Objective: To investigate the self-esteem and defense mechanisms in patients diagnosed with human immunodeficiency virus (HIV)/acquired immune deficiency syndrome (AIDS).
Methods: This prospective, cross-sectional study included 29 patients diagnosed with HIV/AIDS admitted to inpatient or outpatient clinics between March 2018 and January 2019 and 29 healthy subjects. Participants were assessed using a sociodemographic and clinical data form, the Rosenberg Self-Esteem Inventory (RSEI), the Defense Style Questionnaire (DSQ), and the Beck Anxiety Inventory.
Results: Patients with HIV/AIDS had significantly higher scores on the fantasy, psychosomatic symptoms, and parental interest subscales of the RSEI. There was no significant difference between the groups on the other subscales, including the self-esteem subscale. There was no correlation between the duration of the disease and self-esteem. The neurotic defense mechanism and immature defense mechanism subscale scores of the DSQ were significantly higher in the HIV/AIDS group compared to the control group (P < .01). Undoing and reaction formation scores in neurotic defense mechanisms and projection, devaluation, autistic fantasy, and splitting scores in immature defense mechanisms were significantly higher in the HIV/AIDS group compared to controls (P < .05). There was no significant difference between the groups based on the mature defense mechanisms subscale scores.
Conclusions: No difference was found in the self-esteem scores of the HIV/AIDS and control groups, and this finding could be associated with the stability of the self-esteem concept. It was also determined that patient group members utilized neurotic and immature defense mechanisms more often compared to the healthy group, and there was no difference between the groups based on mature defense mechanisms.
ABSTRACT
Objective: To investigate the self-esteem and defense mechanisms in patients diagnosed with human immunodeficiency virus (HIV)/acquired immune deficiency syndrome (AIDS).
Methods: This prospective, cross-sectional study included 29 patients diagnosed with HIV/AIDS admitted to inpatient or outpatient clinics between March 2018 and January 2019 and 29 healthy subjects. Participants were assessed using a sociodemographic and clinical data form, the Rosenberg Self-Esteem Inventory (RSEI), the Defense Style Questionnaire (DSQ), and the Beck Anxiety Inventory (BAI).
Results: Patients with HIV/AIDS had significantly higher scores on the fantasy, psychosomatic symptoms, and parental interest subscales of the RSEI. There was no significant difference between the groups on the other subscales, including the self-esteem subscale. There was no correlation between the duration of the disease and self-esteem. The neurotic defense mechanism and immature defense mechanism subscale scores of the DSQ were significantly higher in the HIV/AIDS group compared to the control group (P < .01). Undoing and reaction formation scores in neurotic defense mechanisms and projection, devaluation, autistic fantasy, and splitting scores in immature defense mechanisms were significantly higher in the HIV/AIDS group compared to controls (P < .05). There was no significant difference between the groups based on the mature defense mechanisms subscale scores.
Conclusions: No difference was found in the self-esteem scores of the HIV/AIDS and control groups, and this finding could be associated with the stability of the self-esteem concept. It was also determined that patient group members utilized neurotic and immature defense mechanisms more often compared to the healthy group, and there was no difference between the groups based on mature defense mechanisms.
Prim Care Companion CNS Disord 2020;22(2):19m02577
To cite: Baykara S, Tartar AS, Korucu T, et al. Self-esteem and defense mechanisms in HIV-positive and AIDS patients. Prim Care Companion CNS Disord. 2020;22(2):19m02577.
To share: https://doi.org/10.4088/PCC.19m02577
© Copyright 2020 Physicians Postgraduate Press, Inc.
aDepartment of Psychiatry, Faculty of Medicine, Fırat University, Elazig, Turkey
bDepartment of Infectious Diseases and Clinical Microbiology, Faculty of Medicine, Fırat University, Elazig, Turkey
*Corresponding author: Sema Baykara, MD, Department of Psychiatry, Firat University Hospital, 23119 Elazig, Turkey ([email protected]).
Acquired immune deficiency syndrome (AIDS) is a serious health problem. In 2018, the World Health Organization reported that approximately 37.9 million people worldwide were living with the human immunodeficiency virus (HIV)/AIDS.1 The diagnosis of HIV can trigger a significant traumatic impact on the patient since it involves long-term social, physical, and psychological problems that might ultimately result in death. Emotional reactions such as fear, guilt, embarrassment, and uncertainty may be observed in individuals recently diagnosed with HIV.2
Self-esteem is the determination of self-worth and social importance of an individual as a social object.3 Individuals with high self-esteem consider themselves smart, attractive, and popular.4 Although they may have made mistakes or had flaws in the past, those with high self-esteem evaluate their current or recent past assessments with a positive perspective, despite contrary views, and believe they have changed in a positive way.5 Their thoughts on the future are more positive and they exhibit higher confidence when they encounter failure compared to individuals with low self-esteem.6
The diagnosis of HIV could impend on self-esteem. A decrease in self-esteem due to disease stigmatization is common during the course of the disease.7 However, a study8 found that while some patients experienced a decrease in self-esteem after HIV diagnosis, others did not, indicating the presence of other factors in these patients that led to more positive outcomes despite adverse conditions.9
A correlation between defense mechanisms and a higher rate of adjustment to life conditions and resulting decrease in the rate of psychiatric disorders has been reported in patients with HIV/AIDS10; however, research in this regard is limited. The present study aimed to investigate the self-esteem and defense mechanisms in patients living with HIV/AIDS.
METHODS
Study Design
This prospective, cross-sectional, descriptive study compared a clinical population of HIV-positive adults to a control group. Thirty-eight patients with HIV (confirmed by Western Blot test) admitted to inpatient or outpatient clinics at the Department of Infectious Diseases and Clinical Microbiology (Fırat University, Elazig, Turkey) between March 2018 and January 2019 were identified. Of these patients, 5 refused to participate and 4 were excluded as they did not meet the study criteria, thus a total of 29 patients were included in the study. The inclusion criteria for the study group included age between 18 and 65 years, ability to read and write, HIV diagnosis, and no neurologic disorders, significant physical pathology, or physiologic disease that could exacerbate the symptoms that were already present. The control group comprised 29 healthy subjects with similar demographics who met the inclusion criteria (with the exception of HIV diagnosis) and included members of the hospital staff or hospital attendants who volunteered to participate.
The study was approved by the local ethics committee (01.03.2018–05–19) and conducted in accordance with the Declaration of Helsinki.11 Written informed consent forms were signed by all participants.
All participants completed a sociodemographic and clinical data form, the Rosenberg Self-Esteem Inventory (RSEI),12 the Defense Style Questionnaire (DSQ),13 and the Beck Anxiety Inventory (BAI).14 The questionnaires were administered during clinical interviews by a senior psychiatric assistant (T.K.).
Sociodemographic and Clinical Data Form
The sociodemographic and clinical data form was developed based on the study objectives, relevant information obtained via literature review, and previous clinical experience. This semistructured form included sociodemographic information, such as age, sex, marital status, education level, occupation, and income level, and clinical data such as duration of HIV, number of hospitalizations due to HIV, and presence of psychosocial assistance.
Rosenberg Self-Esteem Inventory
The RSEI was developed to determine self-esteem in adolescents. The RSEI has been used in studies15,16 conducted with adult psychiatric patients and is a valid instrument. The scale includes 63 questions in 12 subscales. These subscales include self-esteem, continuity of self-concept, trust, sensitivity to criticism, depressive affection, fantasy, psychosomatic symptoms, threatened by interpersonal relations, participation in discussions, parental interest, paternal relationship, and psychic isolation.
Defense Style Questionnaire
The DSQ is a self-evaluation scale that includes 40 items and 20 defenses. The questionnaire is used to experimentally assess the reflections of unconscious defense mechanisms on consciousness levels. Each item is evaluated on a scale of 1 (not applicable at all) to 9 (completely applicable). The 20 defense mechanisms included in the scale were categorized under 3 dimensions: the immature, neurotic, and mature defenses. Immature defenses include mechanisms such as projection, passive aggression, acting out, isolation, devaluation, autistic fantasy, denial, displacement, dissociation, splitting, rationalization, and somatization. Neurotic defenses include undoing, artificial altruism, idealization, and reaction, and mature defenses comprise sublimation, humor, anticipation, and suppression.
Beck Anxiety Inventory
The BAI is used to determine the frequency of anxiety symptoms in individuals. The inventory includes 21 items evaluated on a 3-point Likert-type scale.
Statistical Analysis
The study data were analyzed with SPSS version 22 (IBM Corp, Chicago, Illinois). Descriptive statistics, such as frequencies and percentages for categorical variables and mean ± SD for continuous variables, were used to describe baseline demographic data and clinical characteristics. The variables were investigated using visual (histograms, probability plots) and analytic methods (Shapiro-Wilk test) to determine whether the distribution was normal. The χ2 test was used for the comparison of categorical variables. Mann-Whitney U test or student t test were used to compare continuous variables on the basis of the normality of the data. Pearson correlation coefficient was used to investigate associations between the scores. The significance level was P < .05.
RESULTS
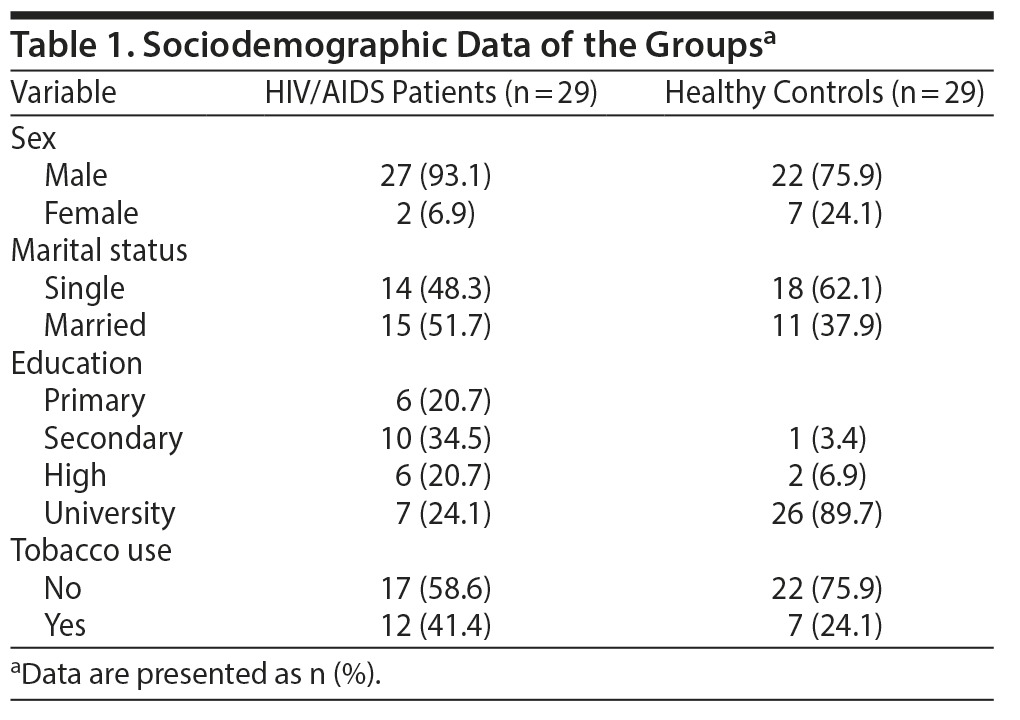
The mean ± SD age was 34.62 ± 10.25 years in the HIV/AIDS group and 30.86 ± 9.43 years in the control group. Twenty-seven (93.1%) patients and 22 (75.9%) controls were men. There were no significant differences between the 2 groups based on age (P = .152), sex (P = .070), marital status (P = .291), or smoking (P = .162). The mean postdiagnosis period was 17.48 ± 31.50 months, and the mean treatment period was 15.83 ± 28.34 months. In the HIV/AIDS group, analysis of the psychiatric disease history data revealed that 17 (58.6%) had no psychiatric diagnosis, while 9 (31%) were diagnosed with anxiety disorder, 2 (6.9%) with depressive disorder, and 1 (3.4%) with mixed anxiety depressive disorder. The sociodemographic data of the HIV/AIDS group are presented in Table 1.
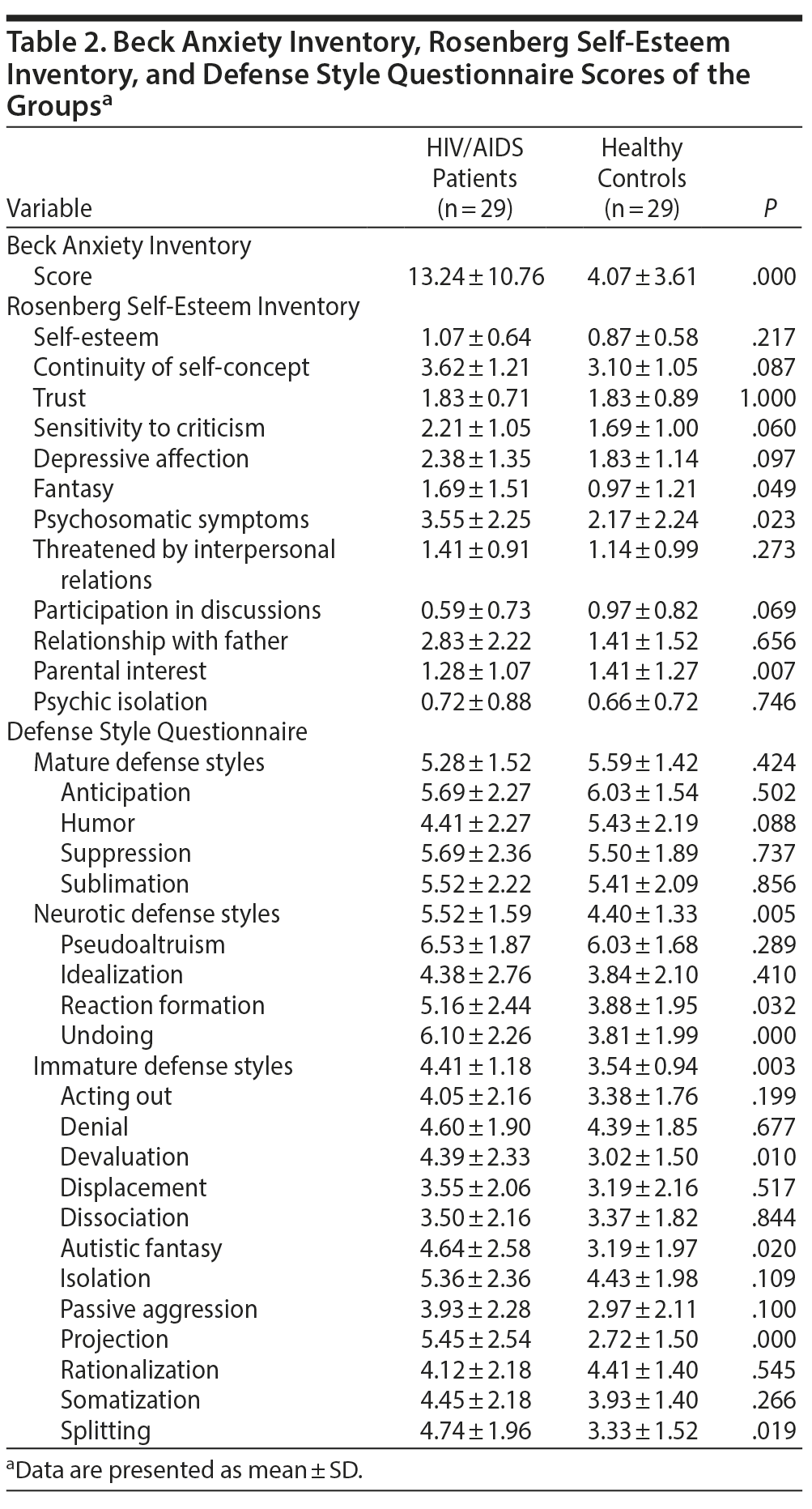
HIV/AIDS patients had significantly higher scores compared to controls on the fantasy (1.69 ± 1.51 vs 0.97 ± 1.21, P = .049), psychosomatic symptoms (3.55 ± 2.25 vs 2.17 ± 2.24, P = .023), and parental interest (2.83 ± 2.22 vs 1.41 ± 1.52, P = .007) subscale scores of the RSEI. There was no significant difference between the groups on the other subscales, including the self-esteem subscale (P = .217). No correlation was determined between disease duration and self-esteem (P = .566, r = 0.111).
The HIV/AIDS group had significantly higher scores compared to controls on the DSQ neurotic defense mechanisms (5.52 ± 1.60 vs 4.40 ± 1.33, P = .005) and immature defense mechanisms (4.41 ± 1.18 vs 3.54 ± 0.94, P = .003). Neurotic defense mechanisms undoing and reaction formation subscale scores (P = .000 and P = .032, respectively) and immature defense mechanisms projection, devaluation, autistic fantasy, and splitting subscale scores (P = .000, P = .010, 0.020, and 0.019, respectively) were significantly higher in the patient group. There was no statistically significant difference between the mature defense mechanisms subscale scores of the 2 groups (P = .424). It was determined that the patient group’s BAI scores were significantly higher compared to the control group (13.24 ± 10.76 vs 4.07 ± 3.61, P = .000). The RSEI, DSQ, and BAI scores are presented in Table 2.
After the correlation between the RSEI and DSQ was analyzed, it was determined that an increase in the trust subscale scores resulted in a decrease in the mature defense mechanisms and neurotic defense mechanisms scores (r = −0.389, P = .037 and r = −0.481, P = .008, respectively), and increases in the fantasy and parental interest subscale scores led to an increase in the immature defense mechanisms scores (r = 0.576, P = .001 and r = 0.638, P = .000, respectively).
DISCUSSION
The present study revealed a significant difference in the RSEI fantasy, psychosomatic symptoms, and parental interest subscale scores: these scores were higher in the HIV/AIDS group. However, there was no significant difference in self-esteem subscale scores of HIV/AIDS patients compared to those of healthy controls. Neurotic and immature defense mechanisms were used more frequently by the HIV/AIDS group compared to the control group; however, there was no difference between the groups based on mature defense mechanisms. BAI scores were significantly higher in the patient group.
A seropositive HIV diagnosis significantly affects patients due to psychological, medical, and social consequences. A study conducted by Pedersen and Elklit10 that investigated defense mechanisms during trauma indicated that patients diagnosed with HIV/AIDS presented significant trauma and stress symptoms. Factors such as the progressive and destructive nature of the disease, stigmatization of these patients by society, and a decrease in self-esteem could lead to the psychosocial stress experienced by HIV/AIDS patients.2,17 Individuals with low self-esteem perceive life more negatively, and their negative thoughts about themselves determine their negative views on their environment and other individuals.18 However, a study by Nicholson and Long8 reported that the self-esteem of HIV-positive patients was not adversely affected. Similarly, no difference was determined between the groups on the RSEI self-esteem subscale in the current study. Furthermore, 58.6% of the patients did not experience psychiatric problems and thus received no psychiatric treatment.
It is known that self-esteem is associated with psychosocial variables such as social support and disease anxiety.8 Dowshen et al19 reported a positive correlation between self-esteem and social support. They found that individuals who disliked and were dissatisfied with themselves were more reluctant to reveal their disease to other individuals and to seek help, which led to a poor social support level.
In the present study, no correlation was determined between the diagnosis period and self-esteem. Savin-Williams and Demo20 argued that self-esteem would exhibit little fluctuation in the stable self-concept, and factors such as social class, maturation, order of birth, sex, and number of siblings were highly important in the formation of a stable self-concept.20 Rosenberg,12 on the other hand, reported that self-esteem was usually relatively stable except for minor deviations.
Heatherton et al18 reported that self-esteem improved with individual experiences over time and was thus relatively stable, and an individual with current high self-esteem would most likely have high self-esteem in the future. Since it was not possible to assess the self-esteem of HIV/AIDS patients before the diagnosis, the net effects of an HIV diagnosis on self-esteem could not be predicted. However, given the above-mentioned research18 and the similar self-esteem scores of patients and controls in the present study, it could be suggested that the study group exhibited stable self-concept even though they were diagnosed with a chronic and stigmatized infection. Furthermore, although the mean diagnosis period in HIV/AIDS patients was 17.48 ± 31.50 months, it was not possible to determine a correlation between the diagnosis period and self-esteem. These findings reinforced the interpretation that factors such as anxiety, social support, and diagnosis period had no adverse effects on self-esteem, which usually exhibits a relatively stable structure. Similarly, despite the high anxiety rate among the patient group, no significant difference was determined between the self-esteem scores of the patient and control groups.
In the present study, significantly higher scores were found for the RSEI fantasy, psychosomatic symptoms, and parental interest subscales in the HIV/AIDS group compared to the control group. The higher fantasy and psychosomatic symptom scores indicated higher symptom levels, while higher parental interest scores indicated lower parental interest. Psychosomatic complaints are common in individuals without social support who cannot express concerns about their disease verbally. A study21 conducted in HIV-positive patients reported high alexithymia rates in these patients and that they experienced difficulty in expressing emotions and physical symptoms and were confused and uncertain when asked about their health. The study by Pedersen and Elklit10 found that 26% to 47% of the patient group diagnosed with HIV experienced emotions of guilt. Patients who experience psychosocial problems such as guilt, stigmatization, disease anxiety, and the feeling they are not loved could exhibit behavior such as not revealing their diagnosis to others and not seeking social support.22 The findings of the present study that indicated high psychosomatic symptom and parental interest subscale scores are consistent with similar findings reported in the literature.10,21,22
Self-defense mechanisms were first described by Freud as unconscious processes that assist the self in combating anxiety-inducing internal and external threats.23 Although HIV diagnosis was associated with several psychosocial problems that require coping such as stigmatization, depression, and reduced social support, the defense mechanisms used by HIV/AIDS patients to cope with these traumatic processes were scarcely investigated in the literature.10 The analysis of the DSQ findings in the present study revealed significant differences between the groups based on the neurotic defense mechanisms and immature defense mechanisms scores, favoring the HIV/AIDS patients. No differences were determined between the groups based on the mature defense mechanisms scores. Pedersen and Elklit10 reported no significant difference between the control and HIV-positive patient groups based on defense mechanisms; however, these patients employed mature and neurotic defense mechanisms more often compared to the control group. The neurotic and immature defense mechanisms are maladaptive in ensuring adaptation to the outside world. The above-mentioned study10 indicated that the defense mechanisms employed by the patients based on their current clinical picture could be different in HIV/AIDS, which exhibits a chronic and inconsistent course, and patients could cope with the disease in the long term through changing defense mechanisms.
In the present study, it was determined that low mature defense mechanisms scores led to an increase in trust subscale scores and high immature defense mechanisms scores led to high fantasy and parental interest subscale scores. A high score on the trust subscale indicates low confidence in others. Vaillant24 reported that mature defense mechanisms were more strongly associated with adaptive functions and health in contrast with the immature defense mechanisms. Despite the association of neurotic defense mechanisms with distress and mental disorder, they exhibit a more protective role in cognitive and affective conflicts compared to the immature defense mechanisms.25 The low employment of mature and neurotic defense mechanisms, which reflect higher adaptive functions, could impair social functionality by reducing trust in others. Given that both cases (ie, social functionality and trust) are clinical indicators that negatively affect functionality, the positive correlations between these cases and immature defense mechanisms that disrupt functionality were consistent with the findings reported in the literature.25
Limitations
Limitations include the small sample size, the inability to consider prediagnosis self-esteem levels and compare findings given that only a few studies have investigated defense mechanisms in HIV/AIDs patients, and the lack of individuals with only a primary education in the control group given the source population. However, this study will contribute to the literature, as it is one of the few studies to investigate this topic.
CONCLUSION
The present study determined that there was no difference between the self-esteem of the HIV-positive patients and healthy controls. These findings could be explained by the relative stability of self-esteem. Also, neurotic and immature defense mechanisms were used more frequently by the patient group compared to the healthy group, and there was no difference between the groups on the basis of the utilization of mature defense mechanisms. Less use of neurotic and immature defense mechanisms is more beneficial for coping with stress factors and the improvement of psychopathology. Treatment success rates for HIV/AIDS, which is a chronic and stigmatized infection, may improve by employing psychotherapeutic approaches that increase the use of functional mature defense mechanisms and limiting the use of nonfunctional defense mechanisms.
Clinical Points
- Self-esteem in HIV-positive patients may be related to the stability of the self-esteem concept.
- Employing psychotherapeutic approaches that increase the use of functional mature defense mechanisms and limiting the use of nonfunctional defense mechanisms in the treatment of HIV/AIDS patients could increase treatment success rates.
Submitted: December 2, 2019; accepted January 17, 2020.
Published online: March 19, 2020.
Potential conflicts of interest: None.
Funding/support: None.
REFERENCES
1. HIV/AIDS. WHO Data and statistic Web site. https://www.who.int/hiv/data/en/. Accessed February 21, 2020.
2. Bond T. HIV Counselling: Report on National Survey and Consultation 1990. Rugby, UK: British Association for Counselling; 1990.
3. Tafarodi RW, Swann WB. Two-dimensional self-esteem: theory and measurement. Pers Individ Dif. 2001;31(5):653–673. CrossRef
4. Crocker J, Park LE. The costly pursuit of self-esteem. Psychol Bull. 2004;130(3):392–414. PubMed CrossRef
5. Ross M. It feels like yesterday: The social psychology of subjective time judgments. Paper presented at Annual Meeting of the Society for Personality and Social Psychology; 2002; Savannah, GA.
6. McFarlin DB, Blascovich J. Effects of self-esteem and performance feedback on future affective preferences and cognitive expectations. J Pers Soc Psychol. 1981;40(3):521–531. CrossRef
7. Durteste M, Kyselyova G, Volokha A, et al; Study of Young People Living with HIV in Ukraine. Anxiety symptoms and felt stigma among young people living with perinatally or behaviourally-acquired HIV in Ukraine: a cross-sectional survey. PLoS One. 2019;14(1):e0210412. PubMed CrossRef
8. Nicholson WD, Long BC. Self-esteem, social support, internalized homophobia, and coping strategies of HIV+ gay men. J Consult Clin Psychol. 1990;58(6):873–876. PubMed CrossRef
9. Bhana A, Mellins CA, Small L, et al. Resilience in perinatal HIV+ adolescents in South Africa. AIDS Care. 2016;28(suppl 2):49–59. PubMed CrossRef
10. Pedersen SS, Elklit A. Traumatisation, psychological defence style, coping, symptomatology, and social support in HIV-positive: a pilot study. Scand J Psychol. 1998;39(2):55–60. PubMed CrossRef
11. Riis P. Perspectives on the Fifth Revision of the Declaration of Helsinki. JAMA. 2000;284(23):3045–3046. PubMed CrossRef
12. Rosenberg M. Self-concept from middle childhood through adolescence. In: Suls J, Greenwald AG, eds. Psychological Perspectives on the Self. Vol 3. Hillsdale, NJ: Lawrence Erlbaum; 1986.
13. Andrews G, Pollock C, Stewart G. The determination of defense style by questionnaire. Arch Gen Psychiatry. 1989;46(5):455–460. PubMed CrossRef
14. Beck AT, Epstein N, Brown G, et al. An inventory for measuring clinical anxiety: psychometric properties. J Consult Clin Psychol. 1988;56(6):893–897. PubMed CrossRef
15. Keser I, Saygin N, Turkan S, et al. Evaluation of self-esteem with internalized stigmatization in patients with mental illness. Eur Psychiatry. 2011;26:461.
16. Roth M, Decker O, Herzberg P, et al. Dimensionality and norms of the Rosenberg Self-Esteem Scale in a German general population sample. Eur J Psychol Assess. 2008;24:190–197. CrossRef
17. Zhang C, Li X, Liu Y, et al. Impacts of HIV stigma on psychosocial well-being and substance use behaviors among people living with HIV/AIDS in China: across the life span. AIDS Educ Prev. 2018;30(2):108–119. PubMed CrossRef
18. Heatherton TF, Wyland CL, Lopez S. Assessing self-esteem. In: Lopez SJ, Snyder CR, eds. Positive Psychological Assessment: A Handbook of Models and Measures. Washington, DC: American Psychological Association; 2003:219–233.
19. Dowshen N, Binns HJ, Garofalo R. Experiences of HIV-related stigma among young men who have sex with men. AIDS Patient Care STDS. 2009;23(5):371–376. PubMed CrossRef
20. Savin-Williams RC, Demo DH. Situational and transitional determinants of adolescent self-feelings. J Pers Soc Psychol. 1983;44(4):824–833. CrossRef
21. Lumley MA, Neely LC, Burger AJ. The assessment of alexithymia in medical settings: implications for understanding and treating health problems. J Pers Assess. 2007;89(3):230–246. PubMed CrossRef
22. Cohen S, Wills TA. Stress, social support, and the buffering hypothesis. Psychol Bull. 1985;98(2):310–357. PubMed CrossRef
23. Cramer P. Defense mechanisms in psychology today: further processes for adaptation. Am Psychol. 2000;55(6):637–646. PubMed CrossRef
24. Vaillant GE. Adaptation to Life. Cambridge, Massachusetts: Harvard University Press; 1995.
25. Battista JR. Empirical test of Vaillant’s hierarchy of ego functions. Am J Psychiatry. 1982;139(3):356–357. PubMed CrossRef
Enjoy this premium PDF as part of your membership benefits!