi N, Molla M, Kase M, et al. 2.41 Efficacy and long-term clinical outcome of comorbid PTSD and ADHD after reminder focused positive psychiatry intervention. J Am Acad Child Adolesc Psychiatry suppl. 2018;57(10):S172. CrossRef
7. Tsai J, El-Gabalawy R, Sledge WH, et al. Post-traumatic growth among veterans in the USA: results from the National Health and Resilience in Veterans Study. Psychol Med. 2015;45(1):165–179. PubMed CrossRef
8. Manicavasagar V, Horswood D, Burckhardt R, et al. Feasibility and effectiveness of a web-based positive psychology program for youth mental health: randomized controlled trial. J Med Internet Res. 2014;16(6):e140. PubMed CrossRef
9. Valdez CE, Lim BH, Parker CP. Positive change following adversity and psychological adjustment over time in abused foster youth. Child Abuse Negl. 2015;48:80–91. PubMed CrossRef
10. Ahmadi N, Chaudhry, Salam S, et al. 2.2 Trial of positive psychiatry in comorbid attention-deficit hyperactive/disorder (ADHD) with posttraumatic stress disorder (PTSD). J Am Acad Child & Adolescent Psychiatry suppl. 2017;56(10):S176–S177. CrossRef
11. Steiner H, Remsing L; Work Group on Quality Issues. Practice parameter for the assessment and treatment of children and adolescents with oppositional defiant disorder. J Am Acad Child Adolesc Psychiatry. 2007;46(1):126–141. PubMed CrossRef
12. Butler J, Kern M. The PERMA-Profiler: a brief multidimensional measure of flourishing. Int J Wellbeing. 2016;6(3):1–48. CrossRef
13. Watkins PC, Woodward K, Stone T, et al. Gratitude and happiness: development of a measure of gratitude, and relationship with subjective well-being. Soc Behav Personal. 2003;31(5):431–452. CrossRef
14. Cann A, Calhoun LG, Tedeschi RG, et al. A short form of the Posttraumatic Growth Inventory. Anxiety Stress Coping. 2010;23(2):127–137. PubMed CrossRef
15. Baek HS, Lee KU, Joo EJ, et al. Reliability and validity of the Korean version of the Connor-Davidson Resilience Scale. Psychiatry Investig. 2010;7(2):109–115. PubMed CrossRef
16. Steinberg A, Brymer M, Decker K, et al. The University of California at Los Angeles Post-Traumatic Stress Disorder Reaction Index. Current Psychiatry Reports. 2004;6:96–100.
17. Pynoos RS, Weathers FW, Steinberg AM, et al. 2015. Clinician-Administered PTSD Scale for DSM-5– Child/Adolescent Version. Scale. National Center for PTSD. www.ptsd.va.gov. Accessed August 12, 2020.
18. Ahmadi N, McQuilkin GL, Akhtar MW, et al. Reproducibility and variability of digital thermal monitoring of vascular reactivity. Clin Physiol Funct Imaging. 2011;31(6):422–428. PubMed CrossRef
19. Hashmi S, Zeng QT. Role of interleukin-17 and interleukin-17-induced cytokines interleukin-6 and interleukin-8 in unstable coronary artery disease. Coron Artery Dis. 2006;17(8):699–706. PubMed CrossRef
20. Matsubara C, Green J, Astorga LT, et al. Reliability tests and validation tests of the Client Satisfaction Questionnaire (CSQ-8) as an index of satisfaction with childbirth-related care among Filipino women. BMC Pregnancy Childbirth. 2013;13(1):235. PubMed CrossRef
21. Stiles WB, Gordon LE, Lani JA. Session evaluation and the Session Evaluation Questionnaire. In: Tryon GS, ed. Counseling Based on Process Research: Applying What We Know. Boston, MA: Allyn & Bacon; 2002:325–343.
22. Deblinger E, Stauffer LB, Steer RA. Comparative efficacies of supportive and cognitive behavioral group therapies for young children who have been sexually abused and their nonoffending mothers. Child Maltreat. 2001;6(4):332–343. PubMed CrossRef
23. Biederman J, Petty C, Spencer TJ, et al. Is ADHD a risk for posttraumatic stress disorder (PTSD)? results from a large longitudinal study of referred children with and without ADHD. World J Biol Psychiatry. 2014;15(1):49–55. PubMed CrossRef
24. Dedert EA, Calhoun PS, Watkins LL, et al. Posttraumatic stress disorder, cardiovascular, and metabolic disease: a review of the evidence. Ann Behav Med. 2010;39(1):61–78. PubMed CrossRef
25. von Känel R, Hepp U, Traber R, et al. Measures of endothelial dysfunction in plasma of patients with posttraumatic stress disorder. Psychiatry Res. 2008;158(3):363–373. PubMed CrossRef
26. Angeli E, Korpa T, Johnson EO, et al. Salivary cortisol and alpha-amylase diurnal profiles and stress reactivity in children with attention deficit hyperactivity disorder. Psychoneuroendocrinology. 2018;90:174–181. PubMed CrossRef
27. Tsai J, Mota NP, Southwick SM, et al. What doesn’t kill you makes you stronger: a national study of US military veterans. J Affect Disord. 2016;189:269–271. PubMed CrossRef
28. Wall-Wieler E, Roos LL, Chateau DG, et al. What predictors matter: risk factors for late adolescent outcomes. Can J Public Health. 2016;107(1):e16–e22. PubMed CrossRef
29. Najavits LM. The problem of dropout from “gold standard” PTSD therapies. F1000Prime Rep. 2015;7:43. PubMed CrossRef
30. Lyon AR, Budd KS. A community mental health implementation of Parent-Child Interaction Therapy (PCIT). J Child Fam Stud. 2010;19(5):654–668. PubMed CrossRef
31. Foa EB, Gillihan SJ, Bryant RA. Challenges and successes in dissemination of evidence-based treatments for posttraumatic stress: lessons learned from prolonged exposure therapy for PTSD. Psychol Sci Public Interest. 2013;14(2):65–111. PubMed CrossRef
32. McCanlies EC, Mnatsakanova A, Andrew ME, et al. Positive psychological factors are associated with lower PTSD symptoms among police officers: post Hurricane Katrina. Stress Health. 2014;30(5):405–415. PubMed CrossRef
33. Janssen L, Kan CC, Carpentier PJ, et al. Mindfulness-based cognitive therapy v. treatment as usual in adults with ADHD: a multicenter, single-blind, randomized controlled trial. Psychol Med. 2019;49(1):55–65. PubMed CrossRef
34. Vernon LL, Dillon JM, Steiner AR. Proactive coping, gratitude, and posttraumatic stress disorder in college women. Anxiety Stress Coping. 2009;22(1):117–127. PubMed CrossRef
35. Hoffart A, Øktedalen T, Langkaas TF. Self-compassion influences PTSD symptoms in the process of change in trauma-focused cognitive-behavioral therapies: a study of within-person processes. Front Psychol. 2015;6:1273. PubMed CrossRef
36. Dahm KA, Meyer EC, Neff KD, et al. Mindfulness, self-compassion, posttraumatic stress disorder symptoms, and functional disability in US Iraq and Afghanistan War Veterans. J Trauma Stress. 2015;28(5):460–464. PubMed CrossRef
37. Grenon SM, Owens CD, Alley H, et al. Posttraumatic stress disorder is associated with worse endothelial function among veterans. J Am Heart Assoc. 2016;5(3):e003010. PubMed CrossRef
38. Serrani Azcurra D. Early markers of endothelial dysfunction posttraumatic stress disorder. Role in atherogenesis [article in Spanish]. Rev Psiquiatr Salud Ment. 2010;3(4):128–136. PubMed CrossRef
39. Violanti JM, Burchfiel CM, Miller DB, et al. The Buffalo Cardio-Metabolic Occupational Police Stress (BCOPS) pilot study: methods and participant characteristics. Ann Epidemiol. 2006;16(2):148–156. PubMed CrossRef
40. Ritov G, Ardi Z, Richter-Levin G. Differential activation of amygdala, dorsal and ventral hippocampus following an exposure to a reminder of underwater trauma. Front Behav Neurosci. 2014;8:18. PubMed CrossRef
41. Yoon SA, Weierich MR. Salivary biomarkers of neural hypervigilance in trauma-exposed women. Psychoneuroendocrinology. 2016;63:17–25. PubMed CrossRef
42. Heath NM, Chesney SA, Gerhart JI, et al. Interpersonal violence, PTSD, and inflammation: potential psychogenic pathways to higher C-reactive protein levels. Cytokine. 2013;63(2):172–178. PubMed CrossRef
43. Anand D, Colpo GD, Zeni G, et al. Attention-deficit/hyperactivity disorder and inflammation: what does current knowledge tell us? a systematic review. Front Psychiatry. 2017;8:228. PubMed CrossRef
Enjoy this premium PDF as part of your membership benefits!