Sulfotransferase 4A1 Haplotype 1 (SULT4A1-1) Is Associated With Decreased Hospitalization Events in Antipsychotic-Treated Patients With Schizophrenia

ABSTRACT
Objective: To evaluate a common genetic variant, sulfotransferase 4A1 haplotype 1 (SULT4A1-1), as a predictor of hospitalization events due to the exacerbation of schizophrenia for patients treated with antipsychotic medications. Haplotypes were determined using single nucleotide polymorphism data.
Method: The study included 417 white subjects from the Clinical Antipsychotic Trials of Intervention Effectiveness (CATIE) study with a DSM-IV diagnosis of schizophrenia. Patients were assigned to 1 of 4 atypical antipsychotics (olanzapine, quetiapine, risperidone, or ziprasidone) or to the first-generation antipsychotic perphenazine. Kaplan-Meier survival analysis and Cox proportional hazards regression models were used to measure if haplotype status impacted hospitalization events for these 5 treatments. Haplotype status was evaluated for its relationship to hospitalization events regardless of treatment and for the individual treatments, with or without previous exacerbation. Data for the CATIE study were collected from January 2001 to December 2004. The current post hoc analysis was performed between May 2011 and August 2011.
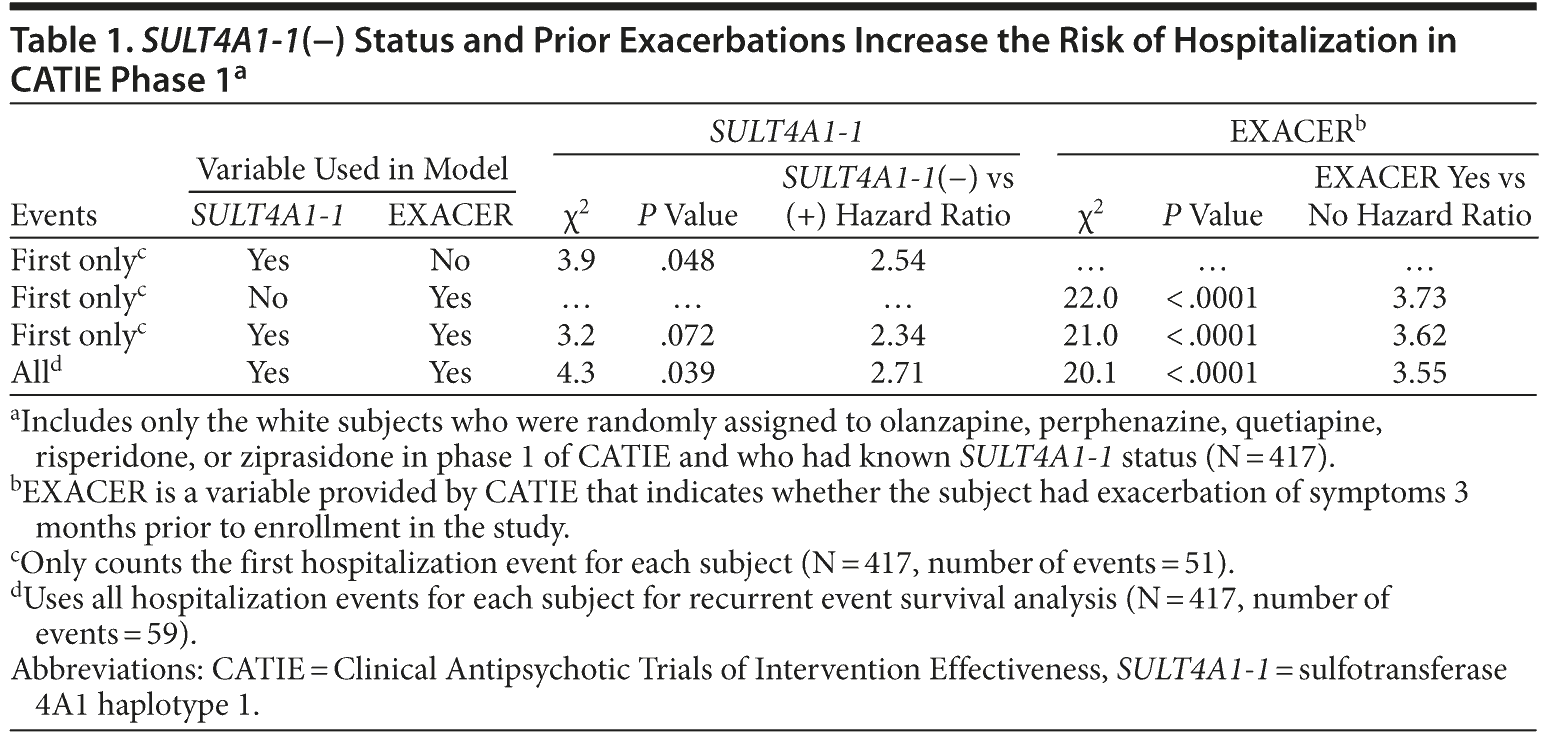
Results: In phase 1 of the trial, considering only the first hospitalization events, the haplotype had a significant impact on hospitalization events, with a hazard ratio for SULT4A1-1(−) versus SULT4A1-1(+) of 2.54 (P = .048). When prior exacerbation was included in the model for phase 1, the hazard ratio was 2.34 (P = .072) considering only the first hospitalization event and 2.71 (P = .039) considering all hospitalization events in the phase. When data for all phases were evaluated, SULT4A1-1(−) status was associated with increased hospitalization risk for subjects treated with olanzapine, with a hazard ratio of 8.26 (P = .041), and possibly for subjects treated with quetiapine, with a hazard ratio of 6.80 (P = .070).
Conclusions: The SULT4A1-1 haplotype may be an important predictor of risk of hospitalization. SULT4A1-1(+) status was significantly associated with decreased risk of hospitalization when the subjects were treated with olanzapine.
Prim Care Companion CNS Disord 2012;14(3):doi:10.4088/PCC.11m01293
© Copyright 2012 Physicians Postgraduate Press, Inc.
Submitted: September 12, 2011; accepted December 16, 2011.
Published online: May 24, 2012.
Corresponding author: Mark D. Brennan, PhD, SureGene, LLC, 600 Envoy Cir Ste 601, Louisville, KY 40299 ([email protected]).
Schizophrenia is a chronic mental illness characterized by periodic relapses or worsening of clinical symptoms (exacerbation). Relapses and the often ensuing hospitalization inflict a deleterious effect on patients and relatives and add greatly to the burden of treating schizophrenia.1 Estimates for the annual cost of schizophrenia in the United States exceeded $62 billion in 2002.2 Hospitalization due to exacerbation or relapse represents one of the largest sources of this expense.1,3 Vasudeva et al4 estimated that patients have a 40% to 50% probability of readmission following an initial hospitalization for a psychiatric disorder. For patients with schizophrenia, the relapse rate ranges from 19% to 100% depending on the number of previous relapses and how well the patients are adherent to prescribed antipsychotic medication.5 According to a recent study, hospitalized patients incur over twice the annual costs compared to those who are not hospitalized, and rehospitalization predicted higher annual cost.3 Given the significance, cost, and impact of hospitalization, the ability to minimize the risk of relapse and rehospitalization by identifying treatments most likely to minimize relapse has great value.
Common genetic variation in the sulfotransferase 4A1 (SULT4A1) gene holds promise as a predictor of hospitalization risk for patients with schizophrenia treated with olanzapine or who might be switched to olanzapine. Previous studies have shown that genetic variation in the SULT4A1 gene is associated with severity of clinical symptoms and response to antipsychotic treatment.6,7 Patients carrying a specific haplotype of the gene, termed SULT4A1-1, have higher baseline psychopathology and display improved long-term response to olanzapine treatment.7
The Clinical Antipsychotic Trials of Intervention Effectiveness (CATIE) study, intended to model clinical practice, has been used for genetic studies of antipsychotic treatment response and prediction of individual difference in treatment outcomes for patients with schizophrenia.8,9 For example, Need et al10 performed a genetic association study of single nucleotide polymorphisms with 21 drug response phenotypes using CATIE. Van den Oord et al11 built a model that predicted individual treatment response using the Positive and Negative Syndrome Scale (PANSS), and McClay and colleagues12 used predicted PANSS scores from that model to conduct a genome-wide association study that identified potential pharmacogenomic biomarkers for antipsychotic response.
The present study examined the CATIE data for the potential influence of SULT4A1-1 haplotype status on hospitalization due to exacerbation of schizophrenia. The impact of SULT4A1-1 haplotype status on hospitalization due to exacerbation was assessed by survival analysis employing Kaplan-Meier and Cox proportional hazard regression. The possible utility of determining SULT4A1-1 haplotype status in the clinical setting is discussed.
METHOD
Subjects and Data
CATIE sample. The details of the CATIE study design, including the treatment phases, informed consent, and details of genotyping, have been described in detail by others.8,9 Briefly, patients with a DSM-IV diagnosis of schizophrenia were randomly assigned to olanzapine, perphenazine, quetiapine, risperidone, or ziprasidone in phase 1 under double-blind conditions. The duration of the study was 18 months. Patients who discontinued the treatment in phase 1 or 2 could receive other treatment in the following phases. Data for the CATIE study were collected from January 2001 to December 2004. The current post hoc analysis was performed between May 2011 and August 2011.
Several variables provided by the CATIE consortium, and made available through the Center for Collaborative Genomic Studies on Mental Disorders, were used for the present study.13 The main dependent variable was “hospitalization due to exacerbation of schizophrenia” provided by the CATIE consortium as the HOSPEXAC variable from the serious adverse events table. This binary variable lists hospitalization as a type of serious adverse event due to exacerbation of schizophrenia, with a value of 1 indicating that exacerbation of schizophrenia was the cause of hospitalization. Several variables were obtained from the demographics and baseline characteristics table, including the other primary variable EXACER. This binary variable described whether or not the subject had experienced exacerbation of symptoms in the 3 months prior to enrollment in the CATIE study. Patient variables for subject age, sex, baseline PANSS total score, and ethnicity were also used.

- Hospitalization, a common complication of schizophrenia, is usually the result of treatment failure and accounts for about one-third of the cost of this illness.
- The sulfotransferase 4A1 haplotype 1 (SULT4A1-1) genetic marker identifies a subset of patients that have lower risk of hospitalization when treated with olanzapine or quetiapine compared to risperidone, ziprasidone, or perphenazine.
- Knowledge of a patient’s SULT4A1-1 status may help to guide choice of antipsychotic treatment for patients with psychosis.
Hospitalization events were tracked for each phase separately. The start day and end day of each phase were taken from the CATIE database table TIMETO, with the variables B1_DAY and ENDDY_1 as the start day and end day for phase 1, respectively. Similarly, B1B_DAY and ENDDY_1B represented the start and end day for phase 1B, with additional phases following the same pattern. The CATIE variables for hospitalization duration (ONSET and STOPDY) were taken as the start and stop day for each hospitalization event. In the special case of multiple hospitalization events in a given phase, we employed recurrent event survival analysis as described below.
To study the impact of prior exacerbation on risk of hospitalization for all 3 phases of the CATIE study, we created a new variable that captured both exacerbations prior to enrollment in the study as well as within-study exacerbations. Briefly, for phase 1A, the value of the modified exacerbation variable EXACER* was the same as the value of the CATIE-defined EXACER variable. For observations in phase 1B, phase 2, and phase 3, if the CATIE-defined exacerbation for the subject was 0 and the subjects had their first hospitalization event in phase k (k = 1, 2, 3), the EXACER* would be 1 for phase k + 1 and k + 2, while the variable would be 0 for phase k and earlier phases. If the CATIE-defined exacerbation (EXACER) for the subject was 1, then EXACER* was also 1 for all time points.
We previously described the methods for determining SULT4A1-1 haplotype status for the 417 white patients who consented to genetic analysis.7 Subjects carrying at least 1 copy of the SULT4A1-1 haplotype (22% of total) were scored as SULT4A1-1(+). Conversely, those subjects with zero copies of the SULT4A1-1 haplotype (78% of total) were scored as SULT4A1-1(−).7
Statistical Analyses
The SAS statistical analysis package (SAS for Windows system, version 9.2, SAS Inc, Cary, North Carolina) was used to perform all of the analyses. For the initial investigation, we used phase 1 data to determine if the haplotype was associated with hospitalization events of patients treated with antipsychotics. For the initial analysis of phase 1 data, only the first hospitalization event due to exacerbation of schizophrenia was counted for each subject. Subjects started at day 1 and were followed until an event occurred or until the end of phase 1 for that subject. Patients were censored if they stayed until the end of phase 1 or left the study before the end of phase 1 but did not experience an event. Otherwise, subjects were classified as having an event in phase 1 if day 1 of the hospitalization occurred between the start and the end of phase 1. We used the Kaplan-Meier method with the log-rank test to assess the difference between groups (PROC LIFETEST in SAS) and to calculate the 18-month survival curves for 3 analytic groups: (1) SULT4A1-1 status only, (2) EXACER status only, and (3) simultaneous analysis of both SULT4A1-1 and EXACER. To calculate hazard ratios (HRs), we used Cox proportional hazard regressions (PROC PHREG in SAS).
To capture multiple hospitalization events in multiple phases, we used recurrent event survival analysis. Briefly, phase 1, 1B, 2, and 3 data were combined. A counting process was used to capture all of the hospitalization events for each subject in a given phase. We treated multiple phases for the same subject as multiple, independent observations. For phases subsequent to phase 1, the day of entry into the following phase was set as day 1. For duration of the corresponding phase, we used either days in phase if no events occurred or the number of days until the events in that phase. When we analyzed the data by treatment, each subject contributed only once in each treatment starting at day 1. Cox proportional hazard regression models were built for each treatment. We included 2 predictors in the model, SULT4A1-1 status as a covariate and exacerbation as a class variable. Survival function estimates and hazard ratios were calculated for the variables SULT4A1-1 haplotype status and modified exacerbation (EXACER*).
Using the SAS options BASELINE and COVARIATES in PROC PHREG, we created survival function estimates for each group on the basis of the Cox proportional hazard regression model, and survival curves were plotted to visualize the difference between groups. The SAS COVSANDWICH (AGGREGATE) option and the ID statement were used to correct for dependence.14 One subject was given risperidone in both phase 2 and phase 3 and experienced no events. Consequently, this subject’s phase 3 data were not used so as to avoid censoring the same subject twice. Subject age, baseline PANSS total score, and sex were evaluated as covariates in the various models.
RESULTS
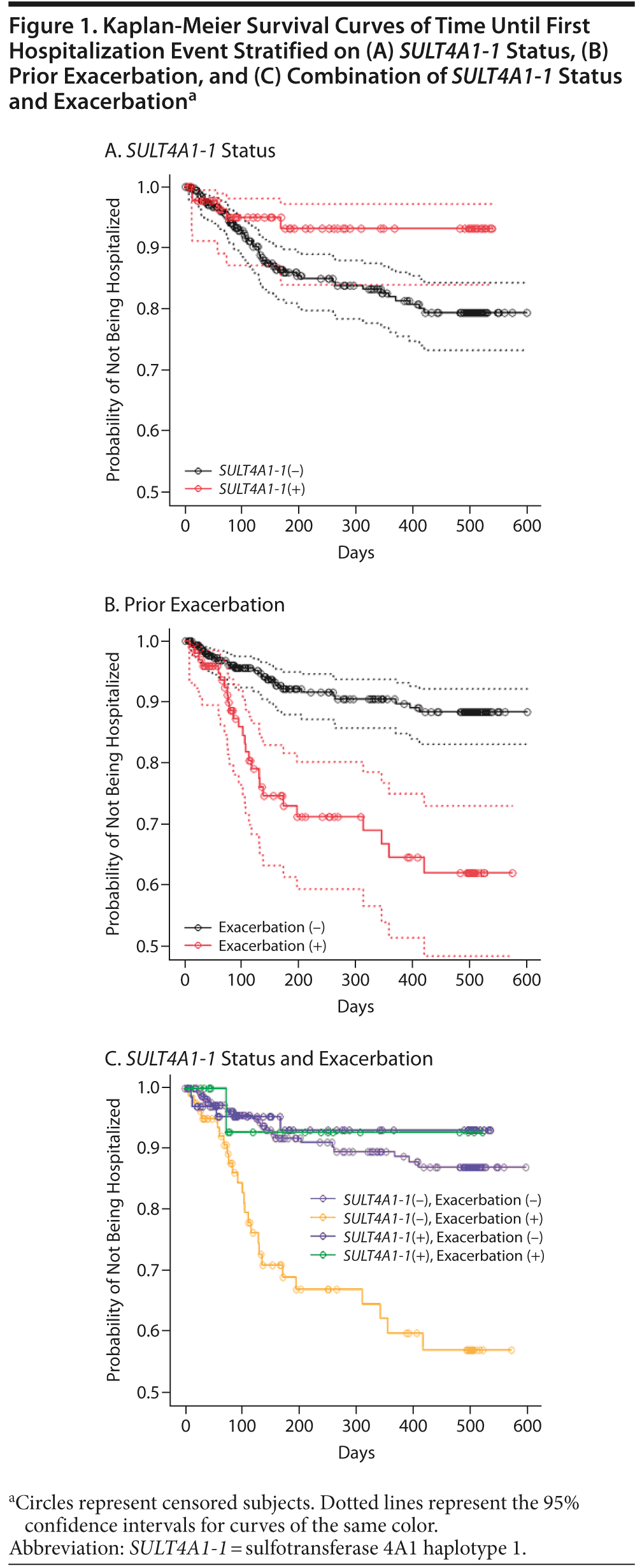
To evaluate the impact of SULT4A1-1 status on hospitalization for schizophrenia in phase 1 of CATIE regardless of treatment, we performed a Kaplan-Meier survival analysis. Figure 1A shows that SULT4A1-1(−) CATIE subjects had a greater risk of hospitalization than SULT4A1-1(+) subjects (log-rank test, P = .040). Cox proportional hazard regression analysis demonstrated that SULT4A1-1(−) patients were 2.54-fold more likely to experience a hospitalization event than SULT4A1-1(+) patients (Table 1, P = .048).
Additionally, since prior, recent exacerbations have been associated with increased risk of future hospitalizations,4 we examined whether prior exacerbation contributed to the risk of hospitalization in CATIE phase 1. Using the CATIE-provided binary variable describing whether the patient had an exacerbation during the 3 months prior to the start of phase 1 of the CATIE trial, Kaplan-Meier and Cox regression analyses confirmed that prior exacerbation was a highly significant predictor for hospitalization (log-rank test, P < .0001) (Figure 1B). The subjects with prior exacerbation had a 3.73-fold greater likelihood of being hospitalized than the subjects without prior exacerbation (Table 1, P < .0001).
Since both SULT4A1-1 status and prior exacerbation predicted risk of hospitalization in phase 1 when considered individually, we next evaluated both variables simultaneously using the same approach. As expected, the overall log-rank test from the Kaplan-Meier method showed that the model incorporating both terms had a highly significant impact on likelihood of hospitalization. Interestingly, despite the strength of the association for prior exacerbation, SULT4A1-1 status remained predictive of hospitalization (Figure 1C). The Cox proportional hazard model showed that SULT4A1-1(−) subjects had a 2.34-fold elevated risk for hospitalization irrespective of exacerbation status (Table 1, P = .072).
Since some subjects experienced multiple hospitalization events, we used recurrent event survival analysis, as described in the Method, to capture all of the hospitalization events in phase 1. This analysis resulted in an HR of 2.71 for SULT4A1-1(−) patients relative to SULT4A1-1(+) patients (Table 1, P = .039). SULT4A1-1(−) subjects with prior exacerbation had a significantly elevated risk of hospitalization compared to all other subject classes. The HRs for these comparisons are 4.03 relative to SULT4A1-1(−) patients without exacerbation, 5.43 relative to SULT4A1-1(+) with exacerbation, and 6.17 relative to SULT4A1-1(+) without exacerbation.
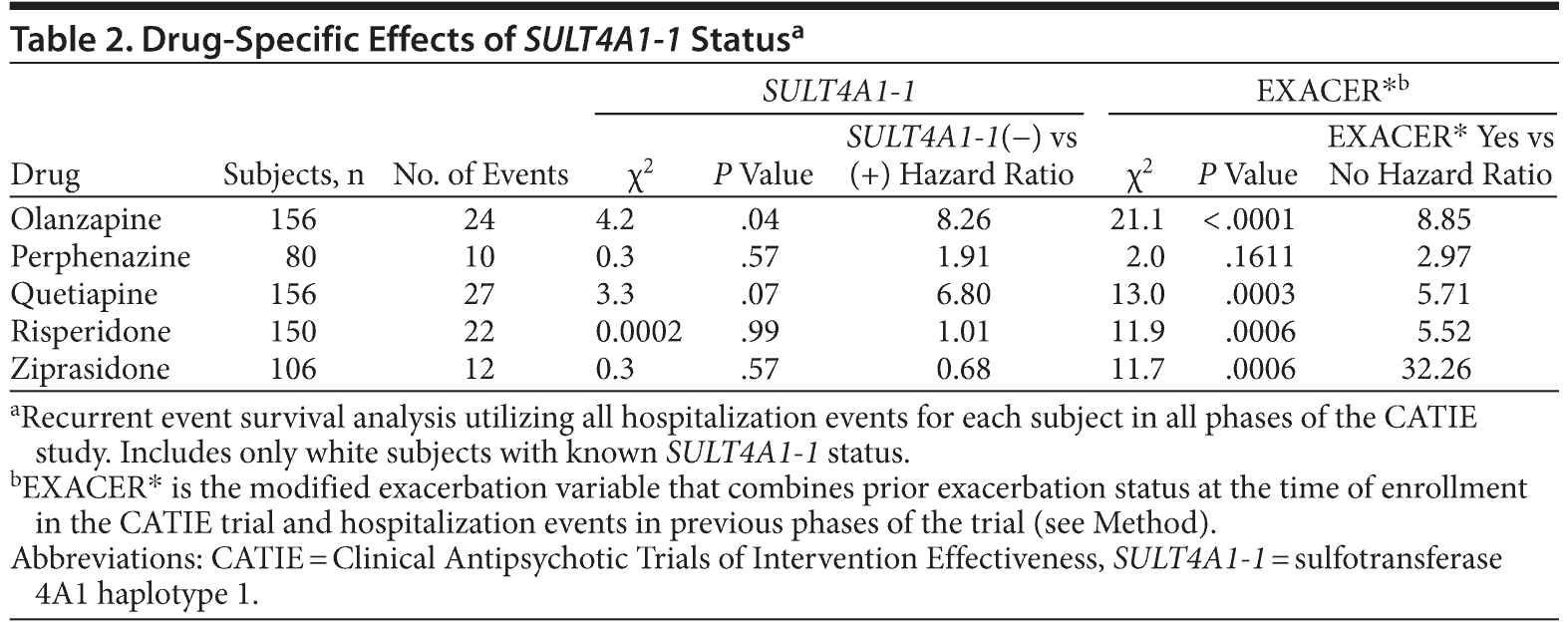
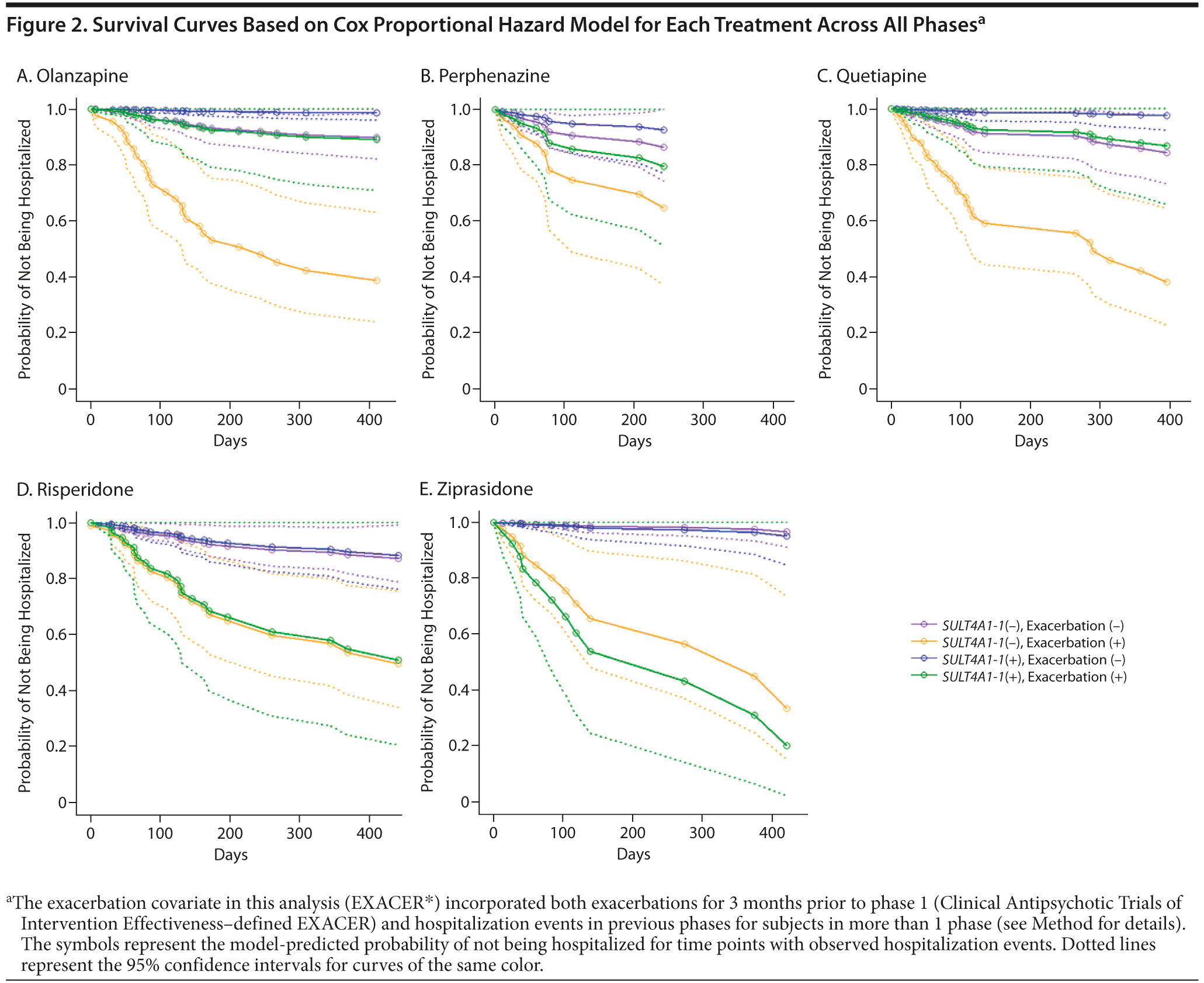
To investigate possible drug-specific effects of the SULT4A1-1 haplotype and/or exacerbation on hospitalization risk, we built Cox proportional hazard models using recurrent event survival analysis separately for olanzapine, perphenazine, quetiapine, risperidone, and ziprasidone. Since these analyses incorporated all phases and all hospitalization events, we built separate models for each drug so as to avoid double counting subjects in a given model. As described in the Method, the Cox proportional hazard model for each treatment utilized exacerbation as a class variable and SULT4A1-1 status as a covariate. In order to apply the model across all phases of the trial, exacerbation (EXACER*) included both the CATIE-provided variable for exacerbation prior to phase 1 (which captured exacerbation 3 months prior to phase 1) and an exacerbation variable for the later phases as described in the Method.
With the exception of perphenazine, prior exacerbation was a highly significant predictor for all drugs, with previous exacerbation increasing the risk of future hospitalizations. In both the olanzapine and quetiapine arms, SULT4A1-1 status altered the risk of hospitalization. SULT4A1-1(−) subjects had a 8.26-fold elevated risk for hospitalization relative to SULT4A1-1(+) subjects when treated with olanzapine (P = .041). Patients treated with quetiapine displayed a similar trend, with SULT4A-1(−) subjects having a 6.80-fold elevated risk for hospitalization relative to SULT4A1-1(+) subjects (P = .070). SULT4A1-1 status did not significantly impact hospitalization risk for perphenazine, risperidone, or ziprasidone. These results are shown in tabular form in Table 2 and graphically in Figure 2A-E.
Additionally, for all of the analyses, we tested the effect of age, sex, and baseline PANSS total score on hospitalization risk. Neither age nor sex significantly impacted hospitalization risk in any of the Cox proportional hazard models listed above. Baseline PANSS total score, a potential confounder of the SULT4A1 and/or exacerbation effect on hospitalization risk, was a significant covariate in the phase 1 Cox proportional hazard models that included SULT4A1-1 status, exacerbation, and baseline PANSS total score. In phase 1, adding baseline PANSS total score to the models reduced the significance and HR for prior exacerbation and modestly increased the significance and HR attributable to SULT4A1-1 status. In contrast, baseline PANSS total score did not significantly impact hospitalization risk in any of the individual drug analyses that included all phases.
DISCUSSION
The present study examined the impact of the SULT4A1-1 haplotype on risk of hospitalization in a large cohort of patients with schizophrenia treated with 5 antipsychotic drugs in the CATIE study. We found significant effects of both SULT4A1-1 status and prior exacerbation on hospitalization risk. Additionally, analysis of the data from all phases showed a significant elevation of hospitalization risk for SULT4A1-1(-) subjects treated with olanzapine. The analysis further showed a trend for SULT4A1-1(−) status to predict greater risk of hospitalization for patients treated with quetiapine. Thus, SULT4A1-1(+) status may mitigate the risk of future hospitalizations for patients with recent prior history of exacerbation when patients are treated with either olanzapine or quetiapine.
The manner in which SULT4A1-1 haplotype status is related to response to olanzapine is unknown. SULT4A1 is expressed primarily in the brain, and olanzapine is metabolized by cytochrome 3A43 in the brain.15,16 Presumably, the haplotype correlates with altered expression of the encoded SULT4A1 protein, which may be involved in either the pharmacodynamic action and/or the metabolism of olanzapine. SULT4A1 has binding affinity for numerous psychoactive compounds including catecholamines and neurosteroids.17 Therefore, one possible explanation for the impact of the SULT4A1-1 haplotype on olanzapine efficacy is that altered SULT4A1 levels could preferentially impact either sulfation or sequestration of olanzapine in the brain.
The present study suggests that SULT4A1-1 status may provide a predictive tool to help reduce the risk of hospitalization. The lower hospitalization rate in the SULT4A1-1(+) patients treated with olanzapine is consistent with previous findings that this patient group shows good improvement in psychopathology.7 Hospitalization for schizophrenia is a key component of the high emotional and economic costs of treating the disease. Most patients with schizophrenia will experience a hospitalization event at some point during the course of their illness.18 Furthermore, once a hospitalization event occurs, future events are more likely.3,4 Predictive tools that identify those patients at greatest risk of hospitalization and/or that identify antipsychotic therapy that can reduce additional hospitalizations could enhance patient care and reduce costs. Medication nonadherence, psychiatric comorbidities, substance abuse, younger age at onset, suicidal ideation, and more severe psychopathology at baseline also predict greater likelihood of future hospitalization.19 Potential interaction between SULT4A1-1 status, antipsychotic medications, and the other predictors of relapse are interesting avenues for future research.
The relatively small number of SULT4A1-1(+) patients is a key limitation in the current study. Additionally, the total number of hospitalizations was low, particularly in the SULT4A1-1(+) olanzapine and quetiapine arms. In any case, the hospitalization rates observed in the CATIE study as a whole are close to the expected levels, both with and without recent exacerbation, on the basis of a recent naturalistic study utilizing a large cohort of patients in the United States.3
In conclusion, the results reported here indicate that the SULT4A1-1 biomarker will be clinically useful to reduce the risk for relapse and hospitalization in approximately 23% of white patients with schizophrenia. If replicated in prospectively designed studies, SULT4A1-1 status could provide a valuable tool for managing the treatment of schizophrenia.
Drug names: olanzapine (Zyprexa), quetiapine (Seroquel), risperidone (Risperdal and others), ziprasidone (Geodon).
Author affiliations: SureGene, LLC, Louisville, Kentucky (Drs Liu, Massey, and Brennan; Mr Ramsey; and Ms Padmanabhan); and Department of Psychiatry, Vanderbilt University, Nashville, Tennessee (Dr Meltzer).
Potential conflicts of interest: Dr Liu and Ms Padmanabhan are employees of SureGene and Drs Massey and Brennan and Mr Ramsey are employees of and stock shareholders in SureGene. Dr Meltzer has served as a consultant to ACADIA, Astellas, Azur, Lundbeck, Merck, Neurex, Neurogen, Novartis, SureGene, and TEVA; has received grant/research support and honoraria from Dainippon Sumitomo, Eli Lilly, Envivo, Janssen, Neurotherapeutics, Pfizer, Roche, and Sunovion; has served on the speakers or advisory boards of Sunovion; is a stock shareholder in ACADIA and SureGene; and has received other financial or material support from Bristol-Myers Squibb (testimony), Dainippon Sumitomo (patent pending), and Janssen.
Funding/support: This work was supported by National Institute of Mental Health grant MH078437 and Kentucky Economic Development Cabinet grants KSTC-184-512-09-071 and KSTC-184-512-10-098 (Dr Brennan). The CATIE trial was funded by a grant from the National Institute of Mental Health (N01 MH900001) along with MH074027. Genotyping for the CATIE study was funded by Eli Lilly.
REFERENCES
1. Weiden PJ, Olfson M. Cost of relapse in schizophrenia. Schizophr Bull. 1995;21(3):419-429. PubMed
2. Wu EQ, Birnbaum HG, Shi L, et al. The economic burden of schizophrenia in the United States in 2002. J Clin Psychiatry. 2005;66(9):1122-1129. PubMed doi:10.4088/JCP.v66n0906
3. Ascher-Svanum H, Zhu B, Faries DE, et al. The cost of relapse and the predictors of relapse in the treatment of schizophrenia. BMC Psychiatry. 2010;10(1):2. PubMed doi:10.1186/1471-244X-10-2
4. Vasudeva S, Narendra Kumar MS, Sekhar KC. Duration of first admission and its relation to the readmission rate in a psychiatry hospital. Indian J Psychiatry. 2009;51(4):280-284. PubMed doi:10.4103/0019-5545.58294
5. Furiak NM, Ascher-Svanum H, Klein RW, et al. Cost-effectiveness model comparing olanzapine and other oral atypical antipsychotics in the treatment of schizophrenia in the United States. Cost Eff Resour Alloc. 2009;7(1):4. PubMed doi:10.1186/1478-7547-7-4
6. Meltzer HY, Brennan MD, Woodward ND, et al. Association of Sult4A1 SNPs with psychopathology and cognition in patients with schizophrenia or schizoaffective disorder. Schizophr Res. 2008;106(2-3):258-264. PubMed doi:10.1016/j.schres.2008.08.029
7. Ramsey TL, Meltzer HY, Brock GN, et al. Evidence for a SULT4A1 haplotype correlating with baseline psychopathology and atypical antipsychotic response. Pharmacogenomics. 2011;12(4):471-480. PubMed doi:10.2217/pgs.10.205
8. Lieberman JA, Stroup TS, McEvoy JP, et al; Clinical Antipsychotic Trials of Intervention Effectiveness (CATIE) Investigators. Effectiveness of antipsychotic drugs in patients with chronic schizophrenia. N Engl J Med. 2005;353(12):1209-1223. PubMed doi:10.1056/NEJMoa051688
9. Sullivan PF, Lin D, Tzeng JY, et al. Genomewide association for schizophrenia in the CATIE study: results of stage 1. Mol Psychiatry. 2008;13(6):570-584. PubMed doi:10.1038/mp.2008.25
10. Need AC, Keefe RS, Ge D, et al. Pharmacogenetics of antipsychotic response in the CATIE trial: a candidate gene analysis. Eur J Hum Genet. 2009;17(7):946-957. PubMed doi:10.1038/ejhg.2008.264
11. van den Oord EJ, Adkins DE, McClay J, et al. A systematic method for estimating individual responses to treatment with antipsychotics in CATIE. Schizophr Res. 2009;107(1):13-21. PubMed doi:10.1016/j.schres.2008.09.009
12. McClay JL, Adkins DE, Aberg K, et al. Genome-wide pharmacogenomic study of neurocognition as an indicator of antipsychotic treatment response in schizophrenia. Neuropsychopharmacology. 2011;36(3):616-626. PubMed doi:10.1038/npp.2010.193
13. Center for Collaborative Genomic Studies on Mental Disorders Web site. https://www.nimhgenetics.org/. Accessed March 14, 2012.
14. Lin DY, Wei LJ. The robust inference for the Cox proportional hazards model. J Am Stat Assoc. 1989;184(408):1074-1078. doi:10.2307/2290085
15. Bigos KL, Bies RR, Pollock BG, et al. Genetic variation in CYP3A43 explains racial difference in olanzapine clearance. Mol Psychiatry. 2011;16(6):620-625. PubMed doi:10.1038/mp.2011.38
16. Liyou NE, Buller KM, Tresillian MJ, et al. Localization of a brain sulfotransferase, SULT4A1, in the human and rat brain: an immunohistochemical study. J Histochem Cytochem. 2003;51(12):1655-1664. PubMed doi:10.1177/002215540305101209
17. Allali-Hassani A, Pan PW, Dombrovski L, et al. Structural and chemical profiling of the human cytosolic sulfotransferases. PLoS Biol. 2007;5(5):e97. PubMed doi:10.1371/journal.pbio.0050097
18. Wong AH, Van Tol HH. Schizophrenia: from phenomenology to neurobiology. Neurosci Biobehav Rev. 2003;27(3):269-306. PubMed doi:10.1016/S0149-7634(03)00035-6
19. Kazadi NJB, Moosa MYH, Jeenah FY. Factors associated with relapse in schizophrenia. South African J Psychiatry. 2008;14(2):52-62.