ABSTRACT
Objective: There is growing recognition of the importance of comorbid eating disorders (ED) among individuals with bipolar disorder (BD). However, most studies on this topic have focused on adult samples, and little is known regarding comorbid ED among youth with BD.
Methods: The sample included 197 youth with DSM-IV BD (BD-I, BD-II, or BD-NOS [not otherwise specified]), aged 13–20 years and recruited from a subspecialized clinic within a tertiary academic health sciences center from 2009 to 2017. Univariate analyses examined demographic and clinical variables among participants with versus without lifetime DSM-IV ED. Variables significant at P < .10 were entered into a backward stepwise regression.
Results: Fifty-six participants (28.4%) had lifetime DSM-IV ED (3.6% anorexia nervosa, 8.1% bulimia nervosa, 16.8% ED not otherwise specified). Significant correlates of lifetime ED were female sex (P < .001), BD-II subtype (P = .03), suicidal ideation (P = .006), suicide attempts (P = .004), non-suicidal self-injury (P < .001), sexual abuse (P = .02), cigarette smoking (P = .001), anxiety disorders (P = .004), posttraumatic stress disorder (P = .004), substance use disorders (P = .006), history of individual therapy (P = .01), and family history of anxiety (P = .01). Significant correlates of no lifetime ED were BD-I subtype (P < .001) and lifetime lithium use (P = .01). The ED group had significantly more severe lifetime depression (P < .001) and significantly more self-reported affective lability (P < .001) and borderline personality traits (P < .001). In multivariate analysis, the most robust predictors of lifetime ED were female sex (odds ratio [OR] = 4.61, P = .004), BD-I subtype (OR = 0.21, P = .03), cigarette smoking (OR = 2.78, P = .02), individual therapy (OR = 3.92, P = .03), family history of anxiety (OR = 2.86, P = .02), and borderline personality traits (OR = 1.01, P = .009).
Conclusions: ED are common among youth with BD and associated with adverse clinical characteristics, many of which converge with prior adult literature. Future studies evaluating specific ED subtypes are warranted, as are treatment studies targeting comorbid ED in youth with BD.
J Clin Psychiatry 2022;83(4):21m14201
To cite: Khoubaeva D, Dimick MK, Roane JL, et al. Comorbid eating disorders in a sample of youth with bipolar disorder: Elevated burden of dimensional and categorical psychopathology. J Clin Psychiatry. 2022;83(4):21m14201.
To share: https://doi.org/10.4088/JCP.21r14201
© Copyright 2022 Physicians Postgraduate Press, Inc.
aCentre for Youth Bipolar Disorder, Centre for Addiction and Mental Health, Toronto, Ontario, Canada
bDepartment of Psychiatry, University of Toronto, Toronto, Ontario, Canada
cDepartment of Psychiatry, Sunnybrook Health Sciences Centre, Toronto, Ontario, Canada
dDepartment of Pharmacology, University of Toronto, Toronto, Ontario, Canada
*Corresponding author: Benjamin I. Goldstein, MD, PhD, Centre for Youth Bipolar Disorder, Centre for Addiction and Mental Health, 100 Stokes St, Toronto, ON, Canada M6J 1H4 ([email protected]).
Bipolar disorder (BD) is a serious mood disorder that carries a high burden of mood symptoms, particularly depression, and is associated with high rates of psychiatric comorbidities.1,2 Whereas comorbidities such as anxiety disorders and substance use disorders (SUD) have been more widely studied and acknowledged, there has been recent growing recognition3 of the burden of comorbid eating disorders (ED) in BD. Rates of any lifetime ED in adults with BD vary (2%–33%)4,5 and are comparatively higher than in the general population, in which rates of 1%–10% have been observed.6,7 Rates for specific ED in adults with BD range from 12.5% for binge eating disorder (BED) to 7.4% for bulimia nervosa (BN) to 3.5% for anorexia nervosa (AN).8 A systematic review reported that rates of any ED comorbidity are similar across BD subtypes,4 while a recent meta-analysis found a negative association between any ED and the BD-I subtype.8 Specifically, BED and AN may be associated with BD-II, and BN with BD-I.8
In addition to increased prevalence of ED, lifetime ED in adults with BD have been associated with several adverse clinical characteristics, such as earlier age at onset of BD,9–14 more severe depressive episodes,13,15 greater number of and more time spent recovering from depressive episodes,9,12–14 greater mood lability and variability,9,10,13 anxiety disorders,9,11,13,16 alcohol use disorders (AUD) and SUD,4,9,11,13,16,17 and suicidality and non-suicidal self-injury (NSSI).9,12,16–18 Additionally, comorbid ED appear more commonly among females with BD,10–12,14,19 similar to non-BD general populations.7 Further, ED in BD have been associated with higher rates of family histories of depression, BD, and alcohol and substance abuse.12 Overall, lifetime ED appear to negatively impact the course of BD through increased burden of several adverse clinical characteristics.
Despite the growth in literature on ED in adults with BD and the peak age at onset of ED being in adolescence,20 this comorbidity remains understudied8 in youth. One study21 of a community youth sample found 8%–9% of youth with BD spectrum disorders reported lifetime ED, though subtypes of BD and ED were not specified in that study. While one report from the Course and Outcome of Bipolar Youth (COBY) study22 found only 4 of 348 youth with BD had a diagnosis of AN or BN, another nationally representative survey23 found 12% of 295 youth with BD reported lifetime binge eating and/or BN. Using a smaller version of the current sample,24 we previously found that 12% of 82 youth with BD had a lifetime diagnosis of BN, and binge eating and emotional eating behaviors were significantly more common among youth with BD compared to psychiatrically healthy controls. Despite the small number of studies, rates of ED among youth with BD are elevated compared to the rates previously reported in a general adolescent sample.25
Whether because studies have not evaluated for ED, or because small samples sizes preclude examination of this topic, there remains a dearth of studies regarding ED comorbidity in youth with BD. As such, we set out to examine the prevalence and correlates of DSM-IV ED in a relatively large clinical sample of Canadian youth with BD.
METHODS
Sample
The sample consisted of 197 youth, aged 13–20 years, with BD-I, BD-II, or BD not otherwise specified (BD-NOS). As BD-NOS was not operationalized in DSM-IV, BD-NOS was determined per the operationalized criteria used in the COBY study26: at least 4 lifetime days with at least 4 hours of either (i) elevated mood with 2 associated manic symptoms or (ii) irritable mood with 3 associated manic symptoms, which were associated with a clear change in functioning, but did not meet full criteria for a manic or hypomanic episode. This operationalized definition is akin to the Diagnostic and Statistical Manual of Mental Disorders, Fifth Edition (DSM-5) criteria for other specified bipolar and related disorder, ie, symptoms characteristic of BD (BD-I or BD-II) but that do not meet full criteria due to symptom count or duration. Participants were recruited from a subspecialty clinic in a tertiary academic health sciences center between 2009 and 2017. Consent was obtained from all participants and their parent/guardian(s) prior to participating. Ethical approval was granted by Sunnybrook Research Institute Research Ethics Board (REB #2295) and Centre for Addiction and Mental Health (CAMH) Research Ethics Board (REB 148/2020) after all data were transferred with the Centre for Youth Bipolar Disorder’s relocation to CAMH.
Procedure
Assessment. All measures were administered by interviewers with a bachelor’s or master’s degree in a health sciences field and training under guidance of the senior author (B.I.G). Study data were collected and managed using REDCap (Research Electronic Data Capture)27,28 tools hosted at Sunnybrook Research Institute and CAMH. BD diagnoses were determined via the Kiddie Schedule for Affective Disorders and Schizophrenia for School Age Children, Present and Lifetime version (K-SADS-PL),29 which uses information from both the participant and their parent/guardian(s) along with available medical records. While DSM-5 was published in 2013, the DSM-5 version of K-SADS-PL became available only in 2016; as such, diagnoses in the current sample are based on DSM-IV. The extended K-SADS Depression Rating Scale (DRS)30 and K-SADS Mania Rating Scale (MRS)31 were used in place of the K-SADS-PL mood sections. The DRS and MRS were used to assess mood symptom severity during the participant’s lifetime most severe episode and current episode; for this study, only the lifetime most severe episode scores were analyzed. The age at onset of BD was defined as the age at which the participant first experienced an episode of mania or hypomania or met criteria for BD-NOS. Diagnoses were confirmed by a consensus meeting with a licensed child-adolescent psychiatrist (B.I.G. or R.H.B.M.) after completion of the interview.
The ED diagnoses included current and lifetime diagnosis of AN, BN, and eating disorder not otherwise specified (ED-NOS). Age at onset of ED was defined as the age at which participant first met criteria for a diagnosis of ED. Participants received an ED-NOS diagnosis if they had threshold ED symptoms associated with clinically significant impairment or distress, but which did not meet full DSM-IV criteria for AN or BN, such as lack of emaciation or amenorrhea; below frequency of binge eating and/or compensatory methods, or consistency of lack of control; and binge-eating disorder. In addition, to meet criteria for ED-NOS, related symptoms had to be beyond what is explained by depression-related changes in appetite, eating, weight, and/or body image.
Comorbid psychiatric diagnoses and other clinical characteristics (eg, psychosis, medication history, psychosocial treatment history [individual, family, and/or group therapy]) were obtained from the K-SADS-PL. The variable “Any anxiety disorder” included generalized anxiety disorder, separation anxiety disorder, agoraphobia, panic disorder, and anxiety disorder not otherwise specified; posttraumatic stress disorder (PTSD) and obsessive-compulsive disorder were analyzed separately. The variable “Any substance use disorders” included alcohol, recreational drugs, and/or prescription medications. The variable “Cigarette smoking” was ascertained from the K-SADS-PL and included any lifetime history of cigarette smoking (computed as “yes” or “no”). A Safety Assessment Form was used to systematically record information, obtained by interview, about physical and sexual abuse, as well as lifetime suicide attempt (SA), suicidal ideation (SI), and NSSI outside of depressive episodes covered in the DRS. The Family History Screen32 interview was used to obtain information on psychiatric history of first- and second-degree relatives from both participant and parent(s). Socioeconomic status (SES) was determined via the 4-factor Hollingshead Scale.33 The Children’s Global Assessment Scale (CGAS)34 was used to rate the most severe past episode, current episode, and past-year highest level episodes of the participant’s global functioning; only most severe past episode and past-year highest level of functioning were included in analyses.
Self-report measures. The Life Problems Inventory (LPI)35 adolescent self-report was used to identify dimensional borderline personality traits using 4 subscales of impulsivity, emotion dysregulation, identity confusion, and interpersonal problems. The Children’s Affective Lability Scale (CALS)36 assesses affect regulation, and data from it are collected using separate adolescent self-report and parent/guardian report.
Anthropometric measures. Body mass index was calculated by dividing weight in kilograms by the square of height in meters. Weight was measured on a Tanita digital scale, and height was measured using a wall-mounted stadiometer. Height and weight measurements were taken twice and averaged for analysis, using recommended approaches.37 Weight measurements were adjusted for clothing as follows: −1.3 kg for long pants and long-sleeved shirt; −1.1 kg for short pants or short sleeves; and −0.9 kg for both short pants and short sleeves.
Statistical Analysis
Descriptive statistics were used to evaluate frequencies of current and lifetime AN, BN, ED-NOS, and any ED. Binge eating was derived from K-SADS Bulimia Nervosa Screen Item 2 and counted as present if it was scored at subthreshold frequency (less than once a week) or threshold (at least once a week). Chronology of age at onset of ED versus BD was categorized into 3 groups: ED preceded BD by ≥ 1 year, BD preceded ED by ≥ 1 year, and onset of ED and BD were within the same year. Correlates of ED were examined using independent-samples t test or Mann-Whitney U test for continuous variables and χ2 tests for categorical variables when appropriate. A false discovery rate (FDR)38 was used to adjust P values for multiple comparisons; a separate FDR adjustment was conducted for family psychiatric history. The FDR-adjusted P value for univariate results is reported in the Results section. All variables found to differ in univariate analysis at P < .1 following FDR adjustment were entered into backward stepwise logistic regression. Default values of inclusion (P < .05) and exclusion (P > .1) were used for the regression. All statistical analyses were conducted using Statistical Package for Social Sciences (SPSS) Version 25.
RESULTS
Prevalence of Eating Disorders Among Youth With BD
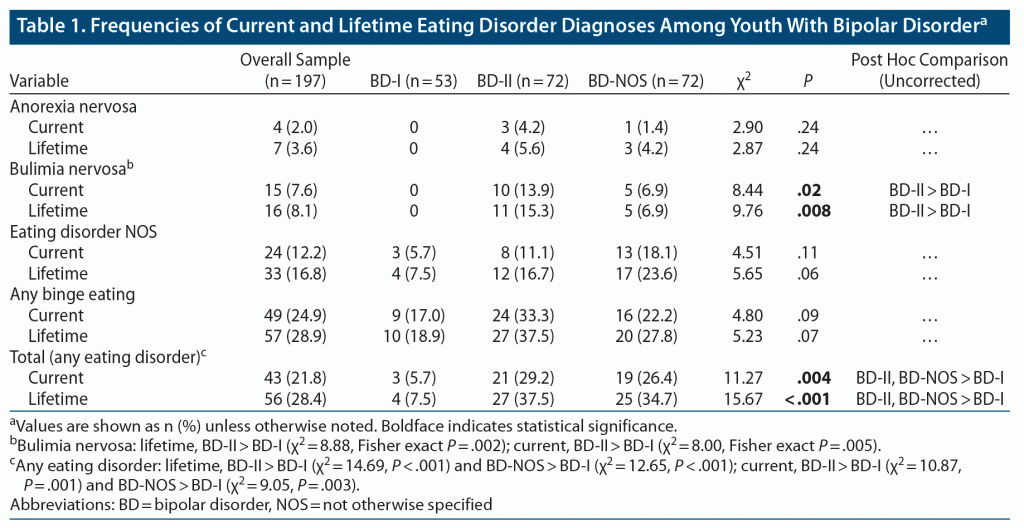
Frequencies of current and lifetime ED are reported in Table 1. Of the 197 participants, 56 (28.4%) reported a lifetime ED diagnosis; n = 7 (3.6%) for AN, n = 16 (8.1%) for BN, and n = 33 (16.8%) for ED-NOS. Additionally, 57 (28.9%) of the total sample reported a lifetime history of binge eating; of these participants, 35 (17.8% of total sample) had an ED diagnosis (n = 3 AN, n = 16 BN, and n = 16 ED-NOS), while 22 (11.2% of total sample) had lifetime binge eating and no ED diagnosis. Participants with BD-II were significantly more likely than those with BD-I to report BN for both lifetime and current periods. There were no significant differences in AN, ED-NOS, or binge eating (with or without an ED diagnosis) by BD subtype. Overall, participants with BD-II and BD-NOS were significantly more likely than those with BD-I to report a lifetime or current eating disorder. Due to sample size considerations, the 3 lifetime ED were grouped together for the purpose of analyses.
Forty-seven participants had data for mean ± SD age at onset of ED, which was 13.28 ± 2.42 years (range, 7–18 years old). Onset of ED preceded BD in 28 (59.6%) of 47 participants, BD onset preceded ED in 8 (17.0%) of 47 participants, and BD and ED onset occurred within the same year in 11 (23.4%) of 47 participants.
Demographic Characteristics
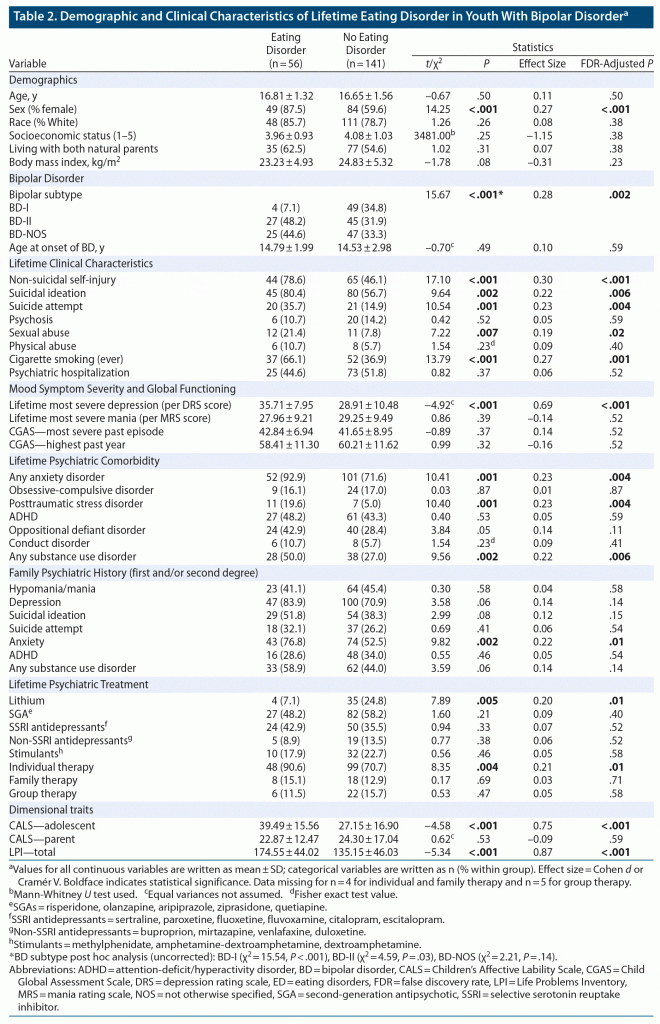
Results of univariate analyses are reported in Table 2. The overall sample had a mean ± SD age of 16.69 ± 1.50 years and were predominantly of female sex (n = 133, 67.5%). The ED group was significantly more likely to be of female sex compared to those without ED (χ2 = 14.3, P < .001); this was the only statistically significant demographic variable.
Clinical Characteristics
There were significant between-group differences in BD subtype (χ2 = 15.7, P = .002), whereby the ED group had significantly fewer participants with BD-I (χ2 = 15.5, uncorrected P < .001) but significantly more participants with BD-II (χ2 = 4.6, uncorrected P = .03). The ED group had significantly higher lifetime most severe depression scores (t = –4.9, P < .001) and were significantly more likely to report lifetime history of NSSI (χ2 = 17.1, P < .001), SI (χ2 = 9.6, P = .006), and SA (χ2 = 10.5, P = .004). The ED group was also significantly more likely to report a history of sexual abuse (χ2 = 7.2, P = .02) and ever smoking cigarettes (χ2 = 13.8, P = .001).
With regard to psychiatric comorbidity, the ED group was significantly more likely to have a lifetime comorbid anxiety disorder (χ2 = 10.4, P = .004), PTSD (χ2 = 10.4, P = .004), and SUD (χ2 = 9.6, P = .006). The ED group was significantly more likely to have a family history of anxiety disorders (χ2 = 9.8, P = .01).
For treatment history, the ED group was significantly less likely to report lifetime lithium use (χ2 = 7.9, P = .01) but significantly more likely to have received individual therapy (χ2 = 8.4, P = .01). Of note, within the ED group, 4 participants had attended an eating disorder clinic and 1 participant received individual therapy specifically to address purging. However, early in the course of this study, specific reasons for attending therapy were not systematically queried.
Lastly, for dimensional traits, the ED group had significantly higher scores on both the adolescent-reported CALS (t = –4.6, P < .001) and LPI self-reports (t = –5.3, P < .001); there were no significant between-group differences in the CALS parent report scores. In a further analysis of the LPI, the ED group had significantly higher scores on all subscales: impulsivity (t = –5.5, uncorrected P < .001), emotional dysregulation (t = –3.3, uncorrected P = .001), identity confusion (t = –3.0, uncorrected P = .003), and interpersonal problems (t = –3.3, uncorrected P = .001).
Multivariate Analysis
The backward stepwise regression controlled for sex, and due to missing data, the regression sample size was n = 170 (n = 50 with ED). Variables included were BD-I subtype, BD-II subtype, lifetime most severe depression scores, NSSI, SI, SA, sexual abuse, cigarette smoking, anxiety disorders, PTSD, SUD, lifetime lithium use, lifetime individual therapy, family history of anxiety, and CALS adolescent and LPI total self-report scores.
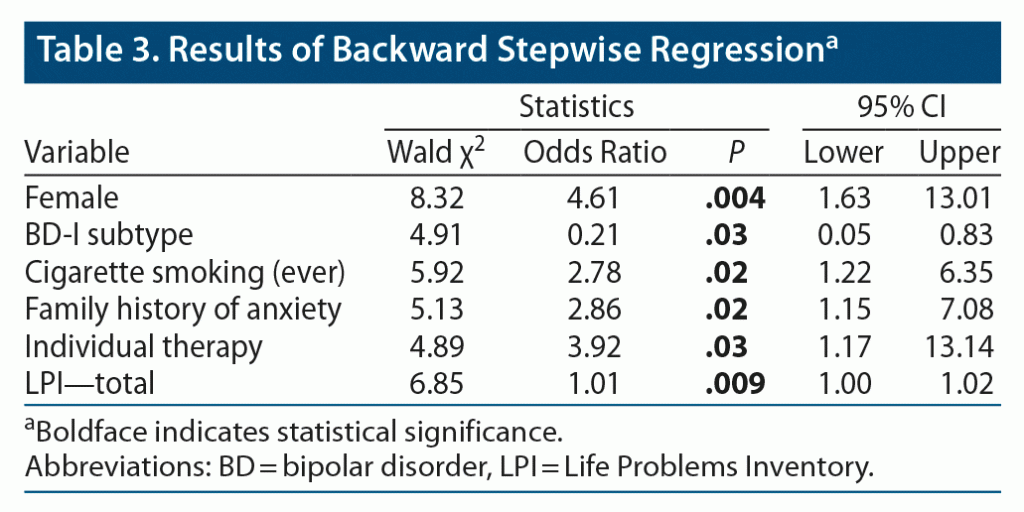
Results of the multivariate analysis can be found in Table 3. The model accounted for 41.4% of the variance (Nagelkerke r2) in lifetime ED. Lifetime ED were significantly positively associated with female sex (odds ratio [OR] = 4.61; 95% CI, 1.63–13.01; P = .004), history of cigarette smoking (OR = 2.78; 95% CI, 1.22–6.35; P = .02), history of individual therapy (OR = 3.92; 95% CI, 1.17–13.14; P = .03), family history of anxiety (OR = 2.86; 95% CI, 1.15–7.08; P = .02), and LPI total score (OR = 1.01; 95% CI, 1.00–1.02 P = .009). Lifetime ED was also significantly negatively associated with BD-I subtype (OR = 0.21; 95% CI: 0.05–0.83; P = .03). All other variables did not remain in the final model.
DISCUSSION
In the present study, nearly one-third of youth with BD had a history of ED, with the most common subtype of ED being ED-NOS. In univariate analyses, lifetime ED were associated with female sex and BD-II subtype as well as with several indicators of psychiatric burden. In multivariate analyses, the variables most robustly positively associated with ED were female sex, borderline personality traits, history of cigarette smoking, history of individual therapy, and family history of anxiety, while BD-I subtype was negatively associated with ED.
We observed a higher rate of any lifetime ED compared to the rates of 8%–9% reported in youth with BD spectrum disorders in the general population,21 though subtypes of ED were not specified in that study. The current study’s lifetime rates of BN and AN are within the range previously reported8 in clinical samples of adults with BD, lower than previously reported23 for BN in adolescents with BD in a general sample, and higher compared to population-based studies25,39 of adolescents. Due to the version of K-SADS-PL used in this study, we were unable to assess for BED, which we address as a limitation. However, the lifetime rate of binge eating is similar to those previously reported in a sample of adults with BD40 for both those with and those without an ED diagnosis (27% and 10%, respectively). Other studies41–43 have found comparable rates of binge eating behavior ranging 16%–45%, though those studies did not specify how many such behaviors occurred within or outside an ED diagnosis. Furthermore, onset of ED preceded onset of BD in the majority of participants with data for age at onset. A prior study19 of adults with BD found that ED typically preceded BD, particularly in females, whereas other studies11,44 reported the reverse order of onset. Overall, the univariate and multivariate results align with those previously reported in adults with BD, in which lifetime ED have been associated with female sex,10–12,14,19 more severe depression,13,15 elevated rates of suicidality and self-injury,9,12,16–18 greater prevalence of comorbid anxiety disorders,9,11,13 SUD,9,14,16 and greater affective lability.9,10
With regard to BD subtype, the ED group was more likely to have BD-II and less likely to have BD-I, and BD-I remained negatively associated with ED. These subtype differences may relate in part to other variables that are differentially associated across BD subtypes, including psychiatric comorbidity, depression severity, and borderline personality traits.45–48 While the findings in adults4 are mixed, a recent meta-analysis8 found that prevalence of AN may be positively associated with BD-II and negatively associated with BD-I, while prevalence of BN may be positively associated with BD-I.
The ED group also demonstrated elevated rates of sexual abuse and PTSD. Little is known regarding the association of ED with sexual abuse or PTSD in BD. One study13 of adults with BD found ED were associated with more childhood trauma, though types of trauma were not specified, and another study16 found that PTSD was a significant correlate of BED in adult patients with BD. Childhood sexual abuse is regarded49,50 as a nonspecific risk factor for ED; this association may be most robust for BN and BED.51
Another notable finding was the positive association between ED and cigarette smoking. The relationship between cigarette smoking and comorbid ED-BD is understudied; one study16 found no differences in nicotine dependence between adult BD patients with versus without BED. The occurrence of cigarette smoking in ED has been well studied outside of BD with evidence for high prevalence of smoking in individuals with BN and BED.52 Previous studies53–55 found that cigarette smoking is common among youth with BD and associated with suicide attempts, SUD, and deficits in emotional regulation,53,54 characteristics that were also observed in the ED group. Perceived weight status and wanting to lose weight have previously been identified56 as significant predictors of ever smoking cigarettes in adolescents, particularly females.
Family history of anxiety was the only familial psychopathology that was significantly elevated in the ED group and remained a positive predictor of ED. This finding aligns with a longitudinal study57 in the general population which found that parental anxiety/depression was associated with increased risk for developing ED in offspring. This is in contrast to a prior study12 that found higher rates of first-degree family history of depression, BD, and alcohol and substance abuse in adults with BD and ED. It warrants noting that all familial psychiatric diagnoses, save for BD and ADHD, were numerically higher in the ED group, with depression, suicidal ideation, and alcohol/substance use disorders approaching significance.
The pattern of findings in the current study aligns with conceptualizations from adult literature4,58 that ED and BD may share underlying vulnerabilities to depression, eating and appetite disturbances, and emotional dysregulation. The overall clinical profile of the ED group, with more severe depression, borderline personality traits and affective lability, and elevated rates of psychiatric comorbidities may explain the association between individual therapy utilization and ED. However, since we did not systematically collect reasons for attending individual therapy (eg, depression, emotional dysregulation, substance use), we cannot ascertain exact reasons for this association. To our knowledge, no studies have evaluated the rates of any psychosocial treatment among youth or adults with comorbid BD and ED. A nationally representative study25 of US adolescents found that youth with AN or BN were significantly more likely to have received treatment from human services (ie, services with a counselor, social worker, religious/spiritual advisor, or mental health crisis hotline) than those without ED.
Strengths and Limitations
The strengths of the current study are that it is based on a relatively large sample, is the first to examine both the prevalence and correlates of lifetime ED in youth with a primary diagnosis of BD, and includes the full DSM-IV spectrum of ED. As such, this study identifies directions for future exploration of this comorbidity in other youth BD samples.
There are also several limitations to consider. First, this study used a retrospective and cross-sectional design, which prevents inference on directionality of the observed findings. Given the young age of the sample, incident new-onset ED are also expected to accumulate with time. Second, ED diagnoses were obtained using DSM-IV criteria and therefore BED was subsumed within ED-NOS. There is evidence that BED may be a particularly overrepresented ED in BD8 and thus warrants further, detailed exploration in youth BD samples. Additionally, DSM-5–defined criteria for ED diagnosis are more permissive than those in DSM-IV,59 meaning that in contemporary clinical samples, rates of ED defined by DSM-5 may be inflated than were found in the present study (see McElroy et al11). Third, the findings are based on a clinical sample of youth with BD in a tertiary outpatient setting and may not be generalizable to community samples. Fourth, despite the large sample, this study was not adequately powered to evaluate ED subtypes separately.
Conclusion and Future Directions
Overall, these findings suggest that youth with BD, particularly females, commonly experience ED and most often before the onset of BD. The associations between ED and a variety of adverse clinical characteristics present several considerations and implications for treatment and future research. For instance, the elevated rates of PTSD and sexual abuse give impetus for assessing trauma history and delivering trauma-informed care in youth presenting with comorbid BD and ED particularly due to the apparent elevated use of individual therapy services. The rates of SA, SI, and NSSI were all significantly higher among those with ED; therefore, assessing for and concurrently treating ED symptoms in youth with BD may also assist in mitigating risk of suicidal and/or self-injurious behavior. Treatment approaches that address key targets of depression, suicidality and self-injury, and borderline personality traits, such as dialectical behavioral therapy,60 should be considered and prioritized in youth with comorbid BD and ED.
Submitted: August 4, 2021; accepted December 9, 2021.
Published online: May 11, 2022.
Relevant financial relationships: Dr Goldstein acknowledges research grant support from Brain Canada, Canadian Institutes of Health Research, Heart and Stroke Foundation, National Institute of Mental Health, and the Departments of Psychiatry at the University of Toronto and Sunnybrook Health Sciences Centre. Dr Goldstein also acknowledges his position as RBC Investments Chair in Children’s Mental Health and Developmental Psychopathology at the Centre for Addiction and Mental Health (CAMH), a joint Hospital-University Chair between the University of Toronto, CAMH, and the CAMH Foundation. Dr Mitchell has received salary support for research from the Departments of Psychiatry at the University of Toronto and Sunnybrook Health Sciences Centre and an honorarium for an educational video from Medscape. Ms Khoubaeva, Ms Dimick, Ms Roane, and Ms Timmins have no real or potential conflicts of interest to disclose.
Funding/support: No direct funding was received for this study. This study was supported by philanthropic donations to the Centre for Youth Bipolar Disorder and by the CAMH Discovery Fund.
Role of the sponsor: The CAMH Discovery Fund had no role in the conduct or publication of the study.
Previous presentation: Presented at the Department of Psychiatry Research Day at the University of Toronto, Ontario, Canada; June 17, 2021 • American Academy of Child and Adolescent Psychiatry 68th Annual Meeting Virtual Conference; October 18–30, 2021.
Acknowledgements: We would like to thank all study participants and families for their time and contributions to this study.
Clinical Points
- Lifetime eating disorders were common among youth with bipolar disorder and most commonly preceded onset of bipolar disorder.
- Among youth with bipolar disorder, lifetime eating disorders were significantly associated with multiple indicators of psychiatric burden. In multivariable analyses, eating disorders were positively associated with female sex, history of cigarette smoking, history of individual therapy, family history of anxiety disorders, and more severe borderline personality traits and were negatively associated with the bipolar I subtype. Overall, correlates aligned with those observed in prior studies of adults with bipolar disorder and comorbid eating disorders.
- Current findings suggest the potential value of incorporating trauma-focused perspectives and targeting emotional dysregulation and borderline personality traits when developing treatment approaches for youth with comorbid bipolar disorder and eating disorders.
References (60)

- Frías Á, Palma C, Farriols N. Comorbidity in pediatric bipolar disorder: prevalence, clinical impact, etiology and treatment. J Affect Disord. 2015;174:378–389. PubMed CrossRef
- McIntyre RS, Calabrese JR. Bipolar depression: the clinical characteristics and unmet needs of a complex disorder. Curr Med Res Opin. 2019;35(11):1993–2005. PubMed CrossRef
- Álvarez Ruiz EM, Gutiérrez-Rojas L. Comorbidity of bipolar disorder and eating disorders. Rev Psiquiatr Salud Ment. 2015;8(4):232–241. PubMed CrossRef
- McDonald CE, Rossell SL, Phillipou A. The comorbidity of eating disorders in bipolar disorder and associated clinical correlates characterised by emotion dysregulation and impulsivity: a systematic review. J Affect Disord. 2019;259:228–243. PubMed CrossRef
- Thiebaut S, Godart N, Radon L, et al. Crossed prevalence results between subtypes of eating disorder and bipolar disorder: a systematic review of the literature. Encephale. 2019;45(1):60–73. PubMed CrossRef
- Duncan AE, Ziobrowski HN, Nicol G. The prevalence of past 12-month and lifetime DSM-IV eating disorders by BMI category in US men and women. Eur Eat Disord Rev. 2017;25(3):165–171. PubMed CrossRef
- Galmiche M, Déchelotte P, Lambert G, et al. Prevalence of eating disorders over the 2000–2018 period: a systematic literature review. Am J Clin Nutr. 2019;109(5):1402–1413. PubMed CrossRef
- Fornaro M, Daray FM, Hunter F, et al. The prevalence, odds and predictors of lifespan comorbid eating disorder among people with a primary diagnosis of bipolar disorders, and vice-versa: systematic review and meta-analysis. J Affect Disord. 2021;280(Pt A):409–431. PubMed CrossRef
- Brietzke E, Moreira CL, Toniolo RA, et al. Clinical correlates of eating disorder comorbidity in women with bipolar disorder type I. J Affect Disord. 2011;130(1–2):162–165. PubMed CrossRef
- Liu X, Kelsoe JR, Greenwood TA; Bipolar Genome Study (BiGS). A genome-wide association study of bipolar disorder with comorbid eating disorder replicates the SOX2-OT region. J Affect Disord. 2016;189:141–149. PubMed CrossRef
- McElroy SL, Crow S, Blom TJ, et al. Prevalence and correlates of DSM-5 eating disorders in patients with bipolar disorder. J Affect Disord. 2016;191:216–221. PubMed CrossRef
- McElroy SL, Frye MA, Hellemann G, et al. Prevalence and correlates of eating disorders in 875 patients with bipolar disorder. J Affect Disord. 2011;128(3):191–198. PubMed CrossRef
- Jen A, Saunders EF, Ornstein RM, et al. Impulsivity, anxiety, and alcohol misuse in bipolar disorder comorbid with eating disorders. Int J Bipolar Disord. 2013;1(1):13. PubMed CrossRef
- Balzafiore DR, Rasgon NL, Yuen LD, et al. Lifetime eating disorder comorbidity associated with delayed depressive recovery in bipolar disorder. Int J Bipolar Disord. 2017;5(1):25. PubMed CrossRef
- Seixas C, Miranda-Scippa A, Nery-Fernandes F, et al. Prevalence and clinical impact of eating disorders in bipolar patients. Br J Psychiatry. 2012;34(1):66–70. PubMed CrossRef
- McElroy SL, Crow S, Biernacka JM, et al. Clinical phenotype of bipolar disorder with comorbid binge eating disorder. J Affect Disord. 2013;150(3):981–986. PubMed CrossRef
- Fornaro M, Perugi G, Gabrielli F, et al. Lifetime co-morbidity with different subtypes of eating disorders in 148 females with bipolar disorders. J Affect Disord. 2010;121(1–2):147–151. PubMed CrossRef
- Moor S, Crowe M, Luty S, et al. Effects of comorbidity and early age of onset in young people with Bipolar Disorder on self harming behaviour and suicide attempts. J Affect Disord. 2012;136(3):1212–1215. PubMed CrossRef
- Loftus J, Scott J, Vorspan F, et al. Psychiatric comorbidities in bipolar disorders: an examination of the prevalence and chronology of onset according to sex and bipolar subtype. J Affect Disord. 2020;267:258–263. PubMed CrossRef
- Solmi M, Radua J, Olivola M, et al. Age at onset of mental disorders worldwide: large-scale meta-analysis of 192 epidemiological studies [published online ahead of print June 2, 2021]. Mol Psychiatry. 2021. PubMed CrossRef
- Wittchen HU, Mhlig S, Pezawas L. Natural course and burden of bipolar disorders. Int J Neuropsychopharmacol. 2003;6(2):145–154. PubMed CrossRef
- Goldstein BI, Birmaher B, Axelson DA, et al. Preliminary findings regarding overweight and obesity in pediatric bipolar disorder. J Clin Psychiatry. 2008;69(12):1953–1959. PubMed CrossRef
Goldstein BI, Blanco C, He JP, et al. Correlates of overweight and obesity among adolescents with bipolar disorder in the National Comorbidity Survey-Adolescent Supplement (NCS-A). J Am Acad Child Adolesc Psychiatry. 2016;55(12):1020–1026. PubMed CrossRef
- Martin K, Woo J, Timmins V, et al. Binge eating and emotional eating behaviors among adolescents and young adults with bipolar disorder. J Affect Disord. 2016;195:88–95. PubMed CrossRef
- Swanson SA, Crow SJ, Le Grange D, et al. Prevalence and correlates of eating disorders in adolescents: results from the national comorbidity survey replication adolescent supplement. Arch Gen Psychiatry. 2011;68(7):714–723. PubMed CrossRef
- Birmaher B, Axelson D, Strober M, et al. Clinical course of children and adolescents with bipolar spectrum disorders. Arch Gen Psychiatry. 2006;63(2):175–183. PubMed CrossRef
- Harris PA, Taylor R, Minor BL, et al; REDCap Consortium. The REDCap consortium: Building an international community of software platform partners. J Biomed Inform. 2019;95:103208. PubMed CrossRef
- Harris PA, Taylor R, Thielke R, et al. Research electronic data capture (REDCap)–a metadata-driven methodology and workflow process for providing translational research informatics support. J Biomed Inform. 2009;42(2):377–381. PubMed CrossRef
- Kaufman J, Birmaher B, Brent D, et al. Schedule for affective disorders and schizophrenia for school-age children-present and lifetime version (K-SADS-PL): initial reliability and validity data. J Am Acad Child Adolesc Psychiatry. 1997;36(7):980–988. PubMed CrossRef
- Chambers WJ, Puig-Antich J, Hirsch M, et al. The assessment of affective disorders in children and adolescents by semistructured interview: test-retest reliability of the schedule for affective disorders and schizophrenia for school-age children, present episode version. Arch Gen Psychiatry. 1985;42(7):696–702. PubMed CrossRef
- Axelson D, Birmaher BJ, Brent D, et al. A preliminary study of the Kiddie Schedule for affective disorders and schizophrenia for school-age children mania rating scale for children and adolescents. J Child Adolesc Psychopharmacol. 2003;13(4):463–470. PubMed CrossRef
- Weissman MM, Wickramaratne P, Adams P, et al. Brief screening for family psychiatric history: the Family History Screen. Arch Gen Psychiatry. 2000;57(7):675–682. PubMed CrossRef
- Hollingshead AA. Four-Factor Index of Social Status. New Haven, CT: Yale University; 1975.
- Shaffer D, Gould MS, Brasic J, et al. A children’s global assessment scale (CGAS). Arch Gen Psychiatry. 1983;40(11):1228–1231. PubMed CrossRef
- Daniel Wagner JHR. Psychometric evaluation of the life problems inventory, a measure of borderline personality features in adolescents. J Psychol Psychother. 2015;05:4. CrossRef
- Gerson AC, Gerring JP, Freund L, et al. The Children’s Affective Lability Scale: a psychometric evaluation of reliability. Psychiatry Res. 1996;65(3):189–198. PubMed CrossRef
- Krebs NF, Himes JH, Jacobson D, et al. Assessment of child and adolescent overweight and obesity. Pediatrics. 2007;120(suppl 4):S193–S228. PubMed CrossRef
- Benjamini Y, Hochberg Y. Controlling the false discovery rate: a practical and powerful approach to multiple testing. J R Stat Soc B. 1995;57(1):289–300. CrossRef
- Ackard DM, Fulkerson JA, Neumark-Sztainer D. Prevalence and utility of DSM-IV eating disorder diagnostic criteria among youth. Int J Eat Disord. 2007;40(5):409–417. PubMed CrossRef
- McElroy SL, Crow S, Blom TJ, et al. Clinical features of bipolar spectrum with binge eating behaviour. J Affect Disord. 2016;201:95–98. PubMed CrossRef
- McAulay C, Mond J, Outhred T, et al. Eating disorder features in bipolar disorder: clinical implications. J Ment Health. 2021:1–11. PubMed CrossRef
- Jons WA, Colby CL, McElroy SL, et al. Statistical methods for testing X chromosome variant associations: application to sex-specific characteristics of bipolar disorder. Biol Sex Differ. 2019;10(1):57. PubMed CrossRef
- Winham SJ, Cuellar-Barboza AB, McElroy SL, et al. Bipolar disorder with comorbid binge eating history: a genome-wide association study implicates APOB. J Affect Disord. 2014;165:151–158. PubMed CrossRef
- Serra G, Koukopoulos A, De Chiara L, et al. Features preceding diagnosis of bipolar versus major depressive disorders. J Affect Disord. 2015;173:134–142. PubMed CrossRef
- Birmaher B, Axelson D, Goldstein B, et al. Four-year longitudinal course of children and adolescents with bipolar spectrum disorders: the Course and Outcome of Bipolar Youth (COBY) study. Am J Psychiatry. 2009;166(7):795–804. PubMed CrossRef
- Axelson D, Birmaher B, Strober M, et al. Phenomenology of children and adolescents with bipolar spectrum disorders. Arch Gen Psychiatry. 2006;63(10):1139–1148. PubMed CrossRef
- Carvalho AF, McIntyre RS, Dimelis D, et al. Predominant polarity as a course specifier for bipolar disorder: a systematic review. J Affect Disord. 2014;163:56–64. PubMed CrossRef
- Green E, Toma S, Collins J, et al. Similarities and differences across bipolar disorder subtypes among adolescents. J Child Adolesc Psychopharmacol. 2020;30(4):215–221. PubMed CrossRef
- Brewerton TD. Eating disorders, trauma, and comorbidity: focus on PTSD. Eat Disord. 2007;15(4):285–304. PubMed CrossRef
- Chen LP, Murad MH, Paras ML, et al. Sexual abuse and lifetime diagnosis of psychiatric disorders: systematic review and meta-analysis. Mayo Clin Proc. 2010;85(7):618–629. PubMed CrossRef
- Caslini M, Bartoli F, Crocamo C, et al. Disentangling the association between child abuse and eating disorders: a systematic review and meta-analysis. Psychosom Med. 2016;78(1):79–90. PubMed CrossRef
- Solmi M, Veronese N, Sergi G, et al. The association between smoking prevalence and eating disorders: a systematic review and meta-analysis. Addiction. 2016;111(11):1914–1922. PubMed CrossRef
- Goldstein BI, Birmaher B, Axelson DA, et al. Significance of cigarette smoking among youths with bipolar disorder. Am J Addict. 2008;17(5):364–371. PubMed CrossRef
- Wilens TE, Martelon M, Anderson JP, et al. Difficulties in emotional regulation and substance use disorders: a controlled family study of bipolar adolescents. Drug Alcohol Depend. 2013;132(1–2):114–121. PubMed CrossRef
- Wilens TE, Biederman J, Adamson JJ, et al. Further evidence of an association between adolescent bipolar disorder with smoking and substance use disorders: a controlled study. Drug Alcohol Depend. 2008;95(3):188–198. PubMed CrossRef
- Lange K, Thamotharan S, Racine M, et al. The relationship between weight and smoking in a national sample of adolescents: role of gender. J Health Psychol. 2015;20(12):1558–1567. PubMed CrossRef
- Bould H, Koupil I, Dalman C, et al. Parental mental illness and eating disorders in offspring. Int J Eat Disord. 2015;48(4):383–391. PubMed CrossRef
- McElroy SL, Kotwal R, Keck PE Jr, et al. Comorbidity of bipolar and eating disorders: distinct or related disorders with shared dysregulations? J Affect Disord. 2005;86(2–3):107–127. PubMed CrossRef
- Call C, Walsh BT, Attia E. From DSM-IV to DSM-5: changes to eating disorder diagnoses. Curr Opin Psychiatry. 2013;26(6):532–536. PubMed CrossRef
- Goldstein TR, Fersch-Podrat RK, Rivera M, et al. Dialectical behavior therapy for adolescents with bipolar disorder: results from a pilot randomized trial. J Child Adolesc Psychopharmacol. 2015;25(2):140–149. PubMed CrossRef
This PDF is free for all visitors!