Introduction: Bipolar disorder is affected by variables that modulate circadian rhythm, including seasonal variations. There is evidence of a seasonal pattern of admissions of mania in various geographical settings, though its timing varies by region and climate. Variables such as age and gender have been shown to affect seasonality in some studies.
Methodology: Data on monthly admission patterns for mania at a general hospital psychiatry unit in Pondicherry, India, were collected for 4 years (2010-2013) and analyzed for seasonality and seasonal peaks. The effects of age and gender were analyzed separately.
Results: There was overall evidence of a seasonal pattern of admissions for mania (P < .01, Friedman test for seasonality), with a peak beginning during the rainy season and ending before summer (P < .0.1, Ratchet circular scan test). Male sex (P < .005, Ratchet circular scan test) and age > 25 years (P < .005, Ratchet circular scan test) were specifically associated with this seasonal peak.
Discussion: The effect of seasons on mania is complex and is modulated by a variety of variables. Our study is consistent with earlier research findings: a greater degree of seasonality for mania in men. It is possible that climatic and individual variables interact to determine seasonal patterns in bipolar disorder in a given setting.
Seasonality of Admissions for Mania: Results From a
General Hospital Psychiatric Unit in Pondicherry, India
ABSTRACT
Introduction: Bipolar disorder is affected by variables that modulate circadian rhythm, including seasonal variations. There is evidence of a seasonal pattern of admissions of mania in various geographical settings, though its timing varies by region and climate. Variables such as age and gender have been shown to affect seasonality in some studies.
Methodology: Data on monthly admission patterns for mania at a general hospital psychiatry unit in Pondicherry, India, were collected for 4 years (2010–2013) and analyzed for seasonality and seasonal peaks. The effects of age and gender were analyzed separately.
Results: There was overall evidence of a seasonal pattern of admissions for mania (P < .01, Friedman test for seasonality), with a peak beginning during the rainy season and ending before summer (P < .0.1, Ratchet circular scan test). Male sex (P < .005, Ratchet circular scan test) and age > 25 years (P < .005, Ratchet circular scan test) were specifically associated with this seasonal peak.
Discussion: The effect of seasons on mania is complex and is modulated by a variety of variables. Our study is consistent with earlier research findings: a greater degree of seasonality for mania in men. It is possible that climatic and individual variables interact to determine seasonal patterns in bipolar disorder in a given setting.
Prim Care Companion CNS Disord 2015;17(3):doi:10.4088/PCC.15m01780
© Copyright 2015 Physicians Postgraduate Press, Inc.
Submitted: January 8, 2015; accepted March 2, 2015.
Published online: June 18, 2015.
Corresponding author: Ravi Philip Rajkumar, MD, Department of Psychiatry, Jawaharlal Institute of Postgraduate Medical Education and Research (JIPMER), Pondicherry–605 006, India
([email protected]).
Bipolar affective disorders have been linked on neurobiological and clinical grounds to disturbances of circadian rhythm.1,2 Variables that alter this rhythm—including seasonal variations in day length and sunlight exposure—may affect the onset3 and course4 of these disorders. It is estimated that about 23%–25% of patients diagnosed with bipolar disorder fulfill criteria for a seasonal pattern, though these data are mostly derived from countries with a temperate or cold climate.4–6
Seasonal variations in the course of mania have been reported from various countries, with a recent review finding evidence of seasonality in 23 of 29 relevant studies.7 Most of these studies have used data on hospital admissions for mania as a measure of seasonality and have yielded variable results depending on their geographical location. A summer peak of admissions for mania has been reported in the United Kingdom,8 Ireland,9 Australia,10 and Taiwan,11 while a slightly earlier peak in spring has been noted in the United States12 and a late winter to spring peak has been reported in Brazil.13,14 On the other hand, some studies have failed to find an overall seasonal pattern,15–17 including a multicentric study covering both the northern and southern hemispheres.18 Variables such as age and gender have been found to affect the seasonality of mania in some samples, with a seasonal pattern reported to be more prominent in younger patients.11 The association of gender with seasonality has yielded mixed results, with a prominent seasonal pattern noted in men in 1 study,11 and in women in another.17
Various factors confound the interpretation of these results. First, there is some evidence that mixed manias may differ from “pure” mania in terms of seasonal variation: a summer peak for mixed—but not pure—mania has been found in data from the United States12 and Canada.16 Second, patient variables such as age and gender may affect seasonality: mania may have a more seasonal pattern in men than in women,11 though the opposite has also been found.17 Similarly, seasonality has been found to be more prominent in younger patients.11 Third, published studies cover a wide range of geographical areas, with marked variations in seasons, climate, rainfall, and sunlight exposure. These variables have also been shown to influence the occurrence of mania.9,13,14,19
Using data from the World Mental Health Survey,20 it is estimated that about 1 million people in India suffer from bipolar spectrum disorders; however, few studies have examined the seasonality of mania in this setting. A study from a South India center found no evidence of seasonality in admissions for mania at a mental health institute.15 However, individual cases of seasonal bipolar disorder have been reported,21 and studies from North India regions, where there is a well-defined winter and large temperature variations across seasons, have found some evidence of seasonality.22,23 As there are significant variations in relevant climatic variables across India, it is unlikely that these results would apply uniformly to other parts of the country. Several regions in South India, including Pondicherry, have no winter per se; rather, there is a long summer followed by a rainy season, with low temperature variation across the year. It is possible that seasonal variations in the course of bipolar disorder would be dampened or minimal in such conditions; however, we cannot rule out a moderating effect of variables other than temperature, such as sunlight exposure or rainfall.24,25 Moreover, seasonality in bipolar disorder has also been reported in regions with low temperature variation.26 In this article, we carried out a preliminary investigation of these factors by examining seasonal variations in admissions for mania at a general hospital psychiatry unit in Pondicherry, South India. In line with the findings discussed above, we also examined the effects of gender and age on seasonality.
METHOD
We obtained information on all inpatient admissions with a diagnosis of manic episode (ICD-10 code F30.1 or F30.2) or bipolar affective disorder, current episode mania (ICD-10 code F31.1 or F31.2) at a general hospital psychiatric unit in Pondicherry over a period of 4 years (2010 to 2013). Pondicherry is a town in South India, located at 11° 56’ north latitude and 79° 53’ east longitude. The catchment area for the hospital includes the town itself and towns and villages in the neighboring state of Tamil Nadu with an approximate radius of 100 km. The climate of Pondicherry is type A (tropical wet and dry) according to the Koppen-Geiger classification.27 The variation of temperatures across the year is relatively low, with a daily mean temperature difference of 46.4°F (8°C) between summers and winters.
The general hospital psychiatry unit in which this study was conducted offers both inpatient and outpatient services. Inpatient care is generally provided to patients at risk of harming themselves or others or when outpatient treatment has failed; most admissions are short-term, lasting 2 to 4 weeks. The mean number of admissions per year for the study period was 495 patients (range, 470–519 patients). All admission diagnoses are made by a trained psychiatrist using the ICD-10 Clinical Descriptions and Diagnostic Guidelines,28 following a focused evaluation and a review of existing case records if available. Information on the age, gender, and diagnosis of the patient is entered verbatim in the psychiatry ward register by the staff nurse on duty and was used as the source of data for this study.
We did not include data on patients with a diagnosis of schizoaffective disorder or those for whom the admission diagnosis was recorded as being uncertain—that is, where mania was considered as a differential diagnosis but other possibilities, such as acute psychosis or schizophrenia, were also documented. A total of 59 cases were excluded for this reason. As at least 1 provisional diagnosis is entered for all admissions, no case was excluded on the grounds of missing data. Numbers of admissions were tabulated per month for each year of the study period. Information on men, women, and young adults (defined for the purpose of this study as those aged ≤ 25 years) was recorded separately. We did not attempt to assess seasonality of admissions for depressive or mixed episodes, as the total number of such cases was low (26 combined), precluding meaningful statistical analysis. No patients were admitted for a hypomanic episode during the study period.
Data were combined and analyzed for seasonal variations using the WINPEPI software package for statistical analysis.29 As there was no increase in the number of cases over time, data on admissions for mania were pooled for each month and then analyzed. Friedman test, a variant of the Kolomogorov-Smirnov test, was used to assess overall deviations from a uniform monthly distribution. Ratchet circular scan test, which compares the number of events in each period of a short length, was used to identify short (2- to 3-month) peaks in admissions for mania. Hewitt’s test ranks monthly totals of events and uses rank sums to identify long (4- to 6-month) seasonal peaks. A value of P < .05 was considered significant for the purpose of this study.
RESULTS
We obtained information on a total of 357 admissions for mania out of a total of 1,978 admissions in the period 2010–2013. The mean number of admissions per year for mania was 89.25 (range, 82–98), with a peak of 98 in the year 2010; there was a trend toward a slight decrease in admissions over time, from 98 in 2010 to 82 in 2013, but this was not statistically significant (P > .2, runs test). There was a total of 204 male and 153 female admissions in the sample. Among these, 135 patients (37.8%, 71 men, 64 women) were young adults aged < 25 years. There was no significant difference in gender proportions between the young adult group and the rest of the sample (women: 64/135 vs 92/222, χ2 = 1.294, P = .26).
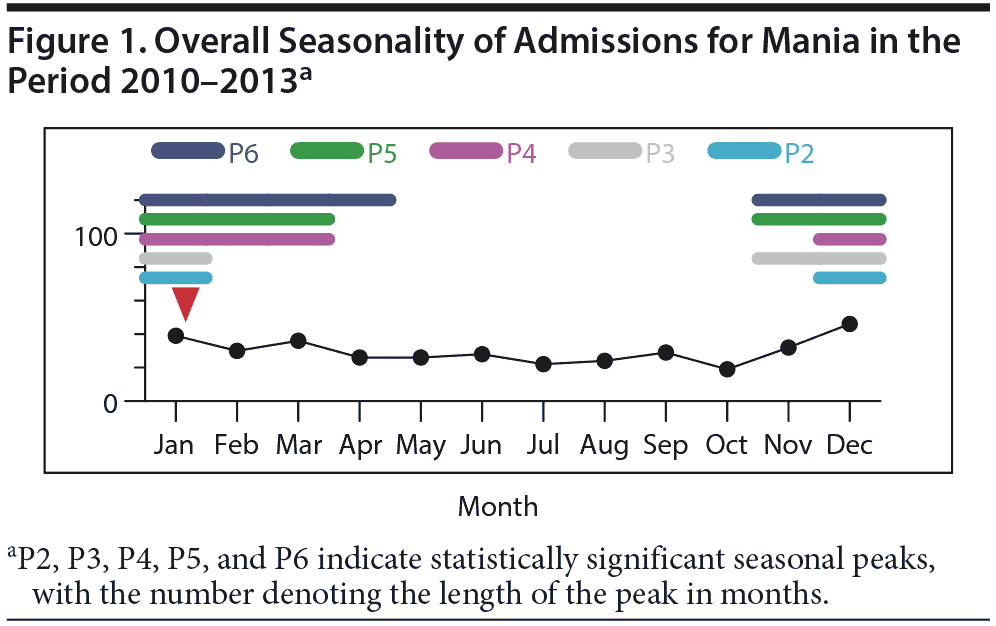
The overall sample of 357 admissions for mania showed statistically significant evidence of seasonal variation (V[n] = 0.099, P < .01, Friedman test). There was highly significant evidence for a 3-month peak of admissions between November and January, covering 32.8% of all admissions (P < .01, Ratchet circular scan test). Hewitt’s rank sum test for a long seasonal peak yielded the most significant results for a 5-month peak between November and March (rank sum = 50, P = .015) (Figure 1).
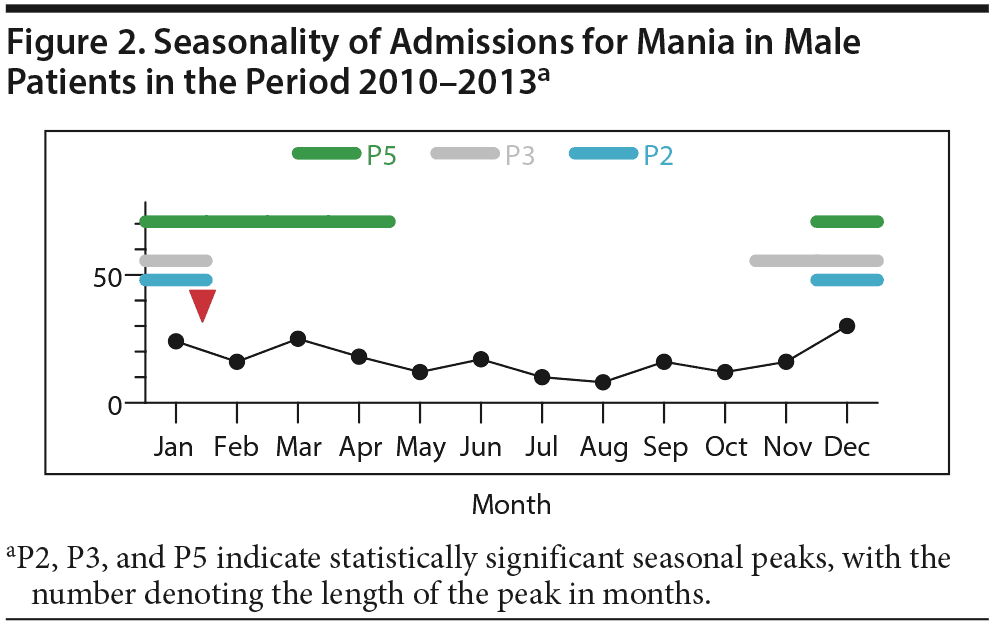
When data for male and female patients were analyzed separately, there was no significant evidence of seasonality in women (P > .1, Friedman test), and no long or short seasonal peak could be identified. However, male patients showed significant evidence of seasonal variation (V[n] = 0.140, P < .01, Friedman test). There was significant evidence for a unique 2-month peak of admissions in men (December and January), accounting for 26.5% of admissions (P < .005, Ratchet circular scan test). Hewitt’s rank sum test for a long seasonal peak was most significant for a 5-month peak between December and April (rank sum = 49, P = .029) (Figure 2).
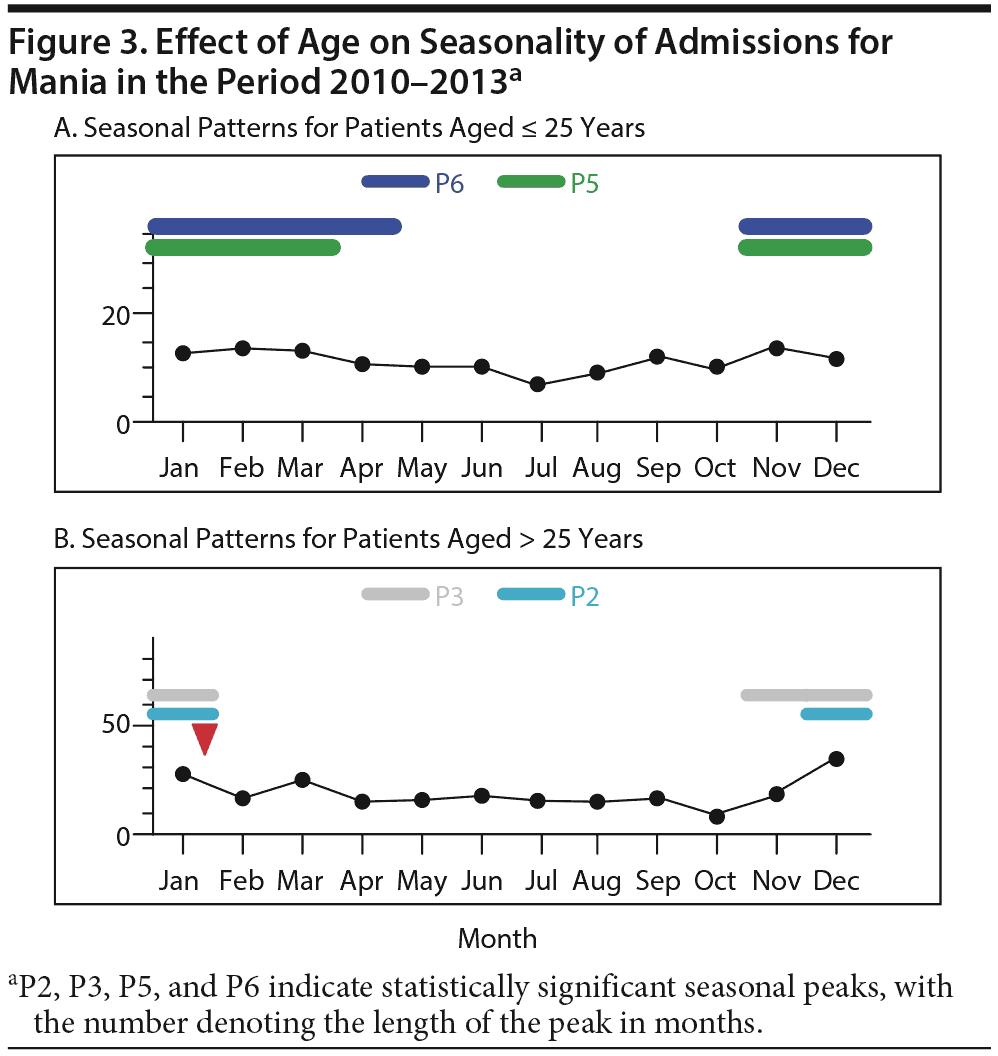
When patients below and above 25 years of age were compared, there was no significant evidence of overall seasonal variation in younger patients (P > .1, Friedman test); however, there was some evidence for a 5-month peak of admissions between November and March (rank sum = 49, P = .029) and a 6-month peak between November and April (rank sum = 55, P = .048). On the other hand, there was stronger evidence of seasonal variation in patients over age 25 (V[n] = 0.116, P < .01, Friedman test), with a significant 2-month peak in December and January covering 26.9% of admissions (P < .005, Ratchet circular scan test) and a 3-month peak from November to January covering 35% of admissions (P < .01, Ratchet circular scan test) but no evidence of a longer peak period for admissions (Figure 3A and B).
When we examined data for each individual year, a clear seasonal pattern was seen for the year 2012 (V[n] = 0.156, P < .05, Friedman test), with significant 3-month (December to February, P < .05, Ratchet circular scan test) and 4-month (December to March, P = .047, Hewitt rank sum test) peaks, which were similar to those for the entire sample. Though similar peaks were found for the other years, they did not reach statistical significance. We could not reliably compare male and female seasonal patterns by year due to the small numbers involved, though there was evidence of a seasonal pattern for male admissions in the year 2013 (P < .05, Friedman test; however, the number of events was 45, and Friedman test requires at least 50 events to yield a reliable result).
DISCUSSION
There was statistically significant evidence of seasonality in the entire sample of admissions for mania, with a 3-month peak between November and January and a 5-month peak between November and March. In Pondicherry, where there is no well-defined winter, the short peak corresponds to the time of maximum rainfall, the northeast monsoon; during this period, day lengths are shorter by about 60 to 90 minutes, and mean temperatures are lower by about 8 degrees. The long peak covers this period and extends it to the onset of summer in the month of March, when temperatures begin to rise significantly and days are longer. Such a pattern suggests that the onset of mania could be related either to lower temperatures or to changes in daily temperature; earlier studies have found that certain symptoms of bipolar disorder may be influenced by changes in temperature24,25 or sunlight exposure.25
Our findings are in sharp contrast with results from Brazil, where a negative correlation was found between rainfall and admissions for mania,14 and Ireland, where day length was positively correlated with admissions for mania.9 Our November–March peak is the opposite of the summer peak of admissions that has been reported in the United Kingdom,8 Ireland,9 and Australia.10 An intermediate peak, covering spring and summer, has been reported in New Zealand.30 These results suggest that a simple linear relationship between climatic variables and the onset of mania is unlikely and may be modulated by other factors. However, there are no significant psychosocial factors, such as local festivals or traditions, which could specifically account for this seasonal variation by modifying activity levels or the intake of substances such as alcohol; although the seasonal peak encompasses the beginning of a new year, this is not a period specifically marked by such changes in Pondicherry.
When comparing men and women, we found stronger evidence of seasonal variation in men, which was broadly comparable to the findings for the entire sample. As our sample had a male preponderance (male to female ratio = 1.33:1), it is likely that this factor accounted for the sample findings overall. This finding replicates the results of a study from Taiwan, which found that seasonality was stronger for mania in men.11 A summer peak for mania was found for women in a sample from England,17 whereas women in our study had no seasonal variation. This finding suggests that gender and climatic variables may interact to determine seasonal patterns in bipolar disorder. There is evidence that estrogen and progesterone can modulate circadian rhythms and that these mechanisms may be relevant to affective disorders,31,32 including bipolar disorder.33 Such effects have not been reported in the literature for testosterone, though diurnal testosterone levels are reduced in depressed men.34 Such explanations must be considered tentative and provisional, as systematic studies of gonadal hormones and their relationship to seasonality in bipolar disorder have not been conducted.
Patients who were older than 25 years showed a seasonal pattern that was roughly similar to the entire sample, except for the absence of a clear long peak; such a pattern was not seen in those below age 25 years. This finding is in contrast with a study from Taiwan that found that seasonality was more prominent in young adults.11 These differences may be accounted for by methodological variations, such as a larger sample size and different statistical methods employed, or by a genuine variation caused by climatic factors. Alternately, seasonality may develop gradually over the course of bipolar disorder, in a manner similar to the gradual emergence of a stable cycle length,35 though this possibility has to be tested in prospective studies.
Our results contradict those of another study from India, which found no evidence of seasonality in admissions for mania over a 9-year period.15 However, the earlier study was conducted in a different region of South India, characterized by a higher altitude, rainfall from June to September (the southwest monsoon), and a lower year-wide variation in temperature; these variations in climate may account for the differences observed. A study from North India found a trend toward more frequent admissions for mania in the rainy season and in winter, overlapping to some extent with our findings22; older studies in this setting have found a summer peak, though they have been based on selected clinical samples rather than the total number of admissions.36
Our study is subject to certain limitations. First, data were obtained from a hospital register: index diagnoses may have changed over time in some patients, though the diagnostic stability of bipolar disorder is generally high.37 Second, the format in which data were entered did not permit a distinction between first episodes of mania, recurrent (“unipolar”) mania, and mania accompanied by depression. Such a distinction may have an impact on seasonality, as shown by earlier research that found a summer peak for unipolar manias in Australia10 and a March peak for first manic episodes in Korea.19 Third, we combined data for a period of 4 years, and clear evidence of seasonality in individual years was found only for 1 year (2012); however, this may result from the relatively low number of admissions per year (82 to 98). Fourth, we did not correct for factors such as humidity, mean temperature, and rainfall, which may have affected the results.9,13,14,19 Fifth, we used a lower age cutoff than an earlier study (25 years vs 35 years)11 to define our sample of young adults; this was done so that the young adult sample would represent adolescents and young adults with bipolar disorder, but may have affected the result. Sixth, we used admissions for mania as a surrogate measure of seasonality. Although this method is widely used in the literature,7 it fails to take into account patients with milder episodes not requiring admission, and it may lead to a miscalculation of the seasonal period, as patients may have been ill for several weeks prior to admission. Seventh, we did not distinguish between psychotic and nonpsychotic mania; there is some evidence that psychotic symptoms may have a distinctive seasonal pattern in bipolar disorder.25 Finally, the year 2011 in Pondicherry was marked by unusually heavy rainfall, including a cyclone in late December38 that caused significant local damage. This event may have triggered manic episodes by social, rather than biological, mechanisms; however, we did not find clear evidence of seasonality when this year was considered alone, which mitigates against this explanation.
Despite these limitations, this study highlights the need to further examine the impact of age and gender—and their interactions with climatic variables—on the seasonality of bipolar disorder. A cautious interpretation of our results suggests that mania admissions peak around a period of greater rainfall and shorter day length,1 and seasonality in mania may be more marked in men and in patients aged > 25.2 Elucidation of the mechanisms underlying these phenomena might shed more light on the processes involved in seasonality in bipolar disorder and their potential therapeutic implications.
Author affiliations: Department of Psychiatry, Jawaharlal Institute of Postgraduate Medical Education and Research (JIPMER), Pondicherry, India.
Potential conflicts of interest: None reported.
Funding/support: None reported.
REFERENCES
1. Gonzalez R. The relationship between bipolar disorder and biological rhythms. J Clin Psychiatry. 2014;75(4):e323–e331. doi:10.4088/JCP.13r08507 PubMed
2. McClung CA. How might circadian rhythms control mood? Let me count the ways. . . . Biol Psychiatry. 2013;74(4):242–249. doi:10.1016/j.biopsych.2013.02.019 PubMed
3. Bauer M, Glenn T, Alda M, et al. Impact of sunlight on the age of onset of bipolar disorder. Bipolar Disord. 2012;14(6):654–663. doi:10.1111/j.1399-5618.2012.01025.x PubMed
4. Geoffroy PA, Bellivier F, Scott J, et al. Bipolar disorder with seasonal pattern: clinical characteristics and gender influences. Chronobiol Int. 2013;30(9):1101–1107. doi:10.3109/07420528.2013.800091 PubMed
5. Faedda GL, Tondo L, Teicher MH, et al. Seasonal mood disorders: patterns of seasonal recurrence in mania and depression. Arch Gen Psychiatry. 1993;50(1):17–23. doi:10.1001/archpsyc.1993.01820130019004 PubMed
6. Schaffer A, Levitt AJ, Boyle M. Influence of season and latitude in a community sample of subjects with bipolar disorder. Can J Psychiatry. 2003;48(4):277–280. PubMed
7. Wang B, Chen D. Evidence for seasonal mania: a review. J Psychiatr Pract. 2013;19(4):301–308. doi:10.1097/01.pra.0000432600.32384.c5 PubMed
8. Myers DH, Davies P. The seasonal incidence of mania and its relationship to climatic variables. Psychol Med. 1978;8(3):433–440. doi:10.1017/S003329170001610X PubMed
9. Carney PA, Fitzgerald CT, Monaghan CE. Influence of climate on the prevalence of mania. Br J Psychiatry. 1988;152(6):820–823. doi:10.1192/bjp.152.6.820 PubMed
10. Jones I, Hornsby H, Hay D. Seasonality of mania: a Tasmanian study. Aust N Z J Psychiatry. 1995;29(3):449–453. doi:10.3109/00048679509064953 PubMed
11. Yang AC, Yang CH, Hong CJ, et al. Effects of age, sex, index admission, and predominant polarity on the seasonality of acute admissions for bipolar disorder: a population-based study. Chronobiol Int. 2013;30(4):478–485. doi:10.3109/07420528.2012.741172 PubMed
12. Cassidy F, Carroll BJ. Seasonal variation of mixed and pure episodes of bipolar disorder. J Affect Disord. 2002;68(1):25–31. doi:10.1016/S0165-0327(00)00325-6 PubMed
13. Volpe FM, Del Porto JA. Seasonality of admissions for mania in a psychiatric hospital of Belo Horizonte, Brazil. J Affect Disord. 2006;94(1-3):243–248. doi:10.1016/j.jad.2006.03.025 PubMed
14. Volpe FM, da Silva EM, dos Santos TN, et al. Further evidence of seasonality of mania in the tropics. J Affect Disord. 2010;124(1–2):178–182. doi:10.1016/j.jad.2009.11.001 PubMed
15. Jain S, Kaliaperumal VG, Chatterji S, et al. Climate and admissions for mania in the tropics. J Affect Disord. 1992;26(4):247–250. doi:10.1016/0165-0327(92)90102-C PubMed
16. Whitney DK, Sharma V, Kueneman K. Seasonality of manic depressive illness in Canada. J Affect Disord. 1999;55(2–3):99–105. doi:10.1016/S0165-0327(98)00197-9 PubMed
17. Suhail K, Cochrane R. Seasonal variations in hospital admissions for affective disorders by gender and ethnicity. Soc Psychiatry Psychiatr Epidemiol. 1998;33(5):211–217. doi:10.1007/s001270050045 PubMed
18. Bauer M, Glenn T, Grof P, et al. Relationship among latitude, climate, season and self-reported mood in bipolar disorder. J Affect Disord. 2009;116
(1–2):152–157. doi:10.1016/j.jad.2008.11.013 PubMed
19. Lee HJ, Kim L, Joe SH, et al. Effects of season and climate on the first manic episode of bipolar affective disorder in Korea. Psychiatry Res. 2002;113
(1–2):151–159. doi:10.1016/S0165-1781(02)00237-8 PubMed
20. Merikangas KR, Jin R, He JP, et al. Prevalence and correlates of bipolar spectrum disorder in the World Mental Health Survey initiative. Arch Gen Psychiatry. 2011;68(3):241–251. doi:10.1001/archgenpsychiatry.2011.12 PubMed
21. Jain S, Mazumdar P, Chatterji S, et al. Seasonal relapses in affective disorder in the Tropics: a prospective follow-up of 12 patients. Psychopathology. 1992;25(3):166–172. doi:10.1159/000284768 PubMed
22. Avashthi A, Sharma A, Gupta N, et al. Seasonality and unipolar recurrent mania: preliminary findings from a retrospective study. Indian J Psychiatry. 1996;38(4):236–239. PubMed
23. Margoob MA, Dutta KS. 10–15 years retrospective study of 50 patients of mdp for seasonal variations. Indian J Psychiatry. 1988;30(3):253–256. PubMed
24. Christensen EM, Larsen JK, Gjerris A, et al. Climatic factors and bipolar affective disorder. Nord J Psychiatry. 2008;62(1):55–58. doi:10.1080/08039480801970049 PubMed
25. Volpe FM, Tavares A, Del Porto JA. Seasonality of three dimensions of mania: psychosis, aggression and suicidality. J Affect Disord. 2008;108
(1–2):95–100. doi:10.1016/j.jad.2007.09.014 PubMed
26. Lee HC, Tsai SY, Lin HC. Seasonal variations in bipolar disorder admissions and the association with climate: a population-based study. J Affect Disord. 2007;97(1–3):61–69. doi:10.1016/j.jad.2006.06.026 PubMed
27. Peel MC, Finlayson BL. Updated world map of the Koppen-Geiger climate classification. Hydrol Earth Syst Sci. 2007;11(5):1633–1644. doi:10.5194/hess-11-1633-2007
28. World Health Organization. ICD-10 Clinical Descriptions and Diagnostic Guidelines. http://www.who.int/substance_abuse/terminology/icd_10/en/. Accessed May 13, 2015.
29. Abramson JH. WINPEPI updated: computer programs for epidemiologists, and their teaching potential. Epidemiol Perspect Innov. 2011;8(1):1. doi:10.1186/1742-5573-8-1 PubMed
30. Mulder RT, Cosgriff JP, Smith AM, et al. Seasonality of mania in New Zealand. Aust N Z J Psychiatry. 1990;24(2):187–190. doi:10.3109/00048679009077681 PubMed
31. Shechter A, Lespérance P, Ng Ying Kin NM, et al. Pilot investigation of the circadian plasma melatonin rhythm across the menstrual cycle in a small group of women with premenstrual dysphoric disorder. PLoS ONE. 2012;7(12):e51929. doi:10.1371/journal.pone.0051929 PubMed
32. Posadas ES, Meliska CJ, Martinez LF, et al. The relationship of nocturnal melatonin to estradiol and progesterone in depressed and healthy pregnant women. J Womens Health (Larchmt). 2012;21(6):649–655. doi:10.1089/jwh.2011.3191 PubMed
33. Kim DR, Czarkowski KA, Epperson CN. The relationship between bipolar disorder, seasonality, and premenstrual symptoms. Curr Psychiatry Rep. 2011;13(6):500–503. doi:10.1007/s11920-011-0233-z PubMed
34. Schweiger U, Deuschle M, Weber B, et al. Testosterone, gonadotropin, and cortisol secretion in male patients with major depression. Psychosom Med. 1999;61(3):292–296. doi:10.1097/00006842-199905000-00007 PubMed
35. Angst J, Sellaro R. Historical perspectives and natural history of bipolar disorder. Biol Psychiatry. 2000;48(6):445–457. doi:10.1016/S0006-3223(00)00909-4 PubMed
36. Avasthi A, Sharma A, Gupta N, et al. Seasonality and affective disorders: a report from North India. J Affect Disord. 2001;64(2–3):145–154. doi:10.1016/S0165-0327(00)00239-1 PubMed
37. Bromet EJ, Kotov R, Fochtmann LJ, et al. Diagnostic shifts during the decade following first admission for psychosis. Am J Psychiatry. 2011;168(11):1186–1194. doi:10.1176/appi.ajp.2011.11010048 PubMed
38. India Meteorological Department, Ministry of Earth Sciences, Government of India. Very severe cyclonic storm “Thane” over the Bay of Bengal (December 25–31, 2011): a report. http://www.imd.gov.in/section/nhac/dynamic/THANE.pdf. Accessed April 6, 2015.
Enjoy this premium PDF as part of your membership benefits!


