Because many patients with bipolar disorder seek treatment in primary care practices, physicians in these settings need to be able to diagnose bipolar disorder and common psychiatric and medical comorbidities and to initiate and manage treatment. Unfortunately, bipolar disorder is often underrecognized. The most common symptoms in patients with bipolar disorder are depressive, but these patients may also have anxiety, mood swings, sleep problems, irritability, difficulty concentrating, relationship issues, alcohol- or drug-related problems, and infections. Social and family history and screening tools can help clarify diagnosis. The goal of treatment should be recovery, but periodic relapse and medication nonadherence should be expected. Primary care physicians should decide what level of intervention their practices can support. To manage these patients effectively, practices may need to train office staff, set up monitoring and follow-up systems, establish links with referral and community support services, develop therapeutic alliances with patients, and provide psychoeducation for patients and significant others. Receiving comprehensive psychiatric and medical care and support can be life-changing for patients with bipolar disorder and their families.
The Role of Primary Care Clinicians in
Diagnosing and Treating Bipolar Disorder
From the Department of Family Medicine, Boston University School of Medicine and Boston Medical Center, Boston, Massachusetts.
This article is derived from the planning teleconference series “Improving the Recognition and Treatment of Bipolar Disorder in Primary Care,” which was held in September 2009 and supported by an educational grant from AstraZeneca.
Dr Culpepper is a member of the advisory boards for AstraZeneca, Eli Lilly, Merck, Pfizer, Sanofi, Takeda, and Wyeth and is a former member (resigned) of the Pfizer and Wyeth speakers bureaus.
Corresponding author: Larry Culpepper, MD, MPH, 1 Boston Medical Center Place, Dowling 5, Boston, MA 02118
([email protected]).
doi:10.4088/PCC.9064su1c.01
© Copyright 2010 Physicians Postgraduate Press, Inc.
Because many patients with bipolar disorder seek treatment in primary care practices, physicians in these settings need to be able to diagnose bipolar disorder and common psychiatric and medical comorbidities and to initiate and manage treatment. Unfortunately, bipolar disorder is often underrecognized. The most common symptoms in patients with bipolar disorder are depressive, but these patients may also have anxiety, mood swings, sleep problems, irritability, difficulty concentrating, relationship issues, alcohol- or drug-related problems, and infections. Social and family history and screening tools can help clarify diagnosis. The goal of treatment should be recovery, but periodic relapse and medication nonadherence should be expected. Primary care physicians should decide what level of intervention their practices can support. To manage these patients effectively, practices may need to train office staff, set up monitoring and follow-up systems, establish links with referral and community support services, develop therapeutic alliances with patients, and provide psychoeducation for patients and significant others. Receiving comprehensive psychiatric and medical care and support can be life-changing for patients with bipolar disorder and their families.
(Prim Care Companion J Clin Psychiatry 2010;12[suppl 1]:4–9)
The role of primary care clinicians in treating patients with mental health disorders has evolved such that primary care is a major source of mental health treatment.1 Although many patients with bipolar disorder are treated in primary care settings, delay in recognition of the disorder is common. Primary care physicians need to be able to
diagnose and treat bipolar disorder and common psychiatric and medical comorbidities, as well as provide regular follow-up, education, and support. This article describes steps that primary care physicians can take to provide comprehensive care for these patients.
Diagnosis of bipolar disorder
Only 39.1% of individuals with bipolar I or II disorder make treatment contact in the year of onset, and the median delay in making initial treatment contact is 6 years.2 Unfortunately, when patients finally seek treatment, bipolar disorder may be poorly recognized in primary care settings, as discussed by J. Sloan Manning, MD, in the article “Tools to Improve Differential Diagnosis of Bipolar Disorder in Primary Care” in this supplement.3 Despite its underrecognition, bipolar disorder is common among patients in primary care offices. In a naturalistic prospective evaluation of 108 consecutive patients with symptoms of anxiety or depression in a family practice setting, 25.9% were diagnosed with bipolar spectrum disorders.4
Symptoms of Bipolar Disorder
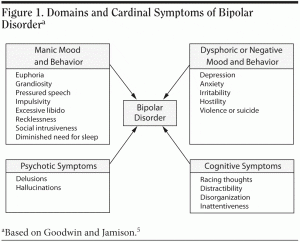
Over time, patients with bipolar disorder display a range of symptoms that can be separated into 4 major domains: manic mood and behavior, dysphoric or negative mood and behavior, psychotic symptoms, and cognitive symptoms (Figure 1).5 The most commonly experienced symptoms are depressive. In a prospective study6 of 146 patients with bipolar I disorder, depressive symptoms occurred in 31.9% of total follow-up weeks, compared with 8.9% of weeks for manic/hypomanic symptoms and 5.9% of weeks for cycling or mixed symptoms. Similarly, in a prospective study7 of 86 patients with bipolar II disorder, depressive symptoms occurred in 50.3% of follow-up weeks, hypomanic symptoms in 1.3% of weeks, and cycling or mixed symptoms in 2.3% of weeks. However, bipolar disorder is not only a disorder of mood and behavioral alterations but also of cognitive impairment. In 146 euthymic outpatients with unipolar and bipolar disorders, a higher number of prior mood episodes was associated with increased cognitive impairment.8 Some patients also display psychotic symptoms.
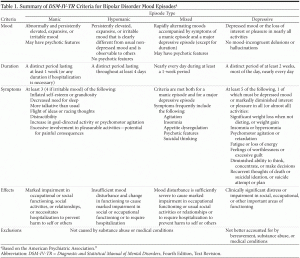
The Diagnostic and Statistical Manual of Mental Disorders, Fourth Edition, Text Revision (DSM-IV-TR)9 classification of mood disorders includes bipolar I disorder, bipolar II disorder, and bipolar disorder not otherwise specified. The DSM-IV-TR characteristics of manic, depressed, and mixed episodes are summarized in Table 1.9 Manic states range from hypomania to full mania, including psychotic mania. While hypomania may be associated with increased creativity and work ability, full mania is often associated with severe functional impairment. Patients with either bipolar I or bipolar II disorder may also have episodes in which manic and depressive symptoms are mixed. At these times, patients feel depressed and hopeless but also have significant energy, impulsivity, and irritability. Mixed episodes are particularly dangerous for patients because intense dysphoria accompanied by high energy and decreased sleep can place them at high risk for suicide. Alcohol use further increases suicide risk.
Common Comorbid Conditions
In patients with bipolar disorder, comorbidity is the rule rather than the exception. In a study10 based on US general population survey data, Kessler and colleagues found that 100.0% of patients with bipolar I disorder reported at least 1 other psychiatric disorder in their lifetimes, and 95.5% reported 3 or more. Anxiety disorders were present in 92.9% of patients with bipolar I disorder, substance use disorders in 71.0%, conduct disorders in 59.4%, and adult antisocial behaviors in 29.0%. Common medical comorbidities include migraine,11 thyroid disease,12 overweight and obesity,13 diabetes, cardiovascular diseases and hypertension, chronic obstructive pulmonary disease and asthma, human immunodeficiency virus, and hepatitis C.14 Comorbidities are discussed in more detail by Terence E. Ketter, MD, in the article “Strategies For Monitoring Outcomes in Patients With Bipolar Disorder”15 in this supplement.
Course of Bipolar Disorder
Bipolar disorder is recurrent, typically has an age at
onset of about 20 years, and may be expressed differently in number and type of mood episodes according to age and gender. Although symptoms are reduced during the euthymic periods between episodes, residual mood symptoms and interpersonal and occupational difficulties may remain.16 Difficulties include cognitive impairment,8 mood instability,16 and living with the social consequences of the illness.17
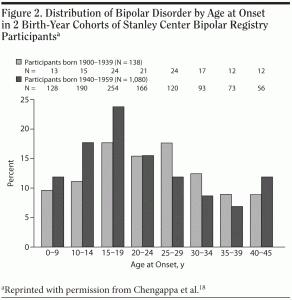
Age at onset appears to be decreasing, with the current median age at onset likely to be during the teenage years (Figure 2).18 In youth, manic and mixed states are more common, but, in adulthood, depression becomes more predominant.19 New-onset bipolar disorder is unusual in the elderly, so suspicion of this diagnosis in older patients should stimulate an investigation for another primary central nervous system disorder.20 However, people with bipolar disorder continue to experience difficulty late in life.21
While some controversy exists in the literature, men may be more likely to experience a manic first episode, while women may be slightly more likely to experience initial depressive episodes.9 Women may also have more frequent mixed episodes and rapid cycling episodes.22
In women, no predictable association between menses and specific mood states has been found,22–24 although slightly more women with bipolar disorder than controls have reported bothersome mood shifts both during and before menses (74% vs 64%).23 Menopause, however, is a high-risk time for worsening of bipolar illness.24
Presentation in Primary Care Practice
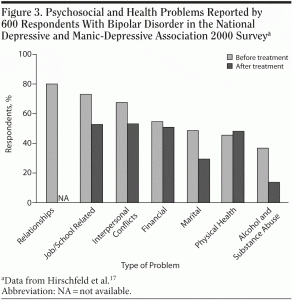
Patients with bipolar disorder present in the primary
care setting with a wide range of symptoms, including depression, anxiety, mood swings, difficulty sleeping, irritability, fatigue, and inability to focus and concentrate.25–28 They also may exhibit physical consequences of their illness, such as alcohol-related problems or sexually transmitted or drug-related infections. Patients’ social histories often uncover other sequelae of the illness, including relationship and marital problems, financial trouble, erratic occupational histories, and legal issues (Figure 3).17,25
Patients with bipolar illness often have family histories of mood disorders.27 Suspicion should be aroused regarding the true condition of absent relatives such as an uncle in prison or a grandparent who died at an early age. These personal and family history warning signs, particularly in patients who have been diagnosed with major depression, should suggest that bipolar disorder may be the correct diagnosis.29 As discussed by Dr Manning in this supplement,3 the Mood Disorder Questionnaire is a screening instrument that may aid recognition of bipolar disorder.
Treatment of bipolar disorder
After patients have screened positive for and been diagnosed with bipolar disorder, clinicians need to initiate treatment. To successfully manage treatment for patients with bipolar disorder in primary care, several steps can be taken, as discussed by Jeffrey L. Susman, MD, in the article “Improving Outcomes in Patients With Bipolar Disorder Through Establishing an Effective Treatment Team” in this supplement.30 Preparing the practice to manage both the psychiatric and medical health care of patients with bipolar disorder and providing education and support to patients and their families over the long-term can optimize the quality of care and avoid crises.
Preparing the Practice to Provide Comprehensive Care
Most primary care settings assume at least a modest role in the long-term care of patients with bipolar disorder. Although primary care physicians can often work with psychiatric colleagues in the long-term monitoring of treatment, some communities have no realistic options for psychiatric treatment. Physicians should determine the level of intervention that the practice can support.
To prepare a primary care practice to treat patients with bipolar disorder, partners in the practice should agree about the role the practice will play in managing these patients. Educating nursing and front office staff in how to manage patients who are disruptive may be necessary. To facilitate follow-up, which is crucial with chronic illnesses such as bipolar disorder, a registry to support monitoring and recall can be created. Establishing ties with a network of psychiatric referral and community support services, including services for management when disruptive manic behavior or suicidality is involved, can help deal with severe cases or crises. Agreement on management responses, before a crisis actually occurs, can be very helpful. Psychiatric consultation may be needed to provide diagnostic and pharmacologic expertise for management of complex cases, including those with comorbidities such as substance abuse or with treatment resistance. Ties to educational and support services for family members should also be established, and a compendium of helpful Web resources should be developed.
Providing Psychiatric Treatment and Education
If patients are a danger to themselves or others, immediate psychiatric referral is appropriate to stabilize patients in an environment safe for them and others. A short-term treatment plan, which might include options to involve medication and emergency and police services, should
be devised for the transition period from primary care to specialist care.
For patients who will not be referred and will be treated in primary care, short- and long-term treatment goals need to be established. The ultimate goal of treatment should be recovery. Effective management begins with successful acute treatment and, after achieving a durable remission, continues with a transition into maintenance treatment, as discussed by Andrew A. Nierenberg, MD, in the article “A Critical Appraisal of Treatments for Bipolar Disorder” in this supplement.31 Psychiatric care of patients with bipolar disorder involves monitoring treatment adequacy, treatment side effects, and adherence to medication.
Strategies can be adopted to manage treatment effectively. For example, in shared care between primary care and specialty care providers, physicians need to name the expectations of each party and clearly communicate these expectations to the patient. Open lines of communication between the primary care physician and consultants should be maintained. Additionally, using Health Insurance Portability and Accountability Act documentation can make management more effective.
Psychiatric care can also be enhanced and outcomes
optimized by establishing an effective therapeutic alliance with patients and their families or caregivers. Taking time to listen and communicating clearly and frankly are key elements in building a therapeutic alliance. In individuals who at the time are competent, the patient and clinician can share decision-making and should agree on the goals of treatment and how to achieve these goals.32 Discussing treatment options and possible side effects and their management can enhance treatment adherence, which can improve outcomes.33 Monitoring and managing symptoms can be enhanced if self-monitoring is encouraged and the patient is able to recognize symptoms of impending relapse.
Pharmacotherapy is effective only if patients take it, and patients with bipolar disorder often do not take their medication as prescribed. For example, in a 2-year study,34 about 40% of euthymic patients with bipolar disorder were nonadherent to medication to some extent. In a study by Keck and colleagues,35 among patients initially hospitalized for a manic or mixed episode, 51% were noncompliant to pharmacotherapy to some extent during 1 year of follow-up. Patients in this study gave many reasons for nonadherence to medication, but the most common was denial of need. Other factors associated with noncompliance have been found to include feeling bothered by having a chronic illness or that one’s mood is controlled by a medication, feeling depressed, and thinking that taking medication is a hassle.36 Dr Ketter discusses this topic in more detail elsewhere in this supplement.15
Strategies to detect nonadherence include monitoring
patients’ appointment-keeping patterns, regularly measuring depressive and manic symptoms, and measuring plasma drug levels; strategies to address nonadherence include treating troublesome side effects, having a frank discussion with the patient and family about their attitudes to medication and history of medication adherence, and educating the patient and family about the disorder and its treatment.33 Byrne et al37 indicated that establishing a collaborative dialogue about medication and involving the patient in the decision-making process is the most effective strategy to improve treatment adherence for patients with mood disorders.
Psychoeducation can prevent relapse by improving adherence to medication, influencing lifestyle, and assisting in the early detection of prodromal symptoms.38 Prodromal symptoms can occur weeks or months before full relapse, and early detection can lead to earlier and more effective treatment.39,40 A study41 of 20 patients with bipolar disorder found that 85% of patients were able to recognize a depressive prodrome and 75% could recognize a manic prodrome relative to a period of remission. Most patients could identify that they had retained insight during the prodromal periods and could identify idiosyncratic symptoms. Manic and depressive prodromes vary among patients, but depressive prodromes can include depressed mood, loss of energy, and difficulty concentrating, while manic prodromes can include increased activity, elevated mood, and decreased need for sleep.39
Several tools are available for use by patients and families to chart the status of bipolar symptoms; they include the Adjective Mood Scale, Kraepelin’s early life charts, the National Institute of Mental Health (NIMH) Life Chart Method, and the Social Rhythm Metric.42 A simplified version of the NIMH life chart, which may offer the best support for clinical decisions, can be found at the Depression and Bipolar Support Alliance Web site, http://www.dbsalliance.org/pdfs/calendarforweb.pdf.
Providing Medical Treatment
The role of the primary care physician includes attending to the medical needs of patients with bipolar disorder in addition to managing the psychiatric disorder and psychiatric comorbidities. Medical needs that may require treatment include medical comorbidities, medication side effects, and routine health care.
Patients with bipolar disorder appear to be at high risk for medical comorbidities and early death, particularly cardiovascular mortality. Additionally, many of the medications used in the chronic treatment of bipolar disorder can result in weight gain, lipid abnormalities, and other long-term side effects, as Dr Nierenberg describes in this supplement.31 Patients with bipolar disorder may also be at high risk for not obtaining routine preventive health care without prompting. Given the behavioral risks in this population, tailored preventive care tactics, such as hepatitis immunizations and long-term birth control methods, may be appropriate. Because sleep changes may trigger (or be the indicator of) a change in mood states, interventions to improve sleep may also be helpful in this population.
Providing Support
The primary care physician can provide families of
patients with bipolar disorder with considerable support. For both the patient and the family, the physician can help in anticipating and preparing for life transitions, which can be stressful even in those without psychiatric disease, such as going away to college, getting married, starting a family, or entering the job market. These are times during which the physician may need to increase monitoring of the patient’s mood state and help in developing new daily routines, such as those related to medication taking. At each visit, the physician should establish whether changes have occurred in occupation, social situation, family situation, or health.
Extra vigilance and support may also be needed if hospitalization of a medical or psychiatric nature occurs. Periodic psychiatric relapse is to be expected in most patients with bipolar disorder. The transition from the hospital back to a home setting may be a high-risk time for patients, especially if hospital-based and ambulatory treatment providers do not communicate and coordinate the transition. The primary care provider can play an important role in such coordination. Social support such as support for reentering employment or reassuming other responsibilities may be required along with stabilization of medication and other treatment regimens.
As with treating any chronic illness, working with patients to improve their adaptive and problem-solving skills and their self-management and self-monitoring skills should be a major priority. Making both the patient and family familiar with local and national support networks may also be helpful.
CONCLUSION
Primary care physicians can provide life-changing psychiatric and medical treatment and support to patients with bipolar disorder and their families. However, this requires considerable effort and expertise over the long-term. Primary care physicians who have prepared their practices to engage in comprehensive care can do so as part of their practice routine rather than through extraordinary effort in response to patient crises. A summary of steps to take to treat patients with bipolar disorder in primary care practices is shown in Table 2.

Disclosure of off-label usage: The author has determined that, to the best of his knowledge, no investigational information about pharmaceutical agents that is outside US Food and Drug Administration−approved
labeling has been presented in this activity.
References
1. Regier DA, Narrow WE, Rae DS, et al. The de facto US mental and
addictive disorders service system: Epidemiologic Catchment Area
prospective 1-year prevalence rates of disorders and services.
Arch Gen Psychiatry. 1993;50(2):85–94. PubMed
2. Wang PS, Berglund P, Olfson M, et al. Failure and delay in initial treatment contact after first onset of mental disorders in the National Comorbidity Survey Replication. Arch Gen Psychiatry. 2005;62(6):
603–613. doi:10.1001/archpsyc.62.6.603 PubMed
3. Manning JS. Tools to improve differential diagnosis of bipolar disorder in primary care. Prim Care Companion J Clin Psychiatry. 2010;12
(suppl 1):17–22.
4. Manning JS, Haykal RF, Connor PD, et al. On the nature of depressive and anxious states in a family practice setting: the high prevalence of
bipolar II and related disorders in a cohort followed longitudinally. Compr Psychiatry. 1997;38(2):102–108. doi:10.1016/S0010-440X(97)90089-4 PubMed
5. Goodwin FK, Jamison KR. Manic-Depressive Illness. New York, NY: Oxford University Press; 1990.
6. Judd LL, Akiskal HS, Schettler PJ, et al. The long-term natural history of the weekly symptomatic status of bipolar I disorder. Arch Gen Psychiatry. 2002;59(6):530–537. doi:10.1001/archpsyc.59.6.530 PubMed
7. Judd LL, Akiskal HS, Schettler PJ, et al. A prospective investigation of the natural history of the long-term weekly symptomatic status of bipolar II disorder. Arch Gen Psychiatry. 2003;60(3):261–269. doi:10.1001/archpsyc.60.3.261 PubMed
8. Kessing LV. Cognitive impairment in the euthymic phase of affective disorder. Psychol Med. 1998;28(5):1027–1038. doi:10.1017/S0033291798006862 PubMed
9. American Psychiatric Association. Diagnostic and Statistical Manual of Mental Disorders, Fourth Edition, Text Revision. Washington, DC: American Psychiatric Association; 2000.
10. Kessler RC, Rubinow DR, Holmes C, et al. The epidemiology of
DSM-III-R bipolar I disorder in a general population survey.
Psychol Med. 1997;27(5):1079–1089. doi:10.1017/S0033291797005333 PubMed
11. Breslau N, Merikangas K, Bowden CL. Comorbidity of migraine and major affective disorders. Neurology. 1994;44(suppl 7):S17–S22. PubMed
12. Kupka RW, Nolen WA, Post RM, et al. High rate of autoimmune thyroiditis in bipolar disorder: lack of association with lithium exposure. Biol Psychiatry. 2002;51(4):305–311. doi:10.1016/S0006-3223(01)01217-3 PubMed
13. McElroy SL, Frye MA, Suppes T, et al. Correlates of overweight and obesity in 644 patients with bipolar disorder. J Clin Psychiatry. 2002;63(3):207–213. PubMed
14. Beyer J, Kuchibhatla M, Gersing K, et al. Medical comorbidity in a bipolar outpatient clinical population. Neuropsychopharmacology. 2005;30(2):401–404. doi:10.1038/sj.npp.1300608 PubMed
15. Ketter TE. Strategies for monitoring outcomes in patients with
bipolar disorder. Prim Care Companion J Clin Psychiatry. 2010;12
(suppl 1):10–16.
16. Benazzi F. Inter-episode mood lability in mood disorders: residual symptom or natural course of illness? Psychiatry Clin Neurosci. 2004;58(5):480–486. doi:10.1111/j.1440-1819.2004.01289.x PubMed
17. Hirschfeld RM, Lewis L, Vornik LA. Perceptions and impact of bipolar disorder: how far have we really come? results of the National Depressive and Manic-Depressive Association 2000 survey of individuals with
bipolar disorder. J Clin Psychiatry. 2003;64(2):161–174. PubMed
18. Chengappa KN, Kupfer DJ, Frank E, et al. Relationship of birth cohort and early age at onset of illness in a bipolar disorder case registry.
Am J Psychiatry. 2003;160(9):1636–1642. doi:10.1176/appi.ajp.160.9.1636 PubMed
19. Coryell W, Fiedorowicz J, Solomon D, et al. Age transitions in the course of bipolar I disorder. Psychol Med. 2009;39(8):1247–1252. doi:10.1017/S0033291709005534 PubMed
20. Hirschfeld MA, Bowden CL, Gitlin MJ, et al, for the Work Group on Bipolar Disorder. Practice Guideline for the Treatment of Patients With Bipolar Disorder, Second Edition. Washington, DC: American Psychiatric Association; 2002. http://www.psychiatryonline.com/pracGuide/pracGuideTopic_8 aspx. Accessed March 15, 2010.
21. Sajatovic M. Aging-related issues in bipolar disorder: a health services perspective. J Geriatr Psychiatry Neurol. 2002;15(3):128–133. PubMed
22. Leibenluft E. Women with bipolar illness: clinical and research issues. Am J Psychiatry. 1996;153(2):163–173. PubMed
23. Diamond SB, Rubinstein AA, Dunner DL, et al. Menstrual problems in women with primary affective illness. Compr Psychiatry. 1976;17(4):
541–548. doi:10.1016/0010-440X(76)90036-5 PubMed
24. Blehar MC, DePaulo JR Jr, Gershon ES, et al. Women with bipolar disorder: findings from the NIMH Genetics Initiative sample. Psychopharmacol Bull. 1998;34(3):239–243. PubMed
25. Piver A, Yatham LN, Lam RW. Bipolar spectrum disorders: new
perspectives. Can Fam Physician. 2002;48(5):896–904. PubMed
26. Manning JS, Haykal RF, Akiskal HS. The role of bipolarity in depression in the family practice setting. Psychiatr Clin North Am. 1999;22(3):
689–703. doi:10.1016/S0193-953X(05)70103-9 PubMed
27. Manning JS. Bipolar disorder in primary care. J Fam Pract. 2003;Mar(suppl):S6–S9.
28. Schuyler D. Depression comes in many disguises to the providers of primary care: recognition and management. J S C Med Assoc. 2000;96(6):267–275. PubMed
29. Akiskal HS. Searching for behavioral indicators of bipolar II in patients presenting with major depressive episodes: the “red sign,” the “rule of three” and other biographic signs of temperamental extravagance, activation and hypomania. J Affect Disord. 2005;84(2–3):279–290. doi:10.1016/j.jad.2004.06.002 PubMed
30. Susman JL. Improving outcomes in patients with bipolar disorder through establishing an effective treatment team. Prim Care Companion J Clin Psychiatry. 2010;12(suppl 1):30–34.
31. Nierenberg AA. A critical appraisal of treatments for bipolar disorder. Prim Care Companion J Clin Psychiatry. 2010;12(suppl 1):23–29.
32. Klein DN, Schwartz JE, Santiago NJ, et al. Therapeutic alliance in depression treatment: controlling for prior change and patient characteristics.
J Consult Clin Psychol. 2003;71(6):997–1006. doi:10.1037/0022-006X.71.6.997 PubMed
33. Colom F, Vieta E. Non-adherence in psychiatric disorders: misbehaviour or clinical feature? Acta Psychiatr Scand. 2002;105(3):161–163. doi:10.1034/j.1600-0447.2002.1e003.x PubMed
34. Colom F, Vieta E, Martínez-Arán A, et al. Clinical factors associated with treatment noncompliance in euthymic bipolar patients. J Clin Psychiatry. 2000;61(8):549–555. PubMed
35. Keck PE Jr, McElroy SL, Strakowski SM, et al. Compliance with maintenance treatment in bipolar disorder. Psychopharmacol Bull. 1997;33(1):87–91. PubMed
36. Pope M, Scott J. Do clinicians understand why individuals stop taking lithium? J Affect Disord. 2003;74(3):287–291. doi:10.1016/S0165-0327(02)00341-5 PubMed
37. Byrne N, Regan C, Livingston G. Adherence to treatment in mood
disorders. Curr Opin Psychiatry. 2006;19(1):44–49. doi:10.1097/01.yco.0000191501.54034.7c PubMed
38. Colom F, Vieta E, Reinares M, et al. Psychoeducation efficacy in bipolar disorders: beyond compliance enhancement. J Clin Psychiatry. 2003;64(9):1101–1105. PubMed
39. Fava GA, Kellner R. Prodromal symptoms in affective disorders.
Am J Psychiatry. 1991;148(7):823–830. PubMed
40. Swann AC. Long-term treatment in bipolar disorder. J Clin Psychiatry. 2005;66(suppl 1):7–12. PubMed
41. Smith JA, Tarrier N. Prodromal symptoms in manic depressive psychosis. Soc Psychiatry Psychiatr Epidemiol. 1992;27(5):245–248. doi:10.1007/BF00788937 PubMed
42. Hörn M, Schärer L, Walser S, et al. Comparison of long-term monitoring methods for bipolar affective disorder. Neuropsychobiology. 2002;45
(suppl 1):27–32. doi:10.1159/000049258 PubMed
Enjoy this premium PDF as part of your membership benefits!

