ABSTRACT
Objective: Wake-up stroke (WUS) comprises a significant proportion of ischemic strokes. However, due to unclear onset, these patients are often not considered for reperfusion therapy. The objective of this study was to investigate the clinical and imaging differences between WUS patients and those with clear-onset stroke, documenting any sex, age, or risk factor predilection for WUS.
Methods: This prospective observational cohort study used an ongoing stroke registry to identify patients with acute ischemic stroke admitted to a hospital in Saudi Arabia within 5 days of symptom onset from April 2018 to March 2020. Patients were classified into 2 groups: WUS and clear-onset stroke.
Results: Among 645 patients, 448 met the criteria for acute ischemic stroke and were included in the study. WUS was identified in 112 (25%) patients. There were no differences in sex or median age between the 2 groups. Diabetes mellitus, hypertension, and dyslipidemia were higher in the WUS group, while atrial fibrillation, history of stroke and epilepsy were higher in the clear-onset stroke group. Bihemispheric stroke was higher in the clear-onset stroke group than in the WUS group (6.0% vs 2.7%).
Conclusions: Only minor dissimilarities between clinical and radiologic features of WUS and clear-onset stroke were found. Circadian patterns of stroke onset were observed in both groups. Stroke was more likely to occur during waking than during sleep, and a diurnal pattern of common occurrence during the morning was documented. Recognition of the acceptable timeframe for acute reperfusion therapy in unwitnessed strokes is crucial so that thrombolytic treatment can be started for these patients.
Prim Care Companion CNS Disord 2022;24(6):21m03216
To cite: Shariff EM, Al Khmais FA, Nazish S, et al. Therapeutic dilemma of wake-up stroke: clinical and brain imaging characteristics and reperfusion as a treatment option. Prim Care Companion CNS Disord. 2022;24(6):21m03216.
To share: https://doi.org/10.4088/PCC.21m03216
© 2022 Physicians Postgraduate Press, Inc.
aDepartment of Neurology, College of Medicine, Imam Abdulrahman Bin Faisal University, Dammam, Saudi Arabia
bDepartment of Family and Community Medicine, Imam Abdulrahman Bin Faisal University, Dammam, Saudi Arabia
cDepartment of Radiology, College of Medicine, Imam Abdulrahman Bin Faisal University, Dammam, Saudi Arabia
*Corresponding author: Erum Mubashir Shariff, MBBS, MD, Department of Neurology, King Fahd Hospital of the University, Imam Abdulrahman Bin Faisal University, Postal Code 31952, Dammam, Saudi Arabia ([email protected]).
Stroke is one of the fastest-emerging cerebrovascular diseases, with high rates of morbidity and mortality and resulting in increased social and economic hardship.1–3 Stroke is a second-leading cause of mortality in Saudi Arabia as per the World Health Organization (WHO).4 The main challenge for the health care system in Saudi Arabia is the lack of stroke awareness.3 Data have shown a stroke incidence of 57.64 per 100,000 person-years, with decreased morbidities and mortalities due to improvement in acute stroke management.5–7
Wake-up stroke (WUS) is defined as the condition in which a patient wakes up with symptoms suggestive of stroke that were not present before sleeping. Approximately 25% of all strokes occur during sleep (ie, the exact time of symptom onset is unknown), resulting in a therapeutic dilemma. These patients are generally not considered candidates for acute reperfusion therapy for ischemic stroke, and very few would qualify for mechanical thrombectomy.4,8,9 Exclusion of a significant number of stroke patients from potentially beneficial reperfusion therapy limits its impact on disease burden, leading to poor outcomes. With the emergence of functional neuroimaging techniques, it is now possible to identify patients with WUS who could have benefited from reperfusion therapy.9 Evidence from clinical and imaging studies suggests the timing of WUS is close to the time of waking up; thus, patients might qualify for reperfusion therapy within the approved timeframe in an emergency setting. Several imaging techniques, including noncontrast computed tomography (CT), CT perfusion, and multimodal magnetic resonance imaging (MRI), can be utilized to identify WUS patients who are still eligible for reperfusion therapy.10
The origin of WUS is unknown. Several studies11–14 have highlighted the role of the circadian rhythm in the occurrence of ischemic stroke at different times of the day. The circadian rhythm not only dictates the endogenous sleep/wake cycle, but also determines behavior and other physiologic function. External factors such as light and nutrition also affect this internal clock,11,12 resulting in a synchronized diurnal cycle alternating with light and dark intervals. The suprachiasmatic nucleus located in the anterior hypothalamus is responsible for regulating the diurnal pattern. Occurrence of ischemic stroke is independently associated with this circadian pattern after controlling for hypertension, diabetes mellitus, dyslipidemia, smoking habits, previous vascular events, and treatment with antiplatelet agents or anticoagulant drugs.13,15 The maximum likelihood of stroke is nevertheless in the morning hours for each stroke subtype, including small artery or lacunar, cardioembolic, large artery, and cryptogenic.13,15 In contrast to ischemic stroke, intracerebral hemorrhage has a greater occurrence rate in the late afternoon, with an occasional observation at night.12,15 Controversies exist in the literature regarding clinical presentations, risk factors, etiology, and prognosis between WUS and clear-onset stroke.16 It has been concluded that WUS patients are likely to be older and have a greater incidence of lacunar strokes with presumed pathophysiology of thrombotic strokes compared to clear-onset ischemic stroke patients.
The objective of this study was to identify clinical and imaging characteristics of WUS in an Arab cohort; to determine any sex, age, or risk factor preference for WUS; and to correlate these findings to the possible mechanisms. This article reviews clinical and imaging characteristics of WUS to provide the most recent research regarding WUS, as well as advances in treatment.
METHODS
This was a prospective observational cohort study using an ongoing stroke registry at King Fahd Hospital of the University (KFHU) from April 2018 to March 2020.
Setting
KFHU is a 500-bed tertiary care teaching hospital that provides multidisciplinary health care to the Eastern Province of Saudi Arabia. The hospital has a well-established 45-bed neurology department, including residents, stroke fellows, stroke consultants, and stroke interventionists, with 24-hour provision of inpatient and outpatient clinical services. KFHU is a referral center for acute stroke reperfusion therapy in the Eastern Province of Saudi Arabia and accepts patients in need of thrombolysis or mechanical thrombectomy falling within the therapeutic window.
Sample
Of 645 patients admitted with a diagnosis of ischemic stroke, 448 fulfilled the inclusion criteria and were included in the study. Inclusion criteria were age ≥ 18 years, presenting within 5 days of symptom onset, and National Institutes of Health Stroke Scale (NIHSS) score ≥ 3. Both first-time and recurrent ischemic stroke events were included. Patients with transient ischemic attacks, defined as symptoms lasting less than 24 hours without neuroradiologic evidence of infarction; those who had negative head MRIs; and those who failed to obtain vascular imaging were excluded.
Data and Instruments
The study was approved by the KFHU institutional review board. In the KFHU stroke registry, data collection was done at baseline (at admission) and at clinic follow-up after discharge from the hospital. The registry data included demographics, vascular risk factors, and detailed history regarding time of stroke onset. All patients were grouped into 2 categories: WUS and clear-onset stroke. Patients waking up from sleep with stroke symptoms (WUS) were classified into group A morning (6:00 am–12:00 pm), Group B (12:01 pm–11:59 pm), and Group C midnight (12 am–5:59 am) based on the wake-up time. The precise recognition time of stroke symptoms was obtained via patient memory or eyewitness account. Patients with clear-onset stroke were those who experienced a stroke during the awake state with a recognized time of stroke onset. Patients underwent a detailed neurologic examination including initial NIHSS score. Stroke location and vascular imaging were assessed by a neuroradiologist. A body mass index > 26 kg/m2 was regarded as obese.
Coexisting variables—diabetes mellitus, hypertension, ischemic heart disease, atrial fibrillation, history of stroke, smoking, dyslipidemia, and obesity—were compared. Stroke severity was assessed with the NIHSS.17 Clinical outcome was assessed using hospital discharge modified Rankin Scale (mRS) scores and 90-day mortality rates. The NIHSS is a 15-item validated tool used in clinical trials to assess stroke severity. It includes testing of conscious level; selective cranial nerves; motor, sensory, and cerebellar functions; language; and inattention. The score range is 0–42, with higher values indicating stroke severity.17 The mRS is a 6-point disability scale with possible scores ranging from 0 to 5 and higher values indicating greater disability. A distinct category of 6 is added for patients who die. Uniform conversations to attain mRS scores are endorsed at 90 days after hospital discharge. The NIHSS score was recorded at admission and discharge. The mRS score was recorded 90 days after discharge.
Symptomatic large vessel stroke is identified when stenosis in a large artery is considered the cause. Etiologic classification of ischemic stroke was approved using the Trial of Org 10172 in Acute Stroke Treatment (TOAST) classification.18 TOAST classification categorizes stroke into 5 subtypes: (1) large artery atherosclerosis/macroangiopathic, (2) cardioembolic, (3) small vessel occlusion (lacune) and small vessel occlusion/microangiopathic, (4) stroke of other determined etiology, and (5) undetermined etiology. TOAST classification has a reliable interobserver agreement for accurately predicting stroke prognosis. Stroke was lateralized to left, right, or bilateral. Anatomically, strokes were classified as anterior or posterior circulation infarction according to the territory of the cerebral vessel involved. Anterior circulation involved anterior cerebral artery and middle cerebral artery, while posterior circulation had either posterior cerebral artery or vertebrobasilar circulation infarctions.
Analysis
Comparative and correlative data analyses were conducted. Descriptive statistics for continuous data are reported as median and interquartile range (IQR), as it is a better representation of skewed data. Categorical data were compared mainly by χ2 test and Fisher exact test when numbers were small between cells. Continuous data were compared with the Kruskal-Wallis test, as they were not normally distributed. A P value < .05 was considered statistically significant. The analysis was performed using SPSS version 22.
RESULTS
We identified 645 patients admitted to the neurology service with a diagnosis of acute ischemic stroke; 448 patients were included, and 197 patients were excluded. Of the excluded patients, 30 had intracerebral hemorrhage, 73 had transient ischemic attacks, and 97 had non-neurologic etiologies (stroke mimics). The mean age of all patients was 60.06 years, and 64.7% were male. Patients with WUS constituted 25% (n = 112) of the sample, while 75% (n = 236) had clear-onset stroke. Among patients with WUS, 59.8% were overweight, which was similar to the clear-onset group (56.5%). Recurrent strokes were found in 11% of the WUS patients compared to 19% of the clear-onset group (P = .04).
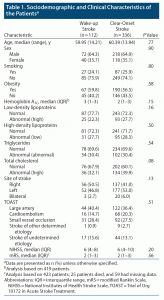
Table 1 presents the clinical characteristics of the patient population according to the time of stroke. A considerably higher risk of stroke incidence in the morning and a lower risk in the late afternoon was confirmed in our cohort of patients. Of 112 patients, 82 had stroke onset from 12 am to 12 pm, which was approximately two-thirds of the WUS patients.
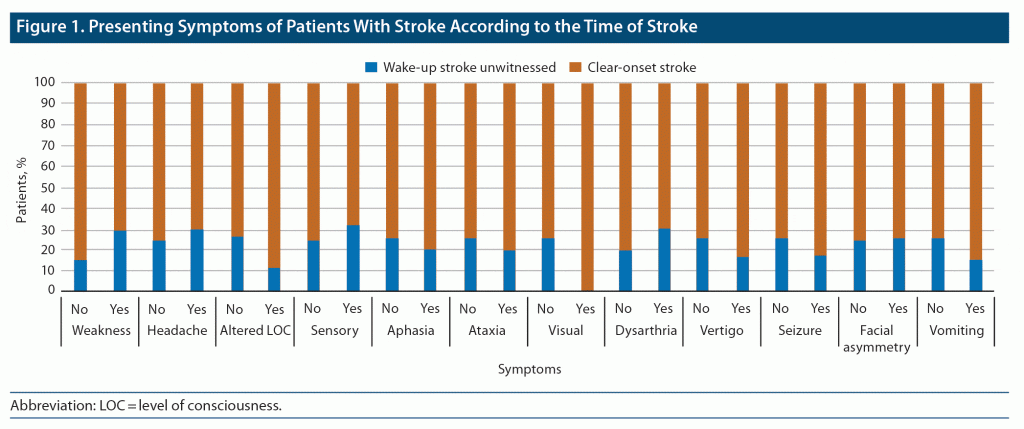
There was no difference in the median NIHSS or mRS scores between the 2 groups. However, hemoglobin A1C (HbA1C) levels were higher among the WUS patients, although this was not statistically significant (P = .15). Regarding TOAST classification, large artery atherosclerosis/macroangiopathic comprised 40.4% of the WUS group and 36.4% of the clear-onset group. No significant associations were observed for low-density lipoproteins, high-density lipoproteins, triglycerides, or total cholesterol. NIHSS score was not associated with HbA1C, obesity, or hypertension. The patients’ symptoms are presented in Figure 1. The highest presenting symptoms for WUS patients were headache, sensory loss, and dysarthria. It is worth noting that all clear-onset patients had visual symptoms.
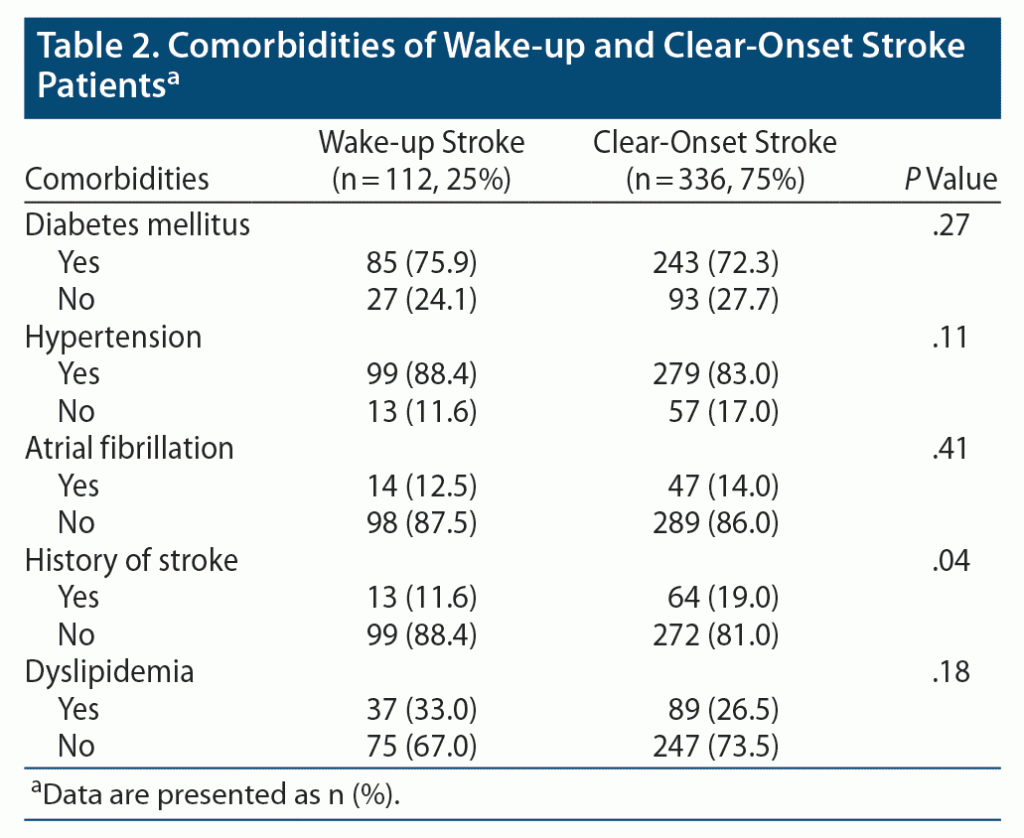
Comorbidities of patients according to the time of stroke are presented in Table 2. Among both WUS and clear-onset patients, the majority of patients were diabetic (75.9% and 72.3%, respectively). A similarly high percentage for both groups was also observed for hypertension.
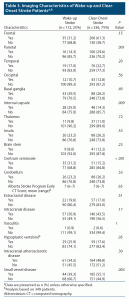
Table 3 describes the MRI/magnetic resonance angiography findings. The only statistically significant results were more parietal lobe involvement in clear-onset strokes (P = .001) and more internal capsule (P = .009) and centrum semiovale strokes (P < .001) in WUS. Small vessel disease (P = .003) was significantly higher in clear-onset stroke, and hypoplastic vertebral artery (P = .05) was higher in WUS. Half of the patients were found to have intracranial atherosclerotic disease in both stroke groups.
DISCUSSION
Several attempts have been made to describe the characteristics of WUS in recent years. It is of upmost importance to understand the pathophysiologic mechanism of WUS. WUS occurs during sleep or in the changeover from sleep to awakening. Diurnal variability of stroke occurrence is a well-known phenomenon that is the pathophysiologic basis of WUS and will hopefully provide insight for prevention in the future. In accordance with available literature, we found a circadian difference in WUS. Hence, we hypothesize that WUS results either from an innate circadian variability due to various stroke-promoting factors or from the biological impact of sleep on these factors.15,16 Research has confirmed that all stroke types, including ischemic and hemorrhagic, occur while awake and in some precise periods of diurnal time. There are various physiologic, pathologic, and lifestyle factors that may contribute to and affect the onset of stroke during sleep or waking.15 Our study suggests that the time of stroke occurrence may not be associated with stroke severity, prognosis, and outcome, with differences between WUS and clear-onset strokes. This finding is contrary to that of Ripamonti et al15 who found a poorer disability score at hospital discharge for WUS compared to clear onset-stroke, as well as a higher risk of death during the first month.
Our study showed that approximately 1 in 4 patients have WUS, which is in line with previous studies16 showing a prevalence ranging from 5%–30%. Interestingly, the patients with WUS in our study had more hemiplegia and dysarthria compared to clear-onset patients. Diabetes, hypertension, and dyslipidemia were documented more often in the WUS group, though this finding was statistically insignificant. In this cohort, we confirmed the diurnal pattern of stroke onset, which is in accordance with previous studies.15,16 A considerably greater risk of stroke incidence in the morning and a lower risk in the late afternoon was documented previously19 and was confirmed in our cohort of patients, while some studies16 have recorded higher incidence from 6 am to noon. Religious practices have been postulated as one of the possible mechanisms of this early morning increase in stroke onset due to the earlier wake-up time of this population for cultural/religious reasons.19 Hypertension is a significant predisposing factor that has been correlated with WUS, reflecting a sympathetic drive. Hypertension is a recognized risk factor for stroke and has well-documented diurnal variation, which is greater in the morning. Other endogenous factors such as a peak in prothrombotic factors, an increase in platelet aggregation, endothelial dysfunction, fluctuating serum catecholamine levels, and autonomic tone are also greater in the morning.14 Additionally, platelet aggregation increases considerably in the morning while changing to upright posture and starting the day-to-day activities. Autonomic nervous system modulations and its variations in advanced age are responsible for daily variation in stroke occurrence and are assumed to facilitate stroke. Modulation of vagal tone during the night is sex specific, being higher in young males, and gradually reduces with increasing age, and it has been associated with stroke risk.20 These variable diurnal patterns of stroke onset in both sexes as well as with aging are partially explained by these differences in mechanisms. Our data clarify that the circadian rhythm, which determines diurnal changes; fluctuations in vitals and physiologic parameters; and the patient’s activities influence stroke occurrence. In our study, diabetes mellitus, hypertension, dyslipidemia, and obesity were more common among WUS patients. On the other hand, history of previous stroke and atrial fibrillation were less frequent in WUS. These findings are in contrast to that of Nahrir et al,16 who found a lower percentage of WUS patients had diabetes mellitus, hypertension, dyslipidemia, ischemic heart disease, and obesity; however, history of previous stroke and atrial fibrillation was more common in WUS. We found the WUS group to be 1 year younger than the clear-onset group, as opposed to other studies in which WUS patients were older.15 The sex-specific risk was different in our study; we found males to have a higher incidence of WUS. Sex-specific diurnal stroke variation has been documented in males who were found to have more stroke incidence in the early morning than in the afternoon, while females were found to have less incidence in the early morning compared to the afternoon.15,16
Patients with WUS were more obese and had more right hemispheric strokes, while both hemispheres were more often involved in clear-onset stroke (P = .06). In our cohort, the most common etiology for WUS was large artery atherosclerotic disease followed by small vessel disease. This finding is contrary to the study by Nahrir et al,16 which revealed more frequent cardioembolic strokes in WUS patients. Nahrir et al16 also found the insular cortex to be involved more frequently along with bihemispheric and left-sided involvement, which is contrary to our findings in which insular cortex, bihemispheric, and left-sided involvement were less frequent in WUS. These differences in risk stratification, etiology, and stroke severity are influenced by these diurnal variations.
CONCLUSIONS
The results of this study indicate that stroke, like many other cardiovascular disorders, occurs typically during the awake state and in the morning hours irrespective of the subtype. We also found that a higher number of WUS patients had some distinguishing features such as a higher rate of large artery atherosclerotic disease.
In primary care settings, diabetes mellitus and hypertension are well-recognized modifiable risk factors for all types of stroke. It is critical to recognize WUS in the primary care setting to ensure early referral to acute stroke care, as many of these patients could benefit from acute reperfusion therapy after appropriate imaging. Several unanswered queries need to be explored as highlighted by this study. Some triggers are suggested to activate the silent atherosclerotic plaque to become inflamed and fissured, resulting in clot formation.
Submitted: December 13, 2021; accepted March 30, 2022.
Published online: November 24, 2022.
Relevant financial relationships: None.
Funding/support: None.
Previous presentations: The data were presented as a poster at the XXV World Congress of Neurology virtual conference; October 3–7, 2021, which was published as an abstract in J Neurol Sci. 2021;429:119681.
Acknowledgments: This study made use of the computational resources and technical services of the Scientific and High Performance Computing Center at Imam Abdulrahman Bin Faisal University.
Clinical Points
- Recognition of the acceptable timeframe for acute reperfusion therapy in unwitnessed strokes is crucial so that thrombolytic treatment can be started for these patients.
- It is critical to recognize wake-up stroke in the primary care setting for early referral to acute stroke care, as many of these patients could benefit from acute reperfusion therapy after obtaining the appropriate imaging.
- Diabetes mellitus and hypertension are important and modifiable risk factors for stroke in the primary care setting.
References (20)

- General Authority for Statistics, The General Population and Housing Census Annual Report. 2010. GASTAT website. Accessed September 9, 2022. https://www.stats.gov.sa/en/13
- Robert AA, Zamzami MM. Stroke in Saudi Arabia: a review of the recent literature. Pan Afr Med J. 2014;17:14. PubMed CrossRef
- Alaqeel A, AlAmmari A, AlSyefi N, et al. Stroke awareness in the Saudi community living in Riyadh: prompt public health measures must be implemented. J Stroke Cerebrovasc Dis. 2014;23(3):500–504. PubMed CrossRef
- Al-Senani F, Al-Johani M, Salawati M, et al. An epidemiological model for first stroke in Saudi Arabia. J Stroke Cerebrovasc Dis. 2020;29(1):104465. PubMed CrossRef
- Memon I, Abu-Shaheen A, Heena H, et al. Point prevalence study for stroke in Saudi Arabia: a cross-sectional survey. Saudi Med J. 2019;8: 93–97.
- Almekhlafi MA. Trends in one-year mortality for stroke in a tertiary academic center in Saudi Arabia: a 5-year retrospective analysis. Ann Saudi Med. 2016;36(3):197–202. PubMed CrossRef
- Alahmari K, Paul SS. Prevalence of stroke in Kingdom of Saudi Arabia: through a physiotherapist diary. Mediterr J Soc Sci. 2016;7(1):228. CrossRef
- Kim YJ, Kim BJ, Kwon SU, et al. Unclear-onset stroke: daytime-unwitnessed stroke vs wake-up stroke. Int J Stroke. 2016;11(2):212–220. PubMed CrossRef
- Dankbaar JW, Bienfait HP, van den Berg C, et al. On behalf of the DUST investigators. Wake-up stroke versus stroke with known onset time: clinical and multimodality CT imaging characteristics. Cerebrovasc Dis. 2018;45(5–6):236–244. PubMed CrossRef
- Kim BJ, Kang HG, Kim HJ, et al. Magnetic resonance imaging in acute ischemic stroke treatment. J Stroke. 2014;16(3):131–145. PubMed CrossRef
- Meng H, Liu T, Borjigin J, et al. Ischemic stroke destabilizes circadian rhythms. J Circadian Rhythms. 2008;6:9. PubMed CrossRef
- Beker MC, Caglayan B, Yalcin E, et al. Time-of-day dependent neuronal injury after ischemic stroke: implication of circadian clock transcriptional factor Bmal1 and survival kinase AKT. Mol Neurobiol. 2018;55(3):2565–2576. PubMed CrossRef
- Casetta I, Granieri E, Fallica E, et al. Patient demographic and clinical features and circadian variation in onset of ischemic stroke. Arch Neurol. 2002;59(1):48–53. PubMed CrossRef
- Omama S, Yoshida Y, Ogawa A, et al. Differences in circadian variation of cerebral infarction, intracerebral haemorrhage and subarachnoid haemorrhage by situation at onset. J Neurol Neurosurg Psychiatry. 2006;77(12):1345–1349. PubMed CrossRef
- Ripamonti L, Riva R, Maioli F, et al. Daily variation in the occurrence of different subtypes of stroke. Stroke Res Treat. 2017;2017:9091250. PubMed CrossRef
- Nahrir S, Khan AH, Al-Senani F. Characteristics of wake-up stroke: an experience from an Arab cohort. Internet J Neurol. 2014;18(1):20443.
- NIH Stroke Scale Training, Part 2. Basic Instruction. Department of Health and Human Services, National Institute of Neurological Disorders and Stroke. The National Institute of Neurological Disorders and Stroke (NINDS) Version 2.0. YouTube website. Accessed September 9, 2022. https://www.youtube.com/watch?v=gzHuNvDhVwE
- Chung JW, Park SH, Kim N, et al. Trial of ORG 10172 in Acute Stroke Treatment (TOAST) classification and vascular territory of ischemic stroke lesions diagnosed by diffusion-weighted imaging. J Am Heart Assoc. 2014;3(4):e001119. PubMed CrossRef
- Torun S, Özdemir G. Very early morning increase in onset of ischemic stroke. Ann Saudi Med. 1994;14(3):201–203. PubMed CrossRef
- Binici Z, Mouridsen MR, Køber L, et al. Decreased nighttime heart rate variability is associated with increased stroke risk. Stroke. 2011;42(11):3196–3201. PubMed CrossRef
Enjoy this premium PDF as part of your membership benefits!