Prim Care Companion CNS Disord 2022;24(6):22br03276
To cite: Mitra S, Dutta S, Weinstein T, et al. A review of the midlevel care provider system in New York State. Prim Care Companion CNS Disord. 2022;24(6):22br03276.
To share: https://doi.org/10.4088/PCC.22br03276
© 2022 Physicians Postgraduate Press, Inc.
aDepartment of Psychiatry, BronxCare Health System, Bronx, New York
bAmerican University of the Caribbean, Cupecoy, Sint Maarten
*Corresponding author: Souparno Mitra, MD, 1276 Fulton Ave, 5th Floor South, Bronx, NY 10460 ([email protected]).
See letter by Cobb et al
Mental health care has become a subject of much discussion and publicity. The National Institute of Mental Health estimated that approximately 52.9 million patients aged ≥ 18 years were currently coping with mental illness in the United States in 2020.1 They also reported that only 44.8% of this patient population received mental health care in the past year and that more women (51.2%) received care than men (37.4%).1 The provision of care was more prominent in the estimated 64.5% of patients with serious mental illness.1
These statistics clearly show the lack of availability of care that exists for the patient population with mental illness. A study2 by the University of Michigan Behavioral Health Workforce Research Center found 41,133 psychiatrists differentially distributed across the United States. In terms of subspecialties, the deficits are even more evident. Of the 3,135 counties in the United States, only 828 had at least 1 child and adolescent psychiatrist, and only 330 had at least 1 geriatric psychiatrist. The mean ratio between urban and rural counties was also statistically significant, with urban counties having 10.62 psychiatrists per 100,000 population versus 3.28 per 100,000 for rural counties.2
According to a Health Resources and Services Administration report, New York State (NYS) had 5,460 psychiatrists with a need for 3,480 psychiatrists as of 2016.3 Although there is a surplus of psychiatrists compared to other areas of the county, NYS is filling the gaps in care with midlevel providers, including psychiatric nurse practitioners, house physicians, and psychiatric physician assistants. The demand to availability ratio is skewed geographically. For example, as per the report,3 NYS had a surplus of about 1,840 full-time equivalents, while Texas, Florida, and Michigan had a shortage of more than 700.
This report reviews the educational qualifications, licensure requirements, and scope of practice for these midlevel providers. The goal is to look at a model that has worked relatively well in densely populated states like NYS and propose a policy to meet the psychiatric needs of patients in other states. Each state has its own policy related to midlevel providers, discussion of which would be beyond the scope of this report.
METHODS
Data from the NYS Education Department (NYSED), Office of the Professions website4 and the Drug Enforcement Agency website5 were reviewed to define the roles and qualifications for midlevel providers in NYS.
RESULTS
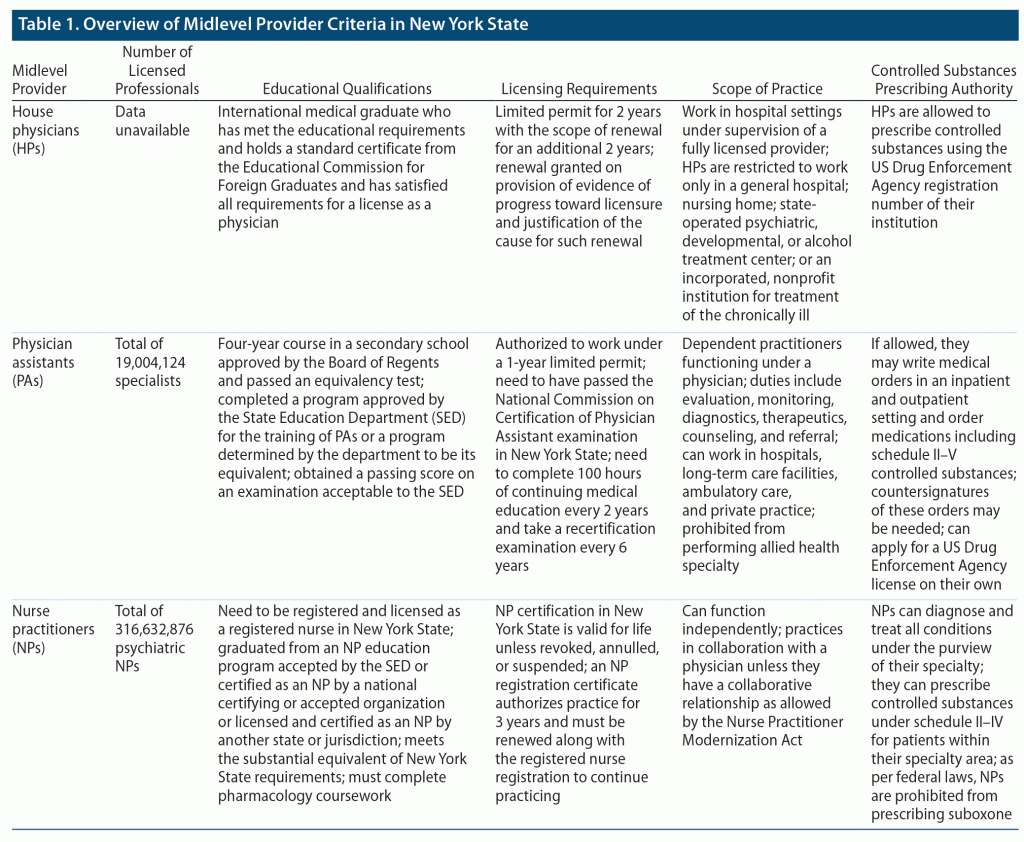
We summarize each level of midlevel provider as per the criteria provided (Table 1).
House Physicians
Number of licensed professionals: Data unavailable.
Educational qualifications: Must be an international medical graduate who has met the educational requirements and holds a standard certificate from the Educational Commission for Foreign Graduates. Alternatively, they must also have satisfied all requirements for a license as a physician except those related to examination and citizenship and permanent residence status in the United States.
Licensing: Upon fulfillment of the previously mentioned qualifications, they can be granted a limited permit for a period of 2 years with the scope of renewal for an additional 2 years. Renewal would only be granted on provision of evidence of progress toward licensure and justification of the cause for such renewal.
Scope of practice: House physicians work in hospital settings under supervision of a fully licensed provider. The supervising physician should be continuously available to the house physician but does not have to be physically present. House physicians are restricted to work only in a general hospital; nursing home; state-operated psychiatric, developmental, or alcohol treatment center; or incorporated, nonprofit institution for the treatment of chronically ill patients.
Application: Submit Form 5A or 5B for limited permit, fee, and other required forms.
Physician Assistants
A physician assistant, as per the American Medical Association, is a skilled person qualified by academic and practical training to provide patient services under the supervision and direction of a licensed physician who is responsible for the performance of that physician assistant. While some states are using the term physician associate, currently the legal title of the profession in NYS is physician assistant and will remain so until legislative and regulatory changes are made to incorporate the new title.
Number of licensed professionals: As of 2019, there were a total of 19,004 physician assistants and 124 specialist assistants in NYS.
Educational qualifications: Physician assistants must have completed a 4-year course of study in a secondary school approved by the Board of Regents and passed an equivalency test. They additionally must have completed a program approved by the NYSED for the training of physician assistants or a program determined by the department to be its equivalent. They also must have obtained a passing score on an examination acceptable to the NYSED.
Licensing: Physician assistants may be authorized to work under a 1-year limited permit. They need to have passed the National Commission on Certification of Physician Assistant Examination, which is the official credentialing examination in NYS. They additionally must complete 100 hours of continuing medical education every 2 years and take a recertification exam every 6 years.
Scope of practice: Physician assistants are dependent practitioners who function under a physician who can delegate to them the performance of any medical procedure that they are trained to perform within the scope of the physician’s expertise. Duties include evaluation, monitoring, diagnostics, therapeutics, counseling, and referral. They can work in hospitals, long-term care facilities, ambulatory care, and private practice. A physician assistant must have 1 and possibly more than 1 supervising physician. A physician may employ or supervise no more than 4 physician assistants at a time. However, they may be allowed to supervise 6 physician assistants in a correctional facility.
If allowed by the supervising physician, they may write medical orders and can order medications including schedule II–V controlled substances in both inpatient and outpatient settings. Additionally, they may apply for a US Drug Enforcement Administration license on their own. However, their prescribing is regulated as per Article 33 of the Public Health Law and Part 80 and 94.2 of Title 10 regulations.5 Their prescription forms must have the name of the supervising physician printed along with the physician assistant’s name. They are prohibited from performing allied health specialty tasks such as radiologic technology or optometry. Physician assistants share responsibility and liability with the supervising physician and may be named in a malpractice suit.
Application: Physician assistants are required to submit form 1 of the NYSED application with a fee of $115 to be registered to practice in NYS.
Nurse Practitioners
In NYS, a nurse practitioner (NP) is a registered professional nurse who has completed advanced nursing education (usually a master’s or doctorate degree) in a NP specialty area and is certified by the NYSED as an NP. NYSED certifies NPs to practice in the following specialty areas: adult health, family health, gerontology, neonatology, obstetrics, oncology, pediatrics and perinatology, psychiatry, school health, women’s health, holistic care, and palliative care.
Number of licensed professionals: There are a total of 31,663 all-specialty NPs and 2,876 psychiatric NPs in NYS.
Educational and licensing requirements: To be certified and registered as an NP in NYS, the provider must be registered and licensed as a registered nurse in NYS. They also must have graduated from an NP education program accepted by the NYSED or certified as an NP by a national certification organization or an organization accepted by the NYSED (eg, American Academy of Nurse Practitioner Certification Board, American Association of Critical Care Nurses, American Nurses Credentialing Center, National Board for Certification of Hospice and Palliative Nurses) or licensed and certified as an NP by another state or jurisdiction and met the substantial equivalent of NYS requirements. They must provide acceptable evidence that they have completed pharmacology coursework.
The requirements for pharmacology certification include completion of at least 3 semester hours of pharmacology coursework or an educational program or combination of courses, which can be an equivalent; passed an examination in pharmacotherapeutics; or passed a nationally recognized examination acceptable for licensure as an NP.
NP certification in NYS is valid for life unless revoked, annulled, or suspended. The NP registration certificate authorizes practice for 3 years and must be renewed along with the registered nurse registration to continue practicing. The laws governing NP certification include Education Law 6910 and 8 NYCRR Part 64.
Scope of practice: NYS education law does not require physicians to supervise NPs, and they can function independently. They are, however, expected to practice in collaboration with a physician unless they have a collaborative relationship as allowed by the Nurse Practitioner Modernization Act. This Act states that NPs with more than 3,600 hours of practice experience may opt to practice and have collaborative relationships with 1 or more qualified physicians or a NYS health department licensed facility.
A collaborative relationship is when an NP communicates in some form with a physician to collaborate care with a patient. If an NP enters into a written practice agreement, the supervising physician may not supervise more than 4 NPs who are colocated with them. This form of collaboration is contractual, while those NPs who qualify under the new law are not required to have a contractual relationship. In the contractual form, the physician must review the NP’s charts once every 3 months.
NPs can diagnose and treat all conditions under the purview of their specialty. They can prescribe controlled substances under schedule II–IV for patients within their specialty area. As per federal laws, NPs are prohibited from prescribing buprenorphine and naloxone.
DISCUSSION
The demand for psychiatric services has been steadily increasing, and it is believed that the need shall exceed the availability of psychiatrists by 12% to 25% in 2025.6 The American Psychiatric Nurses Association projected a deficiency of 250,000 mental health professionals by 2025 due to aging of the workforce, high retirement, and a deficiency of residency slots to fill the gaps.7 However, these gaps may be met by midlevel providers. These health care workers increase the availability of providers to the population, thereby shortening wait times, reducing caseloads for psychiatrists, and ensuring a more efficient health care system.
However, we also need to consider the need for appropriate training and supervision of these midlevel providers. House physicians and physician assistants require supervision by a physician, and NYS limits the number that a physician can supervise, thus ensuring an adequate level of care. The practice of psychiatry requires in-depth knowledge of the human psyche, impeccable interviewing skills, and a thorough knowledge of psychopharmacology.
Midlevel providers are crucial to the provision of mental health services given the gross deficiency in availability of psychiatrists. A 3-pronged approach targeting the following may be a model to be researched to improve the quality and availability of mental health care:
- Increase positions in psychiatric residency programs to bridge the gaps.
- Ensure appropriate interview skills and psychopharmacology training for physician assistants, NPs, and other providers.
- Establish a graded increase in autonomy to midlevel providers based on achievement of certain proficiencies to foster learning and improve patient care.
CONCLUSION
The gaps in the provision of mental health care are slowly increasing, and we need to find innovative solutions to address these needs. Midlevel providers may be the solution to address the gaps in care. However, we also need to ensure availability of adequate training and a collaborative specialist to ensure improved quality of care and patient safety.
Submitted: March 2, 2022; accepted May 18, 2022.
Published online: December 6, 2022.
Relevant financial relationships: None.
Funding/support: None.
Clinical Points
- There is a deficit in the number of mental health providers who can prescribe medications in the United States.
- New York State has successfully attempted to bridge the gaps in the provision of mental health care by employing midlevel providers such as physician assistants, nurse practitioners, and house physicians.
- Midlevel providers working under supervision can help improve the provision of care to patients with mental illness.
References (7)

- SAMHSA. 2020 National Survey on Drug Use and Health. NIH website. Accessed October 15, 2022. https://www.nimh.nih.gov/health/statistics/mental-illness
- University of Michigan Behavioral Health Workforce Research Center. Estimating the Distribution of the U.S. Psychiatric Subspecialist Workforce. University of Michigan Behavioral Health Workforce Research Center website. Accessed October 15, 2022. https://www.behavioralhealthworkforce.org/wp-content/uploads/2019/02/Y3-FA2-P2-Psych-Sub_Full-Report-FINAL2.19.2019.pdf
- HRSA. State-Level Projections of Supply and Demand for Behavioral Health Occupations: 2016–2030. HRSA.gov website. Accessed October 15, 2022. https://bhw.hrsa.gov/sites/default/files/bureau-health-workforce/data-research/state-level-estimates-report-2018.pdf
- Office of the Professions. New York State. NYSED.gov website. Accessed October 15, 2022. http://www.op.nysed.gov/prof/med/rpa.htm
- NY Dept of Health. Part 80: Rules and Regulations on Controlled Substances in NYS. NY.gov website. Accessed October 15, 2022. https://www.health.ny.gov/regulations/controlled_substance/part/80/docs/80.pdf
- National Council for Mental Well Being. The Psychiatric Shortage: Causes and Solutions. Accessed October 15, 2022. https://www.thenationalcouncil.org/resources/psychiatric-shortage-causes-and-solutions/
- APNA. Expanding Mental Health Care Services in America: The Pivotal Role of Psychiatric Mental Health Nurses. APNA.org website. Accessed October 15, 2022. https://www.apna.org/wp-content/uploads/2021/03/Expanding_Mental_Health_Care_Services_in_America-The_Pivotal_Role_of_Psychiatric-Mental_Health_Nurses_04_19.pdf
Enjoy this premium PDF as part of your membership benefits!