Objective: To increase awareness of adult attention-deficit/hyperactivity disorder (ADHD) in the primary care community and to provide guidance for the management of this condition. Despite its increasing prevalence, adult ADHD largely remains underdiagnosed and inappropriately treated in the United States. The publication of the Diagnostic and Statistical Manual of Mental Disorders, Fifth Edition (DSM-5), has provided more clear diagnostic criteria for adult ADHD, but a solid framework supporting the transition of ADHD management from pediatric to adult primary care is lacking.
Data Sources: We searched PubMed and MEDLINE databases (January 1, 1984-June 1, 2016) using combinations of keywords, including ADHD, adult, diagnosis, prevalence, symptoms, treatment, comorbidity, compliance, and guidelines; international treatment guidelines; and the Diagnostic Interview for Adult ADHD websites to identify relevant clinical studies, reviews, meta-analyses, guidelines, and web-based resources describing updates to the DSM.
Study Selection/Data Extraction: In total, 143 citations were selected based on their relevance to adult ADHD diagnosis, treatment, major issues, and practice guidelines.
Results: The update on diagnostic criteria in the DSM-5 may increase the diagnosis of adult ADHD. There are critical differences between childhood and adult ADHD, and specific considerations should be taken with an adult ADHD diagnosis. Adult ADHD is primarily treated with pharmacotherapy assisted by behavior interventions. Caution should be exercised when using stimulants during pregnancy and the postpartum period. Adult ADHD patients often suffer from unemployment, financial difficulties, and an unsuccessful personal life. Adult-specific guidelines may improve adult ADHD treatment.
Conclusions: The successful diagnosis and management of adult ADHD require consideration of many facets including prior medical history and comorbid conditions and use of an individualized, evidence-based treatment approach.
Adult Attention-Deficit/Hyperactivity Disorder Diagnosis, Management, and Treatment in the DSM-5 Era
ABSTRACT
Objective: To increase awareness of adult attention-deficit/hyperactivity disorder (ADHD) in the primary care community and to provide guidance for the management of this condition. Despite its increasing prevalence, adult ADHD largely remains underdiagnosed and inappropriately treated in the United States. The publication of the Diagnostic and Statistical Manual of Mental Disorders, Fifth Edition (DSM-5), has provided more clear diagnostic criteria for adult ADHD, but a solid framework supporting the transition of ADHD management from pediatric to adult primary care is lacking.
Data Sources: We searched PubMed and MEDLINE databases (January 1, 1984–June 1, 2016) using combinations of keywords, including ADHD, adult, diagnosis, prevalence, symptoms, treatment, comorbidity, compliance, and guidelines; international treatment guidelines; and the Diagnostic Interview for Adult ADHD websites to identify relevant clinical studies, reviews, meta-analyses, guidelines, and web-based resources describing updates to the DSM.
Study Selection/Data Extraction: In total, 143 citations were selected based on their relevance to adult ADHD diagnosis, treatment, major issues, and practice guidelines.
Results: The update on diagnostic criteria in the DSM-5 may increase the diagnosis of adult ADHD. There are critical differences between childhood and adult ADHD, and specific considerations should be taken with an adult ADHD diagnosis. Adult ADHD is primarily treated with pharmacotherapy assisted by behavior interventions. Caution should be exercised when using stimulants during pregnancy and the postpartum period. Adult ADHD patients often suffer from unemployment, financial difficulties, and an unsuccessful personal life. Adult-specific guidelines may improve adult ADHD treatment.
Conclusions: The successful diagnosis and management of adult ADHD require consideration of many facets including prior medical history and comorbid conditions and use of an individualized, evidence-based treatment approach.
Prim Care Companion CNS Disord 2016;18(6):doi:10.4088/PCC.16r02000
© Copyright 2016 Physicians Postgraduate Press, Inc.
aRochester Center for Behavioral Medicine, Rochester Hills, Michigan
bJohns Hopkins University School of Medicine, Baltimore, Maryland
*Corresponding author: Joel L. Young, MD, Rochester Center for Behavioral Medicine, 441 South Livernois Rd, Ste 100, Rochester Hills, MI 48307 ([email protected]).
Attention-deficit/hyperactivity disorder (ADHD) is a common, chronic neurodevelopmental disorder characterized by inattention, hyperactivity, and impulsivity.1–3 Once thought to be largely a disorder of childhood, a growing body of evidence suggests that the symptoms of ADHD can persist into adulthood, as 60% of children with ADHD go on to have significant ADHD-related impairments in social, academic, and occupational functioning as adults.3,4 ADHD affects approximately 4.4% to 5.2% of adults between 18 and 44 years of age5,6; however, fewer than 1 of every 5 of these patients are currently diagnosed and/or treated for ADHD.7,8 There is also an increasing number of adults over the age of 50 years who are seeking assessment for ADHD for the first time, and the prevalence in older adults ranges between 2.8% and 3.5%.9 Importantly, if left untreated, adult ADHD can lead to significant functional impairments and reduced quality of life (QoL).7,10–12
Familial, twin, and adoption studies13 reported an estimated mean heritability of 76% for ADHD, making it one of the most heritable psychiatric disorders; yet, isolating the dysfunctional genes that predispose or cause ADHD has proven challenging, and research is ongoing.14 Dysregulation in dopamine and norepinephrine neurotransmission is hypothesized to be involved, and effective pharmacologic ADHD treatments target these pathways; however, the precise mechanisms underlying ADHD pathophysiology remain unclear.4,14,15 Additionally, a portion of cases may arise due to environmental factors, which play a role in susceptibility.16 Environmental factors that correlate with an increased risk of ADHD include prenatal tobacco and alcohol exposure, early exposure to various neurotoxic agents (eg, lead) or neurologic insults, and traumatic brain injury.2,3,16,17
In the United States, primary care physicians and pediatricians treat the vast majority of patients < 18 years of age with ADHD.18 Reframing ADHD as a chronic condition and filling the educational gap for patients and health care providers regarding the increasing number of adults in need of treatment for undiagnosed ADHD is of particular importance. There are profound maturational changes in ADHD-related pathology as patients progress through childhood into adulthood, highlighting the need for increased physician support and specialized behavioral interventions during transitional periods.19 ADHD remains untreated and underdiagnosed in millions of adults in the United States,5 and adults with ADHD suffer the negative consequences with social dysfunction, educational and occupational underachievement, substance abuse, increased risk of motor vehicle accidents, and legal difficulties.12,20–23
While adult ADHD symptomatology differs from the canonical childhood presentations, adults respond well to the same classes of medication used to successfully treat children.19 The psychostimulants methylphenidate and amphetamine are first-line pharmacologic interventions for ADHD and are proven efficacious in treating ADHD patients of all ages.19,24 Additionally, adults with ADHD who have been treated with stimulants prior to the age of 18 appear to have significantly better outcomes across broad QoL measurements as compared with those adult patients who were not treated with stimulants during childhood or adolescence.23
Primary care physicians are increasingly becoming responsible for screening for ADHD in undiagnosed adults and coordinating patient management for pediatric patients as they transition into adulthood. Continual access to primary care for patients with ADHD throughout adulthood is critical for improving QoL for these patients and ensuring adherence to treatment regimens.19 Until recently, physicians have largely lacked adequate resources to diagnose and treat ADHD in adults.25 Despite the updated guidelines from the American Psychiatric Association in the Diagnostic and Statistical Manual of Mental Disorders, Fifth Edition (DSM-5), with criteria to more effectively diagnose adult ADHD in comparison with the previous version (DSM-IV-TR),3,26 a clear framework supporting diagnostics and disease management for ADHD patients as they transition from pediatric to adult primary care is lacking. Owing to the evolving landscape of the diagnostic criteria for ADHD and the number of undiagnosed adults in need of treatment, it is essential to increase awareness in the primary care community about adult ADHD.27,28 In light of the DSM-5 criteria revisions in recent years, this review focuses on recognition of symptoms, diagnostic issues, successful long-term patient management strategies, and treatment options in adult ADHD.
METHODS
The objective of this article is to review the major issues, treatment regimens, and guidelines associated with adult ADHD. A systematic search strategy was used to identify relevant studies pertaining to adult ADHD. Searches were limited to English-language articles. PubMed and MEDLINE databases were searched (January 1, 1984–June 1, 2016) using combinations of keywords, including ADHD, adult, diagnosis, prevalence, symptoms, treatment, comorbidity, compliance, and guidelines. The search included meta-analyses, randomized controlled trials, clinical trials, and reviews. In addition, the Canadian Attention Deficit Hyperactivity Disorder Resource Alliance, National Institute for Health and Care Excellence, European Consensus, and Diagnostic Interview for Adult ADHD websites were searched to obtain international adult ADHD-specific guidelines, along with web-based resources describing updates to the DSM. The DSM-5 and relevant prescribing information for agents of interest were used as primary sources. In total, 143 citations1–143 were selected based on their relevance to the objective and representation of adult ADHD issues and treatment guidelines, as judged by the authors.
DSM History Leading to the Updated ADHD Nosology
Evolution of ADHD definition. The disorder currently recognized as ADHD first appeared in 1968 in the DSM-II.29 ADHD was originally termed hyperkinetic reaction of childhood, implying this disorder was defined primarily by excessive motor activity in children. In 1980, the DSM-III included problems with attention, impulsivity, and hyperactivity in the definition and renamed the disorder attention deficit disorder (with and without hyperactivity).29 The term currently in use (ADHD) was introduced in 1987 (DSM-III-R), and the 3 subtypes of ADHD defined by the presence of excessive symptoms of inattention and hyperactivity-impulsivity (predominantly inattentive, predominantly hyperactive-impulsive, and combined subtypes) were first delineated in 1994 with the publication of the DSM-IV (revised in 2000, DSM-IV-TR).29
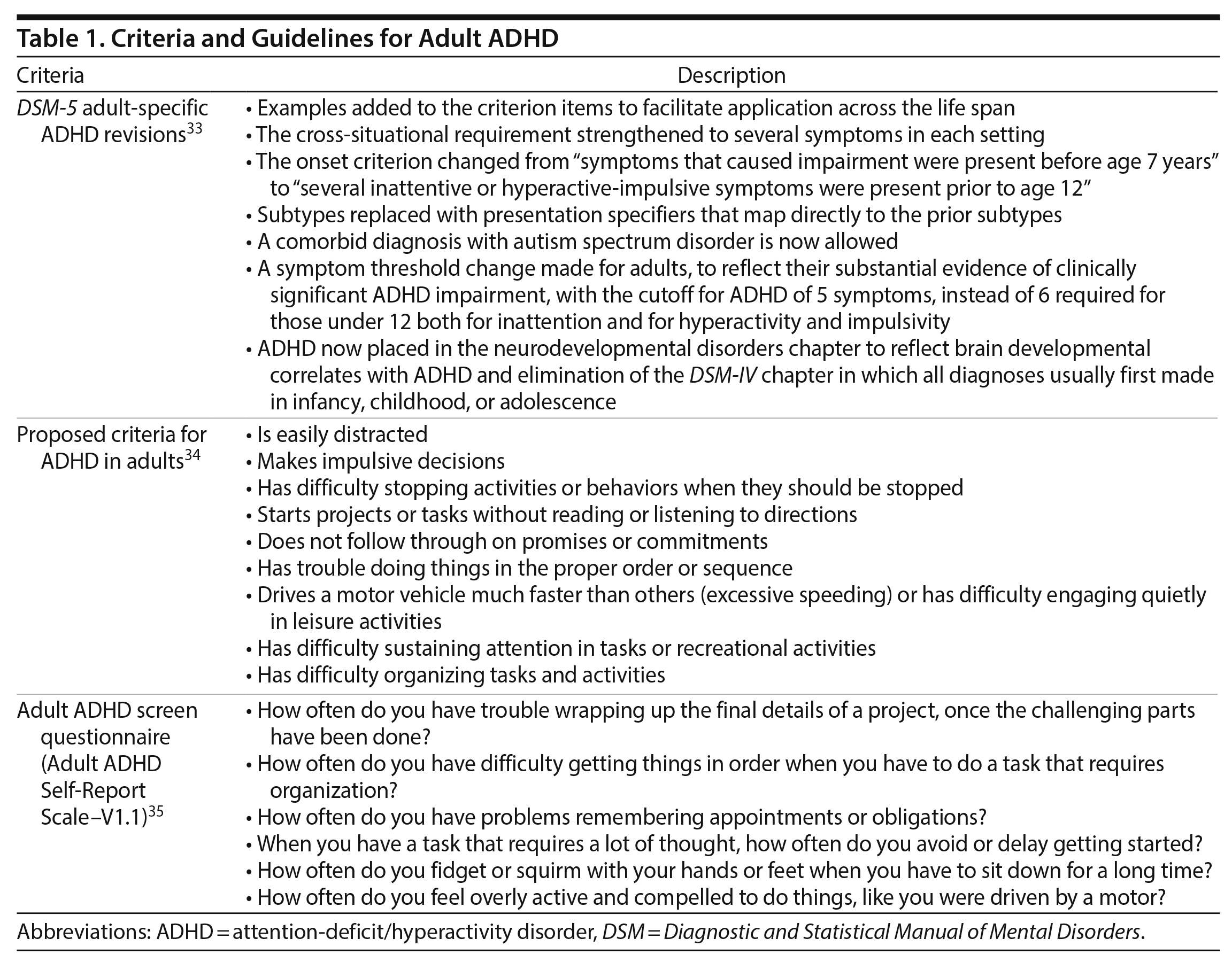
ADHD diagnostic criteria update in the DSM-5. The definition of ADHD as reflected in the DSM-5 published in 2013 represented a 14-year revision process and more accurately incorporates the symptoms of affected adults. This update reflects 2 decades of research supporting the notion that ADHD continues through adulthood for many individuals.30 Current guidelines now include the addition of specific ADHD examples across the life span and an increase in the age at onset criteria from 7 to 12 years; the latter allows for more ADHD diagnoses because of the broadened age range for the first onset.31 Additionally, fewer symptoms are now required to establish a diagnosis of adult ADHD; both inattention and hyperactivity-impulsivity criteria have been lowered for those aged 17 years and older by requiring at least 5 of 9 criteria from either domain instead of 6 of 9.3 Earlier editions of the DSM did not include adequate guidance for clinicians to diagnose adult ADHD, and through the adaptation of criteria for adults, children with ADHD can now more easily continue to receive treatment into adulthood.31,32 Further updates to ADHD nosology include the addition of the autism spectrum as a comorbidity, strengthening of the cross-situational requirement, and the replacement of ADHD subtypes described in DSM-IV with corresponding presentations.3 Lastly, modifiers enabling either the indication of severity (eg, mild, moderate, or severe) or the assessment of the current disease state if full diagnostic criteria are not currently met (eg, in partial remission) are now allowed.3 Taken together, these updates are better suited to diagnose adult ADHD (Table 1).3
Increasing Prevalence of ADHD
in Adults as a Result of DSM-5
The US National Comorbidity Survey Replication estimated that 4.4% of adults met ADHD DSM-IV diagnostic criteria, with worldwide estimates between 1.2% and 7.3% (data collected between 2001 and 2003).6,8 However, less than 15% of these adults were receiving pharmacologic or other treatment, suggesting that ADHD remains undiagnosed and untreated in the majority of cases.5 ADHD is more commonly diagnosed among adult males than females, with an odds ratio of 1.6:1.0.3 The extension of the age-of-onset criterion from 7 to 12 years in the DSM-5 has caused a direct increase in the detection rate of ADHD in 12- to 15-year-olds from 7.38% (DSM-IV) to 10.84% (DSM-5).36 The corresponding definitive statistics for increased detection of adult ADHD have not yet been made available; however, the DSM-5 revisions are expected to significantly increase overall ADHD prevalence rates in adults.37 It is critical for psychiatrists and primary care providers to familiarize themselves with the revised DSM-5 criteria in order to effectively diagnose ADHD in adults in need of proper treatment.
Clinical Presentations of ADHD in Adults
Childhood and adult ADHD exhibit related symptoms; however, there are critical differences between the two. While adults with ADHD tend to experience minimal remission of inattentive symptoms with age, symptoms of hyperactivity/impulsivity tend to dissipate more with age.38 This decline is associated with partial and, in some cases, full remission of ADHD.39 Additionally, while there is no accepted system for assessing emotionality in diagnosing ADHD, a recent study40 reported that 59% of adults with ADHD exhibited emotional dysregulation. In addition to emotional dysregulation, ADHD seems to be commonly accompanied by psychiatric comorbidities such as mood disorders in approximately 38% and anxiety disorders in approximately 47% of adults with ADHD.6,7,23 ADHD symptoms can be masked by these comorbidities, and untreated ADHD in adults with psychiatric comorbidities results in poor clinical and functional outcomes for patients even if they receive treatment for their comorbid conditions.7
Diagnostic Challenges for Adult ADHD
In some cases, adults with ADHD who have been diagnosed in childhood may no longer have access to services and treatment due to loss of coverage during the transition into adulthood.7 Therefore, timely preparation, good clinician relationships, and parental support are essential to facilitate the process of transition for young adults with ADHD. Conversely, some adults are diagnosed with ADHD without a prior childhood diagnosis. A 2004 survey-based study7,41 revealed that only 25% of adults currently diagnosed with ADHD had first received a diagnosis of ADHD prior to the age of 18. The absence of a childhood ADHD diagnosis should not disqualify adults with ADHD from being diagnosed, as at least 3 studies42,44,45 suggest that ADHD impairments may not be evident until adolescence or adulthood for some patients. The extent to which different ages of onset reflect disparate underlying causes of ADHD remains unknown.36 Individuals with adult ADHD may not have received an ADHD diagnosis in childhood due to inadequate access to care or circumstances that masked ADHD-related functional impairments. Furthermore, adults diagnosed with ADHD later in life may not have been diagnosed earlier because, prior to 2013, the DSM criteria were not validated in adults and did not include developmentally appropriate symptoms and thresholds for adults; therefore, many affected adults could not be readily identified by health care professionals.5 In addition to abatement of ADHD symptoms with age, adults may develop effective coping skills that make their impairments less evident or may choose to work in nonchallenging jobs, which may further mask the disorder.43 Lack of awareness regarding differences in how ADHD symptoms present in adult versus pediatric patients may explain the prevalence of underdiagnoses of ADHD in adults.34 Psychiatrists and primary care physicians should therefore be familiar with the presentations of adult ADHD in order to properly manage and treat ADHD and comorbid conditions.
The lack of standardized protocols for adult ADHD diagnosis poses problems for health care professionals and patients alike. There are no accepted biomarkers that are clearly indicative of an ADHD diagnosis; hence, physicians are mostly limited to qualitative assessments of symptoms.46 Diagnosing adult ADHD can be challenging, and it is important that physicians obtain a detailed psychiatric and physical history to exclude or identify comorbid medical and psychiatric disorders to facilitate effective therapy.47,48 The psychiatric conditions that commonly compound an ADHD diagnosis include depression, dysthymia, anxiety disorders, personality disorders, bipolar disorder, substance use disorder including nicotine dependence, and eating disorders.7 As substance abuse is common in adults with ADHD, it is important to assess the risks of potential drug use or criminal behavior before determining the best treatment plan.47,49 In addition, research suggests that ADHD and autism spectrum disorder frequently copresent in patients. A reported 30% to 50% of individuals diagnosed with autism spectrum disorder also have ADHD symptoms and the reported genetic correlations range from approximately 0.5 to 0.7250,51 and are associated with a greater degree of impairments in social processing, adaptive functioning, and executive control.52 Additionally, some classes of medication or substances including anticonvulsants, steroids, antihistamines, nicotine, and caffeine may have side effects that impact attentiveness and mimic ADHD symptoms, further complicating the diagnostic process.47
Diagnostic Tools for Adult ADHD
A reliable diagnosis of adult ADHD is incumbent upon a complete detailed clinical history complemented by various rating scales.47 Ideal key elements include the following: confirming the presence of current impairing ADHD-related symptoms, obtaining school records or speaking with family members to establish a childhood history, evaluating the impairments observed by self and others over the life span, assessing potential medical contributors (pregnancy exposures, repetitive head injuries, concurrent medications), obtaining a complete family history for relevant psychiatric disorders/substance abuse, and eliminating the potential contribution of concurrent acute comorbid psychiatric disorders that may mimic some symptoms of ADHD.43 The combination of the thorough history with DSM-5 screening criteria and the utilization of questionnaires proposed by various groups detailed in Table 1 serve as the best-practice guidelines for the proper identification and diagnosis of adult ADHD.34,53
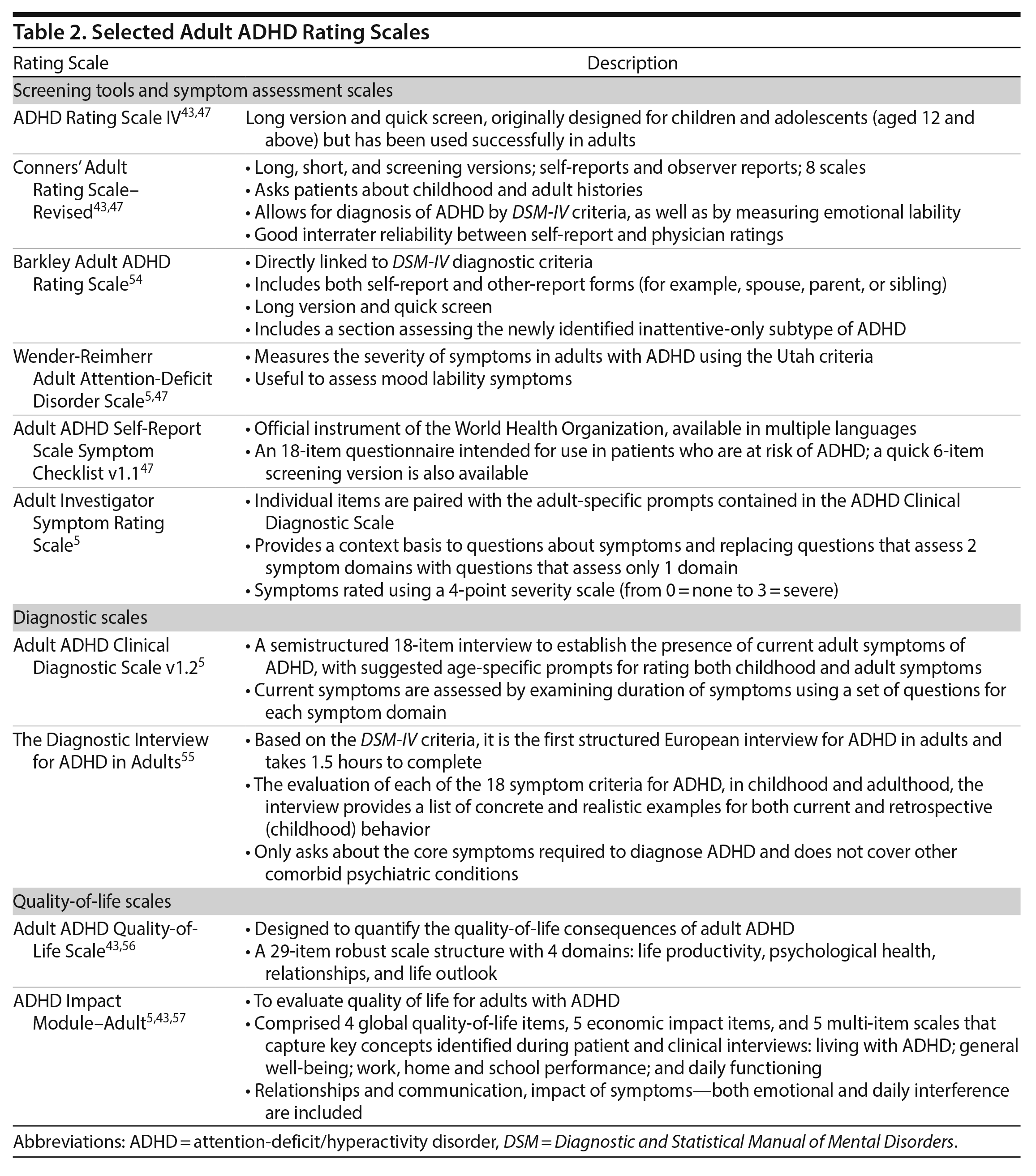
Clinical evaluation and rating scales. Adult-specific rating scales are critically helpful in diagnosing adult symptoms and presentations, while also providing metrics for measuring patient response to treatment and changes in QoL.5 In general, rating scales take 5 to 20 minutes to complete, depending on the scale.47 While these scales are useful, a critical review of responses is necessary, as patients may preferentially report symptoms in settings in which they are less impaired (ie, tasks that they find easy or interesting), which could diminish or mask their illness. Patients may also rate symptoms based on the experience with compensatory skills, thereby underrating the underlying symptom severity.5 Diagnostic interviews are critical tools to evaluate the chronicity and pervasiveness of ADHD symptoms and associated impairments and facilitate correct diagnosis of ADHD in adults.5 Descriptions of some available scales and a diagnostic interview are provided in Table 2.5,43,47
Neuropsychological testing. There is considerable interest in using neuropsychological tests as a clinical tool for ADHD assessment, as some adults with ADHD exhibit defined neuropsychological deficits such as impairments in attention, inhibition, and memory.58,59 Adults with ADHD may display slowed performance in tasks of sustained attention and set shifting, and their use of working memory may be particularly impaired.60 Neuropsychological testing is typically employed in cases of diagnostic uncertainty or for educational purposes.5 However, not all individuals with ADHD have quantifiable neuropsychological deficits; therefore, relying on neuropsychological testing exclusively may miss affected individuals.5,58 Conversely, while some clinicians believe that neuropsychological testing will “sort out the fakers” seeking stimulants, the research suggests that test results from faking may mimic deficits seen in ADHD, further confusing the diagnostic conclusion.61,62
Emerging imaging techniques. Advances in structural and functional imaging research have provided new avenues of study for ADHD disease phenotype, progression, treatment, and heritability.63 Developments in imaging techniques have revealed structural and functional brain differences between individuals with and without ADHD.63 Recent progress has been made toward understanding how ADHD affects the brain’s connectivity through mapping architectural alterations of large-scale brain networks (ie, connectomes) using techniques such as electroencephalography, functional magnetic resonance imaging (MRI), and diffusion MRI in combination with graph theoretical approaches.64 Imaging studies64–67 have revealed several neurologic differences between the brains of ADHD patients and those of healthy individuals. Positron emission tomography showed significant reductions in dopamine transporters and dopamine D2/D3 receptors in the striatum and midbrain of ADHD patients relative to healthy control subjects.64 Decreased volumes of certain brain compartments—including cerebellar regions, subcortical regions, and the total brain matter—have been observed in ADHD patients.65 ADHD also affects neurodevelopment, demonstrated by imaging-detected delayed maturation of specific brain areas as well as the whole brain functional networks in children with ADHD.64 In addition, imaging studies have shown that some ADHD patients exhibit differential activation of neural networks relative to healthy controls in response to the same task.66,67 Finally, the default networks of ADHD patients displayed structural alterations, such as redistribution of regional nodes and lower connectivity.64
The neuroimaging field is continually changing, partially due to computational abilities, allowing for the increasingly precise visualization of connectivity.68 Together, these studies highlight various manifestations of brain network dysfunction in ADHD, shedding light on the pathophysiologic mechanisms in play. However, brain imaging technologies in ADHD are still in their infancy.64 While accumulating evidence has been establishing a clear correlation between brain structural alterations and ADHD symptoms, a full view of structural and functional connectomes in ADHD is still lacking.64 In addition, there is no guidance regarding the clinical utility of the imaging findings. With the rapid progression of the field, we can expect the development of imaging-based assays for the future clinical diagnosis and treatment evaluation in ADHD.64
Treatment Options for Adult ADHD
First-line treatment–pharmacotherapy. Strategies for treating ADHD are multimodal, and the main treatment goals for patients are to improve symptoms, optimize functional performance, and remove behavioral obstacles.69 For adults, pharmacotherapy consisting of stimulants or nonstimulants is the mainstay of ADHD treatment (Table 3).32,47 Several categories of medications (antidepressants, alerting agents, cognitive enhancers) are used to treat ADHD in refractory cases even though this indication is not approved by the US Food and Drug Administration (Table 3).70

Adults and adolescents with ADHD have reported that the positive attributes of stimulant medication include improving social relationships, academic/work functionality, and driving and reducing criminal behavior.23,99–101 Conversely, the negative attributes have been reported to include physical side effects, alterations in perception of sense of self, a loss of personality, stigma associated with medication use, and the inconvenience of taking medication.99 The commonly prescribed stimulants include methylphenidate and amphetamines that are available in immediate- or extended-release formulations based on the technology of delivery.32,47 Medication satisfaction studies102 showed that extended-release medications were preferred by a greater percentage of adults based on the convenience of once-daily dosing. Recent evidence103,104 suggests that adherence and persistence rates improve in ADHD when using long-acting agents (vs short-acting) and stimulants (vs nonstimulants). Extended-release stimulants are more of an abuse deterrent than their immediate-release counterparts, as they induce less euphoria and render drug extraction difficult.105 For these reasons, international practice guidelines101,106,107 recommend extended-release over immediate-release stimulants for ADHD treatment.
Pharmacotherapy issues. Treatment of adult ADHD with psychostimulants consistently yields positive short-term effects; however, confirmation of enduring efficacy is limited, as few trials have evaluated the long-term efficacy and safety of approved ADHD medications for adults.32 Poor adherence or compliance and presence of other comorbid psychiatric disorders may further complicate the determination of treatment benefits in adults with ADHD.48 Ineffectiveness and negative side effects are the most common reasons for discontinuing treatment; however, dosing convenience may be another significant factor in adherence.103 Medication discontinuation or nonadherence is estimated to be between 13.2% and 64% for both children and adults in clinical trial populations over varying lengths of time, with the highest rate found 5 years after treatment initiation, suggesting that adherence negatively correlates with time since treatment initiation.108 However, it is critical to distinguish between side effect–mediated treatment discontinuation and discontinuation due to symptomatic remission, as improper classification may confound calculations of ADHD persistence rates or adherence.104
Formulation-related factors may affect persistence in ADHD treatment. Although definitive evidence in adults is currently lacking, unpleasant taste and difficulty swallowing medication have been reported to negatively impact adherence in children and adolescents with ADHD.109 Interestingly, difficulty swallowing solid oral dosage forms such as tablets or capsules is problematic for some adults as well as children,110 and alternative formulations could potentially improve acceptance in those patients. Giving consideration to convenience and acceptability (to patients and family/caregivers) of differing formulations is crucial to potentially improving adherence.111,112 A variety of newer formulations that circumvent problems associated with swallowing tablets or capsules have been made available (eg, transdermal patch, oral solution, chewable tablet),113 while others have just recently been approved (eg, long-acting chewable tablet, long-acting liquid, and long-acting orally disintegrating tablet).87,91,92 While stimulant-based medications have proven effective in treating adult ADHD and the risks of patients developing an addiction to stimulant medications with longer-acting preparations is low,32,105 the majority of available clinical trial data have been short term and have relied heavily on young and middle-aged adult participants.32 Further studies that assess the long-term benefits and risks in adults along with the benefits and risks in older adult patients over age 50 are warranted.9
Pharmacotherapy for refractory ADHD. While stimulants are highly effective in treating ADHD, responses may vary significantly among individual patients.114,115 For patients with suboptimal response to 1 stimulant, increasing the dose of their current medication or switching to another stimulant may be a feasible solution.115 The d-amphetamine prodrug lisdexamphetamine could be a stimulant alternative for ADHD patients with unsatisfactory response to methylphenidate or amphetamine.115 Combining stimulants with a nonstimulant medication such as atomoxetine, guanfacine, or clonidine has shown positive effects among patients who are resistant to stimulants alone.115 Patients with an insufficient response or intolerable adverse reactions may also switch to a nonstimulant, commonly atomoxetine, as monotherapy.114 In addition, some medications that are not indicated for ADHD treatment have been used “off-label” for patients who are refractory to their current pharmacotherapy. These medications include the antidepressant bupropion and tricyclic antidepressants desipramine and nortriptyline. All of these agents have demonstrated effectiveness in ADHD treatment in clinical studies.70
Cognitive-behavioral therapy. Even though pharmacologic interventions are considered first-line treatments for ADHD, some adults with ADHD are unable to take these medications or continue to experience significant residual and impairing symptoms, which has led to an increased demand for psychosocial approaches targeting ADHD.116 The cognitive-behavioral therapy (CBT) model—which includes use of higher-level organization and planning, behavioral skills training, and cognitive restructuring—has been instrumental in the treatment of adult ADHD, alone and especially in combination with psychopharmacology.116 A review of the literature comparing CBT to other psychotherapeutic modalities found that CBT is helpful as an adjuvant to medication in the treatment of ADHD in adults.117 Indeed, some studies have found CBT to be superior to medication alone.117 CBT helps reduce impairments resulting from executive dysfunction that is not optimally ameliorated with medication.117
Coaching is gaining increasing popularity as an intervention for adults with ADHD. It is a highly individualized intervention in which a personally assigned coach guides the patient in accomplishing tasks and goals.118 Coaching primarily differs from traditional CBT in that the former is more focused on solving specific problems or reaching specific goals and is more accessible to the patient on an as-needed basis. While clinical data assessing the effectiveness of ADHD coaching are limited, preliminary evidence suggests that this intervention may provide beneficial therapeutic effects when used either on its own or as part of a multimodal treatment package for adults with ADHD.118
Impact of ADHD on Adult Life
Outcomes in treated vs untreated adults with ADHD. The outcomes of adult ADHD are best examined in longitudinal studies, which have shown that pharmacologic treatment helped manage ADHD symptoms, decreased the risk of developing comorbid disorders, and improved functional outcomes.119,120 Missed diagnoses during childhood and the absence of treatment have been associated with an increased risk of substance use disorder, as well as educational, occupational, and social impairments in adaptive functioning.6,11 Several studies7,121,122 have demonstrated that adults with ADHD often suffer from educational underachievement, cannot obtain and maintain employment and were less productive due to poor time management, suffered financial hardships, were more likely to engage in criminal activity, were more likely to be divorced, and claimed a greater number of lost workdays. These symptoms can therefore translate into significant financial costs for employees with ADHD and their employers; this is demonstrated by lower household incomes for adults with ADHD compared with the incomes of unaffected individuals.20,123
The symptoms of ADHD—including poor listening skills, a tendency to interrupt others, and being constantly active and easily frustrated—can lead to tensions in relationships with family members, friends, and partners.3 For instance, adolescent women with ADHD in 1 longitudinal study124 experienced more conflict with their mothers, were involved in fewer romantic relationships, and experienced more depressive symptoms than women without ADHD. Studies9 in untreated adults with ADHD over age 50 have shown a reduced sense of self-mastery, diminished QoL, and more social isolation compared with age-matched controls.
A meta-analysis125 found that ADHD was present among 23% of adolescents and adults with various substance use disorders. ADHD also appears to correlate positively with substance use disorder. Patients with ADHD experience substance use disorder earlier, become addicted more easily, and are hospitalized more often relative to people without ADHD who have substance use disorder.126 Moreover, adults with ADHD and substance use disorder have increased rates of criminal behavior, imprisonment, and delinquency.7 Given all of the adverse consequences associated with missed diagnosis of adult ADHD and a relatively high prevalence in the general population,5 it is important for health care providers to screen for ADHD as part of every psychiatric evaluation, employing the rating scales and criteria in Tables 1 and 2.
Managing ADHD during pregnancy and the postpartum period. With increasing recognition of ADHD as a common condition in adults, specific concerns regarding the use of ADHD medication that are unique to the adult population have arisen. For example, there are concerns about effects of potential fetal exposure in pregnant women taking these medications.127 Overall, a limited number of studies have evaluated the use of ADHD medications during pregnancy and the postpartum period. Clinical data suggest that orally delivered stimulants may be transferred to breast milk,128–131 and the use of immediate-release stimulants may be correlated with low milk drug concentrations relative to the established toxic drug level.130 A register-based study132 conducted from 1999 to 2010 found that Danish women who used ADHD medication during pregnancy were more likely to experience induced abortion and miscarriage compared with those who were not exposed; however, it remains to be determined whether findings were related directly to ADHD medication or if confounding factors associated with use of ADHD medication were also involved.132
The consequences of prenatal exposure to methylphenidate remain unclear, although some small sample size studies133,134 suggest that maternal methylphenidate use may be associated with negative fetal outcomes. CBT offers a suitable alternative to medication that can sustain functioning in some women during pregnancy134; however, the benefits of stimulant use may outweigh the risks associated with in utero exposure for some patients.134 The American Academy of Pediatrics135 generally recommends breastfeeding of the newborn for at least 1 year, but specific guidance regarding breastfeeding with the use of stimulants is lacking. Importantly, very few human studies have fully explored the effects of ADHD medication on the developing fetus, with disproportionally less known about amphetamine versus methylphenidate.127 Collectively, evidence suggests that stimulant use during pregnancy is on the rise; therefore, the use of ADHD medication during pregnancy and nursing warrants further research.
Adult ADHD and sleep deprivation. ADHD patients often report sleep and wakefulness disturbances. This disturbance can be related to a close linkage between the brain systems in charge of sleep/wakefulness balance and ADHD symptomatology.136 While up to 40% of ADHD patients have a sleep disorder,137,138 the use of stimulants may also cause insomnia and sleep deprivation.136 Unlike children whose sleepiness may lead to moodiness and aggression, adults with sleep problems often feel drowsy and sluggish.139 As consequences of sleep deprivation, adult ADHD patients can often be late for work or classes and experience difficulty staying awake and alert for their daily tasks (eg, class, business meeting).136 Sleep apnea, not uncommon in adults with ADHD, needs to be ruled out in these circumstances. Some adult patients attempt to manage sleep disturbance by using over-the-counter sleep medications or alcohol; however, these approaches are not always effective and may even exacerbate ADHD symptoms.136
Solutions to sleep deprivation include regular sleep pattern and, potentially, medication. Sleep hygiene refers to the management of bedtime environmental and behavioral factors, such as maintaining a consistent bedtime and establishing routine, relaxing activities that gradually reduce wakefulness levels (eg, watching TV, listening to music).136 Patients with ADHD may adjust their stimulant dosing schedules to improve sleep. The stimulant dose should provide sufficient symptom control until evening while avoiding initial insomnia.136 If the above approaches are unsuccessful or nonapplicable, the patient may use additional medications such as melatonin, clonidine, or tricyclic antidepressants (eg, desipramine and nortriptyline) before bedtime to improve sleep.136
Managing medication side effects. ADHD medications are known to cause side effects. These side effects include increases in both blood pressure and heart rate, leading to increasing concerns that prescription stimulant use may be linked to adverse cardiovascular outcomes.140 However, a recent large population cohort study141 suggested no increased risk of acute myocardial infarction, sudden cardiac death, or stroke for current ADHD medication users relative to nonusers or infrequent users. In addition, no increased risk was found with any specific medication or longer duration of medication use.141 While the risks of serious side effects associated with stimulants and nonstimulants for treating ADHD are thought to be low for healthy adults, physicians should exercise caution when prescribing to patients with cardiovascular disease, seizure disorders, and psychosis.32
Best Practices for Physicians
Treating Adult ADHD Patients
An Internet survey25 of health care providers determined that limited experience in adult ADHD diagnosis and treatment and difficulty in distinguishing ADHD from other disorders are significant barriers to adequate care and management of adult ADHD in both primary care and psychiatry practices. This survey identified a major gap in knowledge and training and further highlights the need to educate all health care providers.25 In addition to the criteria, rating scales, and screening tools described earlier (Tables 1 and 2), there are also international guidelines106,142 that provide useful information for adult ADHD management. The third edition of the Canadian ADHD Practice Guidelines106 provides an Adult Tool Kit and also discusses the specific issues in managing adult ADHD. In addition, the National Institute for Health and Care Excellence guidelines142 and European Consensus101 have detailed chapters that cover the diagnosis and treatment of ADHD in adults. Key recommendations for practice are outlined in Table 4.

CONCLUSIONS
Between 30% and 60% of children with ADHD continue to have significant impairments as adults, and many adults are diagnosed with ADHD without a prior childhood diagnosis.3,4,7,143 However, adult ADHD as a common neuropsychiatric condition is underrecognized, underdiagnosed, and undertreated. Traditional pharmacologic interventions for ADHD are highly effective in treating adult ADHD, as trial-based data demonstrate sustained responses; however, the effects of long-term, consistent medication use are not known.32
If left untreated, adults with ADHD may experience significant functional impairments that can have a detrimental effect on psychological well-being and QoL.7 It is critical to increase and improve health care professionals’ awareness in symptom recognition and management of ADHD throughout the different life stages.43 Adult ADHD presentations are different from children, with reduced hyperactivity/impulsivity, enhanced inner tension/restlessness,7,38 and increased comorbid psychiatric disorders and substance use disorders that may complicate the diagnosis.7 Adult ADHD is primarily treated with pharmacotherapy assisted by behavior interventions, with special considerations given to adult-specific health conditions such as stimulant misuse and abuse, pregnancy and breast feeding, and cardiovascular diseases. Various criteria/guidelines summarized within can help effectively diagnose adult ADHD and highlight issues associated with the management and treatment of ADHD in adults.
The successful diagnosis and management of adult ADHD requires consideration of many facets including prior medical history and comorbid conditions. Improved clinical outcomes can be achieved by treating adult patients with an individualized, evidence-based approach.
Future Directions
Given that long-term trials with adults of all ages are lacking, the long-term benefits versus risks of pharmacologic treatments in adults with ADHD need to be evaluated.32 Additionally, it is important to design studies that evaluate adult-specific health conditions (eg, pregnancy and cardiovascular disease) and comorbidities (eg, psychiatric and physical disorders) that could potentially occur with ADHD, particularly in adults with ADHD over the age of 50. Strengthening adult-specific ADHD guidelines will provide clearer guidance and improve ADHD management among adults.
Submitted: May 26, 2016; accepted September 15, 2016.
Published online: November 17, 2016.
Drug names: atomoxetine (Strattera and others), bupropion (Wellbutrin and others), clonidine (Catapres and others), desipramine (Norpramin and others), dexmethylphenidate (Focalin and others), dextroamphetamine (Dexedrine and others), guanfacine (Intuniv and others), lisdexamfetamine (Vyvanse), methamphetamine (Desoxyn and others), methylphenidate (Ritalin and others), mixed amphetamine salts (Adderall XR and others), nortriptyline (Pamelor, Aventyl, and others).
Funding/support: Funding for this systematic review was provided by Neos Therapeutics, Inc, Grand Prairie, Texas. Editorial support was provided by Tanmayi Mankame, PhD; Liqing Xiao, PhD; and Jennifer Tyson, PhD of AlphaBioCom, LLC, King of Prussia, Pennsylvania, and was funded by Neos Therapeutics, Inc. Drs Mankame, Xiao, and Tyson report no conflicts of interest related to the subject of this article.
Role of the sponsors: The sponsors had no role in the design, analysis, interpretation, or publication of this study.
Potential conflicts of interest: Dr Young reports grants/research support/educational support from Actavis/Forest Laboratories, Alcobra, Allergan, Arbor, Daiichi Sankyo, Neos, NLS Pharma, Otsuka, Pfizer, Rhodes, Shire, Sunovion, Takeda/Lundbeck, and Teva. Dr Goodman reports consultancy support from McNeil, Teva, Lundbeck, Janssen US and Canada, OptumInsight (Ingenix Pharmaceutical Services, Inc), Sunovion, Thomson Reuters, GuidePoint Global, Otsuka, Neos, Ironshore, Rhodes Pharm, Novartis, Major League Baseball, National Football League, American Physician Institute for Advanced Professional Studies LLC, Consumer Reports, and the Children and Adults with ADHD Association and receives honoraria from WebMD, Medscape, American Professional Society of ADHD and Related Disorders, Neuroscience Education Institute, Children and Adults with ADHD Association, and Global Medication Education.
REFERENCES
1. Fredriksen M, Dahl AA, Martinsen EW, et al. Childhood and persistent ADHD symptoms associated with educational failure and long-term occupational disability in adult ADHD. Atten Defic Hyperact Disord. 2014;6(2):87–99. PubMed doi:10.1007/s12402-014-0126-1
2. Thapar A, Cooper M. Attention deficit hyperactivity disorder. Lancet. 2016;387(10024):1240–1250. PubMed doi:10.1016/s0140-6736(15)00238-x
3. American Psychiatric Association. Diagnostic and Statistical Manual of Mental Disorders. Fifth Edition. Washington, DC: American Psychiatric Association; 2013.
4. Wu J, Xiao H, Sun H, et al. Role of dopamine receptors in ADHD: a systematic meta-analysis. Mol Neurobiol. 2012;45(3):605–620. PubMed doi:10.1007/s12035-012-8278-5
5. Goodman DW. ADHD in adults: update for clinicians on diagnosis and assessment. Prim Psychiatry. 2009;16(11):38.
6. Kessler RC, Adler L, Barkley R, et al. The prevalence and correlates of adult ADHD in the United States: results from the National Comorbidity Survey Replication. Am J Psychiatry. 2006;163(4):716–723. PubMed doi:10.1176/ajp.2006.163.4.716
7. Ginsberg Y, Quintero J, Anand E, et al. Underdiagnosis of attention-deficit/hyperactivity disorder in adult patients: a review of the literature. Prim Care Companion CNS Disord. 2014;16(3):doi:10.4088/PCC.13r01600. PubMed doi:10.4088/PCC.13r01600
8. Fayyad J, De Graaf R, Kessler R, et al. Cross-national prevalence and correlates of adult attention-deficit hyperactivity disorder. Br J Psychiatry. 2007;190:402–409. PubMed doi:10.1192/bjp.bp.106.034389
9. Goodman DW, Mitchell S, Rhodewalt L, et al. Clinical presentation, diagnosis and treatment of attention-deficit hyperactivity disorder (ADHD) in older adults: a review of the evidence and its implications for clinical care. Drugs Aging. 2016;33(1):27–36. PubMed doi:10.1007/s40266-015-0327-0
10. Agarwal R, Goldenberg M, Perry R, et al. The quality of life of adults with attention deficit hyperactivity disorder: a systematic review. Innov Clin Neurosci. 2012;9(5–6):10–21. PubMed
11. Barkley RA, Fischer M, Smallish L, et al. Young adult outcome of hyperactive children: adaptive functioning in major life activities. J Am Acad Child Adolesc Psychiatry. 2006;45(2):192–202. PubMed doi:10.1097/01.chi.0000189134.97436.e2
12. Biederman J, Faraone SV, Spencer TJ, et al. Functional impairments in adults with self-reports of diagnosed ADHD: a controlled study of 1001 adults in the community. J Clin Psychiatry. 2006;67(4):524–540. PubMed doi:10.4088/JCP.v67n0403
13. Faraone SV, Mick E. Molecular genetics of attention deficit hyperactivity disorder. Psychiatr Clin North Am. 2010;33(1):159–180. PubMed doi:10.1016/j.psc.2009.12.004
14. Badgaiyan RD, Sinha S, Sajjad M, et al. Attenuated tonic and enhanced phasic release of dopamine in attention deficit hyperactivity disorder. PLoS One. 2015;10(9):e0137326. PubMed doi:10.1371/journal.pone.0137326
15. Kollins SH, Adcock RA. ADHD, altered dopamine neurotransmission, and disrupted reinforcement processes: implications for smoking and nicotine dependence. Prog Neuropsychopharmacol Biol Psychiatry. 2014;52:70–78. PubMed doi:10.1016/j.pnpbp.2014.02.002
16. Froehlich TE, Anixt JS, Loe IM, et al. Update on environmental risk factors for attention-deficit/hyperactivity disorder. Curr Psychiatry Rep. 2011;13(5):333–344. PubMed doi:10.1007/s11920-011-0221-3
17. Yang LY, Huang CC, Chiu WT, et al. Association of traumatic brain injury in childhood and attention-deficit/hyperactivity disorder: a population-based study. Pediatr Res. 2016;80(3):356–362. PubMed doi:10.1038/pr.2016.85
18. Visser SN, Zablotsky B, Holbrook JR, et al. Diagnostic experiences of children with attention-deficit/hyperactivity disorder. Natl Health Stat Rep. 2015;(81):1–7. PubMed
19. Goodman DW, Lasser RA, Babcock T, et al. Managing ADHD across the lifespan in the primary care setting. Postgrad Med. 2011;123(5):14–26. PubMed doi:10.3810/pgm.2011.09.2456
20. Biederman J, Faraone SV. The effects of attention-deficit/hyperactivity disorder on employment and household income. MedGenMed. 2006;8(3):12. PubMed
21. Biederman J, Monuteaux MC, Mick E, et al. Young adult outcome of attention deficit hyperactivity disorder: a controlled 10-year follow-up study. Psychol Med. 2006;36(2):167–179. PubMed doi:10.1017/S0033291705006410
22. Barkley RA, Murphy KR, Dupaul GI, et al. Driving in young adults with attention deficit hyperactivity disorder: knowledge, performance, adverse outcomes, and the role of executive functioning. J Int Neuropsychol Soc. 2002;8(5):655–672. PubMed doi:10.1017/S1355617702801345
23. Rasmussen K, Palmstierna T, Levander S. Differences in psychiatric problems and criminality between individuals treated with central stimulants before and after adulthood [published online ahead of print March 20, 2015]. J Atten Disord. PubMed doi:10.1177/1087054715571740
24. Wigal SB. Efficacy and safety limitations of attention-deficit hyperactivity disorder pharmacotherapy in children and adults. CNS Drugs. 2009;23(suppl 1):21–31. PubMed doi:10.2165/00023210-200923000-00004
25. Goodman DW, Surman CB, Scherer PB, et al. Assessment of physician practices in adult attention-deficit/hyperactivity disorder. Prim Care Companion CNS Disord. 2012;14(4):doi:10.4088/PCC.11m01312. PubMed doi:10.4088/PCC.11m01312
26. Martinez-Raga J, Knecht C, Szerman N, et al. Risk of serious cardiovascular problems with medications for attention-deficit hyperactivity disorder. CNS Drugs. 2013;27(1):15–30. PubMed doi:10.1007/s40263-012-0019-9
27. Young S, Murphy CM, Coghill D. Avoiding the ‘twilight zone’: recommendations for the transition of services from adolescence to adulthood for young people with ADHD. BMC Psychiatry. 2011;11:174. PubMed doi:10.1186/1471-244X-11-174
28. Goodman DW. Unmasking ADHD in adults. Medscape Web site. http://www.medscape.org/viewarticle/768677. Updated 2012. Accessed April 6, 2016.
29. Epstein JN, Loren RE. Changes in the definition of ADHD in DSM-5: subtle but important. Neuropsychiatry (London). 2013;3(5):455–458. PubMed doi:10.2217/npy.13.59
30. Shekim WO, Asarnow RF, Hess E, et al. A clinical and demographic profile of a sample of adults with attention deficit hyperactivity disorder, residual state. Compr Psychiatry. 1990;31(5):416–425. PubMed doi:10.1016/0010-440X(90)90026-O
31. American Psychiatric Association. DSM-5 Fact Sheet 2013. http://www.dsm5.org/documents/adhd%20fact%20sheet.pdf. Accessed 02/10/2016.
32. Volkow ND, Swanson JM. Clinical practice: adult attention deficit-hyperactivity disorder. N Engl J Med. 2013;369(20):1935–1944. PubMed
33. American Psychiatric Association. Highlights of Changes From DSM-IV-TR to DSM-5. Washington, DC: American Psychiatric Association Publishing; 2013:13.doi:10.1056/NEJMcp1212625
34. Barkley RA, Brown TE. Unrecognized attention-deficit/hyperactivity disorder in adults presenting with other psychiatric disorders. CNS Spectr. 2008;13(11):977–984. PubMed doi:10.1017/S1092852900014036
35. Adult ADHD Self-Report Scale–V1. 1 (ASRS-V1.1). https://www.hcp.med.harvard.edu/ncs/ftpdir/adhd/6Q_ASRS_English.pdf. Accessed May 12, 2016.
36. Vande Voort JL, He JP, Jameson ND, et al. Impact of the DSM-5 attention-deficit/hyperactivity disorder age-of-onset criterion in the US adolescent population. J Am Acad Child Adolesc Psychiatry. 2014;53(7):736–744. PubMed doi:10.1016/j.jaac.2014.03.005
37. Steinau S. Diagnostic criteria in attention deficit hyperactivity disorder—changes in DSM-5. Front Psychiatry. 2013;4:49. PubMed doi:10.3389/fpsyt.2013.00049
38. Biederman J, Mick E, Faraone SV. Age-dependent decline of symptoms of attention deficit hyperactivity disorder: impact of remission definition and symptom type. Am J Psychiatry. 2000;157(5):816–818. PubMed doi:10.1176/appi.ajp.157.5.816
39. Karam RG, Breda V, Picon FA, et al. Persistence and remission of ADHD during adulthood: a 7-year clinical follow-up study. Psychol Med. 2015;45(10):2045–2056. PubMed doi:10.1017/S0033291714003183
40. Reimherr FW, Marchant BK, Gift TE, et al. Types of adult attention-deficit hyperactivity disorder (ADHD): baseline characteristics, initial response, and long-term response to treatment with methylphenidate. Atten Defic Hyperact Disord. 2015;7(2):115–128. PubMed doi:10.1007/s12402-015-0176-z
41. Faraone SV, Spencer TJ, Montano CB, et al. Attention-deficit/hyperactivity disorder in adults: a survey of current practice in psychiatry and primary care. Arch Intern Med. 2004;164(11):1221–1226. PubMed doi:10.1001/archinte.164.11.1221
42. Agnew-Blais JC, Polanczyk GV, Danese A, et al. Evaluation of the persistence, remission, and emergence of attention-deficit/hyperactivity disorder in young adulthood. JAMA Psychiatry. 2016;73(7):713–720. PubMed doi:10.1001/jamapsychiatry.2016.0465
43. Turgay A, Goodman DW, Asherson P, et al; ADHD Transition Phase Model Working Group. Lifespan persistence of ADHD: the life transition model and its application. J Clin Psychiatry. 2012;73(2):192–201. PubMed
44. Caye A, Rocha TB, Anselmi L, et al. Attention-deficit/hyperactivity disorder trajectories from childhood to young adulthood: evidence from a birth cohort supporting a late-onset syndrome. JAMA Psychiatry. 2016;73(7):705–712.
45. Oehrlein EM, Burcu M, Safer DJ, et al. National trends in ADHD diagnosis and treatment: comparison of youth and adult office-based visits. Psychiatr Serv. 2016;67(9):964–969.
46. Paris J, Bhat V, Thombs B. Is adult attention-deficit hyperactivity disorder being overdiagnosed? Can J Psychiatry. 2015;60(7):324–328. PubMed
47. Post RE, Kurlansik SL. Diagnosis and management of adult attention-deficit/hyperactivity disorder. Am Fam Physician. 2012;85(9):890–896. PubMed
48. Newcorn JH, Weiss M, Stein MA. The complexity of ADHD: diagnosis and treatment of the adult patient with comorbidities. CNS Spectr. 2007;12(suppl 12):1–14, quiz 15–16. PubMed doi:10.1017/S1092852900026158
49. Charach A, Yeung E, Climans T, et al. Childhood attention-deficit/hyperactivity disorder and future substance use disorders: comparative meta-analyses. J Am Acad Child Adolesc Psychiatry. 2011;50(1):9–21. PubMed doi:10.1016/j.jaac.2010.09.019
50. Leitner Y. The co-occurrence of autism and attention deficit hyperactivity disorder in children—what do we know? Front Hum Neurosci. 2014;8:268. PubMed doi:10.3389/fnhum.2014.00268
51. Davis NO, Kollins SH. Treatment for co-occurring attention deficit/hyperactivity disorder and autism spectrum disorder. Neurotherapeutics. 2012;9(3):518–530. PubMed doi:10.1007/s13311-012-0126-9
52. Murray MJ. Attention-deficit/hyperactivity disorder in the context of autism spectrum disorders. Curr Psychiatry Rep. 2010;12(5):382–388. PubMed doi:10.1007/s11920-010-0145-3
53. Kooij JJS. Adult ADHD: Diagnostic Assessment and Treatment. 3rd ed. London, UK; New York, NY: Springer; 2013. doi:10.1007/978-1-4471-4138-9
54. Barkley RA. Barkley Adult ADHD Rating Scale—IV (BAARS-IV). New York, New York: Guilford Press; 2011.
55. Kooij J. Diagnostic Interview for ADHD in Adults 2.0 (DIVA 2.0) adult ADHD. Diagnostic Assessment and Treatment. Amsterdam, The Netherlands: Pearson Assessment and Information BV; 2010.
56. Brod M, Johnston J, Able S, et al. Validation of the Adult Attention-Deficit/Hyperactivity Disorder Quality-of-Life Scale (AAQoL): a disease-specific quality-of-life measure. Qual Life Res. 2006;15(1):117–129. PubMed doi:10.1007/s11136-005-8325-z
57. Landgraf JM. Monitoring quality of life in adults with ADHD: reliability and validity of a new measure. J Atten Disord. 2007;11(3):351–362. PubMed doi:10.1177/1087054707299400
58. Seidman LJ. Neuropsychological functioning in people with ADHD across the lifespan. Clin Psychol Rev. 2006;26(4):466–485. PubMed doi:10.1016/j.cpr.2006.01.004
59. Hervey AS, Epstein JN, Curry JF. Neuropsychology of adults with attention-deficit/hyperactivity disorder: a meta-analytic review. Neuropsychology. 2004;18(3):485–503. PubMed doi:10.1037/0894-4105.18.3.485
60. Gallagher R, Blader J. The diagnosis and neuropsychological assessment of adult attention deficit/hyperactivity disorder: scientific study and practical guidelines. Ann N Y Acad Sci. 2001;931:148–171. PubMed doi:10.1111/j.1749-6632.2001.tb05778.x
61. Harrison AG, Edwards MJ, Parker KC. Identifying students faking ADHD: preliminary findings and strategies for detection. Arch Clin Neuropsychol. 2007;22(5):577–588. PubMed doi:10.1016/j.acn.2007.03.008
62. Lee Booksh R, Pella RD, Singh AN, et al. Ability of college students to simulate ADHD on objective measures of attention. J Atten Disord. 2010;13(4):325–338. PubMed doi:10.1177/1087054708329927
63. Friedman LA, Rapoport JL. Brain development in ADHD. Curr Opin Neurobiol. 2015;30:
106–111. PubMed doi:10.1016/j.conb.2014.11.007
64. Cao M, Shu N, Cao Q, et al. Imaging functional and structural brain connectomics in attention-deficit/hyperactivity disorder. Mol Neurobiol. 2014;50(3):1111–1123. PubMed doi:10.1007/s12035-014-8685-x
65. Onnink AMH, Zwiers MP, Hoogman M, et al. Brain alterations in adult ADHD: effects of gender, treatment and comorbid depression. Eur Neuropsychopharmacol. 2014;24(3):397–409. PubMeddoi:10.1016/j.euroneuro.2013.11.011
66. Dibbets P, Evers EA, Hurks PP, et al. Differential brain activation patterns in adult attention-deficit hyperactivity disorder (ADHD) associated with task switching. Neuropsychology. 2010;24(4):413–423. PubMed doi:10.1037/a0018997
67. Epstein JN, Delbello MP, Adler CM, et al. Differential patterns of brain activation over time in adolescents with and without attention deficit hyperactivity disorder (ADHD) during performance of a sustained attention task. Neuropediatrics.
2009;40(1):1–5. PubMed doi:10.1055/s-0029-1220686
68. Minati L, Varotto G, D’Incerti L, et al. From brain topography to brain topology: relevance of graph theory to functional neuroscience. Neuroreport. 2013;24(10):536–543. PubMed doi:10.1097/WNR.0b013e3283621234
69. Felt BT, Biermann B, Christner JG, et al. Diagnosis and management of ADHD in children. Am Fam Physician. 2014;90(7):456–464. PubMed
70. Pliszka S; AACAP Work Group on Quality Issues. Practice parameter for the assessment and treatment of children and adolescents with attention-deficit/hyperactivity disorder. J Am Acad Child Adolesc Psychiatry. 2007;46(7):894–921. P
72. Methylin and Methylin ER [package insert]. Hazelwood MO: Mallinckrodt Inc; 2015.
73. Focalin [package insert]. East Hanover, NJ: Novartis Pharmaceutical Corporation; 2015.
74. Adderall [package insert]. Pomona, NY: Barr Laboratories, Inc; 2007.
75. Evekeo [package insert]. Atlanta, GA:
Arbor Pharmaceuticals, LLC; 2015.
76. Desoxyn [package insert]. Deerfield, IL: Ovation Pharmaceuticals, Inc; 2007.
77. Dextrostat [package insert]. Middlesex, NJ: CorePharma, LLC; 2015.
78. ProCentra [package insert]. Newport, KY: Independence Pharmaceuticals; 2015.
79. Zenzedi [package insert]. Atalanta GA: Mikart Inc; 2014.
80. Concerta [package insert]. Titusville, NJ: Janssen Pharmaceuticals, Inc; 2013.
81. Metadate CD [package insert]. Smyrna, GA: UCB Inc; 2014.
82. Ritalin LA [package insert]. East Hanover, NJ: Novartis Pharmaceuticals Co; 2015.
83. Metadate ER [package insert]. Smyrna, GA: Upstate Pharma, LLC; 2014.
84. Daytrana [package insert]. Miami, FL: Noven
85. Quillivant XR [package insert]. Cupertino, CA: NextWave Pharmaceuticals, Inc; 2012.
86. Aptensio XR [package insert]. Coventry, RI: Rhodes Pharmaceuticals LP; 2015.
87. Quillichew ER [package insert]. New York, NY: NextWave Pharmaceuticals Inc; 2015.
88. Methylin ER [package insert]. Hazelwood, MO: Mallinckrodt Pharmaceuticals, Inc; 2015.
89. Focalin XR [package insert]. East Hanover, NJ: Novartis Pharmaceuticals Co; 2015.
90. Adderall XR [package insert]. Wayne, PA: Shire US Inc; 2015.
91. Adzenys XR-ODT [package insert]. Grand Prairie, TX: Neo Therapeutics; 2016.
92. Dyanavel XR [package insert]. Monmouth Junction, NJ: Tris Pharma, Inc; 2015.
93. Dexedrine [package insert]. Horsham, PA: Amedra Pharmaceuticals LLC; 2015.
94. Vyvanse [package insert]. Wayne, PA: Shire US Inc; 2015.
95. Strattera [package insert]. Indianapolis, IN: Lilly USA, LLC; 2015.
96. Intuniv [package insert]. Lexington,MA: Shire US Inc; 2016.
97. Wellbutrin [package insert]. Bridgewater, NJ: Valeant Pharmaceuticals North America LLC; 2014.
98. Norpramin [package insert]. Bridge water, NJ: Sanofi-Aventis U.S. LLC; 2014.
100. Lichtenstein P, Larsson H. Medication for attention deficit-hyperactivity disorder and criminality. N Engl J Med. 2013;368(8):776. PubMed
101. Kooij SJ, Bejerot S, Blackwell A, et al. European consensus statement on diagnosis and treatment of adult ADHD: The European Network Adult ADHD. BMC Psychiatry. 2010;10:67. PubMed doi:10.1186/1471-244X-10-67
102. Kolar D, Keller A, Golfinopoulos M, et al. Treatment of adults with attention-deficit/hyperactivity disorder. Neuropsychiatr Dis Treat. 2008;4(2):389–403. PubMed
103. Gajria K, Lu M, Sikirica V, et al. Adherence, persistence, and medication discontinuation in patients with attention-deficit/hyperactivity disorder—a systematic literature review. Neuropsychiatr Dis Treat. 2014;10:1543–1569. PubMed
104. Ahmed R, Aslani P. Attention-deficit/hyperactivity disorder: an update on medication adherence and persistence in children, adolescents and adults. Expert Rev Pharmacoecon Outcomes Res. 2013;13(6):791–815. PubMed doi:10.1586/14737167.2013.841544
105. Wilens TE, Adler LA, Adams J, et al. Misuse and diversion of stimulants prescribed for ADHD: a systematic review of the literature. J Am Acad Child Adolesc Psychiatry. 2008;47(1):21–31. PubMed doi:10.1097/chi.0b013e31815a56f1
106. Canadian ADHD Practice Guidelines. 3rd ed. Toronto, Canada: Canadian Attention Deficit Hyperactivity Disorder Resource Alliance (CADDRA); 2011.
107. Rabito-Alcón MF, Correas-Lauffer J. Treatment guidelines for attention deficit and hyperactivity disorder: a critical review. Actas Esp Psiquiatr. 2014;42(6):315–324. PubMed
108. Adler LD, Nierenberg AA. Review of medication adherence in children and
adults with ADHD. Postgrad Med. 2010;122(1):184–191. PubMed doi:10.3810/pgm.2010.01.2112
109. Walker-Noack L, Corkum N, Elik N, et al. Youth perceptions of attention-deficit/ hyperactivity disorder and barriers to treatment. Can J Sch Psychol. 2013;28(2):193–218. doi:10.1177/0829573513491232
110. Bhosle M, Benner JS, Dekoven M, et al. Difficult to swallow: patient preferences for alternative valproate pharmaceutical formulations. Patient Prefer Adherence. 2009;3:161–171. PubMed doi:10.2147/PPA.S5691
111. Hodgkins P, Shaw M, Coghill D, et al. Amfetamine and methylphenidate medications for attention-deficit/hyperactivity disorder: complementary treatment options. Eur Child Adolesc Psychiatry. 2012;21(9):477–492. PubMed doi:10.1007/s00787-012-0286-5
112. Wolraich M, Brown L, Brown RT, et al; Subcommittee on Attention-Deficit/Hyperactivity Disorder; Steering Committee on Quality Improvement and Management. ADHD: clinical practice guideline for the diagnosis, evaluation, and treatment of attention-deficit/hyperactivity disorder in children and adolescents. Pediatrics. 2011;128(5):1007–1022. PubMed doi:10.1542/peds.2011-2654
113. Chavez B, Sopko MA Jr, Ehret MJ, et al. An update on central nervous system stimulant formulations in children and adolescents with attention-deficit/hyperactivity disorder. Ann Pharmacother. 2009;43(6):1084–1095. PubMed doi:10.1345/aph.1L523
114. Antshel KM, Hargrave TM, Simonescu M, et al. Advances in understanding and treating ADHD. BMC Med. 2011;9:72. PubMed doi:10.1186/1741-7015-9-72
115. Shim SH, Yoon HJ, Bak J, et al. Clinical and neurobiological factors in the management of treatment refractory attention-deficit hyperactivity disorder. Prog Neuropsychopharmacol Biol Psychiatry. 2016;70:237–244. PubMed doi:10.1016/j.pnpbp.2016.04.007
116. Knouse LE, Safren SA. Current status of cognitive behavioral therapy for adult attention-deficit hyperactivity disorder. Psychiatr Clin North Am. 2010;33(3):497–509. PubMed doi:10.1016/j.psc.2010.04.001
117. Chandler ML. Psychotherapy for adult attention deficit/hyperactivity disorder: a comparison with cognitive behaviour therapy. J Psychiatr Ment Health Nurs. 2013;20(9):814–820. PubMed
118. Knouse LE, Cooper-Vince C, Sprich S, et al. Recent developments in the psychosocial treatment of adult ADHD. Expert Rev Neurother. 2008;8(10):1537–1548. PubMed doi:10.1586/14737175.8.10.1537
119. Bihlar Muld B, Jokinen J, Bölte S, et al. Long-term outcomes of pharmacologically treated versus non-treated adults with ADHD and substance use disorder: a naturalistic study. J Subst Abuse Treat. 2015;51:82–90. PubMed doi:10.1016/j.jsat.2014.11.005
120. Uchida M, Spencer TJ, Faraone SV, et al. Adult outcome of ADHD: an overview of results from the MGH Longitudinal Family Studies of Pediatrically and Psychiatrically Referred Youth with and without ADHD of both sexes [published online ahead of print September 22, 2015]. J Atten Disord. PubMed
121. de Graaf R, Kessler RC, Fayyad J, et al. The prevalence and effects of adult attention-deficit/hyperactivity disorder (ADHD) on the performance of workers: results from the WHO World Mental Health Survey Initiative. Occup Environ Med. 2008;65(12):835–842. PubMed doi:10.1136/oem.2007.038448
122. Brook JS, Brook DW, Zhang C, et al. Adolescent ADHD and adult physical and mental health, work performance, and financial stress. Pediatrics. 2013;131(1):5–13. PubMed doi:10.1542/peds.2012-1725
123. Doshi JA, Hodgkins P, Kahle J, et al. Economic impact of childhood and adult attention-deficit/hyperactivity disorder in the United States. J Am Acad Child Adolesc Psychiatry. 2012;51(10):990–1002.e2. PubMed doi:10.1016/j.jaac.2012.07.008
124. Babinski DE, Pelham WE Jr, Molina BS, et al. Late adolescent and young adult outcomes of girls diagnosed with ADHD in childhood: an exploratory investigation. J Atten Disord. 2011;15(3):204–214. PubMed doi:10.1177/1087054710361586
125. van Emmerik-van Oortmerssen K, van de Glind G, van den Brink W, et al. Prevalence of attention-deficit hyperactivity disorder in substance use disorder patients: a meta-analysis and meta-regression analysis. Drug Alcohol Depend. 2012;122(1–2):11–19. PubMed doi:10.1016/j.drugalcdep.2011.12.007
126. Arias AJ, Gelernter J, Chan G, et al. Correlates of co-occurring ADHD in drug-dependent subjects: prevalence and features of substance dependence and psychiatric disorders. Addict Behav. 2008;33(9):1199–1207. PubMed doi:10.1016/j.addbeh.2008.05.003
127. Louik C, Kerr S, Kelley KE, et al. Increasing use of ADHD medications in pregnancy. Pharmacoepidemiol Drug Saf. 2015;24(2):218–220. PubMed doi:10.1002/pds.3742
128. Hackett LP, Kristensen JH, Hale TW, et al. Methylphenidate and breast-feeding. Ann Pharmacother. 2006;40(10):1890–1891. PubMed doi:10.1345/aph.1H159
129. Ilett KF, Hackett LP, Kristensen JH, et al. Transfer of dexamphetamine into breast milk during treatment for attention deficit hyperactivity disorder. Br J Clin Pharmacol. 2007;63(3):371–375. PubMed doi:10.1111/j.1365-2125.2006.02767.x
130. Spigset O, Brede WR, Zahlsen K. Excretion of methylphenidate in breast milk. Am J Psychiatry. 2007;164(2):348. PubMed doi:10.1176/ajp.2007.164.2.348
131. Steiner E, Villén T, Hallberg M, et al. Amphetamine secretion in breast milk. Eur J Clin Pharmacol. 1984;27(1):123–124. PubMed doi:10.1007/BF02395219
132. Haervig KB, Mortensen LH, Hansen AV, et al. Use of ADHD medication during pregnancy from 1999 to 2010: a Danish register-based study. Pharmacoepidemiol Drug Saf. 2014;23(5):526–533. PubMed doi:10.1002/pds.3600
133. Bolea-Alamanac BM, Green A, Verma G, et al. Methylphenidate use in pregnancy and lactation: a systematic review of evidence. Br J Clin Pharmacol. 2014;77(1):96–101. PubMed doi:10.1111/bcp.12138
134. Freeman MP. ADHD and pregnancy. Am J Psychiatry. 2014;171(7):723–728. PubMed doi:10.1176/appi.ajp.2013.13050680
135. American Academy of Pediatrics. Breastfeeding and the use of human milk. Pediatrics. 2012;129(3): e827–e841. PubMed doi:10.1542/peds.2011-3552
136. Brown TE, McMullen WJ Jr. Attention deficit disorders and sleep/arousal disturbance. Ann N Y Acad Sci. 2001;931:271–286. PubMed doi:10.1111/j.1749-6632.2001.tb05784.x
137. Gau SS, Kessler RC, Tseng WL, et al. Association between sleep problems and symptoms of attention-deficit/hyperactivity disorder in young adults. Sleep. 2007;30(2):195–201. PubMed
138. Kooij JJ, Bijlenga D. The circadian rhythm in adult attention-deficit/hyperactivity disorder: current state of affairs. Expert Rev Neurother. 2013;13(10):1107–1116. PubMed doi:10.1586/14737175.2013.836301
139. National Sleep Foundation. ADHD and sleep. Sleep Foundation Web site. https://sleepfoundation.org/sleep-disorders-problems/adhd-and-sleep. Accessed August 23, 2016.
140. Schelleman H, Bilker WB, Kimmel SE, et al. Methylphenidate and risk of serious cardiovascular events in adults. Am J Psychiatry. 2012;169(2):178–185. PubMed doi:10.1176/appi.ajp.2011.11010125
141. Habel LA, Cooper WO, Sox CM, et al. ADHD medications and risk of serious cardiovascular events in young and middle-aged adults. JAMA. 2011;306(24):2673–2683. PubMed doi:10.1001/jama.2011.1830
142. National Collaborating Centre for Mental Health (UK). Attention Deficit Hyperactivity Disorder. Diagnosis and Management of ADHD in Children, Young People and Adults. NICE Clinical Guidelines, No. 72. Leicester, UK: British Psychological Society (UK); 2009.
143. Moffitt TE, Houts R, Asherson P, et al. Is adult ADHD a childhood-onset neurodevelopmental disorder? evidence from a four-decade longitudinal cohort study. Am J Psychiatry. 2015;172(10):967–977. PubMed doi:10.1176/appi.ajp.2015.14101266
Enjoy this premium PDF as part of your membership benefits!

