Prim Care Companion CNS Disord 2022;24(6):22cr03237
To cite: Ratcliff K, Juneja V, Gupta A, et al. Clozapine rechallenge with recurrent pancreatitis. Prim Care Companion CNS Disord. 2022;24(6):22cr03237.
To share: https://doi.org/10.4088/PCC.22cr03237
© 2022 Physicians Postgraduate Press, Inc.
aDepartment of Psychiatry, Flinders University, College of Medicine and Public Health, South Australia, Australia
bDepartment of Psychiatry, Monash University, Faculty of Medicine, Nursing and Health Sciences, Victoria, Australia
*Corresponding author: Kyle Ratcliff, MD, Flinders Medical Centre, Flinders Drive, Bedford Park, SA, Australia 5042 ([email protected]).
Clozapine is the gold standard for treatment-resistant schizophrenia. Clozapine is thought to trigger an inflammatory response mediated through proinflammatory cytokines interleukins 1–6 and tumor necrosis factor α, often leading to fever and elevated C-reactive protein (CRP). This effect is most pronounced in the first month after clozapine initiation.1
This clozapine-induced inflammatory response is potentially related to benign hyperthermia, myocarditis, and agranulocytosis. Clozapine is also strongly associated with the risk of pneumonia, which is more severe during titration with accompanying high mortality.2 The mechanism of clozapine increasing the risk of pneumonia is likely multifactorial, related to a combination of reducing the defensive mechanisms against infection and aspiration.3 Eight clozapine-induced pancreatitis cases are documented, with only 2 reported cases of successful clozapine rechallenge.4–6 We present a unique case of concurrent pneumonia and pancreatitis following clozapine initiation and recurrence of pancreatitis upon rechallenge.
Case Report
Mr A was a 34-year-old White man diagnosed with schizophrenia at age 18 years. He had an initial trial of clozapine by age 28 years due to treatment-resistant schizophrenia. At clozapine commencement, he had no other medical comorbidities but was mildly overweight and was smoking 40 cigarettes daily. On the third week of clozapine titration (dose of 175 mg), he presented with fever (38.2°C), a productive cough, rhinorrhea, dyspnea, pleurisy, and tachycardia. There was no documentation in the clinical case notes of hypersalivation or sedation to suggest aspiration pneumonia. Elevated inflammatory markers (CRP: 83 mg/L [normal: < 10 mg/L], white cell count [WCC]: 15.9×109/L [normal: 4.0–11.0×109/L], and neutrophilia: 13.2×109/L [normal: 1.5–8.0×109/L] but normal eosinophils [normal: 0.04–0.4×109/L]) and consolidation located in the left-upper and right-middle lung lobes identified on chest computed tomography (CT) confirmed multilobar pneumonia. He was admitted to the medical ward and received a course of intravenous cefazolin. His clozapine level was 130 mcg/L (nontoxic level), taken when he was being assessed for pneumonia. Myocarditis was excluded due to normal echocardiogram and serum troponin level results. Clozapine was only held for a single dose during this period. Mr A insisted on community-based care after he made an adequate clinical recovery from pneumonia with antibiotics despite his inflammatory markers (CRP: 140 mg/L and WCC: 21.2 x109/L) increasing. During outpatient follow-up, 4 days following discharge, his CRP and WCC increased to 160 mg/L and 21.3 x109/L, respectively, leading to hospital readmission. He was diagnosed with asymptomatic clozapine-induced pancreatitis with an elevated lipase of 1,084 U/L (normal: 0–160 U/L) and eosinophilia of 2.69×109/L (normal: 0.04–0.4 x109/L), concurrent with resolving pneumonia. Subsequently, immediate clozapine cessation led to normalizing inflammatory markers, including eosinophils, and his serum lipase improved to 163 U/L a week later.
Over the next 5 years, Mr A made an inadequate clinical recovery, accruing a significant burden of disability related to his schizophrenia and new-onset medical comorbidities (type 2 diabetes and hypercholesterolemia treated with metformin, sitagliptin, and rosuvastatin) despite trials of several antipsychotics. Due to Mr A’s treatment-resistant schizophrenia, a clozapine rechallenge was considered.
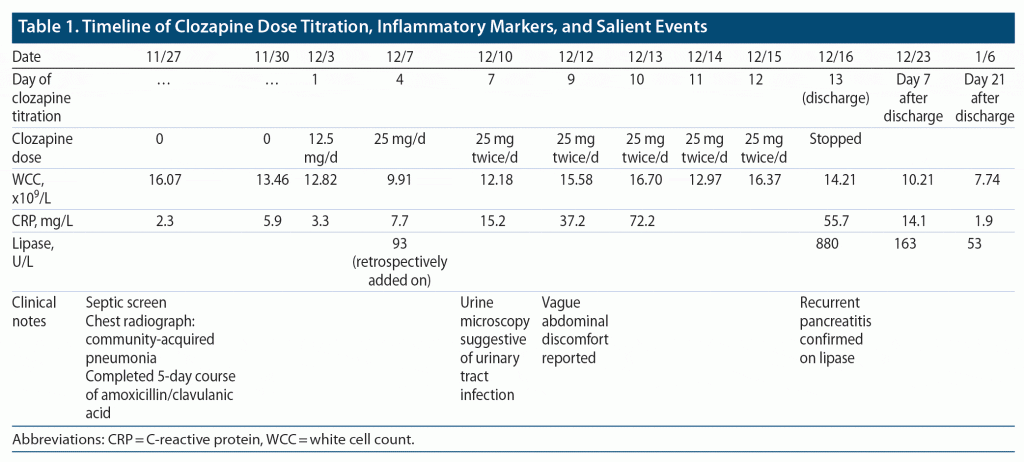
At admission, before the clozapine rechallenge, he was incidentally found to have a mildly elevated WCC of 16.6×109/L and CRP of 2.3 mg/L with no signs of infection. A chest x-ray demonstrated a subtle airspace opacity projected over the left sixth anterior rib, representing early infective consolidation. Mr A was empirically treated with amoxicillin/clavulanic acid for suspected pneumonia before clozapine rechallenge. Evidence suggests that rapid titration of clozapine increases the risk of clozapine-induced pancreatitis.7 Therefore, with a history of clozapine-induced pancreatitis and pneumonia, a conservative clozapine titration protocol was utilized, increasing clozapine slowly by 12.5 mg every 2 days, with frequent monitoring of inflammatory markers (Table 1).
On day 7 of the clozapine rechallenge, Mr A’s CRP increased to 15.2 mg/L, triggering a full septic screen. Urine microscopy revealed elevated white (12×106/L) and red (18×106/L) (normal: < 10) cells suggestive of urinary tract infection, which was treated with oral trimethoprim. However, his urine culture did not grow any organism, and repeat urinary microscopy did not show white cells. Despite the clozapine dose being maintained at 25 mg twice daily and no other focus of infection, his serum WCCs and CRP continued to increase to 16.7×109/L and 72.2 mg/L, respectively, with no elevated troponin or electrocardiogram evidence of myocarditis. Clozapine serum levels were not ordered, but in retrospect should have been done, as infection and pneumonia can be associated with elevated clozapine serum levels and clozapine intoxication.8
On day 9 of clozapine rechallenge (25 mg twice daily), he reported vague abdominal discomfort accompanied by mild post-prandial nausea. On examination, he had mild epigastric tenderness, and investigations demonstrated serum lipase of 800 U/L (normal: 0–160U/L) and eosinophilia of 2.6×109/L (normal: 0.4–0.4×109/L), which confirmed a recurrence of clozapine-induced pancreatitis. Clozapine was immediately stopped, leading to normalization of inflammatory markers and his pancreatitis-related symptoms (see Table 1 for details).
Discussion
This case of recurrent clozapine-induced pancreatitis supports the potentially systemic nature of the clozapine-induced inflammatory response. Moreover, clozapine-induced pancreatitis recurrence at a lower clozapine dose, accompanying eosinophilia, faster symptom onset, and increased symptom severity upon clozapine rechallenge, indicates a possible clozapine-related immune-sensitization effect. Clozapine-induced pancreatitis mediated by this potential immune sensitization mechanism can be potentially life threatening, and rechallenge in most cases (except in only 2 reported rechallenge cases) has been unsuccessful. The specific mechanism of clozapine immune-mediated changes leading to systemic inflammatory reactions such as benign hyperthermia, myocarditis, or pancreatitis requires further research. Clinicians need to be particularly vigilant for recurrent inflammatory reactions upon clozapine rechallenge following initial clozapine-related inflammatory response (eg, pancreatitis), which may be more severe than occurred during the first episode following clozapine initiation, with increased risks likely associated with rapid clozapine titration.7
Published online: December 15, 2022.
Relevant financial relationships: None.
Funding/support: None.
Patient consent: Consent was obtained from the patient to publish the case report, and information has been deidentified to protect anonymity.
References (8)

- Røge R, Møller BK, Andersen CR, et al. Immunomodulatory effects of clozapine and their clinical implications: what have we learned so far? Schizophr Res. 2012;140(1-3):204–213. PubMed CrossRef
- de Leon J, Schoretsanitis G, Smith RL, et al. An international adult guideline for making clozapine titration safer by using six ancestry-based personalized dosing titrations, CRP, and clozapine levels. Pharmacopsychiatry. 202255(2):73–86. PubMed
- Schoretsanitis G, Ruan CJ, Rohde C, et al. An update on the complex relationship between clozapine and pneumonia. Expert Rev Clin Pharmacol. 2021;14(2):145–149. PubMed CrossRef
- Rodriguez V, Hanley K, Arias AJ, et al. Successful clozapine rechallenge following recurrent clozapine-associated pancreatitis: a case report. BMC Pharmacol Toxicol. 2020;21(1):35. PubMed CrossRef
- Chengappa KN, Pelucio M, Baker RW, et al. Recurrent pancreatitis on clozapine re-challenge. J Psychopharmacol. 1995;9(4):381–382. PubMed CrossRef
- Yildiz MI, Karacam Dogan M, Mutlu E, et al. All in one: clozapine-associated acute pancreatitis with multiple organ involvement. J Clin Psychopharmacol. 2021;41(2):214–216. PubMed CrossRef
- Ertuğrul A, Yağcıoğlu EA, Karakaşlı A, et al. Valproate, obesity and other causes of clozapine poor metabolism in the context of rapid titration may explain clozapine-induced myocarditis: a re-analysis of a Turkish case series. Rev Psiquiatr Salud Ment (Engl Ed). 2021. CrossRef
- Ruan CJ, Zhen XY, Ge XL, et al. Pneumonia can cause clozapine intoxication: a case report. Psychosomatics. 2017;58(6):652–656. PubMed CrossRef
Enjoy this premium PDF as part of your membership benefits!