ABSTRACT
Context: Patients with mental health needs are often treated by primary care providers (PCPs). Little is known about current PCP attitudes and comfort level with mental health disorders and treatments despite their role in managing these illnesses.
Objective: To quantify PCP comfort with the management of psychiatric disorders and treatments.
Methods: PCPs in 2 community clinics were given a survey of psychiatric disorders, treatments, and perceived benefit of assistance from a mental health professional (data were collected during provider meetings in May 2017 and February 2021). Questions were ranked using a Likert scale from 1 to 5 with 1 being “least comfortable,” 3 being “neutral,” and 5 being “very comfortable.” Survey responses about medications and disorders were averaged (ie, mean values were calculated) to approximate PCP comfort with providing psychiatric care with and without support.
Results: A total of 71 surveys were sent, and 54 were completed. Overall, respondents indicated comfort greater than neutral in 4 of the 14 disorder-related questions (ie, for anxiety disorders, unipolar depression, attention-deficit/hyperactivity disorder [ADHD], and sleep disorders) and 7 of the 19 treatment-related questions (ie, for selective serotonin reuptake inhibitors [SSRIs]/serotonin-norepinephrine reuptake inhibitors [SNRIs], second-generation antipsychotics, other sleep medications, other antidepressants, stimulants, non-stimulant treatments for ADHD, and tricyclics). SSRIs/SNRIs were the only item with average comfort greater than 4. Mean overall PCP comfort was 2.73 without support. PCP comfort increased significantly with support from a therapist (3.24) or a psychiatrist (4.11) (P < .001), with backup from a psychiatrist providing significantly more comfort than a therapist (P < .001).
Discussion: These data show ongoing low comfort levels of PCPs in treating psychiatric conditions, suggesting a need for ongoing educational and collaborative approaches to address this critical unmet need.
Prim Care Companion CNS Disord 2022;24(1):21m03020
To cite: Stilwell K, Pelkey L, Platt T, et al. Survey of primary care provider comfort in treating psychiatric patients in 2 community clinics: a pilot study. Prim Care Companion CNS Disord. 2022;24(1):21m03020.
To share: https://doi.org/10.4088/PCC.21m03020
© Copyright 2022 Physicians Postgraduate Press, Inc.
aMichigan State University College of Human Medicine, Secchia Center, Grand Rapids, Michigan
bCherry Health, Grand Rapids, Michigan
cPine Rest Christian Mental Health Services, Grand Rapids, Michigan
dRiverside Community Hospital, Riverside, California
*Corresponding author: Kellen Stilwell, MD, Pine Rest Christian Mental Health Services, 300 68th St, Grand Rapids, MI 49548 ([email protected]).
More than half of people with a mental health disorder are untreated.1,2 Access to behavioral health care remains a public health concern as the psychiatric workforce is underpowered to meet the demand.3,4 The patients who do receive care are predominantly treated by primary care providers (PCPs).5,6 Over 50% of all mental health care is delivered by a PCP, and 70% of all PCP visits have mental health drivers.7 Primary care has become the de facto mental health care system for many patients.2
Despite this, many PCPs feel ill-prepared to care for the mental health problems of their patients. According to data from the Association of American Medical Colleges,8 the average number of weeks spent in psychiatric clerkships represents less than 5 percent of total training time in medical school despite the high prevalence of mental illness in primary care settings. Mental health curricula for PCP residencies are evolving to try to meet the need for behavioral health care training.9 A national survey10 of senior internal medicine (IM, n = 279) and family medicine (FM, n = 326) residents found that FM residents were more likely to self-report feeling “very prepared” to treat outpatients with depression than their IM colleagues (74% vs 36%, P = .06). A more recent study11 showed that patients with anxiety, depression, or both disorders were more likely to receive treatment with an antidepressant from an FM doctor than an IM doctor and those with anxiety alone were less likely to receive a benzodiazepine from an FM doctor. Training directors from IM (71%), pediatrics (85%), and obstetrics and gynecology (Ob/Gyn, 92%) programs were more likely than training directors in FM (41%) to report that psychiatry training in their programs was inadequate.12 The American Council for Graduate Medical Education (ACGME) Common Program Requirements outlines behavioral health outcome competencies for primary care residencies. According to section IV.B.1.c, “Residents must demonstrate knowledge of established and evolving biomedical, clinical, epidemiologic and social-behavioral sciences, as well as the application of this knowledge to patient care.”13(p19) Yet, the implementation of this requirement varies significantly. For example, the American Academy of Family Physicians (AAFP) sets clear expectations in its “Recommended Curriculum Guidelines for Family Medicine Residents: Human Behavior and Mental Health.”14 In these guidelines, specific competencies, attitudes, knowledge, and skills are specified, including the ability to perform a mental status examination; use of mental health screening tools, pharmacologic treatments, basic counseling skills in motivational interviewing, and cognitive-behavioral therapy (CBT); addressing drug and alcohol dependency; and referral for treatment when needed. In contrast, specialty-specific ACGME requirements for IM residencies require only “opportunities for experience in psychiatry,” along with other subspecialties.15 It is unclear how existing primary care training translates to providers’ level of comfort in practice, but it is known that providers recognize the need for more education and experience in treating those with mental health conditions.16
“Comfort” is a concept we selected to embody the key elements of competency as well as the willingness to care for psychiatric patients. It includes possessing the knowledge, skills, and attitude to care for those with mental illnesses, as well as a psychological sense of “ease” in doing so. Previous studies have assessed PCPs in various distinct ways by asking about desired training priorities,17 factors that complicate treatment of patients with medical and mental illness,18 and factors that contribute to psychiatric referral by primary care providers.19 To our knowledge, our study is the first to systematically assess PCP “comfort” with provision of psychiatric care. We hypothesized that despite current training requirements, many PCPs would have low comfort levels in managing psychiatric patients. The goal of this project was to objectively quantify the comfort of PCPs with the management of specific classes of psychiatric disorders and treatments. The resulting data provide a recent update to previous studies, fill an important gap in the literature, and could renew attention to the need to support PCPs in their care of patients with mental illnesses.
METHODS
This project was a retrospective analysis of data from a 35-item anonymous survey (see Supplementary Appendix 1) collected from PCPs practicing in FM, pediatrics, IM, and Ob/Gyn at Cherry Health in Grand Rapids, Michigan, and Union Community Care in Lancaster, Pennsylvania. Cherry Health’s data were collected during a provider meeting in May 2017, and the Union Community Care data were collected at a meeting in February 2021. Cherry Health is the largest federally qualified health center (FQHC) in Michigan with 20 locations in 7 rural and urban counties, treating more than 70,000 patients annually. Union Community Care is a patient-centered medical health home with primary care, dental care, behavioral health, and social services with 5 locations in Lancaster, Pennsylvania, serving more than 20,000 patients annually. The survey asked participants to rank their comfort with managing psychiatric disorders as organized in the American Psychiatric Association’s Fifth Edition of the Diagnostic and Statistical Manual of Mental Disorders (DSM-5)20 and within different classes and categories of available treatments. Each survey item was ranked on a Likert scale from 1 to 5, with 1 being “least comfortable,” 3 indicating “neutral,” and 5 being “very comfortable.” Compiled survey results were averaged; all results reported as averages are mean values. The overall PCP comfort was calculated by averaging scores for all 33 of the diagnosis and treatment items in the survey. PCPs were then asked to rank their overall comfort if the patient had a therapist or if there was psychiatric backup. Paired-sample t tests were used to compare comfort without support to comfort with a therapist involved or with psychiatric backup. Data were analyzed using SPSS version 25 (IBM; July 2017), and the study was deemed exempt by the Michigan State University Institutional Review Board.
RESULTS
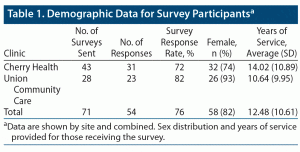
A total of 71 surveys were administered, and 54 completed surveys were collected and analyzed from both sites (31 at Cherry Health and 23 at Union Community Care) for an overall survey response rate of 76%. At Cherry Health, the survey was sent to physicians (8 in IM, 8 in FM, and 9 in pediatrics), physician’s assistants (PAs; 3 in IM, 7 in FM, 1 in women’s health, and 1 in psychiatry), nurse practitioners (NPs; 2 in IM, 2 in FM, and 1 in pediatrics), and 1 nurse midwife practicing in women’s health. PCPs responding to the survey at Cherry Health included 9 practicing in pediatrics, 8 in FM, 7 in IM, and 2 in women’s health (5 did not list their specialty). Union Community Care’s respondents included 9 physicians (8 in FM and 1 in pediatrics), 5 NPs (4 in FM and 1 in Ob/Gyn), and 3 PAs practicing in FM. Six at Union Community Care did not list their specialty. A total of 82% of providers who received the survey were female, and PCPs averaged 12.48 years post-training at the time of the survey (Table 1).
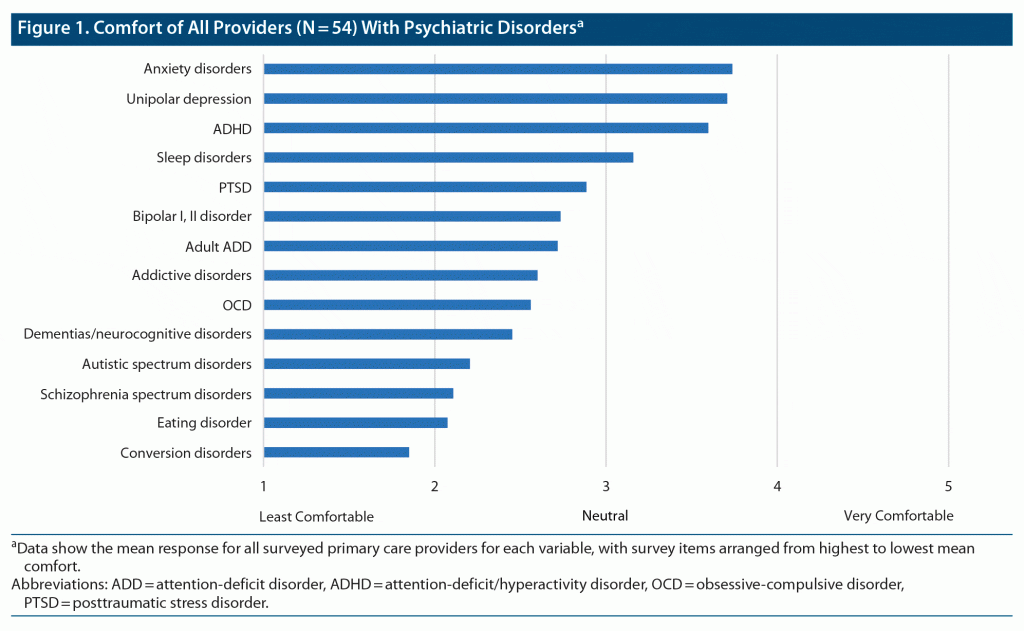
Overall, the surveyed PCPs expressed limited comfort caring for patients with psychiatric disorders, as no diagnoses had mean comfort greater than 4. Comfort treating conversion disorders had a mean score less than 2. Mean scores for posttraumatic stress disorder, bipolar I/II disorders, adult attention-deficit disorder, addictive disorders, obsessive-compulsive disorder, dementia/neurocognitive disorders, autistic spectrum disorders, schizophrenia spectrum disorders, and eating disorders were between 2 and 3. Mean scores for anxiety disorders, unipolar depression, attention-deficit/hyperactivity disorder (ADHD), and sleep disorders were between 3 and 4 (Figure 1).
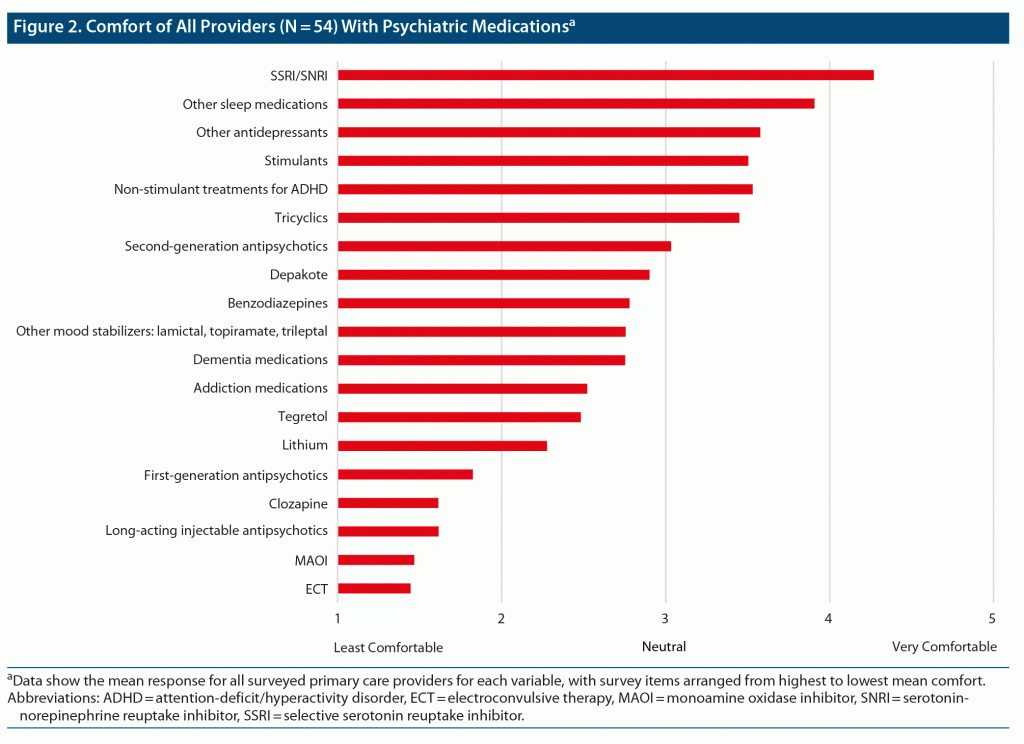
Mean responses from surveyed PCPs for managing first-generation antipsychotics, clozapine, long-acting injectable antipsychotics, monoamine oxidase inhibitors (MAOIs), and electroconvulsive therapy (ECT) were less than 2. Divalproex (Depakote), benzodiazepines, “other mood stabilizers,” dementia medications, addiction medications, carbamazepine (Tegretol), and lithium had mean ratings between 2 and 3. “Other sleep medications,” “other antidepressants,” stimulants, non-stimulants for ADHD, tricyclics, and second-generation antipsychotics had mean ranks between 3 and 4. Only selective serotonin reuptake inhibitors (SSRIs)/serotonin-norepinephrine reuptake inhibitors (SNRIs) were ranked above 4 (Figure 2).
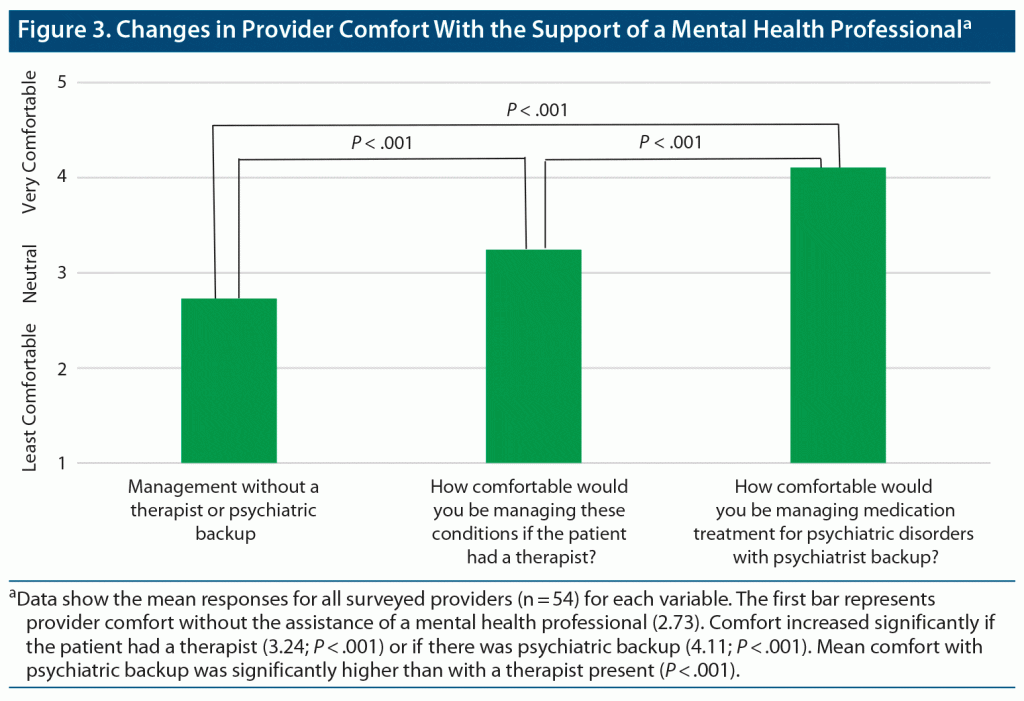
Respondents indicated increased mean comfort with the addition of a therapist (3.24), with further increased comfort when supported by a psychiatrist (4.11) as compared to management without support (2.73). Comfort was significantly greater with the addition of a therapist and with psychiatric backup (P < .001), and comfort was significantly greater with psychiatric backup compared to the addition of a therapist (P < .001) (Figure 3).
DISCUSSION
While there remains a tremendous unmet need for mental health care in the United States with PCPs often filling the gap,5,6 our data indicate that the PCPs we surveyed had low levels of reported comfort treating these disorders. Furthermore, approximately 60% of adults with any mental illness go without care and 30% with depression receive no care at all.21 With this tremendous unmet need, the indirect costs of untreated mental disorders1 and shortage of specialty mental health providers make it critical that PCPs be empowered to meet their patients’ mental health needs. Aside from SSRI/SNRIs, mean rankings did not exceed 4 for any of the disorder or treatment items surveyed, which suggests low overall PCP comfort in providing psychiatric care. Comfort with SSRI/SNRIs was the highest among the surveyed treatments, which aligns with their overall frequency of prescription.6 Patients with certain disorders (eg, eating disorders, schizophrenia spectrum disorders, conversion disorders) or needing specialized treatments (eg, MAOI, clozapine, ECT) with the lowest reported comfort levels may best be referred to specialty care.
It has been shown that the diagnoses made by PCPs show high concordance with those of psychiatrists, and PCP confidence is bolstered by participating in joint consultation.22 The need to train PCPs in mental health has been recognized by the ACGME, and models for enhancing mental health training have been developed and proposed. For example, Cole et al23 published a model curriculum for behavioral health training in primary care, and Matorin and Ruiz24 have outlined an ambulatory care training model for family practice residents. Additionally, Smith and colleagues25 developed a model curriculum for IM residents based on a theoretical framework with a strong evidence base that includes both didactic and clinic experiences across the 3 years of training. In a review of the literature from 1950 to 2000,26 it was recommended that primary care trainees be involved in longitudinal training that includes a high degree of active participation, use of simulation and role-playing, and case-based learning with evaluations that occur in the actual site of practice. Our data highlight possible directions for education, although larger studies will be necessary to inform policy decisions.
Because of the shortage of psychiatrists,4 models for mental health providers to directly support PCPs including telepsychiatry, telehealth consultations, integrated care, and stepped care approaches are being studied and implemented to extend the reach of existing psychiatrists.5,27 For example, the COVID-19 pandemic has led to a rapid expansion in telehealth services,28 and as a result this expansion could provide expert care to people in places that previously did not have such access. Even so, telehealth services are still limited by the number of available mental health experts, and access to telehealth may become restricted by third-party payers post-pandemic.
Another promising approach is to optimize screening strategies to identify psychiatric need in PCP practices and then to implement patient care registries to facilitate identification of cases requiring comanagement using established collaborative care models.29 These collaborative care models could be supported and augmented by technology to bring cost-effective, evidenced-based care to those in need.30–32 It was observed in this survey that physician comfort would increase with the addition of support from a mental health specialist, especially with support from a psychiatrist. Clinical support has been cited as a factor in retention of PCPs, which could be given in the form of education or behavioral health integration/consultation.33 PCPs are on the front line in terms of providing psychiatric care, and this will likely continue to be the case as projected shortages for psychiatrists are expected to continue through 2050.34 In the context of this and the projected burdens of the COVID-19 pandemic on the mental health system,35 renewed attention to PCPs providing psychiatric care is essential.
Limits and Further Work
This study has several limitations. First, to improve the survey in the future, it may be useful to expand the questions that included groupings of individual treatments and disorders (eg, the category “MAOIs” could include “phenelzine, tranylcypromine, etc” as examples), as providers may have different knowledge of treatments within those groups. The addition of “somatic symptom disorders” to the survey may be helpful in future iterations of the survey, as these are commonly seen psychiatric conditions in primary care, although PCP comfort treating “conversion disorders,” a type of somatic disorder, was rated low on the scale (ie, < 2). Second, it would be helpful to inquire in more detail about the quantity and nature of mental health training PCPs received in medical school and postgraduate training. Third, when comfort levels were scored either low or high, follow-up questions about why PCPs responded the way they did would also be helpful. Fourth, the relatively small sample size limited specialty-specific analysis; however, generalizability is enhanced by utilizing results from more than one center. Last, it may have been useful to include disorders seen more frequently in pediatric populations, such as conduct disorder, oppositional defiant disorder, enuresis, encopresis, and others, to better understand the concerns faced by pediatricians.
CONCLUSIONS
This study represents a renewed effort to quantify PCPs’ “comfort” with the psychiatric care they provide. Our results begin to identify gaps in PCP comfort that may be targeted for collaborative care or educational initiatives. Further work to expand the sample size and better understand the needs of PCPs from different specialties and across a broader range of geographic and practice settings is warranted; however, enhanced behavioral health training in all PCP specialties is one strategy that could help address the current levels of discomfort. Varied approaches will be needed to help spread the limited available psychiatric expertise to more patients while continuing to expand, educate, and equip a larger mental health workforce to meet the growing need.
Submitted: May 21, 2021; accepted August 23, 2021.
Published online: February 3, 2022.
Potential conflicts of interest: Dr Achtyes has served on advisory boards for Alkermes, Janssen, Lundbeck/Otsuka, Neurocrine Biosciences, Sunovion, and Teva; has received research support from Alkermes, Astellas, Biogen, Boehringer-Ingelheim, CMS, InnateVR, Janssen, National Network of Depression Centers, Neurocrine Biosciences, Novartis, Otsuka, Pear Therapeutics, and Takeda; and has held stock in AstraZeneca, Johnson & Johnson, Moderna, and Pfizer. Drs Stilwell, Pelkey, Platt, Nguyen, Monteith, and Pinheiro report no disclosures.
Funding/support: None.
Previous presentations: Select data from this study have been presented as posters at the following: Midwest Interprofessional Education and Research Center conference; September 21, 2017; Grand Rapids, Michigan • the Psych Congress national conference; September 16, 2017; New Orleans, Louisiana • the Michigan Psychiatric Society’s Annual Meeting; April 13, 2018; East Lansing, Michigan.
Acknowledgments: The authors would like to thank Sherry Culmer, BS, of Cherry Health for her support in administering and compiling surveys and survey data as well as preparing data for presentation. The authors also thank Kristen Harker CNM, CRNP, of Union Community Care for de-identifying and providing data for this project. Neither has relevant disclosures. In-kind sponsorship was provided by Cherry Health.
Supplementary material: See accompanying pages.
Clinical Points
- Mental health care needs often go untreated, and the existing workforce of expert mental health professionals is underpowered to meet the demand.
- Primary care providers provide the majority of psychiatric care, but many lack the training and support to feel comfortable managing these conditions.
- A multipronged approach including enhanced training, collaborative care models, integrated practices, patient registries, stepped care, expanded access to telehealth, and technology-delivered therapies may be needed to support the treatment of mental health conditions in primary care.
References (35)

- Kessler RC, Berglund PA, Bruce ML, et al. The prevalence and correlates of untreated serious mental illness. Health Serv Res. 2001;36(6 Pt 1):987–1007. PubMed
- Regier DA, Narrow WE, Rae DS, et al. The de facto US mental and addictive disorders service system: epidemiologic catchment area prospective 1-year prevalence rates of disorders and services. Arch Gen Psychiatry. 1993;50(2):85–94. PubMed CrossRef
- Bishop TF, Seirup JK, Pincus HA, et al. Population of US practicing psychiatrists declined, 2003–13, which may help explain poor access to mental health care. Health Aff (Millwood). 2016;35(7):1271–1277. PubMed CrossRef
- Thomas KC, Ellis AR, Konrad TR, et al. County-level estimates of mental health professional shortage in the United States. Psychiatr Serv. 2009;60(10):1323–1328. PubMed CrossRef
- Blount FA, Miller BF. Addressing the workforce crisis in integrated primary care. J Clin Psychol Med Settings. 2009;16(1):113–119. PubMed CrossRef
- Pincus HA, Tanielian TL, Marcus SC, et al. Prescribing trends in psychotropic medications: primary care, psychiatry, and other medical specialties. JAMA. 1998;279(7):526–531. PubMed CrossRef
- Bureau of Primary Healthcare: Mountainview Consulting Group Inc. Integrating primary care and Behavioral Health Services: a Compass and a Horizon. APA website. 2018. Accessed May 4, 2018. http://www.apa.org/practice/programs/rural/integrating-primary-behavioral.pdf
- Association of American Medical Colleges. Clinical Course Required Weeks by Discipline. AAMC Curriculum Inventory, 2019–2020. AAMC website. https://www.aamc.org/data-reports/curriculum-reports/interactive-data/clinical-course-required-weeks-discipline
- Gaskins SE, Badger LW, Gehlbach SH, et al. Family practice residents’ evaluation of a competency-based psychiatry curriculum. J Med Educ. 1987;62(1):41–46. PubMed CrossRef
- Wiest FC, Ferris TG, Gokhale M, et al. Preparedness of internal medicine and family practice residents for treating common conditions. JAMA. 2002;288(20):2609–2614. PubMed CrossRef
- Brieler JA, Scherrer JF, Salas J. Differences in prescribing patterns for anxiety and depression between general internal medicine and family medicine. J Affect Disord. 2015;172:153–158. PubMed CrossRef
- Leigh H, Stewart D, Mallios R. Mental health and psychiatry training in primary care residency programs. Part II. what skills and diagnoses are taught, how adequate, and what affects training directors’ satisfaction? Gen Hosp Psychiatry. 2006;28(3):195–204. PubMed CrossRef
- American Council for Graduate Medical Education. Common Program Requirements [PDF]. July 1, 2019. Chicago: Accreditation Council for Graduate Medical Education. ACGME website. https://www.acgme.org/Portals/0/PFAssets/ProgramRequirements/CPRResidency2019.pdf
- American Academy of Family Physicians. Recommended Curriculum Guidelines for Family Medicine Residents Human Behavior and Mental Health Reprint No. 270. June 2015. AAFP website. https://www.aafp.org/dam/AAFP/documents/medical_education_residency/program_directors/Reprint270_Mental.pdf
- American Council for Graduate Medical Education. Internal Medicine Program Requirements and FAQs. July1, 2017. ACGME website. https://www.acgme.org/Specialties/Program-Requirements-and-FAQs-and-Applications/pfcatid/2/Internal Medicine
- Freed GL, Dunham KM, Switalski KE, et al; Research Advisory Committee of the American Board of Pediatrics. Recently trained general pediatricians: perspectives on residency training and scope of practice. Pediatrics. 2009;123(suppl 1):S38–S43. PubMed
- Kerwick S, Jones R, Mann A, et al. Mental health care training priorities in general practice. Br J Gen Pract. 1997;47(417):225–227. PubMed
- Loeb DF, Bayliss EA, Binswanger IA, et al. Primary care physician perceptions on caring for complex patients with medical and mental illness. J Gen Intern Med. 2012;27(8):945–952. PubMed CrossRef
- Kravitz RL, Franks P, Feldman M, et al. What drives referral from primary care physicians to mental health specialists? a randomized trial using actors portraying depressive symptoms. J Gen Intern Med. 2006;21(6):584–589. PubMed CrossRef
- American Psychiatric Association. Diagnostic and Statistical Manual of Mental Disorders. Fifth Edition. Arlington, VA: American Psychiatric Publishing; 2013.
- Substance Abuse and Mental Health Services Administration. Key Substance Use and Mental Health Indicators in the United States: Results From the 2019 National Survey on Drug Use and Health (HHS Publication No. PEP20-07-01-001, NSDUH Series H-55). Rockville, MD: Center for Behavioral Health Statistics and Quality, Substance Abuse and Mental Health Services Administration; 2020. SAMHSA website. https://www.samhsa.gov/data/
- Saillant S, Hudelson P, Dominicé Dao M, et al. The primary care physician/psychiatrist joint consultation: a paradigm shift in caring for patients with mental health problems? Patient Educ Couns. 2016;99(2):279–283. PubMed CrossRef
Cole SA, Sullivan M, Kathol R, et al. A model curriculum for mental disorders and behavioral problems in primary care. Gen Hosp Psychiatry. 1995;17(1):13–18. PubMed CrossRef
- Matorin AA, Ruiz P. Training family practice residents in psychiatry: an ambulatory care training model. Int J Psychiatry Med. 1999;29(3):327–336. PubMed CrossRef
- Smith RC, Laird-Fick H, D’Mello D, et al. Addressing mental health issues in primary care: an initial curriculum for medical residents. Patient Educ Couns. 2014;94(1):33–42. PubMed CrossRef
- Hodges B, Inch C, Silver I. Improving the psychiatric knowledge, skills, and attitudes of primary care physicians, 1950-2000: a review. Am J Psychiatry. 2001;158(10):1579–1586. PubMed CrossRef
- Katon WJ, Lin EH, Von Korff M, et al. Collaborative care for patients with depression and chronic illnesses. N Engl J Med. 2010;363(27):2611–2620. PubMed CrossRef
- Kopec K, Janney CA, Johnson B, et al. Rapid transition to telehealth in a community mental health service provider during the COVID-19 pandemic. Prim Care Companion CNS Disord. 2020;22(5):20br02787. PubMed CrossRef
- Unützer J, Katon W, Callahan CM, et al; IMPACT Investigators. Improving Mood-Promoting Access to Collaborative Treatment. Collaborative care management of late-life depression in the primary care setting: a randomized controlled trial. JAMA. 2002;288(22):2836–2845. PubMed CrossRef
- Aikens JE, Valenstein M, Plegue MA, et al. Technology-facilitated depression self-management linked with lay supporters and primary care clinics: randomized controlled trial in a low-income sample. Telemed J E Health. 2021;tmj.2021.0042. PubMed CrossRef
- Firth J, Torous J, Nicholas J, et al. The efficacy of smartphone-based mental health interventions for depressive symptoms: a meta-analysis of randomized controlled trials. World Psychiatry. 2017;16(3):287–298. PubMed CrossRef
- Gerhards SAH, de Graaf LE, Jacobs LE, et al. Economic evaluation of online computerized cognitive-behavioral therapy without support for depression in primary care: randomized trial. Br J Psychiatry. 2010;196(4):310–318. PubMed CrossRef
- Walker KO, Ryan G, Ramey R, et al. Recruiting and retaining primary care physicians in urban underserved communities: the importance of having a mission to serve. Am J Public Health. 2010;100(11):2168–2175. PubMed CrossRef
- Satiani A, Niedermier J, Satiani B, et al. Projected workforce of psychiatrists in the United States: a population analysis. Psychiatr Serv. 2018;69(6):710–713. PubMed CrossRef
- Edwards E, Janney CA, Mancuso A, et al. Preparing for the behavioral health impact of COVID-19 in Michigan. Curr Psychiatry Rep. 2020;22(12):88. PubMed CrossRef
Enjoy this premium PDF as part of your membership benefits!