Objective: Body dysmorphic disorder (BDD) is a relatively common psychiatric disorder characterized by preoccupations with perceived defects in physical appearance. This review aimed to explore epidemiology, clinical features, comorbidities, and treatment options for BDD in different clinical settings.
Data Source and Study Selection: A search of the literature from 1970 to 2011 was performed using the MEDLINE search engine. English-language articles, with no restriction regarding the type of articles, were identified using the search terms body dysmorphic disorder, body dysmorphic disorder clinical settings, body dysmorphic disorder treatment, and body dysmorphic disorder & psychodermatology.
Results: BDD occurs in 0.7% to 2.4% of community samples and 13% of psychiatric inpatients. Etiology is multifactorial, with recent findings indicating deficits in visual information processing. There is considerable overlap between BDD and obsessive-compulsive disorder (OCD) in symptom etiology and response to treatment, which has led to suggestions that BDD can be classified with anxiety disorders and OCD. A recent finding indicated genetic overlap between BDD and OCD. Over 60% of patients with BDD had a lifetime anxiety disorder, and 38% had social phobia, which tends to predate the onset of BDD. Studies reported a high level of comorbidity with depression and social phobia occurring in > 70% of patients with BDD. Individuals with BDD present frequently to dermatologists (about 9%-14% of dermatologic patients have BDD). BDD co-occurs with pathological skin picking in 26%-45% of cases. BDD currently has 2 variants: delusional and nondelusional, and both variants respond similarly to serotonin reuptake inhibitors (SRIs), which may have effect on obsessive thoughts and rituals. Cognitive-behavioral therapy has the best established treatment results.
Conclusions: A considerable overlap exists between BDD and other psychiatric disorders such as OCD, anxiety, and delusional disorder, and this comorbidity should be considered in evaluation, management, and long-term follow-up of the disorder. Individuals with BDD usually consult dermatologists and cosmetic surgeons rather than psychiatrists. Collaboration between different specialties (such as primary care, dermatology, cosmetic surgery, and psychiatry) is required for better treatment outcome.
Prim Care Companion CNS Disord 2013;15(4): doi:10.4088/PCC.12r01464
© Copyright 2013 Physicians Postgraduate Press, Inc.
Submitted: September 10, 2012; accepted February 22, 2013.
Published online: July 18, 2013.
Corresponding author: Mohammad Jafferany, MD, Department of Psychiatry and Behavioral Sciences, Central Michigan University, College of Medicine, East Campus, 1000 Houghton Ave, Saginaw, MI 48602 ([email protected]).
A Review of Body Dysmorphic Disorder
and Its Presentation in Different Clinical Settings
ABSTRACT
Objective: Body dysmorphic disorder (BDD) is a relatively common psychiatric disorder characterized by preoccupations with perceived defects in physical appearance. This review aimed to explore epidemiology, clinical features, comorbidities, and treatment options for BDD in different clinical settings.
Data Source and Study Selection: A search of the literature from 1970 to 2011 was performed using the MEDLINE search engine. English-language articles, with no restriction regarding the type of articles, were identified using the search terms body dysmorphic disorder, body dysmorphic disorder clinical settings, body dysmorphic disorder treatment, and body dysmorphic
disorder & psychodermatology.
Results: BDD occurs in 0.7% to 2.4% of community samples and 13% of psychiatric inpatients. Etiology is multifactorial, with recent findings indicating deficits in visual information processing. There is considerable overlap between BDD and obsessive-compulsive disorder (OCD) in symptom etiology and response to treatment, which has led to suggestions that BDD can be classified with anxiety disorders and OCD. A recent finding indicated genetic overlap between BDD and OCD. Over 60% of patients with BDD had a lifetime anxiety disorder, and 38% had social phobia, which tends to predate the onset of BDD. Studies reported a high level of comorbidity with depression and social phobia occurring in > 70% of patients with BDD. Individuals with BDD present frequently to dermatologists (about 9%–14% of dermatologic patients have BDD). BDD co-occurs with pathological skin picking in 26%–45% of cases. BDD currently has 2 variants: delusional and nondelusional, and both variants respond similarly to serotonin reuptake inhibitors (SRIs), which may have effect on obsessive thoughts and rituals. Cognitive-behavioral therapy has the best established treatment results.
Conclusions: A considerable overlap exists between BDD and other psychiatric disorders such as OCD, anxiety, and delusional disorder, and this comorbidity should be considered in evaluation, management, and long-term follow-up of the disorder. Individuals with BDD usually consult dermatologists and cosmetic surgeons rather than psychiatrists. Collaboration between different specialties (such as primary care, dermatology, cosmetic surgery, and psychiatry) is required for better treatment outcome.
Prim Care Companion CNS Disord 2013;15(4): doi:10.4088/PCC.12r01464
© Copyright 2013 Physicians Postgraduate Press, Inc.
Submitted: September 10, 2012; accepted February 22, 2013.
Published online: July 18, 2013.
Corresponding author: Mohammad Jafferany, MD, Department of Psychiatry and Behavioral Sciences, Central Michigan University, College of Medicine, East Campus, 1000 Houghton Ave, Saginaw, MI 48602 (mjafferany @yahoo.com).
Body dysmorphic disorder (BDD), also known as dysmorphophobia and dermatologic nondisease, is a relatively common disorder that occurs in 0.7% to 2.4% of the general population.1–3 The disorder is characterized by a preoccupation with an imagined or slight defect in one’s physical appearance. Alternatively, if there is a slight physical anomaly, the person’s concern is markedly excessive. Their preoccupation is associated with time-consuming rituals, such as mirror gazing or constantly comparing their imagined ugliness with other people or comparing parts of their own body. Patients with BDD have a distorted body image, which may be associated with bullying or abuse during childhood or adolescence. They often seek unnecessary dermatologic treatment and cosmetic surgery.1,2 This review aimed to explore epidemiology, clinical features, comorbidities, and treatment options for BDD in different clinical settings.
METHOD
A search of the literature from 1970 to 2011 was performed using the MEDLINE search engine. English-language articles, with no restriction regarding the type of articles, were identified using the search terms body dysmorphic disorder, body dysmorphic disorder clinical settings, body dysmorphic disorder treatment, and body dysmorphic disorder & psychodermatology.
HISTORICAL PERSPECTIVES
For many centuries, appearance, beauty, and body image have occupied the minds of the human race and have been associated with social distinction. Archaeological references to cosmetics have been discovered in tombs from the ancient Egyptian pharaohs.4 Body dysmorphic disorder has been described for well over a century as dermatologic hypochondriasis, beauty hypochondria, dermatophobia, and, as mentioned previously, dermatologic nondisease.5
The term dysmorphophobia was first coined by Enrico Morselli (1891) to describe worries and complaints over an imagined deformity.6,7 The term was derived from the Greek word dysmorfia, meaning a bad body or unattractive. Dysmorfia first appeared in the Histories of Herodotus referring to the myth of the “Ugliest girl in Sparta.”6,7 Morselli classified dysmorphophobia as a rudimentary paranoia or abortive monomania. He also described taphephobia, which is an obsessional fear of being buried alive associated with frequent reassurance seeking and checking whether death has occurred.6,7 Other examples of historical references for dysmorphophobia include Hanns Kaan (1892) and his book on neurasthenia and obsession; the French psychiatrist Pierre Janet (1903), who described the first possible use of behavior therapy; and Ernest Dupre (1907), who explained the fears as being derived from a disturbance in proprioceptive information.6,7
Body dysmorphic disorder first appeared in the DSM-IV in 1980 and was described as an atypical somatoform disorder.8 The American Psychiatric Association classified BDD as a distinct somatoform disorder in 1987, and it has received particular attention in the media and in clinical research since then.9
CRITERIA FOR BDD DIAGNOSIS
The DSM-IV criteria for diagnosis of BDD are (1) preoccupation with an imagined or barely perceptible defect in appearance, (2) the preoccupation causes marked distress and impairment in social and occupational functioning, and (3) the appearance concern is not better accounted for by another mental disorder.10 Appearance concerns are common in the general population; in BDD, the preoccupation must cause clinically significant distress or impaired social or occupational functioning, which differentiates the disorder from normal appearance concerns. The DSM-IV classification of BDD is controversial in that BDD is classified as a somatoform disorder, while its delusional variant is classified as a psychotic disorder. Phillips et al11 investigated the 2 BDD variants (delusional and nondelusional) and found that 36% of BDD subjects were delusional. Adolescents were found to be more delusional than adults.11 The upcoming DSM-5 recommendation is to move BDD from somatoform disorders to the classification of anxiety and obsessive-compulsive spectrum disorders. There is also discussion of adding a specification for muscle dysmorphia, wherein an individual obsesses that his or her body is too small or insufficiently muscular.
The preoccupation with the perceived defect in appearance is usually an overvalued idea, but individuals can receive an additional diagnosis of delusional disorder, somatic type. The syndrome overlaps with symptoms of delusional disorder, hypochondriasis, and obsessive-compulsive disorder (OCD), and the condition is a subgroup of the broader ICD-10 category of hypochondriasis.6
CLINICAL FEATURES OF BDD
Patients with BDD have a pervasive subjective feeling of ugliness regarding some aspect of their appearance despite a normal or nearly normal appearance. They are convinced that some part of their body is too large, too small, or misshapen. To other people, the appearance is normal or there is a trivial abnormality. In the latter situation, it may be difficult to decide whether the preoccupation is disproportionate. The common concerns are about the nose, ears, mouth, breasts, buttocks, or penis. BDD patients are constantly preoccupied by their beliefs, feeling that other people notice and talk about the supposed deformity, and they blame all of their difficulties on it. They generally feel misunderstood and are secretive about their symptoms because they think they will be viewed as vain or narcissistic. They may be involved in time-consuming behaviors aiming to reexamine, improve, or hide the perceived defect, with considerable social impairment. They are more likely to complain of depression or social anxiety unless they are specifically questioned about symptoms of BDD. Avoidance behaviors such as mirror avoidance or the avoidance of social activities are also common. In children, BDD may present with symptoms of refusing to attend school and planning suicide. The symptoms of BDD are generally similar to symptoms of OCD, but 27% to 39% of patients with BDD are delusional, most of them do not recognize that their belief is due to a mental illness, and insight is poorer in BDD patients than in OCD patients.1,2,12–14
ETIOLOGY AND PATHOPHYSIOLOGY
The etiology of body dysmorphic disorder is multifactorial, including biological, psychological, and sociocultural factors. Neuropsychological and brain-imaging studies have suggested that there may be impairment of frontostriatal and temporoparietaloccipital circuits.15 Feusner et al16 compared patterns of brain activation in patients with BDD and control subjects. They found that patients with BDD had greater left hemisphere activity relative to controls, particularly in lateral prefrontal cortex and lateral temporal lobe regions, for all face tasks (and dorsal anterior cingulate activity for the low spatial frequency task). For the high spatial frequency task, the BDD group showed statistically significant left middle and temporal gyri activation relative to the control group.16 A recent case-control study,17 which aimed to examine patterns of brain activation in BDD subjects, concluded that there were abnormalities in visual processing and frontostriatal systems in BDD that may be associated with symptoms of obsessive thoughts and compulsive behaviors. The findings also indicated hypoactivation of occipital cortex for low spatial frequency faces, which could possibly be due to either primary visual system abnormalities for configural face elements or top-down modulation of visual processing.17
A study of brain morphology18 revealed significantly smaller mean volumes of orbitofrontal cortex and anterior cingulate cortex in individuals with BDD compared to healthy control subjects. The mean white matter volume of those with BDD was found to be larger than that of control subjects. These findings may provide evidence supporting inclusion of BDD as an obsessive-compulsive spectrum disorder.18 Findings of a recent genetic study19 also supported recommendations to group BDD together with OCD. Body dysmorphic and obsessive-compulsive traits were found to share a common genetic basis. About 65% of their phenotypic correlation was explained by shared genetic factors. Serotonin and tryptophan dysregulation has been implicated.19 Neurobiological factors are therefore believed to have implications in the development of BDD. There is limited research on the neurobiological factors, with some evidence suggesting that BDD has a genetic underpinning.9 Abnormal serotonergic and dopaminergic functions are evident by a patient’s response to medications acting on these neurotransmitters. Neuronal injury to the frontotemporal region and deficits in parietal brain region are also suggested etiologic factors. Neurobiology of pathological skin picking, which may be associated with BDD, suggests an increase of symptoms due to dopaminergic agonists, possibly via the same mechanisms by which cocaine and amphetamine increase dopamine in the ventral striatum.20 Patients who abuse such drugs experience uncontrollable skin picking to the extent of causing tissue damage.8,20
Various psychological theories have been hypothesized in an attempt to explain the development of BDD such as the “self-discrepancy theory,” which suggests that, in patients with BDD, there are differences, especially between the self-ideal and self-should.21,22 There are 2 important concepts in the context of the psychopathology of body image that relate to beliefs. The first concept is valence or body image investment, which is a measure of the importance attached to one’s own appearance. The second concept is body image value, which is defined as the evaluation of one’s body image (eg, rating of satisfaction or dissatisfaction).7
Individuals with BDD are thought to be extremely regressed and to have suffered significant trauma that has affected their body integrity at a very early age.23 This trauma may have interfered with their psychological development and their ability to reflect on their own experiences and to form meaningful attachments with others.23
The first experimental study on the psychopathology of mirror gazing in BDD24 revealed that BDD patients have an eternal hope that they will look different to their internal body image or feel comfortable with their appearance, and these patients are uncertain about their body image and demand to know exactly how they look. The study further revealed that BDD patients believe they will feel worse if they resist gazing, and they are driven by a desire to camouflage their appearance or excessively groom to make themselves look their best or to feel comfortable.24
EPIDEMIOLOGY
Body dysmorphic disorder is a relatively common somatoform disorder that occurs in 0.7% to 2.4% of community samples, 2% to 13% of nonclinical student samples, and 13% of psychiatric inpatients. Individuals suffering from BDD present frequently to dermatologists (about 9%–12% of patients seen by dermatologists have BDD) and plastic surgeons (about 6%–15% of patients seeking cosmetic surgery have BDD).3,25 In a prospective study of the course of BDD for up to 8 years in a sample of 514 participants,26 1.8% to 4.8% had current BDD and 2.6% to 6.1% had lifetime BDD.
Patients with BDD attending a psychiatric clinic have been found to have an equal male:female ratio, and they are usually single or separated and unemployed. In the community, more women are affected overall, with the majority experiencing milder symptoms.1 Body dysmorphic disorder usually begins early in adolescence; 1 study found one-third of inpatient adolescents currently had a body image disorder or problematic body image concerns.27
PSYCHIATRIC COMORBIDITY
Patients with BDD have high levels of distress, are highly symptomatic, and have poor well-being; they also have high scores for depression, anxiety, and anger-hostility on assessment questionnaires compared with normal controls. However, the delusional BDD variant is associated with more comorbidity than the nondelusional variant.10,28 A study of Axis I comorbidity in patients with BDD29 showed that 21.7% of BDD participants had 1, 28.6% had 2, and 41.4% had 3 or more Axis I psychiatric comorbidities. Patients with BDD have poor mental health–related quality of life and high lifetime rates of psychiatric hospitalization (48%), suicidal ideation (45%–82%), and suicide attempts (22%–24%).28
Dyl et al27 documented a relationship between weight-related body image concerns and higher levels of psychopathology in adolescents. They found that patients with significant weight/shape concerns also endorsed significantly more symptoms of depression, anxiety, and suicidality, as well as higher levels of dissociation, sexual concerns, and posttraumatic stress disorder symptomatology. Associated comorbidity in BDD may include depression, impairment in social and occupational functioning, social phobias, OCD, skin picking, marital difficulties, and substance abuse.30 Different models have proposed explanations for comorbidity among disorders, such as chance association (random co-occurrence), symptom nonspecificity, and shared etiology or pathophysiology.29 The latter may explain the high comorbidity of anxiety, OCD, and delusional disorder with BDD.
Anxiety disorders frequently co-occur with BDD. Over 60% of BDD patients were reported to have a lifetime history of an anxiety disorder.28 The lifetime co-occurrence rate for social phobia is roughly 38%, which tends to predate the onset of body dysmorphic disorder.8 The psychiatric literature focused on the obsessions and repetitive behaviors of BDD (eg, mirror checking and grooming) has debated its relationship to OCD.31 On the basis of the high comorbidity of BDD with OCD, the concept of shared etiology/pathophysiology was proposed to explain this co-occurrence, and it was suggested that BDD may be considered an obsessive-compulsive spectrum disorder because of similarities between both conditions.28,32 Gunstad and Phillips29 found co-occurrence of OCD plus major depression was the second most frequent Axis I comorbid disorder in BDD (25%). No subject in their study had a history of Tourette’s syndrome, in contrast to the 5% to 10% rate reported for OCD.29 Eisen and colleagues33 compared insight in 64 adult outpatients with DSM-IV OCD and 85 adult outpatients with DSM-IV BDD and found that the overall insight was significantly worse in the BDD group, of which 39% were delusional compared to only 2% of OCD patients. The poorer insight and the delusional characteristic make it difficult to convince patients to accept psychopharmacologic interventions. From a phenomenologic point of view, BDD is thought to be closely connected to shame and guilt, which are reflexive emotions closely connected to development of self-consciousness and intersubjectivity.34
Over the past century, BDD has been hypothesized to be related to OCD; but, more recently, BDD has also been hypothesized and argued to be a form of affective spectrum disorder.32 Nearly all studies report a high level of comorbidity with depression and social phobia, which is estimated to occur in more than 70% of BDD patients and could explain the response of the disorder to selective serotonin reuptake inhibitors (SSRIs).22 Suicidal ideation (78%–81%) and suicidal attempts (24%–28%) are common in individuals with BDD.2 The rate of completed suicide appears to be markedly high in those with BDD, with an annual rate of 0.35%, which is approximately 45 times higher than that of the US general population and higher than that for most other mental disorders.2
In a study examining time-varying associations between BDD and comorbid psychiatric disorders,35 after 1 to 3 years follow-up of 161 participants, significant longitudinal associations between BDD and major depression were found. Change in the status of BDD and major depression was closely linked in time, with improvement in major depression predicting BDD remission, and, conversely, improvement in BDD predicting depression remission.35 The study also found that improvement in OCD predicted BDD remission, but BDD improvement did not predict OCD remission.35 A study including 126 subjects with a mean BDD duration of 16 years36 showed that 79.5% reported a history of suicidal ideation; 27.6% had a history of a suicide attempt, and 2 subjects committed suicide (both were receiving psychiatric treatment at the time of their deaths). At their last interview, both subjects had extremely severe BDD (score of 7 on the Psychiatric Status Rating for BDD) and both considered BDD their primary most problematic diagnosis.36
BDD IN GENERAL DERMATOLOGY
AND COSMETIC DERMATOLOGY SETTINGS
Patients with BDD are most likely to present to cosmetic surgeons; dermatologists; ear, nose, and throat surgeons; or primary care physicians. They are usually not formally diagnosed by mental health professionals until 10 to 15 years after the onset of BDD.1
The motives for those who seek cosmetic procedures are varied and may include desire to enhance self-confidence, body image, and feminine feeling; a desire to show independence and self-empowerment; a desire to overcome issues from an actual or perceived physical abnormality; and a desire to stand out and attract attention or appear more desirable.6
Individuals with BDD may display a variable spectrum of imagined/perceived defects in appearance that can involve quality and quantity of the skin and its related structures (eg, hair, nails, sweat glands, etc), as well as asymmetries or disproportionate appearance. Commonly reported anomalies include hair loss or hypertrichosis, pigmentary disorders, pore size, vessel pattern, pallor, or reddening of the skin, as well as sweating.22
Individuals with BDD might be involved in compulsive behaviors that can sometimes become destructive, frequently worsening a mild or nonexistent condition. Examples of these compulsive behaviors include skin picking, excessive scratching, removing their own moles, scouring their skin with harsh household chemicals, and performing other “do it yourself” procedures with catastrophic results.23
A recent study by Conrado and colleagues37 found higher BDD prevalence in a cosmetic dermatology group (14.0%) compared with general dermatology (6.7%) and control (2.0%) groups. Frequently, the reason for seeking dermatologic treatment was not the main BDD preoccupation, and patients with BDD from the cosmetic group were, in general, unsatisfied with the results of dermatologic treatments.37
Body dysmorphic disorder co-occurs with pathological skin picking in 26% to 45% of cases. Skin picking, also described as neurotic excoriation, behavior varies in severity level patterns and often occurs in the presence of other psychiatric disorders. Skin picking initially relieves tension and provides its own source of distress, shame, embarrassment, and impairment.38 It is time-consuming (often lasting 5–60 minutes per episode) and can result in infections and bleeding.38
Skin picking commonly occurs as a symptom of BDD, but this self-injurious behavior is heterogeneous and can occur as a symptom of a variety of underlying disorders. Skin picking was considered the result of obsessive-compulsive spectrum disorder in 52% of cases.5 It can also appear as a habit and not be triggered by an obsessional thought.5 A case report by O’Sullivan et al39 demonstrated that skin picking secondary to BDD can be very severe, even life-threatening. As a result of using tweezers in an attempt to remove a perceived defect from her skin, a female patient nearly lacerated her carotid artery.39 The patient’s internist and surgeon reported that her wound would have been fatal if it was slightly more lateral. The patient fulfilled the DSM-IV criteria for both BDD and delusional disorder, somatic type, and was responsive to SSRI treatment.39
Hair concerns are common in BDD patients, including preoccupations with hair loss, fear of going bald, and focus on excessive facial hair or too much or too little body hair. Patients may go to great lengths to cover these body areas and may shave, wax, or pluck body hair excessively. Hair plucking can be time-consuming and can be ritualistic. Hair plucking can result in disfigurement, infection, and scarring. The hair plucking associated with BDD should be differentiated from normal hair plucking and that of trichotillomania.5
BDD-BY-PROXY
In rare cases, BDD can present as concerns about someone else’s appearance, so-called BDD-by-proxy. In a reported case, the patient requested to terminate pregnancy based on her beliefs that the child might be born with dysmorphic features, and she had a sense of relief after each termination.40
BDD AND SURGERY
A study by Crerand et al8 noted more than 10 million cosmetic surgical procedures were performed in 2005, raising the interest in psychological characteristics of this population. A review of the research on the psychological characteristics of individuals who seek cosmetic surgery revealed high levels of psychopathology in interview-based investigations for cosmetic surgery patients compared with standardized measurements.3,41
Body dysmorphic disorder is common in cosmetic surgery clinics; between 5% to 15% of patients in cosmetic surgery clinics have BDD.1 A study by Veale and colleagues42 reported the frequency of BDD in patients requesting rhinoplasty by using a screening questionnaire for BDD. They found that 20.7% of patients requesting rhinoplasty had a possible diagnosis of BDD, which they categorized as subclinical or very mild. In a second stage, the researchers compared patients without BDD who had a good outcome after cosmetic rhinoplasty with BDD patients seen in a psychiatric clinic (who crave cosmetic rhinoplasty but do not obtain it). They found that BDD patients are significantly younger, are more depressed and anxious, and are more preoccupied by their nose and check their nose more frequently. These patients have multiple concerns about their body and are more likely to be significantly impaired in their occupation, social life, and intimate relationships and to avoid social situations because of their nose. Therefore, these individuals are more likely to believe that dramatic changes would occur in their life after a rhinoplasty.42
Prevalence screening for BDD in a maxillofacial surgery outpatient clinic found that 17% of patients reported preoccupation, with excessive concern about their appearance causing moderate to severe distress and/or impairment in functioning, and 10% were found to have BDD, with aesthetic appearance being one of the main reasons to seek orthodontic or orthognathic surgical treatment.43 Patients with BDD may present to surgeons with bizarre and serious self-injuries based on their concerns of a malfunctioning body part. Rarely, BDD patients may wish for amputation of a healthy limb, which raises questions regarding ethical and legal issues of such cases. Such patients with extreme symptoms may self-amputate a limb based on their beliefs that it is not functioning.44
BDD, OBESITY, AND EATING DISORDERS
Psychosocial complications of obesity and eating disorders may include body image disturbance and BDD. Body image is a concept different from BDD, and those who have body image disturbance are not necessarily suffering from BDD. Body image is the image a person constructs of how they appear and how they imagine they appear to others. It includes perceptual, cognitive-affective, and behavioral components. Legenbauer and colleagues45 assessed various components of body image in patients with obesity using a photo distortion technique and biological motion distortion device to assess static and dynamic aspects of body image. They used questionnaires that assessed cognitive-affective aspects, bodily attitudes, and eating behavior. Patients with obesity and a binge-eating disorder compared with patients with obesity only were both found to have high levels of body image disturbances with cognitive-affective deficits. Binge-eating disorder subjects also had problems related to perceptual components of body image.45
Patients with anorexia and BDD share severe body image concerns, but little has been written about the relationship between both conditions and their possible overlap. Many patients with anorexia have appearance concerns other than weight and body shape.31 Individuals with eating disorders may also have comorbid BDD. Kollei et al46 assessed 49 subjects with anorexia nervosa and 51 subjects with bulimia nervosa and found that 12% of individuals with eating disorders had comorbid BDD, with their body dysmorphic concerns being unrelated to weight and shape, focusing instead on skin, hair, teeth, nose, and height.
Dixon et al47 used the appearance orientation and appearance evaluation sections of the Multidimensional Body Self Relations Questionnaire to compare body image in preoperative patients and those attending follow-up after lap band gastric restrictive surgery. Major improvements in appearance evaluation occurred with weight loss after surgery, while appearance orientation was found to be similar to community samples, except in superobese (BMI > 50) individuals, who placed significantly less importance on their appearance
MANAGEMENT OF BDD
Research has identified 2 effective treatments for BDD since it was formally recognized as a disorder in 1987: serotonin reuptake inhibitors (SRIs) and cognitive-behavioral therapy (CBT).48 Early case reports showed mixed, but largely negative, outcomes with a variety of psychotropic agents and electroconvulsive therapy.49 Procedures aimed to treat the underlying physical defect, usually performed by a plastic surgeon, dermatologist, or other medical subspecialist, have proved unsuccessful in patients with BDD.50 Worries concerning body image do not seem to be reduced after cosmetic procedures, even if the outcome is objectively acceptable; and patients with BDD generally appear to be dissatisfied with dermatologic treatments.6
Outcomes of cosmetic medical treatment among individuals with BDD gathered from retrospective studies and reports from the cosmetic surgery literature indicate poor outcomes among patients thought to have BDD.7 The probability of full recovery from BDD was 0.76 over 8 years, and probability of recurrence was 0.14 over an 8-year prospective study. In individuals assessed for anxiety disorders, the probability of recovering from BDD was relatively high and probability of BDD recurrence was low.25 In another study,11 delusional and nondelusional subjects had a similar probability of remitting from BDD over 1 year of prospective follow-up.
Pharmacotherapy
The SRIs and SSRIs are often effective for BDD; they are antidepressants that can decrease obsessions and repetitive behaviors. Treatment response in the medication trials was not affected by the degree of insight into their condition.51 Treatment with both medication and psychotherapy can be effective in treating BDD.51 Various therapeutic interventions used for treatment of BDD are summarized in Table 1.
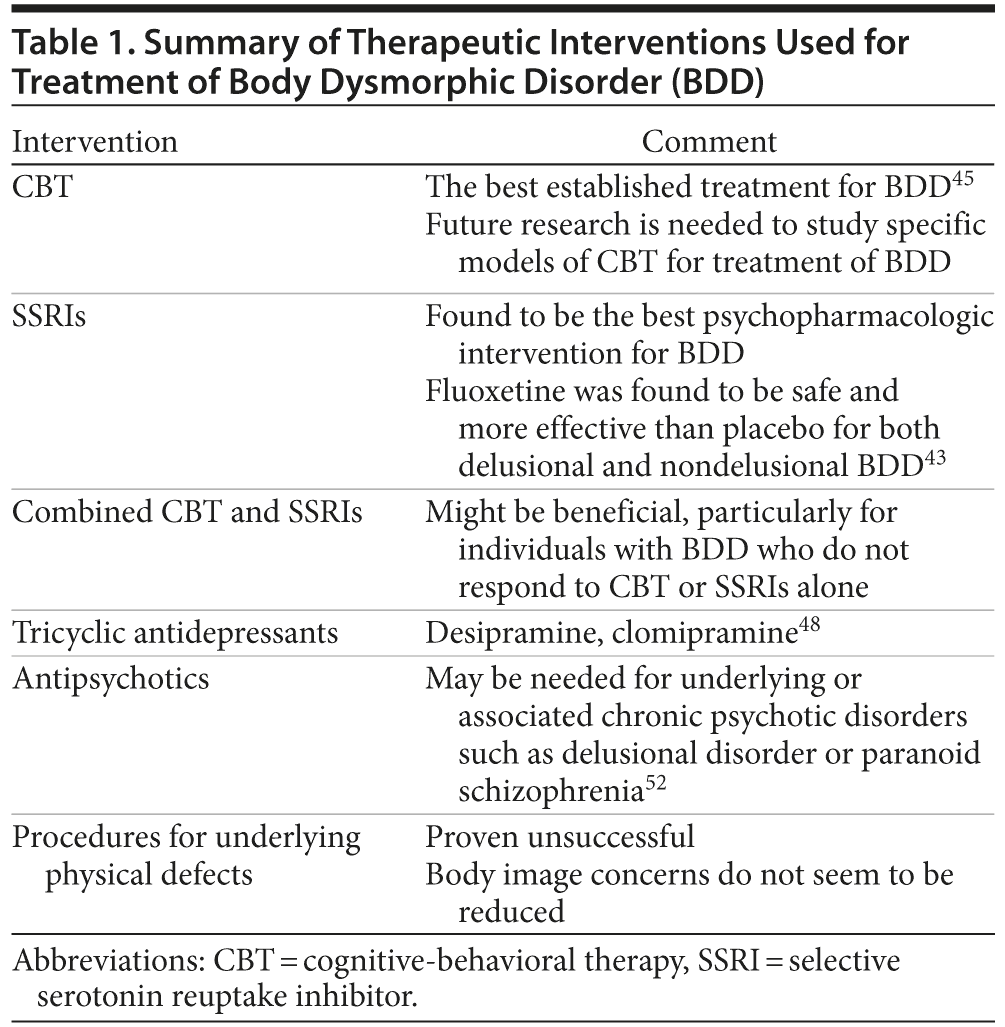
A study including 74 patients with BDD or its delusional variant found fluoxetine to be safe and more effective than placebo in delusional and nondelusional patients with BDD.49 A 16-week open-label fluvoxamine treatment study28 that included 27 subjects showed significant improvement in BDD symptoms for both delusional and nondelusional patients. An open-label study of escitalopram in body dysmorphic disorder52 that included 14 subjects found that almost one-half of subjects were very much improved, and one-third were much improved. There also was a significant decrease in delusionality of appearance beliefs.52
A 16-week randomized, double-blind, crossover-design study of clomipramine and desipramine5 3 found clomipramine to be superior to desipramine in the acute treatment of BDD symptoms. There are mixed results from preliminary reports of augmenting antipsychotics with SSRIs.54 The course of BDD tends to be continuous rather than episodic; although symptom severity and degree of insight can fluctuate over the course of the disorder. Complete remission seems to be rare even after treatment.8
Cognitive-Behavioral Therapy
Cognitive-behavioral therapy is a multifaceted treatment based on learning principles, which have validated efficacy for many disorders. Treatment with CBT involves determining the maladaptive thoughts and behaviors that are maintaining the patient’s BDD symptoms and undermining their functioning and finding ways to change these maladaptive thoughts and behaviors. The treatment also usually involves relaxation training, including deep breathing and muscle relaxation, which could also be applied for patients with BDD.48
A model for BDD should focus on features unique to BDD such as the relationship with reflective surfaces (eg, mirrors or old photos) that may trigger the symptoms.55 A pilot controlled trial conducted by Veale et al5 6 tested a specific CBT model for BDD patients, patients with real disfigurements who seek cosmetic surgery but are emotionally well-adjusted, and healthy controls without any defect. They found significant changes in the group treated with CBT who obtained a 50% reduction in symptoms using the Yale-Brown Obsessive Compulsive Scale (modified for BDD) and Depression Rating Scale as outcome measures.56
Cognitive-behavioral therapy for negative body image may be effective in patients with distorted body image both with and without diagnosis of BDD. Therapy involves modification of intrusive thoughts of body dissatisfaction and overvalued beliefs about physical appearance, exposure to avoided body image situations, and elimination of body checking. Rosen and colleagues57 compared normal weight women with disturbed body image but without eating disorders, who were randomly assigned to CBT with those assigned for minimal treatment; subjects who received CBT showed greater improvements in size overestimation, body dissatisfaction, and behavioral avoidance compared to subjects in minimal treatment.57 In another study,58 cognitive-behavioral body image therapy for BDD was found to be effective; symptoms were significantly decreased in therapy subjects, and the disorder was eliminated in 82% of cases at posttreatment and 77% at follow-up.
A review of 34 randomized controlled trials involving 3,922 patients with somatoform disorders50 found CBT to be the best established treatment for a variety of somatoform disorders including BDD and hypochondriasis.
Pharmacotherapy Versus
Cognitive-Behavioral Therapy
A review by Ipser et al5 9 assessed the efficacy of pharmacotherapy, psychotherapy, or a combination of both treatment modalities for BDD consisting of 5 eligible trials, according to search criteria, including 3 of psychotherapy and 2 of medication. Fluoxetine had overall superiority of medication relative to placebo. Symptom severity reduced significantly in the randomized control trials of fluoxetine and clomipramine. Symptoms were also significantly reduced in 2 CBT trials, and the relapse rate was found to be low in 1 trial of CBT.59
FUTURE BDD CLASSIFICATION
Much more research is needed in all aspects of BDD including symptoms, current diagnostic criteria, classification of its delusional and nondelusional variants, and its relation to other psychiatric disorders. As mentioned previously, there are suggestions for considering BDD as part of the obsessive-compulsive spectrum disorders in the DSM-5, although current findings indicate that it is not simply a subtype of OCD.60,61
THE ROLE OF GENERAL HEALTH PROVIDERS
IN THE IDENTIFICATION AND MANAGEMENT
OF PATIENTS WITH BDD
Statistics regarding the prevalence of BDD in primary care settings are needed to compare the magnitude of the problem with those in dermatology, cosmetic surgery, and other specialties. Statistics are needed to facilitate provision of optimal care for patients with BDD in primary care. Proper evaluation of patients with BDD is essential for understanding the individual’s suffering and for setting a management plan. The assessment may include taking a history, a physical and mental state examination, routine workup to rule out medical causes, and discussion of various psychological and pharmacologic options.
SUGGESTIONS FOR THE MANAGEMENT OF BDD
Suggestions for BDD management are as follows:
- The main clinical features are appearance preoccupations and repetitive behaviors.
- Possible complications may include anxiety, depression, and suicide.
- BDD should be differentiated from other psychiatric disorders such as psychosis and other somatoform disorders.
- Clinically significant distress and impairment in the level of social and occupational functioning may be present.
- Insight is usually impaired.
- Once the diagnosis of BDD is confirmed, psychoeducation should be offered to the patient regarding the disorder and its treatment options. Attempts to correct the perceived defect, medically or surgically, are not useful. It is better to use SSRIs such as fluoxetine, fluvoxamine, escitalopram, and clomipramine.
- Treatment with CBT should be used if available. The choice of treatment depends on many factors, such as patient preference, motivation, and the availability of CBT. However, both CBT and pharmacotherapy may be combined for better outcome.
An approach for management of BDD is summarized in Table 2.

CONCLUSION
An understanding of the psychological basis of body image preoccupations and the clinical presentation of BDD is important in selection of proper therapeutic interventions. It is important to recognize that individuals with BDD may lack insight into the psychological nature of BDD. Knowledge and a high index of suspicion are necessary to diagnose BDD, and clinicians should adopt a multidisciplinary approach in management, including collaboration among those in dermatology, psychiatry, cosmetic surgery, family practice, and other specialties. Treatment with CBT should be considered in individuals with BDD due to its established results. Identification of the psychopathology and determination of whether the BDD variant is of a delusional or nondelusional nature may aid in diagnosis and management, although SSRIs may be effective in both variants. Further research on psychopharmacologic interventions is needed, particularly with regard to the role of antipsychotics in the management of the delusional variant or as adjunctive treatment for difficult cases of a nondelusional nature.
Drug names: clomipramine (Anafranil and others), desipramine (Norpramin and others), escitalopram (Lexapro and others), fluoxetine (Prozac and others), fluvoxamine (Luvox and others).
Author affiliations: Behavioral Sciences Institute, Alain Hospital, Al Ain, United Arab Emirates (Dr Mufaddel); Department of Psychiatry and Behavioral Sciences, Faculty of Medicine and Health Sciences, United Arab Emirates University, United Arab Emirates (Dr Osman); Department of Psychiatry and Behavioral Science, Faculty of Medicine and Health Sciences, United Arab Emirates University, Al Ain, United Arab Emirates (Ms Almugaddam); and Department of Psychiatry and Behavioral Sciences, Central Michigan University, College of Medicine, and Jafferany Psychiatric Services (Dr Jafferany), Saginaw, Michigan.
Potential conflicts of interest: None reported.
Funding/support: None reported.
REFERENCES
1. Veale D. Body dysmorphic disorder. Postgrad Med J. 2004;80(940):67–71. doi:10.1136/pmj.2003.015289 PubMed
2. Phillips KA, Hollander E. Treating body dysmorphic disorder with medication: evidence, misconceptions, and a suggested approach. Body Image. 2008;5(1):13–27. doi:10.1016/j.bodyim.2007.12.003 PubMed
3. Koran LM, Abujaoude E, Large MD, et al. The prevalence of body dysmorphic disorder in the United States adult population. CNS Spectr. 2008;13(4):316–322. PubMed
4. Osman OT. The skin as a mode of communication. Expert Rev Dermatol. 2010;5(5):493–496. doi:10.1586/edm.10.46
5. Castle DJ, Phillips KA, Dufresne RG Jr. Body dysmorphic disorder and cosmetic dermatology: more than skin deep. J Cosmet Dermatol. 2004;3(2):99–103. doi:10.1111/j.1473-2130.2004.00105.x PubMed
6. Osman OT, Mufaddel A, Almugaddam F, et al. The psychiatric aspects of skin disorders. Expert Rev Dermatol. 2011;6(2):195–209. doi:10.1586/edm.11.10
7. Veale D, Neziroglu E. Body Dysmorphic Disorder: A Treatment Manual, First Edition. New York, NY: Wiley Blackwell; 2010:31–39.
8. Crerand CE, Franklin ME, Sarwer DB. Body dysmorphic disorder and cosmetic dermatology. Plast Reconstr Surg. 2006;118(7):167–180. doi:10.1097/01.prs.0000242500.28431.24
9. Hunt TJ, Theinhans O, Ellwood AY. The mirror lies: body dysmorphic disorder. Am Fam Physician. 2008;15;78(2):217–222. PubMed
10. American Psychiatric Association. Diagnostic and Statistical Manual of Mental Disorders, Fourth Edition. Washington, DC: American Psychiatric Association; 1994.
11. Phillips KA, Menard W, Pagano ME, et al. Delusional versus nondelusional body dysmorphic disorder: clinical features and course of illness. J Psychiatr Res. 2006;40(2):95–104. doi:10.1016/j.jpsychires.2005.08.005 PubMed
12. Gelder M, Cowen P, Harrison P. Shorter Oxford Textbook of Psychiatry, Fifth Edition. New York, NY: Oxford University Press; 2006:209–210
13. Sadock BJ, Kaplan HI. Kaplan and Sadock’s Synopsis of Psychiatry: Behavioral Sciences, Clinical Psychiatry, Eighth Edition. New York, NY: Lippincott Williams & Wilkins; 1998:643–660.
14. Buhlmann U, Winter A. Perceived ugliness: an update on treatment-relevant aspects of body dysmorphic disorder. Curr Psychiatry Rep. 2011;13(4):283–288. doi:10.1007/s11920-011-0203-5 PubMed
15. Carey B, Seedat S, Warwick J, et al. SPECT imaging of body dysmorphic disorder. J Neuropsychiatry Clin Neurosci. 2004;16(3):357–359. PubMed
16. Feusner JD, Townsend J, Bystritsky A, et al. Visual information processing of faces in body dysmorphic disorder. Arch Gen Psychiatry. 2007;64(12):1417–1425. doi:10.1001/archpsyc.64.12.1417 PubMed
17. Feusner JD, Moody T, Hembacher E, et al. Abnormalities of visual processing and frontostriatal systems in body dysmorphic disorder. Arch Gen Psychiatry. 2010;67(2):197–205. doi:10.1001/archgenpsychiatry.2009.190 PubMed
18. Atmaca M, Bingol I, Aydin A, et al. Brain morphology of patients with body dysmorphic disorder. J Affect Disord. 2010;123(1–3):258–263. doi:10.1016/j.jad.2009.08.012 PubMed
19. Monzani B, Rijsdijk F, Iervolino AC, et al. Evidence for a genetic overlap between body dysmorphic concerns and obsessive-compulsive symptoms in an adult female community twin sample. Am J Med Genet B Neuropsychiatr Genet. 2012;159B(4):376–382. doi:10.1002/ajmg.b.32040 PubMed
20. Odlaug BL, Grant JE. Pathologic skin picking. Am J Drug Alcohol Abuse. 2010;36(5):296–303. doi:10.3109/00952991003747543 PubMed
21. Veale D, Kinderman P, Riley S, et al. Self-discrepancy in body dysmorphic disorder. Br J Clin Psychol. 2003;42(pt 2):157–169. doi:10.1348/014466503321903571 PubMed
22. Harth W, Gieler U. Psychosomatics and dermatology. Psychosomatic CME Dermatol. 2008;3(2):66–76.
23. Aoki R. Pharmacology, immunology and current developments. In: Benedetto AV. Botulinum Toxin in Clinical Dermatology, First Edition. New York, NY: Taylor & Francis; 2006:16–35.
24. Veale D, Riley S. Mirror, mirror on the wall, who is the ugliest of them all? The psychopathology of mirror gazing in body dysmorphic disorder. Behav Res Ther. 2001;39(12):1381–1393. doi:10.1016/S0005-7967(00)00102-9 PubMed
25. Phillips KA, Menard W, Fay C, et al. Demographic characteristics, phenomenology, comorbidity, and family history in 200 individuals with body dysmorphic disorder. Psychosomatics. 2005;46(4):317–325. doi:10.1176/appi.psy.46.4.317 PubMed
26. Bjornsson AS, Dyck I, Moitra E, et al. The clinical course of body dysmorphic disorder in the Harvard/Brown Anxiety Research Project (HARP). J Nerv Ment Dis. 2011;199(1):55–57. doi:10.1097/NMD.0b013e31820448f7 PubMed
27. Dyl J, Kittler J, Phillips KA, et al. Body dysmorphic disorder and other clinically significant body image concerns in adolescent psychiatric inpatients: prevalence and clinical characteristics. Child Psychiatry Hum Dev. 2006;36(4):369–382. doi:10.1007/s10578-006-0008-7 PubMed
28. Phillips KA, Siniscalchi JM, McElroy SL. Depression, anxiety, anger, and somatic symptoms in patients with body dysmorphic disorder. Psychiatr Q. 2004;75(4):309–320. doi:10.1023/B:PSAQ.0000043507.03596.0d PubMed
29. Gunstad J, Phillips KA. Axis I comorbidity in body dysmorphic disorder. Compr Psychiatry. 2003;44(4):270–276. doi:10.1016/S0010-440X(03)00088-9 PubMed
30. Jafferany M. Psychodermatology: a guide to understanding common psychocutaneous disorders. Prim Care Companion J Clin Psychiatry. 2007;9(3):203–213. doi:10.4088/PCC.v09n0306 PubMed
31. Grant JE, Phillips KA. Is anorexia nervosa a subtype of body dysmorphic disorder? Probably not, but read on… . Harv Rev Psychiatry. 2004;12(2):123–126. doi:10.1080/10673220490447236 PubMed
32. Phillips KA, McElroy SL, Hudson JI, et al. Body dysmorphic disorder: an obsessive-compulsive spectrum disorder, a form of affective spectrum disorder, or both? J Clin Psychiatry. 1995;56(suppl 4):41–51. PubMed
33. Eisen JL, Phillips KA, Coles ME, et al. Insight in obsessive-compulsive disorder and body dysmorphic disorder. Compr Psychiatry. 2004;45(1):10–15. doi:10.1016/j.comppsych.2003.09.010 PubMed
34. Fuchs T. The phenomenology of shame, guilt and the body in body dysmorphic disorder and depression. J Phenomenological Psychol. 2002;33(2):223–243. doi:10.1163/15691620260622903
35. Phillips KA, Stout RL. Associations in the longitudinal course of body dysmorphic disorder with major depression, obsessive-compulsive disorder, and social phobia. J Psychiatr Res. 2006;40(4):360–369. doi:10.1016/j.jpsychires.2005.10.001 PubMed
36. Phillips KA, Menard W. Suicidality in body dysmorphic disorder: a prospective study. Am J Psychiatry. 2006;163(7):1280–1282. doi:10.1176/appi.ajp.163.7.1280 PubMed
37. Conrado LA, Hounie AG, Diniz JB, et al. Body dysmorphic disorder among dermatologic patients: prevalence and clinical features. J Am Acad Dermatol. 2010;63(2):235–243. doi:10.1016/j.jaad.2009.09.017 PubMed
38. Neziroglu F, Rabinowitz D, Breytman A, et al. Skin picking phenomenology and severity comparison. Prim Care Companion J Clin Psychiatry. 2008;10(4):306–312. doi:10.4088/PCC.v10n0406 PubMed
39. O’Sullivan RL, Phillips KA, Keuthen NJ, et al. Near-fatal skin picking from delusional body dysmorphic disorder responsive to fluvoxamine. Psychosomatics. 1999;40(1):79–81. doi:10.1016/S0033-3182(99)71276-4 PubMed
40. Laugharne R, Palazidou E. Dysmorphophobia-by-proxy. J R Soc Med. 1997;90:266. PubMed
41. Sarwer DB, Wadden TA, Pertschuk MJ, et al. The psychology of cosmetic surgery: a review and reconceptualization. Clin Psychol Rev. 1998;18(1):1–22. doi:10.1016/S0272-7358(97)00047-0 PubMed
42. Veale D, De Haro L, Lambrou C. Cosmetic rhinoplasty in body dysmorphic disorder. Br J Plast Surg. 2003;56(6):546–551. doi:10.1016/S0007-1226(03)00209-1 PubMed
43. Vulink NC, Rosenberg A, Plooij JM, et al. Body dysmorphic disorder screening in maxillofacial outpatients presenting for orthognathic surgery. Int J Oral Maxillofac Surg. 2008;37(11):985–991. doi:10.1016/j.ijom.2008.06.005 PubMed
44. Chan JK, Jones SM, Heywood AJ. Body dysmorphia, self-mutilation and the reconstructive surgeon. J Plast Reconstr Aesthet Surg. 2011;64(1):4–8. doi:10.1016/j.bjps.2010.03.029 PubMed
45. Legenbauer T, Vocks S, Betz S, et al. Differences in the nature of body image disturbances between female obese individuals with versus without a comorbid binge-eating disorder: an exploratory study including static and dynamic aspects of body image. Behav Modif. 2011;35(2):162–186. doi:10.1177/0145445510393478 PubMed
46. Kollei I, Schieber K, Zwaan M, et al. Body dysmorphic disorder and nonweight-related body image concerns in individuals with eating disorders. Int J Eat Disord. 2012;46 (1):52–59. doi:10.1002/eat.22067 PubMed
47. Dixon JB, Dixon ME, O’Brien PE. Body image: appearance orientation and evaluation in the severely obese. Changes with weight loss. Obes Surg. 2002;12(1):65–71. doi:10.1381/096089202321144612 PubMed
48. Allen A. Cognitive-behavioral treatment of body dysmorphic disorder. Prim Psychiatry. 2006;13(7):70–76.
49. Phillips KA, Albertini RS, Rasmussen SA. A randomized placebo-controlled trial of fluoxetine in body dysmorphic disorder. Arch Gen Psychiatry. 2002;59(4):381–388. doi:10.1001/archpsyc.59.4.381 PubMed
50. Kroenke K. Efficacy of treatment for somatoform disorders: a review of randomized controlled trials. Psychosom Med. 2007;69(9):881–888. doi:10.1097/PSY.0b013e31815b00c4 PubMed
51. Ipser JC, Sander C. Stein DJ. . Pharmacotherapy and psychotherapy for body dysmorphic disorder. Cochrane Database Syst Rev. 2009;21(1):CD005332. PubMed
52. Phillips KA. An open-label study of escitalopram in body dysmorphic disorder. Int Clin Psychopharmacol. 2006;21(3):177–179. doi:10.1097/01.yic.0000194378.65460.ef PubMed
53. Hollander E, Allen A, Kwon J, et al. Clomipramine vs desipramine crossover trial in body dysmorphic disorder: selective efficacy of a serotonin reuptake inhibitor in imagined ugliness. Arch Gen Psychiatry. 1999;56(11):1033–1039. doi:10.1001/archpsyc.56.11.1033 PubMed
54. Phillips KA. Olanzapine augmentation of fluoxetine in body dysmorphic disorder. Am J Psychiatry. 2005;162(5):1022–1023. doi:10.1176/appi.ajp.162.5.1022-a PubMed
55. Veale D. Advances in a cognitive behavioral model of body dysmorphic disorder. Body Image. 2004;1(1):113–125. doi:10.1016/S1740-1445(03)00009-3 PubMed
56. Veale D, Gournay K, Dryden W, et al. Body dysmorphic disorder: a cognitive behavioral model and pilot randomized controlled trial. Behav Res Ther. 1996;34(9):717–729. doi:10.1016/0005-7967(96)00025-3 PubMed
57. Rosen J, Saltzberg E, Srebnik D. Cognitive behavior therapy for negative body image. Behav Ther. 1989;20(3):393–404. doi:10.1016/S0005-7894(89)80058-9
58. Rosen JC, Reiter J, Orosan P. Cognitive-behavioral body image therapy for body dysmorphic disorder. J Consult Clin Psychol. 1995;63(2):263–269. doi:10.1037/0022-006X.63.2.263 PubMed
59. Ipser JC, Sander C, Stein DJ. Pharmacotherapy and psychotherapy for body dysmorphic disorder. Cochrane Database Syst Rev. 2009;(1):CD005332. PubMed
60. Phillips KA, Wilhelm S, Koran LM, et al. Body dysmorphic disorder: some key issues for DSM-V. Depress Anxiety. 2010;27(6):573–591. doi:10.1002/da.20709 PubMed
61. Toh WL, Rossell SL, Castle DJ. Body dysmorphic disorder: a review of current nosological issues and associated cognitive deficits. Curr Psychiatry Rev. 2009;5(4):261–270. doi:10.2174/157340009789542132
Enjoy this premium PDF as part of your membership benefits!


