Objective: To investigate the prevalence of statin-untreated schizophrenic patients needing treatment according to the 2013 American College of Cardiology and the American Heart Association (ACC/AHA) guidelines and to compare the performance of these guidelines to the 2004 National Cholesterol Education Program Adult Treatment Panel III (NCEP ATP-III) recommendations.
Methods: A cross-sectional study was conducted using medical charts, patient inverventions, and various anthropometric measures between April 2016 and July 2016 at the Psychiatric Hospital of the Cross enrolled 329 patients with schizophrenia (DSM-5 criteria) to determine dyslipidemia and risk for atherosclerotic cardiovascular disease (ASCVD).
Results: Of the patients, 81.25% (130 patients of 160) who need a statin therapy according to the ACC/AHA guidelines would not need a therapy according to the NCEP ATP-III, while only 9.1% of the total population met the criteria for both guidelines concomitantly. A significant difference in favor of the ACC/AHA guideline was found between the 2 guidelines (P < .001). Among the 130 patients who need a statin treatment, 124 (95.4%) had ASCVD ≥ 7.5%, 13 patients (10%) had diabetes, 1 patient (0.8%) had clinical cardiovascular disease (CVD), and none had low-density lipoprotein > 190 mg/dL.
Conclusions: Although our results showed the superiority of the 2013 ACC/AHA guidelines over the 2004 NCEP guidelines for detecting undiagnosed dyslipidemia, the absolute benefit or risk of a statin therapy according to these guideline recommendations remains unclear in this population of schizophrenic patients because the actual occurrence of CVD or statin-related adverse events was not investigated in this study. Further studies are needed to evaluate the reduction in CVD by a statin treatment according to both guidelines and thus compare the actual benefit of statin assignment in schizophrenic patients.
Untreated Dyslipidemia in Lebanese Patients With Schizophrenia
ABSTRACT
Objective: To investigate the prevalence of statin-untreated schizophrenic patients needing treatment according to the 2013 American College of Cardiology and the American Heart Association (ACC/AHA) guidelines and to compare the performance of these guidelines to the 2004 National Cholesterol Education Program Adult Treatment Panel III (NCEP ATP-III) recommendations.
Methods: A cross-sectional study was conducted using medical charts, patient inverventions, and various anthropometric measures between April 2016 and July 2016 at the Psychiatric Hospital of the Cross enrolled 329 patients with schizophrenia (DSM-5 criteria) to determine dyslipidemia and risk for atherosclerotic cardiovascular disease (ASCVD).
Results: Of the patients, 81.25% (130 patients of 160) who need a statin therapy according to the ACC/AHA guidelines would not need a therapy according to the NCEP ATP-III, while only 9.1% of the total population met the criteria for both guidelines concomitantly. A significant difference in favor of the ACC/AHA guideline was found between the 2 guidelines (P < .001). Among the 130 patients who need a statin treatment, 124 (95.4%) had ASCVD ≥ 7.5%, 13 patients (10%) had diabetes, 1 patient (0.8%) had clinical cardiovascular disease (CVD), and none had low-density lipoprotein > 190 mg/dL.
Conclusions: Although our results showed the superiority of the 2013 ACC/AHA guidelines over the 2004 NCEP guidelines for detecting undiagnosed dyslipidemia, the absolute benefit or risk of a statin therapy according to these guideline recommendations remains unclear in this population of schizophrenic patients because the actual occurrence of CVD or statin-related adverse events was not investigated in this study. Further studies are needed to evaluate the reduction in CVD by a statin treatment according to both guidelines and thus compare the actual benefit of statin assignment in schizophrenic patients.
Prim Care Companion CNS Disord 2017;19(3):17m02099
https://doi.org/10.4088/PCC.17m02099
© Copyright 2017 Physicians Postgraduate Press, Inc.
aPsychiatric Hospital of the Cross, Jal Eddib, Lebanon
bDepartment of Family Medicine, Saint-Joseph University, Beirut, Lebanon
cFaculty of Medicine, Lebanese University, Beirut, Lebanon
dFaculty of Pharmacy, Lebanese University, Beirut, Lebanon
eFaculty of Medicine, Universite Saint-Esprit Kaslik, Kaslik, Lebanon
fSchool of Pharmacy, Saint-Joseph University, Beirut, Lebanon
*Corresponding author: Marouan Zoghbi, MD, MS, Psychiatric Hospital of the Cross, PO Box 60096, Jal Eddib, Lebanon ([email protected]).
The lipid level represents an often asymptomatic feature of cardiac risk because an elevated level of low-density lipoprotein (LDL) cholesterol is one of the well-known major modifiable risk factors for the development of cardiovascular disease (CVD).1 The high prevalence of dyslipidemia can be explained by factors related to mental illness, including sedentary lifestyle, poor diet, and effects of the medications used for treatment, some of which have unfavorable effects on various metabolic risk factors for CVD.1,2 Coronary heart disease (CHD) is the number 1 cause of death in the United States.3,4
To reduce the incidence of CVD, it is essential to identify individuals at high risk.5 Cardiovascular risk stratification tools have been developed to help clinicians identify patients, particularly those with cardiovascular risk factors, who should be treated with statins.5,6 It is crucial to set the treatment threshold to weigh cardiovascular risk against adverse events of drug therapy so that undertreatment or overtreatment can be minimized.
Several guidelines are available for treatment of high blood cholesterol. In November 2013, the American College of Cardiology (ACC) and the American Heart Association (AHA) released new guidelines7 on the management of blood cholesterol designed to update and replace the previous Adult Treatment Panel III (ATP-III) report of the National Cholesterol Education Program (NCEP).8 The ATP-III guidelines were based on risk factors count and on the Framingham risk score (FRS) to guide therapy for primary prevention.7 The ACC/AHA guidelines broaden to include all hard atherosclerotic CVD (ASCVD) risk, including CHD and stroke, and developed a new ASCVD risk score. The new guidelines have been reported to potentially overestimate the observed risks of CVD in primary prevention cohorts.9,10 Furthermore, the pooled cohort risk-assessment equations were developed to predict ASCVD in non-Hispanic white and black populations.11,12 The use of this tool in our Lebanese population might be controversial.
Currently, there are still very few studies exploring the difference between the 2 guidelines in different populations, essentially in mental illness. Studies5,7,13 using the 10-year ACC/AHA ASCVD risk score found an overestimation of risk compared to the FRS. Overestimation of this risk is due to the lower cutoff point from 10% in the ATP-III guideline to 7.5% in the ACC/AHA guidelines, encouraging pharmacotherapy treatment above this risk level.14 Risk score estimation has been hypothesized to be a reflection of the CVD therapy (aspirin, lipid-lowering or antihypertensive medication, and revascularization), resulting in reduction of incident CVD events.15
Despite the availability of the guidelines, mentally ill patients often do not receive adequate recognition, monitoring, or care for their physical health conditions,16 leading to high prevalence of undetected and untreated dyslipidemia.16 The impact of application of the new ACC/AHA guidelines to a sensitive population such as psychiatric patients has not been studied.
We investigated the prevalence of statin-untreated patients with schizophrenia needing treatment according to the 2013 ACC/AHA guidelines and compared the performance of these guidelines to the 2004 NCEP ATP-III recommendations.
METHODS
Study Design
A cross-sectional study was conducted between April and July 2016 at the Psychiatric Hospital of the Cross, the largest center for the management of psychiatric disorders in Lebanon. The study protocol was reviewed and approved by the research and ethics committee of the hospital, and subjects provided informed consent.
Study Population
Hospitalized patients aged 18 to 75 years, diagnosed with all types of schizophrenia according to the DSM-5,17 and receiving at least 1 antipsychotic agent for more than 6 weeks were included in the study. Patients treated with a statin at the time of the study and patients suffering from terminal illness affecting lipid levels were excluded.
Sample Size Calculation
A sample of 323 patients was targeted to allow for adequate power (80%) for bivariate analyses to be carried out according to the Epi info sample size calculations with a population size of 40,000 psychiatric patients in Lebanon, an expected frequency of lipid disorder in schizophrenics of 69.9%,15 and 5% confidence limits.18 We distributed 400 questionnaires to take refusals into account.
Questionnaire and Variables
Demographic information (age, sex, geographic region, marital status, employment, educational level, monthly income per house), clinical information of the participants (diagnosis, duration of illness, history of medical illness, and family history of mental disorders), and medication intake at the time of the study were noted from medical records. Social habits of the participants (smoking, alcohol intake) were also collected from the patients via a face-to-face interview.
To assess the participants’ physical activity, we used a self-reporting questionnaire (Framingham Study: Exercise and Physical Activity Questionnaire19) designed for this purpose. The questionnaire was administered in Arabic, the native language in Lebanon.
Assessments of Undiagnosed Dyslipidemia
According to ACC/AHA guidelines,12 statin therapy is recommended for the following:
- Patients with low-density lipoprotein (LDL) ≥ 190 mg/dL
- Patients with diabetes mellitus
- Patients without diabetes but with LDL > 190 mg/dL
- Patients with a 10-year ASCVD risk ≥ 7.5% based on the new pooled cohort risk score.
According to NCEP ATP-III guidelines,20 statin therapy is recommended for the following subcategories:
- Patients with no risk factor or single risk factor (0–1 risk factor) and having an LDL ≥ 190 mg/dL
- Patients with multiple (≥ 2) risk factors whose 10-year risk for hard CHD is > 20% and LDL > 100 mg/dL
- Patients with multiple (≥ 2) risk factors whose 10-year risk for hard CHD is 10%–20% and LDL ≥ 130 mg/dL
- Patients with multiple (≥ 2) risk factors whose 10-year risk for hard CHD is < 10% and LDL ≥ 160 mg/dL.
The risk factors were defined as follows: smoking, hypertension, diabetes, and age (men ≥ 45 years, women ≥ 55 years).20
Laboratory Analysis
Blood samples were drawn from the antecubital vein between 6:00 am and 7:00 am after an overnight fasting (12 hours of fasting) to screen for dyslipidemia. Total cholesterol, high-density lipoprotein cholesterol, LDL cholesterol, and triglycerides were measured by the COBAS INTEGRA 400 plus machine (Roche Diagnostics, Indianapolis, Indiana).
Anthropometric Measures
Participants’ height, weight, and waist circumference were measured with the detecto model 339 balance and a tape meter. Body mass index (BMI) was calculated using the formula body weight (in kilograms) divided by the square of the height (in meters) and classified according to World Health Organization criteria21: underweight (< 18.5), normal (18.5–24.9), overweight (25.0–29.9), and obese (≥ 30.0).
The waist circumference was considered in the normal range, according to NCEP ATP-III guidelines for definition of metabolic syndrome, if the value was < 102 cm for men and < 88 cm for women.
Blood pressure was measured using a sphygmomanometer (ALPK2, a professional traditional aneroid blood pressure monitor). Two blood pressure measurements were made in the upper arm, spaced 1 to 2 minutes apart, by 2 qualified registered nurses, and additional measurements were done if the first 2 were not similar. In this study, the highest reading was taken into account. According to NCEP ATP-III and Eighth Joint National Committee22 guidelines, abnormal blood pressure was considered over 140/90 mm Hg. Patients were considered hypertensive if they were treated with an antihypertensive medication according to their medical file.
Data Analysis
Data entry and analysis were performed on SPSS software version 22 (SPSS Inc, Chicago, Illinois). The independent sample t test was used when comparing 2 groups’ means. Pearson correlation coefficient was used to correlate between quantitative variables. For categorical variables, the χ2 and Fisher exact tests were used when applicable. Significance was defined as a P value < .05.
RESULTS
Baseline Characteristics of the Study Sample
Of the 400 patients, 329 (82.25%) were enrolled in the study, while 71 patients refused to participate. Details regarding sociodemographic and clinical characteristics of the patients are shown in Table 1. The mean ± SD age of the participants was 52.00 ± 12.76 years. Most of them were men (72.9%) and single (85.7%) and had an intermediate level of education, as defined by primary or complementary education (65.7%). The mean ± SD duration of hospitalization was 11.54 ± 11.17 years, while the mean duration of illness was 25.01 ± 13.10 years. In addition, 48% were overweight or obese, and the rest had normal BMIs (51.4%).

Patients Needing Statin Treatment According to
ACC/AHA and NCEP ATP-III Guidelines
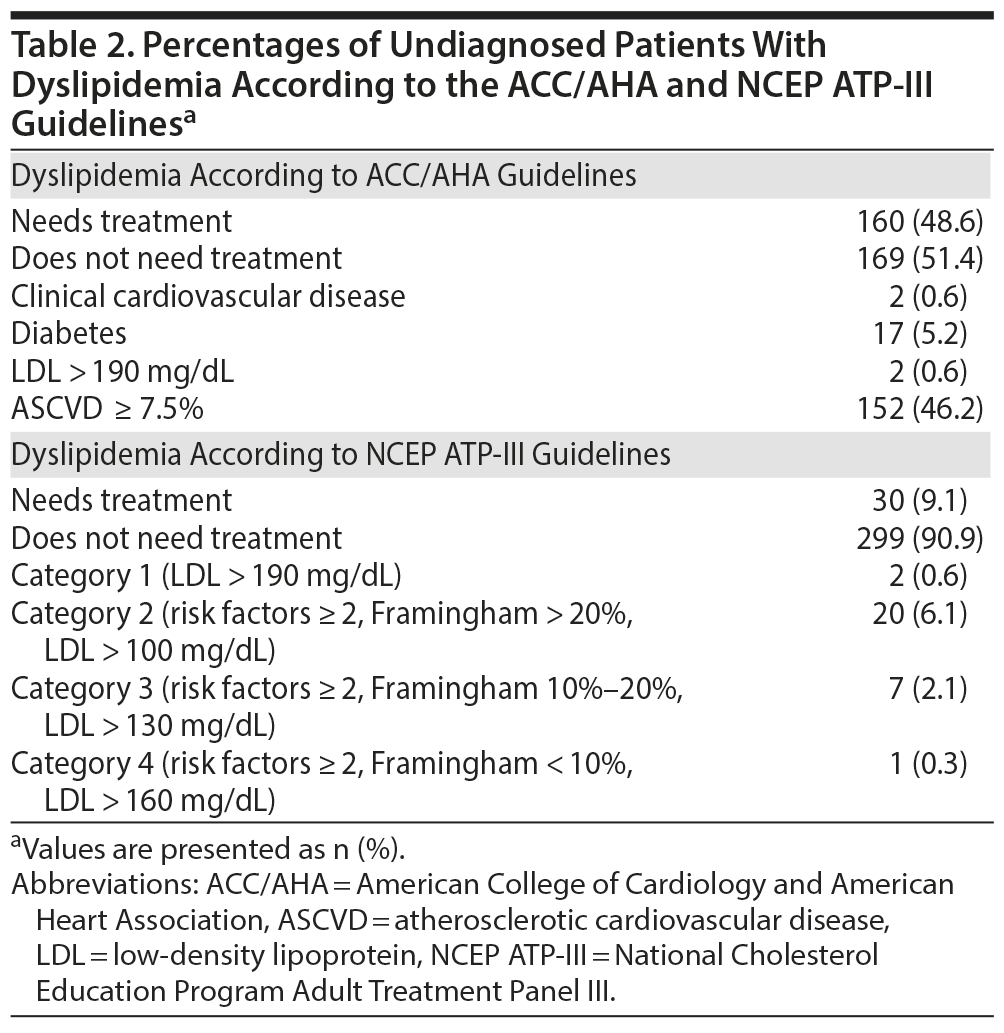
According to the ACC/AHA guidelines, 160 patients (48.6%) needed treatment for dyslipidemia. We found that 152 patients (46.2%) needed treatment because of a high ASCVD score (> 7.5%), 17 patients (5.2%) needed treatment because of diabetes, 2 patients (0.6%) had an LDL level > 190 mg/dL, and 2 patients had clinical CVD (0.6%).
When applying the NCEP ATP-III guidelines to this population, 30 patients (9.1%) needed treatment. Two patients (0.6%) were classified in category 1; 20 patients (6.1%) in category 2; 7 patients (2.1%) in category 3; and 1 patient (0.3%) in category 4 (Table 2).
Bivariate Analysis
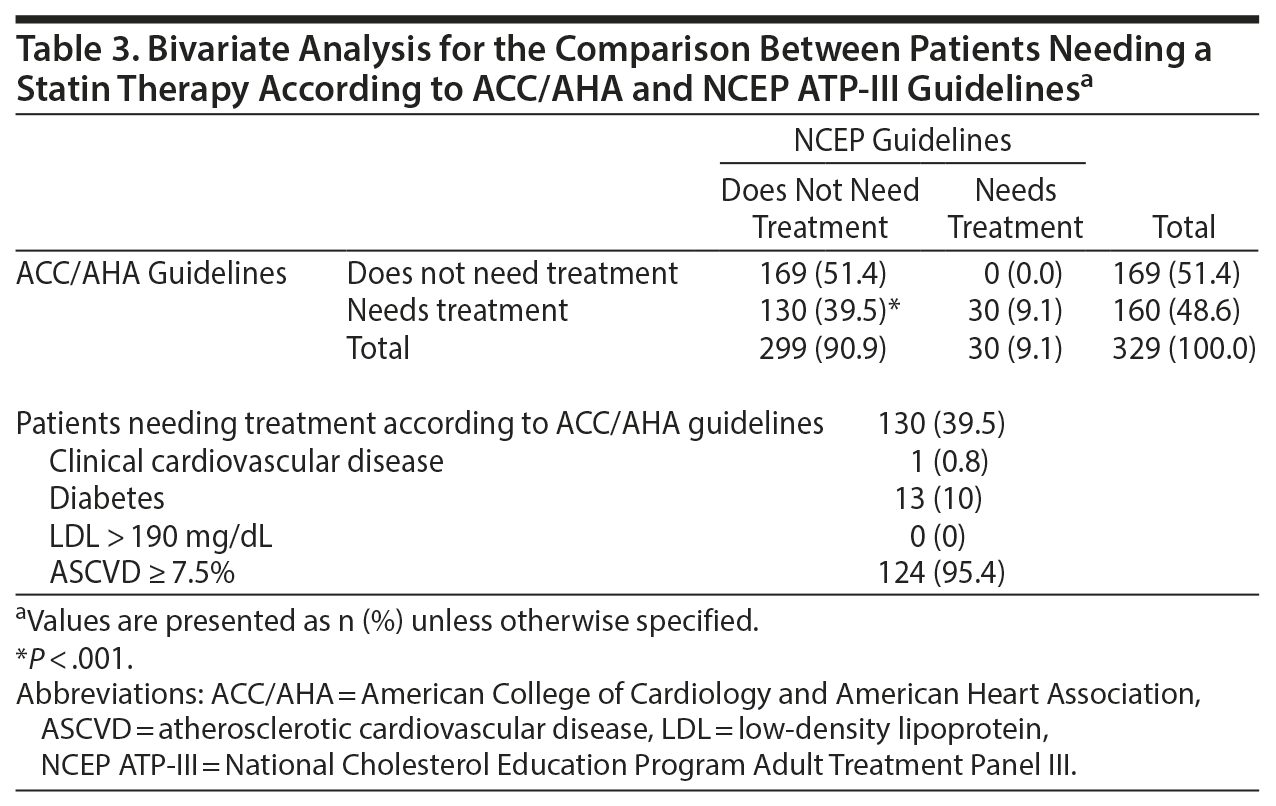
Of the patients who needed a statin therapy according to the ACC/AHA guidelines, 81.25% (130 patients of 160) would not need therapy according to the NCEP ATP-III, and only 9.1% of the total population met the criteria for both guidelines concomitantly. A significant difference in favor of the ACC/AHA guidelines was found between the 2 guidelines (P < .001) (Table 3). Among these 130 patients who needed a statin treatment, 124 (95.4%) had ASCVD > 7.5%, 13 (10%) had diabetes, 1 (0.8%) had clinical CVD, and none had LDL > 190 mg/dL.
Guideline Performance Comparison
Figure 1 shows the distribution of 10-year risk score categories for the ACC/AHA and NCEP ATP-III. The results showed that the percentage of low-risk patients (< 7.5% ASCVD score or < 10% FRS score) was 46.0% and 60.8%, respectively, whereas the percentage of high-risk patients (ASCVD score ≥ 7.5% or FRS score > 10%) was 54.0% and 39.2%, respectively.
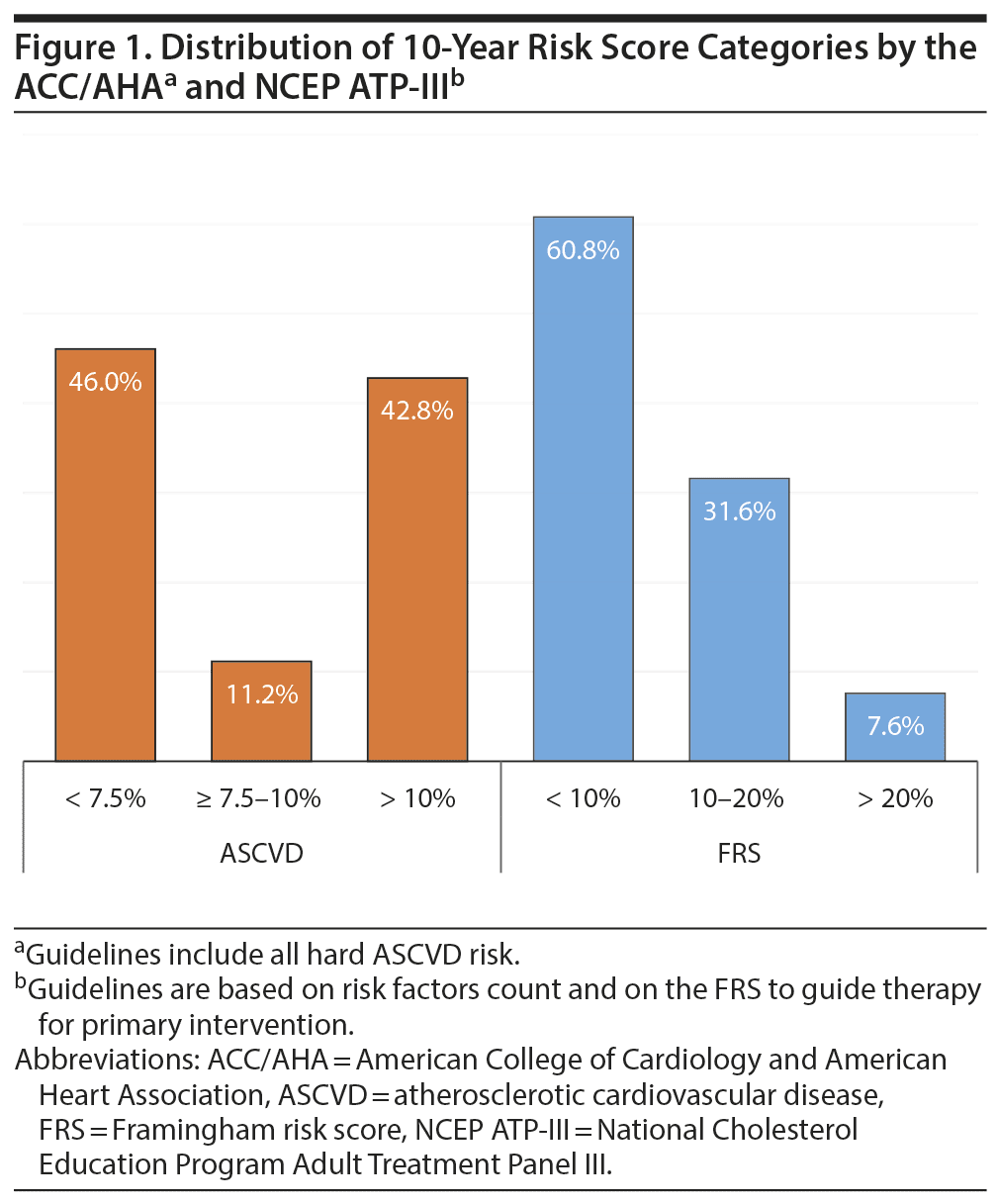
The mean ± SD value of ASCVD risk score is 10.39 ± 7.21 compared to 8.76 ± 6.92 for FRS. The 2 scores were highly and significantly correlated (r = 0.80, P < .001).
DISCUSSION
Cardiovascular mortality remains the major cause of death in patients with schizophrenia. While unnatural causes of death are declining with advances in treatment and multidisciplinary approaches, the rate of cardiovascular mortality is still increasing over time.23 Multiple prospective studies24–27 showed that LDL cholesterol is a major risk factor for the development of CVD; treatment with a statin is recommended to reduce the risk of cardiovascular and cerebrovascular events in high-risk patients.28
Our study showed a high prevalence of patients needing but not receiving treatment. This prevalence goes from approximately 9% to 49% depending on the guidelines adopted for decision-making.
These results are in concordance with previous published results on similar populations. Lahti et al29 showed that despite higher cardiovascular mortality rates in patients with schizophrenia, lipid-lowering agent use was low. Other sources indicate that approximately one-third of eligible patients receive lipid-lowering therapy30,31 or meet desirable LDL goals.32
Defining the threshold to treat with the best benefit to adverse effects ratio has been debated in almost all guidelines. The main difference is in favor of more treatment for the ACC guidelines and is driven mainly by the lower treatment threshold adopted in these guidelines and the greater proportion of patients labeled as high risk when using the ASCVD compared to the Framingham score.
The ATP-III guidelines proposed a revised treatment protocol for LDL cholesterol–lowering therapy based on risk factors count and the Framingham risk of coronary heart disease.20 The ACC/AHA guidelines lowered the threshold to treat to 7.5% risk of nonfatal myocardial infarction (heart attack), coronary heart disease death, or stroke. These guidelines have been used in psychiatric settings,33 and the cost-effectiveness of the 7.5% threshold has been shown acceptable for the primary care setting.34 The last study34 showed that the results are sensitive to patient preference for taking a pill a day, the statin price, and the risk of diabetes.
Patient adherence in the psychiatric setting needs deeper investigation. Schizophrenia has been shown to correlate with better adherence to statin treatment in a study by Owen-Smith et al.35
Statin treatment can lead to well-documented side effects such as hepatic and muscular side effects. Muscular side effect incidence ranges between 1.5% and 10%.36 These side effects are usually of benign nature but can have negative effect on the autonomy of patients with schizophrenia in our opinion. Our experience suggests that hepatic side effects are of concern in schizophrenia because the usual polymedication in this type of patient leads to increased risk of this complication.
Cederberg et al37 found an increased risk of statin-induced diabetes of 46%, with higher doses inducing more diabetes in patients with and without impaired glucose metabolism. Despite this increased diabetes risk, an analysis by Castro et al38 showed a net benefit in favor of statin use despite this increased risk of diabetes when compared to the remarkable reduction in mortality. The risk of diabetes is of special interest in psychiatric patients because of the background risk associated with neuroleptic use.39 Atypical antipsychotics have been shown to increase the metabolic and diabetes risks.40–42
On the other hand, prescribing statins to patients with schizophrenia may cause significant drug-drug interactions in this heavily treated population. A recent review43 of drug interactions with statins showed a potential for interactions with some antidepressants and antiepileptics, classes of drugs usually used in the treatment of some forms of psychosis, while no direct interaction was found with neuroleptics.
Schizophrenia is by itself a chronic and debilitating disease that predisposes patients to coronary artery disease (CAD). The natural progression of schizophrenia, genetics, and the sequelae of treatment all increase the development of CAD risk factors.44
Initiatives are needed to ensure that the burden of CAD in schizophrenic patients is controlled and does not continue to rise. These initiatives include ongoing monitoring for CAD risk factors and improved communication between psychiatrists and consulting/family physicians.44 The Clinical Antipsychotic Trials of Intervention Effectiveness study45 baseline data indicate that dyslipidemia is not being actively screened for or treated, corroborating our results that highlight the need for active screening for hyperlipidemia in patients treated for schizophrenia and for a thoughtful approach in prescribing statins, while keeping the possible side effects and drug-drug interactions in mind. Monitoring for these side effects is equally needed. Future research should focus on the predictive value of the previously described scores for cardiac and vascular events in this specific high-risk population.
LIMITATIONS
Our study has some limitations. The cross-sectional design does not reflect the effect of follow-up treatment and its correlation with cardiac risk factor. Randomized, prospective trials are necessary to examine possible differential effects of specific antipsychotics on cardiac risk factors.
The study was constrained by the lack of validation of the Framingham and ASCVD risk score in the Lebanese population with serious mental illness. While the Framingham formula is valid across many populations and the ASCVD risk score is newly utilized, these equations have not been validated in schizophrenic populations taking antipsychotics. Future research should aim at validating the current CVD risk score or develop one specific for this high-risk population.
Finally, the evaluation of lifestyle activity was done through a direct interview; the information collected directly from patients could have been affected by the low level of cognition and the negative effect of antipsychotic treatment.
CONCLUSION
Although our results showed the superiority of the 2013 ACC/AHA guidelines over the 2004 NCEP ATP-III guidelines for detecting undiagnosed dyslipidemia, the absolute benefit or risk of a statin therapy according to these guideline recommendations remains unclear in this population of schizophrenic patients because the actual occurrence of CVD or statin-related adverse events was not investigated in this study. Further studies are needed to evaluate the reduction in CVD by a statin treatment according to both guidelines and compare the actual benefit of statin assignment in schizophrenic patients.
Submitted: January 20, 2017; accepted March 6, 2017.
Published online: May 18, 2017.
Potential conflicts of interest: None.
Funding/support: Pharmaline funded the laboratory tests.
Role of the sponsor: Pharmaline had no input or contribution to the study design, interpretation, or preparation of the manuscript.
REFERENCES
1. Vanderlip ER, Fiedorowicz JG, Haynes WG. Screening, diagnosis, and treatment of dyslipidemia among persons with persistent mental illness: a literature review. Psychiatr Serv. 2012;63(7):693–701. PubMed doi:10.1176/appi.ps.201100475
2. Newcomer JW, Hennekens CH. Severe mental illness and risk of cardiovascular disease. JAMA. 2007;298(15):1794–1796. PubMed doi:10.1001/jama.298.15.1794
3. Thom T, Haase N, Rosamond W, et al; American Heart Association Statistics Committee and Stroke Statistics Subcommittee. Heart disease and stroke statistics–2006 update: a report from the American Heart Association Statistics Committee and Stroke Statistics Subcommittee. Circulation. 2006;113(6):
e85–e151. PubMed doi:10.1161/CIRCULATIONAHA.105.171600
4. Braunwald E, Antman EM, Beasley JW, et al; American College of Cardiology; American Heart Association. Committee on the Management of Patients With Unstable Angina. ACC/AHA 2002 guideline update for the management of patients with unstable angina and non-ST-segment elevation myocardial infarction–summary article: a report of the American College of Cardiology/American Heart Association task force on practice guidelines (Committee on the Management of Patients With Unstable Angina). J Am Coll Cardiol. 2002;40(7):1366–1374. PubMed doi:10.1016/S0735-1097(02)02336-7
5. Kavousi M, Leening MJ, Nanchen D, et al. Comparison of application of the ACC/AHA guidelines, Adult Treatment Panel III guidelines, and European Society of Cardiology guidelines for cardiovascular disease prevention in a European cohort. JAMA. 2014;311(14):1416–1423. PubMed doi:10.1001/jama.2014.2632
6. Saravane D. Dyslipidemia and Mental Illness. In: Kelishadi R, ed. Dyslipidemia–From Prevention to Treatment. Rijeka, Croatia: INTECH Open Access; 2012. doi:10.5772/27686
7. DeFilippis AP, Young R, Carrubba CJ, et al. An analysis of calibration and discrimination among multiple cardiovascular risk scores in a modern multiethnic cohort. Ann Intern Med. 2015;162(4):266–275. PubMed doi:10.7326/M14-1281
8. Grundy SM, Cleeman JI, Merz CN, et al; Coordinating Committee of the National Cholesterol Education Program. Implications of recent clinical trials for the National Cholesterol Education Program Adult Treatment Panel III guidelines. Arterioscler Thromb Vasc Biol. 2004;24(8):e149–e161. PubMed doi:10.1161/01.ATV.0000133317.49796.0E
9. Ridker PM, Cook NR. Statins: new American guidelines for prevention of cardiovascular disease. Lancet. 2013;382(9907):1762–1765. PubMed doi:10.1016/S0140-6736(13)62388-0
10. Chia YC, Lim HM, Ching SM. Validation of the pooled cohort risk score in an Asian population: a retrospective cohort study. BMC Cardiovasc Disord. 2014;14:163. PubMed doi:10.1186/1471-2261-14-163
11. Arai H, Sasaki J, Teramoto T. Comment on the new guidelines in USA by the JAS guidelines committee. J Atheroscler Thromb. 2014;21(2):79–81. PubMed doi:10.5551/jat.ED001
12. Stone NJ, Robinson JG, Lichtenstein AH, et al; American College of Cardiology/American Heart Association Task Force on Practice Guidelines. 2013 ACC/AHA guideline on the treatment of blood cholesterol to reduce atherosclerotic cardiovascular risk in adults: a report of the American College of Cardiology/American Heart Association Task Force on Practice Guidelines. Circulation. 2014;129(suppl 2):S1–S45. PubMed doi:10.1161/01.cir.0000437738.63853.7a
13. Chia YC, Lim HM, Ching SM. Does use of pooled cohort risk score overestimate the use of statin? a retrospective cohort study in a primary care setting. BMC Fam Pract. 2014;15:172. PubMed doi:10.1186/s12875-014-0172-y
14. Gupta A, Jadhav A, Petkar S, Dubey V. Study of lipid derangement in psychiatric disorder. Indian Medical Gazette. 2013;147(7):253–256.
15. DE Hert M, Schreurs V, Vancampfort D, et al; M DEH. Metabolic syndrome in people with schizophrenia: a review. World Psychiatry. 2009;8(1):15–22. PubMed doi:10.1002/j.2051-5545.2009.tb00199.x
16. Holt RI, Abdelrahman T, Hirsch M, et al. The prevalence of undiagnosed metabolic abnormalities in people with serious mental illness. J Psychopharmacol. 2010;24(6):867–873. PubMed doi:10.1177/0269881109102788
17. American Psychiatric Association. Diagnostic and Statistical Manual of Mental Disorders. Fifth Edition. Arlington, VA: American Psychiatric Association; 2013.
18. Centers for Disease Control and Prevention. Epi Info. CDC website. https://www.cdc.gov/epiinfo/.
19. National Cancer Institute, Division of Cancer and Epidemiology and Genetics, Framingham Study: Exercise & Physical Activity Questionnaire, the Framingham Heart Study. Arch Intern Med 1979. NIH website. http://dceg.cancer.gov/tools/design/questionnaires/physical-activity/framingham-study-physical-activity. Accessed April 26, 2017.
20. Expert Panel on Detection, Evaluation, and Treatment of High Blood Cholesterol in Adults. Executive Summary of the third report of the National Cholesterol Education Program (NCEP) Expert Panel on Detection, Evaluation, and Treatment of High Blood Cholesterol in Adults (Adult Treatment Panel III). JAMA. 2001;285(19):2486–2497. PubMed doi:10.1001/jama.285.19.2486
21. World Health Organization. BMI classification. WHO website. http://apps.who.int/bmi/index.jsp?introPage=intro_3.html. Updated June 2013. Accessed April 26, 2017.
22. James PA, Oparil S, Carter BL, et al. 2014 evidence-based guideline for the management of high blood pressure in adults: report from the panel members appointed to the Eighth Joint National Committee (JNC 8). JAMA. 2014;311(5):507–520. PubMed doi:10.1001/jama.2013.284427
23. Bushe CJ, Taylor M, Haukka J. Mortality in schizophrenia: a measurable clinical endpoint. J Psychopharmacol. 2010;24(suppl 4):17–25. PubMed doi:10.1177/1359786810382468
24. Bonithon-Kopp C, Scarabin P-Y, Taquet A, et al. Risk factors for early carotid atherosclerosis in middle-aged French women. Arterioscler Thromb. 1991;11(4):966–972. PubMed doi:10.1161/01.ATV.11.4.966
25. Giral P, Filitti V, Levenson J, et al; PCV Metra Group. Relation of risk factors for cardiovascular disease to early atherosclerosis detected by ultrasonography in middle-aged normotensive hypercholesterolemic men. Atherosclerosis. 1990;85(2-3):151–159. PubMed doi:10.1016/0021-9150(90)90106-S
26. Wu KK, Folsom AR, Heiss G, et al. Association of coagulation factors and inhibitors with carotid artery atherosclerosis. Early results of the Atherosclerosis Risk in Communities (ARIC) Study. Ann Epidemiol. 1992;2(4):471–480. PubMed doi:10.1016/1047-2797(92)90097-A
27. Heiss G, Sharrett AR, Barnes R, et al. Carotid atherosclerosis measured by B-mode ultrasound in populations: associations with cardiovascular risk factors in the ARIC study. Am J Epidemiol. 1991;134(3):250–256. PubMed doi:10.1093/oxfordjournals.aje.a11607828. World Health Organization. Prevention of Cardiovascular Disease: Pocket Guidelines for Assessment and Management of Cardiovascular risk: Geneva, Switzerland: World Health Organization; 2007.
29. Lahti M, Tiihonen J, Wildgust H, et al. Cardiovascular morbidity, mortality and pharmacotherapy in patients with schizophrenia. Psychol Med. 2012;42(11):2275–2285. PubMed doi:10.1017/S0033291712000396
30. Gotto AM Jr. Lipid management in patients at moderate risk for coronary heart disease: insights from the Air Force/Texas Coronary Atherosclerosis Prevention Study (AFCAPS/TexCAPS). Am J Med. 1999;107(2A):36S–39S. PubMed doi:10.1016/S0002-9343(99)00145-X
31. Durrington P. The human and economic costs of undertreatment with statins. Int J Clin Pract. 2002;56(5):357–368. PubMed
32. Pearson TA. The undertreatment of LDL-cholesterol: addressing the challenge. Int J Cardiol. 2000;74(suppl 1):S23–S28. PubMed doi:10.1016/S0167-5273(99)00108-4
33. McCarron RM. Integrated care at the interface of psychiatry and primary care: prevention of cardiovascular disease. Psychiatr Clin North Am. 2015;38(3):463–474. PubMed doi:10.1016/j.psc.2015.05.005
34. Pandya A, Sy S, Cho S, et al. Cost-effectiveness of 10-year risk thresholds for initiation of statin therapy for primary prevention of cardiovascular disease. JAMA. 2015;314(2):142–150. PubMed doi:10.1001/jama.2015.6822
35. Owen-Smith A, Stewart C, Green C, et al. Adherence to common cardiovascular medications in patients with schizophrenia vs patients without psychiatric illness. Gen Hosp Psychiatry. 2016;38:9–14. PubMed doi:10.1016/j.genhosppsych.2015.07.010
36. Auer J, Sinzinger H, Franklin B, et al. Muscle- and skeletal-related side-effects of statins: tip of the iceberg? Eur J Prev Cardiol. 2016;23(1):88–110. PubMed doi:10.1177/2047487314550804
37. Cederberg H, Stančáková A, Yaluri N, et al. Increased risk of diabetes with statin treatment is associated with impaired insulin sensitivity and insulin secretion: a 6-year follow-up study of the METSIM cohort. Diabetologia. 2015;58(5):1109–1117. PubMed doi:10.1007/s00125-015-3528-5
38. Castro MR, Simon G, Cha SS, et al. Statin use, diabetes incidence and overall mortality in normoglycemic and impaired fasting glucose patients. J Gen Intern Med. 2016;31(5):502–508. PubMed doi:10.1007/s11606-015-3583-0
39. American Diabetes Association; American Psychiatric Association; American Association of Clinical Endocrinologists; North American Association for the Study of Obesity. Consensus development conference on antipsychotic drugs and obesity and diabetes. Diabetes Care. 2004;27(2):596–601. PubMed doi:10.2337/diacare.27.2.596
40. Wirshing DA, Spellberg BJ, Erhart SM, et al. Novel antipsychotics and new onset diabetes. Biol Psychiatry. 1998;44(8):778–783. PubMed doi:10.1016/S0006-3223(98)00100-0
41. Foley DL, Mackinnon A, Morgan VA, et al. Effect of age, family history of diabetes, and antipsychotic drug treatment on risk of diabetes in people with psychosis: a population-based cross-sectional study. Lancet Psychiatry. 2015;2(12):1092–1098. PubMed doi:10.1016/S2215-0366(15)00276-X
42. Wu C-S, Gau SS-F. Association between antipsychotic treatment and advanced diabetes complications among schizophrenia patients with type 2 diabetes mellitus. Schizophr Bull. 2016;42(3):703–711. PubMed doi:10.1093/schbul/sbv187
43. Wiggins BS, Saseen JJ, Page RL 2nd, et al; American Heart Association Clinical Pharmacology Committee of the Council on Clinical Cardiology; Council on Hypertension; Council on Quality of Care and Outcomes Research; and Council on Functional Genomics and Translational Biology. Recommendations for management of clinically significant drug-drug interactions with statins and select agents used in patients with cardiovascular disease: a scientific statement from the American Heart Association. Circulation. 2016;134(21):e468–e495. PubMed doi:10.1161/CIR.0000000000000456
44. Ignaszewski MJ, Yip A, Fitzpatrick S. Schizophrenia and coronary artery disease.
B C Med J. 2015;57(4):154–157.
45. Stroup TS, McEvoy JP, Swartz MS, et al. The National Institute of Mental Health Clinical Antipsychotic Trials of Intervention Effectiveness (CATIE) project: schizophrenia trial design and protocol development. Schizophr Bull. 2003;29(1):15–31. PubMed doi:10.1093/oxfordjournals.schbul.a006986
Enjoy this premium PDF as part of your membership benefits!


