Wernicke-Korsakoff syndrome (WKS) is a life-threatening and underdiagnosed neuropsychiatric condition caused by thiamine deficiency that comprises Wernicke encephalopathy and Korsakoff syndrome. Although mainly associated with chronic alcoholism, WKS can arise from other circumstances. This report describes a series of cases of WKS that were clinically evaluated by liaison psychiatrists on a nonpsychiatric inpatient unit. The cases illustrate a deficit in the recognition and adequate treatment of WKS, demonstrating its clinical complexity and the need to improve physicians’ knowledge.
ABSTRACT
Wernicke-Korsakoff syndrome (WKS) is a life-threatening and underdiagnosed neuropsychiatric condition caused by thiamine deficiency that comprises Wernicke encephalopathy and Korsakoff syndrome. Although mainly associated with chronic alcoholism, WKS can arise from other circumstances. This report describes a series of cases of WKS that were clinically evaluated by liaison psychiatrists on a nonpsychiatric inpatient unit. The cases illustrate a deficit in the recognition and adequate treatment of WKS, demonstrating its clinical complexity and the need to improve physicians’ knowledge.
Prim Care Companion CNS Disord 2020;22(3):19br02538
To cite: Barata PC, Serrano R, Afonso H, et al. Wernicke-Korsakoff syndrome: a case series in liaison psychiatry. Prim Care Companion CNS Disord. 2020;22(3):19br02538.
To share: https://doi.org/10.4088/PCC.19br02538
© Copyright 2020 Physicians Postgraduate Press, Inc.
aDepartment of Psychiatry, Prof. Dr. Fernando da Fonseca Hospital, Amadora, Portugal
bDepartment of Psychiatry, Centro Hospitalar Barreiro-Montijo, Barreiro, Portugal
*Corresponding author: Pedro C. Barata, MD, Department of Psychiatry, Prof. Dr. Fernando da Fonseca Hospital, IC19, 2720-276 Amadora, Portugal ([email protected]).
Wernicke-Korsakoff syndrome (WKS) is a potentially lethal neuropsychiatric condition caused by thiamine deficiency.1-5 This syndrome includes Wernicke encephalopathy and Korsakoff syndrome and frequently occurs in patients with chronic alcoholism.1-4,6 Nevertheless, WKS may also be precipitated by several illnesses unrelated to alcohol, such as malnutritional and hypermetabolic states,1-3 several gastrointestinal tract diseases (eg, pancreatitis, obstruction, Crohn’s disease), hyperemesis gravidarum, human immunodeficiency virus infection,1 or psychiatric disorders (eg, schizophrenia spectrum, anorexia nervosa).1,5 WKS can be iatrogenic, occurring for instance in hemodialyzed patients1,2 or in intravenous feeding1 (providing glucose before thiamine is known to precipitate this syndrome5). WKS is underdiagnosed in most patients.4-8
Classically, Wernicke encephalopathy is associated with a triad of symptoms: mental status changes, ophthalmoplegia, and ataxia. However, these symptoms occur in only 20%-30% of cases.4,5 Caine criteria9 allow the diagnosis of Wernicke encephalopathy in the presence of at least 2 of 4 signals: (1) dietetic deficiencies, (2) oculomotor abnormalities, (3) cerebellar dysfunction, or (4) mental state changes or mild memory deficits.2,3 Wernicke encephalopathy is a potentially reversible medical emergency,2,3,5,6 leading to death in 20% of cases.6 Residual symptoms are common,5 as is the progression to Korsakoff syndrome.3,5,6 In Wernicke encephalopathy, early treatment with high doses of parenteral thiamine can reduce the probability of progression to Korsakoff syndrome3 and improve prognosis.6
Korsakoff syndrome can be defined as a probably permanent neuropsychiatric condition that usually follows an episode of Wernicke encephalopathy,3,5 mainly characterized by a retrograde and anterograde amnesia3,5,6 in a patient with apparent clear consciousness.3 Provoked confabulations are common.6

- Wernicke-Korsakoff syndrome is not rare nor is it exclusive to alcoholics.
- Wernicke-Korsakoff syndrome can occur in malnutritional and hypermetabolic states, gastrointestinal tract diseases, hyperemesis gravidarum, human immunodeficiency virus infection, and psychiatric disorders and can be iatrogenic.
- A shift from the classical Wernicke-Korsakoff syndrome clinical triad to a greater use and awareness of Caine criteria would most certainly increase detection rates.
Deaths associated with WKS are often caused by comorbid diseases, namely cirrhosis or infections—unspecified infections are commonly reported.4 Bronchopneumonia has been reported to be a common specific related infection.4
This report describes a series of cases of WKS that were clinically evaluated by the liaison psychiatrists of the Prof. Dr. Fernando da Fonseca Hospital, Amadora, Portugal, in the nonpsychiatric inpatient units between October 2017 and March 2018.
CASE DESCRIPTIONS
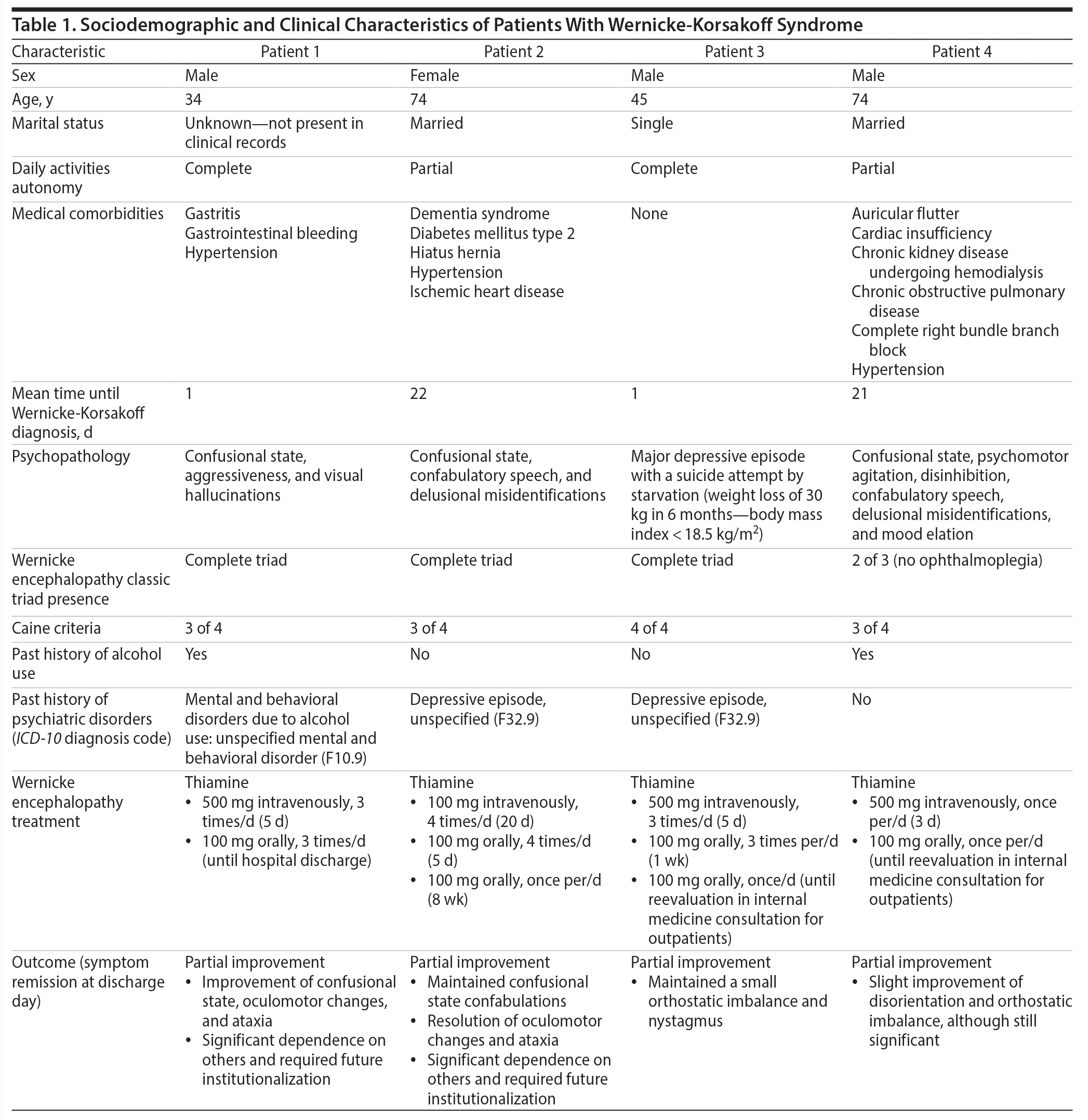
We identified 4 cases of patients with WKS through medical record review. Their sociodemographic and clinical features are presented in Table 1. All patients had symptomatic WKS diagnosed in medical units on the basis of a detailed anamnesis, complementary diagnostic examination, and a clinical presentation consistent with this diagnosis. Three of four patients had the classic Wernicke encephalopathy triad—1 patient had no ophthalmoplegia. All patients met more than 2 Caine criteria.
Patient 2 had dementia prior to WKS onset (see Table 1). However, we are not in a position to state categorically the degree of severity or how or if the dementia contributed to the behaviors leading to WKS.
All patients received psychotropic drugs: antipsychotics to control confusional states and psychomotor agitation (patients 1, 2, and 4), benzodiazepines for the prevention of alcohol withdrawal syndrome (patient 1), and antidepressants for the treatment of a major depressive episode with suicidal ideation (patient 3). All 4 patients were given thiamine to treat WKS (see Table 1 for dosage details). WKS improvement was partial in all cases. Two patients progressed to a significant dependence on others and required future institutionalization.
DISCUSSION
Half of the WKS cases occurred in the sequence of hunger or malnutrition and not in an alcoholic context. Patient 4’s presentation seemed to correspond to an iatrogenic Wernicke encephalopathy diagnosis.
Notwithstanding the sample size, it is important to highlight that WKS manifested the complete classic triad in 75% of the cases—a significant difference from the 15%-30% mentioned in the scientific literature.5 In contrast, all patients fulfilled Caine criteria.
Diagnosis was delayed in the patients with more clinical comorbidities, which may be due to the attribution of WKS symptoms to already existing pathologies. As clinical examination remains the standard in diagnosing WKS, and the classic signs of such a syndrome have low sensitivity, a shift to greater use and awareness of the Caine criteria would most certainly increase WKS detection rates. Other factors that could improve WKS diagnosis include clarifying misconceptions about WKS, as it is not rare or exclusive to alcoholics, and being aware of the associated nonalcoholic medical conditions.4
There are clinical guidelines to support the clinical management of Wernicke encehalopathy.2,4,7,10-12 The Royal College of Physicians guidelines13 recommend that thiamine 500 mg be given parenterally 3 times per day for at least 3 days. If there is any improvement, it is advised to continue thiamine at 250 mg/d parenterally for 5 days. The guidelines13 also recommend that all hypoglycemic patients (who are treated intravenously [IV] with glucose) with evidence of chronic alcohol ingestion be given IV thiamine immediately because IV glucose without thiamine may acutely precipitate Wernicke encephalopathy.2,4 For the treatment of suspected or manifest Wernicke encephalopathy, the European Federation of Neurologic Societies10recommends that thiamine 200 mg be given before any carbohydrate 3 times per day, preferably IV diluted with 100 mL of normal saline and given over 30 minutes. Treatment should be continued until there is no further improvement in signs and symptoms.2,4,10 There is insufficient evidence of the efficacy of thiamine for the treatment of Wernicke-Korsakoff syndrome, and recommendations about the dosage and duration of treatment are acknowledged to be arbitrary.9,11 In half of the cases identified here, the administered doses were lower than those of the recommendations, therefore limiting the treatment’s therapeutic potential.
The partial recovery verified in all cases aligns with data from the literature. The residual symptomatology identified in patient 2 (one of the cases concerning subtherapeutic thiamine administration) included confabulations, a possible progression from Wernicke encephalopathy to Korsakoff syndrome.
It is important to highlight that this report does not specify the medical investigations that indicated that WKS was the most probable etiology (which were elaborated by the medical doctors from the hospital units were the patients were admitted). We consider this a limitation because 3 of 4 patients had several comorbidities that could constitute confusional state causes (eg, hypertension, cardiac insufficiency, dementia, ischemic heart disease, chronic renal disease), and the reader might find that the published data are insufficient to be conclusive of WKS only.
Our study shows the diagnostic complexity of WKS and illustrates that it is imperative to be aware of diagnostic and treatment approaches. The deficit in this syndrome’s recognition (particularly when several medical comorbidities are present or in nonalcoholic WKS) and the unfamiliarity with thiamine’s therapeutic dosage identified in this study reinforce the importance of being acquainted with this medical entity, paving the way for an early diagnosis, a suitable treatment, and a better prognosis.
Submitted: September 2, 2019; accepted December 9, 2019.
Published online: May 7, 2020.
Potential conflicts of interest: None.
Funding/support: None.
Additional information: The ethical committee of Prof. Dr. Fernando da Fonseca Hospital approved a waiver of consent to conduct this study. All information has been de-identified to protect anonymity.
REFERENCES
1. Scalzo SJ, Bowden SC, Ambrose ML, et al. Wernicke-Korsakoff syndrome not related to alcohol use: a systematic review. J Neurol Neurosurg Psychiatry. 2015;86(12):1362-1368. PubMed
2. Sharp CS, Wilson MP, Nordstrom K. Psychiatric emergencies for clinicians: emergency department management of Wernicke-Korsakoff syndrome. J Emerg Med. 2016;51(4):401-404. PubMed CrossRef
3. Arts NJ, Walvoort SJ, Kessels RP. Korsakoff’s syndrome: a critical review. Neuropsychiatr Dis Treat. 2017;13:2875-2890. PubMed CrossRef
4. Isenberg-Grzeda E, Kutner HE, Nicolson SE. Wernicke-Korsakoff-syndrome: under-recognized and under-treated. Psychosomatics. 2012;53(6):507-516. PubMed CrossRef
5. McCormick LM, Buchanan JR, Onwuameze OE, et al. Beyond alcoholism: Wernicke-Korsakoff syndrome in patients with psychiatric disorders. Cogn Behav Neurol. 2011;24(4):209-216. PubMed CrossRef
6. Kopelman MD, Thomson AD, Guerrini I, et al. The Korsakoff syndrome: clinical aspects, psychology and treatment. Alcohol Alcohol. 2009;44(2):148-154. PubMed CrossRef
7. Latt N, Dore G. Thiamine in the treatment of Wernicke encephalopathy in patients with alcohol use disorders. Intern Med J. 2014;44(9):911-915. PubMed CrossRef
8. Nikolakaros G, Ilonen T, Kurki T, et al. Non-alcoholic Korsakoff syndrome in psychiatric patients with a history of undiagnosed Wernicke’s encephalopathy. J Neurol Sci. 2016;370:296-302. PubMed CrossRef
9. Caine D, Halliday GM, Kril JJ, et al. Operational criteria for the classification of chronic alcoholics: identification of Wernicke’s encephalopathy. J Neurol Neurosurg Psychiatry. 1997;62(1):51-60. PubMed CrossRef
10.Galvin R, Br×¥then G, Ivashynka A, et al; EFNS. EFNS guidelines for diagnosis, therapy and prevention of Wernicke encephalopathy. Eur J Neurol. 2010;17(12):1408-1418. PubMed CrossRef
11.Day E, Bentham PW, Callaghan R, et al. Thiamine for prevention and treatment of Wernicke-Korsakoff syndrome in people who abuse alcohol. Cochrane Database Syst Rev. 2013;(7):CD004033. PubMed
12.Infante MT, Fancellu R, Murialdo A, et al. Challenges in diagnosis and treatment of Wernicke encephalopathy: report of 2 cases. Nutr Clin Pract. 2016;31(2):186-190. PubMed CrossRef
13.Thomson AD, Cook CC, Touquet R, et al; Royal College of Physicians, London. The Royal College of Physicians report on alcohol: guidelines for managing Wernicke’s encephalopathy in the accident and Emergency Department. Alcohol Alcohol. 2002;37(6):513-521. PubMed CrossRef
Enjoy this premium PDF as part of your membership benefits!