Because this piece does not have an abstract, we have provided for your benefit the first 3 sentences of the full text.
To the Editor: The thyroid gland normally secretes thyroxine and triiodothyronine. A previous study reported that partial substitution of triiodothyronine for thyroxine improved mood and neuropsychological functions in hypothyroid patients treated with only thyroxine, suggesting an importance of the integrity of the thyroid gland for neuropsychological functions. It is clear that thyroid hormone plays an important role in the brain, influencing mood and cognition; however, the detail mechanisms remain to be elucidated.
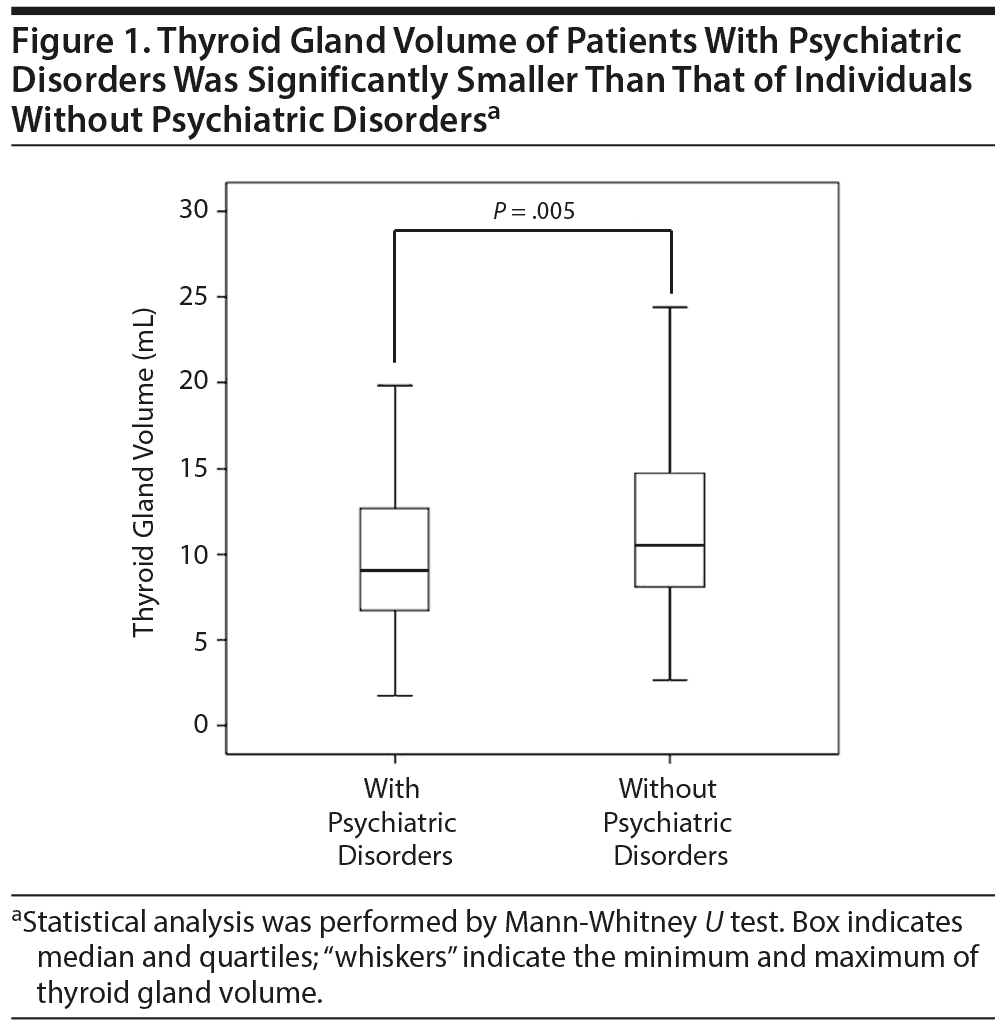
Thyroid Gland Volume Is Significantly Smaller in Patients With Psychiatric Disorders Than in Those Without Psychiatric Disorders
To the Editor: The thyroid gland normally secretes thyroxine and triiodothyronine. A previous study reported that partial substitution of triiodothyronine for thyroxine improved mood and neuropsychological functions in hypothyroid patients treated with only thyroxine,1 suggesting an importance of the integrity of the thyroid gland for neuropsychological functions. It is clear that thyroid hormone plays an important role in the brain, influencing mood and cognition; however, the detail mechanisms remain to be elucidated. Here, we investigated the differences of thyroid gland volume, thyroid hormones, and thyroid autoantibodies between individuals with and without psychiatric disorders.
Method. The study protocol was approved by the Medical Ethics Committee of the National Center for Global Health and Medicine, Tokyo. Of 282 patients who had thyroid ultrasonography between October 2011 and December 2013, we investigated 239 subjects retrospectively. We excluded subjects with autoimmune thyroid diseases and thyroid carcinoma and patients taking lithium. Eighty-one subjects were diagnosed as having psychiatric disorders including schizophrenia (35%), depression (19%), bipolar disorder (7%), neurosis (5%), anxiety disorder (11%), and mood disorders (23%) per DSM-IV criteria by psychiatrists. We measured serum levels of thyroid-stimulating hormone (TSH), free triiodothyronine (FT3), and free thyroxine (FT4) by chemiluminescent enzyme immunoassay (Lumipulse Presto, Fujirebio Inc, Tokyo, Japan). We also measured serum levels of antithyroglobulin antibodies, antithyroid peroxidase antibodies, and TSH receptor antibodies by electrochemiluminescence immunoassay (ECLusys Anti-Tg, Anti-TPO and TRAb, Roche Diagnostics KK, Tokyo, Japan). Thyroid gland volume was determined by ultrasonography for each lobe individually using Brunn’s formula: 0.479 ×— length ×— depth ×— width.2
Results. Thyroid gland volume of patients with psychiatric disorders was significantly smaller than that of individuals without psychiatric disorders (mean ± SD = 11.1 ± 9.3 mL vs 12.5 ± 7.1 mL, P = .005, Mann-Whitney U test) (Figure 1). There were no differences in serum levels of TSH, FT3, and FT4 and positivity for thyroid autoantibodies between individuals with and without psychiatric disorders. Observational epidemiologic studies reported a positive correlation of thyroid volume with body weight, body mass index, and body surface area.3 However, we did not observe significant differences in these anthropometric measurements between the 2 groups. Thyroid gland volume was not correlated with the duration of psychiatric disorders. Among physiologic factors that influence the thyroid gland volume,3,4 only age was significantly lower in patients with psychiatric disorders (50.5 ± 17.4 years, P < .001) compared with individuals without psychiatric disorders (63.7 ± 16.6 years). According to previous studies showing an inverse correlation between thyroid gland volume and age,3 our patients with psychiatric disorders showed remarkably smaller thyroid gland volume compared with individuals without psychiatric disorders for their age.
Charlier et al5 studied a correlation between suicide risk and the weight of the thyroid gland by investigating 576 autopsies, including 299 cases of completed suicide. They found that thyroid weight was significantly smaller in cases of suicide compared with those who died of other causes.5 To take their and our results into consideration, the thyroid gland volume may affect the development and severity of mood and psychiatric disorders. However, several limitations should be considered. Selection bias might have occurred in the present study, and the potential confounding factors including medications might have affected the thyroid gland volume. We cannot explain the underlying mechanisms for the association between thyroid gland volume and psychiatric disorders by the present study. Further studies will be needed to elucidate the association of thyroid gland with psychiatric disorders.
References
1. Bunevicius R, Kazanavicius G, Zalinkevicius R, et al. Effects of thyroxine as compared with thyroxine plus triiodothyronine in patients with hypothyroidism. N Engl J Med. 1999;340(6):424-429. PubMed doi:10.1056/NEJM199902113400603
2. Brunn J, Block U, Ruf G, et al. Volumetric analysis of thyroid lobes by real-time ultrasound (author’s transl) [in German]. Dtsch Med Wochenschr. 1981;106(41):1338-1340. PubMed doi:10.1055/s-2008-1070506
3. Barrרre X, Valeix P, Preziosi P, et al. Determinants of thyroid volume in healthy French adults participating in the SU.VI.MAX cohort. Clin Endocrinol (Oxf). 2000;52(3):273-278. PubMed doi:10.1046/j.1365-2265.2000.00939.x
4. Lee DH, Cho KJ, Sun DI, et al. Thyroid dimensions of Korean adults on routine neck computed tomography and its relationship to age, sex, and body size. Surg Radiol Anat. 2006;28(1):25-32. PubMed doi:10.1007/s00276-005-0042-3
5. Charlier P, Watier L, Ménétrier M, et al. Is suicide risk correlated to thyroid weight? Med Hypotheses. 2012;79(2):264-266. PubMed doi:10.1016/j.mehy.2012.05.005
Author affiliations: Department of Internal Medicine, National Center for Global Health and Medicine Kohnodai Hospital, Chiba (Drs Hamasaki and Yanai); General Internal Medicine, Community Healthcare Studies, Jichi Medical University Graduate School, Tochigi (Drs Hamasaki and Kakei), Japan.
Potential conflicts of interest: None reported.
Funding/support: This study was supported by a grant from the National Center for Global Health and Medicine (25-203).
Role of the sponsor: The sponsor had no role in the design and conduct of the study; collection, management, analysis, and interpretation of data; and preparation, review, or approval of the manuscript.
Published online: August 20, 2015.
Prim Care Companion CNS Disord 2015;17(4):doi:10.4088/PCC.15l01778
© Copyright 2015 Physicians Postgraduate Press, Inc.
Enjoy this premium PDF as part of your membership benefits!