Hospital Admission for Schizophrenia and Discharge Against Medical Advice in the United States
Objective: Hospital discharge against medical advice may leave a patient at risk for adverse health outcomes and/or readmission, yet little is known regarding its occurrence, especially among patients with mental illness. The objective of this study was to discern the prevalence of, and predictive factors for, being discharged against medical advice among hospitalized patients with a primary diagnosis of schizophrenia.
Method: The 2004 US Healthcare Cost and Utilization Project Nationwide Inpatient Sample was used to discern demographic predictors, length of stay, and costs for discharge against medical advice relative to discharge with medical approval. Inpatient discharges from US community hospitals for patients of all ages with The International Classification of Diseases, 9th Revision, Clinical Modification diagnostic codes 295.0-295.9 were included. Conditional logistic regression was used to discern factors predictive of discharge against medical advice, and least squares mean analysis was used to examine differences in length of stay and mean cost per day relative to discharge with medical approval. Least squares means were adjusted for age (continuous), sex, race, region, payer, hospital setting, and bed size.
Results: Within the study population, 1.6% of patients admitted for schizophrenia were discharged against medical advice (n = 3,382/210,722). Patients discharged against medical advice were significantly more likely to be younger (OR = 0.985, 95% CI, 0.982-0.987) and male (OR = 1.421, 95% CI, 1.321-1.529). Race was not a significant factor. Mean ± SE length of stay for discharge against medical advice was 5.0 ± 0.24 days, as compared to 8.7 ± 0.06 days for patients discharged with medical approval (P < .0001). Mean cost per day was significantly higher for discharge against medical advice ($1,886.02 ± 49.67 vs $1,565.79 ± 13.42, P < .0001).
Conclusions: Although the percentage of patients discharged against medical advice was small, the numeric magnitude on a nationwide basis was substantial. The adjusted mean length of stay for discharge against medical advice was significantly reduced, while cost per day was significantly higher. Discharge against medical advice represents a challenge to the provision of care for patients with schizophrenia and may contribute to increased use of primary and specialty outpatient services, rehospitalization rates, morbidity, and mortality.
Prim Care Companion J Clin Psychiatry 2010;12(2):e1-e6
© Copyright 2010 Physicians Postgraduate Press, Inc.
Submitted: April 15, 2009; accepted May 13, 2009.
Published online: March 11, 2010 (doi:10.4088/PCC.09m00827yel).
Corresponding author: David A. Sclar, BPharm, PhD, Pharmacoeconomics and Pharmacoepidemiology Research Unit, Department of Health Policy and Administration, Washington State University, PO Box 646510, Pullman, WA 99164-6510 ([email protected]).
In the United States, the average hospital length of stay has declined significantly over the past 2 decades.1,2 Discharge from hospital against medical advice, or self-discharge, from US acute care and teaching hospitals has been reported to range from 0.8%-2.2%,3-7 with a commonly cited estimate of approximately 1%.8-11 Discharge against medical advice is reported to be associated with a reduction in the continuity of care and an increase in use of primary and specialty outpatient services, morbidity, risk for hospital readmission, and mortality2,3,6,9,11,12; yet, little is known regarding those factors predictive of discharge against medical advice.
Schizophrenia is a psychotic disorder that can impair all aspects of a patient’s life and carries a high risk of suicide and other life-threatening conditions.13-15 Approximately 10% of patients with schizophrenia will die by suicide,16 and a discharge against medical advice is positively correlated with detrimental health outcomes.17,18 The objectives of this study were (1) to discern the prevalence of, and predictive factors for, discharge against medical advice among US patients hospitalized in acute care hospitals with a primary diagnosis of schizophrenia and (2) to contrast hospital length of stay and cost per hospital day for patients discharged against medical advice with that of patients discharged with medical approval in total and by primary payer.
METHOD
Data Source
Clinical Points
- Discharge from hospital against medical advice is positively correlated with detrimental health outcomes.
- Patients with schizophrenia who are discharged against medical advice are more likely to be young and male.
- Discharge against medical advice represents a challenge to the provision of care for patients with schizophrenia due to tension between patients’ rights and psychiatrists’ duties.
The 2004 Healthcare Cost and Utilization Project (HCUP) Nationwide Inpatient Sample (NIS) was the database used for this analysis.19 The NIS is the largest all-payer inpatient care database that is publicly available in the United States and contains charge information on all patients regardless of payer, including persons covered by Medicare, Medicaid, private insurance, and the uninsured, as well as clinical and resource use information typically available from discharge abstracts. This database is maintained by the US Public Health Service’s Agency for Health Care Research and Quality.
The NIS is designed to approximate a 20% sample of US community hospitals defined by the American Hospital Association as “all nonfederal short-term, general and other specialty hospitals, excluding hospital units of institutions.”19 Included among community hospitals are specialty hospitals such as obstetrics and gynecology; ear, nose, and throat; orthopedic; and pediatric institutions. Also included are public hospitals and academic medical centers. Excluded are short-term rehabilitation hospitals, long-term hospitals, psychiatric hospitals, and alcoholism/chemical dependency treatment facilities.
The universe of US community hospitals is divided into strata using 5 hospital characteristics: hospital ownership/control, bed size, teaching status, rural/urban location, and US region. The NIS is a stratified probability sample of hospitals in the frame, with sampling probabilities proportional to the number of US community hospitals in each stratum. The sample for the 2004 NIS was drawn from 1,004 hospitals within the 36 participating HCUP partner states resulting in 8,004,571 patient discharges and 38,661,786 weighted discharges. To facilitate the production of national estimates, both hospital and discharge weights are provided.19
Data contained in each discharge pertinent to this study included patient demographics; expected source of primary payment; diagnostic profiles based on The International Classification of Diseases, 9th Revision, Clinical Modification (ICD-9-CM) coding20; and measures of resource use, including hospital length of stay, total charges, and discharge status. Hospital characteristics were obtained from the American Hospital Association Annual Survey of Hospitals and were merged with each discharge.21
Study Population
The study population was selected from all 2004 patient discharges. Study entry criteria were as follows: (1) patients of all ages; (2) an ICD-9-CM diagnostic code of 295.0-295.9 indicating schizophrenia as the primary diagnosis; (3) Medicare, Medicaid, or private insurance, inclusive of fee for service or managed care, identified as the primary source of insurance coverage; and (4) hospitalization of between 1 and 30 days. A cut off of 30 days hospital length of stay was selected so that the sample would be more representative of patients with episodic admissions, rather than those permanently or near continuously hospitalized with this condition. Ninety-three percent of discharges for schizophrenia were found to have a hospital length of stay of between 1 and 30 days. Having applied the above entry criteria, the final sample used for this analysis consisted of 43,733 discharges. After applying sampling weights provided by HCUP to make the sample representative of the US population, the final sample represented 210,722 discharges. The unit of analysis is the hospital stay.
Statistical Analysis
Statistical analyses were conducted using SAS, version 9.1.3.22 Descriptive statistics were used to characterize the study sample in total and by discharge status: those discharged against medical advice as compared to those discharged with medical approval.
Odds ratios (ORs) and 95% confidence intervals (CIs) were generated by conditional logistic regression (using the SAS procedure PROC Logistic) to discern the influence of patient’s age (continuous), race (white as compared to nonwhite, inclusive of Hispanics), sex, and primary payer type (Medicare, Medicaid, private insurance) on being discharged against medical advice. Models were also run separately by primary payer.
Using the SAS procedures PROC GLM and PROC SURVEYREG, least squares mean analyses were used to examine the dependent variables hospital length of stay and charge per day by discharge status. Least squares means were adjusted for age (continuous), sex, race, region of country (Northeast, Midwest, South, West), primary payer, hospital setting (rural, urban nonteaching, urban teaching), and hospital bed size (small, medium, large). Models were also run separately by primary payer.
The variable mean charge per day was computed as the ratio of total charges to length of stay. In this data set, total charges refer to the hospital bill (ie, charges) and generally do not include the amount billed for physician services or discounts negotiated by specific payers. These charges do not necessarily represent the amount reimbursed to the hospital and are not synonymous with costs.19
RESULTS
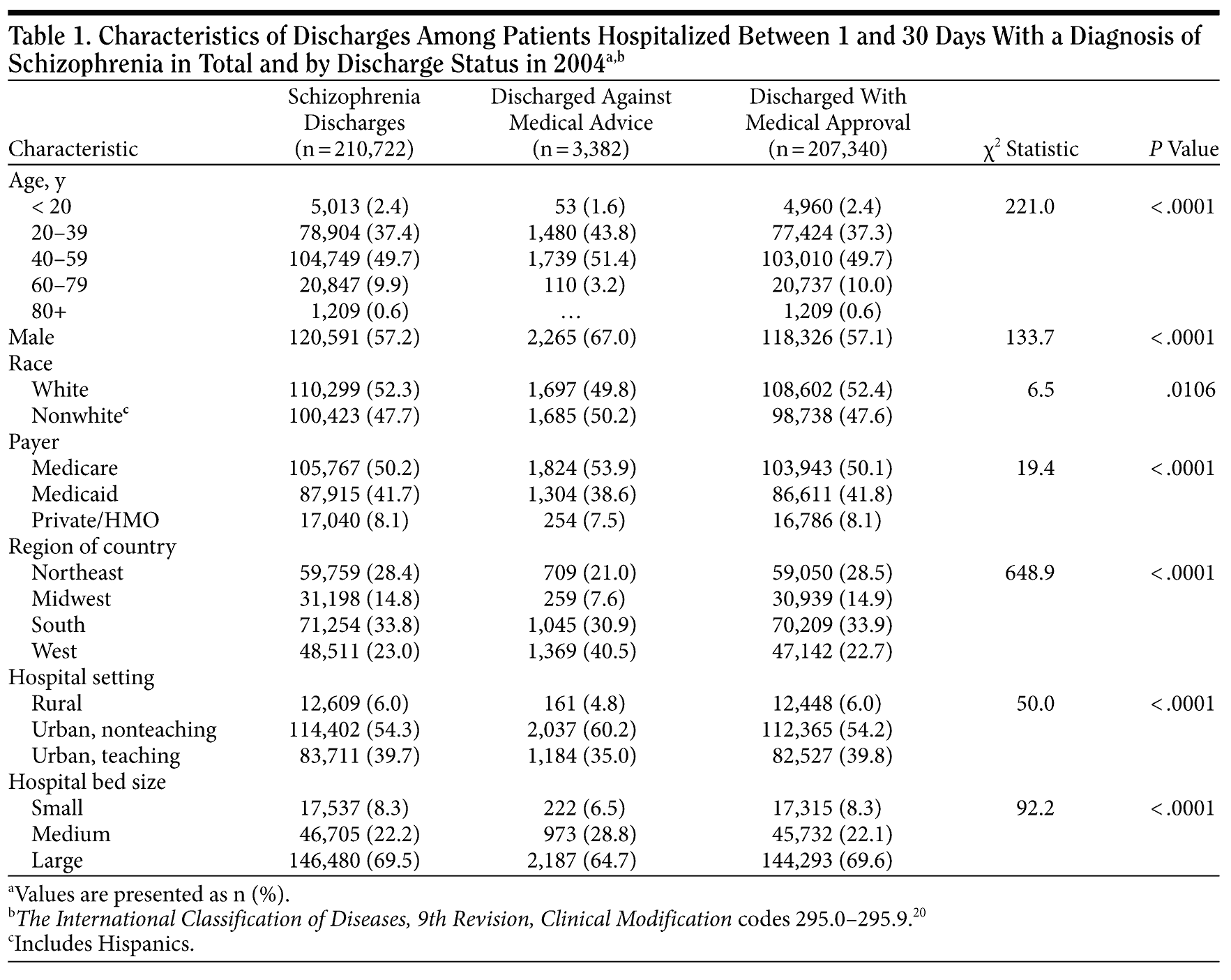
Characteristics of the 210,722 hospital discharges for schizophrenia are presented in Table 1, in total and by discharge status. Overall, patients were predominantly male (57.2%), white (52.3%), and had a mean ± SD age of 42.8 ± 13.3 years. Over half (50.2%) of the study population had Medicare as the primary source of insurance coverage, 41.7% had Medicaid, and only 8.1% reported private insurance. Within the study population, 1.6% of patients were discharged against medical advice (n = 3,382/210,722).
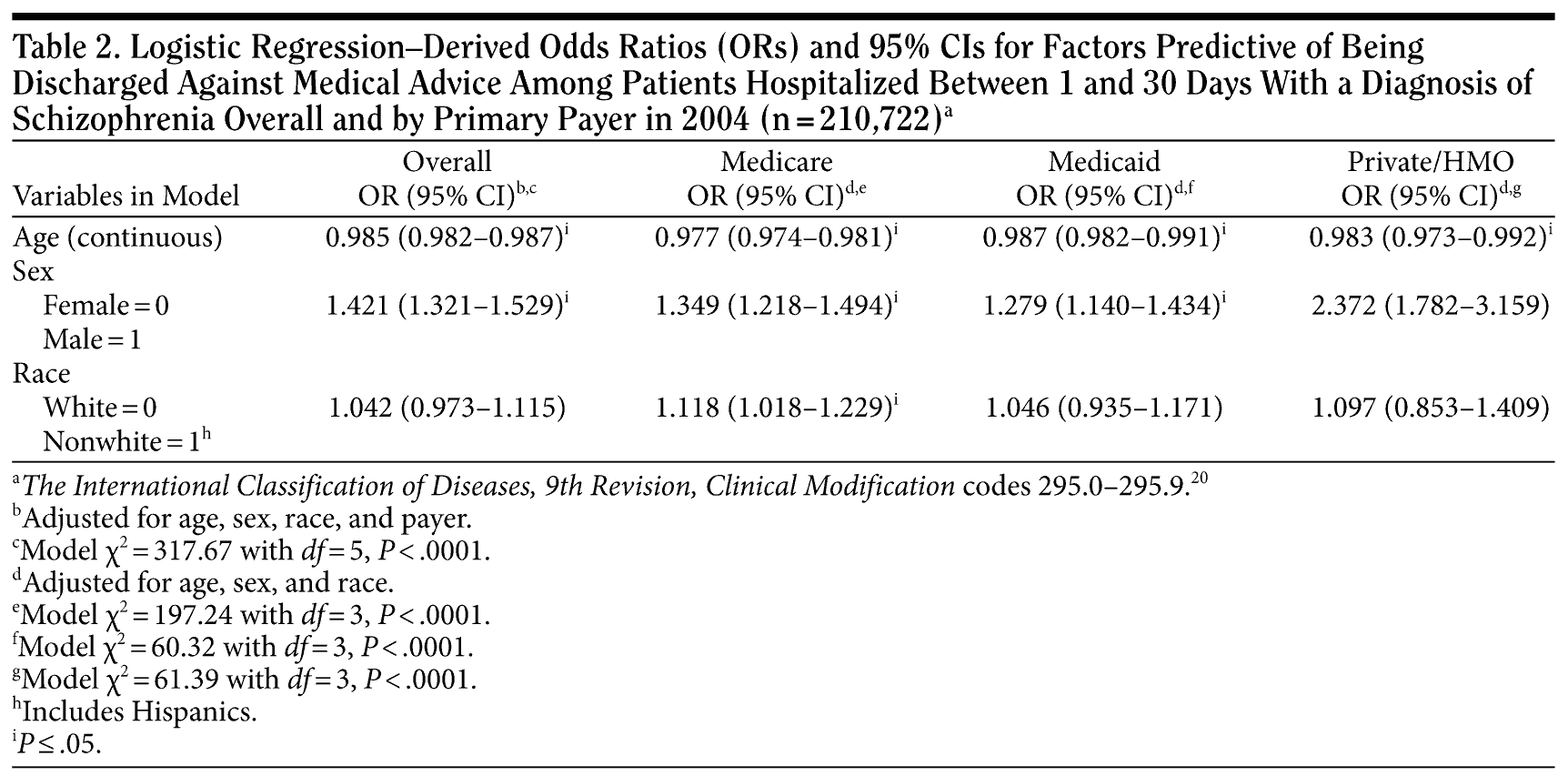
Overall, patients discharged against medical advice were significantly more likely to be younger (OR = 0.985; 95% CI, 0.982-0.987) and male (OR = 1.421; 95% CI, 1.321-1.529), as compared to patients released with medical approval. Race was not a significant factor (Table 2). Separate analyses by primary payer (Medicare, Medicaid, and private insurance) revealed similar results, with younger age and male gender being significant predictors of discharge against medical advice. Among Medicare beneficiaries, being nonwhite was also a significant predictor for being discharged against medical advice (OR = 1.118; 95% CI, 1.018-1.229).
Table 3 presents the adjusted least squares means for hospital length of stay by discharge status. The overall mean ± SE length of stay for patients discharged against medical advice was 5.0 ± 0.24 days, as compared to 8.7 ± 0.06 days (P < .0001) for patients discharged with medical approval. Separate analyses by primary payer revealed similar statistically significant results. The adjusted mean length of stay for patients discharged against medical advice was reduced by 41.1% for Medicare patients, 45.1% for Medicaid patients, and 39.2% for patients with private insurance, as compared to patients discharged with medical approval.
The overall adjusted mean ± SE charge per hospital day for patients discharged against medical advice was significantly higher (P < .0001) ($1,886.02 ± $49.67), as compared to patients discharged with medical approval ($1,565.79 ± $13.42) (Table 4). Similar increases (P < .0001) were discerned within each payer category.
DISCUSSION
Previous studies of psychiatric inpatients hospitalized within psychiatric units have discerned a mean discharge against medical advice rate of approximately 16% across all diagnoses.1,23-26 However, small sample sizes and lack of clarity regarding diagnostic classification have limited the generalizability of these studies. Moreover, most of these studies were undertaken prior to the advent of managed care when inpatient length of stays were longer.1 Over the past 3 decades, the trend in psychiatric patient care has been to shift inpatient treatment away from its traditional parens patriae role to short-term stabilization and acute care.12,27
Our research indicates that, among US patients hospitalized in acute care hospitals with a primary diagnosis of schizophrenia in 2004, 1.6% were discharged against medical advice. This prevalence rate is in the range reported for all patients admitted to US acute care hospitals who subsequently were discharged against medical advice (0.8%-2.2%).3-7 Younger age and male sex were found to be predictive of discharge against medical advice in the aggregate and across payer type. These factors have consistently been reported as predictors of hospital discharge against medical advice across a variety of diagnoses and in a number of hospital settings, including community hospitals,28-30 teaching hospitals,6 and psychiatric units.12,31
Although numerous studies have documented race,1 especially black race,8-10,28 to be a significant predictor of discharge against medical advice, we did not discern a significant difference between whites and nonwhites, inclusive of Hispanics, when examining the entire study population. However, separate analyses by primary payer indicate that nonwhites enrolled in Medicare were approximately 12% more likely to be discharged against medical advice.
After adjusting for potentially confounding factors, inclusive of age, sex, race, region of the country, hospital setting, hospital bed size, and payer, we found the mean ± SE hospital length of stay to have been reduced by 3.7 days for patients discharged against medical advice (5.0 ± 0.24 days) as compared to those discharged with medical approval (8.7 ± 0.06 days). Separate analyses by primary payer revealed a similar magnitude of reduction in hospital length of stay (Medicare, 3.9 days; Medicaid, 3.7; private, 3.1). Interestingly, the adjusted mean ± SE hospital length of stay for patients with private insurance and released with medical approval (7.9 ± 0.21 days) was significantly shorter than that of patients whose primary payer was Medicare (9.5 ± 0.08 days) or Medicaid (8.2 ± 0.10 days).
This finding is in agreement with previous research examining the influence of payer type on hospital length of stay for patients with schizophrenia and may represent a quality-of-care concern.32 If a reduced hospital length of stay has an adverse influence on the care of patients with schizophrenia, then relapse rates and overall costs may actually increase under private insurance programs. On the other hand, if private insurance programs have delivered on the promise of reducing costs while improving the quality and scope of care, then both patients with schizophrenia and society will benefit greatly.
Results stemming from this inquiry indicate the mean charge per hospital day was significantly higher for patients discharged against medical advice relative to patients discharged with medical approval across all patients ($1,886.02 vs $1,565.79) and by primary payer. Findings may reflect greater acuity at the time of hospital admission among patients who were ultimately discharged against medical advice,2 or a reduction in charges (intensity of care) may have occurred during the latter course of a hospital stay for patients discharged with medical approval.
We acknowledge that factors not recorded in the NIS, inclusive of a clinical measure of severity of illness (at time of hospital admission and/or discharge), level of social support, and access to outpatient mental health services, limit the conclusions that may be drawn from our analyses. Moreover, the NIS did not include patients admitted to psychiatric hospitals or alcoholism/chemical dependency treatment facilities. That said, the empirical findings presented herein provide a basic understanding as to the magnitude of, demographic predictors for, and inpatient cost profile for hospital discharge against medical advice among patients with schizophrenia.
Author affiliations: Pharmacoeconomics and Pharmacoepidemiology Research Unit, Department of Health Policy and Administration, and Department of Pharmacotherapy (Dr Sclar and Ms Robison) and Department of Statistics (Dr Sclar), Washington State University, Pullman; and Washington Institute for Mental Illness Research and Training, Spokane (Dr Sclar).
Potential conflicts of interest: The authors report no financial or other relationship relevant to the subject of this article.
Funding/support: This study was supported in full by the Pharmacoeconomics and Pharmacoepidemiology Research Unit, Department of Health Policy and Administration, Washington State University, Pullman.
Previous presentation: Presented in part at the World Congress of the World Association of Social Psychiatry; Prague, Czech Republic; October 23, 2007.
REFERENCES
1. Pages KP, Russo JE, Wingerson DK, et al. Predictors and outcome of discharge against medical advice from the psychiatric units of a general hospital. Psychiatr Serv. 1998;49(9):1187-1192. PubMed
2. Gerbasi JB, Simon RI. Patients’ rights and psychiatrists’ duties: discharging patients against medical advice. Harv Rev Psychiatry. 2003;11(6):333-343. PubMed doi:10.1080/714044395
3. Hwang SW, Li J, Gupta R, et al. What happens to patients who leave hospital against medical advice? CMAJ. 2003;168(4):417-420. PubMed
4. Smith DB, Telles JL. Discharges against medical advice at regional acute care hospitals. Am J Public Health. 1991;81(2):212-215. PubMed
5. Jeremiah J, O’ Sullivan P, Stein MD. Who leaves against medical advice? J Gen Intern Med. 1995;10(7):403-405. PubMed doi:10.1007/BF02599843
6. Weingart SN, Davis RB, Phillips RS. Patients discharged against medical advice from a general medicine service. J Gen Intern Med. 1998;13(8):568-571. PubMed doi:10.1046/j.1525-1497.1998.00169.x
7. Saitz R, Ghali WA, Moskowitz MA. The impact of leaving against medical advice on hospital resource utilization. J Gen Intern Med. 2000;15(2):103-107. PubMed doi:10.1046/j.1525-1497.2000.12068.x
8. Moy E, Bartman BA. Race and hospital discharge against medical advice. J Natl Med Assoc. 1996;88(10):658-660. PubMed
9. Franks P, Meldrum S, Fiscella K. Discharges against medical advice: are race/ethnicity predictors? J Gen Intern Med. 2006;21(9):955-960. PubMed doi:10.1007/BF02743144
10. Fiscella K, Meldrum S, Barnett S. Hospital discharge against advice after myocardial infarction: deaths and readmissions. Am J Med. 2007;120(12):1047-1053. PubMed doi:10.1016/j.amjmed.2007.08.024
11. Lee TH, Short LW, Brand DA, et al. Patients with acute chest pain who leave emergency departments against medical advice: prevalence, clinical characteristics, and natural history. J Gen Intern Med. 1988;3(1):21-24. PubMed doi:10.1007/BF02595752
12. Brook M, Hilty DM, Liu W, et al. Discharge against medical advice from inpatient psychiatric treatment: a literature review. Psychiatr Serv. 2006;57(8):1192-1198. PubMed doi:10.1176/appi.ps.57.8.1192
13. American Psychiatric Association. Practice Guideline for the Treatment of Patients With Schizophrenia. Am J Psychiatry. 1997;154(suppl 4):1-63. PubMed
14. Mortensen PB. Schizophrenia in society: an epidemiological perspective. Dis Manage Health Outcome. 1997;2(2):77-84. doi:10.2165/00115677-199702020-00003
15. Miller DD. Schizophrenia: its etiology and impact. Pharmacotherapy. 1996;16(1, pt 2):2-5. PubMed
16. Hunt IM, Kapur N, Windfuhr K, et al. Suicide in schizophrenia: findings from a national clinical survey. J Psychiatr Pract. 2006;12(3):139-147. PubMed doi:10.1097/00131746-200605000-00002
17. McGlashan TH, Heinssen RK. Hospital discharge status and long-term outcome for patients with schizophrenia, schizoaffective disorder, borderline personality disorder, and unipolar affective disorder. Arch Gen Psychiatry. 1988;45(4):363-368. PubMed
18. Bickley H, Kapur N, Hunt IM, et al. Suicide in the homeless within 12 months of contact with mental health services: a national clinical survey in the UK. Soc Psychiatry Psychiatr Epidemiol. 2006;41(9):686-691. PubMed doi:10.1007/s00127-006-0087-6
19. HCUP Nationwide Inpatient Sample (NIS). Healthcare Cost and Utilization Project (HCUP) 2004. Agency for Healthcare Research and Quality, Rockville, MD. www.hcup-us.ahrq.gov/nisoverview.jsp. Accessed July 12, 2007.
20. US Public Health Service and Health Care Financing Administration. The International Classification of Diseases, 9th Revision, Clinical Modification, vol 2. Washington, DC: Public Health Service; 1989
21. American Hospital Association Annual Survey Database for Fiscal Year 2004, 2006. American Hospital Association; Chicago, IL
22. SAS Institute Inc. SAS Statistical Analysis Software. 9.3.1 edition. Cary, NC; 2003
23. Planansky K, Johnston R. A survey of patients leaving a mental hospital against medical advice. Hosp Community Psychiatry. 1976;27(12):865-867. PubMed
24. Akhtar S, Halfrinch J, Mestayer R. AMA discharge from a psychiatric inpatient unit. Int J Soc Psychiatry. 1981;27(2):143-150. PubMed doi:10.1177/002076408102700210
25. Siegel RL, Chester TK, Price DB. Irregular discharges from psychiatric wards in a VA medical center. Hosp Community Psychiatry. 1982;33(1):54-56. PubMed
26. Dalrymple AJ, Fata M. Cross-validating factors associated with discharges against medical advice. Can J Psychiatry. 1993;38(4):285-289. PubMed
27. Quanbeck C, Frye M, Altshuler L. Mania and the law in California: understanding the criminalization of the mentally ill. Am J Psychiatry. 2003;160(7):1245-1250. PubMed doi:10.1176/appi.ajp.160.7.1245
28. Ibrahim SA, Kwoh CK, Krishnan E. Factors associated with patients who leave acute-care hospitals against medical advice. Am J Public Health. 2007;97(12):2204-2208. PubMed doi:10.2105/AJPH.2006.100164
29. Seaborn Moyse H, Osmun WE. Discharges against medical advice: a community hospital’s experience. Can J Rural Med. 2004;9(3):148-153. PubMed
30. Baptist AP, Warrier I, Arora R, et al. Hospitalized patients with asthma who leave against medical advice: characteristics, reasons, and outcomes. J Allergy Clin Immunol. 2007;119(4):924-929. PubMed doi:10.1016/j.jaci.2006.11.695
31. Phillips MS, Ali H. Psychiatric patients who discharge themselves against medical advice. Can J Psychiatry. 1983;28(3):202-205. PubMed
32. Sclar DA, Robison LM, Skaer TL, et al. Hospital length of stay for schizophrenia: is primary payer an influencing factor? Dis Manage Health Outcome. 1999;5(6):339-347. doi:10.2165/00115677-199905060-00004