Objective: Given that a cohort effect is rarely mentioned as one of the possible contributors to the increased incidence of childhood-onset bipolar disorder in the United States, we reexamined evidence for the phenomenon within our outpatient Bipolar Collaborative Network.
Methods: 968 outpatients (mean age, 41 years) with DSM bipolar disorder from 1995 to 2002 from 4 sites in the United States and 3 in the Netherlands and Germany (abbreviated as Europe) gave informed consent and provided detailed demographic, illness, and family history information on a patient questionnaire. Family history of bipolar disorder, depression, suicide attempt, alcohol abuse, substance abuse, and “other” illness was collected for each parent and the 4 grandparents. Age at onset and family history of illness burden were then assessed as a function of the age of the patient at network entry.
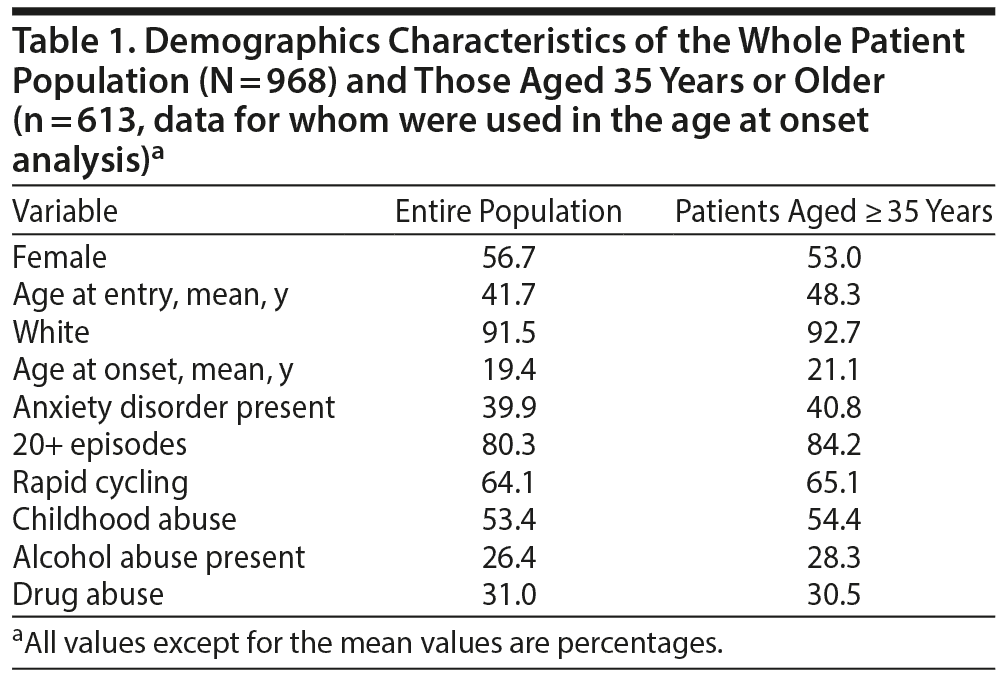
Results: Data for patients aged 35 years or older (n = 613) were included in the first analysis. Compared to older patients, those who were younger when they entered the network had an earlier age at onset of their bipolar disorder (r = 0.33, P < .001). Similarly, the youngest patients at entry (representing the most recent cohorts) had parents and grandparents with more psychiatric illness than patients born in earlier cohorts (n = 968).
Conclusions: These preliminary data, taken with the substantial literature, suggest a cohort effect for earlier age at onset of bipolar disorder and greater burden of psychiatric disorders in 2 generations of direct progenitors of our patients. The resulting likely increase in severity of bipolar illness in future generations based on this earlier age at onset and increased familial loading, particularly in the United States, deserves focused clinical and public health attention and attempts at amelioration.
This work may not be copied, distributed, displayed, published, reproduced, transmitted, modified, posted, sold, licensed, or used for commercial purposes. By downloading this file, you are agreeing to the publisher’s Terms & Conditions.
Further Evidence of a Cohort Effect in Bipolar Disorder:
More Early Onsets and Family History of Psychiatric Illness in More Recent Epochs

ABSTRACT
Objective: Given that a cohort effect is rarely mentioned as one of the possible contributors to the increased incidence of childhood-onset bipolar disorder in the United States, we reexamined evidence for the phenomenon within our outpatient Bipolar Collaborative Network.
Methods: 968 outpatients (mean age, 41 years) with DSM bipolar disorder from 1995 to 2002 from 4 sites in the United States and 3 in the Netherlands and Germany (abbreviated as Europe) gave informed consent and provided detailed demographic, illness, and family history information on a patient questionnaire. Family history of bipolar disorder, depression, suicide attempt, alcohol abuse, substance abuse, and “other” illness was collected for each parent and the 4 grandparents. Age at onset and family history of illness burden were then assessed as a function of the age of the patient at network entry.
Results: Data for patients aged 35 years or older (n = 613) were included in the first analysis. Compared to older patients, those who were younger when they entered the network had an earlier age at onset of their bipolar disorder (r = 0.33, P < .001). Similarly, the youngest patients at entry (representing the most recent cohorts) had parents and grandparents with more psychiatric illness than patients born in earlier cohorts (n = 968).
Conclusions: These preliminary data, taken with the substantial literature, suggest a cohort effect for earlier age at onset of bipolar disorder and greater burden of psychiatric disorders in 2 generations of direct progenitors of our patients. The resulting likely increase in severity of bipolar illness in future generations based on this earlier age at onset and increased familial loading, particularly in the United States, deserves focused clinical and public health attention and attempts at amelioration.
J Clin Psychiatry 2016;77(8):1043-1049
dx.doi.org/10.4088/JCP.15m10121
© Copyright 2016 Physicians Postgraduate Press, Inc.
aBipolar Collaborative Network, Bethesda, Maryland
bDepartment of Psychiatry and Behavioral Sciences, George Washington University, Washington, DC
cDepartment of Psychiatry, VU University Medical Center, Amsterdam, the Netherlands
dDepartment of Psychiatry & Behavioral Neuroscience, University of Cincinnati College of Medicine, Ohio
eLindner Center of HOPE, Mason, Ohio
fBiological Psychiatry Program, University of Cincinnati Medical College, Ohio
gDepartment of Psychiatry and Biobehavioral Sciences, David Geffen School of Medicine, University of California, Los Angeles
hDepartment of Psychiatry, VA Greater Los Angeles Healthcare System, West Los Angeles Healthcare Center, California
iDepartment of Psychiatry and Psychology, Mayo Clinic, Rochester, Minnesota
jNewcastle University, Institute of Neuroscience & Campus of Aging and Vitality, Wolfson Research Centre, Newcastle upon Tyne, United Kingdom
kDepartment of Psychiatry and Behavioral Sciences, Stanford University School of Medicine, Palo Alto, California
lVA Palo Alto Health Care System, Palo Alto, California
mUniversity of Groningen, University Medical Center Groningen, the Netherlands
‘ Dr Altshuler is deceased.
*Corresponding author: Robert M. Post, MD, 5415 W Cedar Ln, Ste 201-B, Bethesda, MD 20814 ([email protected]).
When investigators cite the many potential reasons for the apparent increase in childhood-onset bipolar disorder,1 particularly in the United States, the considerable evidence in the literature for a cohort effect is typically not referenced. Lange and McInnis2 reviewed the literature about the existence of a cohort (year of birth) and anticipation (generational) effect. They found considerable evidence to support the existence of both. In the cohort effect, each birth cohort since the early 1900s appears to have had an earlier age at onset and increased incidence of unipolar depression and bipolar disorder. In addition, many studies have documented an anticipation effect of approximately 10 years’ earlier onset of bipolar disorder in the offspring compared to the parental generation.2 While a cohort effect can sometimes contaminate an anticipation effect, Visscher et al3 found statistically significant support for both effects. More recently, Chengappa et al,4 Parker et al,5 and da Silva Magalh×£es et al6 have continued to find evidence of a cohort effect.
Kessler et al7 reported a strong cohort effect for any affective disorder in his World Health Organization survey of 85,052 individuals, with each of the 17 countries included showing a cohort effect. Similar results were seen by Viana and Andrade.8 Wittchen and Uhmann9 reported a striking cohort effect for major depression. Kessing et al10 report a doubling of the incidence of childhood bipolar disorder in Denmark from 1995-2003 to 2004-2012, but no evidence of an earlier age at onset and stated that, “child bipolar disorders are rarely diagnosed in Denmark.”
An early age at onset of both unipolar depression and bipolar disorder has been consistently associated with a more difficult and adverse course of illness into adulthood.11-18 Thus, early onset may be both a marker of a more severe illness and a portent of many other difficulties, including anxiety and substance abuse comorbidity, more affective episodes, more rapid cycling, and more treatment resistance.11,15-18
In our comparison of bipolar patients from the United States and those from the Netherlands and Germany (abbreviated here as Europe), we found that illness in US patients was more severe and more complex.18 There was a greater incidence of parental and grandparental mood disorders and other disorders in the United States19 as well as psychosocial adversity in childhood.20 The observations of more early onsets of illness in the United States than in Europe in our bipolar network have been replicated by Bellivier et al21 and Etain et al.22 Evidence from epidemiologic studies that included a diagnosis of bipolar disorder not otherwise specified (NOS) in the findings also supports a higher incidence of childhood-onset bipolar disorder in the United States than in many other countries.23 Similarly, if one examines prospective studies of children at risk for psychiatric illness because of a parent with bipolar disorder, one finds that those studies based on populations from the United States have consistently higher incidence of a childhood-onset bipolar disorder than those from Europe or Canada (as reviewed by Post et al19). For example, while Birmaher et al13 and Nurnberger et al24 found a considerable incidence of childhood-onset bipolar disorder in their US high risk studies, Duffy et al,25 for example, in a Canadian population found bipolar disorder was rare in their cohort before late teenage years or the early 20s.
In examining the burden of illness in grandparents compared to parents and siblings of our bipolar probands, we found indirect evidence for a possible cohort effect in that parents of our patients were reported to have greater amounts of overall psychiatric illness burden than the grandparents, suggesting that the more recent parental generation had a higher incidence of multiple illnesses than the prior generation. These data and the more direct evidence of a cohort effect in the literature2-6 led us to reexamine findings in our network that might provide more specific evidence of a cohort effect. To do this, we examined whether patients who were younger at age at entry to the network had an earlier age at onset compared to those who were older at entry. We also hypothesized that younger patients at entry (representing more recently born patients) would have a higher total burden of illness in their family members (parents and grandparents), that is, that these direct relatives of the most recently born patients would have more unipolar and bipolar disorder as well as multiple other illnesses compared to relatives from earlier epochs.
METHODS
The Bipolar Collaborative Network was funded by the Stanley Foundation from 1995 to 2002, and patients were recruited and studied during this period. All outpatients provided written informed consent for naturalistic follow-up. Outpatients (N = 968, mean age = 41 years) with bipolar disorder (75% bipolar I; 21% bipolar II; 2% schizoaffective, bipolar subtype; and 2% bipolar NOS) were recruited from advertisements and local clinics in 4 cities in the United States (Los Angeles, California; Dallas, Texas; Cincinnati, Ohio; and Bethesda, Maryland) (n = 676) and 3 in Europe (Utrecht, the Netherlands; and Freiburg and Munich, Germany) (n = 292) and diagnosed via Structured Clinical Interview for DSM Disorders administered by trained clinicians and research assistants. Patients completed self-rated questionnaires on their retrospective course of illness, demographics, stressors in childhood, and age at onset of bipolar disorder, described as the age at the onset of the first major depressive episode associated with dysfunction or the first manic or hypomanic episode (see Table 1).15,18,26

- 1. Given the ambiguities about the incidence of and trends for increases in childhood bipolar disorder, further assessment of the potential contribution of a year of birth (cohort) effect is timely.
- 2. Our data and those in the literature suggest that more recent birth cohorts (ie, patients younger at study entry) have a higher incidence of early-onset bipolar disorder and more positive family history of psychiatric illness, both of which are consistent with a cohort effect and the likely further increased vulnerability in future generations.
- 3. This evidence of a cohort effect suggests that efforts should be made to better identify those at highest risk and those with early prodromal syndromes so that effective early treatment interventions can be studied and utilized in an attempt to ameliorate or reverse this time trend and its associated greater illness adversity.
Each parental diagnosis was rated by the proband as definite, likely, unlikely, or not present, and a definite or likely rating was taken as a positive diagnosis for that parent.18,19 The diagnoses rated included unipolar depression, bipolar disorder, history of a suicide attempt or completed suicide, alcohol abuse, drug abuse, and “other illnesses” with the statement that they might include, for example, an anxiety disorder. The same ratings were also used for assessment of both maternal and paternal grandparents, any of the patients’ siblings, and any of the patients’ children. The specific distribution of each of these separate illnesses in the parents and grandparents is presented elsewhere.27
We examined the overall burden of all of these psychiatric difficulties in parents and grandparents together (and in the parents and grandparents separately) in relationship to age of the bipolar patient (proband) at network entry (mean age = 41 years; range, 17-81 years). When we examined age at onset of our probands as a function of their age at network entry, we arbitrarily chose to include only patients who were 35 years or older (n = 613), as patients younger than that would artificially and by necessity have an earlier age at onset of their bipolar disorder. For example if a patient was 25 years old at network entry, he or she could not have an age at onset of bipolar illness in late adulthood.
Statistics
The cohort effect was examined in 2 distinct ways. The Pearson r was used to correlate the participant’s age at entry to the network with their age at onset of their bipolar disorder and with their family history of illness. Participants were also binned by decade of birth and a 1-way between-subjects ANOVA was used to examine the relationship between decade of birth and the outcome variables.
RESULTS
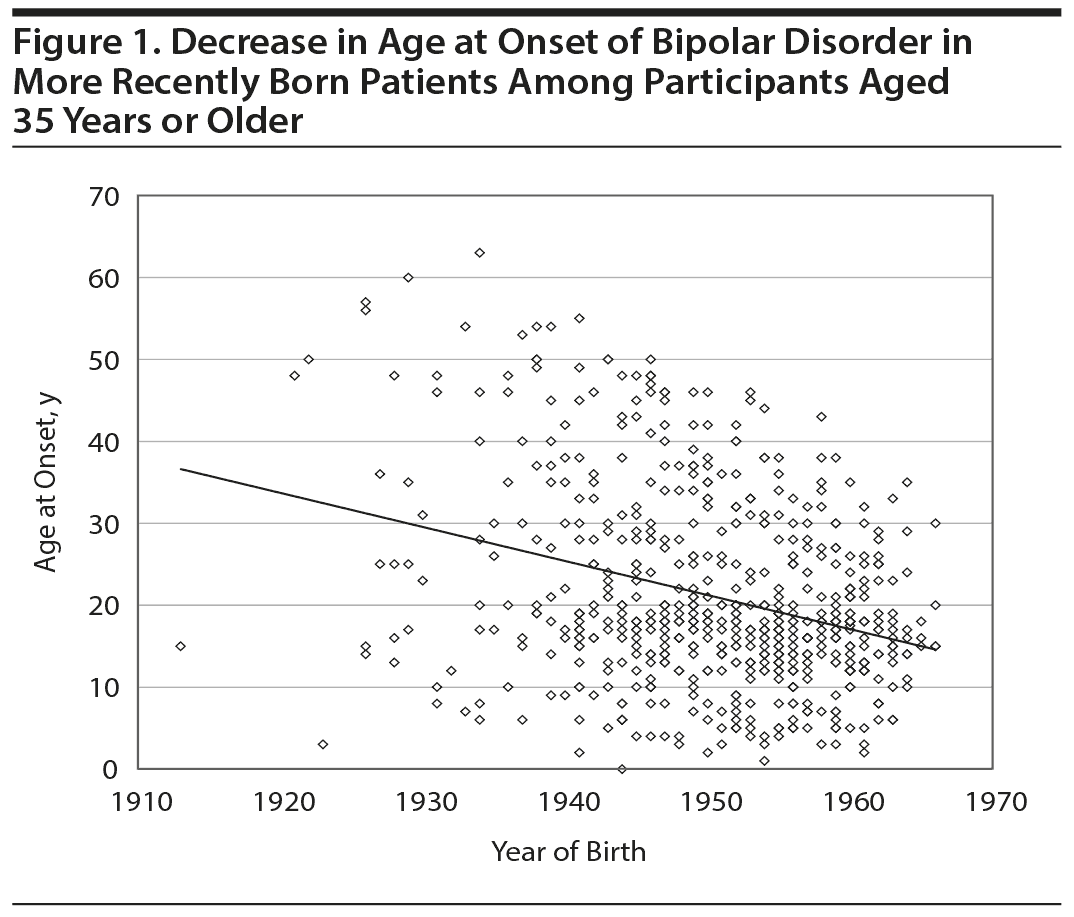
As hypothesized, those from the most recent cohorts (aged 35 to 44 years at network entry) compared to those from earlier cohorts (aged 65-74 years and 75-80 years [or older] at network entry) did had significantly earlier ages at onset of their bipolar disorder. The Pearson r correlation was significant in the overall patient population (r = 0.33, n = 613, P < .001) and, as well, separately in both the US patients (r = 0.29, n = 436, P < .001) and the European patients (r = 0.47, n = 177, P < .001). The cohort effect was also significant in both women (r = 0.37) and men (r = 0.36). We also found that the mean age at onset decreased linearly as a function of the decade of birth from 1920-1929 to 1960-1969, and the analysis of variance indicated high significance for those over 35 years of age (F4,606 = 19.27, P < .0001; Figure 1).
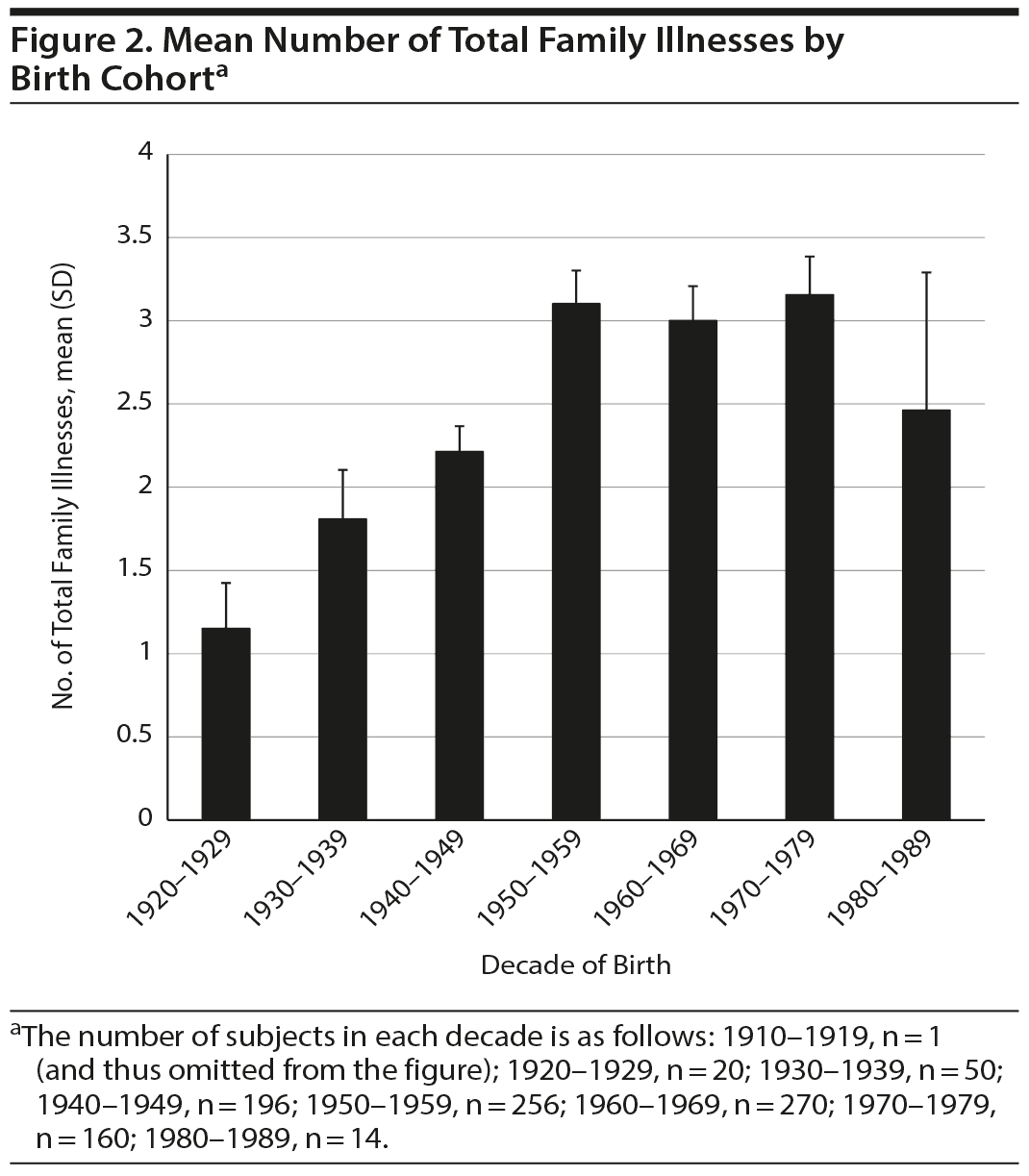
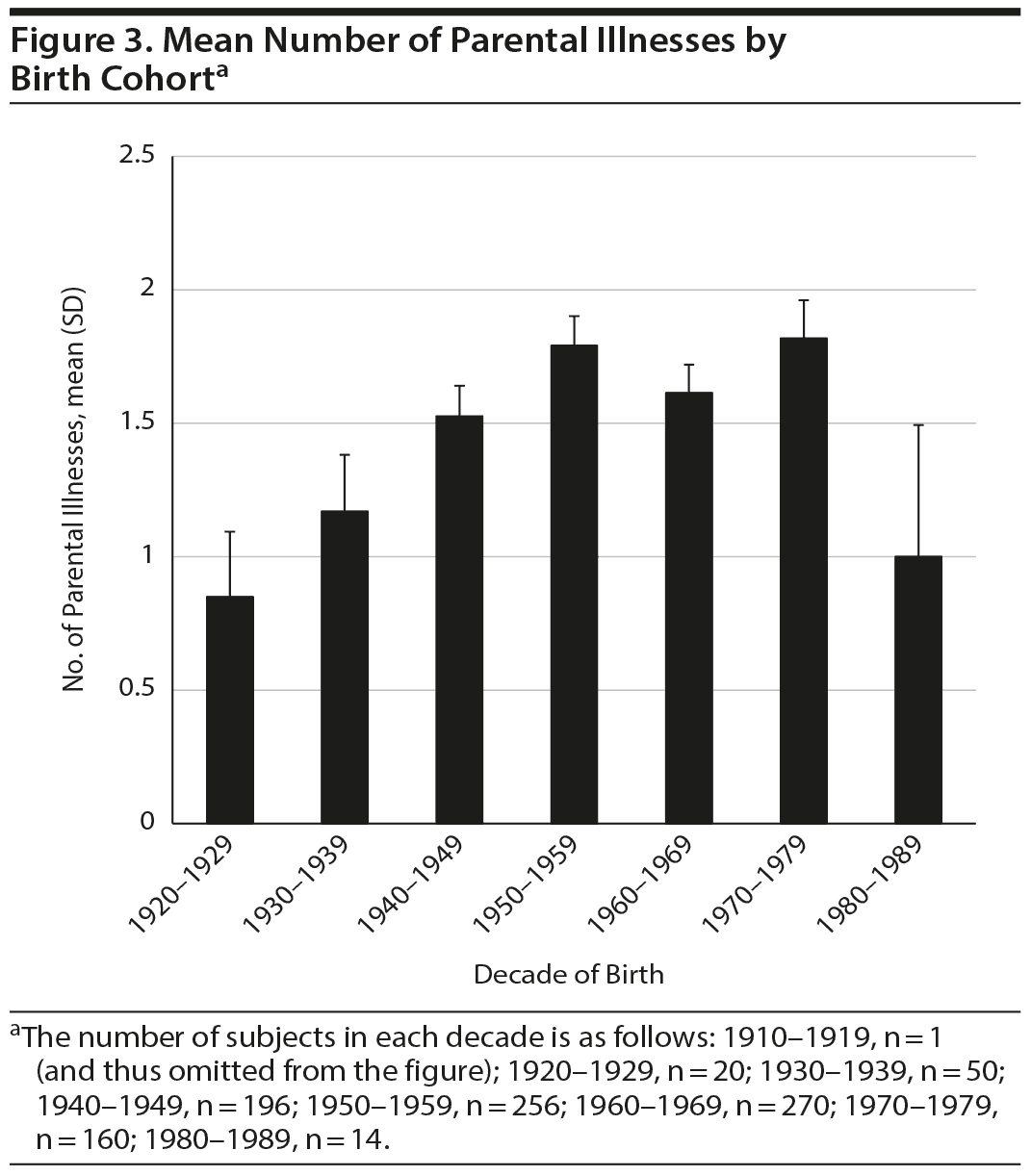
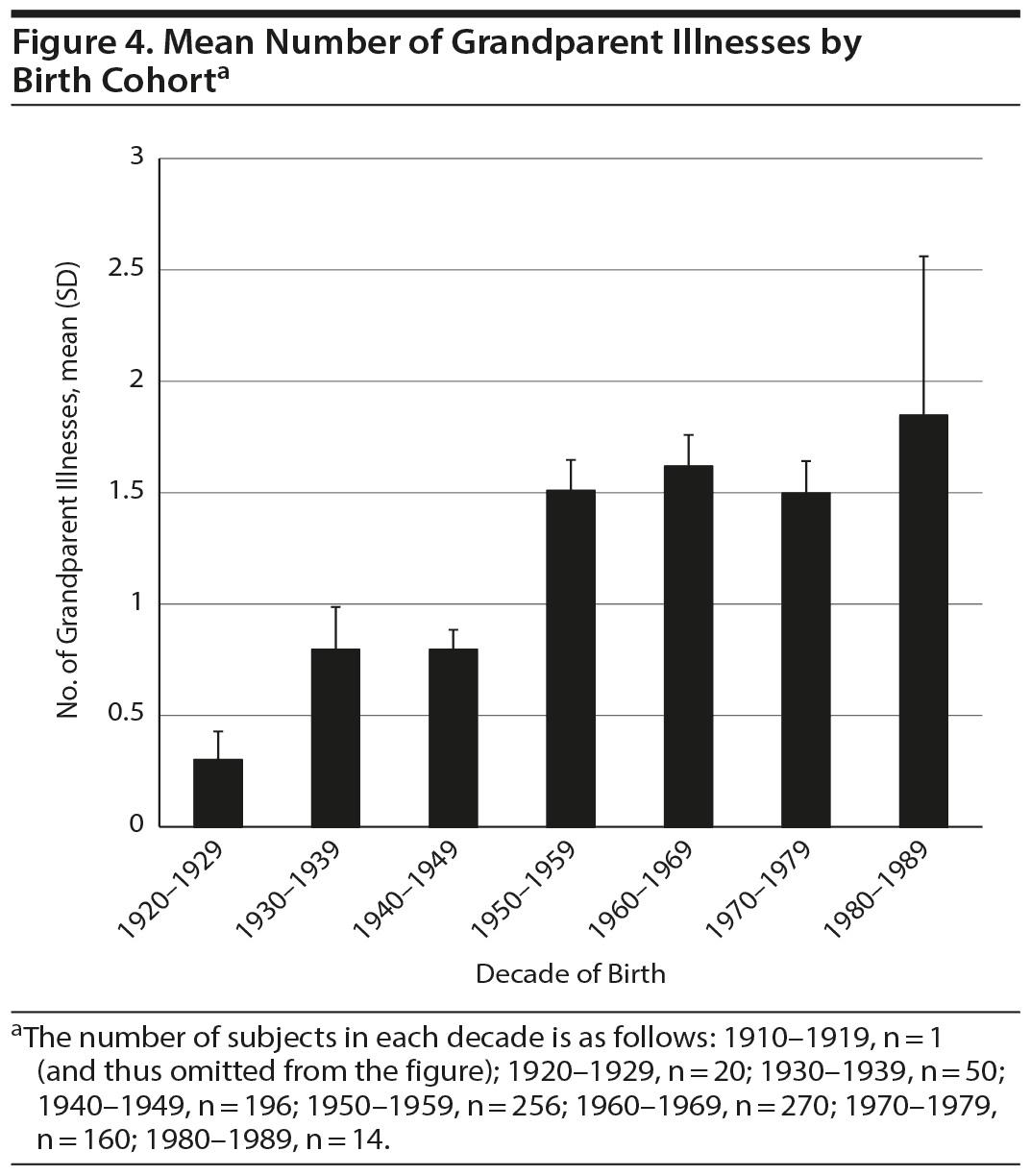
When we examined the burden of psychiatric illness in the parents and grandparents of patients from the most recent cohorts compared to those who were older at entry into the network, we found that the relatives of those who were younger at entry had a greater burden of psychiatric illness than those older at entry (r = −0.146, n = 885, P < .001). This was true both for the illness burden in the grandparents (r = −0.18, n = 885, P < .001) and the parents (r = −0.08, n = 885, P < .05) when viewed separately. When the mean age within the decade of birth was used instead of each individual’s age at entry in to the network (Figures 2, 3, and 4), the more recent increases in total family overall illness (F7,902 = 3.45, P < .005) and total grandparental illness (F7,930 = 4.79, P < .001) remained significant, while total parental illness became a trend (F7,930 = 1.96, P < .057). The reasons for this apparent falloff in total parental psychiatric illness in the most recent decade of 1980-1989 is very likely related to the small size (n = 14) and large standard error of the mean in this subgroup.
DISCUSSION
We found that patients who were younger at the time of their network entry (representing the most recent birth cohorts) did have an earlier age at onset of their bipolar illness compared to those older at entry, consistent with a cohort effect in both the United States and Europe. Those born from 1920 to 1929 had a mean age at onset of 32 years, and the age at onset decreased linearly by decade to a mean of about 17 years in those born from 1960 to 1969. Since there was a possible confound in these findings, as very young patients at entry would have to have earlier ages at onset of illness, we limited the analysis to those 35 years and older at entry.
However, no such artifact would be at play if we looked at illness in parents and grandparents as a function of any age at entry of our bipolar patients. Here again, we found that relatives from earlier cohorts (ie, relatives of patients who were older at entry) had lesser amounts of psychiatric illness than relatives of the younger patients (most recent cohorts). These data are consistent with those of Kessler et al,7 who found cohort effects for mood, substance abuse, and anxiety disorders in the general population of 17 different countries, and similar findings were reported in Brazil.8
Before we discuss these data and their implications, several limitations of this study need to be addressed. The family history data were based on answers from a questionnaire filled out by the bipolar patient and were not based on direct interviews of the family members. It is also possible that there are age-related memory biases such that younger patients are able to remember illness of their relatives better than older patients because of recency effects. However, in the study by Viana and Andrade,8 findings of cohort effects for mood, anxiety, and drug abuse disorders remained significant after controlling for time of disorder onset in the lifespan and age at interview. Another potential artifact could be that more illness in recent cohorts would be recognized since psychiatric illness was becoming less stigmatized, and this lesser stigma could generate a bias in favor reporting more illness in recent cohorts. One could also argue that in families with more illness in the relatives, one might be more cognizant of early symptoms and recognize the illness earlier.
While one could argue that early onsets of mania were poorly recognized until recently, this is less likely to be the determining factor for the cohort effect seen here since we found a similarly robust cohort effect when we examined the ages at onset only for depression (r = 0.31). Moreover, the age at onset of a first depression assessed by detailed clinician-derived life chart methodology in a different population of inpatients with affective disorders also showed a cohort effect with progressive earlier ages at onset of illness in the youngest patients.28
Mitigating these potential limitations is the fact that our findings parallel those in many other studies using different methodologies2 and that our findings were replicated in patients from both the United States and the European populations, which have very different illness characteristics,18 different health care systems, and access to health care. In addition, the incidences of various psychiatric illnesses reported in the parents of the patients from the United States were highly similar to those found by Birmaher at al,14,29,30 which were obtained with direct interviews.
Another potential limitation is the nature of the population in a tertiary care academic research setting, which could limit the generalizability to other populations of patients. Against this view are the findings of a cohort effect in both the more ill patients from the United States as well as in the less ill European patients, and that there were few exclusions for network entry beyond active substance abuse requiring treatment in another facility. Moreover, cohort effects were also seen in the large epidemiologic samples of Kessler et al7 and in other epidemiologic data of Viana and Andrade8 and Wittchen and Uhmann,9 suggesting the likely generalization to other populations ascertained in an unbiased fashion. Another potential concern could be that more ill patients were recruited to the network more recently. However, this would be an unlikely explanation as recruitment of patients spanned only a brief period of time from 1995 to 2002.
Nonetheless, given these potential limitations, the findings of this study should be considered preliminary and in need of replication with other methodologies and in other populations. Yet, our findings are consistent with a large literature (cited in the introduction) documenting the existence of cohort effects in both unipolar and bipolar disorder and anticipation effects at least in bipolar disorder. As such, discussion of the potential mechanisms involved and the clinical and theoretical implications would appear warranted.
Early- compared to late-onset bipolar illness clearly carries a more adverse prognosis for long-term outcome.11,13-16,19 The risk factors for early-onset bipolar illness have been best established for (1) genetic loading and (2) environmental factors such as psychosocial stress in childhood. Assortative mating could also play a role in increasing genetic loading, and we have seen a more than 3 times greater frequency of assortative mating (mostly those with bipolar disorder marrying a spouse with unipolar depression) in the United States than in Europe.18,19 Another psychosocial source of increasing genetic loading in more recent cohorts is a shorter duration of time between birth cohorts in those at highest risk for psychiatric illness compared to those at lowest risk.31 Genetic risk (psychiatric illness in parents and grandparents of patients with bipolar disorder) has been associated to an earlier age at onset of bipolar disorder, and early-onset illness has been suggested as a separate and more virulent form of the illness.32 Consistent with this view is the finding of Priesig et al33 that only early-onset bipolar illness conveyed increased risk of bipolar disorder to the next generation.
Finally, new data suggest that epigenetic effects can have 2 types of transgenerational influences: (1) because of exposure of the offspring to parental illness and its associated behaviors and stressors and (2) even in the absence of direct contact or interaction with the next generation (apparently mediated by epigenetic alterations that persist in sperm or oocyte germ cells).30 Thus, behaviorally based epigenetic effects related to parental illness, stressors, or substances of abuse could be supplemented by germ cell conveyance of vulnerability from the previous generation. Such a contributing germ cell epigenetic mechanism has not been previously discussed or postulated as a possible contributor to the cohort effect, but such a possibility deserves further exploration, particularly since multiple illnesses, including substance abuse, also show cohort effects6,7 and contribute to vulnerability to bipolar disorder.
Substantial data suggest that bipolar disorder is polygenetic,31,34,35 consistent with our recent findings36 that other illnesses beyond those of the affective disorders in family members of our probands very likely contribute to early onset. Antypa and Serretti37 also reported that patients with a positive family history of any mood disorder had an earlier age at onset and more severe form of bipolar disorder.
Thus, one must ask whether the incidence of these other illnesses that contribute to the risk of bipolar disorder in the offspring is also increasing in the population. The evidence is robust for increases in attention-deficit/hyperactivity disorder38 over the past century and very likely is also positive for alcoholism and drug abuse. Kessler et al7 found these time trends or year of birth effects for multiple illnesses in their large epidemiologic study. The effects were particularly large for the affective disorders and substance abuse, while they were smaller but still significant for the anxiety disorder. Similarly, Viana and Andrade8 in S×£o Paulo, Brazil, showed the biggest cohort effect for bipolar disorder (OR = 14.8) and unipolar depressive disorder (OR = 13.9), followed by drug abuse (OR = 9.5) and any anxiety disorder (OR = 2.1). da Silva Magalhaes et al6 also showed a cohort effect for alcohol and substance abuse in addition to age at onset in patients with bipolar disorder.
Lin et al32 suggested a genetic relationship between substance abuse and early-onset bipolar disorder, such that the recent increases in substance abuse could be contributing to cohort effects in bipolar disorder. Thus, since a positive family history of multiple psychiatric disorders appears to be contributing to early-onset bipolar illness and there are apparent cohort effects for many of these disorders (such as anxiety and substance abuse disorders), as well as mood disorders,7,39 the cohort effects observed here for age at onset may be in part based on coexisting cohort effects for multiple psychiatric disorders and their cumulative impact on early onset. On the basis of direct interviews of 2,289 relatives of 523 patients with affective disorder, Klerman et al39 found progressive increases in rates of depression and earlier ages at onset of depression in successive birth cohorts throughout the 20th century.
The data supporting a cohort effect and to whatever extent an anticipation effect is also in play2 have grave implications for the earlier onset, higher incidence, and more complex and treatment-refractory course of illness in our current patients and their future generations. Bipolar disorder is already one of the leading causes of disability, suicide, economic losses, and markedly truncated number of years of life expectancy (years lost primarily because of cardiovascular disorder). The incidence of bipolar disorder in the US population is already high (in the range of 3% to 5%), with some two-thirds of the patients having onset in childhood and adolescence.11,18
To the extent that there is transgenerational genetic and epigenetic transmission of the disorder exacerbated by cohort and anticipation effects, the situation is not only unlikely to improve, but on the contrary is likely to deteriorate further. As such, it appears that new approaches to clinical and public health efforts are in order and need to be mounted on multiple fronts.
One might start by screening children at highest risk and, if they are ill, treating them appropriately for their emerging symptoms.8,40 Psychotherapeutic interventions have proved effective for those at high risk with prodromal syndromes,41,42 and study of safe potentially effective early interventions such as omega-3-fatty acids and N-acetylcysteine would be particularly justified. The view of the need for long-term maintenance of pharmacoprophylaxis after a first or second episode of bipolar disorder needs wider public promulgation and psychoeducational emphasis for affected families. Compared to treatment as usual, specialty clinic treatment for only the first 2 years results in a much more benign course of illness during the next 6 years of follow-up after a first hospitalization for mania.43 The equivalent of this specialty clinic treatment (providing post-hospitalization transitional guidance, illness education and monitoring, psychotherapy, and expert pharmacotherapy) should be made available to the majority of patients in the United States rather than only to the small minority who currently receive this integrated multimodal care or the 20% of adolescents with a bipolar spectrum disorder who receive any care at all.44
Even if no cohort and anticipation effects existed, the current crisis of inadequate approaches to research on and treatment of bipolar disorder in the United States is already of staggering proportions.18,40,45-47 Given the likelihood of increasing difficulties in future generations based on a host of factors driving the likely cohort effects seen here and in the literature, the costs of early-onset bipolar disorder and its pernicious course will greatly worsen unless appropriate therapeutic interventions are generated and delivered.
Submitted: May 18, 2015; accepted April 28, 2016.
Online first: July 5, 2016.
Potential conflicts of interest: Dr Post has been on a speaker/advisory board for AstraZeneca, Sunovion, and Validus in the past 12 months and will be for Takeda and Nestle Health Science-Pamlab in the future. Dr Keck is employed by the University of Cincinnati College of Medicine and University of Cincinnati physicians; is President-CEO of the Lindner Center of HOPE; has presently been a principal investigator or co-investigator on research studies in the last 12 months sponsored by Alkermes, AstraZeneca, Cephalon, GlaxoSmithKline, Eli Lilly and Company, Marriott Foundation, National Institute of Mental Health (NIMH), Orexigen, Pfizer Inc, and Shire; has been reimbursed for consulting in the past 12 months from Shire, Supernus, Otsuka, ProPhase, and Merck; and is a co-inventor on US Patent No 6,387,956: Shapira NA, Goldsmith TD, Keck, PE Jr. (Univ. of Cincinnati) Methods of treating obsessive-compulsive spectrum disorder comprises the step of administering an effective amount of tramadol to an individual,filed March 25, 1999 and approved May 14, 2002 (he has received no financial gain from this patent). Dr McElroy has been a consultant or served on an advisory board for Bracket, F. Hoffmann-La Roche, MedAvante, Naurex, Novo Nordisk, Shire, and Sunovion within the past 12 months and has received grant support from Alkermes, Cephalon, Forest, Marriott Foundation, Naurex, Orexigen, Shire, and Takeda within the past 12 months. Dr Altshuler was on an advisory board for Takeda Pharmaceuticals North America, Inc and H. Lundbeck A/S (Health and Wellness Partners, LLC) in November 2012 and attended an editorial board meeting sponsored by Sunovion Pharmaceuticals (Health and Wellness Partners, LLC) in February 2013; received honorarium as part of the 2014 Award for Research in Mood Disorders given by the American College of Psychiatrists; performed a medical records review for the law offices of Hughes-Sokol-Piers-Resnick DYM, Ltd in January and March 2015; and, during the past 36 months, has been principal investigator and co-investigator on research studies sponsored by NIMH. Dr Frye has received grant support from Assurex, Janssen Research & Development, Mayo Foundation, Myriad, National Institute of Alcohol Abuse and Alcoholism (NIAAA), NIMH, and Pfizer; has consulted for Janssen Research & Development, LLC, Mitsubishi Tanabe Pharma Corporation, Myriad, Sunovion, Supernus Pharmaceuticals, and Teva Pharmaceuticals; and has received CME/Travel Support from the American Physician Institute and CME Outfitters. Mayo Clinic has a financial interest in Assurex and the technology referenced in this publication/presentation. Dr Nolen has received grants from the Netherlands Organisation for Health Research and Development, the European Union, Astra Zeneca, GlaxoSmithKline, and Wyeth and has received honoraria/speaker’s fees from Astra Zeneca and Lundbeck (2010-2015). Dr Suppes received sources of funding from or medications for clinical grants from the National Institute of Mental Health, Sunovion, Elan Pharma International Limited, and VA Cooperative Studies Program; has participated in consulting agreements/advisory boards/speaking engagements for A/S H. Lundbeck, AstraZeneca, and Merck; has received continuing medical education honoraria from Medscape Education and Global Medical Education; has received royalties from Jones and Bartlett and UpToDate; and has received travel reimbursement from AstraZeneca, A/S H. Lundbeck, and Merck in the past 12 months. Dr Kupka has been a speakers/advisory board for Lundbeck. Drs Grunze and Rowe and Ms Leverich have no relevant financial interest or personal affiliations during at least the past 12 months.
Funding/support: Support was provided by the Stanley Medical Research Institute from 1995-2002.
Role of the sponsor: The sponsor played no role in the analysis and interpretation of this manuscript.
REFERENCES
1. Moreno C, Laje G, Blanco C, et al. National trends in the outpatient diagnosis and treatment of bipolar disorder in youth. Arch Gen Psychiatry. 2007;64(9):1032-1039. PubMed doi:10.1001/archpsyc.64.9.1032
2. Lange KJ, McInnis MG. Studies of anticipation in bipolar affective disorder. CNS Spectr. 2002;7(3):196-202. PubMed
3. Visscher PM, Yazdi MH, Jackson AD, et al. Genetic survival analysis of age-at-onset of bipolar disorder: evidence for anticipation or cohort effect in families. Psychiatr Genet. 2001;11(3):129-137. PubMed doi:10.1097/00041444-200109000-00004
4. Chengappa KN, Kupfer DJ, Frank E, et al. Relationship of birth cohort and early age at onset of illness in a bipolar disorder case registry. Am J Psychiatry. 2003;160(9):1636-1642. PubMed doi:10.1176/appi.ajp.160.9.1636
5. Parker G, Brotchie H, Fletcher K. An increased proportional representation of bipolar disorder in younger depressed patients: analysis of two clinical databases. J Affect Disord. 2006;95(1-3):141-144. PubMed doi:10.1016/j.jad.2006.04.024
6. da Silva Magalh×£es PV, Gomes FA, Kunz M, et al. Birth-cohort and dual diagnosis effects on age-at-onset in Brazilian patients with bipolar I disorder. Acta Psychiatr Scand. 2009;120(6):492-495. PubMed doi:10.1111/j.1600-0447.2009.01426.x
7. Kessler RC, Angermeyer M, Anthony JC, et al. Lifetime prevalence and age-of-onset distributions of mental disorders in the World Health Organization’s World Mental Health Survey Initiative. World Psychiatry. 2007;6(3):168-176. PubMed
8. Viana MC, Andrade LH. Lifetime prevalence, age and gender distribution and age-of-onset of psychiatric disorders in the São Paulo Metropolitan Area, Brazil: results from the São Paulo Megacity Mental Health Survey. Rev Bras Psiquiatr. 2012;34(3):249-260. PubMed doi:10.1016/j.rbp.2012.03.001
9. Wittchen HU, Uhmann S. The timing of depression: an epidemiological perspective. Medicographia. 2010;32:115-125.
10. Kessing LV, Vradi E, Andersen PK. Are rates of pediatric bipolar disorder increasing? results from a nationwide register study. Int J Bipolar Disord. 2014;2(1):10. PubMed doi:10.1186/s40345-014-0010-0
11. Perlis RH, Miyahara S, Marangell LB, et al; STEP-BD Investigators. Long-term implications of early onset in bipolar disorder: data from the first 1,000 participants in the systematic treatment enhancement program for bipolar disorder (STEP-BD). Biol Psychiatry. 2004;55(9):875-881. PubMed doi:10.1016/j.biopsych.2004.01.022
12. Carter TD, Mundo E, Parikh SV, et al. Early age at onset as a risk factor for poor outcome of bipolar disorder. J Psychiatr Res. 2003;37(4):297-303. PubMed doi:10.1016/S0022-3956(03)00052-9
13. Birmaher B, Axelson D, Monk K, et al. Lifetime psychiatric disorders in school-aged offspring of parents with bipolar disorder: the Pittsburgh Bipolar Offspring Study. Arch Gen Psychiatry. 2009;66(3):287-296. PubMed doi:10.1001/archgenpsychiatry.2008.546
14. Birmaher B, Gill MK, Axelson DA, et al. Longitudinal trajectories and associated baseline predictors in youths with bipolar spectrum disorders. Am J Psychiatry. 2014;171(9):990-999. PubMed doi:10.1176/appi.ajp.2014.13121577
15. Post RM, Leverich GS, Kupka RW, et al. Early-onset bipolar disorder and treatment delay are risk factors for poor outcome in adulthood. J Clin Psychiatry. 2010;71(7):864-872. PubMed doi:10.4088/JCP.08m04994yel
16. Geoffroy PA, Etain B, Scott J, et al. Reconsideration of bipolar disorder as a developmental disorder: importance of the time of onset. J Physiol Paris. 2013;107(4):278-285. PubMed doi:10.1016/j.jphysparis.2013.03.006
17. Suominen K, Mantere O, Valtonen H, et al. Early age at onset of bipolar disorder is associated with more severe clinical features but delayed treatment seeking. Bipolar Disord. 2007;9(7):698-705. PubMed doi:10.1111/j.1399-5618.2007.00388.x
18. Post RM, Altshuler L, Kupka R, et al. More pernicious course of bipolar disorder in the United States than in many European countries: implications for policy and treatment. J Affect Disord. 2014;160:27-33. PubMed doi:10.1016/j.jad.2014.02.006
19. Post RM, Leverich GS, Kupka R, et al. Increased parental history of bipolar disorder in the United States: association with early age of onset. Acta Psychiatr Scand. 2014;129(5):375-382. PubMed doi:10.1111/acps.12208
20. Post RM, Altshuler L, Leverich G, et al. More stressors prior to and during the course of bipolar illness in patients from the United States compared with the Netherlands and Germany. Psychiatry Res. 2013;210(3):880-886. PubMed doi:10.1016/j.psychres.2013.08.007
21. Bellivier F, Etain B, Malafosse A, et al. Age at onset in bipolar I affective disorder in the USA and Europe. World J Biol Psychiatry. 2014;15(5):369-376. PubMed doi:10.3109/15622975.2011.639801
22. Etain B, Lajnef M, Bellivier F, et al. Clinical expression of bipolar disorder type I as a function of age and polarity at onset: convergent findings in samples from France and the United States. J Clin Psychiatry. 2012;73(4):e561-e566. PubMed doi:10.4088/JCP.10m06504
23. Van Meter AR, Moreira AL, Youngstrom EA. Meta-analysis of epidemiologic studies of pediatric bipolar disorder. J Clin Psychiatry. 2011;72(9):1250-1256. PubMed doi:10.4088/JCP.10m06290
24. Nurnberger JI Jr, McInnis M, Reich W, et al. A high-risk study of bipolar disorder: childhood clinical phenotypes as precursors of major mood disorders. Arch Gen Psychiatry. 2011;68(10):1012-1020. PubMed doi:10.1001/archgenpsychiatry.2011.126
25. Duffy A, Alda M, Crawford L, et al. The early manifestations of bipolar disorder: a longitudinal prospective study of the offspring of bipolar parents. Bipolar Disord. 2007;9(8):828-838. PubMed doi:10.1111/j.1399-5618.2007.00421.x
26. Post RM, Leverich GS, Altshuler LL, et al. Differential clinical characteristics, medication usage, and treatment response of bipolar disorder in the US versus the Netherlands and Germany. Int Clin Psychopharmacol. 2011;26(2):96-106. PubMed doi:10.1097/YIC.0b013e3283409419
27. Post RM, Leverich GS, Kupka R, et al. Increases in multiple psychiatric disorders in parents and grandparents of patients with bipolar disorder from the USA compared with the Netherlands and Germany. Psychiatr Genet. 2015;25(5):194-200. PubMed doi:10.1097/YPG.0000000000000093
28. Frye MA, Ketter TA, Leverich GS, et al. The increasing use of polypharmacotherapy for refractory mood disorders: 22 years of study. J Clin Psychiatry. 2000;61(1):9-15. PubMed doi:10.4088/JCP.v61n0104
29. Birmaher B, Axelson D, Goldstein B, et al. Psychiatric disorders in preschool offspring of parents with bipolar disorder: the Pittsburgh Bipolar Offspring Study (BIOS). Am J Psychiatry. 2010;167(3):321-330. PubMed doi:10.1176/appi.ajp.2009.09070977
30. Birmaher B, Goldstein BI, Axelson DA, et al. Mood lability among offspring of parents with bipolar disorder and community controls. Bipolar Disord. 2013;15(3):253-263. PubMed doi:10.1111/bdi.12060
31. Comings DE. The Gene Bomb: Does Higher Education and Advanced Technology Accelerate the Selection for Genes for Learning Disorders, ADHD, Addictive and Disruptive Disorders? Duarte, CA: Hope Press; 1996.
32. Lin PI, McInnis MG, Potash JB, et al. Clinical correlates and familial aggregation of age at onset in bipolar disorder. Am J Psychiatry. 2006;163(2):240-246. PubMed doi:10.1176/appi.ajp.163.2.240
33. Preisig M, Strippoli MP, Castelao E, et al. The specificity of the familial aggregation of early-onset bipolar disorder: a controlled 10-year follow-up study of offspring of parents with mood disorders. J Affect Disord. 2016;190:26-33. PubMed doi:10.1016/j.jad.2015.10.005
34. Bale TL. Lifetime stress experience: transgenerational epigenetics and germ cell programming. Dialogues Clin Neurosci. 2014;16(3):297-305. PubMed
35. Nurnberger JI Jr, Koller DL, Jung J, et al; Psychiatric Genomics Consortium Bipolar Group. Identification of pathways for bipolar disorder: a meta-analysis. JAMA Psychiatry. 2014;71(6):657-664. PubMed doi:10.1001/jamapsychiatry.2014.176
36. Post RM, Leverich GS, Kupka R, et al. Age of onset of bipolar disorder related to parental and grandparental illness burden. J Clin Psychiatry. In press.
37. Antypa N, Serretti A. Family history of a mood disorder indicates a more severe bipolar disorder. J Affect Disord. 2014;156:178-186. PubMed doi:10.1016/j.jad.2013.12.013
38. Thomas R, Sanders S, Doust J, et al. Prevalence of attention-deficit/hyperactivity disorder: a systematic review and meta-analysis. Pediatrics. 2015;135(4):e994-e1001. PubMed doi:10.1542/peds.2014-3482
39. Klerman GL, Lavori PW, Rice J, et al. Birth-cohort trends in rates of major depressive disorder among relatives of patients with affective disorder. Arch Gen Psychiatry. 1985;42(7):689-693. PubMed doi:10.1001/archpsyc.1985.01790300057007
40. Post RM, Chang K, Frye MA. Paradigm shift: preliminary clinical categorization of ultrahigh risk for childhood bipolar disorder to facilitate studies on prevention. J Clin Psychiatry. 2013;74(2):167-169. PubMed doi:10.4088/JCP.12com08136
41. Fristad MA, Verducci JS, Walters K, et al. Impact of multifamily psychoeducational psychotherapy in treating children aged 8 to 12 years with mood disorders. Arch Gen Psychiatry. 2009;66(9):1013-1021. PubMed doi:10.1001/archgenpsychiatry.2009.112
42. Miklowitz DJ, Schneck CD, Singh MK, et al. Early intervention for symptomatic youth at risk for bipolar disorder: a randomized trial of family-focused therapy. J Am Acad Child Adolesc Psychiatry. 2013;52(2):121-131. PubMed doi:10.1016/j.jaac.2012.10.007
43. Kessing LV, Hansen HV, Hvenegaard A, et al; Early Intervention Affective Disorders (EIA) Trial Group. Treatment in a specialised out-patient mood disorder clinic v. standard out-patient treatment in the early course of bipolar disorder: randomised clinical trial. Br J Psychiatry. 2013;202(3):212-219. PubMed doi:10.1192/bjp.bp.112.113548
44. Merikangas KR, He JP, Burstein M, et al. Lifetime prevalence of mental disorders in US adolescents: results from the National Comorbidity Survey Replication—Adolescent Supplement (NCS-A). J Am Acad Child Adolesc Psychiatry. 2010;49(10):980-989. PubMed doi:10.1016/j.jaac.2010.05.017
45. Post RM. The perfect storm of childhood onset bipolar disorder. Psychiatr Ann. 2009;39:879-886. doi:10.3928/00485718-20090924-06
46. Post RM. Children in the US are at high risk for psychiatric disorders: early monitoring by parents may enhance awareness and treatment. J Pediatr Neurol Med. 2016;1(3):1-4.
47. Post RM. Recognizing depression, anxiety, and externalizing behaviors in children of a parent with mood disorders: weekly symptom monitoring in the Child Network. J Depress Anxiety. 2016;S2:014. In press.
This PDF is free for all visitors!